* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
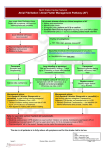
Download Choosing the right drug to fit the patient when selecting oral
Survey
Document related concepts
Transcript
Review doi: 10.1111/joim.12360 Choosing the right drug to fit the patient when selecting oral anticoagulation for stroke prevention in atrial fibrillation A. M. Shields1 & G. Y. H. Lip2,3 From the 1Acute Medicine Directorate, Croydon University Hospital, London; 2University of Birmingham Centre for Cardiovascular Sciences, City Hospital, Birmingham, UK; and 3Aalborg Thrombosis Research Unit, Department of Clinical Medicine, Faculty of Health, Aalborg University, Aalborg, Denmark Abstract. Shields AM, Lip GYH (Croydon University Hospital, London; University of Birmingham Centre for Cardiovascular Sciences, City Hospital, Birmingham, UK; and Aalborg University, Aalborg, Denmark). Choosing the right drug to fit the patient when selecting oral anticoagulation for stroke prevention in atrial fibrillation. (Review). J Intern Med 2015; 278: 1–18. Atrial fibrillation (AF) is the most common cardiac arrhythmia worldwide and is a growing health problem that is associated with a significantly increased risk of stroke and thromboembolism. Oral anticoagulant (OAC) therapy reduces the risk of stroke and all-cause mortality in patients with AF. OAC therapy is commonly given as a wellcontrolled vitamin K antagonist (VKA; e.g. warfarin) and can reduce the risk of stroke in AF patients by almost two-thirds. However, the widespread use of VKAs has been hampered by the unpredictable Introduction Atrial fibrillation (AF) is the most common sustained cardiac arrhythmia, and it is estimated that 1% of the population suffer from AF worldwide [1]. The prevalence of AF, the associated disease burden and the healthcare costs are all rising, commensurate with the ageing population [2, 3]. AF may be caused by valvular, typically rheumatic, disease, but the vast majority of cases are of nonvalvular aetiology. In this review, we will focus on nonvalvular AF. The morbidity and mortality associated with AF are considerable. Through mechanisms dependent on left atrial stasis and the associated endothelial dysfunction and dysregulation of coagulation, AF increases the risk of ischaemic stroke almost fivefold and is the major cardiovascular morbidity with an independent effect on stroke incidence [4]. The risk of stroke secondary pharmacokinetic and pharmacodynamic properties of the drugs and justifiable concerns about the consequent risk of haemorrhage. The non-VKA OACs (NOACs) have revolutionized thromboprophylaxis in AF by providing therapeutic options with predictable pharmacodynamic and pharmacokinetic properties that are as efficacious as warfarin in the prevention of stroke and thromboembolism but are more convenient to use. In this review, we provide a patient-centred framework to assist clinicians in recommending the right OAC therapy to fit the individual patient with AF, including methods for stratifying the risk of stroke and haemorrhage and the chances of achieving tight control of VKA anticoagulation, and we discuss the properties of the NOACs that favour their use in particular patient cohorts. Keywords: anticoagulation, atrial fibrillation, NOAC, stroke, warfarin. to either paroxysmal or permanent AF is the same and, from the perspective of thromboprophylaxis, should be treated in the same manner [5]. The consequences of AF are particularly pronounced in older individuals. Indeed, AF is believed to be responsible for 15% of ischaemic strokes overall, rising to 25% in the elderly population [6] Furthermore, AF is also an independent risk factor for myocardial infarction [7], cognitive decline [8], congestive cardiac failure [9] and all-cause mortality [10]. Thromboprophylaxis is critical for the prevention of strokes in patients with AF. Until recently, vitamin K antagonists (VKAs; e.g. warfarin) and aspirin have been widely used to manage the risk of ischaemic stroke in patients with AF. Aspirin remains in widespread use for primary stroke prevention in patients with AF, despite overwhelming evidence that oral anticoagulation is superior in most clinical situations and that ª 2015 The Association for the Publication of the Journal of Internal Medicine 1 A. M. Shields & G. Y. H. Lip aspirin is only minimally effective and confers a major bleeding risk that is similar to that of wellcontrolled warfarin [11–14]. This evidence is reflected in the most recent National Institute for Health and Care Excellence (NICE) [15] and European Society of Cardiology guidelines [16]. The VKAs are remarkably effective in stroke prevention; for example, well-controlled warfarin treatment can reduce the risk of ischaemic stroke and systemic embolism by up to two-thirds and is associated with a 26% relative risk reduction in all-cause mortality in patients with nonvalvular AF [12, 14, 17]. The risk of ischaemic stroke associated with AF is not homogenous and is dependent on a plethora of stroke risk factors [18]. Moreover, anticoagulation itself is not without risk, most notably of major haemorrhage. The risk of these two extremes of clinical outcome, thromboembolism and haemorrhage, may be amplified by poorly controlled anticoagulation [19]. As such, a variety of scoring systems have been developed to evaluate the risks of thrombosis and bleeding, thus aiding clinical decision-making when initiating anticoagulation [18, 20] (Table 1). The non-VKA oral anticoagulants (NOACs) have changed the landscape of thromboprophylaxis for ischaemic stroke by offering physicians and patients the opportunity to use effective anticoagulants with predictable pharmacokinetic profiles, wide therapeutic windows and fewer drug– drug and drug–food interactions without the need for intensive therapeutic drug monitoring. Individually, the NOACs have been shown to be noninferior to warfarin for the prevention of stroke and systemic embolism in patients with AF, although each has various properties that may favour use in particular patients, allowing physicians to fit the drug to the patient profile (and vice versa) [21–24]. As the therapeutic armamentarium for the management of ischaemic stroke risk in AF has expanded, clinical decision-making in terms of anticoagulant choice has become more complex. In this review, we first discuss the evidence supporting the use of the different anticoagulant drugs in different patient cohorts and conclude by advocating an individualized patient-centred approach to oral anticoagulant choice for patients with AF. 2 ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 Review: Stroke prevention in atrial fibrillation Anticoagulants for treatment of AF Until 2010, the VKAs such as warfarin were the only available oral anticoagulants to protect against stroke in patients with AF. Although warfarin is efficacious in stroke prevention in the context of AF [17], its use is limited by certain practicalities. Slow onset, drug–drug and drug–food interactions [25], genetic polymorphisms in CYP2C9 [26] and the vitamin K epoxide reductase complex subunit [27] and patient factors including comorbidities all affect the pharmacokinetic properties, dosing requirements and anticoagulant effect of warfarin, making it an unpredictable drug requiring regular, sometimes intensive, monitoring of the international normalized ratio (INR) to achieve maximum therapeutic effect and minimum risk of harm to the patient. Even when tight control of anticoagulation is achieved, adverse haemorrhagic events can still occur in patients treated with VKAs. The NOACs (previously referred to as new or novel oral anticoagulants [28]) were developed to provide efficacious anticoagulant drugs with rapid onset, a favourable side effect profile and predictable pharmacokinetic properties obviating the need for therapeutic drug monitoring [29, 30] (Table 2). Two classes of NOACs have been developed, and three drugs are currently licensed for use as anticoagulants in nonvalvular AF [31]: the direct thrombin inhibitors (dabigatran [21]) and the direct factor Xa inhibitors (rivaroxaban [22] and apixaban [24]). A further direct factor Xa inhibitor, edoxaban [23], has completed Phase III clinical trials and is licensed in Japan for use as thromboprophylaxis following lower limb orthopaedic surgery, for prevention of stroke and systemic embolism in nonvalvular AF and for the treatment and prevention of recurrent venous thromboembolism. Licence applications are in progress in Europe and North America for the use of edoxaban, particularly for stroke prevention and treatment of venous thromboembolism. All four agents have been found to be individually noninferior to warfarin for the prevention of stroke and systemic embolism in large, international randomized control trials [21–24]. In the most recent meta-analysis, including data from Phase III trials of all four agents, the NOACs significantly reduced stroke and systemic embolism compared to warfarin [relative risk (RR) 0.81, 95% confidence interval (CI) 0.73–0.91; P < 0.0001], intracranial A. M. Shields & G. Y. H. Lip Review: Stroke prevention in atrial fibrillation Table 1 Recommended risk assessment tools for stroke risk, bleeding risk and successful vitamin K antagonist-based anticoagulation in patients with atrial fibrillation Criteria Points Notes Congestive heart failure 1 Moderate to severe systolic left ventricular [LV] dysfunction, defined Hypertension 1 Patient on antihypertensives or two concurrent readings >140 systolic Age > 75 2 Diabetes 1 1) The CHA2DS2VASc score arbitrarily as left ventricular ejection fraction [LVEF] <40% and/or >90 diastolic Fasting blood glucose >7 mmol L 1 or patient on antihyperglycaemic drugs Stroke/TIA/thromboembolism 2 Vascular disease 1 Prior MI, angina,PCI, CABG, intermittent claudication, previous surgery or percutaneous intervention on the abdominal aorta or the lower extremity vessels, abdominal or thoracic surgery, aterial and venous thrombosis Age 65–74 1 Sex – female 1 Total 9 2) The HAS-BLED Score Hypertension 1 Patient on antihypertensives or two concurrent readings >140 systolic Abnormal liver and/or renal 1 (each) Dialysis, transplant, creatinine >200 lmol L and/or >90 diastolic , cirrhosis, bilirubin >29 upper limit of normal, AST/ALT/ALP >39 upper limit of normal function Stroke 1 1 Bleeding 1 Previous major haemorrhage, anaemia Labile INRs 1 TTR<60% Elderly 1 Age >65 or frail condition Drugs/Alcohol 1 (each) e.g. NSAIDs, >8 units week Total 9 1 3) The SAMeTT2R2 Score Sex – female 1 Age <60 1 Medical history (>2 1 comorbidities) Treatment (interacting drugs) 1 e.g. amiodarone Tobacco use 2 Any current smoking Race (ethnic minority) 2 Total 8 TIA, transient ischaemic attack; LV, left ventricular; LVEF, left ventricular ejection fraction; MI, myocardial infarction; PCI, percutaneous coronary intervention; CABG, coronary artery bypass grafting; INR, international normalized ratio; AST, aspartate aminotransferase; ALT, alanine transaminase; ALP, alkaline phosphatase; TTR, time in therapeutic range; NSAID, nonsteroidal anti-inflammatory drug. ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 3 A. M. Shields & G. Y. H. Lip Review: Stroke prevention in atrial fibrillation Table 2 The pharmacokinetic and pharmacodynamic properties of warfarin and the nonwarfarin oral anticoagulants Molecular target Warfarin Dabigatran Rivaroxaban Apixaban Edoxaban Vitamin K Thrombin Factor Xa Factor Xa Factor Xa dependent clotting factors Dosing in AF Once daily Twice daily Once daily Twice daily Once daily Time to peak 240.00 85–150 30–180 30–120 30–60 96–120 2 2–3 1–2 1–2 40.00 14–17 5–9 (increased to 8–15 9–11 plasma concentration (mins) Time to peak effect (h) Half life (h) 11–13 in elderly) Renal clearance <1% 80% 30% 27% 0.35 Food and drug Foods rich in Strong P-gp Strong CYP3A4 Strong inhibitors Strong P-gp interactions vitamin K, inhibitors and inducers, strong and inducers of inhibitors Substrates of inducers inhibitors of both CYP3A4 and P-gp CYP2C9, CYP3A4 CYP3A4 and P-gp and CYP1A2 Creatine clearance n/a <30 mL min 1 <15 mL min 1 <15 mL min 1 <30 mL min 1 (Japan) below which drug is contraindicated AF, atrial fibrillation; n/a, not applicable; P-gp, permeability glycoprotein. haemorrhage (RR 0.48, 95% CI 0.39–0.59; P < 0.0001) and all-cause mortality (RR 0.90, 95% CI 0.85–0.95; P = 0.0003) but increased the risk of gastrointestinal bleeding (RR 1.25, 95% CI 1.01–1.55; P = 0.04) in patients with AF [32]. Relative risk reductions in major haemorrhage rates were greatest in centres in which the mean time in therapeutic range (TTR) (i.e. mean time spent by patients with an INR between 2.0 and 3.0) was <66%, suggesting that NOACs have an advantage in healthcare systems where adequate control of anticoagulation cannot be achieved [32]. In a Cochrane meta-analysis of direct thrombin inhibitors, it was found that dabigatran 150 mg twice daily was superior to warfarin in the prevention of vascular death and ischaemic events [odds ratio (OR) 0.86, 95% CI 0.75–0.99] and direct thrombin inhibitors were associated with significantly lower rates of fatal and nonfatal major bleeding events, including haemorrhagic strokes (OR 0.87, 95% CI 0.78–0.97) [33]. A meta-analysis of the factor Xa inhibitors has also shown superi4 ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 ority over warfarin in the prevention of ischaemic and haemorrhagic stroke (OR 0.78, 95% CI 0.69– 0.89) and systemic embolic events (OR 0.53, 95% CI 0.32–0.87), and a reduced incidence of intracranial haemorrhage (OR 0.56, 95% CI 0.45–0.70) [34]. However, the evidence for a reduction in major haemorrhages with the factor Xa inhibitors is less robust due to heterogeneity within the studies included in the review [34]; re-analysis with data from the Effective Anticoagulation with Factor Xa Next Generation in Atrial Fibrillation–Thrombolysis in Myocardial Infarction 48 (ENGAGE AF-TIMI 48) study may be beneficial. To date, there is no evidence to suggest that any of the NOACs are superior to the others for the prevention of stroke in AF. Indirect comparison between the NOACs is made difficult by subtle differences between the patient cohorts enrolled in the randomized trials [35]. For example, the Rivaroxaban Once Daily Oral Direct Factor Xa Inhibition Compared with Vitamin K Antagonism for Prevention of Stroke and Embolism Trial in Atrial A. M. Shields & G. Y. H. Lip NO ANTITHROMBOTIC THERAPY REQUIRED CHA2DS2VASc ≥ 2 (female) or CHA2DS2VASc ≥ 1 (male) High risk of haemorrhagic complications Modify bleeding risk where possible e.g. uncontrolled hypertension, labile INRs, concomitant aspirin/NSAID use, alcohol excess HAS-BLED ≥ 3 Determine bleeding risk with HAS-BLED HAS-BLED < 3 Low risk ie. CHA2DS2VASc = 0 (male) or = 1 (female) STEP 1 Determine stroke risk with CHA2DS2VASc Review: Stroke prevention in atrial fibrillation Low risk of haemorrhagic complications STEP 2 Decide on VKA or NOAC Predict control of warfarin anticoagulation using SAMeTT2R2 NOAC SAMeTT2R2 > 2 (consider patient preferences & individual drug characteristics) SAMeTT2R2 0-2 DOSE-ADJUSTED VKA (INR 2.0–3.0) with TTR >70% (regularly review TTR and consider patient preferences) Antiplatelet therapy with aspirin-clopidogrel or – less effectively – aspirin monotherapy (consider only in patients who unwilling/unable to take any form of OAC whether VKA or NOAC Fig. 1 An algorithm for the risk assessment of atrial fibrillation (AF) patients about to start anticoagulation treatment. The assessment of risk of anticoagulation in patients with AF involves the use of the CHA2DS2VASc, HAS-BLED and SAMeTT2R scores to evaluate stroke risk, bleeding risk and likelihood of successful warfarin therapy, respectively. Non-vitamin K antagonist oral anticoagulants (NOACs) may be considered where the SAMeTT2R score predicts poor control of anticoagulation with warfarin. VKA, vitamin K antagonist; INR, international normalized ratio; NSAID, nonsteroidal antiinflammatory drug; OAC, oral anticoagulant; TTR, time in therapeutic range. Fibrillation (ROCKET-AF) trial included patients at greater baseline risk of stroke, and patients in the warfarin arm of this study spent a lower mean percentage of time (mean centre time in therapeutic range (cTTR) 59%) in the therapeutic range (2.0–3.0); by contrast, patients enrolled in the Randomized Evaluation of Long-Term Anticoagulation Therapy (RE-LY), Apixaban for Reduction in Stroke and Other Thromboembolic Events in Atrial Fibrillation (ARISTOTLE) and ENGAGE AFTIMI 48 trials all achieved a mean cTTR above 64% [22]. Nevertheless, particular characteristics of each agent, supported by evidence from clinical trials, may favour its use in specific patient populations. Choosing the right anticoagulant for the right patient There are two major decisions that must be made with respect to anticoagulation in AF. First, should a patient with AF start anticoagulant treatment for thromboprophylaxis and, secondly, which anticoagulant should be used. Here, we provide a framework to help clinicians answer these questions (Fig. 1). Should a patient with AF start anticoagulant treatment? The risk of stroke in AF is not homogenous, but depends on a variety of risk factors. The CHADS2 [congestive heart failure, hypertension, age ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 5 A. M. Shields & G. Y. H. Lip >75 years, diabetes, stroke (doubled)] risk score was developed and successfully validated to assist in risk stratification for patients with AF [36]. However, a number of important risk factors were omitted, including the increasing stroke incidence with age, vascular disease and female gender (in conjunction with other risk factors), which have subsequently been incorporated into the CHA2DS2VASc [congestive heart failure, hypertension, age >75 years (doubled), diabetes, stroke (doubled), vascular disease, age 65–74, sex category (female)] score [18, 37]. The CHA2DS2VASc score has been confirmed as a more effective method of stratifying stroke risk in patients with AF, compared to CHADS2, and is able to identify truly low-risk patients who would not benefit from anticoagulation [38]. Patients with a CHA2DS2VASc score of 0 (male) or 1 (female) are ‘low risk’ should not be prescribed an anticoagulant for stroke prevention as the risks outweigh the benefits. Patients with a CHA2DS2VASc score of ≥1 (male) or ≥2 (female) should be considered for anticoagulation after assessment of their bleeding risk. The CHA2DS2VASc score has been adopted by the European Society of Cardiology [39] and NICE [15] as the gold standard for stratifying stroke risk in patients with AF. Although trials comparing NOACs and warfarin have stratified stroke risk using the older CHADS2 score, the two scores share many important risk factors; no differences in the effect size for efficacy and safety have been observed in the RE-LY [40] and ARISTOTLE [41] trials in relation to CHA2DS2VASc score strata. Modelling studies have also demonstrated the net clinical benefit of different NOACs compared to warfarin across a range of CHA2DS2VASc scores [42]. Overestimation of bleeding risk is a major barrier to anticoagulant therapy, and several scoring systems have been developed to stratify this risk including ATRIA [43], HEMORR2HAGES [44] and HAS-BLED [20]. Of these scoring systems, HASBLED [uncontrolled hypertension (1 point), abnormal renal or liver function (1 point each), stroke (1 point), bleeding history or predisposition (1 point), labile INR (1 point), elderly (age >65 years) or frail (1 point), concomitant drugs/alcohol excess (1 point each)] offers the best prediction of bleeding risk and has been validated in both real-world and clinical trial cohorts [45, 46]. A HAS-BLED score of ≥3 is suggestive of a high risk of bleeding; however, this should not in itself contraindicate the initia6 ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 Review: Stroke prevention in atrial fibrillation tion of anticoagulation but rather alert the clinician to potential modifiable risk factors (e.g. hypertension, polypharmacy, alcohol excess, concomitant use of aspirin or nonsteroidal anti-inflammatory drugs) or guide the decision to initiate a NOAC instead of warfarin (e.g. labile INR) [47]. For example, in patients with a CHA2DS2VASc score of 1 (e.g. male patients with one identified stroke risk factor), the net clinical benefit of dabigatran and apixaban compared to VKA therapy only becomes positive in patients with a HAS-BLED score >3 [42]. Although either a VKA or NOAC may be successfully used as thromboprophylaxis in these patients, the decision of which anticoagulant should be used may be guided by patient choice and whether the patient is likely to achieve rapid and satisfactory control of VKA-based anticoagulation (TTR >70%) (see below). Which anticoagulant class to choose: VKAs or NOACs? Once the decision to initiate anticoagulation has been made, assessment of whether the patient is a suitable candidate for warfarin therapy is required. The net clinical benefit of warfarin increases the longer the patient remains within the therapeutic range achieving net benefit over antiplatelet therapy when the TTR is above 65–70%, with an optimal TTR defined as >70% in a recent European consensus document [48, 49]. Difficulty in achieving adequate control of anticoagulation with warfarin has been cited as a common barrier to its use [50]. In a systemic review, Wan et al. [51] found that poor control of anticoagulation correlated with increased bleeding and thromboembolic risk. Indeed, it has been shown that when TTR falls below 50%, stroke outcomes are worse than if the patient remained untreated [51, 52], and bleeding risk is higher [53]. Various patient factors including alcohol abuse, polypharmacy and hospitalization have been associated with erratic INR control. Furthermore, factors including concurrent diagnoses of dementia, cancer, nonalcohol substance misuse and bipolar disease have been associated with suboptimal anticoagulation [54]. The SAMeTT2R2 score [sex female, age <60 years, medical history (more than two comorbidities), treatment (interacting drugs, e.g. amiodarone for rhythm control), tobacco use (doubled), race (doubled)] has been developed to assist clinicians in deciding which patients are likely to achieve high-quality anticoagulation if A. M. Shields & G. Y. H. Lip treated with warfarin [55]. The SAMeTT2R2 score has been validated in prospective studies. Scores of >2 were associated with significantly increased risk of severe bleeding (RR 1.38, 95% CI 1.12–2.68; P = 0.002) and major haemorrhage as defined by the Bleeding Academic Research Consortium (BARC) (RR 1.77, 95% CI 1.29–2.44; P = 0.0005), and increasing scores correlated with labile INR, stroke, severe bleeding, major BARC bleeding and death [19]. This scoring system has subsequently been validated in a ‘real-world’ cohort of warfarintreated AF patients, and high scores were associated with significantly increased all-cause mortality [hazard ratio (HR) 1.41, 95% CI 1.16–1.67; P = 0.001], adverse cardiovascular events (HR 1.52, 95% CI 1.28–1.83; P < 0.001) and a trend towards increased major bleeding events (HR 1.23, 95% CI 0.99–1.53; P = 0.059) [56]. The importance of achieving satisfactory control of anticoagulation rapidly after starting warfarin has been illustrated by studies examining the incidence of stroke in the first month after warfarin initiation; this period was associated with a 71% increased relative risk of stroke, presumed to be due to the hypercoagulable state [57]. Suboptimal control of INR may contribute to increase the stroke risk and should not be tolerated. As such, we recommend that a patient’s SAMeTT2R2 score is calculated. Those patients with a score of ≤2 are likely to benefit from warfarin (TTR >70%), and therefore, this treatment could be considered [19, 56]. Patients with a SAMeTT2R2 score >2 are more likely to spend a greater amount of time outside the therapeutic range and to be exposed to the consequent risks of thrombosis and haemorrhage. In these patients, a NOAC should be considered, rather than subjecting them to a trial of warfarin or a ‘warfarin stress test’. Which NOAC to choose? Direct comparison of the results from large, international, multicentre randomized control trials of NOACs versus warfarin for thromboprophylaxis in AF is difficult due to differences in the mean CHADS2 score, TTR and rates of stroke and systemic embolism and haemorrhage in the warfarin arms of the trials [58–60]. Predetermined subgroup and post hoc analyses, as well as metaanalyses, have examined the risk and benefits of NOACs in different patient subgroups. These analyses can be helpful in guiding NOAC choices in challenging clinical situations; however, formal Review: Stroke prevention in atrial fibrillation trials are necessary to validate these existing data sets. (Fig. 2). Patients with renal impairment Renal impairment is associated with an increased incidence of stroke (secondary to co-existent risk factors) and is an independent risk factor for haemorrhage (HR 1.27, 95% CI 1.09–1.49) [61] due to dysregulation of coagulation and uraemiamediated platelet dysfunction. It is also common amongst patient with AF; an estimated one-third of individuals experience some degree of renal impairment [62]. Balancing thrombotic and haemorrhagic risk in these patients is complex, but of great importance. Both the incidence of AF and renal impairment increase with age; therefore, determining appropriate and safe anticoagulation for this growing population is an important clinical issue. The CHA2DS2VASc score has proven useful in stratifying patients with end-stage renal disease who require dialysis and are at risk of stroke secondary to AF, but the risk/benefit ratio of anticoagulation for these patients remains unclear [63]. VKAs have a poor safety profile in patients with nondialysis-dependent severe chronic kidney disease [estimated glomerular filtration rate (eGFR) <30 mL min 1], with these patients at a higher risk of major bleeding events and stroke compared to individuals with moderate renal impairment (eGFR 30–60 mL min 1) or compared to individuals with moderate renal impairment (eGRF 30– 60 mL min 1) or those without chronic kidney disease (eGFR > 60 mL min 1) [64]. Furthermore, renal impairment of any degree results in patients spending less time in the therapeutic range, potentially increasing their risk of complications of VKA therapy [64]. Data on the safety and efficacy of NOACs in patients with AF and renal impairment are limited. Dabigatran is principally excreted via the renal route (~80%), and patients with an eGFR <30 mL min 1 were excluded from the RE-LY trial [22, 24]. Although dose adjustment in renal impairment is possible, accumulation of dabigatran in the event of further renal insult is a significant risk and may lead to haemorrhagic complications. Subgroup analysis of the RE-LY trial has shown that the benefits of dabigatran [both 110 and 150 mg twice daily (b.d.)] in terms of stroke reduction and haemorrhage were consistent across all levels of renal function; however, in patients with an eGFR >80 mL min 1, dabigatran ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 7 A. M. Shields & G. Y. H. Lip Review: Stroke prevention in atrial fibrillation Individual patient groups and characteristics Asian patients Elderly patients Renal impairment Previous GI haemorrhage High bleeding risk (HASBLED ≥3) Recurrent stroke despite wellmanaged VKA Consider agents with reduced risk of ICH and major haemorrhage in Asian populations Consider comorbidities and agents with lower extracranial haemorrhage amongst elderly (age>75) Consider agents with lower haemorrhagic complications in moderatesevere renal impairment Consider agents with no increased risk of GI haemorrhage Consider agents with lower incidence of extracranial haemorrhage Consider agent with demonstrable benefit in reducing both ischaemic AND haemorrhagic stroke Preference for low pill burden Consider oncedaily formulations Patient less likely to do well on VKA (SAMeTT2R2 score >2) Avoid ‘trial of warfarin’ and consider NOAC upfront when deciding on OAC in newly diagnosed patient NOACs with characteristics beneficial to target group Apixaban Dabigatran Edoxaban Apixaban Edoxaban Apixaban Apixaban Dabigatran 110 mg Apixaban Dabigatran 110 mg Edoxaban Dabigatran 150 mg Edoxaban Rivaroxaban Any NOAC, but consider patient characteristics when choosing agent Fig. 2 Suggested patient groups in which specific non-VKA oral anticoagulants (NOACs) may be relatively advantageous or disadvantageous. The NOACs are all individually noninferior to warfarin in terms of efficacy for stroke prevention in patients with nonvalvular atrial fibrillation (AF). The evidence that may favour the use of a particular NOAC in various subgroups of patients is summarized. ICH, intracranial haemorrhage; GI, gastrointestinal; OAC, oral anticoagulant; VKA, vitamin K antagonist. was associated with significantly reduced rates of major bleeding compared to warfarin [65]. Fatal haemorrhagic complications have been reported in elderly patients with low body weight and impaired renal function treated with dabigatran [66]. In patients with renal dysfunction (eGFR of 30– 50 mL min 1) enrolled in the ROCKET-AF trial, there were no significant differences between the primary end-point of stroke and systemic embolism, and rates of the principal safety end-point of major and clinically relevant nonmajor bleeding, between warfarinand rivaroxaban-treated patients, although fatal bleeding occurred significantly less often in the rivaroxaban-treated group [67]. Apixaban is principally excreted via the biliary route. Subgroup analysis of the ARISTOTLE trial based on renal function demonstrated that apixaban was more effective than warfarin in the 8 ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 prevention of stroke and systemic embolism in patients regardless of renal function, and the greatest relative risk reduction of major haemorrhage was found in patients with an eGFR <50 mL min 1 [68]. This finding suggests that apixaban may be a favourable choice in patients with renal impairment. Approximately 35% of edoxaban is excreted renally. A formal subgroup analysis of the ENGAGE AF-TIMI 48 trial based on renal function has yet to be published. Elderly patients The prevalence of AF rises with age. Based on epidemiological studies, the prevalence of AF is estimated to be between 10.0% and 17.8% in patients over the age of 85 [69, 70]. Risk factors for stroke including hypertension, diabetes and previous transient ischaemic attack (TIA) are also significantly more likely in elderly patients with AF A. M. Shields & G. Y. H. Lip [70]. The results of the Birmingham Atrial Fibrillation Treatment of the Aged (BAFTA) trial [71] demonstrated that warfarin significantly reduces the incidence of stroke, systemic embolism or intracranial haemorrhage versus aspirin (RR 0.48, 95% CI 0.28–0.80; P = 0.003). In addition, it was shown in the Anticoagulation and Risk Factors In Atrial Fibrillation (ATRIA) study that the net clinical benefit of well-controlled warfarin therapy increases with age [72]. However, despite the evidence demonstrating the clear benefits of warfarin, it remains underused in the elderly. The Complications of Atrial Fibrillation in the BOlogna area (CAFBO) study [73] recently demonstrated that the majority of ischaemic events in patients with AF occurred in elderly individuals who received antiplatelet or no thromboprophylaxis. Furthermore, Hylek et al. [74] found that only 51% of patients aged 65 and over with AF received warfarin on discharge from hospital, with rates decreasing with age; perceived increased bleeding risk, falls and polypharmacy were cited as reasons for underuse. Of note, in a small study conducted in Scotland, UK, it was shown that dependency necessitating domiciliary INR monitoring and not age was a risk factor for bleeding episodes in warfarin-treated patients [75]. Furthermore, it has been estimated that a patient would have to fall more than 295 times per year for the risk of intracranial haemorrhage to outweigh the benefit of warfarin [76]. The NOACs have predictable pharmacokinetic properties with fewer drug–drug interactions and can be given without the need for regular therapeutic drug monitoring, thus offering considerable advantages over warfarin therapy. Patients over the age of 75 years were well represented in the RE-LY (43.1%), ROCKET-AF (31.2%), ARISTOTLE (40.2%) and ENGAGE AF-TIMI 48 (40.1%) trials. Meta-analysis of the trials involving rivaroxaban, apixaban and dabigatran showed that NOACs were more effective than conventional warfarin therapy in the prevention of stroke and systemic embolism; individual drugs were all found to be noninferior to warfarin in the elderly. Furthermore, the NOACs were not associated with any increase in major or clinically relevant bleeding events in patients over 75 years of age [77], although a nonsignificant trend towards higher rates of extracranial haemorrhage in these patients has been reported with dabigatran compared to warfarin [78]. Preliminary evaluation of data from the ENGAGE AF-TIMI 48 Review: Stroke prevention in atrial fibrillation trial has shown no significant interaction of age and major bleeding with edoxaban compared to warfarin [79]. However, the elderly population is extremely heterogeneous with respect to co-existent comorbidities and in each NOAC trial there were extensive exclusion criteria making the results difficult to generalize to the wider elderly population. Further real-world studies comparing anticoagulant therapies are necessary in this increasingly important and prevalent population. Currently, where physicians are unable to offer warfarin as a treatment for older patients with AF, the NOACs potentially provide an efficacious and arguably safer alternative. When deciding which drug to use, patients’ comorbidities and personal preferences for the dosing regimen (e.g. once-daily, twice-daily dosing) should be considered. Also, the fact that dabigatran capsules cannot be crushed and delivered via feeding tubes should be taken into consideration. Patients at high risk of haemorrhage The HAS-BLED score can be used to predict patients at high risk of haemorrhage, with a score of 3 or greater signifying significant risk [20]. In the first instance, attempts should be made to modify risk factors for bleeding before initiating treatment with any anticoagulant. However, where these risk factors cannot be modified, it is prudent to choose an agent with the lowest associated risk of haemorrhage. Compared to warfarin, each of the NOACs dramatically reduces the incidence of intracranial haemorrhage [32]. There are subtle differences between the agents with respect to other types of major haemorrhage. Low-dose dabigatran (RR 0.80, 95% CI 0.69–0.93; P = 0.003), apixaban (RR 0.69, 95% CI 0.60–0.80; P < 0.001) and edoxaban at high (RR 0.80, 95% CI 0.70–0.91; P < 0.001) and low dose (RR 0.47, 95% CI 0.41–0.55; P < 0.001) have demonstrated significantly reduced rates of major haemorrhage compared to warfarin. High-dose dabigatran and rivaroxaban were equivalent to warfarin in terms of the incidence of major haemorrhage, although TTR in the ROCKET-AF trial was lower, potentially raising the rate of haemorrhage in the warfarin arm. A recent meta-analysis has suggested that the NOACs are associated with increased incidence of gastrointestinal haemorrhage [32]. It is interesting that high-dose dabigatran (RR 1.50, 95% CI 1.19– 1.89; P < 0.001), high-dose edoxaban (RR 1.23, ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 9 A. M. Shields & G. Y. H. Lip 95% CI 1.02–1.50; P = 0.03) and rivaroxaban (3.2% vs. 2.2%, P < 0.001) were all associated with a significantly increased risk of gastrointestinal haemorrhage compared to warfarin in their respective trials, but low-dose edoxaban was associated with significantly less gastrointestinal bleeding (RR 0.67, 95% CI 0.53–0.83; P < 0.001). In a further imputed placebo and multiple treatment analysis, low-dose edoxaban was associated with significantly reduced rates of major bleeding than any of the other NOACs, offset by reduced efficacy for stroke prevention but nevertheless with overall benefit in terms of mortality [80]. In summary, in patients at high risk of gastrointestinal haemorrhage, it is reasonable to avoid high-dose dabigatran, high-dose edoxaban and rivaroxaban; low-dose edoxaban may be preferred, despite the reduced efficacy for stroke prevention. In patients with high HAS-BLED scores who have suffered major haemorrhage, low-dose dabigatran, apixaban and edoxaban are all appropriate choices of anticoagulant, but the risk of haemorrhage should be balanced carefully against the risk of stroke and patients’ personal preferences (see below). Patients with existing coronary or peripheral vascular disease The co-existence of coronary or peripheral artery disease and AF has been investigated in a number of clinical trials and real-world studies. The Atrial Fibrillation Clopidogrel Trial With Irbesartan for Prevention of Vascular Events (ACTIVE) W and ACTIVE A studies demonstrated prevalence rates, respectively, of 17% and 14% for previous myocardial infarction and 4% and 5% for peripheral vascular disease in AF patients [81, 82]. Similar prevalence rates have been found in the Danish population [83] and the EuroHeart survey of hospitalized AF patients [84]. Thus, there is considerable scope for the overlap of antiplatelet and anticoagulant treatments in patients with coronary or peripheral vascular disease and concurrent AF. Single and dual antiplatelet therapies provide firstline treatments for patients with coronary or peripheral artery disease [85, 86] and remain the first-line choice for patients with non-cardioembolic ischaemic stroke or TIA [87]. Management of thrombotic and haemorrhagic risk becomes extremely complicated in the context of elective or emergency coronary angioplasty in patients with AF [88]. Interestingly, De Caterina 10 ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 Review: Stroke prevention in atrial fibrillation et al. [89] suggested that 95.3% of patients receiving dual antiplatelet therapy and an oral anticoagulant and 63.8% treated with single antiplatelet therapy and an oral anticoagulant did not have an accepted indication, implying that many patients are put at an unnecessarily high bleeding risk. A comprehensive joint European consensus statement on the management of anticoagulation in patients with acute coronary syndrome or undergoing percutaneous coronary or valve interventions has recently been issued [90]. In all four trials comparing NOACs to warfarin in patients with AF, concurrent aspirin use was associated with higher incidence of major haemorrhage regardless of the treatment arm. However, the incidence of major haemorrhage when a NOAC was co-administered with aspirin was consistently lower than that seen with warfarin (dabigatran 150 mg and 110 mg vs. warfarin: 4.08% year 1 and 3.65% year 1 vs. 4.32% year 1; rivaroxaban vs. warfarin: 2.73% year 1 vs. 3.49% year 1; apixaban vs. warfarin: 2.7% year 1 vs. 3.7%; edoxaban 60 mg and 30 mg vs. warfarin: 3.62% year 1 and 2.00% year 1 vs. 4.71% year 1 [21–24, 78]). These data suggest that the NOACs offer promising safety advantages compared to warfarin when used in conjunction with antiplatelet therapy, but this must be confirmed in future studies. The possible association between dabigatran use and increased risk of myocardial infarction has been extensively investigated. Dabigatran (both 110 and 150 mg b.d.) was associated with higher rates of myocardial infarction compared to warfarin in the original RE-LY study (dabigatran 110 mg: RR 1.35; P = 0.07; dabigatran 150 mg: RR 1.38; P = 0.048) [21], and a meta-analysis showed an odds ratio of 1.33 (95% CI 1.03–1.71; P = 0.03) for acute coronary syndrome or myocardial infarction in studies comparing dabigatran to other anticoagulant treatments for a variety of indications [91]. However, this effect was not observed in an Asian subgroup of the RE-LY study [92], and post hoc analysis of this study including the incidence of silent myocardial events found no significant differences between warfarin- and dabigatran-treated patients [93]. There is some evidence that this effect may not be restricted to dabigatran and may reflect the fact that wellcontrolled warfarin can be protective against cardiac ischaemic events. Numerically, but nonsignificantly, more acute coronary events were recorded, compared to the warfarin-treated groups, A. M. Shields & G. Y. H. Lip in the North American cohort of the ROCKET-AF trial treated with rivaroxaban [22], the low-dose edoxaban arm of the ENGAGE AF-TIMI 48 trial [23], the edoxaban arm of the edoxaban for the treatment of acute, symptomatic venous thromboembolism (HOKUSAI-VTE) study [94] and the aspirin plus clopidogrel arm of ACTIVE-W [82]. Direct evidence of the benefit of NOACs in patients with AF and concurrent vascular disease is lacking. The Anti-Xa Therapy to Lower cardiovascular events in Addition to Standard therapy in subjects with ACS 2 Thrombolysis In Myocardial Infarction 51 (ATLAS ACS 2 TIMI 51) study has shown that rivaroxaban is superior to placebo in reducing cardiovascular and all-cause mortality in patients with recent acute coronary syndrome treated with single or dual antiplatelet therapy [95]. However, the dose of rivaroxaban used (2.5 mg b.d.) was less than that recommended for AF [20 mg once daily (o.d.)] and patients with AF were excluded; therefore, it is impossible to draw any firm conclusions from this study. Currently, there is little evidence to support the use of NOACs as an alternative to warfarin in patients with concurrent coronary or peripheral vascular disease on antiplatelet therapy, particularly in the early period after an episode of acute coronary syndrome or after coronary angioplasty. Further studies are needed to explore whether NOACs may be beneficial to patients in these circumstances. The 2014 joint European consensus document [90], endorsed by the Heart Rhythm Society and the Asia-Pacific Heart Rhythm Society (APHRS), recommends a period of triple therapy (oral anticoagulant, aspirin and clopidogrel), followed by oral anticoagulant and single antiplatelet (preferably clopidogrel) therapy and finally, when the patient is stable, an oral anticoagulant alone. The oral anticoagulant can be either a VKA with TTR >70% or a NOAC. The latter should be given in the lower tested dose used for AF stroke prevention (e.g. dabigatran 110 mg b.d., rivaroxaban 15 mg o.d. and apixaban 2.5 mg b.d.). Asian patients Despite a lower prevalence of AF amongst Asian patients, compared to Caucasians, they have a comparatively greater stroke prevalence due to a higher prevalence of stroke risk factors within the Asian population. However, they also have a much greater incidence of intracerebral haemorrhage, Review: Stroke prevention in atrial fibrillation compared to western populations [96]. The higher rates of haemorrhage remain poorly understood, but have led to significant undertreatment of nonvalvular AF with anticoagulant drugs in the Asian population [97]. Data from the primary randomized control trials and from secondary meta-analyses, regarding the efficacy and bleeding risks of anticoagulants in Asian subgroups of the RE-LY, ROCKET-AF, J-ROCKET-AF, ARISTOTLE and ENGAGE AF-TIMI 48 trials, have recently been reviewed [98, 99]. In summary, the data have shown that the NOACs are equally efficacious compared to warfarin for the prevention of stroke and systemic embolism in the Asian cohorts of these studies. Patients treated with high-dose dabigatran, apixaban or high-dose edoxaban were all shown to have significantly reduced incidence rates of stroke and systemic embolism compared to warfarin (150 mg dabigatran: RR 0.45, 95% CI 0.28–0.72; apixaban: RR 0.64, 95% CI 0.46–0.92; 60 mg edoxaban: HR 0.53, 95% CI 0.31–0.90). Furthermore, dabigatran (150 and 110 mg b.d.), apixaban and edoxaban (60 and 30 mg o.d.) have all shown lower incidence rates of intracranial haemorrhage (RR 0.20–0.41) and major bleeding events (RR 0.52–0.57) than dose-adjusted warfarin in the Asian cohorts [98, 100]. In the Japanese Rivaroxaban Once Daily Oral Direct Factor Xa Inhibition Compared with Vitamin K Antagonism for Prevention of Stroke and Embolism Trial in Atrial Fibrillation (J-ROCKET-AF) trial, rivaroxaban (15 mg o.d.) was found to be as effective as warfarin for stroke prevention, with no difference in the incidence of major haemorrhage [101]. Analysis of the major NOAC trials showed that haemorrhagic and thrombotic complications are more common in Asian patients receiving VKA therapy than in their Caucasian counterparts. In the RE-LY trial, a composite negative clinical outcome (including stroke, systemic embolism, pulmonary embolism, myocardial infarction, major bleeding and death) occurred in 9.65% of Asians compared with 7.61% of non-Asians [102]. Albertsen et al. [103] estimated that the relative risk of stroke in Asian patients receiving VKA therapy within the NOAC trials was 1.70 (95% CI 1.42– 2.03) compared to Caucasians. Of interest, within the RE-LY, ARISTOTLE and ROCKET-AF trials, the average TTR was lower and the percentage of time spent with an INR below 2 was higher amongst the Asian cohorts, compared to non-Asian groups; thus, their protection against stroke was reduced [99]. ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 11 A. M. Shields & G. Y. H. Lip The promising results of the NOAC trials have been reflected in both Japanese [104] and APHRS [105] guidelines for antithrombotic treatment in patients with AF, with NOACs (dabigatran and apixaban in the Japanese and APHRS guidelines, respectively) recommended as first-line anticoagulants for AF patients with a CHADS2 or CHA2DS2VASc score of 1. Warfarin is only recommended if the CHADS2 or CHA2DS2VASc score exceeds 1 and, even then, dabigatran (Japan) or dabigatran, rivaroxaban and apixaban (APHRS) are also recommended treatment options. When deciding between warfarin and a NOAC in Asian patients, it should be noted that the SAMeTT2R2 score automatically assigns Asian patients a score of 2 due to the difficulty in controlling anticoagulation within this population. Although the SAMeTT2R2 score has yet to be independently validated in an Asian cohort, warfarin would only be advisable in the absence of other risk factors that may jeopardize satisfactory control of anticoagulation. Patients with a high risk of stroke or a previous TIA/stroke Currently, there is little evidence to suggest the NOACs are superior to warfarin in the prevention of secondary stroke in patients with AF. A recent meta-analysis of the RE-LY, ROCKET-AF and ARISTOTLE trials demonstrated that dabigatran, rivaroxaban and apixaban were all noninferior to warfarin in this respect [106]. Apixaban was associated with the lowest risk of stroke or systemic embolism in patients who had already suffered a previous stroke or TIA (RR 0.77, 95% CI 0.57– 1.03), although this finding was not statistically significant [24]. The ENGAGE AF-TIMI 48 trial enrolled 1991 (28.3%), 1976 (28.1%) and 2006 (28.5%) patients who had suffered previous stroke or systemic embolism to receive warfarin, highdose and low-dose edoxaban, respectively [23]. The results of subgroup analysis from this study have yet to be published. In the four major clinical trials of NOACs compared to warfarin, patients were stratified by stroke risk using the CHADS2 score. Both highdose dabigatran (150 mg b.d.) (RR 0.73, 95% CI 0.58–0.91; P = 0.005) and apixaban (HR 0.79, 95% CI 0.66–0.95; P = 0.01 for superiority) demonstrated superiority to warfarin in the prevention of stroke and systemic embolism, with high-dose dabigatran also associated with a significantly lower incidence of ischaemic stroke compared to warfarin [21]. Subgroup analysis of the RE-LY trial 12 ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 Review: Stroke prevention in atrial fibrillation by CHADS2 score demonstrated that patients with the highest stroke risk (CHADS2 ≥3) achieved the greatest absolute reduction in risk of stroke with dabigatran 150 mg b.d. compared to warfarin (absolute risk reduction 0.85% year 1, 95% CI 0.16–1.85). Smaller reductions in absolute risk of stroke were seen in patients with a CHADS2 score <3 [107]. However, high-dose dabigatran was associated with a significantly increased rate of gastrointestinal bleeding (RR 1.50, 95% CI 1.19– 1.89; P < 0.001), and this risk should be carefully considered when using dabigatran in patients at high risk of stroke. In the ARISTOTLE trial, patients taking apixaban with a CHADS2 score >3 experienced significantly fewer strokes and systemic emboli than patients taking warfarin. At lower CHADS2 scores, apixaban was noninferior to warfarin. It is noteworthy that the reduced incidence of major haemorrhage associated with apixaban treatment was maintained in the cohort of patients with CHADS2 scores >3, suggesting a potential for use in patients at high risk of both stroke and haemorrhage [24]. Modified intentionto-treat analysis of the ENGAGE AF-TIMI 48 trial showed that high-dose edoxaban (60 mg o.d.) was also superior to warfarin in the prevention of stroke and systemic embolism (RR 0.79, 95% CI 0.63–0.99; P = 0.02 for superiority), but this did not reach statistical significance in the intentionto-treat analysis of the overall population (P = 0.08). Like dabigatran, high-dose edoxaban was associated with a significantly increased incidence of gastrointestinal haemorrhage (RR 1.23, 95% CI 1.02–1.50; P = 0.03) [23]. Rivaroxaban should also be considered for the treatment of patients at high risk of stroke or who have suffered a previous TIA/stroke. The ROCKETAF trial enrolled a cohort of patients at higher baseline risk of stroke (mean CHADS2 score of 3.5) and more patients who had suffered a previous stroke or TIA (55%) compared to the other NOAC trials [22]. Consequently, although it is clear that rivaroxaban is noninferior to warfarin in the prevention of stroke and systemic embolism in this cohort, further studies may be necessary to fully address the relative benefit of rivaroxaban compared to warfarin and other NOACs in patients at low risk of stroke (CHADS2 score of 0–1). Side effects and patient preference Adherence to medication is of greater importance with the NOACs than with warfarin due to their A. M. Shields & G. Y. H. Lip relatively shorter half-lives. Missed doses can lead to suboptimal anticoagulant effect and increased risk of stroke. As such, choosing a medication and achieving a regimen that is agreeable to the patient is essential. Consideration must be given to whether the patient is capable of and wishes to take a twice-daily (dabigatran and apixaban) or once-daily regimen (rivaroxaban and edoxaban). The common side effects of the NOACs are also becoming clear (e.g. dyspepsia with dabigatran) and should allow physicians to select medication choices to better suit their patients’ preferences. Of note, some patients may refuse or be unsuitable for warfarin or NOAC thromboprophylaxis. Combination antiplatelet therapy may have some benefits in reducing the risk of stroke in some patients with AF, although this benefit declines with increasing age and the risk of major bleeding remains [108]. The ACTIVE A trial investigated whether the addition of clopidogrel to aspirin offered any benefit in reducing the risk of vascular events including stroke in patients not suitable for VKA therapy [81]. The results showed that the addition of clopidogrel to aspirin significantly reduced the incidence of major vascular events (RR 0.89, 95% CI 0.81–0.98; P = 0.01) and ischaemic stroke (RR 0.72, 95% CI 0.62–0.83; P < 0.001) but also increased the incidence of major haemorrhage (RR 1.57, 95% CI 1.29–1.92; P < 0.001). Accordingly, the risks and benefits of such treatment should be carefully considered. Considering the individual: a patient-centred approach to anticoagulation The impact of AF on patients is considerable. In addition to the well-documented affect on organic disease, levels of psychological morbidity in AF patients are similar to those seen in patients with myocardial infarction and this negatively influences quality of life [109]. Indeed, individuals with AF have a significantly poorer quality of life compared to patients with coronary heart disease, the general population and matched healthy controls [110]. Stroke contributes to this poorer quality of life and is more severe with greater neurological deficits in patients with AF [111]. The risk of stroke is readily modified by anticoagulant therapy, yet the uptake of this therapy in individuals at high risk of stroke secondary to A with additional risk factors is poor, ranging from 54.9% in UK general practices [112] to 19–51% in patients enrolled in US health insurance schemes Review: Stroke prevention in atrial fibrillation [113]. Thus, the delivery of safe and effective thromboprophylaxis for patients with AF is inherently challenging. Ingelgard et al. [114] classified the barriers to warfarin use into four categories: patient medical characteristics, healthcare system factors, patient capability and patient preferences. Education of both patients and physicians will continue to play an important role in encouraging further use of anticoagulants for thromboprophylaxis. The Atrial Fibrillation Awareness and Risk Education (AF AWARE) group investigated the understanding of and attitudes towards AF of physicians and patients [115]. From the patients’ perspective, 55% of individuals recognized that AF was life threatening, but their principal concern was that of suffering a myocardial infarction or sudden cardiac event, rather than the risk of future stroke. Appropriate assessment and communication of the risk of stroke and the consequent risks and benefits of initiating anticoagulation should form the cornerstone of shared decision-making with patients regarding the management of their AF; communication is most successful when statistical information regarding risk is personalized to the individual [116]. Therefore, NICE has developed a decision-making aid [117] which, through pictorial representation, clearly considers the risk of stroke and haemorrhage associated with anticoagulant use, based on an individual’s CHA2DS2VASc score. Lahaye et al. [118] recently investigated the attitudes of a cohort of 172 inpatients to the initiation of anticoagulation for AF and found considerable interindividual variance in tolerance of bleeding risk in the context of anticoagulation for stroke prevention. In this study, patients were made aware of their individualized stroke risk, based on their CHA2DS2VASc score. On average, to initiate anticoagulation therapy, patients would tolerate a minimum absolute risk reduction in stroke per annum of 0.8%, or a 15% relative risk reduction. Furthermore, patients were willing to accept the risk of 4.4 major haemorrhages to prevent one stroke [118]. In general, patients were extremely stroke averse, regarding a minor stroke as only marginally worse than a major haemorrhage and a moderate or major stroke as equal to or worse than death, respectively [118]. This study, with participants knowing their individualized risk, confirms previous studies performed both in inpatient and outpatient settings demonstrating ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 13 A. M. Shields & G. Y. H. Lip considerable tolerance towards bleeding episodes in the context of thromboprophylaxis [118–120]. Only 12% of patients were medication averse, unwilling to consider treatment even if it was likely to be 100% effective [118]. Ingelgard et al. [114] found that the most common reason why individuals with AF were unwilling to initiate anticoagulation therapy was a reluctance to undertake regular INR monitoring. Physicians, however, have historically been more cautious in recommending anticoagulation therapy for patients with AF, reflected by the low rates of use of VKAs in patients at high risk of stroke [112, 113]. Advancing age, perceived bleeding risk and the risk of falls were all cited as major determinants of the failure to prescribe anticoagulants to patients with AF [114, 121]. Yet, Devereaux et al. [119] found that patients at high risk of stroke from AF placed much greater value on stroke avoidance than their physicians. Collectively, these findings suggest that physicians are not only under-treating patients at risk of debilitating strokes, but are also failing to acknowledge the importance patients place on avoiding these events. As such, physicians must be supported by clear evidence-based guidelines and/or algorithms to assist them in explaining the risk of stroke and anticoagulant-associated haemorrhage to patients with AF, and in managing these risks in partnership with the patient. Unfortunately, only 35% of physicians surveyed by the AF AWARE group thought that information available to patients with AF was easy to understand and 52% of patients surveyed in the West Birmingham Atrial Fibrillation Project study understood why anticoagulation treatment had been initiated for their AF [122]. Conclusion Despite overwhelming evidence demonstrating the net clinical benefit of anticoagulation for stroke prevention in patients with AF and emerging evidence that AF patients generally accept the risk of major haemorrhage to reduce their risk of disabling and debilitating strokes, the rates of anticoagulant prescription for patients with AF remain unacceptably low. The failure to recommend and prescribe anticoagulation is undoubtedly contributing to the stroke epidemic. Selecting and adhering to anticoagulant therapy remains challenging for physicians and patients with AF. Until 2010, VKAs were the only available 14 ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 Review: Stroke prevention in atrial fibrillation oral anticoagulants for patients with AF; the NOACs have revolutionized the field by offering predictable, easy-to-use drugs that are as efficacious as warfarin for stroke prevention, and associated with lower rates of intracranial haemorrhage and, in some circumstances, major haemorrhage. Moreover, it is becoming increasingly clear that in certain groups of patients at high risk of stroke who have historically been undertreated with warfarin (e.g. the elderly or those with renal impairment), the NOACs are superior to warfarin in terms of efficacy and/or safety. Further studies are needed to explore NOAC use in these groups to allow the development of clear unambiguous guidelines that may empower physicians to manage stroke risk more comprehensively in these high-risk patients. We propose a patient-centred, individualized approach to the management of thromboembolic risk in patients with AF. Indeed, with several NOAC drugs now available, we are perhaps ‘spoilt for choice’ and can fit the drug to the patient profile (and vice versa). The cornerstone of this approach is the effective communication of stroke risk and the relative risks and benefits of anticoagulation by the physician to the patient with AF. This depends on calculating patients’ individualized risks of stroke and haemorrhage (using CHA2DS2VASc and HAS-BLED) and their potential to achieve tight control of warfarin-based anticoagulation (using the SAMeTT2R2 score). More importantly, physicians must facilitate patients’ understanding of their individual risks and consider patients’ personal preferences to allow a fully informed and shared decision to be made about initiating anticoagulant therapy. Decision-making aids, such as that developed by NICE, can assist in this process. Conflict of interest statement Dr Adrian Shields has no conflict of interest to declare. Prof. Gregory Lip is a consultant for Bayer, Medtronic, Sanofi, BMS/Pfizer, Daiichi-Sankyo and Boehringer Ingelheim and has been a speaker for Bayer, BMS/Pfizer, Boehringer Ingelheim, Daiichi-Sankyo and Medtronic. Acknowledgements We thank Dr Kaivan Khavandi for medical editorial assistance. Financial support for this assistance was provided by Daiichi Sankyo Europe GmbH. A. M. Shields & G. Y. H. Lip References 1 Lip GY, Brechin CM, Lane DA. The global burden of atrial fibrillation and stroke: a systematic review of the epidemiology of atrial fibrillation in regions outside North America and Europe. Chest 2012; 142: 1489–98. 2 Naccarelli GV, Varker H, Lin J et al. Increasing prevalence of atrial fibrillation and flutter in the United States. Am J Cardiol 2009; 104: 1534–9. 3 Kim MH, Johnston SS, Chu BC et al. Estimation of total incremental health care costs in patients with atrial fibrillation in the United States. Circ Cardiovasc Qual Outcomes 2011; 4: 313–20. 4 Wolf PA, Abbott RD, Kannel WB. Atrial fibrillation as an independent risk factor for stroke: the Framingham Study. Stroke 1991; 22: 983–8. 5 Friberg L, Hammar N, Rosenqvist M. Stroke in paroxysmal atrial fibrillation: report from the Stockholm Cohort of Atrial Fibrillation. Eur Heart J 2010; 31: 967–75. 6 Lloyd-Jones D, Adams RJ, Brown TM et al. Heart disease and stroke statistics–2010 update: a report from the American Heart Association. Circulation 2010; 121: e46–215. 7 Chao TF, Huang YC, Liu CJ et al. Acute myocardial infarction in patients with atrial fibrillation with a CHADS-VASc score of 0 or 1: a nationwide cohort study. Heart Rhythm 2014; 11: 1941–7. 8 Kilander L, Andren B, Nyman H et al. Atrial fibrillation is an independent determinant of low cognitive function: a crosssectional study in elderly men. Stroke 1998; 29: 1816–20. 9 Stewart S, Hart CL, Hole DJ et al. A population-based study of the long-term risks associated with atrial fibrillation: 20year follow-up of the Renfrew/Paisley study. Am J Med 2002; 113: 359–64. 10 Benjamin EJ, Wolf PA, D’Agostino RB et al. Impact of atrial fibrillation on the risk of death: the Framingham Heart Study. Circulation 1998; 98: 946–52. 11 Aguilar MI, Hart R, Pearce LA. Oral anticoagulants versus antiplatelet therapy for preventing stroke in patients with non-valvular atrial fibrillation and no history of stroke or transient ischemic attacks. Cochrane Database Syst Rev 2007;(3): CD006186. 12 van Walraven C, Hart RG, Singer DE et al. Oral anticoagulants vs aspirin in nonvalvular atrial fibrillation: an individual patient meta-analysis. JAMA 2002; 288: 2441–8. 13 Ogilvie IM, Welner SA, Cowell W et al. Ischaemic stroke and bleeding rates in ‘real-world’ atrial fibrillation patients. Thromb Haemost 2011; 106: 34–44. 14 Hart RG, Pearce LA, Aguilar MI. Meta-analysis: antithrombotic therapy to prevent stroke in patients who have nonvalvular atrial fibrillation. Ann Intern Med 2007; 146: 857–67. 15 NICE. Atrial fibrillation: the management of atrial fibrillation. NICE 2014. Available at: www.nice.org.uk 16 European Heart Rhythm A, European Association for Cardio-Thoracic S, Camm AJ et al. Guidelines for the management of atrial fibrillation: the Task Force for the Management of Atrial Fibrillation of the European Society of Cardiology (ESC). Europace 2010; 12: 1360–420. 17 Investigators AF. Risk factors for stroke and efficacy of antithrombotic therapy in atrial fibrillation. Analysis of pooled data from five randomized controlled trials. Arch Intern Med 1994; 154: 1449–57. Review: Stroke prevention in atrial fibrillation 18 Lip GY, Nieuwlaat R, Pisters R et al. Refining clinical risk stratification for predicting stroke and thromboembolism in atrial fibrillation using a novel risk factor-based approach: the euro heart survey on atrial fibrillation. Chest 2010; 137: 263–72. 19 Lip GY, Haguenoer K, Saint-Etienne C et al. Relationship of the SAME-TT2R2score to poor quality anticoagulation, stroke, clinically relevant bleeding and mortality in patients with atrial fibrillation. Chest 2014; 146: 719–26. 20 Pisters R, Lane DA, Nieuwlaat R et al. A novel user-friendly score (HAS-BLED) to assess 1-year risk of major bleeding in patients with atrial fibrillation: the Euro Heart Survey. Chest 2010; 138: 1093–100. 21 Connolly SJ, Ezekowitz MD, Yusuf S et al. Dabigatran versus warfarin in patients with atrial fibrillation. N Engl J Med 2009; 361: 1139–51. 22 Patel MR, Mahaffey KW, Garg J et al. Rivaroxaban versus warfarin in nonvalvular atrial fibrillation. N Engl J Med 2011; 365: 883–91. 23 Giugliano RP, Ruff CT, Braunwald E et al. Edoxaban versus warfarin in patients with atrial fibrillation. N Engl J Med 2013; 369: 2093–104. 24 Connolly SJ, Eikelboom J, Joyner C et al. Apixaban in patients with atrial fibrillation. N Engl J Med 2011; 364: 806–17. 25 Holbrook AM, Pereira JA, Labiris R et al. Systematic overview of warfarin and its drug and food interactions. Arch Intern Med 2005; 165: 1095–106. 26 Aithal GP, Day CP, Kesteven PJ et al. Association of polymorphisms in the cytochrome P450 CYP2C9 with warfarin dose requirement and risk of bleeding complications. Lancet 1999; 353: 717–9. 27 D’Andrea G, D’Ambrosio RL, Di Perna P et al. A polymorphism in the VKORC1 gene is associated with an interindividual variability in the dose-anticoagulant effect of warfarin. Blood 2005; 105: 645–9. 28 Husted S, de Caterina R, Andreotti F et al. Non-vitamin K antagonist oral anticoagulants (NOACs): no longer new or novel. Thromb Haemost 2014; 111: 781–2. 29 Yeh CH, Fredenburgh JC, Weitz JI. Oral direct factor Xa inhibitors. Circ Res 2012; 111: 1069–78. 30 Lee CJ, Ansell JE. Direct thrombin inhibitors. Br J Clin Pharmacol 2011; 72: 581–92. 31 De Caterina R, Husted S, Wallentin L et al. General mechanisms of coagulation and targets of anticoagulants (Section I). Position Paper of the ESC Working Group on Thrombosis-Task Force on Anticoagulants in Heart Disease. Thromb Haemost 2013; 109: 569–79. 32 Ruff CT, Giugliano RP, Braunwald E et al. Comparison of the efficacy and safety of new oral anticoagulants with warfarin in patients with atrial fibrillation: a meta-analysis of randomised trials. Lancet 2014; 383: 955–62. 33 Salazar CA, del Aguila D, Cordova EG. Direct thrombin inhibitors versus vitamin K antagonists for preventing cerebral or systemic embolism in people with non-valvular atrial fibrillation. Cochrane Database Syst Rev 2014;(3): CD009893. 34 Bruins Slot KM, Berge E. Factor Xa inhibitors versus vitamin K antagonists for preventing cerebral or systemic embolism in patients with atrial fibrillation. Cochrane Database Syst Rev 2013;(8): CD008980. 35 Skjoth F, Larsen TB, Rasmussen LH et al. Efficacy and safety of edoxaban in comparison with dabigatran, rivaroxaban and ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 15 A. M. Shields & G. Y. H. Lip 36 37 38 39 40 41 42 43 44 45 46 47 48 16 apixaban for stroke prevention in atrial fibrillation. An indirect comparison analysis. Thromb Haemost 2014; 111: 981–8. Gage BF, Waterman AD, Shannon W et al. Validation of clinical classification schemes for predicting stroke: results from the National Registry of Atrial Fibrillation. JAMA 2001; 285: 2864–70. Karthikeyan G, Eikelboom JW. The CHADS2 score for stroke risk stratification in atrial fibrillation–friend or foe? Thromb Haemost 2010; 104: 45–8. Olesen JB, Torp-Pedersen C, Hansen ML et al. The value of the CHA2DS2-VASc score for refining stroke risk stratification in patients with atrial fibrillation with a CHADS2 score 0–1: a nationwide cohort study. Thromb Haemost 2012; 107: 1172–9. Camm AJ, Lip GY, De Caterina R et al. 2012 focused update of the ESC Guidelines for the management of atrial fibrillation: an update of the 2010 ESC Guidelines for the management of atrial fibrillation. Developed with the special contribution of the European Heart Rhythm Association. Eur Heart J 2012; 33: 2719–47. Oldgren J, Ezekowitz JA, Alings M et al. Dabigatran versus warfarin and impact of CHAD2-VASC score on outcome in atrial fibrillation patients: a RE-LY subgroup analysis (Abstract). J Am Coll Cardiol 2011; 57: E7. Lopes RD, Al-Khatib SM, Wallentin L et al. Efficacy and safety of apixaban compared with warfarin according to patient risk of stroke and of bleeding in atrial fibrillation: a secondary analysis of a randomised controlled trial. Lancet 2012; 380: 1749–58. Banerjee A, Lane DA, Torp-Pedersen C et al. Net clinical benefit of new oral anticoagulants (dabigatran, rivaroxaban, apixaban) versus no treatment in a ‘real world’ atrial fibrillation population: a modelling analysis based on a nationwide cohort study. Thromb Haemost 2012; 107: 584– 9. Fang MC, Go AS, Chang Y et al. A new risk scheme to predict warfarin-associated hemorrhage: the ATRIA (Anticoagulation and Risk Factors in Atrial Fibrillation) Study. J Am Coll Cardiol 2011; 58: 395–401. Gage BF, Yan Y, Milligan PE et al. Clinical classification schemes for predicting hemorrhage: results from the National Registry of Atrial Fibrillation (NRAF). Am Heart J 2006; 151: 713–9. Apostolakis S, Lane DA, Guo Y et al. Performance of the HEMORR(2)HAGES, ATRIA, and HAS-BLED bleeding riskprediction scores in patients with atrial fibrillation undergoing anticoagulation: the AMADEUS (evaluating the use of SR34006 compared to warfarin or acenocoumarol in patients with atrial fibrillation) study. J Am Coll Cardiol 2012; 60: 861–7. Roldan V, Marin F, Fernandez H et al. Predictive value of the HAS-BLED and ATRIA bleeding scores for the risk of serious bleeding in a “real-world” population with atrial fibrillation receiving anticoagulant therapy. Chest 2013; 143: 179–84. Lane DA, Lip GY. Use of the CHA(2)DS(2)-VASc and HASBLED scores to aid decision making for thromboprophylaxis in nonvalvular atrial fibrillation. Circulation 2012; 126: 860– 5. Connolly SJ, Pogue J, Eikelboom J et al. Benefit of oral anticoagulant over antiplatelet therapy in atrial fibrillation depends on the quality of international normalized ratio ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 Review: Stroke prevention in atrial fibrillation 49 50 51 52 53 54 55 56 57 58 59 60 61 62 63 64 control achieved by centers and countries as measured by time in therapeutic range. Circulation 2008; 118: 2029–37. De Caterina R, Husted S, Wallentin L et al. Vitamin K antagonists in heart disease: current status and perspectives (Section III). Position paper of the ESC Working Group on Thrombosis-Task Force on Anticoagulants in Heart Disease. Thromb Haemost 2013; 110: 1087–107. Baczek VL, Chen WT, Kluger J et al. Predictors of warfarin use in atrial fibrillation in the United States: a systematic review and meta-analysis. BMC Fam Pract 2012; 13: 5. Wan Y, Heneghan C, Perera R et al. Anticoagulation control and prediction of adverse events in patients with atrial fibrillation: a systematic review. Circ Cardiovasc Qual Outcomes 2008; 1: 84–91. Morgan CL, McEwan P, Tukiendorf A et al. Warfarin treatment in patients with atrial fibrillation: observing outcomes associated with varying levels of INR control. Thromb Res 2009; 124: 37–41. Gallego P, Roldan V, Marin F et al. Cessation of oral anticoagulation in relation to mortality and the risk of thrombotic events in patients with atrial fibrillation. Thromb Haemost 2013; 110: 1189–98. Razouki Z, Ozonoff A, Zhao S et al. Pathways to poor anticoagulation control. J Thromb Haemost 2014; 12: 628– 34. Apostolakis S, Sullivan RM, Olshansky B et al. Factors affecting quality of anticoagulation control among patients with atrial fibrillation on warfarin: the SAMe-TT(2)R(2) score. Chest 2013; 144: 1555–63. Gallego P, Roldan V, Marin F et al. SAME-TTR score, time in therapeutic range and outcomes in anticoagulated patients with atrial fibrillation. Am J Med 2014; 127: 1083–8. Azoulay L, Dell’Aniello S, Simon TA et al. Initiation of warfarin in patients with atrial fibrillation: early effects on ischaemic strokes. Eur Heart J 2014; 35: 1881–7. Skjoth F, Larsen TB, Rasmussen LH. Indirect comparison studies–are they useful? Insights from the novel oral anticoagulants for stroke prevention in atrial fibrillation. Thromb Haemost 2012; 108: 405–6. Harenberg J, Marx S, Wehling M. Head-to-head or indirect comparisons of the novel oral anticoagulants in atrial fibrillation: what’s next? Thromb Haemost 2012; 108: 407–9. Kansal AR, Sharma M, Bradley-Kennedy C et al. Dabigatran versus rivaroxaban for the prevention of stroke and systemic embolism in atrial fibrillation in Canada. Comparative efficacy and cost-effectiveness. Thromb Haemost 2012; 108: 672–82. Friberg L, Benson L, Lip GY. Balancing stroke and bleeding risks in patients with atrial fibrillation and renal failure: the Swedish Atrial Fibrillation Cohort study. Eur Heart J 2015; 36: 297–306. Kooiman J, van de Peppel WR, van der Meer FJ et al. Incidence of chronic kidney disease in patients with atrial fibrillation and its relevance for prescribing new oral antithrombotic drugs. J Thromb Haemost 2011; 9: 1652–3. Chao TF, Liu CJ, Wang KL et al. Incidence and prediction of ischemic stroke among atrial fibrillation patients with endstage renal disease requiring dialysis. Heart Rhythm 2014; 11: 1752–9. Kooiman J, van Rein N, Spaans B et al. Efficacy and safety of vitamin K-antagonists (VKA) for atrial fibrillation in non- A. M. Shields & G. Y. H. Lip 65 66 67 68 69 70 71 72 73 74 75 76 77 78 79 80 dialysis dependent chronic kidney disease. PLoS One 2014; 9: e94420. Hijazi Z, Hohnloser SH, Oldgren J et al. Efficacy and safety of dabigatran compared with warfarin in relation to baseline renal function in patients with atrial fibrillation: a RE-LY (Randomized Evaluation of Long-term Anticoagulation Therapy) trial analysis. Circulation 2014; 129: 961–70. Legrand M, Mateo J, Aribaud A et al. The use of dabigatran in elderly patients. Arch Intern Med 2011; 171: 1285–6. Fox KA, Piccini JP, Wojdyla D et al. Prevention of stroke and systemic embolism with rivaroxaban compared with warfarin in patients with non-valvular atrial fibrillation and moderate renal impairment. Eur Heart J 2011; 32: 2387–94. Hohnloser SH, Hijazi Z, Thomas L et al. Efficacy of apixaban when compared with warfarin in relation to renal function in patients with atrial fibrillation: insights from the ARISTOTLE trial. Eur Heart J 2012; 33: 2821–30. Heeringa J, van der Kuip DA, Hofman A et al. Prevalence, incidence and lifetime risk of atrial fibrillation: the Rotterdam study. Eur Heart J 2006; 27: 949–53. Langenberg M, Hellemons BS, van Ree JW et al. Atrial fibrillation in elderly patients: prevalence and comorbidity in general practice. BMJ 1996; 313: 1534. Mant J, Hobbs FD, Fletcher K et al. Warfarin versus aspirin for stroke prevention in an elderly community population with atrial fibrillation (the Birmingham Atrial Fibrillation Treatment of the Aged Study, BAFTA): a randomised controlled trial. Lancet 2007; 370: 493–503. Singer DE, Chang Y, Fang MC et al. The net clinical benefit of warfarin anticoagulation in atrial fibrillation. Ann Intern Med 2009; 151: 297–305. Palareti G, Salomone L, Cavazza M et al. Stroke/thromboembolism and intracranial hemorrhage in a ‘real world’ atrial fibrillation population: the CAFBO STUDY (Complications of Atrial Fibrillation in the BOlogna area). Chest 2014; 146: 1073–80. Hylek EM, D’Antonio J, Evans-Molina C et al. Translating the results of randomized trials into clinical practice: the challenge of warfarin candidacy among hospitalized elderly patients with atrial fibrillation. Stroke 2006; 37: 1075–80. Goudie BM, Donnan PT, Fairfield G et al. Dependency rather than old age increases the risk of warfarin-related bleeding. Br J Gen Pract 2004; 54: 690–2. Man-Son-Hing M, Nichol G, Lau A et al. Choosing antithrombotic therapy for elderly patients with atrial fibrillation who are at risk for falls. Arch Intern Med 1999; 159: 677–85. Sardar P, Chatterjee S, Chaudhari S et al. New oral anticoagulants in elderly adults: evidence from a meta-analysis of randomized trials. J Am Geriatr Soc 2014; 62: 857–64. Eikelboom JW, Wallentin L, Connolly SJ et al. Risk of bleeding with 2 doses of dabigatran compared with warfarin in older and younger patients with atrial fibrillation: an analysis of the randomized evaluation of long-term anticoagulant therapy (RE-LY) trial. Circulation 2011; 123: 2363– 72. Senoo K, Lane D, Lip GYH. Oral anticoagulants for stroke prevention in atrial fibrillation: anticoagulants in atrial fibrillation. Curr Probl Cardiol 2014; 39: 319–44. Verdecchia P, Angeli F, Lip GY et al. Edoxaban in the evolving scenario of non vitamin K antagonist oral anticoagulants imputed placebo analysis and multiple treatment comparisons. PLoS One 2014; 9: e100478. Review: Stroke prevention in atrial fibrillation 81 Investigators AWGotA, Connolly S, Pogue J et al. Clopidogrel plus aspirin versus oral anticoagulation for atrial fibrillation in the Atrial fibrillation Clopidogrel Trial with Irbesartan for prevention of Vascular Events (ACTIVE W): a randomised controlled trial. Lancet 2006; 367: 1903–12. 82 Investigators A, Connolly SJ, Pogue J et al. Effect of clopidogrel added to aspirin in patients with atrial fibrillation. N Engl J Med 2009; 360: 2066–78. 83 Olesen JB, Lip GY, Hansen PR et al. Bleeding risk in ‘real world’ patients with atrial fibrillation: comparison of two established bleeding prediction schemes in a nationwide cohort. J Thromb Haemost 2011; 9: 1460–7. 84 Nieuwlaat R, Capucci A, Camm AJ et al. Atrial fibrillation management: a prospective survey in ESC member countries: the Euro Heart Survey on Atrial Fibrillation. Eur Heart J 2005; 26: 2422–34. 85 Hamm CW, Bassand JP, Agewall S et al. ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation: the Task Force for the management of acute coronary syndromes (ACS) in patients presenting without persistent STsegment elevation of the European Society of Cardiology (ESC). Eur Heart J 2011; 32: 2999–3054. 86 Task Force on the management of STseamiotESoC, Steg PG, James SK et al. ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. Eur Heart J 2012; 33: 2569–619. 87 European Stroke Organisation (ESO) Executive Committee; ESO Writing Committee. Guidelines for management of ischaemic stroke and transient ischaemic attack 2008. Cerebrovasc Dis 2008; 25: 457–507. 88 Olesen JB, Gislason GH, Torp-Pedersen C et al. Atrial fibrillation and vascular disease–a bad combination. Clin Cardiol 2012; 35(Suppl 1): 15–20. 89 De Caterina R, Ammentorp B, Darius H et al. Frequent and possibly inappropriate use of combination therapy with an oral anticoagulant and antiplatelet agents in patients with atrial fibrillation in Europe. Heart 2014; 100: 1625–35. 90 Lip GY, Windecker S, Huber K et al. Management of antithrombotic therapy in atrial fibrillation patients presenting with acute coronary syndrome and/or undergoing percutaneous coronary or valve interventions: a joint consensus document of the European Society of Cardiology Working Group on Thrombosis, European Heart Rhythm Association (EHRA), European Association of Percutaneous Cardiovascular Interventions (EAPCI) and European Association of Acute Cardiac Care (ACCA) endorsed by the Heart Rhythm Society (HRS) and Asia-Pacific Heart Rhythm Society (APHRS). Eur Heart J 2014; 35: 3155–79. 91 Uchino K, Hernandez AV. Dabigatran association with higher risk of acute coronary events: meta-analysis of noninferiority randomized controlled trials. Arch Intern Med 2012; 172: 397–402. 92 Hori M, Connolly SJ, Ezekowitz MD et al. Efficacy and safety of dabigatran vs. warfarin in patients with atrial fibrillation– sub-analysis in Japanese population in RE-LY trial. Circ J 2011; 75: 800–5. 93 Hohnloser SH, Oldgren J, Yang S et al. Myocardial ischemic events in patients with atrial fibrillation treated with dabigatran or warfarin in the RE-LY (Randomized Evaluation of Long-Term Anticoagulation Therapy) trial. Circulation 2012; 125: 669–76. ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 17 A. M. Shields & G. Y. H. Lip 94 Hokusai VTEI, Buller HR, Decousus H et al. Edoxaban versus warfarin for the treatment of symptomatic venous thromboembolism. N Engl J Med 2013; 369: 1406–15. 95 Mega JL, Braunwald E, Wiviott SD et al. Rivaroxaban in patients with a recent acute coronary syndrome. N Engl J Med 2012; 366: 9–19. 96 Ducrocq G, Bhatt D, Labreuche J et al. Geographic differences in outcomes in outpatients with established atherothrombotic disease: results from the REACH Registry. Eur J Prev Cardiol 2014; 21: 1509–16. 97 Goto S, Oh S, Cools F et al. Regional differences in use of antithrombotic therapy for stroke prevention in atrial fibrillation and associated outcomes: European and Asian insights. Eur Heart J 2013; 34(Suppl 1): 790–1. 98 Sabir I, Khavandi K, Brownrigg J et al. Oral anticoagulants for Asian patients with atrial fibrillation. Nat Rev Cardiol 2014; 11: 290–303. 99 Chiang CE, Wang KL, Lip GY. Stroke prevention in atrial fibrillation: an Asian perspective. Thromb Haemost 2014; 111: 789–97. 100 Koretsune Y, Yamashita T, Yang Y et al. Edoxaban vs warfarin in East Asian (including Japanese) patients with atrial fibrillation – an ENGAGE AF-TIMI 48 subanalysis. Abstract: presented at the Japanese Circulation Society 2014 Annual Scientific Meeting, 2014. 101 Hori M, Matsumoto M, Tanahashi N et al. Rivaroxaban vs. warfarin in Japanese patients with atrial fibrillation – the J-ROCKET AF study. Circ J 2012; 76: 2104–11. 102 Hori M, Connolly SJ, Zhu J et al. Dabigatran versus warfarin: effects on ischemic and hemorrhagic strokes and bleeding in Asians and non-Asians with atrial fibrillation. Stroke 2013; 44: 1891–6. 103 Albertsen IE, Rasmussen LH, Overvad TF et al. Risk of stroke or systemic embolism in atrial fibrillation patients treated with warfarin: a systematic review and meta-analysis. Stroke 2013; 44: 1329–36. 104 Ogawa S, Hori M. Urgent statement on antithrombotic therapy of atrial fibrillation. Circ J 2011; 75: 2719–21. 105 Ogawa S, Aonuma K, Tse H-F et al. The APHRS’s 2013 statement on antithrombotic therapy of patients with nonvalvular atrial fibrillation. J Arrhythm 2013; 29: 190– 200. 106 Gomez-Outes A, Terleira-Fernandez AI, Calvo-Rojas G et al. Dabigatran, rivaroxaban, or apixaban versus warfarin in patients with nonvalvular atrial fibrillation: a systematic review and meta-analysis of subgroups. Thrombosis 2013; 2013: 640723. 107 Oldgren J, Alings M, Darius H et al. Risks for stroke, bleeding, and death in patients with atrial fibrillation receiving dabigatran or warfarin in relation to the CHADS2 score: a subgroup analysis of the RE-LY trial. Ann Intern Med 2011; 155: 660–7, W204. 108 van Walraven C, Hart RG, Connolly S et al. Effect of age on stroke prevention therapy in patients with atrial fibrillation: the atrial fibrillation investigators. Stroke 2009; 40: 1410–6. 18 ª 2015 The Association for the Publication of the Journal of Internal Medicine Journal of Internal Medicine, 2015, 278; 1–18 Review: Stroke prevention in atrial fibrillation 109 Thrall G, Lip GY, Carroll D et al. Depression, anxiety, and quality of life in patients with atrial fibrillation. Chest 2007; 132: 1259–64. 110 Thrall G, Lane D, Carroll D et al. Quality of life in patients with atrial fibrillation: a systematic review. Am J Med 2006; 119: 448 e1–e19. 111 Lamassa M, Di Carlo A, Pracucci G et al. Characteristics, outcome, and care of stroke associated with atrial fibrillation in Europe: data from a multicenter multinational hospitalbased registry (The European Community Stroke Project). Stroke 2001; 32: 392–8. 112 Mohammed MA, Marshall T, Nirantharakumar K et al. Patterns of warfarin use in subgroups of patients with atrial fibrillation: a cross-sectional analysis of 430 general practices in the United Kingdom. PLoS One 2013; 8: e61979. 113 Lang K, Bozkaya D, Patel AA et al. Anticoagulant use for the prevention of stroke in patients with atrial fibrillation: findings from a multi-payer analysis. BMC Health Serv Res 2014; 14: 329. 114 Ingelgard A, Hollowell J, Reddy P et al. What are the barriers to warfarin use in atrial fibrillation?: development of a questionnaire. J Thromb Thrombolysis 2006; 21: 257–65. 115 Aliot E, Breithardt G, Brugada J et al. An international survey of physician and patient understanding, perception, and attitudes to atrial fibrillation and its contribution to cardiovascular disease morbidity and mortality. Europace 2010; 12: 626–33. 116 Edwards A, Elwyn G, Mulley A. Explaining risks: turning numerical data into meaningful pictures. BMJ 2002; 324: 827–30. 117 NICE NIfHaCE. Atrial fibrillation: medicines to help reduce your risk of a stroke – what are the options?, 2014. 118 Lahaye S, Regpala S, Lacombe S et al. Evaluation of patients’ attitudes towards stroke prevention and bleeding risk in atrial fibrillation. Thromb Haemost 2014; 111: 465–73. 119 Devereaux PJ, Anderson DR, Gardner MJ et al. Differences between perspectives of physicians and patients on anticoagulation in patients with atrial fibrillation: observational study. BMJ 2001; 323: 1218–22. 120 Alonso-Coello P, Montori VM, Diaz MG et al. Values and preferences for oral antithrombotic therapy in patients with atrial fibrillation: physician and patient perspectives. Health Expect 2014; doi: 10.1111/hex.12201. [Epub ahead of print]. 121 Pugh D, Pugh J, Mead GE. Attitudes of physicians regarding anticoagulation for atrial fibrillation: a systematic review. Age Ageing 2011; 40: 675–83. 122 Lip GY, Kamath S, Jafri M et al. Ethnic differences in patient perceptions of atrial fibrillation and anticoagulation therapy: the West Birmingham Atrial Fibrillation Project. Stroke 2002; 33: 238–42. Correspondence: Gregory Y. H. Lip, University of Birmingham Centre for Cardiovascular Sciences, City Hospital, Birmingham B187QH, UK. (fax: 0121 554 4083; e-mail: [email protected]).