* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Antiinflammatory Drugs
Survey
Document related concepts
Pharmacogenomics wikipedia , lookup
Discovery and development of ACE inhibitors wikipedia , lookup
Pharmacognosy wikipedia , lookup
Neuropharmacology wikipedia , lookup
Plateau principle wikipedia , lookup
Discovery and development of integrase inhibitors wikipedia , lookup
Development of analogs of thalidomide wikipedia , lookup
Drug interaction wikipedia , lookup
Hyaluronic acid wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Discovery and development of cyclooxygenase 2 inhibitors wikipedia , lookup
Transcript
Anti-inflammatory
Drugs
# Lab 4 #
Inflammation:
• it is a biological response of vascular
tissues to harmful stimuli, such as
pathogens, damaged cells, or
irritants.
• Inflammation may ends with either :
Complete healing
of tissues
Permanent destruction
of tissues
Signs of inflammation
• Redness:
Due to vasodilatation by effects of
releasing of histamine, bradykinin
and prostaglandin.
• Hotness:
Due to increased blood flow.
Signs of inflammation
• Swelling:
due to increased vascular
permeability by the released
mediators and increased the exudate
in the inflammed area
• Pain:
due to irritation of nerve ending by
inflammation and the pressure of the
swelling on the nerve ending.
• Inflammatory mediators:
– histamine
– 5-HT (serotonin)
– Bradykinin
– Prostaglandins (eg PGE2 )
– Interleukines
– Substance P
– Nitrous oxide
Main
inflammatory
mediator
Phases of
Inflammation
• Fluid phase (vascular phase):
Increased vasodilatation leads to
increased permeability of the vascular
bed to plasma protein.
- Increasing fluid will help in:
1- dilution of the irritant
2- increase conc. of antibodies from blood
to inflamed area
3- supply nutrients to the immune cells.
Phases of
Inflammation
• Cellular phase (exudative
phase):
Involves migration of tissue
macrophages and
polymorphonuclear leukocytes
(PMNL) to the inflamed area.
• Fibrous phase (proliferative
phase):
A new connective tissue (fibrous)
Classification of the
Inflammation
• Non – immunological :
Induced by chemical irritants such as formalin
• Immunological :
Induced by infections such as bacterial infection
Anti-inflammatory
Drugs
Steroidal
- Cortisone
- Hydrocortisone
Non-steroidal
- Acetaminophen
- Aspirin
Steroids (SAIDs)
- Containing steroid moiety in their sturcure
Glucocorticoids (GC)
Cortisone
Glucocorticoids (GC)
Synthetic
Natural
- Cortisone
- Hydrocortisone
Fluorinated
Glucocorticoids
- Betamethasone
- Dexamethasone
- Predinsone
Liver enzymes
Prednisolone
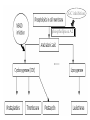
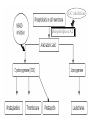
Glucocorticoids (GC)
Mechanism of Action :
- They act by indirect inhibition of the enzyme phospholipase A2
which activate synthesis of arachidonic acid with subsequent
formation of prostaglandins.
- They induce synthesis of a protein “lipocortin-1” which has
the inhibitory effect on phospholipase A2.
GC inhibition
phospholipase A2
Side Effects :
• Immunosuppression
• Hyperglycemia due to increased gluconeogensis, insulin resistance, and
impaired glucose tolerance ("steroid diabetes");
• Steroid-induced osteoporosis: reduced bone density (osteoporosis,
• Osteoporosis , higher fracture risk, slower fracture repair)
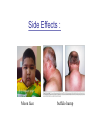
• Redistribution of body fat: moon face, buffalo hump and truncal obesity.
• Adrenal insufficiency
• Muscle breakdown (proteolysis), weakness; reduced muscle mass and repair
• Anovulation, irregularity of menstrual periods
• Growth failure, pubertal delay
• Increased plasma amino acids, increased urea formation;
• Glaucoma due to increased cranial pressure
Side Effects :
Moon face
buffalo hump
Non-Steroidal Anti-inflammatory Drugs
(NASID)
• They don’t contain steroid moiety
• They also have analgesic and antipyretic activity
Mechanism of Action :
• NSAIDs inhibit synthesis of PGs which are the main factors
Playing a role in the inflammaltion.
• Inhibit synthesis of PGs through inhibition of cyclooxygenase
Enzymes which are responsible for production of PGs
GC inhibition
phospholipase A2
Cyclooxygenese ( COX ) Isoforms :
COX 2
COX 1
- Constitutive
- Many tissues ( blood vessels
stomach and kidney )
COX 3
- inducible
-By inflammatory processes
and mediators
has recently been described
Non-Steroidal Anti-inflammatory Drugs
(NASID)
Non-selective
COX inhibitors
- Aspirin
- Ibuprofen
- Diclofenac
- Meloxicam
selective COX2
inhibitors
- Celecoxib
- Rofecoxib
Side Effects :
• Unwanted effects, owing largely to inhibtion of COX1
Particularly in the elderly and include :
- Despepsia, nausea and vomiting , ulceration and gastric
damage in chronic users, with risk of hemorrhage
- Reversible renal insufficiency
- Analgesic-associated nephropathy ( irreversible )
- Liver disorders, in high doses, e.g. acetaminophen
Measurement the activity
of
anti-inflammatory drugs
- Method :
Paw Oedema Method
- Principle :
induction a chemical inflammation
by injecting an irritant ( formalin ) into
rat’s paw
- Objective :
measure the anti-inflammatory activity of
diclofenac and hydrocortisone with
different doses )
-Procedure :
1- select 5 rats
2- inject each rat 1 ml urethane for anesthesia.
3- select one as control and inject the rest of them intraperitoneal
rat 1 >>> control
rat 2 >>> 40 mg/kg diclofenac
rat 3 >>> 80 mg/kg diclofenac
rat 4 >>> 20 mg/kg hydrocortisone
rat 5 >>> 40 mg/kg hydrocortisone
4- after 1 hr , inject 0.1 ml formalin in each rat ( 2 to 5 ) into
their paws >>> to induce inflammation.
5- after 1 hr , take the reading using the plythysmometer of each
rat paw ( right and left ).
6- calculate the inflammation and response % for each drug.
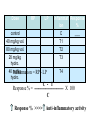
Dose
RP
LP
control
40 mg/kg vol.
80 mg/kg vol.
20 mg/kg
hydro.
40 Inflammation
mg/kg
= RP - LP
hydro.
inflammat Response
ion
%
C
___
T1
T2
T3
T4
C - T
Response % = ــــــــــــــــــــــــــــــــــــــــX 100
C
Response % >>>> Anti-inflammatory activity