* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Anemia in Pregnancy
Survey
Document related concepts
Birth control wikipedia , lookup
Prenatal development wikipedia , lookup
Breech birth wikipedia , lookup
HIV and pregnancy wikipedia , lookup
Menstruation wikipedia , lookup
Maternal health wikipedia , lookup
Prenatal testing wikipedia , lookup
Women's medicine in antiquity wikipedia , lookup
Prenatal nutrition wikipedia , lookup
Fetal origins hypothesis wikipedia , lookup
List of medical mnemonics wikipedia , lookup
Maternal physiological changes in pregnancy wikipedia , lookup
Transcript
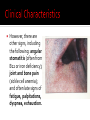
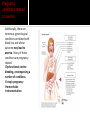
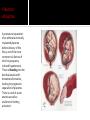
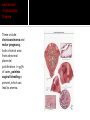
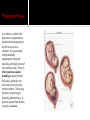
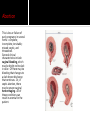
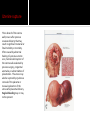
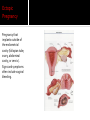
David M. Ellis University of Gambia Gynecology/Obstetrics 2 November, 2009 Definition Incidence Etiology and Pathogenesis Causes and Stages Clinical characteristic/ Correlates in Pregnancy Diagnostic Approach Management and Therapy/ Pregnancy Anemia is functionally defined as a decrease in the competence of blood to carry oxygen to tissues, thereby causing tissue hypoxia. Clinically, it refers to a decrease in the normal concentration of hemoglobin or erythrocytes. However, anemia is not a disease per se but an expression of an underlying disorder or disease. Anemia in pregnancy is a condition of oxygen delivery incompetence during the term of pregnancy. Anemia in Africa has been defined by WHO as Hb ≤10 g/dl. Severity: Moderate: 7-10.9 g/dl Severe: 4-6.9 g/dl Very severe: less than 4 g/dl According to one 1980s World Health Organization, world incidence of anemia in pregnancy is perhaps 51%. Developed countries had an incidence of 14%. However, Africa had an incidence of 63% for all pregnant women ages 15-49. Hemoglobin is the intracellular protein of erythrocytes responsible for transport of oxygen from the lungs to the tissues. Its synthesis is controlled by iron concentration within the cell. Each Hb molecule is capable of carrying 4 molecules of O2, one molecule bound to each of 4 iron-cored heme structures of hemaglobin. Oxygen affinity (the ease with which Hb binds and releases oxygen) is dependent on pO2, pH, pCO2, 2,3-DPG, and temperature and can be depicted by the oxygen dissociation curve. Right-shifting of the curve results in decreased O2 affinity. Increased CO2, heat, and acid decrease O2 affinity. Left-shifting leads to increased affinity. High O2 concentrations increase oxygen affinity. Hemoglobin occupies 33% of the volume of an erythrocyte and accounts for 90% of the cell’s dry weight. Its concentration is reported as mean corpuscular hemoglobin (MCH). In anemic states, the erythrocyte may contain less hemoglobin and/or there may be fewer erythrocytes present, often due to compromises in the erythrocyte membrane or metabolic pathways. Red cell membranes are supported by a protein skeleton. Inherent variants within these proteins manifest as abnormalities of shape, as in sphero-, ellipto-, and ovalocytosis. Erythrocytes obtain ATP from breakdown of glucose, 95% of which is metabolized by anaerobic glycolysis. There are a number of enzymyopathies accounting for the limitations in number of RBCs and in optimal delivery of O2. Based on a 5000 ml blood volume in a normal adult, the total body mass of hemoglobin is approximately 750 g. Since the normal erythrocyte lifespan is about 120 d., and the amount synthesized must be balanced with amount lost, the body loses and produces about 6.25 g of hemoglobin per day. If erythrocyte survival time is decreased by hemolysis or hemorrhage, the bone marrow producing them can be increased by a factor of up to 10, so that erythrocyte life span may decrease to about 18 days before marrow compensation is inadequate and anemia develops. If erythrocyte production cannot be increased to match the erythrocyte loss, anemia develops. Screening for anemia generally relies on the relative hemoglobin and hematocrit (% of total blood volume consisting of erythrocytes). However, there are a few instances when the hemoglobin or hematocrit concentration may be misleading. One such case, common in pregnancy, is hypervolemia, a total blood volume increase caused by a plasma volume increase while the erythrocyte mass remains stable. In such case, Hb/Hct concentrations will appear falsely decreased from hemodilution. On average, total red cell mass increases throughout pregnancy by 25%. The circulating plasma volume increases by about 40%. Thus, there is a normal dilutional drop in Hb level. Blood Loss- May be acute, as in trauma; May be chronic, as in parasitic hookworm infestation. Decreased Red Blood Cell Production May be nutritional, as in deficiency of iron, folates, B12, vitamins; May be depressed bone marrow function: Secondary anemias (HIV, TB, Carcinomas) Aplastic anemias (Chemicals, Radiation, Drugs) Thalassemias Increased RBC Destruction- RBC Abnormalities Hb (Sickle Cell Disease); Enzymatic (G6PD Deficiency); Membrane-related (Spherocytosis) Increased RBC Destruction- Abnormal Hemolysis continued Immune Hemolysis (Autoimmune, Fetomaternal, Incompatible Transfusion) Non-Immune Hemolysis (Infection-i.e., Malaria, Venoms, Burns, Hypersplenism) Risk factors for anemia in pregnancy can be drawn from causes of anemia often found in pregnancy: excessive blood loss, poor diet, malabsorption, chronic disease, thyroid endocrinopathy. Anemia reduces the O2 carrying capacity of the blood. The body compensates by 1) increasing the release of O2 from Hb to the tissues; 2) increasing cardiac output; 3) enhancing blood flow to tissues with high O2 requirements; 4) increasing respiration. The severity of the anemia may be considered as passing through four stages: Compensated- in mild to moderate anemia. O2 curve shifts to right (decreased O2 affinity), increasing O2 release to tissue by up to 40%. Vasodilation of myocardium as well as skin and kidneys. Breathlessness on exertion only. Decompensatedoccurs when Hb falls below 7 g/dl. Major compensatory mechanism is increased cardiac output. Stroke volume and heart rate are raised at rest. Patients are breathless even at rest. Life threatening-If Hb falls below 5 g/dl, respiratory distress may occur, showing as tachyphnea and at least one sign of nasal flaring, chest indrawing, or deep breathing. Resulting electrolyte changes: acidosis. Anemic heart failureIf Hb falls below 3 g/dl, O2 supply to the myocardium becomes insufficient, and no further increase of cardiac output is possible. High-output cardiac failure develops. Many times, anemia may be asymptomatic. However, what we usually associate with anemia are signs like pallor of the conjunctiva and nail beds as well as spooning of the nails, koilonychia. However, there are other signs, including the following: angular stomatitis (often from B12 or iron deficiency); joint and bone pain (sickle cell anemia); and often late signs of fatigue, palpitations, dyspnea, exhaustion. In West Africa, the most common correlate causes to anemia in pregnancy are nutritional deficiencies like iron, folic acid, B12, and vitamins. Parasitic infections from malaria and hookworm are also common. Pregnancy conditions related to anemia Additionally, there are numerous gynecological conditions correlated with blood loss and whose outcome may lead to anemia. Many of these conditions are pregnancyrelated. •Dysfunctional uterine bleeding, encompassing a number of conditions. •Ectopic pregnancy •Hemorrhoids •Instrumentation Look specifically at the disorders of pregnancy in Dysfunctional Uterine Bleeding: Ectopic pregnancy; Placenta previa; Hydatidiform mole; Choroio-epithelioma; Abortion or Premature sep. of the placenta. Placental Abruption A premature separation of an otherwise normally implanted placenta before delivery of the fetus, one of the most common risk factors of which is pregnancyinduced hypertension. There is bleeding into the decidua basalia with hematoma formation, leading to progressive separation of placenta. There is a risk of acute anemia as well as evidence of clotting activation. Gestational Trophoblastic Disease These include choriocarcinoma and molar pregnancy, both of which arise from abnormal placental proliferation. In 95% of cases, painless vaginal bleeding is present, which can lead to anemia. Placenta Previa A condition in which the placenta is implanted in a location that leaves part or all of the cervical os covered. It is associated with potentially catastrophic maternal bleeding and obstruction of the uterine outlet. There is often painless vaginal bleeding in about 70% of the cases, generally not until late second or early third trimester. There may be heavy or prolonged bleeding after delivery. It goes to reason that anemia may be a sequelae. Abortion This is loss or failure of early pregnancy in several forms: complete; incomplete; inevitable; missed; septic, and threatened. General clinical characteristics include vaginal bleeding, which may be bright red to dark in color. Or there may be bleeding that changes to a dark brown discharge that continues. Or, in septic abortion, there may be severe vaginal hemorrhaging. All of these conditions can result in anemia for the patient. Uterine rupture This is breech of the uterine wall (new or after previous cesarean delivery) that may result in significant maternal or fetal morbidity or mortality. Often caused by abnormal healing of a previous uterine scar, mechanical disruption of the uterine wall weakened by previous surgery, congenital anomalies, or abnormalities of placentation. The uterus may also be ruptured by injudicious removal of the placenta or manual exploration of the uterus after placental delivery. Vaginal bleeding may or may not be present. Ectopic Pregnancy Pregnancy that implants outside of the endometrial cavity (fallopian tube, ovary, abdominal cavity, or cervix). Signs and symptoms often include vaginal bleeding. Hemorrhoids These are symptomatic dilation of the hemorroidal venous plexus resulting in perianal swelling, itching, pain, and hematochezia. Hemorrhoids are extremely common as pregnancy progresses and have no effect on pregnancy itself. However, one possible complication is anemia. This is a condition that can cause anemia in pregnancy but one not commonly listed in books because for the most part it is inexcusable and usually results from lack of thoroughness and close observation by medical personnel. Last week, the house officer and I were called to the post-natal ward to examine a woman who had rechecked herself into the hospital after giving birth two days previously…. 24 yr old Fula; Grvda 2, para 1 plus 0. Previous full term SVD delivery 6/07 at RVTH. Current pregnancy: booked at 20 wks. w early hyperemesis. 12/9: Hb 8.8 g/dL w Dx: 3rd tri hemataemesis 14/9: USS:Twin pregnancy 1st cephalic/2nd breech Normal fetal heart beat, movement; normal fluid; anterior placenta. 30/10: Dx: Placenta previa, schedule for C-S According to mother, she first went into labor before C-S was done and was attempting to deliver breech. After, all she remembered was that she had an operation. 30/10: C-S for “occlusive placenta previa” completed. Alive babies referred to neonatal unit where both died. 31/10: Patient discharged to return for dressing change 6/11. Patient returned 1/11 for admission with Hb of 7.5. Called to exam at 1100 hrs. P/C: Abdominal pain and dizziness Hx P/C: Patient had given birth to twins via C-Section that had resulted from breech presentation. She had been in active labor before the C-S. What we saw O/E. What’s your move? Rembr Hx. Instrumentation On V/E, we noted a vaginal tear of approximately 7 cm through the posterior vaginal wall, and through the uterovaginal fascia. The next morning, the consultant discovered no one had cleaned this area and it was filled with leaking feces. She was concerned the tear had breeched the rectal fascia as well as compromised the external and internal sphincter muscles. How could this have happened? The best we can speculate, a tear occurred between the time the C-S was scheduled and then carried out. Perhaps in labor, there was an episiotomy instrumentation or a tear simply from the breech presentation. Whatever the case, there were presumable oversights. Never assume anything. Always be methodical and thorough. Use your clinical skills. Rule out the obvious or highly suspicious. Be skeptical of lab results. A good history is 70% of the diagnosis. In West Africa, we are always suspicious of nutritional and parasitic anemia. With distrust for accurate lab results, we usually treat empirically with Ferrous sulfate/folic acid tabs. How many mg of iron and folic acid are in one tab? How much does a pregnant woman need daily? And for how long? But what if you suspect pernicious anemia, order B12, and then continue to treat patient with folate? It will reverse the anemia but progressive and irreversible neurologic damage may result. In suspect cases, FBC w peripheral morphology and red cell indices; BF; stool microscopy; Hb electrophoresis for sickling. Anemia is not an indication for termination of pregnancy or induction of labor. Vaginal delivery is allowed unless there are contraindications. Severe anemia where the patient is already in Congestive HF risks maternal death. Exchange transfusion with diuretics. Transfusion is always contraindicated unless indicated. If patient goes into labor already in heart failure, allow labor in propped up position with O2 and assisted 2nd stage of labor using vacuum extraction. Depends on the cause. Management of obstetric conditions depend on many factors, including pregnancy term, medical, obstetric and gyne history, the presenting complaint and possible complications. The most common causes of anemia in pregnancy in West Africa are nutritional as well as parasites. Hemoglobin counts and blood film are commonly requested. Remember that one must go beyond Hb to MCV to accurately ascertain the cause of anemia. Education at the clinic/community level. Haemantinics (ferrous sulfate, 200 mg/day, plus folic acid 500 µg/d.) Given to all expectant mothers. Antimalarials in areas of high endemicity. Mebendazole 100 mg where hookworm is present. Increased dietary fruit (Vitamin C utilization of micronutrients). Avoid dietary chelators like tannins in tea. Delay next pregnancy 3 years to replenish micronutrient stores. Refine your clinical skills. Be methodical in your history taking and examination. Read between the lines. Be aware that anemia is usually a symptom and how it can affect the outcome of the pregnancy. Have available the RBC indice reference ranges. Know common dosages of medications used in anemia treatment. Be thorough and conscientious. Cook, G.C. (ed.) Manson’s Tropical Diseases (21st). UK: Saunders Publishing, 2003. Magowan, B. (ed.) Clinical Obstetrics (2nd). Edinborough: Saunders Publishing, 2009. McKenzie, S.B. Clinical Laboratory Hematology. New Jersey: Prentice Hall, 2004. Parry, E. (ed.) Principles of Medicine in Africa (3rd). Cambridge: Cambridge U Press, 2004. Smith, R.P. Netter’s Obstetrics. New Jersey: Icon Learning, 2002.