* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download 26 slides
Survey
Document related concepts
Transcript
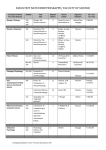
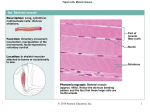
MONDAY, SEPTEMBER TH 26 This week’s agenda: Monday – Tissue and Skin Lecture Tuesday – Debrief skin lab and UV lab Wednesday – Burns Case Study Thursday – Review/Tutorials Friday – Tissues and Skin Exam Body Tissues Tissues Groups of cells with similar structure and function Four primary types: 1. 2. 3. 4. © 2015 Pearson Education, Inc. Epithelial tissue (epithelium) Connective tissue Muscle tissue Nervous tissue 1. Epithelial Tissues! © 2015 Pearson Education, Inc. Epithelial Tissues Locations: Body coverings Body linings Glandular tissue Functions: Protection Absorption Filtration Secretion © 2015 Pearson Education, Inc. Epithelium Characteristics Cells fit closely together and often form sheets The apical surface is the free surface of the tissue The lower surface of the epithelium rests on a basement membrane Avascular (no blood supply) Regenerate easily if well nourished © 2015 Pearson Education, Inc. Figure 3.17a Classification and functions of epithelia. Apical surface Basal surface Simple Apical surface Basal surface Stratified (a) Classification based on number of cell layers © 2015 Pearson Education, Inc. Classification of Epithelia Shape of cells Squamous Flattened, like fish scales Cuboidal Cube-shaped, like dice Columnar Column-like © 2015 Pearson Education, Inc. Figure 3.17b Classification and functions of epithelia. Squamous Cuboidal Columnar (b) Classification based on cell shape © 2015 Pearson Education, Inc. Figure 3.17c Classification and functions of epithelia. Number of layers One layer: simple epithelial tissues More than one layer: stratified epithelial tissues Squamous Diffusion and filtration Secretion in serous membranes Protection Cuboidal Secretion and absorption; ciliated types propel mucus or reproductive cells Secretion and absorption; ciliated types propel mucus or reproductive cells Protection; these tissue types are rare in humans Cell shape Columnar Transitional Protection; stretching to accommodate distension of urinary structures (c) Function of epithelial tissue related to tissue type © 2015 Pearson Education, Inc. Simple Epithelia Simple squamous Single layer of flat cells Location—usually forms membranes Lines air sacs of the lungs Forms walls of capillaries Forms serous membranes (serosae) that line and cover organs in ventral cavity Functions in diffusion, filtration, or secretion in membranes © 2015 Pearson Education, Inc. Figure 3.18a Types of epithelia and their common locations in the body. Air sacs of lungs Nucleus of squamous epithelial cell Basement membrane (a) Diagram: Simple squamous © 2015 Pearson Education, Inc. Nuclei of squamous epithelial cells Photomicrograph: Simple squamous epithelium forming part of the alveolar (air sac) walls (275×). Simple Epithelia Simple cuboidal Single layer of cube-like cells Locations: Common in glands and their ducts Forms walls of kidney tubules Covers the surface of ovaries Functions in secretion and absorption; ciliated types propel mucus or reproductive cells © 2015 Pearson Education, Inc. Figure 3.18b Types of epithelia and their common locations in the body. Nucleus of simple cuboidal epithelial cell Basement membrane (b) Diagram: Simple cuboidal © 2015 Pearson Education, Inc. Simple cuboidal epithelial cells Basement membrane Connective tissue Photomicrograph: Simple cuboidal epithelium in kidney tubules (250×). Simple Epithelia Simple columnar Single layer of tall cells Goblet cells secrete mucus Location: Lines digestive tract from stomach to anus Mucous membranes (mucosae) line body cavities opening to the exterior Functions in secretion and absorption; ciliated types propel mucus or reproductive cells © 2015 Pearson Education, Inc. Figure 3.18c Types of epithelia and their common locations in the body. Nucleus of simple columnar epithelial cell Basement membrane (c) Diagram: Simple columnar © 2015 Pearson Education, Inc. Mucus of a goblet cell Simple columnar epithelial cells Basement membrane Photomicrograph: Simple columnar epithelium of the small intestine (575×). Simple Epithelia Pseudostratified columnar All cells rest on a basement membrane Single layer, but some cells are shorter than others giving a false (pseudo) impression of stratification Location: Respiratory tract, where it is ciliated and known as pseudostratified ciliated columnar epithelium Functions in absorption or secretion © 2015 Pearson Education, Inc. Figure 3.18d Types of epithelia and their common locations in the body. Cilia Pseudostratified epithelial layer Pseudostratified epithelial layer Basement membrane Basement membrane Connective tissue (d) Diagram: Pseudostratified (ciliated) columnar © 2015 Pearson Education, Inc. Photomicrograph: Pseudostratified ciliated columnar epithelium lining the human trachea (560×). Stratified Epithelia Stratified squamous Named for cells present at the free (apical) surface, which are flattened Functions as a protective covering where friction is common Locations—lining of the: Skin (outer portion) Mouth Esophagus © 2015 Pearson Education, Inc. Figure 3.18e Types of epithelia and their common locations in the body. Nuclei Stratified squamous epithelium Basement membrane (e) Diagram: Stratified squamous © 2015 Pearson Education, Inc. Stratified squamous epithelium Basement membrane Connective Photomicrograph: tissue Stratified squamous epithelium lining of the esophagus (140×). Stratified Epithelia Stratified cuboidal—two layers of cuboidal cells; functions in protection Stratified columnar—surface cells are columnar, and cells underneath vary in size and shape; functions in protection Stratified cuboidal and columnar Rare in human body Found mainly in ducts of large glands © 2015 Pearson Education, Inc. Stratified Epithelia Transitional epithelium Composed of modified stratified squamous epithelium Shape of cells depends upon the amount of stretching Functions in stretching and the ability to return to normal shape Locations: urinary system organs © 2015 Pearson Education, Inc. Figure 3.18f Types of epithelia and their common locations in the body. Basement membrane Transitional epithelium Basement membrane Transitional epithelium Connective tissue (f) Diagram: Transitional © 2015 Pearson Education, Inc. Photomicrograph: Transitional epithelium lining of the bladder, relaxed state (270×); surface rounded cells flatten and elongate when the bladder fills with urine. Glandular Epithelium Gland One or more cells responsible for secreting a particular product Secretions contain protein molecules in an aqueous (water-based) fluid Secretion is an active process © 2015 Pearson Education, Inc. Glandular Epithelium Two major gland types Endocrine gland Ductless; secretions diffuse into blood vessels All secretions are hormones Examples include thyroid, adrenals, and pituitary © 2015 Pearson Education, Inc. Glandular Epithelium Two major gland types Exocrine gland Secretions empty through ducts to the epithelial surface Include sweat and oil glands, liver, and pancreas Includes both internal and external glands © 2015 Pearson Education, Inc. 2. Connective Tissue! © 2015 Pearson Education, Inc. Connective Tissue Found everywhere in the body Includes the most abundant and widely distributed tissues Functions: Provides protection Binds body tissues together Supports the body © 2015 Pearson Education, Inc. Connective Tissue Characteristics Variations in blood supply Some tissue types are well vascularized Some have a poor blood supply or are avascular Extracellular matrix Nonliving material that surrounds living cells © 2015 Pearson Education, Inc. Extracellular Matrix Two main elements 1. Ground substance—mostly water along with adhesion proteins and polysaccharide molecules 2. Fibers Produced by the cells Three types: 1. Collagen (white) fibers 2. Elastic (yellow) fibers 3. Reticular fibers (a type of collagen) © 2015 Pearson Education, Inc. Connective Tissue Types From most rigid to softest, or most fluid: Bone Cartilage Dense connective tissue Loose connective tissue Blood © 2015 Pearson Education, Inc. Connective Tissue Types Bone (osseous tissue) Composed of: Osteocytes (bone cells) sitting in lacunae (cavities) Hard matrix of calcium salts Large numbers of collagen fibers Functions to protect and support the body © 2015 Pearson Education, Inc. Figure 3.19a Connective tissues and their common body locations. Bone cells in lacunae Central canal Lacunae Lamella (a) Diagram: Bone © 2015 Pearson Education, Inc. Photomicrograph: Cross-sectional view of ground bone (165×) Connective Tissue Types Cartilage Less hard and more flexible than bone Found in only a few places in the body Chondrocyte (cartilage cell) is the major cell type © 2015 Pearson Education, Inc. Connective Tissue Types Hyaline cartilage Hyaline cartilage is the most widespread type of cartilage Composed of abundant collagen fibers and a rubbery matrix Locations: Larynx Entire fetal skeleton prior to birth Epiphyseal plates Functions as a more flexible skeletal element than bone © 2015 Pearson Education, Inc. Figure 3.19b Connective tissues and their common body locations. Chondrocyte (cartilage cell) Chondrocyte in lacuna Lacunae Matrix (b) Diagram: Hyaline cartilage © 2015 Pearson Education, Inc. Photomicrograph: Hyaline cartilage from the trachea (400×) Connective Tissue Types Elastic cartilage (not pictured) Provides elasticity Location: Supports the external ear Fibrocartilage Highly compressible Location: Forms cushionlike discs between vertebrae of the spinal column © 2015 Pearson Education, Inc. Figure 3.19c Connective tissues and their common body locations. Chondrocytes in lacunae Chondrocytes in lacunae Collagen fibers © 2015 Pearson Education, Inc. Collagen fiber (c) Diagram: Fibrocartilage Photomicrograph: Fibrocartilage of an intervertebral disc (150×) Connective Tissue Types Dense connective tissue (dense fibrous tissue) Main matrix element is collagen fiber Fibroblasts are cells that make fibers Locations: Tendons—attach skeletal muscle to bone Ligaments—attach bone to bone at joints and are more elastic than tendons Dermis—lower layers of the skin © 2015 Pearson Education, Inc. Figure 3.19d Connective tissues and their common body locations. Ligament Tendon Collagen fibers Collagen fibers Nuclei of fibroblasts Nuclei of fibroblasts (d) Diagram: Dense fibrous © 2015 Pearson Education, Inc. Photomicrograph: Dense fibrous connective tissue from a tendon (475×) Connective Tissue Types Loose connective tissue types Areolar tissue Most widely distributed connective tissue Soft, pliable tissue like “cobwebs” Functions as a universal packing tissue and “glue” to hold organs in place Layer of areolar tissue called lamina propria underlies all membranes All fiber types form a loose network Can soak up excess fluid (causes edema) © 2015 Pearson Education, Inc. Figure 3.19e Connective tissues and their common body locations. Mucosa epithelium Lamina propria Elastic fibers Collagen fibers Fibroblast nuclei Fibers of matrix Nuclei of fibroblasts (e) Diagram: Areolar © 2015 Pearson Education, Inc. Photomicrograph: Areolar connective tissue, a soft packaging tissue of the body (270×) Connective Tissue Types Loose connective tissue types Adipose tissue Matrix is an areolar tissue in which fat globules predominate Many cells contain large lipid deposits with nucleus to one side (signet ring cells) Functions Insulates the body Protects some organs Serves as a site of fuel storage © 2015 Pearson Education, Inc. Figure 3.19f Connective tissues and their common body locations. Nuclei of fat cells Vacuole containing fat droplet Nuclei of fat cells Vacuole containing fat droplet (f) Diagram: Adipose © 2015 Pearson Education, Inc. Photomicrograph: Adipose tissue from the subcutaneous layer beneath the skin (570×) Connective Tissue Types Loose connective tissue types Reticular connective tissue Delicate network of interwoven fibers with reticular cells (like fibroblasts) Locations: Forms stroma (internal framework) of organs, such as these lymphoid organs: Lymph nodes Spleen Bone marrow © 2015 Pearson Education, Inc. Figure 3.19g Connective tissues and their common body locations. Spleen White blood cell (lymphocyte) Reticular cell Blood cell Reticular fibers Reticular fibers (g) Diagram: Reticular © 2015 Pearson Education, Inc. Photomicrograph: Dark-staining network of reticular connective tissue (400×) Connective Tissue Types Blood (vascular tissue) Blood cells surrounded by fluid matrix known as blood plasma Soluble fibers are visible only during clotting Functions as the transport vehicle for the cardiovascular system, carrying: Nutrients Wastes Respiratory gases © 2015 Pearson Education, Inc. Figure 3.19h Connective tissues and their common body locations. Blood cells in capillary Neutrophil (white blood cell) Red blood cells White blood cell Red blood cells (h) Diagram: Blood © 2015 Pearson Education, Inc. Monocyte (white blood cell) Photomicrograph: Smear of human blood (1290×) 3. Muscular Tissue! Muscle Tissue Function is to contract, or shorten, to produce movement Three types: 1. Skeletal muscle 2. Cardiac muscle 3. Smooth muscle © 2015 Pearson Education, Inc. Muscle Tissue Types Skeletal muscle Voluntarily (consciously) controlled Attached to the skeleton and pull on bones or skin Produces gross body movements or facial expressions Characteristics of skeletal muscle cells Striations (stripes) Multinucleate (more than one nucleus) Long, cylindrical shape © 2015 Pearson Education, Inc. Figure 3.20a Type of muscle tissue and their common locations in the body. Nuclei Part of muscle fiber (a) Diagram: Skeletal muscle © 2015 Pearson Education, Inc. Photomicrograph: Skeletal muscle (195×) Muscle Tissue Types Cardiac muscle Involuntarily controlled Found only in the heart Pumps blood through blood vessels Characteristics of cardiac muscle cells Striations Uninucleate, short, branching cells Intercalated discs contain gap junctions to connect cells together © 2015 Pearson Education, Inc. Figure 3.20b Type of muscle tissue and their common locations in the body. Intercalated discs Nucleus (b) Diagram: Cardiac muscle © 2015 Pearson Education, Inc. Photomicrograph: Cardiac muscle (475×) Muscle Tissue Types Smooth (visceral) muscle Involuntarily controlled Found in walls of hollow organs such as stomach, uterus, and blood vessels Peristalsis, a wavelike activity, is a typical activity Characteristics of smooth muscle cells No visible striations Uninucleate Spindle-shaped cells © 2015 Pearson Education, Inc. Figure 3.20c Type of muscle tissue and their common locations in the body. Smooth muscle cell Nuclei (c) Diagram: Smooth muscle © 2015 Pearson Education, Inc. Photomicrograph: Sheet of smooth muscle (285×) 3. Nervous Tissue! © 2015 Pearson Education, Inc. Nervous Tissue Composed of neurons and nerve support cells Function is to receive and conduct electrochemical impulses to and from body parts Irritability Conductivity Support cells called neuroglia insulate, protect, and support neurons © 2015 Pearson Education, Inc. Figure 3.21 Nervous tissue. Brain Nuclei of supporting cells Spinal cord Nuclei of supporting cells Cell body of neuron Neuron processes © 2015 Pearson Education, Inc. Cell body of neuron Neuron processes Diagram: Nervous tissue Photomicrograph: Neurons (320×) Figure 3.22 Summary of the major functions and body locations of the four tissue types: epithelial, connective, muscle, and nervous tissues. Nervous tissue: Internal communication • Brain, spinal cord, and nerves Muscle tissue: Contracts to cause movement • Muscles attached to bones (skeletal) • Muscles of heart (cardiac) • Muscles of walls of hollow organs (smooth) Epithelial tissue: Forms boundaries between different environments, protects, secretes, absorbs, filters • Lining of GI tract organs and other hollow organs • Skin surface (epidermis) Connective tissue: Supports, protects, binds other tissues together • Bones • Tendons • Fat and other soft padding tissue © 2015 Pearson Education, Inc. Tissue Repair! Tissue Repair (Wound Healing) Tissue repair (wound healing) occurs in two ways: 1. Regeneration Replacement of destroyed tissue by the same kind of cells 2. Fibrosis Repair by dense (fibrous) connective tissue (scar tissue) © 2015 Pearson Education, Inc. Tissue Repair (Wound Healing) Whether regeneration or fibrosis occurs depends on: 1. Type of tissue damaged 2. Severity of the injury Clean cuts (incisions) heal more successfully than ragged tears of the tissue © 2015 Pearson Education, Inc. Events in Tissue Repair Inflammation Capillaries become very permeable Clotting proteins migrate into the area from the bloodstream A clot walls off the injured area Granulation tissue forms Growth of new capillaries Phagocytes dispose of blood clot and fibroblasts Rebuild collagen fibers © 2015 Pearson Education, Inc. Events in Tissue Repair Regeneration of surface epithelium Scab detaches Whether scar is visible or invisible depends on severity of wound © 2015 Pearson Education, Inc. Regeneration of Tissues Tissues that regenerate easily Epithelial tissue (skin and mucous membranes) Fibrous connective tissues and bone Tissues that regenerate poorly Skeletal muscle Tissues that are replaced largely with scar tissue Cardiac muscle Nervous tissue within the brain and spinal cord © 2015 Pearson Education, Inc. Tissue Development! © 2015 Pearson Education, Inc. Development Aspects of Cells and Tissues Growth through cell division continues through puberty Cell populations exposed to friction (such as epithelium) replace lost cells throughout life Connective tissue remains mitotic and forms repair (scar) tissue With some exceptions, muscle tissue becomes amitotic by the end of puberty Nervous tissue becomes amitotic shortly after birth. © 2015 Pearson Education, Inc. Developmental Aspects of Cells and Tissues Injury can severely handicap amitotic tissues The cause of aging is unknown, but chemical and physical insults, as well as genetic programming, have been proposed as possible causes © 2015 Pearson Education, Inc. Developmental Aspects of Cells and Tissues Neoplasms, both benign and cancerous, represent abnormal cell masses in which normal controls on cell division are not working Hyperplasia (increase in size) of a tissue or organ may occur when tissue is strongly stimulated or irritated Atrophy (decrease in size) of a tissue or organ occurs when the organ is no longer stimulated normally © 2015 Pearson Education, Inc. Membranes! © 2015 Pearson Education, Inc. Body Membranes Functions of body membranes Cover body surfaces Line body cavities Form protective sheets around organs Classified according to tissue types © 2015 Pearson Education, Inc. Classification of Body Membranes Epithelial membranes Cutaneous membranes Mucous membranes Serous membranes Connective tissue membranes Synovial membranes © 2015 Pearson Education, Inc. Cutaneous Membrane Cutaneous membrane skin Dry membrane Outermost protective boundary Superficial epidermis is composed of keratinized stratified squamous epithelium Underlying dermis is mostly dense (fibrous) connective tissue © 2015 Pearson Education, Inc. Figure 4.1a Classes of epithelial membranes. Cutaneous membrane (skin) (a) Cutaneous membrane (the skin) covers the body surface. Mucous Membranes Surface epithelium type depends on site Stratified squamous epithelium (mouth, esophagus) Simple columnar epithelium (rest of digestive tract) Underlying loose connective tissue (lamina propria) Lines all body cavities that open to the exterior body surface Moist membranes adapted for absorption or secretion © 2015 Pearson Education, Inc. Figure 4.1b Classes of epithelial membranes. Mucosa of nasal cavity Mucosa of mouth Esophagus lining Mucosa of lung bronchi (b) Mucous membranes line body cavities open to the exterior. Serous Membranes (Serosa) Surface is a layer of simple squamous epithelium Underlying layer is a thin layer of areolar connective tissue Lines open body cavities that are closed to the exterior of the body Serous membranes occur in pairs separated by serous fluid Visceral layer covers the outside of the organ Parietal layer lines a portion of the wall of ventral body cavity © 2015 Pearson Education, Inc. Figure 4.1d Classes of epithelial membranes. Outer balloon wall (comparable to parietal serosa) Air (comparable to serous cavity) Inner balloon wall (comparable to visceral serosa) (d) A fist thrust into a flaccid balloon demonstrates the relationship between the parietal and visceral serous membrane layers. Serous Membranes Specific serous membranes Peritoneum Abdominal cavity Pleura Around the lungs Pericardium Around the heart © 2015 Pearson Education, Inc. Figure 4.1c Classes of epithelial membranes. Parietal pleura Visceral pleura Parietal peritoneum Visceral peritoneum Parietal pericardium Visceral pericardium (c) Serous membranes line body cavities closed to the exterior. Connective Tissue Membrane Synovial membrane Connective tissue only Lines fibrous capsules surrounding joints Lines bursae Lines tendon sheaths Secretes a lubricating fluid © 2015 Pearson Education, Inc. Figure 4.2 A typical synovial joint. Ligament Joint cavity (contains synovial fluid) Articular (hyaline) cartilage Fibrous layer Articular Synovial capsule membrane Integumentary System! Integumentary System Integumentary system includes: Skin (cutaneous membrane) Skin derivatives Sweat glands Oil glands Hair Nails © 2015 Pearson Education, Inc. Skin (Integument) Functions Protects deeper tissues from: Mechanical damage (bumps) Chemical damage (acids and bases) Bacterial damage Ultraviolet radiation (sunlight) Thermal damage (heat or cold) Desiccation (drying out) Keratin protects the skin from water loss © 2015 Pearson Education, Inc. Skin Functions Aids in loss or retention of body heat as controlled by the nervous system Aids in excretion of urea and uric acid Synthesizes vitamin D Cutaneous sensory receptors detect touch, temperature, pressure, and pain © 2015 Pearson Education, Inc. Table 4.1 Functions of the Integumentary System (1 of 2). Table 4.1 Functions of the Integumentary System (2 of 2). Skin Structure Epidermis—outer layer Stratified squamous epithelium Cornified or keratinized (hardened by keratin) to prevent water loss Avascular Most cells are keratinocytes Dermis Dense connective tissue © 2015 Pearson Education, Inc. Figure 4.3 Skin structure. Hair shaft Dermal papillae Epidermis Papillary layer Dermis Pore Appendages of skin • Eccrine sweat gland • Arrector pili muscle • Sebaceous (oil) gland • Hair follicle • Hair root Reticular layer Hypodermis (subcutaneous tissue) Nervous structures • Sensory nerve fiber • Lamellar corpuscle • Hair follicle receptor (root hair plexus) Cutaneous vascular plexus Adipose tissue Skin Structure Subcutaneous tissue (hypodermis) is deep to dermis Not technically part of the skin Anchors skin to underlying organs Composed mostly of adipose tissue Serves as a shock absorber and insulates deeper tissues © 2015 Pearson Education, Inc. Layers of the Epidermis The epidermis is composed of up to five layers The epidermis is avascular Most of the cells in the epidermis are keratinocytes Keratin, a fibrous protein, makes the epidermis tough The layers are covered, next, from deepest to most superficial © 2015 Pearson Education, Inc. Dermis Two layers: 1. Papillary layer (upper dermal region) Projections called dermal papillae Some contain capillary loops Others house pain receptors (free nerve endings) and touch receptors Fingerprints are identifying films of sweat 2. Reticular layer (deepest skin layer) Blood vessels Sweat and oil glands Deep pressure receptors (lamellar corpuscles) © 2015 Pearson Education, Inc. Dermis Overall dermis structure Collagen and elastic fibers located throughout the dermis Collagen fibers give skin its toughness Elastic fibers give skin elasticity Blood vessels play a role in body temperature regulation Nerve supply sends messages to the central nervous system © 2015 Pearson Education, Inc. Figure 4.5 Light micrograph of the two regions of the dermis (100×). Epidermis Papillary layer Dermis Reticular layer Skin Color Three pigments contribute to skin color: 1. Melanin Yellow, reddish brown, or black pigments 2. Carotene Orange-yellow pigment from some vegetables 3. Hemoglobin Red coloring from blood cells in dermal capillaries Oxygen content determines the extent of red coloring © 2015 Pearson Education, Inc. Melanin Pigment (melanin) produced by melanocytes Color is yellow to brown to black Melanocytes are mostly in the stratum basale Melanin accumulates in membrane-bound granules called melanosomes Amount of melanin produced depends upon genetics and exposure to sunlight © 2015 Pearson Education, Inc. Alterations in Skin Color Redness (erythema)—due to embarrassment, inflammation, hypertension, fever, or allergy Pallor (blanching)—due to emotional stress (such as fear), anemia, low blood pressure, impaired blood flow to an area Jaundice (yellowing)—liver disorder Bruises (black and blue marks)—hematomas © 2015 Pearson Education, Inc. Appendages of the Skin Cutaneous glands are all exocrine glands Sebaceous glands Sweat glands Hair Hair follicles Nails © 2015 Pearson Education, Inc. Figure 4.3 Skin structure. Hair shaft Dermal papillae Epidermis Papillary layer Dermis Pore Appendages of skin • Eccrine sweat gland • Arrector pili muscle • Sebaceous (oil) gland • Hair follicle • Hair root Reticular layer Hypodermis (subcutaneous tissue) Nervous structures • Sensory nerve fiber • Lamellar corpuscle • Hair follicle receptor (root hair plexus) Cutaneous vascular plexus Adipose tissue Appendages of the Skin Sebaceous (oil) glands Produce sebum (oil) Lubricant for skin Prevents brittle hair Kills bacteria Most have ducts that empty into hair follicles; others open directly onto skin surface Glands are activated at puberty © 2015 Pearson Education, Inc. Figure 4.7a Cutaneous glands. Sweat pore Eccrine gland Sebaceous gland Sebaceous gland duct Dermal connective tissue Hair in hair follicle Secretory cells (a) Photomicrograph of a sectioned sebaceous gland (100×) Appendages of the Skin Sweat (sudoriferous) glands Produce sweat Widely distributed in skin © 2015 Pearson Education, Inc. Appendages of the Skin Two types of sudoriferous glands 1. Eccrine glands Open via duct to pore on skin surface Produce sweat © 2015 Pearson Education, Inc. Appendages of the Skin Sweat: Composition Mostly water Salts and vitamin C Some metabolic waste Fatty acids and proteins (apocrine only) Function Helps dissipate excess heat Excretes waste products Acidic nature inhibits bacteria growth Odor is from associated bacteria © 2015 Pearson Education, Inc. Figure 4.7b Cutaneous glands. Sweat pore Eccrine gland Sebaceous gland Dermal connective tissue Eccrine gland duct Secretory cells (b) Photomicrograph of a sectioned eccrine gland (205×) Appendages of the Skin Two types of sudoriferous glands 2. Apocrine glands Ducts empty into hair follicles Begin to function at puberty Release sweat that also contains fatty acids and proteins (milky or yellowish color) © 2015 Pearson Education, Inc. Appendages of the Skin Hair Produced by hair follicle Root is enclosed in the follicle Shaft projects from the surface of the scalp or skin Consists of hard keratinized epithelial cells Melanocytes provide pigment for hair color Hair grows in the matrix of the hair bulb in stratum basale © 2015 Pearson Education, Inc. Appendages of the Skin Associated hair structures Hair follicle Dermal and epidermal sheath surround hair root Arrector pili muscle Smooth muscle Pulls hairs upright when person is cold or frightened Sebaceous gland Sudoriferous gland © 2015 Pearson Education, Inc. Figure 4.10 Structure of a nail. Lunule Lateral nail fold (a) Free edge of nail (b) Body Cuticle Root of nail of Proximal Nail nail nail fold matrix Nail bed Bone of fingertip Burns! Skin Homeostatic Imbalances Burns Tissue damage and cell death caused by heat, electricity, UV radiation, or chemicals Associated dangers Dehydration Electrolyte imbalance Circulatory shock Result in loss of body fluids and invasion of bacteria © 2015 Pearson Education, Inc. Rule of Nines Way to determine the extent of burns Body is divided into 11 areas for quick estimation Each area represents about 9 percent of total body surface area The area surrounding the genitals (the perineum) represents 1 percent of body surface area © 2015 Pearson Education, Inc. Figure 4.11a Burns. Totals Anterior and posterior head and neck, 9% 41/2% Anterior and posterior upper limbs, 18% Anterior and posterior 41/2% trunk, 36% 41/2% Anterior trunk, 18% Perineum, 1% 9% 9% Anterior and posterior lower limbs, 36% 100% (a) Severity of Burns First-degree burns (partial-thickness burn) Only epidermis is damaged Skin is red and swollen Second-degree burns (partial-thickness burn) Epidermis and upper dermis are damaged Skin is red with blisters Third-degree burns (full-thickness burn) Destroys entire skin layer; burned area is painless Requires skin grafts Burn is gray-white or black © 2015 Pearson Education, Inc. Figure 4.11b Burns. Burns of increasing severity, from top to bottom: first-degree, second-degree, third-degree. (b) Critical Burns Burns are considered critical if Over 25 percent of body has second-degree burns Over 10 percent of the body has third-degree burns There are third-degree burns of the face, hands, or feet © 2015 Pearson Education, Inc. Homeostatic Imbalances! © 2015 Pearson Education, Inc. Skin Homeostatic Imbalances Infections Athlete’s foot (tinea pedis) Caused by fungal infection Boils and carbuncles Caused by bacterial infection Cold sores Caused by virus © 2015 Pearson Education, Inc. Skin Homeostatic Imbalances Infections and allergies Contact dermatitis Exposures cause allergic reaction Impetigo Caused by bacterial infection Psoriasis Cause is unknown Triggered by trauma, infection, stress © 2015 Pearson Education, Inc. Figure 4.12 Cutaneous lesions. (a) Cold sores (b) Impetigo (c) Psoriasis Skin Cancer Cancer—abnormal cell mass Classified two ways 1. Benign Does not spread (encapsulated) 2. Malignant Metastasizes (moves) to other parts of the body Skin cancer is the most common type of cancer © 2015 Pearson Education, Inc. © 2015 Pearson Education, Inc. Skin Cancer Types Basal cell carcinoma Least malignant Most common type Arises from stratum basale © 2015 Pearson Education, Inc. Figure 4.13a Photographs of skin cancers. (a) Basal cell carcinoma Skin Cancer Types Squamous cell carcinoma Metastasizes to lymph nodes if not removed Early removal allows a good chance of cure Believed to be sun-induced Arises from stratum spinosum © 2015 Pearson Education, Inc. Figure 4.13b Photographs of skin cancers. (b) Squamous cell carcinoma Skin Cancer Types Malignant melanoma Most deadly of skin cancers Cancer of melanocytes Metastasizes rapidly to lymph and blood vessels Detection uses ABCD rule © 2015 Pearson Education, Inc. ABCD Rule A Asymmetry Two sides of pigmented mole do not match B Border irregularity Borders of mole are not smooth C Color Different colors in pigmented area D Diameter Spot is larger than 6 mm in diameter E = Evolving Changing over time, especially after age 18 © 2015 Pearson Education, Inc. Figure 4.13c Photographs of skin cancers. (c) Melanoma Developmental Aspects of Skin In youth, skin is thick, resilient, and well hydrated With aging, skin loses elasticity and thins Skin cancer is a major threat to skin exposed to excessive sunlight Balding and/or graying occurs with aging; both are genetically determined; other factors that may contribute include drugs and emotional stress © 2015 Pearson Education, Inc. HOMEWORK Make sure all of your assignments are up to date! Thursday is the last day to get any homework checked off, but the sooner the better! This week Tuesday – Debrief skin lab and UV lab Wednesday – Burns Case Study Thursday – Review/Tutorials Friday – Tissues and Skin Exam