* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Haynes, J
Survey
Document related concepts
Transcript
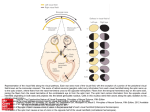
Sphenoidal Wing Meningioma Diagnosis Complicated by Existing Vision Loss from Optic Disc Drusen Abstract 44 year-old female with history of optic disc drusen presents with monocular vision loss. Optometrically guided radiological workup reveals compressive parasellar meningioma. Serial visual fields demonstrate tumor induced functional decline and resolution post neurosurgical resection. Case History 44 year-old Caucasian female presents with a chief complaint of insidious loss of vision over the past 8 months. The patient’s ocular history is remarkable for visual field loss OU secondary to bilateral optic disc drusen and reduced central acuity OS. The patient’s medical history is positive for migraine headaches and systemic allergies. She notes no recent headaches or neurological changes. The patient has no other pertinent medical history. The patient’s current medications include, loratidine 10 mg qday, methocarbamol 500 mg qhs prn, naproxen 250 mg bid, and promethazine 25 mg q6hours prn. Pertinent Findings BCVA were 20/20 OD and 20/150+ OS. A mild APD was noted OS. EOMs were full. Amsler grid findings were normal OD, but the patient had difficulty seeing the entire grid OS and reported that all lines appeared slanted and wavy. Slit lamp exam findings were normal. Dilated eye examination showed normal retinal structures with normal macular findings. Optic disc drusen were noted OS>OD as previously described in prior exam findings, and were consistent with prior photo documentation. OCT of macula was performed showing normal findings OU. OCT of the retinal nerve fiber layer, although it showed thinning of the RNFL based on normative databases OU, showed no changes from prior readings. Humphrey visual field showed a stable superior nasal defect OD, but the OS field showed substantial change from prior readings. Scattered defects had previously been documented OS, but new paracentral defects were now present, dropping the VFI from 71% to 51%. The mean deviation had also decreased from -13.29 dB to -19.44 dB in the span of less than one year. MRI of the brain with and without contrast revealed a 3.2cm lesion located at the midline, superior to the pituitary gland, and inferior to the optic chiasm. The lesion’s anterior base was located on the planum sphenoidale and it extended posteriorly to the posterior-most portion of the pituitary fossa. Differential Diagnoses · Compressive space occupying lesion · Optic disc drusen · NAAION Diagnosis and Discussion The lesion was identified as a sphenoidal wing meningioma. The decision to pursue further testing and identify the lesion could have been compromised by the patient’s prior diagnosis of optic disc drusen. Had the visual changes been misattributed to the drusen, the correct diagnosis could have substantially been delayed. According to at least one study on suprasellar meningiomas, delay of treatment was shown to be a prognostic factor for poorer visual outcomes. 1 This type of vision loss is not typical of drusen; especially with no change in the appearance of the drusen from baseline photo documentation or changes to the retinal nerve fiber layer with OCT imaging, as certain studies have shown visual field defects correspond with progressively thinner nerve fiber layer on OCT.2,3,4 Field defects most typical of optic nerve drusen include arcuate defects, enlarged blind spot, and generalized constriction of the field. Effects on central visual field and visual acuity are less common, and more often are associated with secondary problems related to optic disc drusen such as ischemic optic neuropathy5,6. Meningiomas are about twice as likely to be found in women as in men, and typically occur in patients aged 40-80. Most meningiomas are benign, and can remain asymptomatic for long durations of time until they finally cause symptoms from compression of nearby structures, as was the case with this patient. Meningiomas located near the sphenoid bone can often compress the optic nerve and lead to unilateral vision loss. They may also compress the cavernous sinus and cause diplopia or numbness of the face, complaints which this patient did not describe.7 Treatment/Management The patient was scheduled shortly after diagnosis for surgery to remove the tumor. After successful removal of the mass with orbitofrontal craniotomy resection, the patient’s vision improved to 20/30. The visual field also showed significant improvement in the paracentral defects that were previously present. VFI increased to 81%, and mean deviation improved to -9.70 dB. Conclusion This case demonstrates the pivotal role that optometrists can play in a patient’s healthcare. For this patient, a compressive lesion in the brain initially presented with ocular complications before any other symptoms were experienced. Had proper measures not been taken to identify the correct underlying cause of the vision loss, treatment for the patient could have been significantly delayed, and the visual outcome could have been adversely affected. Works Cited 1. Zevgaridis, D., R. J. Medele, A. Muller, A. C. Hischa, and H.-J. Steiger. "Meningiomas of the Sellar Region Presenting with Visual Impairment: Impact of Various Prognostic Factors on Surgical Outcome in 62 Patients." Acta Neurochirurgica 143.5 (2001): 471-76. 2. Roh S, Noecker RJ, Schuman JS, Hedges TR, 3rd, Weiter JJ, Mattox C. “Effect of optic nerve head drusen on nerve fiber layer thickness.” Ophthalmology. 1998;105:878–85. 3. Gili, Pablo, Patricia Flores-Rodríguez, María Dolores Martin-Ríos, and Carmen Carrasco Font. "Anatomical and Functional Impairment of the Nerve Fiber Layer in Patients with Optic Nerve Head Drusen." Graefes Arch Clin Exp.10 (2013): 2421-428. 4. Casado, Alfonso, Gema Rebolleda, Laura Guerrero, Marina Leal, Inés Contreras, Noelia Oblanca, and Francisco J. Muñoz-Negrete. "Measurement of Retinal Nerve Fiber Layer and Macular Ganglion Cell–inner Plexiform Layer with Spectral-domain Optical Coherence Tomography in Patients with Optic Nerve Head Drusen." Graefes Arch Clin Exp Ophthalmol Graefe's Archive for Clinical and Experimental Ophthalmology 252.10 (2014): 1653-660. 5. Lee, A., and M. Zimmerman. "The Rate of Visual Field Loss in Optic Nerve Head Drusen." American Journal of Ophthalmology 139.6 (2005): 1062-066 6. Obuchowska, and Z. Mariak. "[Visual Field Defects in the Optic Disc Drusen]." Klin Oczna 12th ser. 110.10 (2008): 357-60. Web 7. "Facts about Meningiomas." Brigham and Women's Hospital, 27 Feb. 2015. Web. 13 Aug. 2015. <http://www.brighamandwomens.org/Departments _and_Services/ neurosurgery/meningioma/meningiomafacts.aspx>