* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Common Iliac Arteries External Iliac Artery EMBRYOLOGIC NOTES
Survey
Document related concepts
Transcript
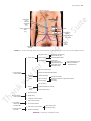
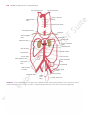
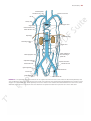
216 CHAPTER 5 The Abdomen: Part II—The Abdominal Cavity ■■ EMBRYOLOGIC NOTES ■■ Development of the Suprarenal Glands ■■ The cortex develops from the coelomic mesothelium covering the posterior abdominal wall. At first, a fetal cortex is formed; later, it becomes covered by a second final cortex. After birth, the fetal cortex retrogresses, and its involution is largely completed in the first few weeks of life. The medulla is formed from the sympathochromaffin cells of the neural crest. These invade the cortex on its medial side. By this means, the medulla comes to occupy a central position and is arranged in cords and clusters. Preganglionic sympathetic nerve fibers grow into the medulla and influence the activity of the medullary cells. Three lateral visceral branches: the suprarenal artery, renal artery, and testicular or ovarian artery Five lateral abdominal wall branches: the inferior phrenic artery and four lumbar arteries Three terminal branches: the two common iliac arteries and the median sacral artery (Fig. 5.72) These branches are summarized in Diagram 5.1. Common Iliac Arteries The right and left common iliac arteries are the terminal branches of the aorta. They arise at the level of the 4th lumbar vertebra and run downward and laterally along the medial border of the psoas muscle (Figs. 5.63 and 5.72). Each artery ends in front of the sacroiliac joint by dividing into the external and internal iliac arteries. At the bifurcation, the common iliac artery on each side is crossed anteriorly by the ureter (Fig. 5.72). Susceptibility to Trauma at Birth At birth, the suprarenal glands are relatively large because of the presence of the fetal cortex; later, when this part of the cortex involutes, the gland becomes reduced in size. During the process of involution, the cortex is friable and susceptible to damage and severe hemorrhage. External Iliac Artery The external iliac artery runs along the medial border of the psoas, following the pelvic brim (Fig. 5.63). It gives off inferior vena cava cisterna chyli hepatic veins inferior phrenic artery sympathetic trunk suprarenal vein celiac artery suprarenal artery renal vein superior mesenteric artery renal artery y lumbar arteries inferior mesenteric artery testicular artery common iliac artery external iliac artery internal iliac artery deep circumflex iliac artery inferior epigastric artery median sacral artery FIGURE 5.72 Aorta and inferior vena cava. Basic Anatomy 217 inferior vena cava celiac artery (T12) superior mesenteric artery (L1) xiphisternal joint (T9) transpyloric plane (L1) inferior mesenteric artery (L3) intercristal inter cristal plane (L4) aorta common iliac vessels anterior superior iliac spine external iliac vessels symphysis pubis internal iliac vessels FIGURE 5.73 Surface markings of the aorta and its branches and the inferior vena cava on the anterior abdominal wall. left gastric artery a. Celiac artery splenic artery hepatic artery short gastric arteries (six) splenic arteries (six) left gastroepiploic artery cystic artery right gastric artery gastroduodenal artery right hepatic artery left hepatic artery right gastroepiploic artery superior pancreaticoduodenal artery jejunal and ileal arteries 1. Three anterior visceral branches inferior pancreaticoduodenal artery b. Superior mesenteric artery middle colic artery right colic artery ileocolic artery anterior cecal artery posterior cecal artery—appendicular artery ileal artery colic artery left colic artery c. Inferior mesenteric artery sigmoid arteries (two or three) superior rectal artery a. Suprarenal artery 2. Three lateral visceral branches b. Renal artery c. Testicular or ovarian artery a. Inferior phrenic artery 3. Five lateral abdominal wall branches 4. Three terminal branches b. Four lumbar arteries a. Two common iliac arteries external iliac artery internal iliac artery b. Median sacral artery DIAGRAM 5.1 Branches of Abdominal Aorta 218 CHAPTER 5 The Abdomen: Part II—The Abdominal Cavity C L I N I C A L Veins on the Posterior Abdominal Wall N O T E S Inferior Vena Cava Aortic Aneurysms Localized or diffuse dilatations of the abdominal part of the aorta (aneurysms) usually occur below the origin of the renal arteries. Most result from atherosclerosis, which causes weakening of the arterial wall, and occur most commonly in elderly men. Large aneurysms should be treated by open surgical repair. Endovascular repair can also be used by the introduction of a stent graft through one of the iliac arteries with access through the femoral arteries in the groin. Embolic Blockage of the Abdominal Aorta The bifurcation of the abdominal aorta where the lumen suddenly narrows may be a lodging site for an embolus discharged from the heart. Severe ischemia of the lower limbs results. the inferior epigastric and deep circumflex iliac branches (Fig. 5.72). The artery enters the thigh by passing under the inguinal ligament to become the femoral artery. The inferior epigastric artery arises just above the inguinal ligament. It passes upward and medially along the medial margin of the deep inguinal ring (Fig. 4.4) and enters the rectus sheath behind the rectus abdominis muscle. The deep circumflex iliac artery arises close to the inferior epigastric artery (Fig. 5.72). It ascends laterally to the anterior superior iliac spine and the iliac crest, supplying the muscles of the anterior abdominal wall. Internal Iliac Artery The internal iliac artery passes down into the pelvis in front of the sacroiliac joint (Fig. 5.72). Its further course is described on page 256. Location and Description The inferior vena cava conveys most of the blood from the body below the diaphragm to the right atrium of the heart. It is formed by the union of the common iliac veins behind the right common iliac artery at the level of the 5th lumbar vertebra (Fig. 5.72). It ascends on the right side of the aorta, pierces the central tendon of the diaphragm at the level of the 8th thoracic vertebra, and drains into the right atrium of the heart. The right sympathetic trunk lies behind its right margin and the right ureter lies close to its right border. The entrance into the lesser sac separates the inferior vena cava from the portal vein (Fig. 5.7). The surface markings of the inferior vena cava are shown in Figure 5.73. Tributaries The inferior vena cava has the following tributaries (Fig. 5.72): ■■ ■■ ■■ ■■ Two anterior visceral tributaries: the hepatic veins Three lateral visceral tributaries: the right suprarenal vein (the left vein drains into the left renal vein), renal veins, and right testicular or ovarian vein (the left vein drains into the left renal vein) Five lateral abdominal wall tributaries: the inferior phrenic vein and four lumbar veins Three veins of origin: two common iliac veins and the median sacral vein The tributaries of the inferior vena cava are summarized in Diagram 5.2. If one remembers that the venous blood from the abdominal portion of the gastrointestinal tract drains to 1. Two anterior visceral tributaries—the hepatic veins a. Right suprarenal vein (the left drains into the left renal vein) 2. Three lateral visceral tributaries b. Renal veins c. Right testicular or ovarian vein (the left drains into the left renal vein) 3. Five lateral abdominal wall tributaries a. Inferior phrenic vein b. Four lumbar veins external iliac vein 4. Three tributaries of origin a. Two common iliac veins b. Median sacral vein DIAGRAM 5.2 Tributaries of Inferior Vena Cava internal iliac vein Basic Anatomy 219 C L I N I C A L N O T E S Blunt trauma to the aorta is most commonly caused by headon automobile crashes. Rupture of the tunica intima and media occurs and is quickly followed by rupture of the turnica adventitia. The initial rupture of the intima and media is probably mainly caused by the sudden compression of the aorta against the vertebral column, while the delayed rupture of the adventitia is caused by the aortic blood pressure. Unless quickly diagnosed by MRI, and surgical treatment instituted, death follows. anatomic inaccessibility of the vessel behind the liver, duodenum, and mesentery of the small intestine and the blocking presence of the right costal margin make a surgical approach difficult. Moreover, the thin wall of the vena cava makes it prone to extensive tears. Because of the multiple anastomoses of the tributaries of the inferior vena cava (Fig. 5.75), it is impossible in an emergency to ligate the vessel. Most patients have venous congestion of the lower limbs. Obliteration of the Abdominal Aorta and Iliac Arteries Compression of the Inferior Vena Cava Trauma to the Abdominal Aorta Gradual occlusion of the bifurcation of the abdominal aorta, produced by atherosclerosis, results in the characteristic clinical symptoms of pain in the legs on walking (claudication) and impotence, the latter caused by lack of blood in the internal iliac arteries. In otherwise healthy individuals, surgical treatment by thromboendarterectomy or a bypass graft should be considered. Because the progress of the disease is slow, some collateral circulation is established, but it is physiologically inadequate. However, the collateral blood flow does prevent tissue death in both lower limbs, although skin ulcers may occur. The collateral circulation of the abdominal aorta is shown in Figure 5.74. Trauma to the Inferior Vena Cava Injuries to the inferior vena cava are commonly lethal, despite the fact that the contained blood is under low pressure. The the liver by means of the tributaries of the portal vein, and that the left suprarenal and testicular or ovarian veins drain first into the left renal vein, then it is apparent that the tributaries of the inferior vena cava correspond rather closely to the branches of the abdominal portion of the aorta. Inferior Mesenteric Vein The inferior mesenteric vein is a tributary of the portal circulation. It begins halfway down the anal canal as the superior rectal vein (Figs. 5.22, 5.26, and 5.48). It passes up the posterior abdominal wall on the left side of the inferior mesenteric artery and the duodenojejunal flexure and joins the splenic vein behind the pancreas. It receives tributaries that correspond to the branches of the artery. Splenic Vein The splenic vein is a tributary of the portal circulation. It begins at the hilum of the spleen by the union of several veins and is then joined by the short gastric and left gastroepiploic veins (Figs. 5.22 and 5.48). It passes to the right within the splenicorenal ligament and runs behind the pancreas. It joins the superior mesenteric vein behind the neck of the pancreas to form the portal vein. It is joined by veins from the pancreas and the inferior mesenteric vein. The inferior vena cava is commonly compressed by the enlarged uterus during the later stages of pregnancy. This produces edema of the ankles and feet and temporary varicose veins. Malignant retroperitoneal tumors can cause severe compression and eventual blockage of the inferior vena cava. This results in the dilatation of the extensive anastomoses of the tributaries (Fig. 5.75). This alternative pathway for the blood to return to the right atrium of the heart is commonly referred to as the caval–caval shunt. The same pathway comes into effect in patients with a superior mediastinal tumor compressing the superior vena cava. Clinically, the enlarged subcutaneous anastomosis between the lateral thoracic vein, a tributary of the axillary vein; and the superficial epigastric vein, a tributary of the femoral vein, may be seen on the thoracoabdominal wall (Fig. 5.75). Superior Mesenteric Vein The superior mesenteric vein is a tributary of the portal circulation (Figs. 5.22, 5.26, and 5.48). It begins at the ileocecal junction and runs upward on the posterior abdominal wall within the root of the mesentery of the small intestine and on the right side of the superior mesenteric artery. It passes in front of the third part of the duodenum and behind the neck of the pancreas, where it joins the splenic vein to form the portal vein. It receives tributaries that correspond to the branches of the superior mesenteric artery and also receives the inferior pancreaticoduodenal vein and the right gastroepiploic vein (Fig. 5.22). Portal Vein The portal vein is described on page 194. Lymphatics on the Posterior Abdominal Wall Lymph Nodes The lymph nodes are closely related to the aorta and form a preaortic and a right and left lateral aortic (para-aortic or lumbar) chain (Fig. 5.76). 220 CHAPTER 5 The Abdomen: Part II—The Abdominal Cavity right subclavian artery left subclavian artery intercostal posterior intercos arteries internal thoracic artery thoracic part of aorta musculophrenic c artery diaphragm diaph superior epigastric c artery phrenic artery phre left renal artery middle colic artery superior mesenteric artery abdominal aorta right colic artery lumbar arteries marginal artery ileocolic artery left colic artery inferior epigastric artery inferior mesenteric artery fourth lumbar artery sigmoid arteries sig deep circumflex x iliac artery internall iliac artery superio superior rectal artery middle rectal artery arter median sacral artery inferior rectal a artery FIGURE 5.74 The possible collateral circulations of the abdominal aorta. Note the great dilatation of the mesenteric arteries and their branches, which occurs if the aorta is slowly blocked just below the level of the renal arteries (black bar). The preaortic lymph nodes lie around the origins of the celiac, superior mesenteric, and inferior mesenteric arteries and are referred to as the celiac, superior mesenteric, and inferior mesenteric lymph nodes, respectively. They drain the lymph from the gastrointestinal tract, extending from the lower one third of the esophagus to halfway down the anal canal, and from the spleen, pancreas, gallbladder, and greater part of the liver. The efferent lymph vessels form the large intestinal trunk (see Fig. 1.18 and below). The lateral aortic (para-aortic or lumbar) lymph nodes drain lymph from the kidneys and suprarenals; from the testes in the male and from the ovaries, uterine tubes, and fundus of the uterus in the female; from the deep lymph vessels of the abdominal walls; and from the common iliac nodes. The efferent lymph vessels form the right and left lumbar trunks (see Fig. 1.18 and below). Lymph Vessels The thoracic duct commences in the abdomen as an elongated lymph sac, the cisterna chyli. This lies just below the diaphragm in front of the first two lumbar vertebrae and on the right side of the aorta (Fig. 5.76). The cisterna chyli receives the intestinal trunk, the right and left lumbar trunks, and some small lymph vessels that descend from the lower part of the thorax. Basic Anatomy 221 brachiocephalic subclavian vein vein superior vena cava first rib axillary vein azygos vein hemiazygos veins internal thoracic vein lateral thoracic vein diaphragm inferior vena cava ascending lumbar vein lumbar veins inferior epigastric vein superficial epigastric vein external iliac vein inferior mesenteric vein ascending to portal vein superior rectal vein internal iliac vein inguinal ligament middle rectal vein femoral vein great saphenous vein inferior rectal vein FIGURE 5.75 The possible collateral circulations of the superior and inferior venae cavae. Note the alternative pathways that exist for blood to return to the right atrium of the heart if the superior vena cava becomes blocked below the entrance of the azygos vein (upper black bar). Similar pathways exist if the inferior vena cava becomes blocked below the renal veins (lower black bar). Note also the connections that exist between the portal circulation and systemic veins in the anal canal. Lymphatic Drainage of the Gonads The importance of the lymph drainage of the testis was emphasized on page 132. Nerves on the Posterior Abdominal Wall Lumbar Plexus The lumbar plexus, which is one of the main nervous pathways supplying the lower limb, is formed in the psoas muscle from the anterior rami of the upper four lumbar nerves (Fig.5.77).The anterior rami receive gray rami communicantes from the sympathetic trunk, and the upper two give off white rami communicantes to the sympathetic trunk. The branches of the plexus emerge from the lateral and medial borders of the muscle and from its anterior surface. The iliohypogastric nerve, ilioinguinal nerve, lateral cutaneous nerve of the thigh, and femoral nerve emerge from the lateral border of the psoas, in that order from above downward (Fig. 5.34). The iliohypogastric and ilioinguinal nerves (L1) enter the lateral and anterior abdominal walls (see page 124). The iliohypogastric nerve supplies the skin of the lower part of the anterior abdominal wall, and the ilioinguinal nerve passes through the inguinal canal to supply the skin of the groin and the scrotum or labium majus. The lateral cutaneous nerve of the thigh