* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Differential diagnosis of broad complex tachycardia
Survey
Document related concepts
Transcript
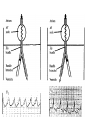
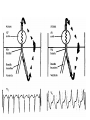
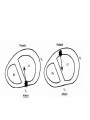
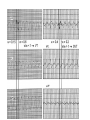
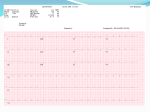
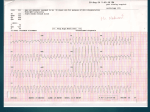
Differential diagnosis of broad complex tachycardia Dr.Deepak Raju Definitions • Wide Complex Tachycardia(WCT)-a rhythem with QRS duration ≥ 120 ms and heart rate > 100 bt/min • Ventricular tachycardia-a WCT originating below the level of His bundle • SVT-tachycardia dependent on participation of structures at or above the level of His bundle • LBBB morphology-QRS complex duration ≥ 120 ms with a predominantly negative terminal deflection in lead V1 • RBBB morphology-QRS complex duration ≥ 120 ms with a predominantly positive terminal deflection in V1 • LBBB&RBBB morphology denote morphological appearance of QRS complexresult from direct myocardial activation Causes of regular WCT • Ventricular tachycardia– Most common cause of WCT in general population(80%) – 95% of WCT in pts with structural heart disease • Supraventricular tachycardia with abnormal interventricular conduction(15% to 30% of WCT) – SVT with BBB aberration; • fixed(present during normal rhythem) • functional(present only during WCT) • Functional aberration results from sudden change in cycle length when parts of the His-Purkinje system are partially or wholly inexcitable • Functional RBBB commoner because of longer refractoriness • Linking phenomenon -Functional BBB may persist for several successive impulses because the bundle branch that is blocked antegradely may be activated trans-septally via its contralateral counterpart • AV reentrant tachycardia (AVRT) – Orthodromic AVRT – antegrade conduction over the AV node and retrograde conduction through accessory pathway.WCT occurs in aberrant conduction,either rate related or preexisting – Antidromic AVRT – antegrade conduction over the accessory pathway and retrograde conduction over the AV node result in WCT • Pre-excited tachycardia- SVT with ventricular activation occurs predominantly via accessory pathway – Mahaim pathway mediated tachycardia • antegrade conduction through mahaim(nodoventricular) pathway and retrograde through AV node • Tachycardia with LBBB morphology and left axis • episodes of pre-excited tachycardia without exhibiting pre-excitation during sinus rhythm • Wide QRS complex tachycardia occur because absence of retrograde conduction over accessory pathway – SVT with a wide complex due to abnormal muscle spread of impulse • RBBB in pts undergone rt.ventriculotomy • LBBB in pts with DCM – SVT with wide complex due to drug or electrolyte induced changes • Ι A, Ι C,amiodarone,tricyclic antidepressants • Hyperkalemia – Ventricular paced rhythems • LBBB with left axis Causes of irregular WCT • Any irregular supraventricular rhythem(AF,EAT or atrial flutter with varying conduction) with aberrant ventricular conduction • AF with ventricular preexcitation-if the ventricular rate in AF is >220/min or shortest R-R int is <250 msec bypass tract should be considered • Polymorphic VT • Torsade de pointes SVT Vs VT- history and physical examination • History of prior heart disease favour VT – Prior MI,angina or CCF – Each factor -95% PPV for VT • H/o similar episodes for >3 yrs-SVT more likely • First episode of WCT after MI-VT more likely • Older age grp>35 yrs-VT more likely • Findings of AV dissociation-favour VT – Cannon a waves – Variable intensity of S1 • AV dissociation can be brought out by carotid sinus massage,adenosine • Termination in response to CSM, adenosine,valsalva-suggest SVT ECG features-QRS morphology • SVT with aberrancy-QRS complex must be compatible with some form of BBB or FB • If not,diagnosis by default is VT Specific morphologies of QRS • V1 with RBBB – SVT with aberration• initial portion of QRS not affected by RBBB aberration • Triphasic complex (rabbit ear sign)with rt peak taller • r S R (r-septal activation,S-activation of LV,R-activation of RV) – pattern s/o VT • • • • Monophasic R Broad(>30 msec)initial R qR Triphasic complex with lt.peak taller V6 with RBBB • SVT with aberration – qRs,Rs,RS(R/S>1) – Delayed RV activation produces a small S wave in V6 • pattern s/o VT – rS,QS,Qrs,QR – RS with R/S<1 – Large S due to RV component of ventricular activation+depolarisation of some portion of LV as activation propagates away from V6 V1 -LBBB • SVT with aberrancy – r S, QS – Rapid initial forces(narrow r&rapid smooth descent to nadir of S) – Initial forces are relatively preserved • VT – – – – – – Broad R/deep S QS with a slow descent to S wave nadir Initial R >30 msec s/o VT,wider the R greater likelihood Notch in downstroke of S Interval from onset of QRS to nadir of S >60 msec Taller R during WCT than sinus rhythem V6 -LBBB • SVT with aberrancy – Lacks initial Q wave – Monophasic R or RR’ • VT – QR,QS,QrS,Rr’ – Patterns consistent with SVT may be seen QRS complex duration • 69% of VT had QRS duration >140 ms-Wellens et al • VT probable when QRS duration >140 ms with RBBB morphology ,>160 ms with LBBB morphology • QRS duration > 160 msec-a strong predictor of VT regardless of bundle--branch block morphology • QRS duration < 140 msec does not exclude VT QRS axis • Mean QRS axis in the normal range favors SVT with aberrancy • Right superior axis -90 to ± 180° suggests VT • Axis shift during WCT of > 40° favors VT • LBBB morphology with rt axis deviationalmost always due to VT • RBBB with a normal axis-uncommon in VT Concordant pattern • Concordant precordial R wave progression pattern(all precordial leads predominantly positive or predominantly negative) • High specificity for VT (90%) • Low sensitivity(observed in only 20%of VTs) • Exception –antidromic AVRT w/ a left posterior accessory pathway-positive concordance • Concordance of the limb leads-predominantly neg QRS complex in limb leads s/o VT A V dissociation • Most useful ECG feature • Complete AV dissociation seen in 20 to 50 % of VT(sensitivity .2 to .5,specificity 1) • 15 to 20% of VT has 2nd degree V A block • Lewis leads-p waves seen better with arm leads at various levels on opposite sides of sternum • Psudo p waves-contour of terminal portion of QRS may resmble p-inspect simultaneous recording in other leads • Variation in QRS complex altitude during WCTdue to summation of p wave on the QRS complex –clue to presence of AVD • 30% of VT has 1:1 retrograde conduction-CSP or adenosine used to block retrograde conduction to diagnose VT • When the atrial rate<ventricular rate-s/o VT • Atrial rate>ventricular rate s/o SVT with conduction block Evidences of AV dissociation • Fusion beat – when one impulse originating from the ventricle and a second supraventricular impulse simultaneously activate the ventricular myocardium – Morphology intermediate b/w sinus beat&pure ventricular complex • Capture beat – normal conduction momentarily captured control of ventricular activation from the VT focus Onset of tachycardia • Episode initiated by a premature p wave-SVT • If begins with a QRS-can be ventricular or supraventricular • If first wide QRS preceded by a sinus p with a shorter PR int.-usually VT • Presence of Q waves during a WCT –s/o old MI-s/o VT • Patients with post MI VT maintain Q wave in the same territory as in NR • DCM-Q waves during VT,which was not there in sinus rhythem • Psudo Q –retrograde p deforming the onset of QRS • QRS complex during WCT narrower than NR – In presence of BBB during NR,a WCT with a narrower complex indicate VT • Contralateral BBB in NR and in WCT s/o VT • QRS alternans– alternate beat variation in QRS amplitude>0.1 mV – occurs with equal frequency in WCT due to VT &SVT,but grter no.of leads show this (7 Vs 4) in SVT with aberrancy(Kremer et al;Am J Cardiol) • Multiple WCT configurations– More than one QRS configuration during a WCT – VT more likely – 51% of pts with VT,8% with SVT in one series Importance of sinus rhythem ECG • Differentiation between VT and SVT with antegrade conduction over accessory pathway • Aberrancy is rate related or pre existing • Presence of premature complexes in sinus rhythem • Old MI • QT interval • ECG clues to any other structural heart disease • rule out ECG artifacts which may be misdiagnosed as WCT VT Vs preexcited tachycardia • Characteristics specific for VT – Predominantly negative QRS complexes in V4-V6 – Presence of a QR complex in one or more leads V2-V6 – More QRS complex than P • 75% sensitivity&100%specificity for VT(Stierer et al) Criteria for diagnosis • Griffith et al;1991 – QRS morphology in V 1&aVF,change in QRS axis grter than 40 from normal rhythem&h/o MI – Predictive accuracy greater than 90% in detecting VT • Kremer et al ;1988 – Precordial concordance,NW axis,monophasic R in lead V1 Brugada criteria • Brugada et al analysed 554 cases of WC tachycardias with a new algorithm(circulation 1991) • Sensitivity of the four consecutive steps was 98.7%&specificity was 96.5% • Four criteria for VT sequentially evaluated • If any satisfied diagnosis of VT made • If none are fulfilled-SVT Evaluation of RS complexes Measurement of RS interval New aVR algorithm • Vereckei et al;Heart Rhythm 2008 • 483 WCT (351 VT, 112 SVT, 20 preexcited tachycardia)analysed • Greater sensitivity for VT diagnosis than Brugada algorithm(96.5% vs 89.2%, P .001) • Greater specificity for diagnosing SVT compared with Brugada criteria • Reasons for using a VR – Duriing SVT with aberrancy,initial septal activation and main ventricular activation directed away from lead aVR, so negative complex – Exception-inferior MI-initial r wave (rS complex) during NSR or SVT – Initial dominant R suggest VT typically originating from inferior or apical region • VT originating from other sites-show a slow initial upward vector f/b main vector pointing downward and creates a predominantly negative QRS in lead aVR. • Exception-VT originating from the most basal septum or free wall • Vi/Vt (ventricular activation velocity ratio) – Vi –initial ventricular activation velocity – Vt –terminal ventricular activation velocity – Both measured by the excursion (in mV) ECG during initial (Vi) and terminal (Vt) 40 msec of QRS complex Thank you