* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Retinal vessel photocoagulation: a quantitative comparison
Survey
Document related concepts
Transcript
418
Invest. Ophthalmol. Vis. Sci.
March 1981
Reports
rise, electroretinogram, extracellular potassium, subretinal space, pigment epithelium, photoreceptors
REFERENCES
1. Noell WK: Studies on the Electrophysiology and
Metabolism of the Retina. Randolph Field, Texas,
1953, USAF School of Aviation Medicine.
2. Marmor MF and Lurie M: Light-induced electrical
responses of the retinal pigment epithelium. In The
Retinal Pigment Epithelium, Marmor MF and Zinn
KM, editors. Cambridge, Mass., 1979, Harvard
University Press, pp. 226-244.
3. Skoog KO: The directly recorded standing potential
of the human eye. Acta Ophthalmol 53:120, 1975.
4. Tiuimer R, editor: Electro-oculography: its clinical
importance. Bibl Ophthalmol, No. 85, 1976.
5. Carr RE and Siegel IM: Clinical evaluation of retinal
pigment epithelial disorders. In The Retinal Pigment Epithelium, Marmor MF and Zinn KM,
editors. Cambridge, Mass., 1979, Harvard University Press, pp. 381-394.
6. Oakley B II and Green DG: Correlation of lightinduced changes in retinal extracellular potassium
concentration with c-wave of the electroretinogram.
J Neurophysiol 39:1117, 1976.
7. Oakley B II: Potassium and the photoreceptor dependent pigment epithelial hyperpolarization. J
Gen Physiol 70:405, 1977.
8. Steinberg RH, Schmidt R, and Brown KT: Intracellular responses to light from the cat pigment
epithelium: origin of the electroretinogram c-wave.
Nature 227:728, 1970.
9. Steinberg RH, Oakley B II, and Niemeyer G:
Light-evoked changes in [K + ] o in the retina of the
intact cat eye. J Neurophysiol 44:897, 1980.
10. Niemeyer G: Electrooculography in isolated, perfused mammalian eyes. Experientia 36:699, 1980.
11. Steinberg RH: Rod and cone contributions to
S-potentials from the cat retina. Vision Res 9:1319,
1969.
12. Schmidt R and Steinberg RH: Rod-dependent intracellular responses to light recorded from the
pigment epithelium of the cat retina. J Physiol
(Lond) 217:71, 1971.
13. Imaizumi K, Atsumi K, Takahashi F, and Yoshida G:
Experimental studies in ERG and EOG of the rabbit's eye. In The Clinical Value of Electroretinography (ISCERG Symposium, Ghent). Basel, 1968,
S. Karger, pp. 74-82.
14. Gouras P and Carr RE: Light-induced responses of
monkey retina before and after central retinal artery
interruption. INVEST OPHTHALMOL 4:310, 1965.
15. Thaler A and Heilig P: EOG and ERG components
in ischemic retinopathy. Ophthalmol Res 9:38,
1977.
16. Textorius O, Skoog KO, and Nilsson SEG: Studies
on acute and late states of experimental central retinal artery occlusion in the cynomolgus monkey. II.
Influence on the cyclic changes in the amplitude of
the c-wave of the ERG and in the standing potential
of the eye. Acta Ophthalmol 56:665, 1978.
17. Ponte F and Lodato G: Electro-oculographic investigations in central retinal vessel occlusions. (15th
ISCEV Symposium). Doc Ophthalmol Proc Ser
15:155, 1977.
Retinal vessel photocoagulation: a quantitative comparison of argon and krypton laser
effects.
MICHAEL WIEDER,
OLEG POMER-
ANTZEFF, AND JULIANNE SCHNEIDER.
Retinal arteries of owl monkeys were photocoagulated
with single exposures to argon laser green light (514 nm),
krypton laser green light (531 nm), and krypton laser
yellow light (568 nm). The distribution of damage along
the vessel in different retinal layers was characterized
geometrically after serial sectioning of the histopathologic
material. Krypton laser radiation (green and, to an even
greater extent, yellow) produced measurably greater effects on retinal vessels and adjacent structures than on
deeper retinal levels; argon laser radiation (green) produced greater effects on the pigment epithelium. Krypton
yellow produced the greatest total effect. The location of
damage to the retinal arteries and pigment epithelium
differed, with the peak of the damage around the arteries
being farther from the optic disc than was the peak of the
pigment epithelial damage.
The absoi-ption maxima for oxyhemoglobin (542
and 577 nm)1 are closer to the krypton laser green
(531 nm) and yellow (568 nm) wavelengths 2 than to
the argon laser green (514 nm) wavelength. We
compared the efficacy of the krypton and argon
laser wavelengths in photocoagulating retinal
vessels.
The krypton red line, which is effective in photocoagulating the outer retina and choroid, 3 " 6 was
not included in this study because of its poor absorption by hemoglobin. The blue argon wavelength (488 nm) was also excluded because of (1) its
preferential scattering by the ocular media, (2) its
absorption by xanthophyll in the macula and the
yellow pigment in older crystalline lenses, 7 " 9 and
(3) the relative susceptibility of the retina to photochemical damage from shorter wavelength radiation.10
Materials and methods. Fourteen owl monkeys,
each weighing 800 to 1200 gm, were anesthetized
with an intramuscular injection of sodium pentobarbital. The pupils were dilated with 10%
phenylephrine hydrochloride and 0.3% scopolamine hydrobromide, and a modified LO-VAC
0146-0404/81/030418+07$00.70/0 © 1981 Assoc. for Res. in Vis. and Ophthal., Inc.
Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933098/ on 06/16/2017
Volume 20
Number 3
Reports
419
A
STEP 1
STEP 2
STEP 3
0
50
100
150
RELATIVE POSITION ON VESSEL
200
{»t
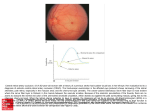
Fig. 1. A, Schematic summary of damage assessment. 1. Serial sectioning of specimens perpendicular to vessel axis. 2. Measurement of cross-sectional area of vacuolization around
vessel, vacuolization in photoreceptor layer, and vessel on all affected sections. 3. Plotting of
these three area measurements vs. their relative position along the vessel axis. (Papilla = optic
disc.) B and C, Fluorescein angiograms taken about 2 hr after treatment. B} Fluorescence of
three arterial (numbered J, 2, 3) and three control lesions about 1 min after injection. C, About
2 min after injection, staining of lesions J and 2 has almost disappeared. Histologic examination
showed pigment epithelium damage and vessel damage in lesion 3 but no pigment epithelium
damage in lesions 1 or 2.
contact lens (Medical Instrument Research Associates, Waltham, Mass.) was placed on the cornea.
A krypton ion laser (Model 170; Spectra Physics,
Mountain View, Calif.) and an argon laser photocoagulator (Model MF 2000; Medical Instrument Research Associates), operated at single
wavelengths and equipped with the same type of
delivery system, were used to make single lesions
on major retinal vessels at the posterior pole of the
monkey eyes. A spot size of 50 /xm, an exposure
time of 100 msec, and a power of 50 mW (monitored at the cornea) were kept constant. Lesions
were made with argon green light (514 nm), krypton green light (531 nm), and krypton yellow light
(568 nm). Burns made in areas of the retina devoid
of visible vessels served as controls and facilitated
orientation. Fluorescein angiography and monochromatic fundus photography were routinely per-
Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933098/ on 06/16/2017
420
Invest. Ophthalmol. Vis. Sci.
March 1981
Reports
B
C
Fig. 2. Sections of photocoagulated retina. (Hematoxylin and eosin; bar = 50 fxm.) A, On the
right is an example of damage at all retinal levels (produced by 531 nm krypton light). Unaffected vein is seen at left. B, Higher magnification of the damaged vessel in A. C, This bum
(produced by 568 nm krypton light) shows no appreciable pigment epithelium damage on any
section. D, Note fragmentation and necrosis in the vessel wall (produced by 568 nm krypton
light), Artery is empty owing to systemic perfusion.
Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933098/ on 06/16/2017
Volume 20
Number 3
Reports
A
B
Fig. 3. A and B, Two sections from one burn. B, Approximately 50 /Am downstream from A,
exhibits little damage in the outer retinal layers but much more destruction in and around the
artery than does A. (Hematoxylin and eosin; bar = 50 /xm.) C, Schematic longitudinal sections
through vascular burns to illustrate the influence of heat convection and obliquity of the laser
beam (solid line) on the location of the vessel damage. Arroics, Direction of the blood flow;
dashed tine, normal to the retina.
Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933098/ on 06/16/2017
421
422
Invest. Ophthalmol. Vis. Sci.
March 1981
Reports
i
D
6
10 -
E
D
DO
D X#
INAL DAMAGE
3
t—
•
n
X
x
I
x
x
•
•
x
X
m
10*-
INNER
LU
105-
D
••
D
D
X
XX
10^
105
106
OUTER RETINAL DAMAGE (urn'
Q KR 568 nm
•
KR 531 nm
10
10 6
VOLUME OF INNER VACUOLES
X AR 514 nm
Fig. 4. A, Distribution of vacuolization. Each data point represents one burn. Inner retinal
damage is defined as the total volume of vacuolization around the vessel; outer retinal damage,
as the volume of vacuolization at the level of the photo receptors. Volume of vacuoles was
computed from vacuole area on each section. Burns in shaded area had extensive damage both
around the vessel and at the level of the photoreceptors. B, Relationship between reduction of
vessel lumen and inner retinal vacuolization. The vessel lumen decreases as the size of the
vacuoles around the vessel increases.
formed. Approximately 3 hr after treatment, the
animals underwent systemic perfusion with a solution of 1% glutaraldehyde and 2.5% formalin in
0.2M phosphate buffer; the eyes were then enucleated and fixed for 3 days in 10% formalin. Serial
6 /Am sections cut perpendicular to the vessel axis
were prepared for light microscopy (Fig. 1). The
cross-sectional areas of (1) the vessel, (2) the vacuoles around the vessel, and (3) the vacuoles in the
photo receptor layer were measured on 50 histologic sections with a microscope stage micrometer and an electronic digitizing table.
Results. Lesions produced by light of all three
colors had a similar histologic appearance; they
varied only in the extent of the damage to the
different retinal tissues (Fig. 2). Arterial walls
showed some loss of structure at the site of the
greatest laser beam interaction, but holes were
never observed. Vacuole formation around the
vessel and reduction in vessel diameter were both
greatest in the center of the lesion and smallest at
its periphery. Vacuoles similar to those around
vessels characterized the damage to the receptor
layers. The pigment epithelium was detached and
partially dispersed. The extent of damage to the
outer nuclear layer appeared to be related to the
amount of damage to the vessel and/or the pigment epithelium. The choriocapillaris appeared to
be compressed locally by the vacuoles in the receptor layer, but deeper choroidal structures were
not affected.
In Fig. 1, A, the areas of the vessel, the outer
vacuole, and the inner vacuole measured on various sections are plotted against the relative position of the sections along the vessel axis.
Fluorescein angiography showed leakage only
in burns with pigment epithelium defects (Fig. 1,
B and C). If the lesion was confined to the artery
and the adjacent structures, only the vessel wall
stained, and this staining disappeared in late
phases of the dye transit. Thus fluorescein dye did
not penetrate into the vacuoles that surrounded
the vessel (Fig. 1, B).
In all experiments, the peak of damage around
the arteries was always more peripheral (i.e.,
farther from the optic disc) than that of the damage
at the pigment epithelium (Fig. 3). This peripheral
shift of the vascular damage varied between 10 and
90 /xin at all wavelengths and was generally larger
than the shift resulting from the oblique incidence
Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933098/ on 06/16/2017
Volume 20
Number 3
of the laser beam. To assess the possible influence
of heat convection by the moving blood, we coagulated retinal veins and found that the inner retinal
damage was much less shifted toward the periphery than it was in the case of arteries; in some
burns, the damage was even shifted toward the
optic disc (Fig. 3, C).
The measurements of the volume of affected tissue permitted a quantitative comparison of the effects of the wavelengths investigated. Both wavelengths of krypton laser light tended to produce
more vacuolization around the vessel and less in
the outer retinal layers than did the argon green.
Krypton yellow produced the greatest total effect.
Fig. 4, A, shows the relationship between inner
and outer retinal damage. Any reduction of the
vessel lumen was directly related to the size of the
inner vacuoles: the vessel lumen decreased as the
size of the vacuoles around the vessel increased
(Fig. 4, B).
Discussion. Various factors affect the distribution of damage in a vascular lesion produced by
photocoagulation. The damage to the outer retinal
layer varies with the vessel diameter; such
damage is more extensive when smaller vessels
are treated. With small vessels, less energy is absorbed by the blood and more is transmitted to the
outer retina. In our experiments, arterial diameters ranged from 45 to 100 (xm, with an average of
about 65 /xm. The distribution of vessel diameters
for the three wavelengths investigated was not
significantly different.
Furthermore, owing to variations in power,
working distance, and astigmatism introduced by
the contact lens, retinal energy density may vary
by a factor of 2 in either direction even under ideal
conditions.11 Since the computed energy density
in our experiments was approximately 255 J/cm2
(ocular transmission not taken into account), actual
energy density probably varied between 170 and
340 J/cm2, which caused a relatively large variation in the distribution of damage. It is reasonable
to assume, however, that these variations affected
the results with all three laser wavelengths similarly.
In some burns, extensive damage was present at
both the inner and the outer retinal level (shaded
area, Fig. 4, A). In these burns, the energy density appears to have been higher than average because of a combination of the factors mentioned
above. These results do not exhibit any significant
wavelength dependency. With increasing power,
however, not only does the difference between
the argon and krypton wavelengths become less
Reports
423
appreciable but also the range of clinically safe
applications is exceeded.
In the remaining lesions (unshaded area, Fig. 4,
A), which represent the average and low range of
the energy variation, the damage pattern varied
with wavelength. Krypton green and yellow light
produced measurably greater effects on the arteries and adjacent structures than on deeper retinal levels; argon green light produced greater effects on the pigment epithelium.
Our findings also suggest that the location of the
damage in and around the vessel is determined by
the angle of the coagulating beam incidence as
well as by the direction (and probably rate) of the
blood flow.
We conclude that in many cases of diabetic
retinopathy, branch-vein occlusion, sickle cell
anemia, and other retinal vascular conditions
where direct coagulation of retinal vessels is appropriate, treatment with the krypton green and
yellow wavelengths should be more successful
than conventional argon laser treatment.
We thank Ms. Sandra J. Spinks for her illustrative and
photographic contributions.
From the Department of Retina Research, Eye Research Institute of Retina Foundation, Boston, Mass.
This work was supported by grant EY02725 from the
National Eye Institute, National Institutes of Health,
and by the Massachusetts Lions Eye Research Fund,
Inc. This paper was presented in part at the meeting of
the Association for Research in Vision and Ophthalmology, May 1980, Orlando, Fla. Submitted for publication
July 14, 1980. Reprint requests: Library, Eye Research
Institute of Retina Foundation, 20 Stamford St., Boston,
Mass. 02114.
Keywords: krypton laser, argon laser, retinal vessel photocoagulation, owl monkeys, histopathology
REFERENCES
1. Van Assendelft OW: Spectrophotometry of haemoglobin derivatives. Springfield, 111., 1970, Charles C
Thomas, Publisher.
2. L'Esperanee FA Jr: Clinical photocoagulation with
the krypton laser. Arch Ophthalmol 87:693, 1972.
3. Schulenburg WE, Hamilton AM, and Blach RK: A
comparative study of argon laser and krypton laser
in the treatment of diabetic optic disc neovascularisation. Br J Ophthalmol 63:412, 1979.
4. Marshall J and Bird AC: A comparative histopathological study of argon and krypton laser irradiations
of the human retina. Br J Ophthalmol 63:657, 1979.
5. Bird AC and Grey RHB: Photocoagulation of disciform macular lesions with krypton laser. Br J
Ophthalmol 63:669, 1979.
Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933098/ on 06/16/2017
424
Invest. Ophthalmol. Vis. Sci.
March 1981
Reports
6. L'Esperance FA Jr: The ocular histopathologic effect
of krypton and argon laser radiation. Am J Ophthalmol 68:263, 1969.
7. Wald G: Human vision and the spectrum. Science
101:653, 1945.
8. Boettner EA and Wolter JR: Transmission of the
ocular media. INVEST OPHTHALMOL 1:776, 1962.
9. Pomerantzeff O, Kaneko H, Donovan RH, Schepens CL, and McMeel JW: Effect of the ocular-
media on the main wavelengths of argon laser emission. INVEST OPHTHALMOL 15:70, 1976.
10. Ham WT Jr, Mueller HA, Ruffolo JJ Jr, and Clarke
AM: Sensitivity of the retina to radiation damage as
a function of wavelength. Photochem Photobiol
29:735, 1979.
11. Pomerantzeff O and Schepens CL: Variation of energy density in argon laser photocoagulation. Arch
Ophthalmol 93:1033, 1975.
Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933098/ on 06/16/2017