* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download I - UAB School of Optometry
HIV and pregnancy wikipedia , lookup
Viral phylodynamics wikipedia , lookup
Herpes simplex research wikipedia , lookup
Canine distemper wikipedia , lookup
Marburg virus disease wikipedia , lookup
Vectors in gene therapy wikipedia , lookup
Canine parvovirus wikipedia , lookup
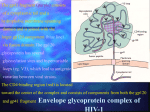
FUN2: 11:00-12:00 Scribe: Teresa Kilborn Monday, October 20, 2008 Proof: Ashley Holladay Dr. Bucy Immunology Page 1 of 6 Pathology- Immunopathology and Acquired Immunodeficiency Syndrome This lecture began by finishing the slides from the previous lecture. I. Rheumatoid Arthritis [S35] a. The mic was late picking up so the following are my notes: i. The Rheumatoid factor is an IgM Ab that binds to the Fc of IgG. The Rheumatoid factor is an Ab that is a diagnostic marker for RA; however 10% of people with RA do not have the Rheumatoid factor b. If you add an Ab to another Ab you would get immune complexes and immune complex disease would be a big feature of it but people with RA hardly ever get glomerulonephritis which is the hallmark of immune complex disease. c. The lesion in RA is called pannus tissue [S36] i. It develops in the same way that other types of inflammatory lesion develop but it occurs in particular tissue at the synovial lining of joints and it can erode into the bone tissue and deform the joint. ii. [S37] When you get inflammation that erodes the joint then you get mechanical abnormalities of the joint and this inflammatory lesion can get exuberant like in the thyroid gland where you have germinal center formation. iii. In RA, the inflammatory tissue grows up into villi structures full of reactive cells and a very activated synovium. iv. [S38] People get rheumatoid nodules in which there is a necrotic center in the skin and a big granuloma forms around that. Sometimes this points to mechanical injury. v. [S39] In the synovium itself you can have a huge amount of inflammatory tissue and a lot of plasma cells and many of those plasma cells are making rheumatoid factor so there may be some bacteria in there that is driving this process. vi. [S40] Like inflammatory bowel disease particularly Chrom’s disease, inhibition of TNF alpha a cytokine that is a molecule made by T cells and activates macrophages is a effective treatment for the symptoms of RA, but if you stop taking it then the disease tends to recur and so you can think of TNF alpha inhibitors as having the activity of corticosteroids in that inhibit immune responses but with a lot less side effects compared to corticosteroids. vii. [S41] The inflammatory process can become injured and you get acute inflammatory cells and you can get effusions in RA with a lot of fluid collecting in joint spaces. This is a picture of where it is eroded into the bone and causes mechanical deformation. II. Systemic Lupus [S42] a. The only example that he talks about of immune complex disease. b. It is one of the classic systemic autoimmune diseases. c. Any DNA complexes are often implicated in the pathogenesis, but to the degree that he understands it, the primary lesion seems to be a deregulation of the stringency of B cells forming Ab. d. You can get auto-Ab to a ton of different molecules: clotting factors, DNA, microsomes, fragments of dead cells of various types, constituents of nuclear proteins, etc. Presumably that is just because that is the material lying around with these hyperactive B cells that just make Ab to whatever it selects out the specificities that they are around and then those Ab that form nasty immune complexes are what actually cause the disease. e. [S43] There are a lot of different forms. The injury to the kidney during lupus is primarily where the morbidity is. You can get several different kinds of glomerulonephritis from this, from membranous to the focal proliferative form. Sometimes this proliferation is more diffuse and that has to do with where the immune complexes are located because of their size and charge structure. f. [S44] You can also have skin lesions where the Ab deposition along the dermal/ epidermal junction with disruption of the skin g. [S45] This causes a particular characteristic butterfly shaped rash over the bridge of the person’s nose. Oftentimes you will someone who has active lupus and you can recognize it down the hall. (Slide 46 deleted) Acquired Immunodeficiency Syndrome (New Powerpoint) III. HIV [S1] a. People are treated with a combination of various drugs for HIV referred to as HAART- Highly active antiretroviral therapy- 20 different drugs are actively used against HIV and it is difficult to keep up with which exact combination drugs a particular patient is on during studies so as long as you have a highly active combination it ends up being about the same. b. [S2] HIV is still new a relatively new disease as opposed to diseases such as tuberculosis that have been around as long as people and are hence found in Egyptian mummies. i. The first isolate of HIV was in Central Africa in 1959 ii. Recently there was another isolate found in a specimen from the early 60’s, but the epidemic really didn’t start until the late 70’s FUN2: 11:00-12:00 Scribe: Teresa Kilborn Monday, October 20, 2008 Proof: Ashley Holladay Dr. Bucy Immunology Page 2 of 6 iii. It is not completely clear why this is, but there is some evidence that it may be because of recent development in Central Africa that allowed for the disease which may have been smoldering there to break out into the larger population. iv. When he was in med school, it was referred to as a gay related immunodeficiency (GRID) because it was localized in homosexual men and no one knew what it was. At the time, deferential diagnosis was based upon 10 different things. The fact that it was a new virus was at the top of the list, but they still really had no idea what was going on. v. It was given the name human immunodefincency virus in 1984 vi. The first drug was developed in 1987. AZT was previously used as an anticancer drug so it was already developed, it was produced, there was a lot of toxicity and it was used to treat some people and has activity but the type of activity it has is if you are in the end stage of HIV and are treated with it you might live 18 months instead of 12 months. Not a big bonus but statistically quite significant. vii. The identification of the 3 stages. AIDS is the end stage of the HIV infection. The idea of the early stage and the long asymptomatic clinical stage was not understood until the 1990’s viii. The development of a new assay called competitive RT-PCR in 1993 allowed you to measure quantitatively the amount of viral RNA in the patient’s blood which correlated to the amount of virus. ix. Combination anti-retroviral drugs were developed in 1995 and represented effective treatment x. [S3]These combinations of drugs were introduced into Africa later than in Western Europe and the US. As of this year there are still more new infections than there are deaths of HIV so the epidemic is still expanding in terms of numbers of people xi. The new protease inhibitor was introduced in 1995 and the number of deaths dramatically decreased after that introduction. Previous to that people were regularly dying from the end stage HIV. The new class of drugs prevented that. xii. [S4] Another way of looking at that, this is the death rate from HIV infection during that period of time. In early 1980s, it was recognizable, but rare. It grew like a rocket during the 1980s passing by other causes of death in young adults. The introduction anti-retroviral drugs deceased the deaths but did not bring it all of the way down because there are still a huge number of people still infected and people are now becoming resistant to the drugs and the virus is growing again and can result in death. xiii. [S5] WHO keeps track of the infections. A random sample of people on the streets of Batswana would result in 30% showing infection using blood testing. In the United States, the rate is around .5%. If you calculate the lifetime incidence rate, as epidemiologists do, you would find that a 10 year old boy in Africa has 95% chance of dying from HIV. c. Basic Biology of HIV [S6] i. It is a retrovirus. This means that it has RNA genomes that are integrated into the chromosome of the host at infection. ii. The viral particle is made up of several different proteins. One is the gp120 and a stalk called gp41. iii. The rest of the surface is lipid so the Ab that would normally be able to neutralize the virus (like how the polio virus is neutralized) and you can get immunized to virus and prevent polio because you have Ab for the capsid of the exterior proteins and the Ab can clear the virus before it can infect the cells. iv. The problem with HIV is that the molecules are super variable. There are so many different genetic changes that any one isolate doesn’t effectively block other different molecules in HIV. v. Another important molecule is the capsid proteins (yellow) called p24. If there is an immune response of T cells that is somewhat effective, it is to these capsid proteins and the reason is that they have to fit together very tightly to make an effective capsid. If there are mutations in these proteins then the virus is not as health or fit of a virus and can’t grow as fast because the capsid is sort of floppy. So those are good targets for the immune system. But again, people who are infected have immune responses to these proteins but it is not good enough of an immune response to block disease progression. d. The life cycle of HIV [S7] i. The life cycle of particular infectious round starts with viral entry and the CD 4 molecule on the surface of cells and one of two different co receptors is how the virus gets in using the gp120 and gp41 to insert itself into the cell. ii. Reverse transcription changing the RNA molecule into DNA. That DNA integrates into the host chromosome and then transcriptional activation of the integrated provirus is when you have the virus that is in the chromosome and then production of viral proteins, assembly and maturation of viral particle and then that feeds back to make another round of infection. iii. [S8] Points out that in different stages of the life cycle are where different drugs to treat HIV work. The first and best target in the sense of a unique step of the viral life cycle is reverse transcription. Mammals, we don’t have any process that transcribes RNA into DNA so the enzyme, reverse transcriptase, that does FUN2: 11:00-12:00 Scribe: Teresa Kilborn Monday, October 20, 2008 Proof: Ashley Holladay Dr. Bucy Immunology Page 3 of 6 that, is absolutely characteristic of retroviruses. You can have a poison for that enzyme and it will not affect the host enzymes. Unfortunately, most drugs that block reverse transcriptase also block the DNA dependent DNA polymerase that allows you to have proliferative cells. AZT was used previously as an anti cancer drug because it blocks the proliferation of cells. It blocks the RNA into DNA step a lot better than it blocks the DNA into DNA step, but still AZT suppresses cells such as bone marrow where you need a lot of cells proliferating. If you take a drug that blocks that then you have anemia and other problems so that limits the dosages that can be given of these reverse transcriptase. There is a new drug that blocks the integration of the cDNA into the chromosome of the target. iv. Outside, in the maturation of the viral particles there is an enzymes called protease. Protease is a unique enzyme to the virus. It makes a proteolytic cleavage of capsid proteins to allow them to lock down together before you get the RNA into the capsid. You don’t want to lock it up, but once it gets formed inside the viral particle, the protease clips the capsid and it tightens up and is prepared to be injected into the next cell. If that enzyme is blocked by different drugs then the viral particle is there, but it can’t infect any new cells so that stops the infection. v. There are also drugs that block this entry process by interacting with the gp41. vi. [S9] This goes through the processes of this entry step showing that there are two different chemokine receptors that interact with CD4. One of the tricky things about the virus is that the site of the virus on the gp120 that binds to CD4 is covered up in the protein structure. There is a loop of protein that covers the site that actually binds to CD4. The site that binds to CD4 is the only conserved structure in the gp120. The rest of it can be anything and that fools the Ab that the host produces. If you get an Ab that binds to that special site where the CD4 and gp120 bind to each other then that can neutralize the virus. That Ab can prevent the virus from infecting other cells. Most Ab don’t bind to that site because the B cells cannot see it because that site on the intact protein are covered up by other parts of the intact protein. This chemokine receptor interaction is thought to function in opening up of that site to allow the virus to bind better to CD4 and then the gp120 is the molecule that sticks a syringe into the lipid bilayer and shoots the RNA into the inside of the cell and then the infection proceeds. e. [S10] There are two kind of coreceptors. One is CCR5 and then other is CXCR4. 1. CXCR4 has one ligand called SDF1 and that is the only ligand that binds to that cytokine and it is on a lot of different cells particularly T cells. 2. Macrophages have a fair amount of CCR5, but T cells tend to have to be activated in order to express CCR5 early on these were called T tropic viruses tend to use one or the other of these receptors, but they can mutate and go back and forth in a particular viral isolate. 3. There is an example of a particular viral mutation a deletion of 32 base pairs in the middle of the CCR5 allele that is relatively common in Caucasians of central European decent. The allele frequency is about 16% and homozygotes are maybe 1-2% of the population. If one is homozygous for delta 32 of the CCR5, the first result is that you are not sick, it is an asymptomatic mutation although it is a homozygous defect. But, those individuals are almost completely resistant to being infected with HIV. It was discovered when a couple of individuals came into a New York City clinic claiming that all of their friends were dead of HIV and that they had been exposed multiple times, but failed to ever test positive. From these individuals, they found this defect. The cytokine receptor seems to be involved in the response to cholera. People that have this mutation may be more resistant to getting severe diarrhea and cholera. It is thought that this defect was selected for when the cholera epidemic swept through Europe similarly to how heterozygous sickle cell trait protects someone from malaria. The CCR5 gene was not sitting around waiting to be protective against HIV, but it suggests that people cannot be infected from the CXCR4. If you are a mutant and have just the one co-receptor you can’t get infected with the virus that grows with the other co-receptor. A nurse in San Francisco got a needle stick from a patient that was dying from HIV and had a T tropic virus that used the CXCR4, but when she first got viremic about 2-3 weeks later she actually had the other co-receptor using virus so the virus had mutated to grow out in that individual to the other type and both the virus in her and the virus in the patient she got stuck with were completely sequenced and it was totally clear that that was the one she got infected with and yet that was the mutation at that one site so early infection for whatever reason seems to depend primarily or almost exclusively on the CCR5 co-receptor. f. [S11] One of the things about retroviruses is that there is a latent infection 1. Latent has two meanings. a. Latent means that it is there, but obvious. Clinical latency is when you have the infection but you don’t have symptoms. From a cell biology standpoint there is also latency and that is FUN2: 11:00-12:00 Monday, October 20, 2008 Dr. Bucy Scribe: Teresa Kilborn Proof: Ashley Holladay Immunology Page 4 of 6 where the cell is infected but it is not producing virions actively. There are two kinds of that latency. i. One is called pre-integration latency which is after reverse transcription and therefore the cDNA is present in the cell. If you measure the DNA of the virus then that cell is infected if it has the viral DNA. Viral RNA doesn’t really count because the virions have the RNA and they can just be stuck on the cell and not really effecting the cell. So only the DNA really marks an infected cell. But if the DNA is not integrated into the chromosome, it cannot make more infectious virus so this doesn’t count in the sense of propagating the infection. ii. The really bad news part of HIV is the integrative latent part of the virus. That is where the virus is integrated into the chromosome, but it is not transcriptionally active. It is not making viral proteins. This is a very rare or uncommon circumstance, but it is established very early on in the infection and probably this fact that there are these latently infected CD4 T cells is the major reservoir of infection. You are probably aware that if you have HIV you can take these different cocktails of drugs and they work because they block viral replication, but you can go for a long period of time with undetectable virus. But if you stop taking the drugs then the viral infection almost always comes back. Where it comes back from is the idea of the reservoir and probably this population of latently infected cells which maybe account for 10^5- 10^6 cells in your whole body. Whereas in every mL of blood there are more T cells than that. Throughout your whole body that really isn’t that many. There are about 10^1210^13 T cells in your body so 10^5 latently infected cells is a very tiny fraction. g. Another trick of HIV, that is uncommon among infections, is an extremely high viral mutation rate. [S12] 1. It occurs from two places. One, the reverse transcriptase is a sloppy enzymes that makes a lot of mistakes that don’t hammer the virus very bad because just one effective infection generates another infection. It is like a dandelion that doesn’t care how many seeds it makes. It just needs to make one that will make a lot more seeds so the population can be continued. 2. Secondly, the enzyme that generates the RNA from DNA is also not a high fidelity enzyme. The RNA particles that are packaged in the virus are made by the host enzyme. For mRNA, if you make a 1000 mRNA that make a protein, if one of those mRNA has a defect in it, that is not a big deal. But if that one molecule gets packaged into a virus and that particular mutation allows it to escape the action of a drug, then that turns out to be a big deal. The virus is very rapidly evolving in terms of the sequence. It is estimated that there is about 1000 different variations in the sequences of the virus in any one individual at any given time. 3. There are a lot of subtle genetic forms of the virus which means that there are sequences that are waiting to grow out when drug therapy comes out for them to escape that particular drug interaction. h. [S13] The diagnosis of DNA can be made at the primary infection of HIV, but usually is not. 1. Most people don’t have a very symptomatic primary infection, but it is made during the latent phase by measuring Ab made to the virus. You can measure the viral RNA in plasma but that assay is more expensive. If you have Ab that are positive for the virus they are confirmed by a Western Blot which is a procedure in which proteins are run out on a gel and separated by molecular weight and then the Ab are tested if they bind proteins of particular weights. If you bind gp120 and gp24, two proteins that are characteristic of HIV, then that confirms that it is HIV. Sometimes, rarely you can have reactivity in the first test but it is actually cross reactivity and it is not actually HIV, so it is confirmed with Western blot test. 2. If you are exposed with a needle stick or some blood exposure to someone that has HIV you can be treated with prophylactic anti-viral therapy and that is supposedly very effective in preventing the new infection. Most places have a rapid response program if you do get a needle stick from someone who has HIV. You can take anti-viral drugs for a month and that can block the infection. i. [S14] The Ab testing is used to diagnosis the infection. P24 was earlier used to monitor to detect the virus in the blood but has changed to focus on viral RNA. The extent of viremia, which is a measure of the amount of virus in the blood, is a measure of the rate of progress of the virus. The CD4 T cells are the cells that are infected and they are depleted over time with the virus. The classic model is that HIV is a train heading down a track towards a cliff. The CD4 count is a measure of how far on the track you are to the cliff. The lower the CD4 count, the closer you are to the cliff or the end stage. The viral load is like how fast the train is moving. So if you stop the train from moving by treating the patient with antiviral drugs you can stop the train just before the cliff or way back and you are still on the track. On the other hand, the closer you get, the more likely you are to fall off the cliff. Furthermore the faster you are moving, the shorter amount of time it takes before the CD4 count FUN2: 11:00-12:00 Scribe: Teresa Kilborn Monday, October 20, 2008 Proof: Ashley Holladay Dr. Bucy Immunology Page 5 of 6 depletion. High viral load correlates with rapid decrease of CD4. Low viral load, CD4 isn’t depleted as quickly. Because the virus can mutate, oftentimes people become resistant to the treatment they are on. Laboratory testing can determine which drugs the virus is resistant to or susceptible to so the drugs that should be used next can be determined from this. i. [S15] These days you should always treat any human bodily fluids as if they were contaminated with HIV, TB, or Hepatitis even though most people are not. If you do get a needle stick at UAB there is a hotline number to call and the treatment is if the suspicion is high for HIV you can be treated with anti-viral drugs. If that treatment is initiation within a couple of days, it is extremely effective. If you wait a few weeks, it probably won’t be as good, so it is important to take immediate action. ii. [S16] 1. Acute infection syndrome occurs within a few weeks of the infectious episode and has symptoms similar to the flu. Sometimes people have swollen lymph nodes, sore throat, or a rash. Less than ½ of the individual infected can remember even having such an event. When people are detected it is usually long after such acute episode. Studies have been done to track down people with such symptoms and then characterize their symptoms to learn about it, but most people are completely missed at this stage. 2. The clinically latent period of the infection has very few symptoms. The viral load or the amount of the virus in the blood measures how fast the disease is progressing. The amount of CD4 T cells tells how far the disease has progressed. 3. The end stage of the disease is marked by CD4 T cell count dropping below 200 cells/mL of blood. The normal count is around 1000, but this varies. Therefore the end stage is when 80% of the CD4 T cells have been killed. The immune system begins to decompensate because the CD4 T cells are needed to control immune response and when you go below that number you start to get opportunistic infections and that is what kills you. Untreated, the median survival of the end stage of the disease is 12-18 months. So the idea that HIV infection is as being always fatal was characterized when treatment was not available and when the disease was already in the end stage. j. [S17] The chart plots the number of CD4 T cells versus viral load. In acute infection you have a rapid rise in the virus and then decrease when you have an immune response, but it does not go completely away. It stays fairly stable for a long period of time. Notice one is in weeks and the other years. People that are at the top have a faster decline of CD4 cells, but if you maintain a viral level below 5000, disease progression is very slow. Then when you get to a critical point of CD4 cells, the viral level goes up because the immune response is decompensating and the virus is growing out. The decrease in CD4 cells speeds up. People can get down to around 10 CD4 T cells and then they are really susceptible to opportunistic infections. k. [S18] Exactly what is going on during the clinically latent period is not exactly clear or what maintains the low viral load. This cartoon shows what are thought to be responsible for the destruction of CD4 T cells. 1. Probably the main one is the mechanism in the middle. T cells not infected are trying to make an immune response and die. 2. The mechanism at the far right definitely occurs and may be the key mechanism by which CD4 T cells are killed. The virally infected cells are recognized by the immune system and killed because they are infected. 3. Whether the mechanism at the far left occurs in vivo is still unclear. 4. The upshot is CD4 T cells is that they are more like neurons than myeloid cells in that when they die they are dead and are not reconsituted. T cells are produced by the thymus which starts to fade away after the age of 3. People who are 70 only have 2-3% of thymic activity. So if you kill CD4 T cells then that specificity is lost and the only place they can come back from is the thymus. The thymus can divide and make new cells but in general one of the daughter cells dies and one lives, they can change their function but they don’t generate new receptors. This leads to a defective immune system. l. [S19] Once the immune system is defective, you can have all types of infections and neoplasms such as kaposi sarcoma which is actually a viral infection of endothelial cells with a virus called HHV8 and it grows like a cancer because that infection grows locally. Because you can’t kill the virally infected cells you get a neoplastic lesion. Non-Hodgekin’s lymphoma are fairly common because of an infection of a virus, Epstein barr virus which can infect B cells and cause lymphomas and if you don’t have an immune system to block that kind of viral infection you can get these lymphomas but a number of infections listed here: pheumocystosis is fairly common, candidiasis that causes thrush or mucosal infection of the throat, viral infection such as cytogegalovirus that can cause C and B retinitis as a major complication and end stage HIV disease as well as pulmonary and other manifestations. FUN2: 11:00-12:00 Scribe: Teresa Kilborn Monday, October 20, 2008 Proof: Ashley Holladay Dr. Bucy Immunology Page 6 of 6 m. [S20]When you take any anti-viral medication there is a very rapid drop in plasma viral load and the rate initially of the fall is very rapid and exponential and what that shows is the virus is constantly infecting new cells and if you just block new cells from being infected, the total amount of virus falls rapidly. The ½ life of a cell infected with HIV is only about 1 day at chronic infection. Those who have high viral load and low viral load all fall at about the same rate so the viral load correlates with the number of virally infected cells and each cell acts autonomously dying at the same rapid rate. But on average each cell makes a virion at infects one new cell and that process happens once every day and slowly grinds down the population of CD4 cells. n. [S21] If you treat with anti-retroviral drugs, not only is there a drop in virus, but there is a rapid increase in the number of CD4 T cells in the blood initially. That is because there is an inflammation in the lymphoid tissues and there are cells that are sequestered in the lymph nodes and spleen that are not normally in the blood. When you resolve the active infect the T cell re-equilibrate and you have an increase in the blood but that increase only lasts a couple weeks. Then you get a constant number and after that there is not much further improvement. You are not susceptible to any opportunistic infection after being treated with any anti-retroviral drug which means that the viral replication or viremia is quite immunosuppressive per se and if you just get rid of the viral replication then the immune system is largely reconstituted at least with respect of getting an opportunistic infection. o. [S22] Despite initially optimism, if you maintain therapy for a long period of time, you don’t kill off the virus. There is a reservoir of infection, probably latent infection, that are able to replicate virus even in the presence of drug at a low rate resulting in the redevelopment of active infection if the drugs are stopped. When growth is low there is slow evolution of the virus into different species variations (quasi species). In order to select and fix a mutation you have to have growth. If there is no growth, there is no room for sequences to grow out and you don’t get sequence evolution. The worst thing is to take a little bit of the drug. If you are not taking any of the drug than there is nothing for the virus to select against. The right amount of drug and there is no growth. Too little, and the drug is there to select mutants but not to block the growth. A little bit of the drug in the presence of the virus is the worst recipe. Study of prisoners in Florida where direct observed therapy was used (nurse would give the prisoner the drug to take and observe them taking it) showed no resistant strains of virus over two years. In clinical trial populations where you tell patients to take the medications or they will die, 15-20% of them don’t take the medications and that’s what happens to them. Non-adherence to the regime is the main reason for resistance development. p. [S23] The goal of HIV therapy is to treat the infection and keep viral replication low which leads to low mutation rate and monitor CD4 levels and viral load. If the viral load goes up on therapy that shows resistance development and the approach is usually to switch drugs. The idea that one could eradicate the infection is a dashed hope. Ten years ago there were people that reasonably opportunistic, but now no one really thinks that is possible. The thought of inducing low replication with drugs but immunizing people with drugs to get immune control is still a viable alternative, but hasn’t worked out get. He believes that this is because they are not many good vaccines to immunize people with HIV.