* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Outcome of Cushing`s Disease following Transsphenoidal Surgery
Survey
Document related concepts
Eradication of infectious diseases wikipedia , lookup
Epidemiology of metabolic syndrome wikipedia , lookup
Fetal origins hypothesis wikipedia , lookup
Public health genomics wikipedia , lookup
Seven Countries Study wikipedia , lookup
Epidemiology wikipedia , lookup
Transcript
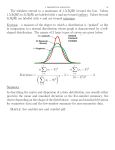
ORIGINAL E n d o c r i n e ARTICLE C a r e Outcome of Cushing’s Disease following Transsphenoidal Surgery in a Single Center over 20 Years Zaki K. Hassan-Smith, Mark Sherlock, Raoul C. Reulen, Wiebke Arlt, John Ayuk, Andrew A. Toogood, Mark S. Cooper, Alan P. Johnson, and Paul M. Stewart Centre for Endocrinology, Diabetes, and Metabolism (Z.K.H.-S., M.S., W.A., M.S.C., P.M.S.), Institute for Biomedical Research, School of Clinical and Experimental Medicine, University of Birmingham, Birmingham B15 2TT, United Kingdom; Departments of Endocrinology (A.A.T., J.A.) and Ear, Nose, and Throat Surgery (A.P.J.), University Hospitals Birmingham National Health Service Foundation Trust, Queen Elizabeth Hospital Birmingham, Birmingham B15 2TH, United Kingdom; and School of Health and Population Sciences (R.C.R.), University of Birmingham, Birmingham B15 2TT, United Kingdom Context: Historically, Cushing’s disease (CD) was associated with a 5-yr survival of just 50%. Although advances in CD management have seen mortality rates improve, outcome from transsphenoidal surgery (TSS), the current first-line treatment, varies significantly between centers. Objectives: The aim of the study was to define outcome including mortality in a cohort of CD patients treated with TSS over 20 yr. Design: We conducted a retrospective cohort study of 80 patients who underwent TSS to treat CD between 1988 and 2009. In 72 cases, data on clinical features and outcomes were collected from medical records. In eight patients, records were unavailable, but in all cases mortality data were obtained from National Health Service (NHS) registries and recorded as standardized mortality ratio. Setting: The study was conducted in a United Kingdom tertiary referral center. Patients or Other Participants: Adult patients confirmed to have CD participated in the study. Interventions: All patients underwent TSS. Main Outcome Measure: Patients were subdivided into groups based on disease response after initial treatment. Mortality according to subgroup was also assessed. Results: Median follow-up for clinical data was 4.6 yr. Three outcome groups were identified: cure, 72% (52 of 72); persistent disease, 17% (12 of 72); and disease recurrence, 11% (eight of 72). Median time to recurrence after initial remission was 2.1 yr (interquartile range, 1.3–3.1 yr). Mean follow-up for mortality was 10.9 yr. Thirteen of 80 patients had died: five of 52 in the cure group, two of eight in the disease recurrence group, two of 12 with persistent disease, and four of eight of those followed up by NHS registry search only. Overall, the standardized mortality ratio was 3.17 [95% confidence interval (CI), 1.70 –5.43], whereas in the cure group it was 2.47 (95% CI, 0.80 –5.77), and it was 4.12 (95% CI, 1.12–10.54) for disease recurrence/persistent disease groups. Conclusions: We report long-term cure rates in excess of 70%. Mortality is increased in CD and may be higher in patients with persistent/recurrent disease compared to patients cured after initial treatment. (J Clin Endocrinol Metab 97: 1194 –1201, 2012) ISSN Print 0021-972X ISSN Online 1945-7197 Printed in U.S.A. Copyright © 2012 by The Endocrine Society doi: 10.1210/jc.2011-2957 Received October 26, 2011. Accepted December 29, 2011. First Published Online January 25, 2012 1194 jcem.endojournals.org Abbreviations: BMI, Body mass index; CD, Cushing’s disease; CI, confidence interval; CSF, cerebrospinal fluid; DI, diabetes insipidus; IQR, interquartile range; MRI, magnetic resonance imaging; RR, relative risk; SMR, standardized mortality ratio; TSS, transsphenoidal surgery; UFC, urinary free cortisol. J Clin Endocrinol Metab, April 2012, 97(4):1194 –1201 J Clin Endocrinol Metab, April 2012, 97(4):1194 –1201 ushing’s disease (CD) is rare, with an incidence of up to 2 per million of the population/year (1), and it has a poor prognosis when left untreated. In his original case series, Harvey Cushing (2) observed a 4.6-yr median survival. Excess mortality is attributed largely to cardiovascular disease, and previous series have suggested that the risk normalizes with biochemical cure (3). Excess circulating cortisol produces significant morbidity through changes in body composition (sarcopenia, osteoporosis, central obesity), adverse metabolic profile (dyslipidemia, insulin resistance, diabetes mellitus), and arterial hypertension (4). In early series, adrenal surgery and pituitary radiotherapy were the mainstays of treatment for CD (5). Subsequently, transsphenoidal surgery (TSS) was established as the first-line treatment of choice (6 –10). However, a survey of 30 U.S. centers found that remission rates varied greatly, from between 90 and 100% in the best performing centers to as low as 10% (11). Surgical expertise and experience and the number of procedures per year are possible explanations for this variation. On this background, we describe the experience of a single center over two decades in the management of patients treated with TSS for CD. Our primary aims were 2-fold: 1) to assess the performance of a single center in the surgical treatment of CD by determining initial remission, long-term cure, and complication rates; and 2) to determine mortality rate in patients with CD, identify contributing factors, and establish the effect of cure on mortality. jcem.endojournals.org C Patients and Methods Inclusion and exclusion criteria Eighty patients who underwent TSS for CD between 1988 and 2009 were identified from the operating lists of a single surgeon (A.P.J.), at a United Kingdom tertiary referral center (University Hospitals Birmingham NHS Foundation Trust, Queen Elizabeth Hospital) and were included in this retrospective cohort study (Fig. 1). Fifty-eight of the 72 patients with information available underwent microscopic TSS (1988 –2007), with the remaining 14 undergoing endoscopic TSS (2005–2009). Demographic details All CD patients were treated with TSS as first-line definitive therapy. The median age at diagnosis was 40 yr [interquartile range (IQR), 31–50 yr], with a male to female ratio of 1:3.7. Median clinical follow-up after surgery was 4.6 yr (IQR, 1.7–9.7 yr). Median follow-up for mortality was 10.9 yr (IQR, 4.9 –15.6 yr). Clinical follow-up data were available on 72 patients. Clinical features at diagnosis At diagnosis, features associated with CD included arterial hypertension (78%), obesity (68%), osteoporosis (33%), dia- 1195 Paents post TSS N = 80 NHS Registry Search Only N=8 Notes assessed N = 72 Median clinical follow up 4.6yrs (IQR 1.7-9.7) Inial remission N = 60 (83%) Persistent disease N = 12 (17%) Cure N = 52 Recurrence N=8 Mean me to recurrence 2.1yrs (IQR 1.3-3.1) FIG. 1. Study design and treatment outcomes. Eighty patients with CD treated with TSS were identified from operative records. Full case notes were available in 72 of these patients, with data on clinical features, diagnostic tests, surgical complications, treatments, outcomes, and mortality recorded using a standardized proforma. Case notes were unavailable in eight patients; however, all patients were included in a search of NHS registries for mortality. Postoperatively patients were divided into two treatment outcome groups—initial remission and persistent disease— on the basis of biochemical data. Over follow-up, patients were further divided into cure and recurrence groups on the basis of clinical and biochemical data. betes mellitus (31%), dyslipidemia (12%), deep vein thrombosis (7%), and history of cardiovascular disease (6%). Of the 22 patients with diabetes, six were diet-controlled, 10 were prescribed oral hypoglycemic medications, and six were treated with insulin. Notable symptoms and signs were bruising (42%), hirsutism (36% of women), striae (29%), proximal myopathy (25%), thinning of skin (15%), buffalo hump (14%), and moon face (14%). Assessment of baseline electrocardiograms revealed evidence of left ventricular hypertrophy in 14% of patients, and cardiac ischemia in 8%. Eight of 18 (45%) patients with bone densitometry results available had normal bone density, six of 18 (33%) had evidence of osteopenia, and four of 18 (22%) had osteoporosis. Four of 66 (6%) patients had hypokalemia at diagnosis, and median urinary free cortisol (UFC) was significantly higher in these patients [154 g/dl; IQR, 96 –177 g/dl (4240 nmol/liter; IQR, 2669 – 4890 nmol/liter)] compared with those who were normokalemic [21 g/dl; IQR, 15– 40 g/dl (598 nmol/liter; IQR, 416-1102 nmol/liter); P ⫽ 0.003, Mann Whitney test). Diagnostic criteria Diagnosis was confirmed by P.M.S. and colleagues at the Department of Endocrinology at Queen Elizabeth Hospital Birmingham by adherence to agreed protocols. Diagnosis and differential diagnosis were confirmed on the basis of biochemical tests including UFC, diurnal measurements of serum ACTH and cortisol, low- and high-dose dexamethasone suppression tests, and CRH tests. Early cases underwent computed tomography scanning of the pituitary (n ⫽ 16); however, from 1992, all patients underwent magnetic resonance imaging (MRI) (n ⫽ 56). Patients’ x-ray films were reported by specialist neuroradiologists and reviewed by both surgeons and endocrinologists in a joint clinic and, more recently (from 2008 onward), a monthly 1196 Hassan-Smith et al. Cushing’s Disease Postoperative Outcomes J Clin Endocrinol Metab, April 2012, 97(4):1194 –1201 pituitary multidisciplinary team meeting. Selected patients with discordant results underwent inferior petrosal sinus sampling before first TSS (n ⫽ 13). tered with and approved by the University Hospitals Birmingham Clinical Audit Department. Surgical technique Results If a suspected adenoma was identified at surgery, it was removed along with a small part of adjacent tissue to check clear histological margins. The general approach to surgery was to remove the adenoma completely and to prevent damage to normal tissue. MRI was used initially to lateralize tumor and indicate initial area of surgical exploration (n ⫽ 39). In the event that no adenoma was identified on MRI, a full exploration of the gland was performed, with the complete removal of adenoma if identified. If an adenoma was not identified, approximately three fourths to seven eighths of the gland was removed. Data collection Clinical records were available from 72 cases. In the remaining eight patients, full clinical records were unavailable, but mortality data on all 80 cases was ascertained from an electronic search of National Health Service (NHS) registries. In patients no longer under follow-up locally, referring endocrinologists were contacted to obtain current clinical data (n ⫽ 14). For the assessment of mortality, status was recorded as either dead or alive, as of November 29, 2010. Death certificates were obtained to establish cause of death. Treatment outcome groups Eighty-three percent (60 of 72) achieved an initial disease remission, of which eight suffered disease recurrence. Median time to recurrence was 2.1 yr (IQR, 1.3–3.1 yr). Of the three outcome groups, cure was achieved in 72% (52 of 72), persistent disease in 17% (12 of 72), and recurrent disease in 11% (eight of 72) (or eight of the 60 patients achieving initial remission, 13%). A proportion (seven of 12) of the persistent disease group had normal initial postoperative serum cortisol levels. There was no statistically significant difference in numbers achieving initial remission between those undergoing TSS before and after the year 2000 (27 of 34 ⫽ 79%, 33 of 38 ⫽ 87%, respectively; P ⫽ 0.53, using Fisher’s exact test). All 14 patients treated with endoscopic TSS achieved long-term remission, although the median follow-up period was shorter than the group as a whole, at 25 months (IQR, 18.0 –38.5 months). Criteria for short- and long-term outcome In 72 patients, median follow-up was 4.6 yr. Patients were categorized into two groups—initial remission and persistent disease—according to outcome after TSS. Initial remission was defined by a morning postoperative cortisol level of less than 1.8 g/dl (50 nmol/liter) (measured between d 4 and wk 6). Patients were then further categorized into three long-term outcome groups: cure, recurrent disease, and persistent disease. Cure defined those patients with ongoing absence of hypercortisolism at last follow-up. Recurrent disease was defined on biochemical grounds (raised UFC or failure of cortisol suppression on dexamethasone suppression test) and on clinical grounds after initial remission. Persistent disease was defined biochemically by a postoperative cortisol of more than 1.8 g/dl (50 nmol/liter). Mortality Follow-up data on mortality were available in 80 patients, with a median follow-up of 10.9 yr. Mortality was assessed by the standardized mortality ratio (SMR), calculated as the ratio of observed over expected deaths (12). The expected number was estimated by multiplying age, calendar year, and sex stratumspecific mortality rates for the general population of England and Wales by the corresponding person-years at risk among the CD patients. Overall survival by clinical follow-up was estimated by Kaplan-Meier curves and the log-rank test used to test for differences. A multivariable Cox regression model with attained age as the time metric was used to derive relative risks (RR) for the factors sex and age (⬍40 yr vs. at least 40 yr). Statistical significance was taken as a P value ⬍0.05. Ethics The study was completely retrospective in nature and involved no intervention beyond usual patient care. It was regis- Resolution of clinical features Arterial hypertension Of the 56 of 72 (78%) patients with hypertension at baseline, 37 were on antihypertensive medications. Thirty percent (11 of 37) of patients reduced their antihypertensive medication within 6 wk of surgery, and 32% (12 of 37) stopped these medications altogether. There were statistically significant reductions in systolic and diastolic blood pressure between diagnosis, 6 wk, and final followup. However, there was no statistically significant difference between blood pressure at 6 wk and final follow-up (Table 1). Obesity Height and weight data were available on 36 patients. Median body mass index (BMI) at baseline was 30 kg/m2 (IQR, 27–35 kg/m2). There were statistically significant reductions in BMI between diagnosis and 6 wk postoperatively and between 6 wk and final follow-up. Second-line treatment for persistent and recurrent disease Further treatment for active disease included revision TSS (n ⫽ 16), bilateral adrenalectomy (n ⫽ 9), and radiotherapy (n ⫽ 8). For recurrent disease (n ⫽ 8), this was subdivided into TSS (n ⫽ 6), adrenalectomy (n ⫽ 5), radiotherapy (n ⫽ 3), and no treatment (n ⫽ 1). For persis- J Clin Endocrinol Metab, April 2012, 97(4):1194 –1201 TABLE 1. Resolution of clinical features: changes in BMI, systolic blood pressure, and diastolic blood pressure between diagnosis and post-TSS Systolic blood Diastolic blood pressure pressure BMI (mm Hg)b (mm Hg)c (kg/m2)a Diagnosis 30 (27–35) 150 (130 –162) 90 (80 –100) 6 wk post-TSS 29 (27–34) 124 (110 –150) 80 (76 –90) Final follow-up 27 (23–32) 130 (116 –140) 82 (76 – 86) Data are expressed as median (IQR). a Median BMI for the group preoperatively was 30 kg/m2 (IQR, 27–35 kg/m2), at 6 wk this was reduced to 29 kg/m2 (IQR, 27–34 kg/m2), and by final follow-up this was reduced to 27 kg/m2 (IQR, 23–32 kg/m2). Diagnosis vs. 6 wk, P ⫽ 0.006; diagnosis vs. final follow-up, P ⫽ 0.0004; and 6 wk vs. final follow-up, P ⫽ 0.003, Wilcoxon matched pairs test. b At diagnosis, median systolic blood pressure was 150 mm Hg (IQR, 130 –162 mm Hg). At 6 wk this dropped to 124 mm Hg (IQR, 110 – 150 mm Hg) (P ⬍ 0.0001). At final follow-up, it was 130 mm Hg (IQR, 116 –140 mm Hg) (P ⬍ 0.0001). c Median diastolic blood pressure was 90 mm Hg (IQR, 80 –100 mm Hg) at diagnosis, dropping to 80 mm Hg (IQR, 76 –90 mm Hg) (P ⬍ 0.0001) 6 wk postoperatively, whereas at final follow-up it was 82 mm Hg (IQR, 76 – 86 mm Hg) (P ⬍ 0.0001). There were no significant changes in blood pressure between 6 wk postoperative and final follow-up. tent disease, this was subdivided into TSS (n ⫽ 10), radiotherapy (n ⫽ 5), and adrenalectomy (n ⫽ 4). Only one patient had persistent disease at final follow-up. Complications of surgery Common postoperative complications included transient diabetes insipidus (DI) (35%) and cerebrospinal fluid (CSF) leak (11%) (eight of 72 total; six required repair and two resolved spontaneously). Infrequent complications included meningitis (n ⫽ 3), sinusitis (n ⫽ 2), septal perforation (n ⫽ 1), and blocked lacrimal duct (n ⫽ 1). There were no statistically significant differences in complication rates, including between endoscopic and microscopic TSS. Hypopituitarism rates Preoperatively there were limited data recorded on rates of hypopituitarism. However, the frequency of TSH deficiency was 11% (four of 38) and of gonadotropin deTABLE 2. jcem.endojournals.org 1197 ficiency, 17% (seven of 41). In the immediate postoperative period, all patients were put on replacement doses of hydrocortisone. Of the patients achieving cure (n ⫽ 52), hypothalamic-pituitary-adrenal axis recovery was observed in 23 (44%) patients over the follow-up period. At final follow-up, 51 of 72 (71%) patients had deficiency of at least one pituitary hormone, with ACTH being affected in the majority of these cases. Frequencies of TSH and LH/FSH deficiencies were significantly higher in the recurrent/persistent disease groups (75 and 50%) vs. the cure groups (37 and 21%) (P values 0.004 and 0.02, respectively, using Fisher’s exact test). Mortality There were 13 deaths. Five occurred in the cure group, two in the recurrent disease group, two with persistent disease, and four in the group followed up only by NHS registry data. Causes of death as recorded on death certificates were: cardiovascular disease in eight cases, cancer in three cases, infection in one case, and CD in one case. The overall SMR was 3.17 [95% confidence interval (CI), 1.70 –5.43], on the basis of 13 deaths being observed in our cohort, compared with 4.10 expected (Table 2). The SMR for the patients achieving cure was lower at 2.47 (95% CI, 0.80 –5.77), and SMR for recurrent/persistent disease was 4.12 (95% CI, 1.12–10.54), but this did not reach statistical significance. Kaplan-Meier analysis was performed for the group overall and divided into treatment outcome group. There were no statistically significant differences in time to death between these groups. Median age at death was 57 yr (IQR, 57– 64 yr). Female sex had a RR of 4.5 (95% CI, 0.58 –34.54), whereas the RR for age at diagnosis (⬍40 or ⬎40 yr) was 0.31 (95% CI, 0.09 –1.15). Predictive indicators of cure Logistic regression analysis, with models adjusted for age at diagnosis, sex, and age at final follow-up, was used to identify possible predictors of long-term cure vs. persistent/recurrent disease. Pituitary adenoma histology positive for ACTH staining was associated with an odds ratio of 4.4 (95% CI, 1.3–15.3; P ⫽ 0.015). Preoperative Standardized mortality ratios Overall Persistent and recurrent disease Cured Observed deaths 13 4 5 Expected deaths 4.10 0.97 2.02 SMR 3.17 4.12 2.47 95% CIa 1.70 –5.43 1.12–10.54 0.80 –5.77 P value ⬍0.001 0.34 0.03 The overall SMR was 3.17 (95% CI, 1.70 –5.43) on the basis of 13 deaths being observed in our cohort, compared to 4.10 expected. The SMR for the patients achieving cure was lower at 2.47 (95% CI, 0.80 –5.77), and SMR for disease recurrence/persistent disease was 4.12 (95% CI, 1.12–10.54). a CI and P values were calculated using Fisher’s exact test. 1198 Hassan-Smith et al. Cushing’s Disease Postoperative Outcomes UFC below 1000 nmol/liter was associated with an odds ratio of 3.6 (95% CI, 0.9 –14.1; P ⫽ 0.05). Preoperative systolic blood pressure (odds ratio, 1.0; 95% CI, 0.3–3.3) and MRI evidence of pituitary adenoma (odds ratio, 1.9; 95% CI, 0.5–7.6) did not reach statistical significance. Discussion With a follow-up for mortality in excess of 10 yr, our study is surpassed only by one study that included historical data going back as far as 1960 (13). After Harvey Cushing’s first description, the female preponderance of CD was recognized (2). Our study reports a male-to-female ratio of 1:3.7, compared with previously described series that range from 1:2 to 1:15 (3). The reasons for the gender differences in CD are unknown; however, estrogen responsiveness of corticotroph adenoma tissue has been implicated (14, 15). The clinical features of CD result from the effects of excess glucocorticoids on target tissues. The phenotype is one of altered body composition, with sarcopenia, osteoporosis, thinning of the skin, fatty liver, and obesity with increased visceral to peripheral adipose stores, with major morbidity and mortality resulting from cardiovascular disease. The most commonly reported symptoms and signs for all patients in this study (bruising, striae, proximal myopathy, and thinning of skin) are those that are recognized to most reliably distinguish CD from obesity (1). Our data on clinical features present at diagnosis support previous findings, with high frequencies of hypertension (78%), obesity (68%), and diabetes mellitus (31%). The increase in blood pressure along with other factors may be implicated in the altered left ventricular structure and function associated with glucocorticoid excess (16). Although more commonly associated with the state of apparent mineralocorticoid excess induced by saturation of 11-hydroxysteroid dehydrogenase type 2 with cortisol in ectopic ACTH syndrome (17), hypokalemia was found at a frequency of 6% in our study. Our results demonstrate that high cortisol production rates are associated with hypokalemia in CD, in keeping with saturation of 11-hydroxysteroid dehydrogenase type 2. Also of note is the significant frequency of deep vein thrombosis in the cohort (7%), which is likely to be secondary to glucocorticoidinduced hypercoagulability (18). Thorough preoperative assessment of comorbidities with optimization of therapy (i.e. antihypertensives, antithrombotic measures) would improve outcomes. Data on changes in body weight after TSS in CD are scarce and are limited to small case series with limited follow-up (19, 20). Our data demonstrate the rapid and J Clin Endocrinol Metab, April 2012, 97(4):1194 –1201 sustained clinical improvements seen after successful TSS. Reductions in blood pressure occur in the first 6 wk, whereas for BMI there are significant reductions after longer follow-up. Previous studies have shown normalization of blood pressure patterns in CD after TSS (21). However, it has been suggested that cardiovascular risk factors, including BMI, waist-hip ratio, serum lipids, and markers of insulin resistance and of atherosclerosis, remain elevated for as long as 5 yr after normalization of hypercortisolemia (22). Our initial remission (83%), persistent disease (17%), and recurrent disease (13%) rates compare well with other series from large specialist centers, with ranges in the literature of 65–90, 10 –24, and 5–22% (8 –10, 13, 23, 24), respectively. Median time to recurrence in previous series ranged between 20 and 84 months (25, 26). There are fewer data on cure rates after single surgery, but our rate of 72% is very favorable compared to previously described studies (56 –72%). In the event of persistent or recurrent disease, second-line treatment in our cohort involved a combination of therapies, achieving a high remission rate (98%) at final follow-up. A limitation of our study due to its retrospective nature was the absence of data on postoperative UFC, suppression after dexamethasone suppression test, and diurnal rhythm of cortisol secretion. For this reason, a strict biochemical definition for initial remission was used (serum cortisol ⬍1.8 g/dl). This meant that the subgroup of patients with normal rather than undetectable cortisol secretion postoperatively could not be fully characterized. Transient DI and postoperative CSF leak were the most common complications after TSS. Our complication rates were in the range of those previously described (transient DI, 6 –58%; CSF leak, 2–13%) (27). There were low rates of other recognized complications. Rates of TSH (33%), LH/FSH (29%), and GH (29%) deficiencies at final follow-up are similar to those reported in a previous large study (TSH, 32%; LH/FSH, 30%; GH, 32%) (10). It has been suggested that GH deficiency is underreported in patients with long-term cure from CD, with rates of 65% seen in a prospective study (28). However, our rates of hypopituitarism of any degree (71%) and ACTH deficiency (57%) are in the upper end of the range described in the literature (37–59%) (10, 29). The primary explanation for this could be that this is a reflection of the aggressive pursuit of cure, as evidenced by our high cure and initial remission rates. Alternatively, this could be due to differences in study design, with our rates purely reflecting those at final follow-up, after multiple treatments in some cases. The significant differences in rates of TSH and LH/FSH between the cure and recurrent disease groups highlight the more aggressive approach taken in J Clin Endocrinol Metab, April 2012, 97(4):1194 –1201 TABLE 3. jcem.endojournals.org 1199 Comparison of studies First author, Period of year (Ref.) Patients TSS Etxabe, 1994 (6) 49 1975–1992 (17 yr) Swearingen, 1999 (7) 161 1978 –1996 (18 yr) Pikkarainen, 1999 (30) 63 1981–1994 (13 yr) Lindholm, 2001 (8) 73 1985–1995 (10 yr) Hammer, 2004 (9) 289 1975–1998 (23 yr) Dekkers, 2007 (10) 74 1977–2005 (28 yr) Clayton, 2011 (13) 60 1960 –2009 (49 yr) This paper 80 1988 –2009 (21 yr) SMR persistent/ Initial recurrent Overall remission Follow-up No. of SMR disease SMR (95% CI) (%) (months) deaths cure 88 56 5/49 N/A N/A 3.80 (2.5–17.9) 90 96 6/159 N/A N/A 0.98 (0.44 –2.2) 34 84 6/43 N/A N/A 2.67 (0.89 –5.2) 66 96 7/73 0.31 5.1 1.70 (0.7–3.5) 82 132 25/289 1.18 (N/S) 2.8 1.42 (0.95–2.1) 80 120 12/74 1.8 (N/S) 4.38 2.39 (1.2–3.9) 90 180 13/60 3.3 16 4.80 (2.8 – 8.3) 83 132 13/80 2.47 (N/S) 4.12 3.17 (1.7–5.3) Our initial remission rate of 83% sits in the range of 33.8 –90% reported by previous studies. Our follow-up period of 132 months is only surpassed by one other study (Clayton et al.). Taking the studies as a whole, it is clear that overall mortality is increased in CD and in those with recurrent and persistent disease. Although there is improvement in mortality after effective treatment of CD, excess mortality persists. N/A, Not available; N/S, not significant. patients with more active disease and the associated morbidity. A limitation of this study, due to its retrospective nature, is that we did not have full data sets for the whole cohort. The literature as a whole has documented that mortality is increased in CD (6, 10, 30) (Table 3), and it has been suggested that with effective therapy long-term survival normalizes to that of the background population (7–9). In contrast, persistent/recurrent disease has been associated with a poor outcome, providing an evidence base for early intervention (3). These conclusions are drawn from a relatively small sample number, with small numbers of deaths, and median follow-up periods of under 10 yr. We report a greater than 3-fold excess mortality risk, with data suggestive of a reduction in mortality in the cured vs. the disease recurrence/persistent disease groups, although this difference does not reach statistical significance. With an SMR of 2.47 (95% CI, 0.80 –5.77), there may be an ongoing excess mortality even after cure of CD. We can speculate as to the cause of any persisting excess mortality, with candidates being cardiovascular risk factors and effects of hypopituitarism. Our findings are supported by those of Clayton et al. (13), who found an overall SMR of 4.8 (95% CI, 2.8 – 8.3), with an SMR for vascular disease of 13.8 (95% CI, 7.2–36.5), and an SMR for those in remission of 3.3 (95% CI, 1.7– 6.7). It is significant that our study and that of Clayton et al. (13) have median follow-up periods that are longer than most other studies in the literature at 10.9 and 15 yr,respectively. Our cohort demonstrated the hallmarks of effective therapy, with significant weight loss and improvement in blood pressure sustained on average across the cohort, although there was also evidence of possible permanent end-organ cardiovascular effects, with the significant proportion of patients having evidence of left ventricular hypertrophy and myocardial ischemia on electrocardiogram. Iatro- genic effects such as surgery and radiotherapy induced hypopituitarism, and overreplacement of glucocorticoid replacement could account for excess mortality. To address these issues, a large population-based study of mortality is required, with coordination between centers at a national or international level. Furthermore, longer-term prospective studies of the cardiovascular effects of CD are required to guide and develop future therapies. The identification of factors predictive of postoperative clinical outcomes is important both for counseling of patients and to guide further management. Previously suggested predictors of remission and cure of CD include age at diagnosis, presence of hypertension or diabetes (13), early and 6-wk postoperative serum cortisol (25, 31), early postoperative serum ACTH (32), ACTH response to CRH testing (33), postoperative metyrapone (34), desmopressin testing (35), low-dose dexamethasone testing (36), identification of tumor at surgery, and histology positive for a corticotropinoma (31, 37). This study confirmed previous findings of ACTH-positive histology as a predictor of cure. However, 60% of those with negative histology still achieved cure with single TSS, a finding that is now well recognized (38). Also of clinical importance is the identification of preoperative UFC as a prognostic marker. Recent data have suggested that positive preoperative MRI findings are associated with a higher chance of achieving initial remission (39). However, our data support previous findings that preoperative MRI findings are not predictive of long-term cure (40). The clinical utility of such prognostic indicators would be to incorporate them into a clinical outcome score to predict long-term remission or disease recurrence. In summary, this study comprises the United Kingdom’s largest cohort study of long-term outcomes and mortality in CD. The center’s initial and long-term remission rates are comparable to those seen in world-leading 1200 Hassan-Smith et al. Cushing’s Disease Postoperative Outcomes specialist centers and serve to underline the importance of an experienced surgeon working closely with dedicated endocrinologists in the treatment of CD. Our results suggest that despite significant improvements in BMI and blood pressure after TSS, there remains an excess mortality after effective treatment of CD. Further international consortium-based studies are required to refine outcome measures. Acknowledgments The authors thank Dr. D. Jenkins (Worcester Royal Hospital), Dr. J. J. Milles (Good Hope Hospital), Dr. C. Close (Taunton and Somerset Hospital), and Dr. P. M. Horrocks (Warwick Hospital) for providing follow-up data, and Dr. J. Hodson (University of Birmingham) for useful discussions. Address all correspondence and requests for reprints to: Prof. P. M. Stewart, Dean of Medicine, Centre for Endocrinology, Diabetes, and Metabolism, Second Floor Institute for Biomedical Research, School of Clinical and Experimental Medicine, University of Birmingham, Birmingham B15 2TT, United Kingdom. E-mail: [email protected]. Disclosure Summary: The authors have nothing to declare. References 1. Newell-Price J, Bertagna X, Grossman AB, Nieman LK 2006 Cushing’s syndrome. Lancet 367:1605–1617 2. Cushing H 1932 The basophil adenomas of the pituitary body and their clinical manifestations (pituitary basophilism). Bull Johns Hopkins Hosp 50:137 3. Sherlock M, Ayuk J, Tomlinson JW, Toogood AA, Aragon-Alonso A, Sheppard MC, Bates AS, Stewart PM 2010 Mortality in patients with pituitary disease. Endocr Rev 31:301–342 4. Fernandez-Rodriguez E, Stewart PM, Cooper MS 2009 The pituitary-adrenal axis and body composition. Pituitary 12:105–115 5. Plotz CM, Knowlton AI, Ragan C 1952 The natural history of Cushing’s syndrome. Am J Med 13:597– 614 6. Etxabe J, Vazquez JA 1994 Morbidity and mortality in Cushing’s disease: an epidemiological approach. Clin Endocrinol (Oxf) 40: 479 – 484 7. Swearingen B, Biller BM, Barker 2nd FG, Katznelson L, Grinspoon S, Klibanski A, Zervas NT 1999 Long-term mortality after transsphenoidal surgery for Cushing disease. Ann Intern Med 130:821– 824 8. Lindholm J, Juul S, Jørgensen JO, Astrup J, Bjerre P, Feldt-Rasmussen U, Hagen C, Jørgensen J, Kosteljanetz M, Kristensen L, Laurberg P, Schmidt K, Weeke J 2001 Incidence and late prognosis of Cushing’s syndrome: a population-based study. J Clin Endocrinol Metab 86:117–123 9. Hammer GD, Tyrrell JB, Lamborn KR, Applebury CB, Hannegan ET, Bell S, Rahl R, Lu A, Wilson CB 2004 Transsphenoidal microsurgery for Cushing’s disease: initial outcome and long-term results. J Clin Endocrinol Metab 89:6348 – 6357 10. Dekkers OM, Biermasz NR, Pereira AM, Roelfsema F, van Aken MO, Voormolen JH, Romijn JA 2007 Mortality in patients treated for Cushing’s disease is increased, compared with patients treated for nonfunctioning pituitary macroadenoma. J Clin Endocrinol Metab 92:976 –981 J Clin Endocrinol Metab, April 2012, 97(4):1194 –1201 11. Burch W 1983 A survey of results with transsphenoidal surgery in Cushing’s disease. N Engl J Med 308:103–104 12. Breslow NE, Day NE 1987 Statistical methods in cancer research. Volume II. The design and analysis of cohort studies. IARC Sci Publ 82:1– 406 13. Clayton RN, Raskauskiene D, Reulen RC, Jones PW 2011 Mortality and morbidity in Cushing’s disease over 50 years in Stoke-on-Trent, UK: audit and meta-analysis of literature. J Clin Endocrinol Metab 96:632– 642 14. Pecori Giraldi F, Moro M, Cavagnini F 2003 Gender-related differences in the presentation and course of Cushing’s disease. J Clin Endocrinol Metab 88:1554 –1558 15. Chaidarun SS, Alexander JM 1998 A tumor-specific truncated estrogen receptor splice variant enhances estrogen-stimulated gene expression. Mol Endocrinol 12:1355–1366 16. Muiesan ML, Lupia M, Salvetti M, Grigoletto C, Sonino N, Boscaro M, Rosei EA, Mantero F, Fallo F 2003 Left ventricular structural and functional characteristics in Cushing’s syndrome. J Am Coll Cardiol 41:2275–2279 17. Stewart PM, Walker BR, Holder G, O’Halloran D, Shackleton CH 1995 11-Hydroxysteroid dehydrogenase activity in Cushing’s syndrome: explaining the mineralocorticoid excess state of the ectopic adrenocorticotropin syndrome. J Clin Endocrinol Metab 80:3617– 3620 18. Van Zaane B, Nur E, Squizzato A, Dekkers OM, Twickler MT, Fliers E, Gerdes VE, Büller HR, Brandjes DP 2009 Hypercoagulable state in Cushing’s syndrome: a systematic review. J Clin Endocrinol Metab 94:2743–2750 19. Boscaro M, Arnaldi G 2009 Approach to the patient with possible Cushing’s syndrome. J Clin Endocrinol Metab 94:3121–3131 20. Lönn L, Kvist H, Ernest I, Sjöström L 1994 Changes in body composition and adipose tissue distribution after treatment of women with Cushing’s syndrome. Metabolism 43:1517–1522 21. Fallo F, Sonino N, Barzon L, Pistorello M, Pagotto U, Paoletta A, Boscaro M 1996 Effect of surgical treatment on hypertension in Cushing’s syndrome. Am J Hypertens 9:77– 80 22. Colao A, Pivonello R, Spiezia S, Faggiano A, Ferone D, Filippella M, Marzullo P, Cerbone G, Siciliani M, Lombardi G 1999 Persistence of increased cardiovascular risk in patients with Cushing’s disease after five years of successful cure. J Clin Endocrinol Metab 84:2664 – 2672 23. Atkinson AB, Kennedy A, Wiggam MI, McCance DR, Sheridan B 2005 Long-term remission rates after pituitary surgery for Cushing’s disease: the need for long-term surveillance. Clin Endocrinol (Oxf) 63:549 –559 24. Yap LB, Turner HE, Adams CB, Wass JA 2002 Undetectable postoperative cortisol does not always predict long-term remission in Cushing’s disease: a single centre audit. Clin Endocrinol (Oxf) 56: 25–31 25. Esposito F, Dusick JR, Cohan P, Moftakhar P, McArthur D, Wang C, Swerdloff RS, Kelly DF 2006 Clinical review: early morning cortisol levels as a predictor of remission after transsphenoidal surgery for Cushing’s disease. J Clin Endocrinol Metab 91:7–13 26. Pereira AM, van Aken MO, van Dulken H, Schutte PJ, Biermasz NR, Smit JW, Roelfsema F, Romijn JA 2003 Long-term predictive value of postsurgical cortisol concentrations for cure and risk of recurrence in Cushing’s disease. J Clin Endocrinol Metab 88:5858 –5864 27. Prevedello DM, Pouratian N, Sherman J, Jane Jr JA, Vance ML, Lopes MB, Laws Jr ER 2008 Management of Cushing’s disease: outcome in patients with microadenoma detected on pituitary magnetic resonance imaging. J Neurosurg 109:751–759 28. Cavagnini F, Scacchi M, Pecori Giraldi F 2008 Hypopituitarism in Cushing’s disease. J Endocrinol Invest 31:44 – 47 29. Rees DA, Hanna FW, Davies JS, Mills RG, Vafidis J, Scanlon MF 2002 Long-term follow-up results of transsphenoidal surgery for Cushing’s disease in a single centre using strict criteria for remission. Clin Endocrinol (Oxf) 56:541–551 30. Pikkarainen L, Sane T, Reunanen A 1999 The survival and well- J Clin Endocrinol Metab, April 2012, 97(4):1194 –1201 31. 32. 33. 34. 35. being of patients treated for Cushing’s syndrome. J Intern Med 245: 463– 468 Martino J, Acebes JJ, Montanya E, Masuet C, Brell M 2007 [Analysis of early prognostic factors for risk of treatment failure in Cushing’s disease treated by trans-sphenoidal pituitary surgery]. Med Clin (Barc) 128:330 –332 Flitsch J, Knappe UJ, Lüdecke DK 2003 The use of postoperative ACTH levels as a marker for successful transsphenoidal microsurgery in Cushing’s disease. Zentralbl Neurochir 64:6 –11 Nishizawa S, Oki Y, Ohta S, Yokota N, Yokoyama T, Uemura K 1999 What can predict postoperative “endocrinological cure” in Cushing’s disease? Neurosurgery 45:239 –244 Alwani RA, de Herder WW, van Aken MO, van den Berge JH, Delwel EJ, Dallenga AH, De Jong FH, Lamberts SW, van der Lely AJ, Feelders RA 2010 Biochemical predictors of outcome of pituitary surgery for Cushing’s disease. Neuroendocrinology 91:169 – 178 Losa M, Bianchi R, Barzaghi R, Giovanelli M, Mortini P 2009 Persistent adrenocorticotropin response to desmopressin in the early postoperative period predicts recurrence of Cushing’s disease. J Clin Endocrinol Metab 94:3322–3328 jcem.endojournals.org 1201 36. McCance DR, Gordon DS, Fannin TF, Hadden DR, Kennedy L, Sheridan B, Atkinson AB 1993 Assessment of endocrine function after transsphenoidal surgery for Cushing’s disease. Clin Endocrinol (Oxf) 38:79 – 86 37. Acebes JJ, Martino J, Masuet C, Montanya E, Soler J 2007 Early post-operative ACTH and cortisol as predictors of remission in Cushing’s disease. Acta Neurochir (Wien) 149:471– 477; discussion 477– 479 38. Pouratian N, Prevedello DM, Jagannathan J, Lopes MB, Vance ML, Laws Jr ER 2007 Outcomes and management of patients with Cushing’s disease without pathological confirmation of tumor resection after transsphenoidal surgery. J Clin Endocrinol Metab 92:3383– 3388 39. Ciric I, Zhao JC, Du H, Findling JW, Molitch ME, Weiss RE, Refetoff S, Kerr WD, Meyer J 2012 Transsphenoidal surgery for Cushing’s disease: experience with 136 patients. Neurosurgery 70:70 – 81 40. Salenave S, Gatta B, Pecheur S, San-Galli F, Visot A, Lasjaunias P, Roger P, Berge J, Young J, Tabarin A, Chanson P 2004 Pituitary magnetic resonance imaging findings do not influence surgical outcome in adrenocorticotropin-secreting microadenomas. J Clin Endocrinol Metab 89:3371–3376 Members have FREE online access to current endocrine Clinical Practice Guidelines. www.endo-society.org/guidelines