* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Sudden Cardiac Death
Survey
Document related concepts
Saturated fat and cardiovascular disease wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Rheumatic fever wikipedia , lookup
Heart failure wikipedia , lookup
Electrocardiography wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Coronary artery disease wikipedia , lookup
Transcript
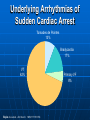
Inhospital SCD Doc.Dr Emir Fazlibegović,ESC,FESC Prof.Dr Mustafa Hadžiomerović, ESC,FESC 5th International Congress of cardiologysts and angyologysts of Bosnia and Herzegovina,Sarajevo 2010. Time references in SCD Biological Model of SCD Magnitude of SCA in the U.S. Stroke3 167,366 Lung Cancer2 157,400 Breast Cancer2 40,600 AIDS1 42,156 1 2 3 4 SCA claims more lives each year than these other diseases combined 450,000 SCA4 #1 Killer in the U.S. U.S. Census Bureau, Statistical Abstract of the United States: 2001. American Cancer Society, Inc., Surveillance Research, Cancer Facts and Figures 2001. 2002 Heart and Stroke Statistical Update, American Heart Association. Zheng Z. Circulation. 2001;104:2158-2163. Magnitude of SCA in the U.S. ~450,000 per year1 1,200 per day • 1 every 80 seconds Although SCA is the first presentation of cardiac disease in 20-25% of patients, most cases occur in patients with clinically recognized heart disease.2 1 Zheng 2 Z. Circulation. 2001;104::2158-2163. Myerburg RJ, Heart Disease, A textbook of Cardiovascular Medicine. 6th ed. 2001. W.B. Saunders, Co. SCA Different from MI SCA Caused by heart electrical system problem. MI Occurs when one or more of the arteries that supply blood to the heart muscle becomes blocked. The affected area loses blood supply (ischemia) and results in damage to the heart tissue. SCA and MI Symptoms SCA Symptoms: Collapse and loss of consciousness Cessation of normal breathing Loss of pulse and blood pressure SCA has few to no premonitory signs and death is usually rapid--within one hour. www.americanheart.org MI Symptoms: Uncomfortable pressure, fullness, squeezing, or pain in the center of the chest lasting more than few minutes Pain spreading to the shoulders, neck, or arms Chest discomfort with lightheadedness, fainting, sweating, nausea, or shortness of breath Atypical chest pain, stomach or abdominal pain Nausea or dizziness Shortness of breath and difficulty breathing Unexplained anxiety, weakness, or fatigue Palpitations, cold sweat, or paleness An impending MI typically has many premonitory signs that may develop over the course of hours or days. Etiology of SCD -An estimated 13 million people had coronary heart disease (CHD) in the U.S. in 2002. 1 -Sudden death was the first manifestation of CHD in 50% of men and 63% of women. 1 -CHD accounts for at least 80% of sudden cardiac deaths in Western cultures.3 Etiology of Sudden Cardiac Death2,3 5% Other* 15% Cardiomyopathy * ion-channel abnormalities, valvular or congenital heart disease, other causes 80% Coronary Heart Disease 1 American Heart Association. Heart Disease and Stroke Statistics—2003 Update. Dallas, Tex.: American Heart Association; 2002. 2 Adapted from Heikki et al. N Engl J Med, Vol. 345, No. 20, 2001. 3 Myerberg RJ. Heart Disease, A Textbook of Cardiovascular Medicine. 6th ed. P. 895. Causes of in-hospital mortality The cause of death in hospital is most often noncardiac, usually being due to anoxic encephalopathy or to respiratory complications from long-term respirator dependence Only about 10 percent of patients die from recurrent arrhythmia, while approximately 30 percent die from a low cardiac output or cardiogenic shock PROVOKING FACTORS Electrolyte disturbances • Any reversible metabolic abnormalities should be identified and corrected, particularly hypokalemia and hypomagnesemia which may predispose to ventricular tachyarrhythmias Antiarrhythmic drugs • Whenever possible, antiarrhythmic drugs should be discontinued prior to any diagnostic studies PROVOKING FACTORS Use of an illicit drug such as cocaine can directly cause arrhythmia or produce coronary artery vasospasm and ischemia A prolonged QT interval which may be acquired (due, for example, to a drug or electrolyte disturbance) or inherited Arrhythmic Cause of SCD 12% Other Cardiac Cause 88% Arrhythmic Cause . Albert CM. Circulation. 2003;107:2096-2101 Underlying Arrhythmias of Sudden Cardiac Arrest Torsades de Pointes 13% Bradycardia 17% VT 62% Bayés de Luna A. Am Heart J. 1989;117:151-159. Primary VF 8% Per 100,000 Standard US Population SCD Rates for Males and Females White Black American Indian/Alaska Native Asian/Pacific Islander 600 502.7 500 407.1 400 336.1 300 270.5 258.8 212.6 200 130.0 100 153.4 0 Males Females . Zheng Z. Circulation. 2001;104(18):2158-2163 Incidence of Sudden Death Increases with Age During a 38 years follow-up of subjects in the Framingham Heart Study, the annual incidence of sudden death increased with age in both men and women.However, at each age, the incidence of sudden death is higher in men than women. (Am Heart J 1998; 136:205) SCD gender 300 270 257 250 232 296 275 272 253 242 241 209 200 150 150 100 50 171 143 133 162 164 174 185 144 122 100 96 93 92 86 82 85 85 84 78 78 72 72 72 65 64 68 61 61 54 20 00 20 01 20 02 20 03 20 04 20 05 20 06 20 07 20 08 20 09 0 No. Death No. SCD MEN FEME SCD age 20 00 20 01 20 02 20 03 20 04 20 05 20 06 20 07 20 08 20 09 200 185 174 171 180 162 164 157 144 160 150 143 133 137 133 122 140 122 123 114 123 113 120 101 97 100 80 60 40 33 40 28 30 27 29 23 21 33 23 20 12 8 5 4 4 2 2 2 1 1 0 No. SCD < 45 45-65 > 65 30% 8% 1% 1% CH F 0% A. AI M M EZ EN TE RI SU CA DD E EN DE AT H 10% 9% FV 13% 14% BO SI S 20% TH RO M 70% IC AH V FOE DE CA M RD A IA C AR RE ST SC D AO RT SH .D CO IS K EC CA . RD IO GE NE S M T % SCD in Clinical Hospital Mostar (10 years) 61% 60% 50% 40% 22% 24% 6% 0% Clinical Substrates Associated with VF Arrest Congestive heart failure • The presence of CHF increases overall mortality and the incidence of SCD in both men and women • AIM ,cardiogenic shock , ICV CHF Predict Increased Sudden Death and Overall Mortality During a 38 years follow-up of subjects in the Framingham Heart Study, the presence of CHF significantly increased sudden death and overall mortality in both men and women. *P <0.001. SCD in CHF 80% 72% 70% 63% 60% 59% 60% 58% 57% 56% 55% 63% 65% 50% 40% 30% 20% 10% %MT SCD 29,32% 28,40% 27,97% 25,15% 23,17% 26,49%26% 22,22% 13,93% 14,37% 20 00 g 20 01 g 20 02 g 20 03 g 20 04 g 20 05 g 20 06 g 20 07 g 20 08 g 20 09 g 0% CHF In people diagnosed with CHF, sudden cardiac death occurs at 6-9 times the rate of the general population.1 American Heart Association. Heart and Stroke Statistical –2003 Update. Dallas, Tex.: American Heart Association: 2002. 1 Clinical Substrates Associated with VF Arrest Myocardial ischemia and infarction • Acute myocardial infarction is associated with an approximate 15% risk of VF within the first 24 to 48 hours, with the incidence falling to only 3 percent over the next several days • When VF is provoked by an AMI, symptoms of the infarction are present for minutes to hours before sudden death occurs; over 80 percent of VF episodes occur within the first 6 hours Control Group Mortality at 2 years SCD Rates in Post-MI Patients with LV Dysfunction 30 28 Total Mortality Arrhythmic Mortality 28 21 20 20 18 16 14 16 12 10 10 19,8 9,4 7 0 TRACE CAPRICORN EMIAT MADIT MUSTT Inducible MUSTT Registry MADIT II* Total Mortality ~20-30%; SCD accounts for ~50% of the total deaths. References in slide notes. * MADIT-II mortality values at 20 months. SCD in AIM 80% 72% 70% 63% 63% 65% 59% 60% 58% 57% 56% 55% 60% 50% 40% 0,2917 0,2649 0,2529 0,2469 0,2339 0,2317 0,1967 20% 0,1867 0,1729 0,1119 10% 30% 20 00 20 g 01 20 g 02 20 g 03 20 g 04 20 g 05 20 g 06 20 g 07 20 g 08 20 g 09 g 0% %MT SCD AIM SCD IN ICV 80% 72% 65% 58% 70% 63% 59% 63% 60% 56% 55% 57% 60% 50% 40% 30% 20 00 20 g 01 20 g 02 20 g 03 20 g 04 20 g 05 20 g 06 20 g 07 20 g 08 20 g 09 g 22,80% 20% 17,82% 16,08% 13,58% 14,05% 14% 13,41% 10,53% 9,02% 10% 2,08% 0% %MT SCD ICV SCD IN SCHOCK CARDIONGENES 80% 70% 63% 60% 72% 60% 59% 58%57% 56% 55% 63% 65% 50% 40% 30% 20% 18,75% 18,03% 17,29% 14,63% 16,08% 12,35% 12,67% 10% 7,60% 8,62% 7,57% 20 00 20 g 01 20 g 02 20 g 03 20 g 04 20 g 05 20 g 06 20 g 07 20 g 08 20 g 09 g 0% %MT SCD Schock cardiogenes SCD in AHF 80% 72% 70% 63% 60% 59% 55% 56% 60% 58%57% 63% 65% 50% 40% %MT SCD 30% AHF-OEDEMA 20% 20 00 20 g 01 20 g 02 20 g 03 20 g 04 20 g 05 20 g 06 20 g 07 20 g 08 20 g 09 g 15,52% 14,29% 13,19% 10,53% 10,66% 10,67% 9,09% 8,02% 10% 8,54% 6,49% 0% SCD in CARDIAC ARREST 80% 70% 63% 60% 58% 59% 56% 55% 57% 60% 72% 63% 65% 50% 40% %MT SCD 30% CARDIAC ARREST 20% 20 00 20 g 01 20 g 02 20 g 03 20 g 04 20 g 05 20 g 06 20 g 07 20 g 08 20 g 09 g 10,67% 10,49% 9,19% 10% 7,02% 8,64% 9,84% 8,05% 7,52% 3,66% 3,47% 0% SCD on the road to Hospital 80% 72% 70% 63% 60% 59% 58% 57% 56% 55% 60% 63% 65% 50% 40% %MT SCD 30% SUDDEN DEATH 20% 20 00 20 g 01 20 g 02 20 g 03 20 g 04 20 g 05 20 g 06 20 g 07 20 g 08 20 g 09 g 16,39% 10,37% 9,72% 10% 6,90% 4,20% 3,24%2% 2,34% 2,26% 2,47% 0% SCA Resuscitation Success vs. Time* 100 90 Chance of success reduced 7 - 10% each minute 80 70 60 % Success *Non-linear 50 40 30 20 10 0 1 2 3 4 5 6 Time (minutes) Cummins RO. Annals Emerg Med. 1989;18:1269-1275. 7 8 9 SCA Chain of Survival Statistics 5% estimated SCA out-of-hospital survival2,3 Even in the best EMS/early defibrillation programs it is difficult to have high survival times due to many SCA events not being witnessed and the difficulty of reaching victims within 6-8 minutes. • 40% SCAs not witnessed or occur in sleep1 • 80% SCAs occur at home1 1 Swagemakers V. J Am Cardiol. 1997;30:1500-1505 2 Ginsburg W. Am J Emer Med. 1998;16:315-319. 3 Cobb LA. Circ. 1992;85:I98-102. Sudden Cardiac Death Incidence 400,000 - 500,000/year in U.S. Only 2% - 15% reach the hospital Half of these die before discharge High recurrence rate Risk of Sudden Death: Data from GISSI-2 Trial 1.00 1.00 0.98 p log-rank 0.002 0.96 Survival Survival 0.96 0.98 0.94 0.92 0.94 0.92 0.90 0.90 0.88 0.88 p log-rank 0.0001 A B 0.86 0.86 0 30 60 90 120 150 180 0 Days Patients without LV Dysfunction 30 60 90 120 Days No PVBs 1-10 PVBs/h > 10 PVBs/h Patients with LV Dysfunction 150 180 People who’ve had a heart attack and have LV dysfunction (less than or equal to 40%) have a sudden death rate that’s similar to a CHF population. “People who’ve had a heart attack have a sudden death rate that’s 4-6 times that of the general population.”1 1American Heart Association. Heart Disease and Stroke Statistics—2003 Update. Dallas, Tex.: American Heart Association; 2002. Treatments to Reduce SCD Correcting Ischemia • Revascularization • Beta-blocker Preventing Plaque Rupture • Statin • ACE inhibitor • Aspirin Stabilizing Autonomic Balance • Beta-blocker • ACE inhibitor Zipes DP. Circulation. 1998;98:2334-2351. Pitt B. N Engl J Med. 2003;348:1309-1321. Improving Pump Function • ACE inhibitor • Beta-blocker Prevention of Arrhythmias • Beta-blocker • Amiodarone Terminating Arrhythmias • ICDs • AEDs Prevent Ventricular Remodeling and Collagen Formation • Aldosterone receptor blockade Symptoms in terminal episodes Type of symptoms Without symptom Summ. % Men % Feme % t p 9 3,63 6 4,02 3 3,03 0,422 p < 0,05 130 52,42 76 51 54 41,54 0,547 p <0,05 10 4,03 6 4,05 4 4,04 0,005 p<0,05 6 2,42 5 3,35 1 1,01 1,113 p< 0,05 10 4,03 5 3,35 5 5,05 0,639 p <0,05 Uncomfortable 1 0,41 0 0 1 1,01 1,005 p< 0,05 Chest pressure 35 14,11 20 13,42 15 15,15 0,379 p< 0,05 Palpitation 3 1,21 3 2,01 0 0 1,749 p< 0,05 Dessines 7 2,82 4 2,68 3 3,03 0,159 p< 0,05 37 14,93 24 16,1 13 13,13 0,656 p<0,05 248 100 149 60,08 99 39,92 Chest pain Dyspnea General failure Nausea Combined symptoms Summary Summary 1 Defibrillation is the only effective treatment for SCA. Few SCA victims are treated quickly enough to survive. Summary 2 High risk SCA patients can be identified: low LVEF, HF, prior MI, and prior SCA or VT/VF event. ICD and CRT-D therapies can prevent SCA. Most eligible patients are not receiving device therapy. Some healthcare organizations have developed care pathways to identify and treat patients at high risk of SCA. Summary 3 Detailed in ESC and ACC/AHA/HRS Device Guidelines for SCD/SCA and VODIČ ZA SCD ESC UKBIH 2010 Epstein AE, et al. Circulation. 2008;117:e350-408.