* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download 08. Odontogenic sinusitis
Survey
Document related concepts
Transcript
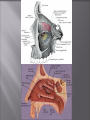
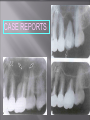
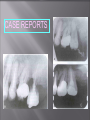
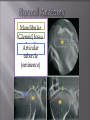
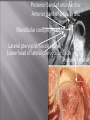
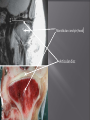
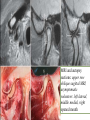
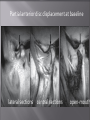
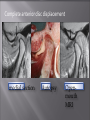
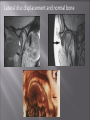
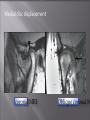
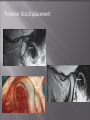
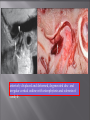
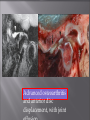
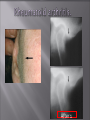
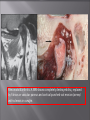
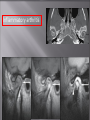
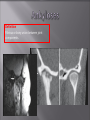
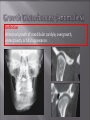
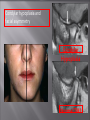
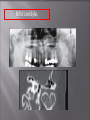
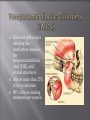
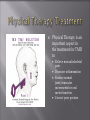
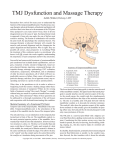
Odontogenic sinusitis: classification, etiology, pathogenesis, clinical features, differential diagnosis, treatment, complications, prevention. arthritis, arthrosis temporomandibular joint (TMJ): classification, clinical course, diagnosis, treatment, complications and prevention. TMJ syndrome of pain disfunction. Surgical TMJ arthroscopy. CLINICAL SYMPTOMS ACUTE SINUSITIS < 3 weeks SUBACUTE SINUSITIS 3 weeks-3 months CHRONIC SINUSITIS > 3 months SYMPTOMS Bloked nose Headache Fever Yellow or green-coloured mucus from the nose Swelling of the face Aching teeth in the upper jaw Loss of the senses of smell and taste Persistent cough Generally feeling unwell MAXILLARY SINUSITIS FROM DENTAL ORIGIN 1.Periapical abscess 2.Periodontal diseases 3.Infected dental cyst 4.Dental material in antrum 5.Oroantral communication 1.Periapical abscess Acute sinusitis Anaerobic organisms 2.Periodontal diseases Lane & O’Neal Chronic sinusitis 5 years examination irrigation + antibiotics communication with the maxillary sinus via a periodontal pocket 3.Infected dental cyst Periapical cyst Most common of all cysts of the oral region Epithelium rest of Malassez The cyst enlarges in to the maxillary sinus 4.Dental material in antrum 1.Displacement of root extraction third molar > second molar > canine Pa or occlusal film 2.Implant 3.Root canal overfilling loss of lamina dura CASE REPORTS CASE REPORTS 1.Antral puncture and sinus irrigation 2.Intranasal antrostomy or Nasoantral Window 3.Caldwell – luc operation 3.Caldwell – luc operation Mandibular condyle Glenoid fossa (head) Articular tubercle (eminence) Posterior band of articular disc Anterior band of articular disc Mandibular condyle (head) Lateral pterygoid muscle raphe Lower head of lateral pterygoid muscle Posterior disc att Mandibular condyle (head) Articular disc MRI and autopsy sections: upper row oblique sagittal MRI, asymptomatic volunteer: left lateral, middle medial, right opened mouth Partial anterior disc displacement at baseline lateral sections central sections open-mouth Complete anterior disc displacement medial section Autopsy Openmouth MRI Lateral disc displacement and normal bone Medial disc displacement coronal MRI Oblique coronal M Posterior disc displacement Definition Non-inflammatory focal degenerative disorder of synovial joints, primarily affecting articular cartilage and sub-condylar bone; initiated by deterioration of articular soft-tissue cover and exposure of bone. Clinical Features Crepitation sounds from joint(s) Restricted or normal mouth opening capacity Pain or no pain from joint areas and/or of mastication muscles Occasionally, joints may show inflammatory signs Women more frequent than men anteriorly displaced and deformed, degenerated disc and irregular cortical outline with osteophytosis and sclerosis of condyle . Advanced osteoarthritis and anterior disc displacement, with joint Imaging Features •Abnormal signal on T2-weighted image from condyle marrow: increased signal indicates marrow edema; reduced signal indicates marrow sclerosis or fibrosis •Combination of marrow edema signal and marrow sclerosis signal in condyle most reliable sign for histologic diagnosis of osteonecrosis •Marrow sclerosis signal may indicate advanced osteoarthritis without osteonecrosis, or osteonecrosis Definition Inflammation of synovial membrane characterized by edema, cellular accumulation, and synovial proliferation (villous formation). Clinical Features Swelling of joint area, not frequently seen in TMJ Pain (in active disease) from joints Restricted mouth opening capacity Morning stiffness, in particular stiff neck Dental occlusion problems; “my bite doesn’t fit” Crepitation due to secondary osteoarthritis After 1 Rheumatoid arthritis. A MRI shows completely destroyed disc, replaced by fibrous or vascular pannus and cortical punched-out erosion (arrow) with sclerosis in condyle. Psoriatic arthropathy. Oblique coronal and oblique sagittal CT images show punched-out erosion in lateral part of condyle (arrow). Psoriatic arthropathy. MRI shows contrast enhancement within bone erosion and in joint space, consistent with thickened synovium/pannus formation. Openmouth MRI shows reduced condylar translation but normally located disc (and normal bone in this section) Inflammatory arthritis Definition Fibrous or bony union between joint components. Definition Abnormal growth of mandibular condyle; overgrowth, undergrowth, or bifid appearance. Condylar hypoplasia and facial asymmetry Condylar Hypoplasia Normal TMJ Bifid condyle. Calcium Pyrophosphate Dehydrate Crystal Deposition Disease (Pseudogout) Synovial Chondromatosis Benign tumor characterized by cartilaginous metaplasia of synovial membrane, usually in knee, producing small nodules of cartilage, which essentially separate from membrane to become loose bodies that may ossify. Different pathologies affecting the masticatory muscles, the temporomandibular joint (TMJ), and related structures Affects more than 25% of the population 90% of those seeking treatment are women Facial pains/Muscle spasms Pain/tenderness in the muscles of mastication and joint Joint sounds (popping, clicking) Limited jaw motion Jaw locking open or closed Headaches Teeth grinding Abnormal swallowing Uncomfortable “off” bite Inability to comfortably open/close mouth Dizziness/vertigo Ringing in the ears Visual disturbances Insomnia Tingling in hands/fingers Deviation of jaw to one side Osseous Anatomy The articulation between the condyles of the mandible and the temporal bone, which is part of the cranium. The articular surface of the condyle is convex and the articular eminence of the temporal bone is concave. Working together: Dentists Orthodontists Psychologists Physical Therapists Ear, Nose, Throat Doctor Physicians Alternative Medicine MRI X-Ray Dental examination for bite alignment Physical Therapy is an important aspect in the treatment for TMD to: Relieve musculoskeletal pain Decrease inflammation Restore normal joint/muscular movements for oral motor function Correct poor posture History Posture Watch, feel, listen to jaw with AROM Opening between 40-50mm Protrusion/retraction between 8-10mm Lateral deviation while opening (S or C curve) Lateral excursion 8-10mm Ligamentous Laxity testing Transverse Ligament Alar Ligament Cervical ROM testing Palpate joints/muscles for tenderness Therapeutic Exercises Manual Therapy Modalities Electromyographic (EMG) Biofeedback Dental Splint Improve muscular coordination Increase muscular strength Postural exercises Active ROM exercises Muscles of mastication Cervical spine muscles General mobility Make a “clicking” sound with the tongue on the roof of the mouth. This slightly opens the jaw with the tongue on the palate behind the front teeth, which is the resting position of the jaw and the first portion of relaxation exercises. Place tip of tongue on palate behind teeth and draw small circles. Place tip of tongue on hard palate and blow air out, rolling the tongue, or making a “r r r r” sound. Begin with proper resting position of the jaw. Teach the patient control while elevating and depressing the mandible throughout the first half of the ROM. Keeping the tongue on the roof of the mouth, the patient opens the mouth while trying to keep the chin in midline. Use a mirror for visual reinforcement. If the jaw deviates to one side, teach the patient to practice lateral deviation to the opposite side without creating pain or excessive motion. Long Axis Distraction: Sitting/Supine PT positioned opposite of affected side Use hand opposite of affected jt. side Thumb in mouth on last molar Apply gentle downward pressure with thumb Hold for ~30 seconds 23x/session Bilaterally Anterior Glide Same hand placement Slightly distract using DIP of thumb while gliding anteriorly Oscillate for 30 seconds Lateral Glide Thumb on tongue side of last molar Use whole hand to oscillate laterally Medial Glide Stand on affected side Thumb on lateral side of last molar Glide medially Avoid: Large bites Excessive chewing Removing food from teeth with tongue Gum chewing Chewy foods: bagels, sandwiches, steak, ice, crunchy fruits/vegetables, caramel, nuts etc. Relaxation techniques to reduce stress/muscle tension Maintain good posture 5-10 % dx w/TMJ Dysfunction fail to have relief of medical tx, and require surgery Antiinflammatories, soft diet, hot compresses, muscle relaxants >2 weeks: intraoral occlusion splints, med tx Recurrent or chronic: permanent dental correction Patient Factors Outpatient H& P, Blood chemistries, CBC, PT, PTT, U/A, serum HCG, Chest x-ray or ECG as appropriate Room Set-up X-rays in room Position during procedure Supplies and equipment Arm sleds, headring pillow Special considerations: high risk areas Supine w/head donut pillow, tuck arms to side Elbows—ulnar nerves Prep Shave preauricular area Cotton to ears to prevent pooling of povidone-iodine & caution w/eyes; entire facial area prepped from hairline, down to shoulder, and laterally to include mouth and chin Special considerations Nasal intubation Prophylactic antibiotics & steriods State/Describe incision Small stab incision w/# 11 before trocar is introduced at superior joint space General: basic pack drape and split head sheet, gowns & gloves, towels, basin set, prep set, sterile adhesive wound drape, irrigation pouch, skin marker, raytex, Specific Suture & Blades (# 11) Medications on field (name & purpose) Catheters & Drains: n/a Drapes: head turban for initial drape; pad pt forehead with a folded towel; plastic adhesive wound drape to cover ET tube and mouth; split sheet and large sheet for body drape, (laser: 4 wet towels around pt’s face; moistened cotton in external auditory canals, irrigation collection pouch at base of ear and TMJ) 2 60 mL syringes 4 10 mL syringes 1 1-mL syringe Needles: 18 g, 21 g, 25 g Skin stapler Eye pads Sterile water and saline 1000 mL Lactated Ringers for irrigation 30 in extension tubing Stopcock General: suction, Lactated Ringer’s IV bag for irrigation, marking pen Specific TMJ instrument set 0 degree arthroscope 30-degree arthroscope 70-degree arthroscope Cannulas Sharp & dull obturators Light cord, camera & cord, small joint rotary shaver General: suction system Specific Monitor/light source/camera tower, shaver control unit, IV pole for irrigant Fluid infusion system Bipolar ESU Holmium laser Irrigation solution is injected into the joint space to distend the capsule LR solution is preloaded in syringe w/needle attached. After small stab incision is placed, surgeon inserts a sheath w/sharp obturator into superior joint space. After space is entered, the sharp is replaced with a dull obturator to further direct the sheath into the joint without damaging the intraarticular tissue or adjacent neurovascular structures. #11 blade with # 7 handle will be ready Trocar/cannula is preassembled. Expect trocor to be returned. Be prepared to assist with connections of video/light cord connections. Irrigation is infused into the joint LR solution is connected to the cannua via extension tubing Joint is examined Prepare to operate remote control for still photos If functional surgery is needed, a second stab wound is made Pass skin knife. Prepare additional equipment (probe, shaver, grasper) Final visual inspection is performed Additional photos may be taken Cannuale are removed and excess fluid removed Wound is closed and dressing placed Prepare for closure; count Pass suture; prepare dressings, reorganize equipment & supplies if procedure is bilateral Steps may be repeated contralaterally Repeat steps Thank you