* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download PICC Complication Management
Survey
Document related concepts
Transcript
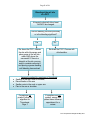
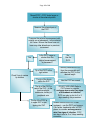
Page 1 of 19 PICC Complication Management Velindre Cancer Centre A guide for healthcare professionals in the care and management of PICC-related complications bases on presenting symptoms. Meinir Hughes IV Access Specialist Nurse Updated Jan 2107 Reference will be provided at the end of the document for ease of use Page 2 of 19 Complication management Index Page 3 Unable to obtain a blood sample from a PICC Administration of bolus urokinase into a PICC without a blood return 4 Bleeding at the exit site 5 6 Signs of dressing allergy 7 Redness, swelling or pain of the arm above the PICC 8 Thrombosis assessment form Unable to flush a PICC – complete occlusion 9 Administration of bolus urokinase into a blocked PICC using 3 way tap 10 Migrated PICC 12 Leaking PICC 13 Pain in the chest neck or shoulder 14 Signs of exit site infection 15 Stuck PICC – unable to remove the PICC 16 Complete migration of a severed PICC 17 Patient with signs of systemic infection – catheter-related blood stream inf 18 References 19 PICC Complication Management May 2016 Page 3 of 19 Unable to obtain a blood sample from a PICC Flush the PICC with 5-10 mls of N. Saline 0.9% using a positive pressure technique Still no blood return: Ask pt to take deep breaths. Change the patients position, lie patient flat or sit up/ask to lie on their side. Still no blood return: Remove the dressing and check for any signs of catheter kinking. Change the needlefree connector. Carefully remove the upper portion of the securacath to separate the two portions and observe for kinks. Replace the upper portion of the securacath and attempt to withdraw blood. Still no blood return: Chest X-ray to determine tip location of the catheter. Nb: If no X-ray facilities available i.e outreach/out of hrs, proceed with urokinase. If the catheter tip is in the correct location administer a bolus dose of urokinase 10,000 units - follow instructions page 4. Repeat urokinase if unsuccessful. If catheter tip is NOT in the correct location, DO NOT use and contact PICC placer/ANP/Dr. If no blood return after 3 x doses of urokinase, consult PICC placer/ANP. Consider lineogram to determine prescence of a fibrin sheath PICC Complication Management May 2016 Page 4 of 19 Administration of bolus Urokinase into a PICC without a blood return You do NOT need to use a 3 way tap for the bolus administration of urokinase when there is only a partial occlution – i.e unable to get a blood return but can flush. Equipment required: Procedure incorporating ANTT Plastic tray Non-sterile gloves 1 x 10ml syringe Blunt needle Urokinase 10,000units - Urokinase can be given by a named individual using a Patient Group Direction I x 5ml vial diluents (water or saline – see urokinase data (box)) 2 x green clinell wipe Needle free connector Procedure: 1. Wash hands. 2. Clean the tray with clinell antiseptic wipes and leave to dry. 3. Place unopened equipment into the tray: syringe, blunt needle, urokinase vial, non-sterile gloves, diluents vial, needle-free connector and 2 x clinell wipes. 4. Put on non-sterile gloves. 5. Remove the cap from the urokinase vial and clean the bung with the clinell. Make sure to use a part of the clinell not touched by the gloves. 6. Open the syringe & needle taking care not to contaminate key parts and draw up 1.5ml of the diluent. 7. Reconstitute the Urokinase with 1.5ml of diluent. Draw up 1.5ml of Urokinase solution into syringe. 8. Place the syringe filled with urokinase back into the syringe packaging or place a red end on the tip of the syringe to protect the key part. 9. Remove the needle free connector from end of the PICC, clean the very end of the PICC with a clinell – clean with a part of the clinell you have not touched – leave to dry. 10. Attach the syringe containing the Urokinase to the line and infuse 0.5ml into the PICC at 10 minute intervals until all 1.5mls administered. Label the line to inform that there is a urokinase lock in situ. 11. Apply a new needle free connector to end of PICC and leave the Urokinase insitu for one hour 12. Withdraw the Urokinase lock. If blood withdrawal is possible flush with 15-20 mls of saline. 13. If the procedure is unsuccessful on the first attempt, flush the catheter and then repeat the procedure again without delay – it is safe to flush the PICC after 1hr. PICC Complication Management May 2016 Page 5 of 19 Bleeding at the exit site of a PICC A biopatch soiled with blood must ALWAYS be changed. Has the bleeding occurred previously or is the bleeding significant? Yes Re- dress the PICC, cleanse the site with chloraprepp and place gauze at the exit site under AND above the securacath! If there is a biopatch at the site you may need to consider removing it and placing a gauze dressing until bleeding has resolved. No Re-dress the PICC. Cleanse with chlorhexidine. Assess the patient for symptoms of thrombosis: Swelling of the arm, neck or shoulder; Discolouration of the arm Swollen veins in the neck or upper arm Pain in the arm or shoulder If symptoms are present, follow the algorithm for Thrombosis: Page 7 If symptoms are not present, ensure that patient has a follow up appointment for a review. PICC Complication Management May 2016 Page 6 of 19 Redness and tenderness or blistering beneath the PICC dressing: Allergy to dressing Are the symptoms severe with redness + + open wounds or blistering? Yes No Apply cavilon beneath all the dressing. Review patient in 2-4 days. Apply a Duoderm dressing beneath the PICC. DO NOT use cavilon and duoderm! Refer to guidelines: PICC care and management. Has the allergy improved? Symptoms are much worse – blistering etc No Yes Review patient in 2-4 days to assess and consider prescribing piriton if experiencing severe itching. Is there an improvement when patient is reviewed? No If slightly worse, change the dressing to a different one: IV 3000/ hydrofilm/Mepitel dressing. DO NOT USE CAVILON. Review in 2-4 days Yes Dress with biotain or mefix – both dressings must be removed before IV therapy to examine PICC site. If allergy remains and securacath present, cover loosely with gauze and bandage. Continue to apply cavilon beneath all the dressing. Review in 2-4 days. Re-dress using duoderm and assess patient every 4-5 days. If symptoms clear up, attempt to dress without duoderm with a different dressing from the original. If allergy persists – remove the line. PICC Complication Management May 2016 Page 7 of 19 The patient has a swollen, inflamed, red or painful arm, hand or neck: Consider Thrombosis. Asses the patient for the following symptoms: Bleeding at exit site Discolouration of the arm (cyanosis/redness) Pain in arm shoulder or neck Protruding veins in the chest, arm or neck Difficulty moving the arm You will need to do the following: Chest X-ray to verify tip placement Doppler Ultrasound If Doppler US not available and symptoms are significant – give LMWH whilst awaiting Doppler Contact an appropriate practitioner: IV Access Nurse; ANP or PICC placer Positive result: Complete thrombosis assessment form. Page 8 Review X-ray result for tip tocation and verify that PICC is functioning – flushing and blood withdrawal present. Take bloods: Fbc; Rlb; Coag screen Prescribe anticoagulant therapy – currently low molecular weight heparin Make an appointment for re-assessment according to thrombosis assessment form. If the patient is on LMWH when thrombosis is diagnosed, registrar to review case with Haematologist. Yes if: The PICC is not in the correct position on X-ray There is evidence of severe/extensive thrombosis i.e peripheral vein; axilla and subclavian. Symptoms do not improve or get worse after 24-48 hrs Symptoms of infection are present. However, medical guidance will be required. It is recommended that removal takes place after 48hrs of anticoagulation. As a general rule, the PICC can be used when there is a DVT present unless the patient condition determines otherwise. Should the PICC be removed? No if: Symptoms are mild or improve when re-assessed The Doppler shows less extensive thrombosis. This has to correspond with the PICC tip being in correct location and the PICC is functioning i.e giving blood and flushing. PICC Complication Management May 2016 Page 8 of 19 PICC-related Thrombosis assessment form: Suspected or diagnosed UEDVT Name of patient: ……………………………… Hospital Number: …………………………… Date: ..................... Assess each patient’s symptoms: A. On presentation – day 1 B. Day 3 C. Day 6 D. Day 10 Perform PICC X-ray. Is the tip of the PICC correctly positioned in lower SVC?: yes Is the catheter functioning: Patent to flushing and blood withdrawal present?: no yes no Blood samples taken: Fbc: Coag screen: Renal and liver profile: Treatment given: ………………………………………………………………………………... Symptoms Present (please circle) a. Pain in: neck, arm or shoulder 0 1 2 no pain mild pain moderate pain 1 No swelling minimal swelling no 3 b. Swelling of: the neck, arm or shoulder 0 yes severe pain yes no State yes or no e. Limb discolouration State yes or no f. Headaches State yes or no g. Poor movement of the arm yes 100% movement 75% movement 50% movement If swelling of the arm exists please measure at each assessment date. Please state measurement from the exit site to area of swelling: ………… cms …….. Score …….... Score ……... Score …….. Score Score Score Score Score Score Score Score Score ……cm ……cm ……cm …….cm extensive swelling d. Bleeding at the exit site 2 Date 3 State yes or no 1 Date very severe c. Dilated collateral veins 0 Date 4 2 significant swelling Date no 3 < 25% movement Measurement of arm circumference at measuring site: Signature: PICC Complication Management May 2016 Page 9 of 19 Unable to flush a PICC Change end connector. Remove the dressing - check for any external kinks or any damage to the line. Carefully remove the PICC from the securacath and manipulate gently between finger and thumb. Ask pt to change position. Attempt to flush but do not use excessive force Yes: Use the PICC Can you flush the line? Use the 3 way tap method to infuse 10,000 units (re-constituted as instructed) into the PICC. See instructions page 10. There is NO need to X-ray the PICC at this stage unless symptoms of migration are present. Are you able to withdraw blood from the PICC and flush it? Yes Use the PICC Probable cause is blood within the lumen of the line. No X-ray to determine tip location. Repeat the infusion of Urokinase using the 3 way tap a further 2 times if required. Are you able to withdraw blood from the PICC and flush it? No Determine probable cause of the occlusion. Has TPN been infusing or has there been a drug incompatibility leading to precipitate? If Yes: Contact pharmacy for advice. No Seek advice from PICC placer or ANP PICC Complication Management May 2016 Page 10 of 19 Administration of bolus urokinase into a blocked PICC using a 3 way tap Equipment required Plastic tray Pair of non-sterile gloves 2 x luer lock 10ml syringes Blunt needle 3 way tap Urokinase 10,000units - Urokinase can be given by a named individual using a Patient Group Direction 1 x 5mls vial of diluents (saline or water) (usually written on the urokinase box) Green clinell wipe x 2 Needle free connector Sharps bin Procedure: Using ANTT principles: 1. Wash hands. 2. Check Urokinase details in usual way, e.g., Name; Dose; Expiry Date; Route of administration. 3. Clean plastic tray with clinell antiseptic wipes and leave to dry. 4. Place unopened equipment into the tray: 2 x syringes, blunt needle, 3 way tap, urokinase vial, non-sterile gloves, diluent and 2 x clinell. 5. Put on non-sterile gloves. 6. Remove the cap from the urokinase vial and clean the bung with the clinell. Make sure to use a part of the clinell not touched by the gloves. 7. Open one syringe and the blunt needle and draw up 1.5mls of the diluents. 8. Reconstitute the Urokinase with 1.5mls of diluent. Draw up 1.5mls of Urokinase solution into syringe. 9. Open the 3 way tap and carefully prime with the Urokinase solution. 10. Make sure to protect all the key parts of the 3 way tap prior to placing back on the tray. 11. Remove the needle free connector from end of the PICC, clean the very end of the PICC with a clinell – clean with a part of the clinell you have not touched. Attach 3-way tap to the end of the lumen. 12. Close the 3 way tap to the patient: attach the syringe containing the urokinase onto the three way tap at 3 o’clock and an empty syringe onto 6 o’clock (see picture – next page) PICC Complication Management May 2016 Page 11 of 19 13. Turn the tap OFF to the Urokinase syringe (3 o’clock – picture below left), pull back on the empty syringe (6 o’clock) to create vacuum in catheter to approximately 8-9mls and hold the plunger at aprox 8mls whilst at the same time slowly turning the closed position onto the empty syringe (picture below right). Stop turning once you see a small amount of Urokinase enter the PICC. 14. Repeat the procedure from point number 12 another 3 times every 5 minutes until all the urokinase has been infused. Occasionally, urokinase will leak into the empty syringe – when this happens turn the 3 way tap off to the patient to infuse the urokinase into the original syringe and perform the procedure again from point 12. 15. Apply a new needle free connector to the end of PICC and leave the Urokinase insitu for one hour. 16. After one hour, attempt to withdraw the Urokinase lock and establish a blood return. If blood withdrawal is possible flush with 15-20 mls of saline. If blood return is not present, flush the PICC with 10mls of Normal Saline 0.9% and attempt to establish a blood return again – this is safe to do after one hour. 17. If no blood return present repeat the whole process without delay – this can be done up to another 2 times. It is recommended although NOT necessary (i.e if this occurs when X-ray is closed) to perform a chest X-ray after the first attempt fails. 18. Decontaminate tray and dispose of equipment according to hospital procedure, and document clearly in patient’s notes. PICC Complication Management May 2016 Page 12 of 19 Moved PICC – PICC looks longer or shorter at the external portion. Measure the external part of the PICC. Compare the external measurement with original one at placement - in the notes or on Canisc. Ensure that there have not been any other alterations i.e previous movement. Yes Chest X-ray to review tip location Is the PICC longer or shorter than the original measurement at placement? No. Use the PICC Tip of the PICC in the right atrium Carefully remove the PICC from the securacath and withdraw the PICC to the desired length. The tip of the line is within the SVC Use the PICC as normal. The tip of the PICC is out of the SVC – in the brachiocephalic, subclavian, axillary or peripheral vein. The tip of the PICC is in upper SVC or just tipping into SVC DO NOT USE LINE: Refer to PICC placer to consider exchange over a wire if no signs of thrombosis or infection. PICC can stay in situ for 2 or 3 days awaiting this procedure. Assess need for the PICC. If last treatment – use the PICC and remove. If for further treatments refer to PICC placer to consider exchange over a wire if no signs of infection. PICC PICC Complication Management May 2016 can stay in situ for 2 or 3 days awaiting procedure. Page 13 of 19 Leaking at the site of the PICC or a leak from a split in the PICC If the PICC is leaking from the exit site or from a split in the line, DO NOT use the PICC. If the PICC is no longer required for therapy, remove the PICC. Keep the PICC for the IV Access Specialist to examine. If the PICC is still required, refer to a PICC placer or ANP. PICC replacement will be necessary. PICC Complication Management May 2016 Page 14 of 19 Pain in the shoulder, neck or chest Consider Migration of the tip of the catheter into a location other than the SVC Extravasation Damaged PICC Examine arm and chest for signs of extravasation Flush the PICC with Saline and observe for any symptoms Thrombosis Review patient for other symptoms of thrombosis. See page: 7 Ensure PICC is giving a blood sample. If in doubt request lineogram Request chest X-ray to determine tip position. PICC Complication Management May 2016 Page 15 of 19 Redness or pain at the exit site of the PICC Is the redness associated with swelling or exudate at the site? Yes Collect swab from site. Please make sure all relevant information and diagnosis is clearly written on the form. No Consider early signs of infection Evaluate symptoms. If there is redness, exudate, swelling or pain at the exit site within 2 cm of exit site – treat as infection. Also: Consider reaction to the securacth: Treat as exit site infection Cleanse the site with chlorhexidine in alcohol and allow to dry for 2 mins. Prescribe oral anti biotics. If symptoms are fairly significant, consider removal of the PICC. Send tip for C&S. Prior to removal, cleanse the exit site thoroughly in order to prevent contamination of the tip as it passes through the skin. –. Is there clear straw colour watery exudate without redness, pyrexia? Consider lymph drainage Cleanse the exit site with chlorhexidine 2% in alcohol and leave to dry Advise patient to report any exacerbation of the redness or any other symptoms: pain, swelling or exudate Assess for symptoms of systemic infection: Rigors and pyrexia or general deteoriation. If present – follow guidelines for suspected systemic infection promptly. See page 18. NB: Biopatches are not to be used as treatment of infections once diagnosed. PICC Complication Management May 2016 Page 16 of 19 Stuck PICC. Unable to remove a PICC NEVER forcefully remove a PICC. Place a dressing securely over the PICC and X-ray the patient: Request a chest, arm and shoulder X-ray. Observe the X-ray closely for any knots in the line. No Knots. Apply heat along the length of the vein for 10 mins then attempt to remove. If still no success: A Knot is visable on X-ray No success No risks: Is it within normal working hrs; is there a radiologist on site? Refer to interventional radiologist in the nearest teaching hospital Assess the patient for any risks associated with a stuck PICC. If no risk, patient can be discharged and to attend VCC for another attempt in 1-3 days. Still no success. If risks Yes No success With a radiologist present, attempt to place a wire into the PICC under fluoroscopy and attempt to remove the PICC – great care must be taken when using a wire and ONLY experienced practitioner such as a Doctor, ANP or PICC placer should attempt. Clamp the external part of the line which has been cut !! Replace the securacath! Refer to vascular surgeon. Refer to vascular surgeons in the nearest teaching hospital. Remove both parts of the securacath! (This is to ensure that the Surgeons don’t have this as an obstacle). PICC Complication Management May 2016 Page 17 of 19 Complete migration of a severed portion of a PICC into the venous system Is the patient at home and there is clear indication that the PICC has completely migrated (you may ask the patient to take a picture and email to VCC to establish for certain) Yes; patient is at home and there is clear indication that a portion of the PICC has completely migrated: Advise patient to lay flat. Assess patients condition: If difficulty breathing or other acute symptoms, 999 ambulance to be On admission to the unit contacted to attend local acute Establish that there is no hospital external part of the PICC that If asymptomatic, advise pt to lie flat can be located and arrange for direct referral to an interventional radiologist or surgeon in patients local acute hospital. No: Patient is in Velindre: Lie patient flat Monitor patient closely Record observations, NEWS Contact IV Access specialist bleep 157 or ANP Assess patient’s condition: If difficulty breathing or other acute symptoms, give oxygen and dial 999 ambulance. Place patient in steep left lateral position if it is suspected that PICC is obstructing the pulmonary valve. If patient asymptomatic; On call Medical Registrar to refer to the Vascular suite in the X-ray department at UHW If out of hours patient will need to be admitted under the care of the surgical team. Contact the Vascular room to request that all parts of the PICC (external and internal) are saved to send for analysis PICC Complication Management May 2016 Page 18 of 19 Patient presenting with symptoms of systemic infection and has a CVC (Central Venous Catheter) in situ. Please use along with full guidelines on the intranet. Yes Follow the neutropenic sepsis policy Yes Yes Is the patient pyrexial? Is the patient neutropenic? Is or has the patient been experiencing rigors associated with flushing of the line on admission or at home? Highly suspicious of a CVC related infection. Inform Registrar/Consultant and observe patient closely. No No Is or has the patient been experiencing rigors associated with flushing of the line on admission or at home? No No Take blood cultures from CVC and peripheral vein. Observe patient for symptoms of infection Check observations ½ hourly; observe for signs of septic shock. Observe urinary output closely – start a fluid balance chart Blood sampling: Fbc, Emergency U + E Blood cultures - from BOTH CVC (all lumens) AND peripheral vein. When taking blood cultures from a CVC, take separate samples from each lumen and do not discard the first blood. If there is a high suspicion of line infection i.e significant history of rigors post flush and or patient unwell – take blood cultures from the line BUT DON’T flush but remove the line! CVC to be left in situ Assess the criteria for immediate removal – see section 3 of CVC infection guidelines Give broad spectrum antibiotics through the line. (according to neutropenic sepsis policy) IV ANTIBIOTICS MUST BE GIVEN AS SOON AS POSSIBLE Continue to monitor patient closely. If blood culture is positive, seek microbiology advice (see table 1) Line may need to be removed. CVC to be removed Treat with antibiotics peripherally. According to neutropenic sepsis policy if neutropenic or seek microbiology advice If the CVC is to remain in situ, treat with antibiotics according to organism specific guidelines and seek microbiology advice (see table 2) If the patient continues to have signs of infection after 48hrs or is deteriorating clinically– remove the line. Send line tip to microbiology for culture & inform infection control nurse PICC Complication Management May 2016 Page 19 of 19 References Baskin. J et al. (2009) Management of occlusion and thrombosis associated with long term indwelling central venous catheters. Lancet 374 (9684) 159 Bertoglio S et al. Efficacy of normal saline versus heparinized saline solution for locking catheters of totally implantable long-term central vascular access devices in adult cancer patients. Cancer Nursing 2012; 35: E35–E42. Clinical Practice Guidelines for chronic kidney disease: evaluation and classification. https://www.kidney.org/sites/default/files/docs/ckd_evaluation_classification_stratification.pdf Dougherty L and Lamb J (2008) Intravenous Therapy in Nursing Practice: Second edition. Oxford, Blackwell Publishing Drewett (2000) Central venous catheter removal: procedures and rationale, British Journal of Nursing 9 (22). Frank D, et al (2000) The treatment and outcome of cancer patients with thromboses on centrel venous catheters. Journal of Thrombosis and Thrombolysis 10 271-275. Hoch J. (1997) Management of complications of long term venous access. Seminars in Vascular Surgery 10 (3) 135-143. Infusion Nursing Society. Standards of Practice. Journal of Infusion Nursing (2006); 29(1S) James L, Bledsoe L, Hadaway L.(1993) A retrospective look at tip location and complications of PICC lines. Journal of Intravenous Nursing 16 (2) Lauson M (1991) Partial occlusion of indwelling central venous catheters. Journal of Intravenous Nursing 14 (3). Loveday H, et al (2014) epic3: National Evidence-based guidelines for preventing healthcare associated infections in NHS hospitals in England. Journal of Hospital Infection 86 sup 1 Macklin D. (1997) How to manage PICCs. American Journal of Nursing 97 (9) 27-32. O’Grady et al. (2011). Guidelines for the prevention of intravascular catheter-related infection. Clinical Infectious Diseases 52 (9) 162-193. Pettit J. (2007) Technological advances for PICC placement and management. Advances in Neonatal care. 7 (3) 122-131. RCN (2003/Nov 2005) Standards for infusion therapy Richardson D, Bruso P (1993) Vascular access devices – management of common complications. Journal of Intravenous Nursing 16 (1) 44-49. Rowley S. (2009) Improving standards of aseptic practice through an ANTT trust wide implementation process: a matter of prioritisation and care. Journal of Infection Prevention 10 (1) sup18-23 Savage K, et al (1999) Outpatient use of low molecular wright heparin (Dalteparin) for the treatment of deep vein thrombosis of the upper extremily. Thromb Haemost 82 1008-10 Scales K (1999) Vascular access in the acute care setting in Dougherty L, Lamb J (Eds) IV therapy in nursing practice. Edinburgh, Churchill Livingstone. Simcock. L. (2001) Managing occlusions in central venous catheters. 197 (21) 36 The Royal Marsden Hospital (1993) Care of patients with central venous lines. Manual of Standards of Care. 3rd edition. 69. Todd J (Feb 1998) Peripherally inserted catheters. Professional Nurse. 13 (5). Weinstein TSJ et al (1997) Plumer’s principles and practice of intravenous therapy. Sixth edition. Philadelphia PA. JB Lippincott. . PICC Complication Management May 2016