* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Case Study: CABG - Heidi Schultz OHSU Dietetic Intern
Survey
Document related concepts
Transcript
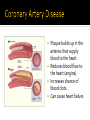
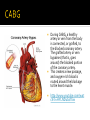
Heidi Schultz Oregon Health & Science University 4/19/2010 83 year-old Vietnamese female. Admitted to the hospital on 2/17/10 with chest pain. Pt was inpatient for a total of 22 days. 18 days in CICU. This case study will cover her 22 day inpatient stay. Pt seen at another hospital 10/2009. Dx with severe 3-vessel coronary artery disease. Pt seen at this hospital early February for pneumonia; treated and discharged. On 2/17/10 (Day 1), Pt was admitted to the ER at another hospital. Complaints of chest pain. Tx to this hospital for surgery. Colonoscopy CABGx3 Respiratory distress/pneumonia/vented Nutrition consulted beginning Day 9 TF Metabolic acidosis Stabilized Oral PO Education provided Consult with JCAHO PT IS A VEGETARIAN Typical intake: Breakfast: ▪ 2 slices of bread or cereal; coffee with 4 bags of sugar. Lunch: ▪ Homemade Vietnamese soup with veggies. Dinner: ▪ Stir-fry vegetables with tofu and white rice or noodles. Snacks/desserts: ▪ Pt likes chocolate and cookies. Height: 60” (152 cm) Weight: 142 lb (64.5 kg) Weight Change: No significant change BMI: 27.8 (overweight) IBW: 100 lbs (45.5kg) %IBW: 142% Glucose/Endocrine Profile: • Glucose, casual: 133 mg/dL high (Ref 60-99) Electrolyte and Renal Profile: • Lytes: WDL • Troponin: negative for MI Nutritional Anemia Profile: ▪ ▪ ▪ ▪ HGB: 8.3 g/dL low (Ref 11.7-15.7) Hematocrit: 24% intitially low; 33% after two units low (Ref 34.9-46.9) Iron 27 ug/dL low (Ref 40-150) Ferritin WDL Vital Signs: Blood Pressure 125/70; WDL HR 80 and regular; WDL Respiratory rate 18; WDL Personal History Pt is an 83 year-old female. Vietnamese. Moved to US from Vietnam in 1982. Non-English speaking. Social History Pt lives at home with her son. Pt is a non-smoker and non-drinker. Pt does not speak English. Pt uses a walker and is not physically active. Decreased exercise tolerance. Code Status: Full Code Medical History Coronary Artery Disease Thalassemia Pneumonia Asthma DM2 Hypercholesterolemia HTN C-section Purpose Drug Considerations Antihypertensive Diovan 160 mg can also ↓ Hgb, Hct Platelet Aggregation Inhibitor for ↓ risk of MI Plavix 75 mg Oral Hypoglycemic/ Sulfonylurea Glipizide LX 10 mg Anti-hyperlipidemic Simvastatin 40 mg Anti-hyperglycemic Metformin 1000 mg Anti-diabetic Actos 45 mg Asthma Singulair 10 mg Osteoperosis Actonel 150 mg Anti-asthma (as needed) Albuterol can also ↑ TG, LDL Can ↑ glucose; angina Plaque builds up in the arteries that supply blood to the heart. Reduces blood flow to the heart (angina). Increases chance of blood clots. Can cause heart failure. An inherited blood disorder: Mediterraneans/Asians/African Americans. Abnormal hemoglobin. Hemoglobinopathy Thalassemia: ▪ Underproduction of globin protein (either alpha or beta chain). Sickle-cell anemia: ▪ Abnormality of globin protein (mutant of beta globin chain). Thalassemia Minor: • Have small red blood cells but few symptoms. • Typically no specific treatment needed. Thalassemia Major: • Babies may be stillborn or develop severe anemia in their first year of life. • Severe Thalassemia can lead to heart failure and early death. Regular blood transfusions often required. • Require chelation therapy to remove excess iron from the body. • Too much iron can damage the brain, heart, liver and endocrine system. • Folate supplements. Pt admitted to another hospital with chest pain. Pt tx to this hospital for CAD surgery. MD unsure that surgery is indicated. Symptoms may be related to anemia. GI evaluation requested. Pt underwent colonoscopy. 5 polyps removed. Otherwise normal colonoscopy. No obvious source of long-term GI blood loss. Scheduled CABG. During CABG, a healthy artery or vein from the body is connected, or grafted, to the blocked coronary artery. The grafted artery or vein bypasses (that is, goes around) the blocked portion of the coronary artery. This creates a new passage, and oxygen-rich blood is routed around the blockage to the heart muscle. http://www.youtube.com/wat ch?v=HYLNDuGsTEw Pt underwent a Triple Coronary Artery Bypass Graft. Pt tolerated surgery well. Pt experienced respiratory distress and was intubated. Sedated with Propofol. Fat emulsion. 1.1 kcal/cc. Rate of Propofol was 4 cc/hour. Adds about 11 grams of fat every 24 hours. TGs were checked: 103 mg/dL (Ref <149). Respiratory Distress w/Hypoxemia Renal Insufficiency ▪ Creatinine 2 mg/dL high (Ref .5 to 1.1) ▪ GFR 34 mL/min/1.73m2 low (Ref 75) Metabolic Acidosis ▪ pH ABG 7.30 low (Ref 7.35-7.45) Hypotension ▪ BP 98/43 low Possible Health Care Associated Pneumonia (HCAP) ▪ Procalcitonin 1.17 ng/mL high (Rev .05 - .50) Received 2 units PRBCs in past 24 hours PreTransfusion PostTransfusion Reference Range RBC 3.08 10^ 12/L WDL 3.8 to 5.20 Hgb 8.6 g/dL 11.1 g/dL 11.7 to 15.7 Hct 25.3% 32.4% 24.9% to 46.9% Nutrition received a Consult for TF: NG Tube Energy needs - Penn State equation used 1500 kcal/day Protein 1.2 g/kg (78 grams/day) Fluid: 1500 ml Formula: Jevity 1.2 (house) high fiber Goal rate of 55 ml/hr Provide 1584 kcal 1069 ml free water from TF; 300 ml from flushes (total 1369 ml) Will get additional free water from IVF Nutrition Summary: Day 9 pt experienced respiratory distress resulting in reintubation; NG placed today to meet nutritional needs. Pt was ordering and eating adequate amount of kcal here prior to intubation as per records. PES: Oral intake inadequate related to intubation as evidenced by NPO. Plan is short-term enteral feeding with goal of attaining adequate kcal and protein. Purpose Drug Administration Wound healing Vitamin C 1,000 mg PO BID Electrolytes Klor-Con M20 PO BID Antihypertensive Captopril 6.25mg PO q8H Platelet agg inhibitor Plavix 75 mg PO daily Antihypertensive Lopressor 25 mg PO BID Antibiotic Bactroban Nasal Topical BID Antibiotic Cipro 400 mg 200 ml IV daily Antibiotic Azactam .5 gm 25 ml IV q 6 H Antisecretory Protonix 40 mg 10 ml IV daily Hyperglycemia Reg Insulin 150 units 1.5 mL IV qBag Sedation Propofol 1,000 mg 100 ml IV demand Sympathomimetic Dobutamine 500 mg 40 ml IV qBag Pt still vented. Pt still hypotensive (109/55) with chronic metabolic acidosis. Pt taken off Propofol and put on Versed. HCAP with fever (101.3 F) persisting. Acute renal insufficiency improved. Respiratory – stable vent settings. Started TF yesterday. Labs noted – Complete Metabolic Panel: BUN 40 mg/dL high Creatinine 1.35 mg/dL high Protein, Total 5.7 g/dL low Pre-albumin 11 low Albumin 2.6 g/dL low Lytes WDL Pt hemodynamically stable and off pressors. MD changed TF to 2-Cal Concentrated. Pt needs 2 Cal HN Prosource Combined Calories 1500 1200 60 1320 Rate Na 25 ml/hr Na 25 ml/hr Protein 78 g 50 g 15 g 80 g 427 ml free; 300 ml flushes. na 427 ml free; 300 ml flushes. Free Water 1500 ml Nutrition Summary: Day 13; pt has been on TF for 4 days while intubated in CCU; did not reach goal volume (55 ml/hr) on Jevity 1.2; yesterday MD changed to two-cal for minimal fluid; RD added 2 packets of Prosource protein per day to increase protein intake. This enables the current TF order to meet 88% of est Cal needs; 102% est protein needs. Nut problem: Ongoing Pt tolerating concentrated formula well and is at goal rate. Labs noted – Nutrition Panel: Glucose 140 high BUN 46 high Phosphorus 1.7 low Albumin 3.1 low Lytes WDL Nutrition Summary: Pt intubated and receiving adequate nutrition and protein with TF and 2 Prosource per day. Pt tolerating TF at goal rate. Pt continues with anemia most likely due to Thalassemia. Nut Problem: Ongoing. NPO x7 days. Diet order changed to mechanical soft with cyclic TF at night. Energy needs calculated with Mifflin: REE = 1019 x 1.2 Activity Factor x 1.2 Stress Factor = 1467 Compared to 25 kcal/kg = 1612 kcal Anticipating PO intake to be inconsistent at first, use higher range of: ▪ 1600 kcal for energy needs ▪ Protein 1 g/kg = 65 grams per day ▪ Fluids per MD Cyclic TF Order Goal 1600 kcal/day (1000 kcal from TF; 600 kcal from oral PO) Formula: 2 cal HN concentrated; 40 ml/hour for 12 hours at night Provides: 480 ml (960 kcal); 40 g protein; 336 ml water; 4 free water flushes of 160 ml each (976 ml total water). Pt still on fluid restriction. Nutrition Summary: As per nurse, pt is to continue with TF during evening only and consume mechanical soft during the day. Recommend continue with 2-Cal Concentrated at rate of 40 ml/hr for 12 hours. Will order calorie count as well. Nutrition Problem: Ongoing; pt extubated on Day 17 of stay; Day 9 of TF. Oral intake continues to be inadequate. TF discontinued (11 days TF). NG removed. Pt ambulating. Diet order changed to general diet w/2000 ml fluid restriction. Consult received for nutrition education for low-fat/low-sodium, heart-healthy diet. RD on duty did not perform nut ed due to confusion about diet order. Pt transferred to the floor. Nut Summary: Pt discontinued TF 3/8; appetite for oral PO is improving. Pt is ambulating and hemodynamically stable. Pt consumed 900 kcal and 108 carb for lunch yesterday. Will perform low-fat, low-cholesterol nut ed today. Nut Problem: Improved. Pt consuming adequate PO with >1200 kcal intake yesterday and continued adequate intake today. Provided Heart-Healthy Eating handouts in both English and Vietnamese. Took typical dietary intake. Discussed TLC diet: Limit sat and trans fats. Limit cholesterol. Increase omega-3s. Increase fiber. Continue eating plant based/soy foods. Referred pt to outpatient RD visit for diabetes education. PT IS A VEGETARIAN Typical intake: Breakfast: ▪ 2 slices of bread or cereal; coffee with 4 bags of sugar. Lunch: ▪ Homemade Vietnamese soup with veggies. Dinner: ▪ Stir-fry vegetables with tofu and white rice or noodles. Snacks/desserts: ▪ Pt likes chocolate and cookies. Why was TF changed? How have we accommodated the patient’s language barrier and cultural preferences? How do we decide which patients to assess? Pt was discharged from the hospital on 3/11/10. Oral diet. Nutrition problem improved. No Albumin/Pre-Albumin. Pt transferred home. PT and OT through Home Health. In the past month, the pt has been readmitted twice due to non-nutritional complications/complaints. National Heart Lung and Blood Institute: http://www.nhlbi.nih.gov/health/dci/Diseases/Cad/CAD_WhatIs.html; Accessed 4/8/10 American Dietetic Association: www.eatright.org; Accessed 4/8/10 National Institute of Health: Medline Plus http://www.nlm.nih.gov/medlineplus/ency/article/000587.htm; Accessed 4/8/10 Charles JC, Heilman RL. Metabolic Acidosis. Hospital Physician, March 2005: 37-42. Van Den Berghe G, Wouters P, Weekers F, et al. Intensive insulin therapy in critically ill patients. N Engl J Med. 2001: 345:1359-1367. Miller J, Kee. Keeping your patient hemodynamically stable. Nursing. May 2007: 37(5) 36-41. Niedert KC. Position of the ADA: Liberalization of the Diet Perscription Improves Quality of Life for Older Adults in Long-term Care. Journal of the American Dietetic Association (Position Paper). 2005: 1955-1965. Kollef MH, Bedient TJ, Isakow W, Witt CA. The Washington Manual of Critical Care. Published by Lippincott Williams & Wilkins 2008. Pronsky ZM. Food Medication Interactions; 15th Edition. Pagana KD, Pagana TJ. Mosby’s Diagnostic and Laboratory Test Reference; 9th Edition. Published by Elsevier Inc. 2009. Hemila H, Louhiala P. Vitamin C for preventing and treating pneumonia. Cochrane Database of Systematic Reviews 2007, Issue 1. Art No.CD005532.DOI:10.1002/14651858. CD005532.pub2.