* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Noninvasive Evaluation of Right Atrial Pressure
Survey
Document related concepts
Management of acute coronary syndrome wikipedia , lookup
Heart failure wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Marfan syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Myocardial infarction wikipedia , lookup
Artificial heart valve wikipedia , lookup
Cardiac surgery wikipedia , lookup
Electrocardiography wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Transcript
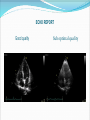
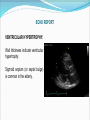
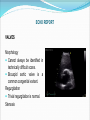
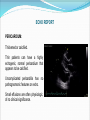
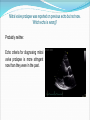
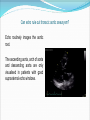
Dr W Arshad & Dr AS Kurbaan Cardiology Department Homerton University Hospital, London Topics 1. GP Open access echo 2. GP Open access Holter GP OPEN ACCESS ECHOCARDIOGRAPHY “GP open access echocardiography refers to cardiac ultrasound imaging which is requested by, reported to, and acted upon by GPs.” AIMS OF PRESENTATION Structured approach to reading echo reports. Address issues encountered by referring GPs. AIMS OF PRESENTATION Structured approach to reading echo reports. Address issues encountered by referring GPs. ECHO REPORT HOMERTON UNIVERSITY HOSPITAL NHS FOUNDATION TRUST GP OPEN ACCCESS ECHOCARDIOGRAPHY REPORT SURNAME FORENAME DATE OF BIRTH GENDER HOSPITAL NUMBER DATE OF STUDY INDICATION MEASUREMENTS Men Women Ventricular septal thickness (mm) 6-12 6-12 Mitral E velocity (m/s) LV end diastolic dimension (mm) 42-59 39-53 Mitral A velocity (m/s) LV posterior wall thickness (mm) 6-12 6-12 Aortic flow (mmHg) 30-40 27-38 ≥55 ≥55 LV end systolic dimension (mm) Left atrium (mm) Pulmonary flow (mmHg) Aorta (mm) LV ejection fraction (%) FINDINGS ECG shows sinus rhythm. LEFT VENTRICLE: Normal left ventricular size. No left ventricular hypertrophy. No regional wall motion abnormality. Good long axes function. Overall good left ventricular function. LEFT ATRIUM: Normal size. No colour flow across atrial septum. AORTIC VALVE: Trileaflet, opens well. MITRAL VALVE: Mobile leaflets. Normal filling pattern. RIGHT VENTRICLE: Normal size. No right ventricular hypertrophy. Good long axis function. Overall good right ventricular function. RIGHT ATRIUM: Normal size. PULMONARY VALVE: Normal. TRICUSPID VALVE: Normal. CONCLUSION Normal study. OPERATOR Dr Waleed Arshad POSITION Associate Specialist Cardiologist The operator holds Accreditation in Transthoracic Echocardiography by British Society of Echocardiography, Accreditation in Transthoracic Echocardiography by European Society of Echocardiography, Diplomate Adult Comprehensive Echocardiography by National Board of Echocardiography USA and Fellowship of American Society of Echocardiography. ECHO REPORT INDICATION: The value of echocardiogram is greatest when a single focused question can be asked, answered by echocardiographer, & lead to change in management by GP. If trends in improvement or deterioration are of interest, echocardiographer needs results of previous studies, especially if they are carried outside Homerton Hospital. ECHO REPORT DATE OF STUDY: Does this report reflect the patient’s current clinical status? RHYTHM: Was the rhythm interpretable? What was the rhythm? Sinus rhythm/Sinus rhythm with ectopics/Atrial fibrillation Did the rhythm interfere with assessment of left and right ventricular function? ECHO REPORT IMAGE QUALITY: Can vary from excellent to uninterpretable. In technically difficult/sub optimal studies, pathology “not seen” does not necessarily mean “not present”. What was the reason for technical difficult/sub optimal study? ECHO REPORT Good quality Sub optimal quality ECHO REPORT CHAMBER SIZES: The table lists the measured chamber size (diameters) and compares them with normal values. Increased values chamber dilatation. indicate Transverse diameter under estimates true volume of an enlarged left atrium. Men Women Ventricular septal thickness (mm) 6-12 6-12 LV end diastolic dimension (mm) 42-59 39-53 LV posterior wall thickness (mm) 6-12 6-12 30-40 27-38 ≥55 ≥55 LV end systolic dimension (mm) Left atrium (mm) Aorta (mm) LV ejection fraction (%) ECHO REPORT VENTRICULAR HYPERTROPHY: Wall thickness indicate ventricular hypertrophy. Sigmoid septum (or septal bulge) is common in the elderly. ECHO REPORT LV SYSTOLIC FUNCTION Circumferential/Radial Mid wall Base Longitudinal Subendocardial Subepicardial free wall Papillary muscles ECHO REPORT LV SYSTOLIC FUNCTION Radial Ejection fraction is a poor indicator of LV function Wall motion Global abnormalities suggest cardiomyopathy Regional abnormalities suggest ischaemia/infarction Wall motion score Index Longitudinal Amplitude Velocity Timing ECHO REPORT LV DIASTOLIC FUNCTION LV diastolic dysfunction precedes development of LV systolic dysfunction. Increased LA size is morphologic expression diastolic dysfunction. a of Redfield MM, Jacobsen SJ, Burnett JC Jr, et al. Burden of systolic and diastolic ventricular dysfunction in the community: Appreciating the scope of the heart failure epidemic. JAMA 2003; 289:194. ECHO REPORT VALVES Morphology Cannot always be identified in technically difficult scans. Bicuspid aortic valve is a common congenital variant. Regurgitation Trivial regurgitation is normal. Stenosis ECHO REPORT MASS OR THROMBUS: Ability to detect mass or thrombus is only as good as the images. TTE does not image the left atrial appendage adequately, therefore TOE is needed. ECHO REPORT PERICARDIUM: Thickened or calcified. Thin patients can have a highly echogenic, normal pericardium that appears to be calcified. Uncomplicated pericarditis has no pathognomonic features on echo. Small effusions are often physiologic, of no clinical significance. ECHO REPORT CONCLUSION: Important cardiac findings. Referral to Cardiology team might be advised – ideally clinical decisions should be made by physicians who have knowledge of their patients. AIMS OF PRESENTATION Structured approach to reading echo reports. Address issues encountered by referring GPs. Left ventricular ejection fraction was different in another recent echo. Which study was correct? Probably both. Ejection fraction depends on preload and afterload, both of which can change dramatically and quickly according to patient’s condition. Ejection fraction also depends upon the method by which it is calculated. Ejection fraction is rarely measured properly by Simpson’s method but more often by Teicholtz. What is importance of longitudinal function? Long axes is abnormal in hypertension, hypertrophy, coronary artery disease, cardiomyopathy and conduction disease. Long axes is an independent predictor of prognosis in cardiovascular disease. How should I manage longitudinal dysfunction? Systolic or diastolic dysfunction Systolic – Same treatment as radial systolic dysfunction Diastolic – Same treatment as global diastolic dysfunction How should I manage LV diastolic dysfunction? The treatment remains empiric since trial data are limited. The general principles are: Control of systolic & diastolic hypertension. Control of heart rate, particularly in patients with atrial fibrillation. Control of pulmonary congestion and peripheral oedema with diuretics. Coronary revascularisation in patients with coronary heart disease. 2013 ACCF/AHA Guideline for the management of heart failure. J Am Coll Cardiol. 2013;62(16):e147-e239. doi:10.1016/j.jacc.2013.05.019 2012 ESC Guidelines for the diagnosis & treatment of acute & chronic heart failure. European Heart Journal. 20121;33:1787–1847 doi:10.1093/eurheartj/ehs104 How should I manage valvular heart disease (VHD)? History & Physical examination A careful history is of great importance in the evaluation of patients with VHD, because decisions about treatment are based on the presence or absence of symptoms. Due to the slow, progressive nature of many valve lesions, patients may not recognize symptoms because they may have gradually limited their daily activity levels. A detailed physical examination should be performed to diagnose and assess the severity of valve lesions based on a compilation of all findings made by inspection, palpation and auscultation. How should I manage valvular heart disease (VHD)? Investigations ECG - to confirm heart rhythm. Chest x-ray to assess the presence or absence of pulmonary congestion and other lung pathology. Echocardiogram to correlate findings with initial impressions based on the initial clinical evaluation. The Echocardiogram will also be able to provide additional information, such as the effect of the valve lesion on the cardiac chambers and great vessels, and to assess for other concomitant valve lesions. How should I manage valvular heart disease (VHD)? Frequency of echocardiograms Aortic stenosis Aortic regurgitation Mitral stenosis Mitral regurgitation Mild 3–5 y 3–5 y 3–5 y 3–5 y Moderate 1–2 y 1–2 y 3–5 y 1–2 y 6–12 months 6–12 months 1–2 y 6–12 months Dilating LV: more frequently Once every year when MVA <1.0 Dilating LV: more frequently Severe cm2 2014 AHA/ACC Guideline for the management of patients with valvular heart disease. J Am Coll Cardiol. 2014;63(22):e57-e185. doi:10.1016/j.jacc.2014.02.536 How should I manage bicuspid aortic valve? Surveillance for aortic valve dysfunction (stenosis, regurgitation, or both) and for disease of the aortic root and ascending aorta. The bicuspid aortic valve is inherited as an autosomal dominant condition with incomplete penetrance and also appears in sporadic cases. Therefore, screening by echocardiography for first degree relatives for bicuspid aortic valve and aortic root & ascending aorta dilation. Mitral valve prolapse was reported on previous echo but not now. Which echo is wrong? Probably neither. Echo criteria for diagnosing mitral valve prolapse is more stringent now than they were in the past. Can echo rule out thoracic aortic aneurysm? Echo routinely images the aortic root. The ascending aorta, arch of aorta and descending aorta are only visualised in patients with good suprasternal echo windows. How should I manage thoracic aortic aneurysm? General principles of cardiovascular prevention: Strict control of hypertension Cessation of smoking Imaging: When an aortic aneurysm is identified at any location, assessment of the entire aorta and aortic valve is recommended at baseline and during follow-up. 2014 ESC Guidelines on the diagnosis and treatment of aortic diseases. European Heart Journal. 2014;35:2873–2926 doi:10.1093/eurheartj/ehu281 How frequent should be surveillance of thoracic aortic aneurysm? Every six months for large aneurysms and annually for those with smaller aneurysms. Patient with large thoracic aortic aneurysms should be under care of Cardiology/Cardiothoracic teams. Summary Echo is essential for cardiovascular evaluation and follow up. A structured approach to reading echo reports is necessary. This brief review has tried to address many issues encountered by referring GPs. PRINCIPLES 1. How ‘severe’ is the abnormality? E.g. 4 beats of VT vs 30 secs 2. What are the symptoms? Chest pain, syncope etc. 3. Is there an associated cardiac abnormality Impaired ventricular function SEVERITY OF THE ABNORMALITY ‘Abnormal findings not uncommon Ectopy <1% usually ok, 2% or more consider assessment Bigeminy/Trigeminy (?frequency) PAF (30s or multiple runs) SVT (15-20 beats) VT (>8 beats, multifocal) ‘HIGH RISK’ SYMPTOMS/HISTORY Known IHD, angina, heart attack, CABG, PCI Known arrhythmia Impaired LV Previous stroke Known peripheral arterial disease Syncope/presyncope Family history of sudden cardiac death Multiple vascular risk factors: HTN/DM ‘HIGH RISK’ CARDIAC INVESTIGATIONS Impaired LV <55% EF impaired, <30% severely impaired Regional wall motion abnormality Moderate/severe valvular abnormality Known IHD e.g. high calcium score EXAMPLE: 15 BEATS OF ‘SVT’ Patient 1: 25, female palpitations long standing otherwise well Patient 2: 73, female, previous TIA (no cause found) Patient 3: 18 male, almost blacked out at gym SUMMARY How ‘bad’ is what they have got? Are there other worrying aspects of the case? Rapid Access Atrial Fibrillation Clinic Why? - To provide a rapid diagnosis of atrial fibrillation in patients presenting for the first time in the community or in patients with ongoing unresolved issues with their management. - To facilitate the early initiation of anticoagulation and other treatments for atrial fibrillation. Rapid Access Atrial Fibrillation Clinic What will the clinic offer? - One stop - Echo (if needed) on the day - Holter (if needed) fitted on the day - Accurate diagnosis - Access to Consultant Cardiologist/Electrophysiologist