* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Understanding its origins and mechanism of action
Survey
Document related concepts
Point mutation wikipedia , lookup
Genetic code wikipedia , lookup
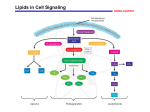
Lipid signaling wikipedia , lookup
Nucleic acid analogue wikipedia , lookup
Peptide synthesis wikipedia , lookup
Enzyme inhibitor wikipedia , lookup
Catalytic triad wikipedia , lookup
Metalloprotein wikipedia , lookup
Fatty acid metabolism wikipedia , lookup
Citric acid cycle wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
Biochemistry wikipedia , lookup
Amino acid synthesis wikipedia , lookup
Butyric acid wikipedia , lookup
Biosynthesis wikipedia , lookup
15-Hydroxyeicosatetraenoic acid wikipedia , lookup
Transcript
Not intended for US or UK use Acetylsalicylid acid – the active ingredient in Aspirin®: Understanding its origins and mechanism of action The origins of aspirin go back to ancient times. Greek physician Hippocrates (460–377 B.C.) was aware of the analgesic properties of willow bark juice, as was the Father of Botany Theophrastus (372–287 B.C.). While the therapeutic properties of the willow were forgotten by the medical profession of the Middle Ages, it continued to play an important role in popular medicine. Herb specialists boiled up willow bark and gave their suffering patients the bitter concoction. Not until 1763 did Reverend Edward Stone give a report to the British Royal Society on experiments with salix bark extract conducted on 50 fever patients. In 1829, salicin was crystallized by the French pharmacist, Pierre Joseph Leroux, and the Italian chemist Raffaelle Piria further processed it into salicylic acid. By the end of the 19th century, scientists were looking for a way to make salicylic acid (Fig. 1) more tolerable. This approach was first successful in 1897: Legend has it that at Bayer’s pharmaceutical laboratories, the young chemist Dr. Felix Hoffmann’s father had been tortured by the pain of rheumatism for years, and Hoffmann wanted to help him. The sodium salicylate used in his father’s therapy caused nausea because of its offensive taste, so Hoffman looked for a method of modifying salicylic acid to make it more tolerable. He was finally successful when he chose acetylation: He was able to synthesize chemically pure and stable acetylsalicylic acid, or “aspirin” (Fig. 2). By esterifying salicylic acid, the substance became more tolerable and less aggressive towards mucosal membranes. For a long time, scientists believed that acetylsalicylic acid inhibited pain by influencing the central nervous system. Then, in 1971, the British pharmacologist Sir John Vane and his research team demonstrated that aspirin actually inhibits the formation of certain - 1/3 - prostaglandins and thromboxanes.1 Prostaglandins and thromboxanes are hormone-like substances responsible for different processes in the body. Prostaglandins are mediators of pain, fever and inflammation; thromboxanes are mediators of platelet aggregation. They are derived from an essential fatty acid called arachidonic acid with the help of the enzyme cyclooxygenase (COX). COX is available in two isoforms, COX-1 and COX-2. Aspirin inhibits both the enzymes cyclooxygenase 1 (COX-1) and cyclooxygenase 2 (COX2). By adding an acetyl group (−C(O)CH3) to an amino acid residue, the COX enzymes lose their ability to transform arachidonic acid into prostaglandins. This has the effect of blocking the channel in the enzyme and arachidonic acid cannot enter the active site of the enzyme. By inhibiting this enzyme, the synthesis of prostaglandins is blocked. To produce more prostaglandins, the body has to form new COX enzymes that are not affected by aspirin, a process that may take several days. In pain relief, aspirin inhibits COX-2 by blocking the active site of the enzyme due to irreversible acetylation, and also by a reversible salicylate blockade. Consequently, this prevents the synthesis of prostaglandins from arachidonic acid reducing pain, fever and inflammation. In cardiovascular event prevention, aspirin inhibits COX-1 in platelets also by blocking the active site of the enzyme due to irreversible acetylation. Again, arachidonic acid cannot enter the active site of the enzyme and as a result, aspirin can reduce platelet aggregation and can prevent blood from clotting. Fig. 1 Salicylic acid 1 Fig. 2 Acetylsalicylic acid Flower R, Gryglewski R, Herbaczyńska-Cedro K et al. Effects of anti-inflammatory drugs on prostaglandin biosynthesis. Nat New Biol 1972;238(82):104–106. - 2/3 - Contact: Anne Coiley, phone +862 404-6314 E-mail: [email protected] August, 2015 Forward-Looking Statements This release may contain forward-looking statements based on current assumptions and forecasts made by Bayer Group or subgroup management. Various known and unknown risks, uncertainties and other factors could lead to material differences between the actual future results, financial situation, development or performance of the company and the estimates given here. These factors include those discussed in Bayer’s public reports which are available on the Bayer website at www.bayer.com. The company assumes no liability whatsoever to update these forward-looking statements or to conform them to future events or developments. - 3/3 -