* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Document
Survey
Document related concepts
Remote ischemic conditioning wikipedia , lookup
Coronary artery disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Rheumatic fever wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Heart failure wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
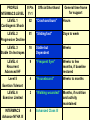
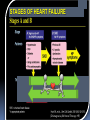
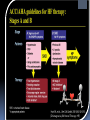
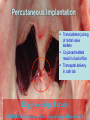
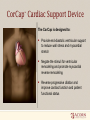
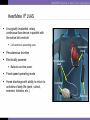
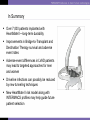
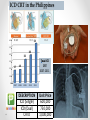
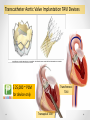
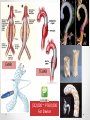
Heart Failure Surgery The Last Frontier Gerardo S. Manzo, MD, FPCS, FPCC Bringing Global Trends in Cardiology Closer to Home PHA Convention 26 May 2012 et al. Circulation 2006;113:e684-e685 Copyright © American Heart Association STAGES OF HEART FAILURE (Divinagracia,RA Novel Therapy HF) (Divinagracia,RA Novel Therapy HF) STAGES OF HEART FAILURE (Divinagracia,RA Novel Therapy HF) (Divinagracia,RA Novel Therapy HF) Stage D : Refractory HF Therapy • • • • All Stage A, B and C Mechanical assist devices Heart transplantation Continuous IV inotropic infusion for palliation • Hospice care Surgical Options for the Failing Ventricle PHA Annual 2005 GSManzo Transmyocardial Revascularization (laser) End-to-End Mitral Repair (Everest Clip/ Alfieri) Cardiomyoplasty CorCap Cardiac Support Device (mesh) Coapsys LV Support Device (intracavitary rod) Partial Left Ventriculectomy (Batista) Stem Cell Therapy ??? Mechanical Circulatory Support Devices Heart Transplantation Percutaneous Implantation Transcatheter joining of mitral valve leaflets Co-joined leaflets result in dual orifice Transeptal delivery in cath lab Edge-to-Edge Repair 5th Annual Heart Failure Convention March 08 GSM EVEREST (Endovascular Valve Edge-to-Edge REpair Study) CorCap Cardiac Support Device ™ The CorCap is designed to: Provide end-diastolic ventricular support to reduce wall stress and myocardial stretch Negate the stimuli for ventricular remodeling and promote myocardial reverse remodeling Reverse progressive dilation and improve cardiac function and patient functional status Annuloplasty : Transventricular / Transatrial / Epicardial Approach Intracavitary shortening rod connecting two external pads to shorten septolateral dimension of LV and mitral annulus 5th Annual Heart Failure Convention March 08 GSM Myocor Surgical Coapsys System Surgical Approaches to Heart Failure HFSA 2010 Recommendations HFSA 2010 Practice Guideline Surgery Recommendation 10.1 It is recommended that the decision to undertake surgical intervention for severe HF be made in light of the following: Functional status Prognosis based on severity of underlying HF co-morbid conditions. Procedures should be done at centers with the following: Demonstrable expertise Multidisciplinary medical and surgical teams experienced in the selection, care, and perioperative and long-term management of high risk patients with severe HF Strength of Evidence = C Lindenfeld J, et al. HFSA 2010 Comprehensive Heart Failure Guideline. J Card Fail 2010;16:e1-e194. HFSA 2010 Practice Guideline Heart Transplantation Recommendation 10.2 Evaluation for heart transplantation is recommended in selected patients with the following: severe HF debilitating refractory angina or ventricular arrhythmia that cannot be controlled despite drug, device or alternative surgical therapy. Strength of Evidence = B Lindenfeld J, et al. HFSA 2010 Comprehensive Heart Failure Guideline. J Card Fail 2010;16:e1-e194. HFSA 2010 Practice Guideline Mitral Valve Repair or Replacement Recommendation 10.3 Isolated mitral valve repair or replacement for severe mitral regurgitation secondary to ventricular dilatation in the presence of severe LV systolic dysfunction is not generally recommended. Strength of Evidence = C Lindenfeld J, et al. HFSA 2010 Comprehensive Heart Failure Guideline. J Card Fail 2010;16:e1-e194. HFSA 2010 Practice Guideline Surgery Recommendation 10.4 “Batista Procedure” Partial left ventricular resection is not recommended in nonischemic cardiomyopathy. Strength of Evidence = B Lindenfeld J, et al. HFSA 2010 Comprehensive Heart Failure Guideline. J Card Fail 2010;16:e1-e194. HFSA 2010 Practice Guideline Mechanical Support Recommendation 10.5 Patients awaiting heart transplantation who have become refractory to all means of medical circulatory support should be considered for a mechanical support device as a bridge to transplant. Strength of Evidence = B Lindenfeld J, et al. HFSA 2010 Comprehensive Heart Failure Guideline. J Card Fail 2010;16:e1-e194. HFSA 2010 Practice Guideline Permanent Mechanical Assistance Recommendation 10.6 Permanent mechanical assistance using an implantable assist device may be considered in highly selected patients with severe HF refractory to conventional therapy who are not candidates for heart transplantation, particularly those who cannot be weaned from IV inotropic support at an experienced HF center. Strength of Evidence = B Lindenfeld J, et al. HFSA 2010 Comprehensive Heart Failure Guideline. J Card Fail 2010;16:e1-e194. HFSA 2010 Practice Guideline “Bridge to Decision” Recommendation 10.7 (NEW in 2010) The following patients should be considered for urgent mechanical circulatory support as a “bridge to decision”: Patients with refractory HF and hemodynamic instability and/or compromised end-organ function with relative contraindications to cardiac transplantation or permanent mechanical circulatory assistance, who are expected to improve with time or restoration of an improved hemodynamic profile These patients should be referred to a center with expertise in the management of patients with advanced HF Strength of Evidence = C Lindenfeld J, et al. HFSA 2010 Comprehensive Heart Failure Guideline. J Card Fail 2010;16:e1-e194. The Role Of INTERMACS in Patient Selection LongerUse Term Forfor Extended / DurableCirculatory Support Mechanical Lynne Warner Stevenson Investigational indications will be discussed No conflicts related to MCS INTERMACS: Patient Selection Patient Profile/ Status: INTERMACS Levels 1. Critical cardiogenic shock 2. Progressive decline 3. Stable but inotrope dependent 4. Recurrent advanced HF 5. Exertion intolerant 6. Exertion limited 7. Advanced NYHA III PROFILE NTERMACS LEVEL # Pts Yr 1 Official Shorthand General time frame for support LEVEL 1 Cardiogenic Shock 82 “Crash and burn” Hours LEVEL 2 Progressive Decline 81 “Sliding fast” Days to week LEVEL 3 Stable On Inotropes 18 Stable but Dependent Weeks LEVEL 4 Recurrent Advanced HF 9 “Frequent flyer” Weeks to few months, if baseline restored Level 5 Exertion Tolerant 4 “Housebound” Weeks to months LEVEL 6 Exercise Limited 3 “Walking wounded” Months, if nutrition and activity maintained INTERMACS Advance NYHA III 4 Advanced Class III The Fourth INTERMACS Annual Report: 4,000 implants and counting James K. Kirklin, MD, David C. Naftel, PhD, Robert L. Kormos, MD, Lynne W. Stevenson, MD, Francis D. Pagani, MD, PhD, Marissa A. Miller, DVM, MPH, J. Timothy Baldwin, PhD and James B. Young, MD The Journal of Heart and Lung Transplantation Volume 31, Issue 2, Pages 117-126 (February 2012) DOI: 10.1016/j.healun.2011.12.001 Copyright © 2012 Terms and Conditions Figure 4 Source: The Journal of Heart and Lung Transplantation 2012; 31:117-126 (DOI:10.1016/j.healun.2011.12.001 ) Copyright © 2012 Terms and Conditions Figure 10 Source: The Journal of Heart and Lung Transplantation 2012; 31:117-126 (DOI:10.1016/j.healun.2011.12.001 ) Copyright © 2012 Terms and Conditions Device Strategy 1. Bridge to Recovery (BTR) 2. Bridge to “Decision” 3. Bridge to a Bridge 4. Bridge to Transplant (BTT) 5. Destination Therapy 6. Rescue Therapy The CentriMag & PediVas: Magnetically Levitated Pumps for ECMO & VAD’s; Neonates to Adults Stephen Harwood, CCP, CPC, BA CentriMag & PediVas CentriMag® System Components Pump Motor Console Indications The CentriMag and PediVas pumps are classified as short term devices (30 days) Are often used as a ‘bridge’ from one point in treatment to another They are well suited in the critical setting because they are extremely easy to institute They have been widely used as ventricular support devices, but also are popular in ECMO /ECLS circuits as well Longest duration : 304 days followed by HeartMate II Contemporary Outcomes With the HeartMate II® LVAS David J. Farrar, PhD Vice President, Research and Scientific Affairs Thoratec Corporation J138-0711 HeartMate II® LVAS A surgically implanted, rotary continuous-flow device in parallel with the native left ventricle Left ventricle to ascending aorta Percutaneous driveline Electrically powered Batteries and line power Fixed-speed operating mode Home discharge with ability to return to activities of daily life (work, school, exercise, hobbies, etc.) Implantable Pump Percutaneous Lead Controller Batteries HeartMate II—Indications for Use HeartMate II is the first and only FDA-approved continuous-flow device for both Bridge-to-Transplantation (BTT) and Destination Therapy (DT). Bridge-to-Transplantation Risk of imminent death from nonreversible left ventricular failure Candidate for cardiac transplantation Destination Therapy NYHA Class IIIB or IV heart failure Optimal medical therapy 45 of last 60 days Not a candidate for cardiac transplantation Clinical Outcomes Based on INTERMACS Profile Length of Stay Post-VAD Actuarial Survival Post-VAD Less acutely ill, ambulatory patients in INTERMACS profiles 4–7 had better survival and reduced length of stay compared to patients who were more accurately ill in profiles 1–3. Group 1: INTERMACS 1 Group 2: INTERMACS 2–3 Group 3: INTERMACS 4–7 Boyle, Ascheim, Russo, et al. JHLT. 2011;30:4. Contemporary Destination Therapy Results Park SJ. AHA Scientific Sessions, November 2010. In Summary Over 7,000 patients implanted with HeartMate II—long-term durability Improvements in Bridge-to-Transplant and Destination Therapy survival and adverse event rates Adverse-event differences in LVAD patients may lead to targeted approaches for men and women Driveline infections can possibly be reduced by new tunneling techniques New HeartMate II risk model along with INTERMACS profiles may help guide future patient selection Stage D : Refractory HF Therapy • • • • All Stage A, B and C Mechanical assist devices Heart transplantation Continuous IV inotropic infusion for palliation Is Device Therapy • Hospice care unaffordable for Filipino patients? About 250,000 Americans each year have an ICD implanted at the cost of about $100,000 each. Weisfeldt, Myron L., and Susan L. Zeiman. "Advances in the Prevention and Treatment of Cardiovascular Disease: One of the most important contributors to improved human survival is the treatment of cardiovascular disease". Health Affairs. Vol. 26, No. 1, pp. 2537 January 2007 ICD CRT in the Philippines 54 60 50 38 40 32 Total Series1 ICD CRT 2007-2011 30 20 17 18 2007 1 2008 2 10 0 2009 3 2010 4 2011 5 DESCRIPTION ICD (Single) ICD (Dual) CRTD Unit Price 600,000 750,000 1,000,000 Over 40,000 TAVI as of Nov 2011 First procedure by Alain Cribier in France 2002 Transcatheter Aortic Valve Implantation TAVI Devices Transfemoral TAVI $ 25,000 ~ P1M for device only Transapical TAVI EVAR TEVAR $12,000 ~ P 500,000 For Device CentriMag® System Components Pump $10,500 ~ P 590,000 For Patient Device Motor Console $70,000 ~ P 3.9M For Hospital HEART TRANSPLANTATION Overall ISHLT 2011 J Heart Lung Transplant. 2011 Oct; 30 (10): 1071-1132 NUMBER OF HEART TRANSPLANTS REPORTED BY YEAR 5000 4000 Other Europe North America 3500 3000 2500 2000 1500 1000 500 0 19 82 19 83 19 8 19 4 85 19 86 19 87 19 88 19 8 19 9 90 19 91 19 92 19 93 19 94 19 9 19 5 96 19 97 19 98 19 99 20 00 20 0 20 1 02 20 03 20 04 20 05 20 0 20 6 07 20 08 20 09 Number of Transplants 4500 ISHLT 2011 J Heart Lung Transplant. 2011 Oct; 30 (10): 1071-1132 NOTE: This figure includes only the heart transplants that are reported to the ISHLT Transplant Registry. As such, the presented data may not mirror the changes in the number of heart transplants performed worldwide ADULT HEART TRANSPLANTATION Kaplan-Meier Survival by Era (Transplants: 1/1982 – 6/2009) 100 1982-1991 vs. 1992-2001: p = 0.8460 1982-1991 vs. 2002-6/2009: p < 0.0001 1992-2001 vs. 2002-6/2009: p < 0.0001 Survival (%) 80 60 1982-1991 (N=20,504) 40 1992-2001 (N=36,879) 2002-6/2009 (N=22,477) 20 HALF-LIFE 1982-1991: 10.2 years; 1992-2001: 10.7 years; 2002-6/2009: NA 0 0 1 2 ISHLT 3 4 5 6 7 8 Years 2011 J Heart Lung Transplant. 2011 Oct; 30 (10): 1071-1132 9 10 11 12 13 14 15 ADULT HEART RECIPIENTS Cross-Sectional Analysis Functional Status of Surviving Recipients (Follow-ups: 1995 - June 2010) 100% 80% 60% 40% 20% No Activity Limitations Performs with Some Assistance Requires Total Assistance 0% 1 Year (N = 16,087) ISHLT 3 Years (N = 14,235) 2011 J Heart Lung Transplant. 2011 Oct; 30 (10): 1071-1132 5 Years (N = 12,181) ADULT HEART RECIPIENTS Employment Status of Surviving Recipients Age at Follow-up: 25-55 Years (Follow-ups: 1995 - June 2010) 100% 80% Retired Not Working 60% Working Part Time 40% Working Full Time Working (FT/PT status unknown) 20% 0% 1 Year (N = 9,115) ISHLT 3 Year (N = 6,967) 5 Year (N = 5,163) 2011 J Heart Lung Transplant. 2011 Oct; 30 (10): 1071-1132 ADULT HEART RECIPIENTS Rehospitalization Post-transplant of Surviving Recipients (Follow-ups: 1995 - June 2010) 100% 80% 60% 40% 20% No Hospitalization Hospitalized: Rejection Only Hospitalized: Rejection + Infection Hospitalized: Not Rejection/Not Infection Hospitalized: Infection Only 0% Up to 1 Year Between 2 and 3 Years (N = 26,546) (N = 22,651) ISHLT 2011 J Heart Lung Transplant. 2011 Oct; 30 (10): 1071-1132 Between 4 and 5 Years (N = 19,481) Global Burden of Heart Disease Global Burden of Heart Disease Focused on Prevention & Risk Modification o genetic susceptibility o marked environmental changes usually secondary to • urbanization • increasing affluence • influences from early childhood to adulthood. Individual Burden of Heart Failure Direct Costs of Care o Inpatient : Frequent Re-hospitalization o Rehabilitation o Follow-up care o Cost of Devices Indirect Costs o Loss of employment o “Medicare” benefits o Family expenses Heart Failure Surgery in the Philippines • Create Multidisciplinary medical and surgical teams experienced in the selection, care, and perioperative and long-term management of high risk patients with severe HF • Implement evidence based HF therapies • Develop expertise on appropriate surgical procedures for HF • Increase patient awareness on available treatment options We need to stop condemning our Stage D Heart Failure patients… …and conquer the last frontiers of Philippine cardiology... THANK YOU