* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Stomach and Peptic Ulcer Disease
Survey
Document related concepts
Gastroenteritis wikipedia , lookup
Rocky Mountain spotted fever wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
Meningococcal disease wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Oesophagostomum wikipedia , lookup
Eradication of infectious diseases wikipedia , lookup
Schistosomiasis wikipedia , lookup
Onchocerciasis wikipedia , lookup
Chagas disease wikipedia , lookup
Leptospirosis wikipedia , lookup
Leishmaniasis wikipedia , lookup
Visceral leishmaniasis wikipedia , lookup
Transcript
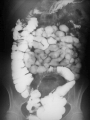
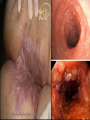
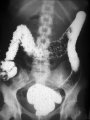
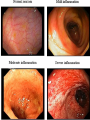
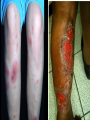
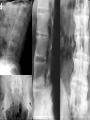
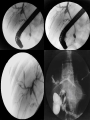
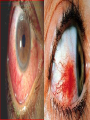
Inflammatory Bowel Disease Internal Medicine Lecture Series November 21, 2007 Ron Barac, D.O. Inflammatory Bowel Disease Crohn’s disease Ulcerative colitis Pathogenesis of IBD is unknown! Familial Patterns of IBD 10-25% occurrence of IBD in relatives Strong concordance by disease category Genetic vs. environmental influences still unresolved Etiological theories of IBD Genetic Smoking Dietary Infection Immunological Psychogenic? Epidemiology of IBD Factor Ulcerative Colitis Crohn’s Disease Incidence (per 100,000) 2-10 1-6 Prevalence (per 100,000) 35-100 10-100 Racial incidence High in whites High in whites Ethnic incidence High in Jews High in Jews Sex Slight female preponderance Slight female preponderance Age of onset 15-25 ?55-65 15-25 ?55-65 Smoking Fewer smokers than expected More smokers than expected Crohn’s disease First documented case by Morgagni in 1761 Crohn’s disease - Description Chronic inflammation that may involve any part of the GI tract from mouth to anus. • associated with many extraintestinal features Frequently manifested by abdominal pain and diarrhea Often complicated by intestinal fistulization, obstruction or both. Typically affects the ileum, colon, and/or perianal region Distribution is asymmetric/segmental Tendency toward lifelong recurrence Crohn’s Disease - Pathology Earliest/most frequent mucosal lesion: crypt injury secondary to neutrophil infiltration Distribution of crypt lesions is typically more focal Crypt injury is followed by microscopic ulceration of intestinal mucosa over a lymphoid follicle Macrophage/other inflammatory cells invade and proliferate in the lamina propria. Loose aggregates of macrophages ultimately organize into discrete noncaseating granulomas, which consist of epithelioid cells with multinucleated giant cells. While granulomas seem to be a pathognomonic feature of Crohn’s disease, absence of granulomas does not rule out the diagnosis. Crohn’s Disease – Clinical Presentation Pain - colicky RLQ/suprapubic region Diarrhea Fever - usually low grade, higher spiking fevers signify complications Weight loss - typically 10-20% of body weight Gross bleeding - unusual, massive bleeding in only 12% Perineal disease - fissures/fistulas and/or abscesses Crohn’s disease Flexible sigmoidoscopy: • rectal sparing is common • distal colon may be unremarkable or mildly erythematous in 50-70% of patients Colonoscopy: • contraindicated in acute Crohn’s disease • mucosal involvement is discontinuous with intervening “skip” areas of normal mucosa Plain films of abdomen UGI/small bowel series • 60-70% of patients have some ileum involvement Barium enema Crohn’s Disease Complications Fistula formation • • • • enterocutaneous enterovesical enteroenteric/enterocolic rectovaginal/rectovesical Intraabdominal abscess Bowel obstruction Growth failure in pediatric/adolescent patients Malignancy • gastrointestinal • squamous cell CA of anus • squamous cell CA of vulva Ulcerative Colitis First recognized by Wilkes in 1859 Ulcerative Colitis Inflammatory disorder that affects the rectum and extends proximally to affect a variable extent of the colon. Cause of the disease and factors determining its clinical course are unknown. Ulcerative Colitis - Pathology Inflammation predominantly confined to the mucosa/submucosa Characteristic histologic finding in UC is the crypt abscess • crypt abscesses are not specific for UC though Crypt abscesses are comprised of PMNs and degenerated or necrotic epithelial cells in the crypts of Lieberkuhn. Coalescence of adjacent crypt abscesses produce the mucosal ulcerations which typify ulcerative colitis. Ulcerative Colitis – Clinical Presentation Hematochezia Diarrhea - not always present Pain - lower abdominal/crampy, relieved by BM’s Fever - only seen in severe cases Weight loss Clinical assessment of disease severity Mild: (60% of patients) • < 4 stools per day with or without blood, with no systemic disturbances and normal ESR. Moderate: (25% of patients) • > 4 stools per day but with minimal systemic disturbances Severe: (15% of patients) • > 6 stools daily with blood and evidence of systemic disturbance as shown by fever, tachycardia, anemia, or an ESR > 30. Ulcerative Colitis Flexible sigmoidoscopy: • • • • assess disease activity in acute UC Rectal involvement in 95% cases of UC Mucosal involvement is continuous and non-segmented Mucosa is granular/friable with discrete ulcerations Colonoscopy: • relatively contraindicated in acute UC due to increased risk of perforation. • useful in chronic UC to evaluate disease extent, evaluate strictures, and surveillance of colonic CA Plain films of abdomen Barium enema: • contraindicated in acute UC • useful in chronic UC – “lead pipe” colon • colonic strictures should be considered malignant until proven otherwise Ulcerative Colitis Complications Toxic megacolon Free perforation Massive colonic hemorrhage Colon cancer: • Major risk factors are extent and duration of disease • Colonoscopic surveillance with biopsies should be done yearly in patients with universal colitis of 10 yrs. duration or left-sided colitis of 20 yrs. duration. Exclusion of Infectious Colitis Exclusion of infectious Colitis may be clinically, endoscopically, and histologically indistinguishable from IBD. • stool for ova and parasites • stool cultures for enteric pathogens Patients with proctitis • exclude STDs if there is a history of anal intercourse Patients with diarrhea and recent antibiotic use • exclude pseudomembranous colitis • check stools for C. difficile toxin Extraintestinal Manifestations of IBD 33% of IBD patients will have one or more manifestations in their lifetime. Extraintestinal manifestations may be related to bowel disease activity, may be independent of bowel disease, or may occur as a consequence of bowel disease. • • • • • Dermatologic Rheumatologic Hepatobiliary Ocular Renal Dermatologic manifestations Erythema nodosum • most common skin manifestation of IBD • occurs in 9% of UC, 15% of CD • directly related to bowel disease activity and resolves with control of the disease • erythema nodosum is non-specific for IBD Pyoderma gangrenosum • occurs in 2-5% UC, 1-2% of CD • clinical course is independent of bowel disease • treatment with intralesional/systemic steroids Rheumatologic manifestations Axial arthritis • Ankylosing spondylitis 18-20% of patients with IBD, more common in males clinical course independent of bowel disease assoicated with HLA-B27 haplotype “bamboo” spine on plain x-rays • Sacroilitis independent of bowel disease associated with HLA-B27 haplotype plain films show obliteration of sacroiliac joint space Peripheral arthritis • Activity parallels bowel disease activity • Peripheral arthritis in IBD is mono-articular (affects large joints such as knee, wrist, ankles), asymmetric, migratory, seronegative, and is unassociated with deformity or erosive changes. Hepatobiliary Manifestations Primary sclerosing cholangitis • • • • • • 4-6% of patients with UC 70% of patients with PSC have UC associated with DRW-52A haplotype clinical course is independent of bowel disease diagnosis made by ERCP; suggested by liver biopsy cholangiocarcinoma is a complication of PSC Pericholangitis Cholelithiasis • cholesterol stones may occur in CD patients with terminal ileal involvement • Occurs in 15-30% of patients with small bowel CD • Resection or disruption of ileal absorptive surface causes alteration of enterohepatic circulation and bile salt depletion Chronic active hepatitis Ocular Manifestations Uveitis • Clinical course is independent of bowel disease activity • Associated with HLA-B27 haplotype • Clinical presentation is painful, injected eye with opacity in the anterior chamber. Episcleritis Renal Manifestations Nephrolithiasis • Urate stones associated with ulcerative colitis • Oxate stones associated with Crohn’s disease Obstructive hydronephritis • Associated with Crohn’s disease but not UC • Caused by local extension of bowel inflammation to ureters Pyelonephritis IBD TREATMENT Aminosalicylates Used for both CD and UC Active component is 5-aminosalicyclic acid (5-ASA) Mode of action • inhibition of lipoxygenase enzyme in the alternate arachidonic acid pathway resulting in decreased production of leukotrienes Examples: • sulfasalazine (Azulfidine), olsalazine (Dipentum), mesalamine (Pentasa, Asacol), topical mesalamine (Rowasa) Both oral/topical forms are effective in maintaining remission in UC. Sulfasalazine 5-ASA linked by an azo bond to sulfapyridine Azo bond is split by bacteria in distal ileum/colon releasing the active 5-ASA moiety 90% of the adverse effects of sulfasalazine are related to the sulfapyridine moiety Adverse effects include: • • • • Rash, fever, headaches Reversible male infertility Folate deficiency Agranulocytosis Indications: • Mild to moderate UC • Mild to moderate Crohn’s colitis, ileocolitis, less effective in Crohn’s ileitis • Maintenance of remission in UC Sulfasalazine – Safety in Pregnancy and Breast Feeding Crosses placenta and appears in milk No adverse effect on pregnancy No teratogenicity No kernicterus Mesalamine Active moiety is 5-ASA Adverse effects: • Nausea, flatulence, diarrhea • Fever, rash • Pancreatitis, pericarditis, colitis Indications: • same as for sulfasalazine STEROIDS Systemic corticosteroids: • Indicated in short term treatment of moderate/severe UC or CD • Not shown to maintain remission in either UC or CD • Preparations: Oral: prednisone, prednisolone Parental: hydrocortisone, corticotropin (ACTH) Topical corticosteroids • Indicated in treatments of proctitis or leftsided colitis • Advantage is minimalization of systemic effects of steroids • Preparation: hydrocortisone enemas Budesonide (controlled ileal release) • Corticosteroid with high 1st-pass hepatic metabolism • Used as an alternative to prednisone • Effective in mild to moderately active Crohn’s ileitis and/or right colon involvement • Effective for prolongation of time to relapse and maintenance • More effective than mesalamine for maintenance of remission of patients with steroid-dependent Crohn’s disease Metronidazole Indications: • fulminant UC • active CD (mild/moderate) • perianal disease/fistulae Adverse effects: • peripheral neuropathy • disulfiram-like reaction • teratogenicity precludes use in pregnancy Immunosuppressive agents 6-Mercaptopurine (6-MP) and Azathioprine are the only medications known to induce/maintain remission in CD Indications: • • • • • steroid-dependent refractory disease perianal disease refractory fistulae maintenance of remission Disadvantage is delay in response to treatment • mean time of clinical response is 3-4 months Complications of treatment: • • • • neutropenia bone marrow suppression – 2% cases pancreatitis – 3.3% lymphoma Cyclosporine: • may have role in acute or severe UC/CD • Has quick onset of action but limited by serious side effects. Infiximab • Chimeric mouse/human monoclonic antibody against tumor necrosis factor alpha • Used in moderate to severe Crohn’s and ulcerative colitis • Very active for fistulizing Crohn’s disease • Useful for both induction & maintenance of remission • Patients should be evaluated for latent TB prior to treatment (can also be associated with reactivation of HBV infection) • Possible association with rare lymphomas Surgical Management of IBD Ulcerative colitis • Proctocolectomy with ileostomy • Ileoanal anastomosis Crohn’s disease • Stricturoplasty • Fistulectomy • Segmental resection