* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Contact
West Nile fever wikipedia , lookup
Microbicides for sexually transmitted diseases wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Cryptosporidiosis wikipedia , lookup
Chagas disease wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Sarcocystis wikipedia , lookup
Meningococcal disease wikipedia , lookup
Onchocerciasis wikipedia , lookup
Trichinosis wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Visceral leishmaniasis wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Neonatal infection wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Hepatitis C wikipedia , lookup
Schistosomiasis wikipedia , lookup
Hepatitis B wikipedia , lookup
Marburg virus disease wikipedia , lookup
Leptospirosis wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Oesophagostomum wikipedia , lookup
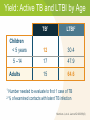
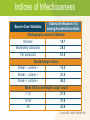
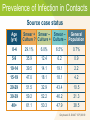
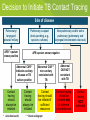
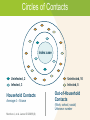
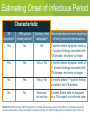
Module 15 – March 2010 TB Contact Investigation Project Partners Funded by the Health Resources and Services Administration (HRSA) Module Overview Overview: Value (yield) of contact evaluation Clinical factors influencing transmission Evaluating contacts and determining priorities Vulnerable contacts Treatment of infected contacts International Standards 18 and 19 Learning Objectives At the end of this presentation participants will be able to: Describe the criteria used and method for determining an infectious period Evaluate the risk of transmission based on the clinical extent of disease and diagnostic tests Determine who among contacts is at greatest risk should infection occur Identify and evaluate contacts who are at increased risk for TB infection Definitions Case – a particular instance of disease (e.g., TB). A case is detected, documented and reported Index case – the first person who presents for evaluation as a confirmed or suspected case of tuberculosis Source case – the case or person that was the original source of infection for secondary cases or contacts Definitions (2) Contact –someone who is at risk for acquiring M. tuberculosis infection by sharing airspace with an index case Converter – a person whose test result for M. tuberculosis has changed from negative (uninfected) to positive (infected) Window period – refers to the interval between infection and detectable reactivity to the tuberculin skin test (TST) Why do we do TB contact investigations (CI)? Remember!! Every TB Case Began as a TB Contact Contact investigation helps to: TB Index Case Identify additional TB cases Identify persons with latent TB infection TB Case TB Contacts Prevent the further spread of TB Save someone’s life TB Contacts TB Cases ISTC Standard 18 All providers of care for patients with TB should ensure that persons who are in close contact with patients who have infectious TB are evaluated and managed in line with international recommendations. The determination of priorities for CI is based on the likelihood that a contact: 1. Has undiagnosed TB 2. Is at high risk of developing TB if infected 3. Is at risk of having severe TB if the disease develops 4. Is at high risk of having been infected by the index case ISTC Standard 18 (2) The highest priority contacts for evaluation are: Persons with TB symptoms Children aged <5 years Contacts with known or suspected compromised immune systems, particularly HIV infection Contacts of patients with MDR/XDR tuberculosis Other close contacts are a lower priority group Standards for Public Health Systematic Review of Contact Investigations Yield for all active TB among household contacts was 4.5% Pooled yield for confirmed TB among household contacts was 2.3% Nearly one-half of the household contacts evaluated had LTBI indicated by a positive tuberculin skin test, but a negative evaluation for active TB Morrison J, et al. Lancet ID 2007 Yield: Active TB and LTBI by Age TB1 LTBI2 Children < 5 years 12 30.4 5 –14 17 47.9 15 64.6 Adults 1 Number needed to evaluate to find 1 case of TB 2 % of examined contacts with latent TB infection Morrison J, et al. Lancet ID 2008;8(6) TB Contact Investigation Steps 1. Decide whether to initiate a contact investigation 2. Interview the index case 5 7 6 3. Examine sites of transmission 4. Prioritize contacts 4 3 5. Locate and evaluate contacts 6. Treat and follow-up contacts 1 2 7. Evaluate contact investigation activities Step 1: Decide if a CI should be initiated To make this decision, you will be assessing for: Evidence that the index case may be infectious Presence of vulnerable contacts • Those with an immature or weakened immune system Review Medical Record Site of TB disease TB symptoms and approximate date of onset Test results • Sputum AFB smear and culture results Including dates of specimen collection • Chest X-ray results and date TB treatment (medications, dosage, and date treatment was started) Method of treatment administration • DOT or self-administered Assessing Infectiousness High degree of infectiousness • Sputum smear-positive pulmonary TB (PTB) • Symptomatic with cough • Cavitation on chest radiograph (correlates with positive smear) • Laryngeal tuberculosis Lesser degree of infectiousness • • • • Sputum smear-negative, culture-positive PTB Minimal if any cough Lesser radiographic extent of disease Extrapulmonary TB Indices of Infectiousness Tuberculin Reactors (%) among household contacts Radiographic extent of disease Minimal 16.1 Moderately advanced 28.3 Far advanced 61.5 Bacteriologic status Smear –, culture – 14.3 Smear –, culture + 21.4 Smear +, culture + 44.3 Mean 8-hour overnight cough count < 12 27.5 12-48 31.8 48 43.9 Source-Case Variables Loudon RG. ARRD 1969;99:109 Prevalence of Infection in Contacts Source case status Age (yrs) Smear + Smear – Smear – General Culture ? Culture + Culture – Population 0-4 29.1% 6.0% 6.5% 0.7% 5-9 35.9 12.4 6.2 0.9 10-14 39.5 14.1 19.1 2.2 15-19 47.0 18.1 18.1 4.2 20-29 51.5 32.9 43.4 10.5 30-39 59.2 52.2 46.2 21.3 40+ 61.1 50.3 47.9 38.5 Grzybowski S. BIUAT 1975;60:90 How do we decide to initiate the contact tracing process? Decision to Initiate TB Contact Tracing Site of disease Pulmonary/ laryngeal/ pleural/ miliary AFB * sputum smear positive Pulmonary suspect (tests pending, e.g., sputum, cultures) AFB sputum smear-negative Abnormal CXR** indicates cavitary disease or TB culture positive Contact tracing should always be initiated * Acid-fast bacilli; Non-pulmonary and/or extra pulmonary (pulmonary and laryngeal involvement ruled out) Contact tracing should always be initiated Abnormal CXR ** non-cavitary consistent with TB Contact tracing should be initiated if sufficient resources * * Chest radiograph Abnormal CXR NOT consistent with TB Contact tracing should be initiated only in extreme circumstances Contact tracing NOT indicated Who is Responsible for Conducting TB Contact Investigations? The National TB Program is responsible for ensuring contact tracing occurs and this includes ensuring: Identification and evaluation of contacts Treatment of contacts found to have TB disease Preventive treatment of contacts with TB infection Monitoring of treatment and adherence to prescribed regimens A system is in place to assess completion of treatment How Quickly Should a TB Contact Investigation be Carried Out? Begin as soon as TB is diagnosed or strongly suspected in a patient Initiate no more that 7 working days after the case is reported to the National TB Program Contacts should be examined within 14 working days after the index patient has been diagnosed Rationale for Prompt Contact Tracing Some contacts may develop TB disease very quickly after being exposed to and infected with M. tuberculosis • Infants and children <5 years of age • HIV-infected or other immunosuppressed Increases likelihood that all contacts will be found and evaluated Contact Investigation Case Study Part 1 Step 2: Interview the Index Case Conduct a minimum of 2 interviews • 1st interview ≤1 business day of reporting for infectious patients ≤3 business days for others • 2nd interview 1–2 weeks later • May need additional interviews TB Interview Goals Provide appropriate TB education Identify problems/concerns Determine period of infectiousness (IP) and where patient spent time during IP Identify contacts and locating information Establish contact investigation priorities Reinforce follow through with treatment plan Circles of Contacts Index case Uninfected, 2 Uninfected, 10 Infected, 3 Infected, 5 Household Contacts Average 4 – 5/case Out-of-Household Contacts (Work, school, social) Unknown number Morrison J, et al. Lancet ID 2008;8(6) Initial Interview Preparation 1. Review TB patient’s medical records 2. Determine interview objective and strategy 3. Arrange interview place and time TB Interview Components Introduction Education Contact List Conclusion Follow-up Identification of Contacts Focus on those in the same household but don’t neglect out-of-household contacts Tailor interview to patient’s circumstances (homeless, congregate living facility, etc.) Determine the circumstances of exposure, and attempt to quantify the closeness and duration Determine if there are other persons within the group of contacts who have symptoms associated with TB Determine Infectious Period The timeframe during which an individual with TB disease is capable of transmitting infection This timeframe is determined by estimating the duration of the individual’s symptoms, especially coughing In the absence of symptoms, this timeframe is determined based on the date of diagnosis of TB disease Estimating Onset of Infectious Period Characteristic TB AFB sputum symptoms? smear positive? Cavitary chest Recommended minimum beginning radiograph? of likely period of infectiousness Yes No No 3 months before symptom onset or 1st positive findings consistent with TB disease, whichever is longer Yes Yes Yes or No 3 months before symptom onset or 1st positive findings consistent with TB disease, whichever is longer No Yes Yes or No 3 months before 1st positive finding consistent with TB disease No No Abnormal, not cavitary 4 weeks before date of diagnosis as a TB suspect or confirmed case SOURCE: Modified from the California Department of Health Services Tuberculosis Control Branch; California Tuberculosis Controllers Association. Contact Investigation Guidelines. Berkley, CA: California Department of Health Services; 1998, p.23. Closing the Infectious Period Infectious period closed when all the following criteria are met: Effective treatment for ≥ 2 weeks, Diminished symptoms, and Bacteriologic response Contact Investigation Case Study Part 2 Step 3: Examine Sites of Transmission Visit the sites where the patient spent time during the infectious period Components of the field investigation include: • Interview, test & provide TB information to contacts • Identify additional contacts • Assess physical conditions of the setting (room size, ventilation, airflow, etc.) Levels of Exposure Closeness and duration of exposure: Grading exposure settings 1. 2. 3. 4. Size of a car Size of a bedroom Size of a house Larger than a house Estimating critical exposure duration Thresholds are highly variable Exposure duration threshold should be determined by index case characteristics, settings, contact risk factors Step 4: Prioritize Contacts Concentric Circle Approach Concentric Circle Approach Household / Residence Environment + Infectiousness Index Patient Leisure / Recreation Environment Work / School Environment Exposure intensity Susceptibility of the contact Close contacts (high risk) Other-than-close contacts (medium risk) Other-than-close contacts (low risk) Prioritizing Contacts High priority contacts are determined by: 1. Most likely to be infected 2. Most likely to progress to disease if infected Factors for Assigning Priority Consider: Infectiousness of the TB case Environment where transmission likely occurred Infectiousness Environment Freq/duration Frequency, duration and proximity of exposure Susceptibility factors: • Age, immune system status Priorities in Contact Evaluation At greatest risk of acquiring infection • Close contacts of smear positive index cases • Persons with HIV infection • Highly exposed persons At greatest risk of active TB • Children <5 years of age • Persons with HIV infection • Persons with other immunocompromising conditions or therapies Contact Investigation Case Study Part 3 Step 5: Locate and Evaluate Contacts Initial Assessments of Contacts Approach to evaluation of contacts may vary depending on local circumstances, resources, and policies Evaluation: Question contacts about symptoms and evaluate if symptoms are present • TST followed by chest X-ray (CXR) for all positive Mantoux (≥5 mm induration) • CXR all children < age 5 and any symptomatic or immunocompromised contacts regardless of TST • Sputum examinations for all symptomatic contacts and any with CXR abnormalities suggestive of TB Step 6: Treat & Follow-up Contacts Rationale: Risk of active tuberculosis is greatest soon after infection occurs Contacts of infectious cases are likely to have been infected recently Treatment of those found to have a positive tuberculin skin test will reduce the likelihood of active tuberculosis Treatment for LTBI: Evaluation Evaluate all potential LTBI treatment candidates for active TB Identify those who have been treated previously Identify those with contraindications to treatment for LTBI (prior allergic reactions, severe unstable liver disease) Identify co-morbid conditions and other medications being used ISTC Standard 19 Children <5 years of age and persons of any age with HIV infection who are close contacts of an infectious index patient and who, after careful evaluation, do not have active tuberculosis, should be treated for presumed latent TB infection with isoniazid Treatment for LTBI: Priorities Children <5 years of age Persons with HIV infection Persons with other immunocompromising conditions Close contacts of highly infectious index case Persons with other conditions that increase risk (example: silicosis) Other Treatment Considerations “Window-period” prophylaxis – treatment (usually INH) given to high risk contacts with an initial negative TST during the period following last contact until the follow-up TST Priorities for initiating window-period prophylaxis include: • Children <5 years of age • Persons with HIV infection Exposure to drug resistant TB – consult an expert in the management of drug resistant TB Follow-up All Contacts found to have latent TB infection (LTBI) and started on treatment should receive monthly visit by a nurse or physician MDR-TB exposure – seek expert consultation; follow-up for 2 years post exposure Contact Investigation Case Study Part 4 Step 7: Evaluate C.I. Activities Management of care and follow up of TB case and contacts Epidemiologic analysis of the investigation in progress to allow prioritization of program activities and resources Program evaluation—measure how well objectives are being met Deciding Whether to Expand Testing Evidence of Recent Transmission: Infection in a child (<5 years of age) TST converters Secondary case TB disease in any contact assigned a low priority Contact Investigation Case Study Part 5 Summary: ISTC Standards Covered* Standard 18: All providers of care for patients with TB should ensure that persons who are in close contact with patients who have infectious TB are evaluated and managed in line with international recommendations. The highest priority contacts for evaluation are: Persons with symptoms suggestive of tuberculosis Children aged <5 years Contacts with known or suspected immunocompromise, particularly HIV infection Contacts of patients with MDR/XDR tuberculosis Other close contacts are a lower priority group * Abbreviated versions Summary: ISTC Standards Covered* (2) Standard 19: Children <5 years of age and persons of any age with HIV infection who are close contacts of an infectious index patient and who, after careful evaluation, do not have active tuberculosis, should be treated for presumed latent tuberculosis infection with isoniazid. * Abbreviated versions Summary Between 4 - 5 % of household contacts of new cases will be found to have active TB and up to 50% may have LTBI The likelihood of transmission relates directly to the bacillary burden of the index case Environmental factors also play an important role Priorities for evaluation include children <5 years of age, persons with HIV infection, and highly exposed contacts Treatment is indicated for high priority contacts with LTBI and during the “window period”