* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download File - Sara Patton`s e
Survey
Document related concepts
Transcript
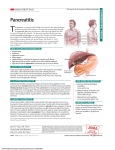
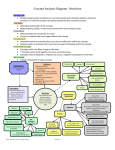
Case Study Report: The Use of Nutrition Support in Pancreatitis Sara Patton Dietetic Intern ARAMARK Healthcare Distance Learning Dietetic Internship Paoli Hospital March 15, 2013 Abstract Pancreatitis is inflammation of the pancreas and usually begins as a sudden attack1. Gallstones and alcohol abuse account for more than 80% of reported acute pancreatitis case, making them the two most common etiological factors. In severely ill patients, complications may occur such as multiple organ failure and pancreatic necrosis. In such severe cases, an oral diet is usually not an option 3. The initiation of nutrition support as standard practice when an oral diet is not feasible is becoming a more common practice. In the past, the common undisputed plan of care was to put the pancreas “at rest” by making the patient nil per os (NPO), which means nothing by mouth 1. By having the patient fasting, the assumption was that the pancreas would not be stimulated to produce any secretions. However, new studies have found that if the pancreas was keep at baseline secretions, the patient would have better outcomes and short length of stays 4. The timing of initiating EN has been thought to be within 48hours to help reduce incidences of multi-organ failure, pancreatic infectious complications, and mortality4. The main aim of nutrition support is to help cover the body’s elevated demands due to protein catabolism and metabolic instability. When providing the elevated needs via enteral nutrition, it is important to prevent over stimulation of pancreatic secretions and to keep them at baseline4. Disease Description The pancreas is a glandular flattened organ that lies in the upper abdomen behind the stomach. The pancreas has both exocrine and endocrine function. Endocrine functions include producing glucagon, insulin and somatostatin. Exocrine functions include secreting enzymes directly into the intestinal lumen to help in digestion of macronutrients. Neural and hormonal responses play a major role in the regulation of exocrine secretions. Some outside factors that influence pancreatic function include the anticipation, sight and taste of food. In a healthy pancreas, the secretions during a meal can be divided into three phases: the cephalic phase, gastric phase, and ending with the intestinal phase1. Pancreatitis is inflammation of the pancreas and usually begins as a sudden attack1. Once the pancreas is inflamed, its digestive enzymes, mainly trypsin, attack the tissue that produces said enzymes 2. Furthermore, once trypsin begins to attack the pancreatic tissue, it can cause bleeding, tissue damage, and cause blood vessels to swell. It can be classified as either acute or chronic pancreatitis2. If these attacks continually reoccur, then it is considered chronic pancreatitis. Mahan, Escott-Stump, and Raymond write that pancreatitis is “characterized by edema, cellular exudates, and fat necrosis. The disease can range from mild and self-limiting to severe, with auto digestion, necrosis, and hemorrhage of pancreatic tissue1”. In 1974, Ranson and colleagues had distinguished 11 sign and symptoms that have prognosis significance of pancreatitis. Ranson’s criteria are: age >55 years white blood count >1600m3 blood glucose levels >200mg/100mL lactic deydrogenase >350units/L aspartate transaminase >250units/L hematocrit decrease of>10mg/dL blood urea nitrogen increase of >5mg/dL arterial PO2 <60mm Hg base deficit >4mEq/L fluid sequestration >6000mL serum calcium level <8mg/mL These symptoms can be measured within the first 48 hours of admission, and therefore determine likely outcomes of the patient’s hospitalization. By assessing the clinical presentations of the patient, the degree of intervention can be obtained (see figure1)3. Pancreatitis can result from chronic alcoholism, biliary tract disease, hypertriglyceridemia, hypercalcemia, gallstones, trauma, certain drugs or some viral infections. Alcohol is thought to contribute to about 60-90% of the development of chronic pancreatitis2. “Obesity appears to be a risk factor for the development of pancreatitis and an increased severity1”. Pancreatitis can result from one or multiple compounding factors. Physical symptoms of pancreatitis can include nausea, vomiting, abdominal distention, steatorrhea, and continuous or intermittent pain varying in intensity to sever upper abdominal pain which can radiate to the back. More severe cases of pancreatitis can be complicated by hypotension, oliguria, dyspnea, and extensive destruction of pancreatic tissue. The destruction of pancreatic tissue leads to fibrosis in which enzyme production is diminished. Evidence-Based Nutrition Recommendations The main factor in pain felt in acute pancreatitis is related to the secretion mechanisms of pancreatic enzymes and bile. With many patients who acute pancreatitis, the intake of normal food is often intolerable. The standard nutrition care in the past was to put the pancreas “at rest” by making the patient nil per os (NPO), which means nothing by mouth1. The thought behind this action was to prevent the stimulation of the pancreas by withholding food. The initiation of nutrition support as a means of providing proper nutrition during times of pancreatitis is becoming more popular compared to the “old” standard of pancreatic rest. Enteral nutrition is the overall preferred method for nutrition support when compared to parenteral. However, the exact route of enteral feeding is still dependant on more studies4. Coté GA et al, 2011, in a multicenter controlled study, found that the pathogenesis of chronic pancreatitis is still unknown. There are several mechanisms thought to be at work to produce the progression of the disorder, but the main culprit appears to be chronic inflammation. Historically, alcohol abuse has been the widespread common factor of chronic pancreatitis. However, this article discusses the recent decline in alcohol use as the stand alone contributory factor in pancreatitis. Although alcohol still remains as the common etiology of pancreatitis, more and more patients are presenting with non-alcoholic pancreatitis. New genetic analysis is helping researchers to find a link between previously unrecognized factors that are contributory to developing the disease. The interactions between possible “culprit” genes and environmental dynamics may hold the key to future pancreatitis research 2. Spanier, et al, 2010, in a literature review of nasogastric feedings in patients with acute pancreatitis, found that enteral nutrition should be initiated as soon as possible to influence better outcomes. Gallstones and alcohol abuse account for more than 80% of reported acute pancreatitis case, making them the two most common etiological factors. In severely ill patients, complications may occur such as multiple organ failure and pancreatic necrosis. In such severe cases, an oral diet is usually not an option. The idea of pancreatic rest disregards the persistence of basal pancreatic secretions. There are three components of pancreatic secretion: protein enzymes, fluid volume, and bicarbonate. The protein enzyme output is the main perpetuation of the inflammatory process, and therefore suppression of protein enzyme output theoretically would be adequate in putting the pancreas to “rest”. Having the pancreas reduced to baseline stimulation by using nutrition support can help maintain gut integrity 4. The use of an elemental, semielemental or polymeric formula is still unclear as to which would have the better outcome. The idea in using an elemental and semielemental formula is that they would require less digestion and therefore cause less pancreatic secretions. The timing of initiating EN has been thought to be within 48hours to help reduce incidences of multi-organ failure, pancreatic infectious complications, and mortality. One study discussed in the article cites the initiation of EN within 36 hours when compared to after 36hours in the ICU population and found that earlier initiation helped to reduce the length of stay in the hospital. Overall, once a patient is unable to consume sufficient oral intake within 5-7days or is predicted to not be able to meet estimated needs, nutrition support should begin. Enteral nutrition is preferred over total parenteral nutrition, and TPN should only be used if EN cannot be tolerated 4. Ioannidis, et all, 2008, in a series of controlled clinical studies on the effectiveness of enteral nutrition, shows that enteral nutrition should be the preferred route in patients with acute pancreatitis. Approximately 75% of patients diagnosed with mild acute pancreatitis have a mortality rate below 1% and is increased up to 20% if the disease progresses to a severe necrotizing form. Acute malnutrition is often observed and can lead to further complications. The main aim of nutrition support is to help cover the body’s elevated demands due to protein catabolism and metabolic instability. When providing the elevated needs via enteral nutrition, it is important to prevent over stimulation of pancreatic secretions and to keep them at baseline. Parenteral nutrition support can increase complications in patients’ with pancreatitis due to uncontrolled hyperglycemia and infection. Another downfall to using parenteral nutrition as a first line of support is that parenteral nutrition is more expensive than enteral. Only patients’ with severe pancreatitis that cannot tolerate enteral nutrition support should be considered for parenteral 5. Mirtallo, et all 2012, in a systematic review and evaluation of published literature provides an evidence based review for nutrition support of pancreatitis. After evaluating different trials and studies of patients’ with pancreatitis, the base energy requirements were found to range from 25-35kcal/kg/d and energy expenditure stayed around 25kcal/kg/d regardless of whether the patient has acute, chronic or sepsis with pancreatitis. Concerning patients’ on parenteral and enteral nutrition, it was found that patients receiving parenteral were better able to meet the higher caloric goals. However, the patients also had higher incidences of hyperglycemia. These findings still beg to question whether or not patient outcomes would be improved from delivery of fewer calories and the need to reconsider the volume or dose of feedings. The current guidelines in place for nutrition therapy in patients with pancreatitis have been assessed to be universally applicable6. Case Presentation The patient is a 53 year old Caucasian male who came to the emergency room after experiencing significant abdominal pain and vomiting earlier that afternoon. The symptoms began earlier that day acutely after eating lunch. The pain began to radiate towards his back and is not relieved with any change in position or fasting. The patient was begun on dilaudid in the ER, which did help the pain a little. NCP: Assessment: Client History: The patient is a 53 year old male whom does not have many issues with medical problems. His past medical history does include hypertension, hyperlipidemia, kidney stones, non-alcoholic fatty liver disease, and possible hypertriglyceridemia. The patient was once told that his liver enzymes were elevated when he was trying to give blood, in which he discovered that he had non-alcoholic fatty liver disease. His family history is non-contributory. The patient does not smoke, drinks socially, and has no history of illicit drug use. Food/Nutrition-Related History: The patient has recently lost about 44 pound intentionally over the last 4 months by restricting his diet and aggressively adhering to a workout regimen. The patient had restricted his diet to about 1200kcals/day. The patient stated that he was “getting too big” and therefore decided to lose weight. The patient reported wanting to get healthier. The patient denied any chewing/swallowing difficulties and any food allergies. Nutritionally pertinent medications were: lovenox: anticoagulant. May cause nausea, vomiting, abdominal pain, GI bleeding, constipation, black tarry stool7 dilaudid: analgesic, antitussive, narcotic.Helps relieve moderate to severe pain. May cause anorexia, decrease wt, increased thirst, dehydration, nausea, vomiting 7 primaxin: antibiotic. May cause taste changes, nausea, vomiting, abdominal pain, diarrhea, dyspenia 7 ativan: anti-anxiety. Limit caffeine and grapefruit. May cause dry mouth, nausea, vomiting, diarrhea, constipation, anorexia 7 protonix: proton pump inhibitor, antigerd. May cause decrease acid secretions, increased gastric pH, nausea, diarrhea 7 Nutrition-Focused Physical Findings: Upon admission, the patient had a blood pressure of 123/73, heart rate of 55 and temperature of 97.5 degrees Fahrenheit. The patient presented awake and oriented x3 but with a mildly anxious affect. The patient reported no appetite and was currently nauseous. The patient is capable of self care and self feeding. There was significant tenderness to the epigastric area in his abdomen, with mild palpitations. There were no apparent signs of muscle and or fat wasting. The patient was presenting with the classic signs of pancreatitis. Anthropometric Measurements: Height: 70in Weight: 87.5kg Usual Body weight: 107.4kg % weight change: 18.62% in 4 months IBW: 75.20kg %IBW: 115% BMI 27.58. overweight per standards 8 Calculations for the above measurements can be found in table 1. Biochemical Data/Medical Tests: The nutritionally relevant biochemical data collected on the pt are described in table 2. Medical tests performed/findings: CT ABD and Pelvis with Contrast (2/08/13). Findings: Acute pancreatitis, mild hypoenhancement of body and tail of pancrease relative to the head, likely secondary to sever edema. Early pancreatic necrosis possible. Irregular fundus of gallbladder. Nonobstructive left renal calculi MRI Abdomen without Contrast(2/08/13): Findings: Cholelithiasis, extensive peripancreatic edema. Small amount upper abdominal ascites. Trace bilateral pleural effusions. CT Abdomen with IV Contrast (2/11/13): Findings New moderate right and small pleural effusions. Severe pancreatitis with evidence of necrosis in portions of the body and tail. Wall thickening of small bowel loops in vicinity of pancreas. Abdomen Survey/KUB (2/12/13): Dobhoff Tube placement. Feeding tube in place with its tip in the right upper part, likely overlying distal body of the stomach. Nutrition Needs: Calories: 2175kcals (using 25kcals/kg actual body weight) Protein: 130.5-174gm Protein (using 1.5-2.0grams/kg actual body weight) Fluid: 2175-2610mL (using 25-30mL/kg actual body weight) Calculations explained in table 3 8. Nutrition Status Classification: In compliance with ARAMARK’s nutrition status classification, the patient is classified at moderate nutrition risk due to vomiting (3 points), low albumin (3 points), diagnosis of acute pancreatitis (3 points). Table 4 explains the nutrition status classification and the point system 9. Diagnosis-Related Group: In accordance to ARAMARK’s diagnosis-related group, the patient falls into the category of Unspecified PCM (Protein Calorie Malnutrition) due to his reported inadequate protein and/or calorie intake for > 7 days, and his albumin levels < 3.5 (patient’s albumin level: 2.4) 9 NCP: Diagnosis: Inadequate Oral Intake (NI-2.1) related to decreased ability to consume sufficient energy/food-nutrition-related knowledge deficit concerning appropriate oral food intake as evidenced by weight loss, nausea/vomiting, reported insufficient intake of energy when compared to requirements, and sever acute pain 10. (See Table 5). The patient reported very low PO intake prior to admission due to his abdominal pain. Furthermore, the patient had been restricting his diet to 1200kcals/day, which is below is estimated daily requirements. NCP: Intervention: Meidcal Intervention: Antibiotic stopped- no detection of infection was present. CT ABD and Pelvis with Contrast (2/08/13). Findings: Acute pancreatitis, mild hypoenhancement of body and tail of pancrease relative to the head, likely secondary to sever edema. Early pancreatic necrosis possible. Irregular fundus of gallbladder. Nonobstructive left renal calculi MRI Abdomen without Contrast(2/08/13): Findings: Cholelithiasis, extensive peripancreatic edema. Small amount upper abdominal ascites. Trace bilateral pleural effusions. CT Abdomen with IV Contrast (2/11/13): Findings New moderate right and small pleural effusions. Severe pancreatitis with evidence of necrosis in portions of the body and tail. Wall thickening of small bowel loops in vicinity of pancreas. Abdomen Survey/KUB (2/12/13): Dobhoff Tube placement. Feeding tube in place with its tip in the right upper part, likely overlying distal body of the stomach. Nutrition Intervention: Enteral Nutrition (ND-2.1) 10: recommend start tube feeding of Peptamen AF @15mL/hrx 24hr, increase by 10mL/hr until goal of 75mL/hr x 24hr is reached. Recommend flush 125mL H2O every 4 hours. Peptamen AF is an elemental formula which may be easier on the patient to digest. Once the tube feeding is at the goal rate of 75mL/hr it will provide 1800mL total volume, 2160kcals, 137grams protein, 99 grams fat, 1460mL water. Total water flushes will provide 750mL water for a total of 2210mL water. (see Table 6 for calculations). NCP: Monitoring and Evaluation: Enteral Nutrition Intake (FH-1.3.1) 10. Begin Enteral nutrition infusion on 2/12/13 using Peptamen AF at a rate beginning at 15mL/hr, increasing by 10mL/hr until goal of 75mL/hr x 24hr with water flushes of 125mL every 4 hours. Monitor Enteral nutrition initiation and rate advancement. Follow-up: On 2/13/13 the patient was receiving the goal rate of 75mL/hr of the tube feeding. The patient did not report and nausea or vomiting, no abdominal distention, and no aspiration. The patient appeared to be tolerating his tube feeding at goal rate. As of 2/15/13, the Dobhoff tube was removed and advanced to a clear liquid, then a low-fat diet, both of which he tolerated. Patient reported minimal abdominal discomfort and was tolerating orals for over 24 hours. The patient was discharged to home on 2/16/13. Patients’ discharge plan is as follows: Follow up with PCP in 1 week with CBC and CMP and to discuss with GI as well as PCP regarding resuming back on Simvastatin as well as low-dose Aspirin. Avoid Tylenol products and NSAIDs. Ambulate as tolerated GI follow-up as recommended Not to drive while on pain medications Conclusion Many patients admitted to the hospital with acute or chronic pancreatitis are often unable to consume an oral diet. The pain associated from eating often brings an overall aversion to food. Having pancreatitis can increase the nutrient needs of the body due to inflammation, possible infection, and multi-organ failure. The increased demand on the body is hard to reach when the patients do not want to eat. Therefore, the initiation of nutrition support is becoming a standard practice when the patient is predicted to be NPO for an extended period of time, or if the patient already presents as malnourished. Enteral nutrition support helps give the pancreas a “rest” but encourages base-line pancreatic secretions. The patient was taken off the tube feeding after three days and started on an oral diet. After 24 hours of monitoring, the patient was tolerating his diet, and was ready to go home. The patient was discharged on a low-fat diet. The patient was scheduled for several gastroenterology follow-ups to monitor pancreatic function. Appendix Figure 13: Table 1: Anthropometric Calculations Height Weight Usual Body Weight % Weight change Ideal Body Weight (IBW) % Ideal Body Weight (%IBW) Body Mass Index (BMI) 70 inches 192.4lbs /2.2kg = 87.5kg 236.25lbs/2.2kg= 107.4kg (236.25lbs-192.4lbs)/236.25lbs x 100= 18.62% 106lbs for first 5 feet, 6 lbs for every inch over. 6 x10in = 60lbs. 106 +60= 166lbs. 166/2.2kg= 75.20kg 236.25lbs / 192.4lbs= 115% [192.4lbs / (70in)² ] x 703= 27.58 Table 2 Biochemical Data RBC WBC Count Creatinin Sodium Potassium Chloride 136-144 3.6-5.1 98- Count 4.54.5-5.8 10.8K/UL mEq/L mEq/L Glucose BUN e Albumin 70-99mg/dL 8-20mg/dL 0.8- 3.4-5.0g/dL 109mEq/L K/UL 1.3mg/dL 2/07 15.5 (H) 5.38 141 4.2 106 141(H) 23(H) 1.1 5.0 2/08 12.1(H) 4.91 141 4.0 110(H) 130(H) 23(H) 0.9 3.9 2/09 14.8(H) 4.67 144 3.7 115(H) 101(H) 18 0.7(L) 3.2(L) 2/10 12.4(H) 4.45(L) 144 3.7 115(H) 114(H) 18 0.7(L) 3.2(L) 2/11 9.9 3.90(L) 143 3.9 114(H) 102(H) 19 0.6(L) 2.9(L) 2/12 9.9 3.94(L) 144 3.5(L) 113(H) 98 16 0.5(L) 142 3.6 112(H) 109(H) 16 0.5(L) 141 3.4(L) 110(H) 123(H) 13 0.5(L) 2.6(L) Within normal limits Low: Vomiting, diarrhea, laxatives High: Dehydratio n, diarrhea, decreased kidney function High: medications , stress, illness High: kidney damage, kidney stones, dehydration Low: decrease d kidney function Low: nephritic syndrome, acute/chronic inflammation 2/13 2/14 Rationale 9.9 3.96(L) High: stress, certain medications , infection Low: Blood loss, kidney function Table 3: Nutrition Calculations: Calories Protein Fluid 25kcals/kg x 87.5kg 1.5-2.0 grams/kg x 87.5kg 25-30mL/kg x 87.5kg 2175kcals 130.5-174gm 2175-2610mL Table 4: ARAMARK Classification6 : Nutrition Status Classification Points Normal (Status 1) 0-5 Mildly Compromised (Status 2) 6-7 Moderately Compromised (Status 3) 8-11 Severely Compromised (Status 4) 12 Nutrition Status Classification Time Frames for Reassessment/Followup Normal (Status 1) 5-7 days Mildly Compromised (Status 2) 4-6 days Moderately Compromised (Status 3) 3-5 days Severely Compromised (Status 4) 1-4 days Table 5: Diagnosis Terminology/PES Statement Nutrition Diagnosis Terminology / PES Statements Doma Nutrition Relat Etiology As Signs and/or Symptoms in Diagnosis ed to eviden Terminolog ced by y Intak (NI-2.1) Relat decreased As weight loss, e Inadequate ed to ability to eviden nausea/vomiting, Oral Intake consume ced by reported insufficient sufficient intake of energy when energy/foodcompared to nutritionrequirements, and sever related acute pain knowledge deficit concerning appropriate oral food intake Peptamen AF Nutrition Information (courtesy of Nestle Healthcare Nutrition Product Guide) Table 6: Tube Feeding Calculations: Total Volume (mL) 75mL x 24hrs= 1800mL (1.8 Liters) Total Calories (kcals) 1800mL x 1.2kcals/mL= 2160kcals Total Protein (grams) 1.8L x 76grams protein/L= 136grams Total Fat (grams) 1.8 Lx 54.8grams fat/L= 99grams Free Water (mL) 1.8L x 811mL= 1460mL Water Flushes 125 x 6= 750mL Total Water 1460mL + 750mL= 2210mL Works Cited 1. Escott-Stump S, Mahan KL, Raymond JL. Krause’s Food and the Nutrition Care Process, 13th ed. St. Louis: Elsevier Inc.; 2012. 2. Coté GA, Yadav D, Slivka A, et al. Alcohol and Smoking as Risk Factors in an Epidemiology Study of Patients With Chronic Pancreatitis. Clinical Gastroenterology and Hepatology. 2011;9(3): 266-273 3. Curtis CS, Kudsk KA. Nutrition Support in Pancreatitis. Surgical Clinics. 2007; 97(6): 1403-14215 4. Spanier BWM, Bruno MJ, Mathus-Vliegen EMH. Enteral Nutrition and Acute Pancreatitis: A Review. Gastroenterology Research and Practice. 2011;vol 2011:1-9. doi:10.1155/2011/857949 5. Ioannidisi O, Lavrentieva A, Botsiosi D. Nutrition Support in Acute Pancreatitis. Journal of the Pancreas. 2008; 9(4): 375-390 6. Mirtallo JM, Forbes A, McClave ST, Jensen GL, Waltzberg DL, Davies AR. International Consensus Guidelines for Nutrition Therapy in Pancreatitis. Journals of Parenteral and Enteral Nutrition. 2012;36(3): 284-291. doi:10.1177/01486071 12440823 7. Crowe JP, Pronsky ZM, Food Medication InteractionsTM , 17th ed. Birchrunville: Food-Medications Interactions; 2012 8. Width M, Reinhard T. The Clinical Dietitian’s Essential Pocket Guide. Baltimore: Lippincott Williams & Wilkins; 2009. 9. ARAMARK Healthcare. Assessment and education policy #2: Nutrition status classification worksheet. Patient Food Services: Policies and Procedures, Volume IV; 2010 10. American Dietetic Association. International Nutrition Terminology (IDNT) Reference Manual: Standardized Language for the Nutrition Care Process. Chicago, IL; 2011.