* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Health care facility design, construction and renovation
Traveler's diarrhea wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Childhood immunizations in the United States wikipedia , lookup
Transmission (medicine) wikipedia , lookup
Sociality and disease transmission wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
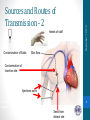
Sarcocystis wikipedia , lookup
Gastroenteritis wikipedia , lookup
Carbapenem-resistant enterobacteriaceae wikipedia , lookup
Marburg virus disease wikipedia , lookup
Common cold wikipedia , lookup
Hepatitis C wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Hepatitis B wikipedia , lookup
Schistosomiasis wikipedia , lookup
Anaerobic infection wikipedia , lookup
Urinary tract infection wikipedia , lookup
Neonatal infection wikipedia , lookup
Prevention of Intravascular Device-Associated Infections 1. Describe the relevance and impact of intravascular Device-Associated infections. 2. Identify infection sources and routes of transmission for intravascular infections. 3. Outline the main recommendations to prevent those infections. December 1, 2013 Learning objectives 2 • 30 minutes December 1, 2013 Time involved 3 • Intravenous (IV) infusions among the commonest invasive procedures (peripheral or central) • IV central catheters are the main source of bloodstream infection (CLABSI) • Infections associated: December 1, 2013 Introduction • Cellulitis, abscess, thrombophlebitis, bacteraemia, endocarditis • Principles to prevent infections similar for central and peripheral catheters 4 • Strict asepsis for insertion and maintenance of catheters • Insertion site dry and protected with a sterile dressing • No touch technique • IV line secure without movements • Closed system • Inspection of the insertion site daily • Remove the catheters as soon as possible • No reuse of catheters intended for single use • Healthcare personnel educated and their knowledge assessed • Alternative routes for hydration or parenteral therapy December 1, 2013 Key points 5 December 1, 2013 Sites of possible contamination of intravascular infusions 6 • Sources of contamination intrinsic or extrinsic • Most microorganisms from the patient’s skin flora • Contamination of device hub also a source of infection • S. aureus - 60 to 90% of infections December 1, 2013 Sources and Routes of Transmission - 1 7 Hands of staff Contamination of fluids Skin flora Flora del paciente December 1, 2013 Sources and Routes of Transmission - 2 Contamination of insertion site Injections ports Contaminación de las conexiones 8 Seed from distant site Main source of infection Prevention Infusion fluids Monitor sterilisation Ensure fluid is pyrogen free. Avoid damage to containers Inspect containers Addition of medications Aseptic technique Sterile medications Carry out procedures in the pharmacy. Sterile device for accessing the system. Single-dose vials If multi-dose vials have to be used: Refrigerate after opening Wipe diaphragm with 70% isopropanol Warmingcontainer Ensure no contamination Dry warming systems are preferred. December 1, 2013 Prevention of Infections - 1 9 Main source of infection Prevention Insertion of catheter Thorough hand disinfection and sterile gloves Thoroughly disinfect the skin insertion site. Catheter site Cover with sterile dressing Remove catheter if signs of infection occur. Inspect site every 24 hours. Change dressing only when necessary. Do not use antimicrobial ointments. Injection ports Clean with 70% isopropanol and allow to dry Close ports that are not needed with sterile stopcocks. Changing of infusion set Replace no more frequently than 72 hours (blood and lipids every 24 hours). Thorough hand disinfection Use good aseptic technique. December 1, 2013 Prevention of Infections - 2 10 • Routine changes of peripheral IV catheters not required • In adults recommendation to change every 72-96 hours to reduce phlebitis • In children should not be replaced routinely December 1, 2013 General Comments - 1 • Routine replacement of central catheters not necessary • Central catheters used only when indicated • Non-essential catheters removed • Risk of infection increases with length of catheterisation 11 • Teflon or polyurethane catheters associated with fewer infections • Steel needles same rate of infection as Teflon catheters December 1, 2013 General Comments - 2 • Steel needles complicated by infiltration of IV fluids • Well-trained staff to set up and maintain infusions • Masks, caps, and gowns not necessary for insertion of peripheral IV lines • Use of non-sterile barriers will protect the operator if blood exposure likely 12 • • • • • • Place arm on a clean sheet or towel Hand hygiene (alcohol hand rub or antiseptic soap) Dry hands on a paper or unused linen towel Hand hygiene (gloves does not replace it) Not remove hair (if necessary clip, avoid shaving) Disinfect skin site, apply for 30 seconds and allow drying December 1, 2013 Protocol for peripheral infusions - 1 • 0.5% chlorhexidine-alcohol, 2% tincture of iodine, 10% alcoholic povidone-iodine, or isopropanol). • Chlorhexidine products should not be used in children younger than 2 months 13 • Cannula preferably in an upper limb • Secure sterile dressing • Transparent dressings allow inspection of the site December 1, 2013 Protocol for peripheral infusions - 2 • Secure cannula, label with insertion date • Assess need for catheter every 24 hours • Inspect catheter daily • Avoid cut downs, especially in the leg • Cannulae and sets must be sterile 14 • Selection of site • Higher infections for jugular and femoral • Maximum barriers • Disinfect skin with 2% chlorhexidine/alcohol • Change transparent dressings once a week or if soiled, loose, or damp, gauze every two days • Replace sets not for blood or lipids no more than 72 hours December 1, 2013 Additional guidelines for central catheters 15 • Systemic antibiotic prophylaxis • Topical use of antimicrobial ointments • Routine replacement of central venous catheters • Routine use of antibiotic locks for central venous catheters • Routine use of in-line filters December 1, 2013 Measures that should not be considered as part of a general prevention policy: 16 • Marschall J, et al. Strategies to prevent central lineassociated bloodstream infections in acute care hospitals. Infect Control Hosp Epidemiol 2008; 29(suppl. 1): S22-S30. http://www.jstor.org/stable/10.1086/591059 • Marchaim D, et al. Epidemiology of bacteraemia episodes in a single center: increase in Gram-negative isolates, antibiotics resistance, and patient’s age. Eur J Clin Microbiol Infect Dis 2008; 27:1045-51. • Standards for infusion therapy. Royal College of Nursing, 2010. http://www.rcn.org.uk/__data/assets/pdf_file/0005/785 93/002179.pdf December 1, 2013 References - 1 17 • Marschall J. Catheter-associated bloodstream-infections: Looking outside of the ICU. Am J Infect Control 2008; 36:172.e5-8. • Collignon PJ, et al. Intravascular catheter bloodstream infections: an effective and sustained hospital-wide prevention program for 8 years. Med J Austr 2007; 187:551-554. • Guidelines for the Prevention of Intravascular CatheterRelated Prevention of Intravascular Device-Associated Infections Infections, 2002. MMWR 2002; 51:1-26. http://www.cdc.gov/mmwr/preview/mmwrhtml/rr5110 a1.htm December 1, 2013 References - 2 18 1. 2. IV central catheters are the main source of bloodstream infection . T/F? The main strategy to prevent CLABSI is a) b) c) d) 3. Avoid unnecessary catheters Good selection of insertion site Teflon catheters Change peripheral catheters every 72 hours December 1, 2013 Quiz Which measure should not be considered to prevent intravascular infections? a) b) c) d) Aseptic technique in insertion and maintenance of catheters Skin antisepsis with 2% chlorhexidine/alcohol Routine replacement of central venous catheters Maximum barriers for insertion of central catheters 19 • IFIC’s mission is to facilitate international networking in order to improve the prevention and control of healthcare associated infections worldwide. It is an umbrella organisation of societies and associations of healthcare professionals in infection control and related fields across the globe . • The goal of IFIC is to minimise the risk of infection within healthcare settings through development of a network of infection control organisations for communication, consensus building, education and sharing expertise. • For more information go to http://theific.org/ December 1, 2013 International Federation of Infection Control 20