* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download SIRS - MODS
Survey
Document related concepts
Adaptive immune system wikipedia , lookup
Neonatal infection wikipedia , lookup
Acute pancreatitis wikipedia , lookup
Adoptive cell transfer wikipedia , lookup
Cancer immunotherapy wikipedia , lookup
Polyclonal B cell response wikipedia , lookup
Molecular mimicry wikipedia , lookup
Sjögren syndrome wikipedia , lookup
Hygiene hypothesis wikipedia , lookup
Pathophysiology of multiple sclerosis wikipedia , lookup
Immunosuppressive drug wikipedia , lookup
Innate immune system wikipedia , lookup
Transcript
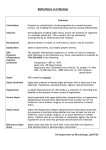
Close window to return to IVIS in collaborazione con RICHIESTO ACCREDITAMENTO SOCIETÀ CULTURALE ITALIANA VETERINARI PER ANIMALI DA COMPAGNIA SOCIETÀ FEDERATA ANMVI organizzato da certificata ISO 9001:2000 INFORMATION SCIVAC Secretary Palazzo Trecchi, via Trecchi 20 Cremona Tel. (0039) 0372-403504 - Fax (0039) 0372-457091 [email protected] www.scivac.it Close window to return to IVIS In: 50° Congresso Nazionale Multisala SCIVAC, 2005 – Rimini, Italia SIRS – MODS – Sepsis Kate Hopper BVSc. MVS, DACVECC Small Animal Emergency & Critical Care University of California, Davis Sepsis describes an infectious process that causes a systemic inflammatory response (SIRS) evidenced by fever, tachypnea, tachycardia and leukocytosis (Table 1). Mortality from sepsis occurs as a result of acquired, progressive abnormalities in organ function, a process known as multiple organ dysfunction syndrome (MODS). This syndrome is characterized by abnormalities developing in organs that were not affected by the original insult and is associated with high morbidity and mortality rates. Clinical management of septic patients is complex and challenging. It requires initial identification of at risk animals, intense monitoring and nursing care and aggressive management of any abnormalities that develop. The Inflammatory Response: Local tissue injury and ischemia trigger local and in many cases, systemic inflammatory responses. The magnitude of these responses correlates with the magnitude of the injury itself. An exaggerated or dysregulated inflammatory response can overwhelm the normal host protective mechanisms and cause tissue damage in its own right. This widespread inflammatory injury can lead to a sepsis like condition but it is not necessarily associated with an infectious cause. The Local Inflammatory Response: Following an insult or injury there is cellular damage, endothelial disruption and tissue ischemia. Damaged cells and ischemic tissue will release mediators that activate effector cells of the innate immune system such as tissue macrophages. Once activated, these cells will produce cytokines such as tumor necrosis factor alpha (TNF-a), interleukin-1 beta (IL-1ß ), IL-6 and chemokines. Local endothelial cells are activated from their usual quiescent state by stimuli such as direct injury, endotoxin and/or cytokines. These locally activated endothelial cells will express adhesion molecules, release pro-inflammatory cytokines and activate coagulation. Endothelial cell damage and exposure of endothelial cells to pro-inflammatory cytokines will result in vasodilation and local increases in capillary permeability with subsequent movement of plasma proteins and fluid into the interstitial space. Endothelial cell expression of selectins and intercellular adhesion molecules (ICAMs) in combination with cytokines and chemokines will result in the rolling, adhesion and transmigration of circulating leukocytes into the surrounding damaged tissue. Neutrophils are vital to this inflammatory response. Once activated they release proteases, elastases and reactive oxygen species to kill damaged cells and microorganisms allowing effective phagocytosis and tissue repair. Activation of numerous other inflammatory pathways accompanies this local inflammatory response including complement, coagulation, the kinin system and the arachadonic acid cascade. This inflammatory reaction is also responsible for the elaboration of factors required for new cell growth, angiogenesis etc. that is essential for tissue repair. The local inflammatory response is an appropriate and vital component of both host defense and recovery from injury. It leads to the classic signs of redness, heat, swelling and pain of the injured tissue but there are no associated systemic signs. Close window to return to IVIS Systemic Inflammation: The systemic inflammatory response syndrome (SIRS) occurs when there is release of inflammatory mediators into the systemic circulation. These trigger global responses that are the clinical markers of SIRS; fever or hypothermia, tachycardia, tachypnea, decreased or elevated total white blood cell count etc (Table 1). The systemic inflammatory response occurs when a local site of inflammation is severe enough to allow ‘overflow’ of mediators into the circulation instead of restricting them to the region of injured tissue only. Systemic release of mediators can also occur in response to a systemic insult such as bacteremia or endotoxemia. The magnitude of SIRS varies from mild to severe; in general mild to moderate SIRS is a normal and beneficial response to a significant insult. It is vital for immunocompetancy and without it there is increased morbidity and mortality. A severe SIRS response may be detrimental causing cellular dysfunction and tissue damage that is more significant than the primary insult itself. Table 1: Clinical recognition of SIRS Dogs = 2 or more of; Cats = 3 or more of*; Tachypnea Tachypnea – rate > 40 bpm Tachycardia Heart rate < 140 or > 225 bpm Hyper or Hypothermia Temperature <37.8ºC or > 39.7ºC High or Low wbc or > 10% Bands WBC < 5000/µl or > 19,500/µl or > 5% Bands *Brady CA et al. JAVMA 2000;217(4):531-535 The major causes of SIRS are infection, trauma, pancreatitis, burn injury and immune reactions. Effectively any insult that leads to cell damage will produce an inflammatory response and has the potential for causing SIRS. It is important to note that although infection is a common cause of SIRS it is not the only cause. The systemic inflammatory response syndrome as the name states is a syndrome, a collection of clinical signs occurring together. The presence of SIRS in a patient provides no information regarding the primary disease process or case prognosis. Rather it is an observation that can aid in evaluating the severity of illness and may identify patients at greater risk of developing acquired organ dysfunction. Multiple Organ Dysfunction Syndrome: Multiple organ dysfunction syndrome (MODS) is characterized by progressive acquired derangements in the function of organs not damaged by the original insult or injury. How does an organ remote from the site of the initial injury become damaged? This process is one of inflammation mediated damage and is a consequence of the hosts own cellular responses. A delicate balance exists between the beneficial and detrimental effects of systemic inflammation. With systemic release of inflammatory mediators all the effects of local inflammation as listed above can occur on a global scale. Widespread endothelial cell activation is seen as a critical component of this response. As mentioned above controlled mild to moderate SIRS is an appropriate and beneficial reaction to significant injury or insult but severe SIRS may have detrimental effects to the host. Severe SIRS will lead to global endothelial activation causing generalized vasodilation and increases in capillary permeability; this contributes to hypovolemia, hypotension, hypoproteinemia and interstitial edema. Widespread neutrophil activation in combination with global endothelial activation can lead to indiscriminate tissue invasion; activated neutrophils transmigrating into healthy, uninjured tissue. The release of cytotoxic substances by these cells will cause uncontrolled tissue damage and cell death. Generalized endothelial activation is the precursor of disseminated intravascular coagulation (DIC) which can result in microvascular thrombi formation. In vital organs the combination of hypoperfusion, microthrombosis and direct cellular damage can lead to loss of function and if severe, organ failure may result. Close window to return to IVIS Table 2: Definitions of common terms relevant to sepsis Term Definition Infection The host response to the presence of micro-organisms or tissue invasion by micro-organisms. Bacteremia The presence of viable bacteria in circulating blood. SIRS Systemic inflammatory response to an insult or injury as evidenced by tachypnea, tachycardia, abnormal body temperature, abnormal white cell count MODS Multiple organ dysfunction syndrome – the presence of altered organ function requiring intervention in a critically ill patient Sepsis SIRS and an infection Severe Sepsis Sepsis associated with organ dysfunction, hypoperfusion or hypotension. Septic Shock Hypotension in a septic patient despite adequate fluid resuscitation Bibliography: Brady CA et al. JAVMA 2000;217(4):531-535 Hotchkiss RS, Karl IE. The pathophysiology and treatment of sepsis. N Engl J Med 2003;348(2):138-150 Macintire DK, Drobatz KJ, Haskins SC and Saxon WD. Small animal emergency and critical care medicine. Lippincott Williams & Wilkins, Baltimore 2005 nd Marino PL, The ICU Book, 2 Ed. Williams & Wilkins, Baltimore 1998 Schrier RW, Wang W. Acute renal failure in sepsis. N Engl J Med 2004;352(2):159-169 Tracey KJ. The inflammatory reflex. Nature 2002;420(19):853-859 This manuscript is reproduced in the IVIS website with the permission of the Congress Organizing Committee