* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download PDF - Oftalmo.com
Survey
Document related concepts
Bevacizumab wikipedia , lookup
Eyeglass prescription wikipedia , lookup
Visual impairment wikipedia , lookup
Vision therapy wikipedia , lookup
Idiopathic intracranial hypertension wikipedia , lookup
Blast-related ocular trauma wikipedia , lookup
Retinitis pigmentosa wikipedia , lookup
Fundus photography wikipedia , lookup
Mitochondrial optic neuropathies wikipedia , lookup
Macular degeneration wikipedia , lookup
Transcript
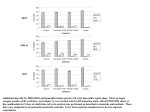
ARCH SOC ESP OFTALMOL 2008; 83: 615-618 SHORT COMMUNICATION OPTICAL COHERENCE TOMOGRAPHY STUDY IN TAMOXIFEN MACULOPATHY MACULOPATÍA POR TAMOXIFENO. ESTUDIO MEDIANTE LA TOMOGRAFÍA DE COHERENCIA ÓPTICA BAGET-BERNALDIZ M1, SOLER LLUIS N1, ROMERO-AROCA P2, TRAVESET-MAESO A1 ABSTRACT RESUMEN Case report: We describe the case of a patient who presented with progressive and bilateral loss of vision. She had been treated with tamoxifen for 13 years. We performed fluorescein angiography and optical coherence tomography in order to study the macula. Discussion: Loss of visual acuity related to tamoxifen maculopathy may be caused either by retinal nerve fibre atrophy or macular oedema. Macular findings obtained by fluorescein angiography and optical coherence tomography are complementary (Arch Soc Esp Oftalmol 2008; 83: 615-618). Caso clínico: Se describe el caso de una paciente que acudió por pérdida bilateral y progresiva de la visión después de haber recibido tratamiento con tamoxifeno durante 13 años. Para el estudio detallado de las alteraciones maculares se realizaron la angiografía fluoresceínica y la tomografía de coherencia óptica. Discusión: La pérdida de visión debido a la maculopatía por tamoxifeno puede ser debida tanto a la atrofia de las capas de fibras nerviosas de la retina como a la presencia de edema macular. Los hallazgos maculares obtenidos mediante la angiografía fluoresceínica y la tomografía de coherencia óptica son complementarios. Key words: Tamoxifen maculopathy, fluorescein angiography, optical coherence tomography. Palabras clave: Maculopatía por tamoxifeno, angiografía fluoresceínica, tomografía de coherencia óptica. INTRODUCTION Tamoxifen is a drug having anti-estrogen effect frequently used as a coadjutant treatment in breast cancer. Ocular alterations at the cornea, retina and optic nerve have been described with this drug, even utilizing low doses (1). In general, it is esti- Received: 24/9/07. Accepted: 29/8/08. Ophthalmology Dept. Sant Joan Hospital. Universitat i Virgili. Reus. Spain. 1 Graduate in Medicine. 2 Ph.D. in Medicine. Correspondence: M. Baget Bernaldiz C/. Selva del Camp, 11 43392 Castellvell del Camp (Tarragona) Spain E-mail: [email protected] mated that the ocular toxicity prevalence caused by tamoxifen is low (2). Patients suffering loss of vision in relation to tamoxifen usually exhibit whitish-yellowish crystal deposits in the nervous fiber and internal layers of the retina (3). In these cases, a fluorescein angiography (FA) study is useful because it frequently identifies the presence of BAGET-BERNALDIZ M, et al. A 53 year-old female diagnosed with breast cancer in June 1992. She underwent a radical mastectomy and tamoxifen was prescribed at a dosage of 20 mg/d, which she took regularly for 13 years (aggregate dose 95 g). During the last year of use of tamoxifen she exhibited a progressive loss of bilateral vision. The ophthalmological assessment made 6 months after the onset of symptoms revealed a visual acuity (VA) of 0.6 and 0.4 in the right eye (RE) and left eye (LE), respectively. Intraocular pressure and biomicroscopic exploration were normal. The eye fundus showed the presence of multiple whitish-yellowish spots dispersed in both posterior poles, involving both foveae (fig. 1). A FA study was made, evidencing the presence of slight bilateral macular edema (fig. 2). The OCT study showed a single foveal cyst with focal disruption of the photoreceptor line without increased macular thickness in RE and reduced foveal thickness in the LE (fig. 3). The differential diagnostic was mainly based on the dominant drusen and the fundus albipunctatus. The patient did not refer premature vision loss in any of her forbearers and did not exhibit a significant deposit of crystals on the nasal side of the optic nerve, the typical area of involvement in dominant drusen cases. In addition, she did not refer nyctalopia and the scotopic function of the electroretinogram was normal. The phototopic function of the left eye was slightly depressed, with the elec- Fig. 1: Bilateral retinography. Multiple whitish-yellowish spots dispersed on both posterior poles. Fig. 2: Bilateral fluorescein angiography showing slight fluorescein loss in both foveae. macular edema. In addition, it has recently been observed that a supplementary study of the macula in these patients by means of Optical Coherence Tomography (OCT) can provide anatomical details not evidenced by FA (4,5). Treatment of tamoxifen maculopathy consists in discontinuing its use, upon which some patients exhibit improved vision. CASE REPORT 616 ARCH SOC ESP OFTALMOL 2008; 83: 615-618 Tamoxifen an optic coherence tomography Fig. 3: Bilateral OCT showing a foveal cyst with disruption of the photo receptor line in RE and foveal atrophy in the LE. troculogram being normal in both eyes. The patient was diagnosed with tamoxifen retinopathy and recommended to discontinue the use of the drug. Twelve months after discontinuation her VA improved slightly only in the RE, reaching 0.75. Since then and after 2 years of follow-up her VA has remained stable. During said period the OCT pattern as remained unchanged. DISCUSSION The study of tamoxifen maculopathy has usually been made via eye fundus exploration and fluores- cein angiography. The instant case only had the eye fundus and FA and would have involved a diagnostic of slight bilateral macular edema but the OCT allowed a more detailed observation of the macular pathology. Therefore, as observed by Gualiano et al (4) and Bourla et al (5), there isn’t always a correspondence between angiographic evidence of macular edema and the presence of said edema via OCT. Consequently, we believe that OCT, as a supplement to FA can provide anatomical details of the macula which confirm with greater certainty the visual symptoms and may assist in establishing a visual prognosis for these patients. In our case a visual improvement was observed 12 months in the eye with the foveal cyst (RE) after discontinuing the use of the drug. This was not the case in the eye with established foveal atrophy (LE). More tamoxifen maculopathy cases analyzed with OCT need to be published in order to determine the different macular patterns and their corresponding visual prognosis. REFERENCES 1. Pavlis NA, Petris C, Briassoulis E, Klouvas G, Psilas C, Repapis J, et al. Clear evidence that long-term, low-dose tamoxifen treatment can induce ocular toxicity. A prospective study of 63 patients. Cancer 1992; 69: 2961-2964. 2. Heier JS, Dragoo RA, Enzenauer RW, Waterhouse WJ. Screening for ocular toxicity in asymptomatic patients treated with tamoxifen. Am J Ophthalmol 1994; 117: 772-775. 3. Mittra R, Mieler W, Drug toxicity of the posterior segment. In: Ryan SJ. Retina. St. Louis: Mosby; 2001; II: 1790. 4. Gualino V, Cohen SY, Delyfer MN, Sahel JA, Gaudric A. Optical coherente tomography findings in tamoxifen retinopathy. Am J Ophthalmol 2005; 140: 757-758. 5. Bourla DH, Sarraf D, Schwartz SD. Peripheral retinopathy and maculopathy in high-dose tamoxifen theraphy. Am J Ophthalmol 2007; 144: 126-128. ARCH SOC ESP OFTALMOL 2008; 83: 615-618 617