* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Notes: Notes: Objective: Demonstrate knowledge of the principles of
Survey
Document related concepts
Transcript
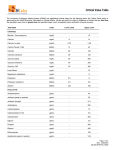
Notes: Dangerous on its own... or in combination CASE FOUR Dr. Maude St-Onge Dr. Dominique Piquette Notes: Objective: Demonstrate knowledge of the principles of clinical pharmacology, frequent drug interactions and their prevention/management. PART ONE Published by Articulate® Presenter www.articulate.com Notes: It is Tuesday night and you are on call for the ICU. You don't really mind because it has been one of those dark and humid days of November. At 3:00 AM, you get called by the Rapid Response Team (CRRT) nurse for your assistance. She is on the medicine floor assessing a 75-year-old patient admitted 24 hours ago for possible urosepsis. The patient is now obtunded, tachycardic, tachypneic and has a fever at 41.1oC. The CRRT nurse informs you that the story is actually quite obscure. Notes: “The patient was found by the police on the street. Nobody could provide any information about his past medical history or his medication. Unfortunately, the Medicine Team could not obtain any details from the patient himself because he was very confused on admission. No record of previous admission to this hospital was available and no contact information was found.” Published by Articulate® Presenter www.articulate.com Notes: When the Medicine Team first saw the patient in the Emergency Department, the patient was tachycardic at 120/min and hyperthermic (40oC). His BP and saturation were normal. His blood sugar was 11 mmol/L. His urine looked cloudy and the Medicine Team thought he was probably septic from a urinary source because his chest x-ray was unremarkable. Notes: Blood work and pancultures were sent and the patient was empirically treated with PIP-TAZO. A CT scan of his head was ordered to look for other sources of confusion, but only showed signs of remote strokes. Earlier this evening, the Medicine Team was unable to perform a lumbar puncture because of patient's lack of cooperation. Even with two persons holding him, they were not able to position him correctly. Published by Articulate® Presenter www.articulate.com Notes: “I’m worried about our Mr. Dos here because of some abnormal movements of the body that I noticed when I arrived. I’m really not sure if it was rigors, tremors, or seizures. The patient is mostly agitated now.” The patient’s current vital signs are: RR: 36/min HR: 140/min BP: 100/50 mmHg Sat 93% (6L/min) Temp: 41.1oC BS: 13 mmol/L Published by Articulate® Presenter www.articulate.com Notes: An ECG was done and showed, according to the Medicine resident, a sinus tachycardia. The CRRT nurse concludes by saying: Notes: “Can you please come and assess this patient? I’m not comfortable leaving him on the ward.” Notes: Objectives: - Discuss the differential diagnosis of hyperthermia. - Discuss the risk factors and the clinical presentation of the following diagnosis: serotonin syndrome, neuroleptic malignant syndrome, anticholinergic toxicity, malignant hyperthermia. - Describe the management of undifferentiated severe hyperthermia. PROPERTIES Allow user to leave interaction: Show ‘Next Slide’ Button: Completion Button Label: QUESTIONS: - Which non-infectious etiology(ies) could explain this patient's hyperthermia? - Assuming that the etiology of this patient's fever is infectious, which sources would you include in your differential diagnosis? Anytime Show upon completion Next Slide - How does the presence of neurological symptoms influence your differential diagnosis? - Which clinical findings would you look for during Published by Articulate® Presenter www.articulate.com your physical exam? - Would you treat symptomatically the hyperthermia? - Why? Notes: PART TWO Published by Articulate® Presenter www.articulate.com A few minutes later, you arrive at the bedside to evaluate the patient. You perform a physical examination. The patient has good bilateral air entry with normal heart sounds. His abdomen is soft with normal bowel sounds. He is warm to touch with bouncing pulses. He is diaphoretic and has no skin mark or lesion. The pupils are 5 mm and reactive, with no cranial nerve deficit. He has spontaneous tremors, hyperreflexia predominant in the lower limbs, and inducible clonus. You don’t notice any focal neurological finding. The muscle tone is hard to assess because the patient doesn't collaborate. You can't flex his neck. The results of the blood work done by the CRRT nurse 30 minutes ago are back: Blood Gas Type pH pCO2 pO2 Bicarbonate Saturation FiO2 CBC Hemoglobin WBC Count Neutrophils Lymphocytes Monocytes Eosinophils Basophils Platelet Count Hematocrit ARTERIAL 7.30 20 85 15 0.93 ? 7.35 - 7.45 35 - 45 mm Hg 80 - 100 mm Hg 21 - 28 mmol/L 0.90 - 1.00 120 13.4 10.3 3 0.6 0 0.1 250 0.400 115 - 165 g/L 4.0 - 11.0 x 10E9/L 2.0 - 7.5 x 10E9/L 1.0 - 4.0 x 10E9/L 0 - 1.0 x 10E9/L 0 - 0.7 x 10E9/L 0 x 0.3 x 10E9/L 150 - 400 x 10E9/L 0.340 - 0.490 L/L Published by Articulate® Presenter www.articulate.com Notes: Notes: Notes: Calcium Profile Calcium Magnesium Phosphate Albumin 2.38 0.60 0.65 25 2.20 - 2.60 mmol/L 0.70 - 1.05 mmol/L 0.87 - 1.52 mmol/L 35 - 50 g/L Electrolytes Sodium Potassium Chloride CO2 Total 135 4.0 110 15 135 - 147 mmol/L 3.5 - 5.0 mmol/L 95 - 107 mmol/L 22 - 30 mmol/L Glucose- Random 14.0 4.0 - 8.0 mmol/L INR PTT 1.2 32.0 0.9 - 1.10 INR 24.0 - 34.0 SECS Renal Profile Urea Creatinine 5.5 90 3.0 - 7.0 mmol/L 44 - 106 umol/L Notes: CK + CK-MB CK 850 < 195 IU/L 4 2- 6 ng/mL <0.01 < 0.05 Troponin T 0.07 < 0.10 ug/L Lactate - Serum 1.2 0.5 - 2.0 mmol/L Bilirubin - Total 18 <20.0 umol/L AST 55 <31 IU/L ALT 40 <31 IU/L ALP 118 40 – 120 IU/L mB Mass mB Mass Fraction Liver Profile Published by Articulate® Presenter www.articulate.com Notes: YESTERDAY - EMERGENCY DEPARTMENT Blood Gas Type pH pCO2 pO2 Bicarbonate Saturation FiO2 ARTERIAL 7.33 25 85 18 0.93 ? 7.35 - 7.45 35 - 45 mm Hg 80 - 100 mm Hg 21 - 28 mmol/L 0.90 - 1.00 Electrolytes Sodium Potassium Chloride CO2 Total 136 3.8 108 18 135 - 147 mmol/L 3.5 - 5.0 mmol/L 95 - 107 mmol/L 22 - 30 mmol/L Glucose- Random 10.0 4.0 - 8.0 mmol/L Notes: Renal Profile Urea 5.0 3.0 - 7.0 mmol/L Creatinine 80 44 - 106 umol/L Lactate - Serum 1.0 0.5 - 2.0 mmol/L Salicylates <1.0 <1.0 mmol/L Ethanol 10 0 mmol/L Osmolarity 300 280-300 Osm/L Tox screen (urine) negative N.B.: A TSH was sent in the Emergency Room and is normal. Published by Articulate® Presenter www.articulate.com Notes: The CRRT nurse has already inserted a Foley catheter and two 16-gauge peripheral IVs. A liter of normal saline is almost finished. You agree with the nurse that the patient needs to come to the ICU. You are wondering if you should intubate him and sedate him to do the lumbar puncture. While the transfer is being organized, you ask the nurse to give another bolus of fluid, to administer some IV thiamine, and to give some IV antibiotics for meningitis. Notes: You notice in the chart that the social worker and the pharmacist were able to reach the shelter where Mr. Dos lives. He was known for substance abuse disorder (amphetamines, heroin, LSD, alcohol) and was recently started on Fluphenazine for a psychotic disorder (but was poorly compliant). Published by Articulate® Presenter www.articulate.com Notes: PROPERTIES Allow user to leave interaction: Show ‘Next Slide’ Button: Completion Button Label: Objectives: - Differentiate pharmacodynamic interactions (additive effect, synergistic effect, antagonist effect) from pharmacokinetic interactions (absorption, distribution, metabolism, excretion). - Identify which drugs/substances/interaction s can give a serotonin syndrome and discuss by which mechanism. - Identify which drugs can give a neuroleptic malignant syndrome and discuss the potential pathogenesis. - Identify which drugs/substances can cause withdrawal syndrome and discuss by which mechanism. Anytime Show upon completion Next Slide Questions: - How worried are you about this patient? - How do you explain his metabolic acidosis? - How is the information provided by the pharmacist and social worker helpful? - Have you modified your working diagnosis at this point? - Could you discuss the pharmacodynamic and pharmacokinetic interactions relevant for this patient? - How would you find additional information on this topic if necessary? Published by Articulate® Presenter www.articulate.com Notes: PART THREE Notes: A few hours later, the patient has been intubated and sedated. A new attempt at performing the lumbar puncture was unsuccessful because the patient was very stiff and couldn't be properly positioned. At the end, you paralyzed the patient to complete the procedure. The patient's heart rate is now 120/min (sinus rhythm), the blood pressure is 110/55 mmHg, and the temperature is 39oC despite the cooling blanket. His latest CK level is 10 000 IU/L with positive myoglobinuria. The preliminary results of the lumbar puncture are non-contributory. Published by Articulate® Presenter www.articulate.com Notes: You decide to call the Poison Control Center, who suggests to treat this patient for neuroleptic malignant syndrome with Dantrolene. They also suggest to add Cyproheptadine in case of a serotonin syndrome. You also increase the Midazolam infusion and add a Propofol infusion. Over the next 4h, the patient seems to respond well to the Dantrolene administration. He becomes less rigid and the temperature drops to 38oC. Notes: Around 7:00 AM, just when you think that you are getting things under control, the patient develops a rapid unstable atrial fibrillation. You cardiovert him and he returns into sinus rhythm at 110/min with occasional short runs of atrial fibrillation up to 180/min. You decide that your last contribution to his care (at least for this call) will be a loading dose of Amiodarone (150 mg) followed by an IV infusion. Published by Articulate® Presenter www.articulate.com Notes: You wake up around 12:30 pm on your post-call day thinking... “Shoot! Did I order any medication that could make the patient's condition even worse??” Notes: When you see the patient 24h later, he is still sedated and no longer rigid. His CK level is decreasing. However, his FiO2 requirements have increased and his chest X-ray shows signs of pulmonary edema. His blood pressure is 100/70 mmHg. His ECG follows: Published by Articulate® Presenter www.articulate.com Notes: Questions: - How would you measure the QT interval of this patient? Is it normal? - Can you describe the rhythm? How would you manage the patient at this point? PROPERTIES Allow user to leave interaction: Show ‘Next Slide’ Button: Completion Button Label: Anytime Show upon completion Next Slide Notes: You notice that a bedside 2D echo was performed yesterday and documented a decreased left ventricular function although difficult to assess because of the atrial fibrillation. The IVC was measured at 2 cm and was not collapsing easily. The central venous saturation is currently 65%. The fluid balance is now positive by 6L. The patient has a good urine output and does not demonstrate any sign of organ hypoperfusion. His magnesium level is normal, but his potassium is 5.6 mmol/L. He is afebrile and all cultures have been negative thus far. Published by Articulate® Presenter www.articulate.com Notes: You decide to add Digoxin to his medication. However, you are concerned about potential interactions with other medications. The ICU pharmacist is sadly on vacation this week. You also need to decide if this patient needs to be started on Warfarin. Notes: Objectives: - Identify risk factors for drug interactions in the ICU. - Identify frequent drug interactions with Amiodarone and Digoxin, by which mechanisms they occur and how to prevent it. - Identify which drugs can cause hyperkalemia and by which mechanisms. - Identify which drugs can prolong QTc. - Identify frequent drug interactions with Warfarin and how to prevent it. PROPERTIES Allow user to leave interaction: Show ‘Next Slide’ Button: Completion Button Label: Questions: - How do you explain this patient hyperkaliemia? - How would you manage it? Anytime Show upon completion Next Slide - Describe the common drug interactions involving medications used to treat atrial fibrillation? - How can you prevent them? Published by Articulate® Presenter www.articulate.com Notes: The patient finally improved and got extubated. Unfortunately, because of his baseline psychosis, it was impossible to obtain a history for the present illness. The meningitis treatment was completed and the patient was eventually transferred to the Psychiatric Unit. References Boyer, E.W., Shannon, M. The serotonin syndrome. N Eng J Med. 352, 1112-1120 (2005). Hadad, E., Weinbroum, A.A., Ben-Abraham, R. Drug-induced Hyperthermia and Muscle Rigidity: a Practical Approach. Eur J Emer Med. 10, 149-154 (2003). Jenkins, D.H. Substance Abuse and Withdrawal in the Intensive Care Unit. Surg Clin N Am. 80 (3), 1033-1053 (2000). Spriet, I., Meersseman, W., De Hoon, J., Von Winckelmann, S., Wilmer, A., Willems, L. Mini-series II: Clinical Aspects. Clinically Relevant CYP450-mediated Drug Interactions in the ICU. Intens Care Med. 35, 603-612 (2009). Streetman, D.S. Metabolic Basis of Drug Interactions in the Intensive Care Unit. Crit Care Nurs. 22 (4), 1-13 (2000). Notes: RCPSP OBJECTIVES: 7.5 Intoxication Published by Articulate® Presenter www.articulate.com 7.5.1 The ability to formulate a differential diagnosis for a patient potentially suffering from a toxic syndrome and undertake a sequential plan to support organ function, prevent further absorption, alter distribution, and if possible, enhance elimination by natural and mechanical means. 7.5.2 Demonstrate knowledge of: 7.5.2.1 the general support, together with any specific antidotes or supportive therapy pertinent to individual intoxicants 7.5.2.2 the pharmacology of common intoxicants 7.5.2.3 strategies to reduce absorption and enhance elimination (hemodialysis, hemoperfusion) 7.5.2.4 the need of patients and families for emotional and psychiatric support 8.2 Pharmacotherapy 8.2.1 Have a thorough knowledge of indications, risks, and side effects of relevant pharmacotherapy. 8.2.2 Demonstrate knowledge of: 8.2.2.1 the principles of clinical pharmacology 8.2.2.2 the pharmacologic and therapeutic applications of drugs 8.2.2.3 side effects, drug interactions associated with medications Published by Articulate® Presenter www.articulate.com