* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Papules, Purpura, Petechia and Other Pediatric Problems: A
Neglected tropical diseases wikipedia , lookup
Herpes simplex wikipedia , lookup
Meningococcal disease wikipedia , lookup
Marburg virus disease wikipedia , lookup
Cysticercosis wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Typhoid fever wikipedia , lookup
Dirofilaria immitis wikipedia , lookup
Gastroenteritis wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Neonatal infection wikipedia , lookup
Leishmaniasis wikipedia , lookup
Hepatitis C wikipedia , lookup
African trypanosomiasis wikipedia , lookup
Hepatitis B wikipedia , lookup
Visceral leishmaniasis wikipedia , lookup
Neisseria meningitidis wikipedia , lookup
Onchocerciasis wikipedia , lookup
Leptospirosis wikipedia , lookup
Oesophagostomum wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Rocky Mountain spotted fever wikipedia , lookup
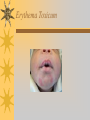
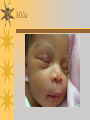
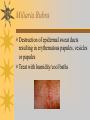
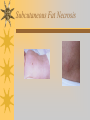
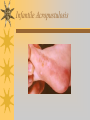
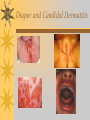
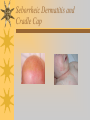
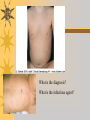
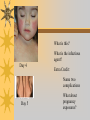
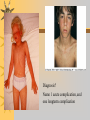
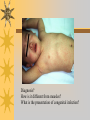
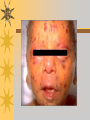
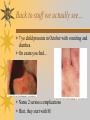
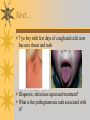
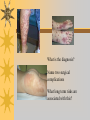
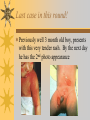
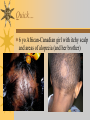
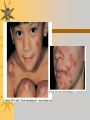
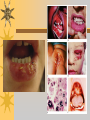
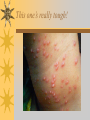
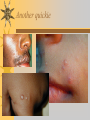
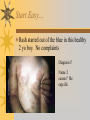
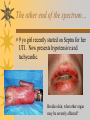
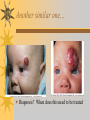
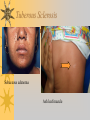
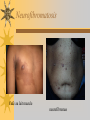
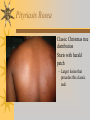
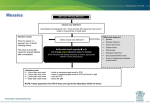
Papules, Purpura, Petechia and Other Pediatric Problems: A Review of Peds Derm David Chaulk PEM Fellow April 15th, 2004 Neonatal Nasties… Erythema Toxicum Bad name…not toxic Usually occurs in first days of life 50% of healthy babies Erythematous macules +/- pustules and papules Etiology unknown No treatment necessary Erythema Toxicum Milia Retention of keratin and sebaceous material Usually disappears by 3-4 weeks No treatment Milia Miliaria Rubra Destruction of epidermal sweat ducts resulting in erythematous papules, vesicles or papules Treat with humidity/cool baths Subcutaneous Fat Necrosis Secondary to pressure in utero or during labour Occurs during first days or weeks Circumscribed erythematous or violaceous plaques Infrequently associated with hypercalcemia Subcutaneous Fat Necrosis Infantile Acropustulosis As it says… Pustules (vesicles) on the hands, feet and dorsal surfaces Intensely pruritic and recurrent Occurs between 2-10 mos and resolves 2436 mos Treated with anithistamines and fluorinated corticosteroids if severe Infantile Acropustulosis Infantile Acne Closed comedones and inflammatory papules May last 1-2 years Usually family history Most don’t require treatment May use topical treatment such as benzoyl peroxide Diaper and Candidal Dermatitis Contact diaper dermatitis is caused by irritants, soaps detergents etc. Candida is differentiated by satellite lesions – Widespread, pinpoint raised erythematous lesions with white scales – GI source and frequently post antibiotics Diaper and Candidal Dermatitis Seborrheic Dermatitis and Cradle Cap Mainly involves scalp, face, trunk and intertriginous areas Greasy, scaly, patch erythema Unknown etiology Treatment is hydration, mineral oil, petroleum, shampoos Seborrheic Dermatitis and Cradle Cap The Rash Relay! Two teams, limited info. & Spot Diagnosis Start with Infectious Stuff… First one’s easy…or is it? 3 yo girl, second visit to ED in four days. First time, high fever without clear focus. No other symptoms. Now returns with rash and fever has resolved What is the diagnosis? What is the infectious agent? Roseola Infantum Macular or maculopapular rash appearing after defervescence on 3rd or 4th day of illness Child usually looks well despite high fever and it is often associated with febrile seizure Human herpes virus 6 (HHV-6) Another easy one… It’s spring, you’re in the ED seeing a 6 yo girl with a rash. Yesterday it was only on her cheeks now it’s on her arms (extensors) What is this? What is the infectious agent? Day 4 Extra Credit: Name two complications Day 5 What about pregnancy exposures? Parvovirus B19 Aka: erythema infectiosum and fifth disease Usually affects kids aged 3-12 years Most common is spring 6-14 day incubation period Day 1:slapped cheek Day 2:lacy, erythematous rash on extensors Day 6 fading rash with lacy, marble appearance Parvovirus B19 Complications: – Arthritis, aplastic anemia and hemolytic anemia Pregnancy – – – – 50% of women seropositive before pregnancy Likelihood of transmission if exposed 30-50% If fetus infected 2-10% rate of loss Thus risk is actually fairly low Now for a couple of hard ones… 3 yo girl with high fever, cough, runny nose, looks unwell. Rash started on face initially and is now spreading. Parents are granola types and the child isn’t immunized Diagnosis? Name 1 acute complication, and one longterm complication Measles (Rubeola) Starts with cough, coryza and conjunctivitis, then Koplik spots and morbilliform rash Rash fades after 3-7 days in same order that it started Acute complications: OM and pneumomia Long term: SSPE Another tough one… This time a 2 year old unimmunized child, presents with 3 days history of URT symptoms. Parents bring him in because they notice his glands are swollen and he has a rash Diagnosis? How is it different from measles? What is the presentation of congenital infection? Rubella Generalized maculopapular rash with cervical, postauricular and occipital LN 3-5 days of viral prodrome followed by mobile rash that goes from head to toe in 24h May get petechiae on the palate Essentially not as sick/ not as high fever as measles These are the blueberry babies Back to stuff we actually see… 7 yo child presents in October with vomiting and diarrhea On exam you find… Name 2 serious complications Hint, they start with M Coxsackie Hand, Foot and Mouth Disease Highly contagious and usually occurs in late summer, fall Viral illness precedes rash, start as macules and evolve into vesicles 25-65% get lesions on hands and feet Usually get lymphadenopathy and may get dehydration Serious but rare complications include myocarditis and meningoencephalitis Next… 7 yo boy with few days of cough and cold, now has sore throat and rash Diagnosis, infectious agent and treatment? What is the pathognomonic rash associated with it? Scarlet Fever Exotoxin mediated rash secondary to GAS infection of the pharynx or skin Oral mucosal rash (petechial), strawberry tongue Erythematous, blanchable, generalized rash Intense in skin folds with linear, petechial eruptions – Pastia Lines May get desquamation 5 days post Treat with Penicillin Gotta know this one… 4 year old girl, sick for a week now, cough runny nose, rash. Parents bring her in because she cries all the time Name the diagnostic criteria What is the treament What are we trying to prevent with treatment? Kawasaki’s Disease FEEL My Conjunctivits Fever – greater than 5 days plus four of: Extremitity changes (erythema, edema) Erythematous Rash (can be any rash except petechial) Lymphadenopathy (>1.5 cm, may be unilateral) Mucositis (bright red lips, strawberry tongue) Conjunctivitis (bilateral, non-purulent) Kawasaki’s Disease Other frequently associated findings: – – – – – – – – Irritability (~90%) Urethritis/sterile pyuria (70%) Aseptic meningitis (50%) Hepatitis (30%) Arthralgia/arthritis (10-20%) Hydrops of the gallbladder (10%) Myocarditis/CHF (5%) uveitis Kawasaki’s Disease Untreated 20% will develop coronary aneurysms with treatment less than 5% Treatment – IVIG 2 g/kg – High dose ASA 80-100 mg/kg until afebrile then: – Low dose ASA 5 mg/kg for 6-8 weeks if no evidence of aneurysms Case I had last week… Todd no comments: 4 yo girl with one week history of rash Started on steroids by fp, not improving, thinks they are getting worse. Also complaining of ankle pain and swelling What is the diagnosis? Name two surgical complications What long term risks are associated with this? Henoch-Schonlein Purpura Unknown etiology but frequently follows viral infection ? Autoimmune Rash is erythematous papules followed by purpura Frequently associated with joint pain and swelling Abdo pain not uncommon, sometimes as presenting feature Henoch-Schonlein Purpura Surgical Complications Include: – Intussusception – Testicular torsion Long term complications: – Glomuerulonephritis/renal disease – Hypertension No effective treatment. – Soft evidence for steroids reducing abdominal pain and risk of torsion. Not effective for rash. Last case in this round! Previously well 3 month old boy, presents with this very tender rash. By the next day he has the 2nd photo appearance Staphylococcal Scalded Skin Syndrome AKA TEN (toxic epidermal necrolysis) Exotoxin mediated reaction to coagulase positive staphylococcal infection In adults more commonly caused by drug reaction Rash is initially erythematous, sandpaper like and very tender Staphylococcal Scalded Skin Syndrome After 2-3 days skin will peel (Nikolsky sign) Pathognomonic facies, crusting perioral erythema with fissures at the nasolabial folds and corner of mouth Spares MM, palms and soles Now for the speed round Spot Diagnosis First 10 yo girl, very itchy rash mostly affecting web spaces Scabies The culprit Sarcoptes scabeii Scabies Usual locations Scabies Spread by skin to skin contact and causes extreme pruritis Frequent secondary infections The mite tunnels into the stratum corneum and lives in burrows Scabies Treatment is 5% permethrim, underwear and sheets need to be washed in hot water Family needs to be treated as well Pregnant women and children less than 6 mos treated with sulfur Quick… 6 yo African-Canadian girl with itchy scalp and areas of alopecia (and her brother) Tinea capitis Superficial infection caused by dermatophytes Annular configuration with erythema and scaling Treated treated with antifungals If not improving think secondary infection Starting to feel itchy yet… 7 yo Oriental girl was playing in sandbox last week. Given topical antibiotics. Not improving. Rash now spreading to other areas of the body. Some look like blisters that have broken open according to the mom. Impetigo Caused by strep or staph Mainly face, head neck and extremities affected Classically honey crusted appearance May be bullous or vesiculopustular form Treated systemically with 1st or 2nd gen cephalosporin Also important to treat topically Herpes Simplex Vesicular lesions on an erythematous base Kids usually get primary gingivostomatitis Heals within 2-4 weeks Recurrence not usually as severe unless immunocompromised This one’s really tough! Varicella Zoster “dew drop on a rose pedal” Won’t get into a whole lot Watch for secondary infection…necrotising fascitis Older children/adults more likely to have complicated course – Pneumonitis, encephalitis, hepatitis, myocarditis Infectious before vesicles appear until all are crusted Another quickie Molluscum Contagiosum Viral (DNA pox virus) Dome shaped umbilicated papule Highly contagious and auto-inoculable Treatment is curettage, freezing, or they will resolve on there own in 6-9 mos What is the problem with the vaccine for this illness? Meningococcemia Immediate Management – – – – ABC’s, Labs (w/coags), IV access Less than 1 mo amp and cefotaxime More than 1 mo, cefotax and vanco Supportive Measures Close/high risk contacts prophylactic cipro Vaccine covers A,C,Y, W135 but 35-40% of cases are due to B The Rash Relay Part II Non-Infectious Rashes Start Easy… Rash started out of the blue in this healthy 2 yo boy. No complaints Diagnosis? Name 2 causes? Be sepcific Erythema Multiforme Macules, papules and pathognomonic target or iris lesions Often idiopathic, maybe secondary to drugs (sulfa’s, dilantin, barbituates). May also be secondary to HSV or Mycoplasma The other end of the spectrum… 9 yo girl recently started on Septra for her UTI. Now presents hypotensive and tachycardic. Besides skin, what other organ may be severely affected? Stevens-Johnson Syndrome Also known as EM major Severe bullous erythema with mucocutaneous involvement Can have severe eye involvement – corneal ulcerations, uveitis Causes the same as EM, often due to HSV Treatment is supportive care and wound management Next… 14 yo boy with a chronic illness and recently noticed the following painful rash on his legs Diagnosis What chronic disease does this boy likely have? Erythema Nodusum Deep, tender erythematous, nodules on extensor surfaces of extremities Often secondary to infections (strep is common), IBD, sarcoidosis and drugs (commonly OCP) Treat underlying cause Just the picture… Diagnosis? Name two complications Sturge-Weber Syndrome Nevus Flammeus or port wine stain in V1 trigeminal distribution Made up of mature, dilated dermal capillaries Associated with seizures, hemiparesis, intracranial calcifications and glaucoma Another similar one… Diagnosis? When does this need to be treated Strawberry Hemangioma Dilated capillaries present at birth Usually worse in first 6 mos and resolve by 5 years May be multiple and associated with thrombocytopenia and consumptive coagulpathy Treatment only required if interfering with vital structure (eg., vision) Getting close to the end! Diagnosis? What treatments do you think were used? Atopic Dermatitis/Eczema Pruritic inflammation of the epidermis in a patient who has or a family history of atopy Commonly secondarily affected Treatment includes moisturizers and emollients, topical steroids, systemic steroids in more severe cases and immune modulators like tacrolimus The End is Near… Some things you should recognize but we won’t talk about! Tuberous Sclerosis Sebaceous adenoma Ash leaf macule Neurofibromatosis Café au lait macule neurofibromas Pityriasis Rosea Classic Christmas tree distribution Starts with herald patch – Larger lesion that precedes this classic rash Child Abuse lighter slap Lamp cord slap Hot water submersion Ehlers-Danlos Party Trick Gorlin Sign The End!