* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Carbohydrate Metabolism - BITS Academic Resource Center
Metalloprotein wikipedia , lookup
Biochemical cascade wikipedia , lookup
Photosynthesis wikipedia , lookup
Mitochondrion wikipedia , lookup
Butyric acid wikipedia , lookup
Fatty acid synthesis wikipedia , lookup
Basal metabolic rate wikipedia , lookup
Amino acid synthesis wikipedia , lookup
Photosynthetic reaction centre wikipedia , lookup
Biosynthesis wikipedia , lookup
NADH:ubiquinone oxidoreductase (H+-translocating) wikipedia , lookup
Nicotinamide adenine dinucleotide wikipedia , lookup
Evolution of metal ions in biological systems wikipedia , lookup
Fatty acid metabolism wikipedia , lookup
Light-dependent reactions wikipedia , lookup
Electron transport chain wikipedia , lookup
Microbial metabolism wikipedia , lookup
Glyceroneogenesis wikipedia , lookup
Phosphorylation wikipedia , lookup
Blood sugar level wikipedia , lookup
Adenosine triphosphate wikipedia , lookup
Oxidative phosphorylation wikipedia , lookup
Biochemistry wikipedia , lookup
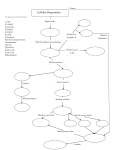
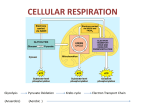
Carbohydrate Metabolism Carbohydrate Metabolism Carbohydrate metabolism is a fundamental biochemical process that ensures a constant supply of energy to living cells. The most important carbohydrate is glucose, which can be broken down via glycolysis, enter into the Kreb's cycle and oxidative phosphorylation to generate ATP. Oxidative phosphorylation is a combination of two simultaneous processes; the electron transport chain and chemiosmotic coupling. The electron transport chain (also known as the respiratory chain) comprises 4 complexes located in the inner mitochondrial membrane. NADH and FADH2, produced from glycolysis and the Krebs cycle, release electrons at certain points in the chain, which are passed from one electron acceptor to the next. Each time an electron is passed from one complex to the next, it loses energy. Chemiosmotic coupling harnesses the energy from the electron transport chain and uses it to transport H+ across the inner mitochondrial membrane, establishing a concentration gradient. ATP synthase is found in the inner mitochondrial membrane and this enzyme uses the energy from H+ ion flux to synthesize ATP. Three ATP molecules can be made from each pair of electrons from NADH and two ATP molecules are made from a pair of electrons from FADH2. Further important pathways in carbohydrate metabolism include, pentose phosphate pathway (conversion of hexose sugars into pentoses) Glycogenesis (conversion of excess glucose into glycogen, stimulated by insulin) Glycogenolysis (conversion of glycogen polymers into glucose, stimulated by glucagon) Gluconeogenesis (de novo glucose synthesis). Amino acids and Glycerol can be used to produce glucose (liver) More glucose is produced via gluconeogenesis than glycogenolysis. Glycolysis is the breakdown of glucose into pyruvic acid There are multiple diseases that arise from improper carbohydrate metabolism, Diabetes Mellitusis caused by a lack of, or a resistance to, insulin leading to hypo- or hyperglycemia. Lactose intolerance is a common allergy in adults and results from a lack of the enzyme lactase, which converts lactose disaccharides (found in dairy products) into glucose monosaccharides. Much rarer diseases such as galactosemia and von Gierke's diseases are caused by congenital mutations in enzymes involved in glucose metabolic pathways. Metabolism Anabolism: Food supplies raw materials for synthesis reactions. Synthesize: DNA and RNA. Proteins. Triglycerides. Glycogen. Catabolism: Hydrolysis (break down monomers down to CO2 and H2O): Hydrolysis reactions and cellular respiration. Gluconeogenesis. Glycogenolysis. Lipolysis. Amphibolism: Acts as link between the anabolic and catabolic pathways. (e. g) TCA Cycle Balance Between Anabolism and Catabolism The rate of deposit and withdrawal of energy substrates, and the conversion of 1 type of energy substrate into another; are regulated by hormones. Antagonistic effects of insulin, glucagon, GH, T3 and cortisol balance anabolism and catabolism. Insert fig. 19.4 How do we use food components in catabolic and anabolic pathways? Involves specific chemical reactions: - Each reaction is catalyzed by a specific enzyme. - Other compounds, besides those being directly metabolized, are required as intermediates or catalysts in metabolic reactions - adenosine triphosphate (ATP) - nicotinamide adenine dinucleotide (NAD+) - flavin adenine dinucleotide (FAD+) - Coenzyme A ATP ATP is the energy currency of the cell The structure of ATP is similar to that of nucleic acids The energy in ATP is “carried” in the phosphate groups - to convert ADP into ATP requires energy - the energy is stored as potential energy in the phosphate group bond - removal of the third phosphate releases that energy NADH, FADH2 NAD+ can accept a hydrogen ion and become reduced to NADH: NAD+ + 2[H+] + 2e- NADH + H+ The added hydrogen ion (and electrons) can be carried to and used in other reactions in the body. FAD+ is similarly reduced to FADH2. NADH and FADH carry hydrogen ions and electrons to the enzymes in the electron transport chain of the mitochondria, allowing ATP production there. Coenzyme- A The enzyme coenzyme A converts acetyl groups (2-carbon structures) into acetyl CoA, which can then be used in metabolic reactions During the course of acetyl CoA production, energy is released and is used to convert NAD+ to NADH Cellular Respiration Generating ATP from food requires glycolysis, the Krebs Cycle and electron transport chain. Overall reaction: C6H12O6 + 6 O2----> 6 CO2 + 6 H2O + 38 ATP + heat The Main point: the break down of glucose releases LOTS of energy: - about 40% in usable form (ATP) - about 60% as heat Glycolysis Glycolysis is the breakdown of glucose into pyruvic acid Two main steps are involved, occurring in the cytoplasm of cells (no organelles involved). The two main steps of glycolysis Step one: glucose glucose 6-phosphate ATP ATP fructose 1,6diphosphate Step two: fructose 1,6diphosphate 2 pyruvic acid 2 NADH 2 ATP 2 ATP What happens to pyruvic acid? In aerobic respiration (oxygen present): - pyruvic acid moves from cytoplasm to mitochondria - pyruvic acid (3 carbons) is converted to acetyl group (2 carbons), producing CO2 in the process - acetyl group is converted to acetyl CoA by coenzyme A - acetyl CoA is used in the Krebs cycle. Kreb’s Cycle / TCA cycle / Citric acid cycle Acetyl CoA combines with oxaloacetic acid, forming citric acid A series of reactions then occurs resulting in: - one ATP produced - three NADH and one FADH2 produced (go to electron transport chain) - two CO2 molecules produced Electron-transport Chain The main point: NADH and FADH2 carry H+ ions to the electrontransport chain, resulting in production of ATP To do this, the H+ ions are moved along the transport chain, eventually accumulating in the outer mitochondrial compartment The H+ ions move back into the inner mitochondrial compartment via hydrogen channels, which are coupled to ATP production. At the end of the transport chain, four hydrogen ions join with two oxygen molecules to form water: 4 H+ + O2 ----> 2 H2O In the absence of oxygen, the transport chain stalls (no ATP production) Net Result of Glycolysis, Citric Acid Cycle, and Electron Transport Chain: Production of ATP (stored, potential energy for chemical reactions in the body; 40% of energy released). Production of heat (maintains body temperature; 60% of energy released). Also, production of CO2 and H2O. Storage and Utilization of Glycogen Excess glucose can be stored as glycogen. glucose glucose 6-phosphate glucose 1-phosphate glycogen Stored glycogen can be utilized, by glycogenolysis. Glycogenolysis: -glycogen is broken down into glucose 6phosphate - liver transforms glucose 6-phosphate glucose, maintaining blood glucose levels to Diabetes mellitus is a metabolic condition characterized by an inability to regulate blood glucose levels. It is caused by either defects in insulin production and secretion (Type I) or defects in insulin signaling (Type II) Type I Diabetes or insulin-dependent or juvenile diabetes It is usually due to autoimmune attack of β-islet cells in the pancreas. It can also be idiopathic and there is increasing evidence of a viral etiology. The normal function of β-islet cells is to produce insulin in response to elevated blood glucose, which in turn promotes the conversion of glucose into glycogen for storage. Destruction of βislet cells prevents insulin production and subsequently manifests as hyperglycemia. Genetic susceptibility genes for type I diabetes have been identified and include IDDM1, which codes for a MCH II complex that is displayed on the surface of β-islet cells. Certain polymorphisms of this gene result in the display of improper antigens on the surface of β-cells, leading to their targeting for destruction by T-cells. Type II Diabetes or non-insulin-dependent or obesity-related diabetes It is characterized by insulin resistance and a loss of insulin sensitivity. Insulin levels may be increased (hyperinsulinemia) or decreased (hypoinsulinemia). Other factors that contribute include decreased activity of glucose transporters, increased hepatic glucose production and delayed β-cell sensitivity to hyperglycemia. The etiology of type II diabetes is unknown, but it is associated with obesity (particularly central obesity), sedentary lifestyle, high sugar diet, total body irradiation (a cancer treatment), hypertension and increasing age. Pharmacological Interventions First line treatment for type I diabetes is insulin replacement therapy. Type II diabetes is initially treated by attempts to maintain glycemic control with diet modifications. Pharmacological interventions, such as metformin, are used later. Diabetic complications are prevalent and uncontrolled, so there is intense interest in developing pharmacological agents that allow better management of this condition. Novel antidiabetic treatments include fibroblast growth factor-21 analogs, renal sodium-glucose transporter inhibitors, free fatty acid receptor ligands, dipeptidyl peptidase IV (DPPIV) inhibitors and more Blood glucose are : carbohydrate metabolism exist 1. Glycolysis 2. Glycogenesis 3. HMP Shunt 4. Oxidation of Pyruvate 5. Kreb’s Cycle / TCA cycle / Citric acid cycle 6. Change to lipids Fasting blood glucose carbohydrate metabolism : 1. Glycogenolysis 2. Gluconeogenesis GLYCOLYSIS (Total ATP formed is 7) Glycolysis oxidation of glucose energy It can function either aerobically or anaerobically pyruvate Occurs in the cytosol of all cell AEROBICALLY GLYCOLYSIS : Pyruvate Mitochondria CoA Kreb’s Cycle lactate oxidized to Acetyl CO2 + H2O + ATP Glycolysis CH2O C 6 CH2OH 5 H H H Dihydroxyacetone phosphate 1 H OH 3 OH 2 NAD+ + 2 P 6 2 NADH + 2H+ CH2O P HCOH ADP C O P O OH2C O H H H OH 2 Glucose 6-phosphate HCOH 3-Phosphoglyceric acid (2 molecules) COOH 2 ATP P CH2O OH OH 1, 3-Bisphosphoglyceric acid (2 molecules) 2 ADP 7 H OH P Glyceraldehyde 3-phosphate 5 Glucose (1 molecule) 1 HO CH2O OH ATP H HCOH 2 H P O CH2OH O 4 HO H C O P 8 P OH2C 6 O 1 5 H CH2OH CH2OH HCO 2 H HO 4 Phosphofructokinase H 3 Fructose 6-phosphate ATP OH2C H H 4 O P COOH CH2O HO OH CH2 Phosphoenolpyruvic acid (2 molecules) 2 ADP O H 9 C ADP P 2-Phosphoglyceric acid (2 molecules) COOH OH 3 OH P P OH Fructose 1, 6-bisphosphate 10 2 ATP CH3 C O COOH Pyruvic acid (2 molecules) OXIDATION OF PYRUVATE Occur in mitochondria Oxidation of 1 mol Pyruvate + 3 mol ATP 1 mol Acetyl-CoA CH3COCOOH + HSCoA + NAD+ CH3CO-SCoA + NADH (Acetyl-CoA) (Pyruvate) Catalyzed by Pyruvate dehydrogenase enzyme This enzyme need CoA as coenzyme In Thiamin deficiency, oxidation of pyruvate is impaired lactic and pyruvic acid GLYCOGENESIS Synthesis of Glycogen from glucose Occurs mainly in muscle and liver cell The reaction : Glucose Glucose-6-P Hexokinase / Glucokinase Glucose-6-P Glucose-1-P Phosphoglucomutase Glucose-1-P + UTP UDPG + Pyrophosphate UDPG Pyrophosphorylase GLYCOGENESIS Glycogen synthase catalyzes the formation of α- 1,4-glucosidic linkage in glycogen Branching enzyme catalyzes the formation of α1,6-glucosidic linkage in glycogen Finally the branches grow by further additions of 1 → 4-glucosyl units and further branching (like tree!) GLYCOGENOLYSIS The breakdown of glycogen Glycogen phosphorylase catalyzes cleavage of the 1→4 linkages of glycogen to yield glucose-1phosphate α(1→4)→α(1→4) glucan transferase transfer a trisaccharides unit from one branch to the other Debranching enzyme hydrolysis of the 1→6 linkages The combined action of these enzyme leads to the complete breakdown of glycogen. GLYCOGENOLYSIS Phosphoglucomutase Glucose-1-P Glucose-6-P Glucose-6-phosphatase Glucose-6-P Glucose Glucose-6-phosphatase enzyme a specific enzyme in liver and kidney, but not in muscle Glycogenolysis in liver yielding glucose export to blood to increase the blood glucose concentration In muscle glucose-6-P glycolysis Glycogenesis and Glycogenolysis GLUCONEOGENESIS Pathways that responsible for converting noncarbohydrate precursors to glucose or glycogen In mammals occurs in liver and kidney Major substrate : 1. Lactic acid from muscle, erythrocyte 2. Glycerol from TG hydrolysis 3.Glucogenic amino acid Gluconeogenesis meets the needs of the body for glucose when carbohydrate is not available from the diet or from glycogenolysis A supply of glucose is necessary especially for nervous system and erythrocytes. The enzymes : 1. Pyruvate carboxylase 2. Phosphoenolpyruvate karboxikinase 3. Fructose 1,6-biphosphatase 4. Glucose-6-phosphatase HMP SHUNT/HEXOSE MONO PHOSPHATE SHUNT / PENTOSE PHOSPHATE PATHWAY / Phosphogluconate pathway An alternative route for the metabolism of glucose / glycolysis It does not generate ATP but has two major function : 1. The formation of NADPH synthesis of fatty acid and steroids (Oxidative non-reversible phase) 2. The synthesis of ribose / erythrose nucleotide and nucleic acid formation as well as aromatic aminoacid synthesis (Non-Oxidative reversible phase) • It’s primary role is anabolic rather than catabolic • It takes place in the cytosol HMP SHUNT Active in : liver, adipose tissue, adrenal cortex, thyroid, erythrocytes, testis and lactating mammary gland Its activity is low in muscle In erythrocytes : HMP Shunt provides NADPH for the reduction of oxidized glutathione by glutathione reductase reduced glutathione removes H2O2 glutathione peroxidase HMP SHUNT Glutathione reductase G-S-S-G 2-G-SH (oxidized glutathione) (reduced glutathione) Glutathione peroxidase 2-G-SH + H2O2 G-S-S-G + 2H2O This reaction is important accumulation of H2O2 may decrease the life span of the erythrocyte damage to the membrane cell hemolysis HMP SHUNT Regulation of HMP shunt pathway Glucose 6-phosphate DH is the regulatory enzyme. NADPH is a potent competitive inhibitor of the enzyme. Usually the ratio NADPH/NADP+ is high so the enzyme is inhibited. But, with increased demand for NADPH, the ratio decreases and enzyme activity is stimulated. The reactions of the non-oxidative portion of the pentose pathway are readily reversible. The concentrations of the products and reactants can shift depending on the metabolic needs of a particular cell or tissue. Increase in ATP: a putative inhibitor of these steps BLOOD GLUCOSE Blood glucose is derived from the : 1. Diet the digestible dietary carbohydrate yield glucose blood 2. Gluconeogenesis 3. Glycogenolysis in liver Insulin play a central role in regulating blood glucose blood glucose Glucagon blood glucose Growth hormone inhibit insulin activity Epinephrine stress blood glucose The Krebs cycle (Total ATP formed is 34) Also known as citric acid cycle TCA cycle Occurs in matrix of mitochondria Series of redox reactions 2 decarboxylation reactions release CO2 Reduced coenzymes (NADH and FADH2) are the most important outcome One molecule of ATP generated by substrate-level phosphorylation Final pathway for the oxidation of carbohydrtaes. The Krebs Cycle CO2 CH3 CoA C O COOH C O CH3 NADH + H+ + Pyruvic NAD acid Acetyl coenzyme A To electron transport chain Oxaloacetic acid NADH + H+ CH2 COOH NAD+ COOH HCOH To electron transport chain H2C COOH HOC COOH 1 H2O H2C COOH Citric acid 8 CH2 COOH Malic acid H2O Fumaric acid CoA COOH C O 2 7 H2C COOH COOH CH HC HC COOH COOH FADH2 HOC COOH KREBS CYCLE H Isocitric acid 3 6 FAD NAD+ H2C COOH CO2 H2C COOH CoA Succinic acid GTP H2C COOH GDP ADP NADH + H+ 5 CO2 CH2 O C S CoA ATP Succinyl CoA H2C COOH HCH 4 O C COOH Alpha-ketoglutaric acid NAD+ NADH + H+ To electron transport chain Enzymes and Energetics in TCA Cycle 1. Citrate synthase 2. Aconitase 3. Isocitrate dehydrogenase 4. α-Ketoglutarate dehydrogenase 5. Succinate thiokinase 6. Succinate dehydrogenase 7. Fumarase 8. Malate dehydrogenase In TCA cycle, 4 mol. of NADH (approx. equal to 2.5 ATP) and 1 mol. of FADH2 (approx. equal to 1.5 ATP) are produced / each mol. of acetylCoA catabolized in one turn of the cycle. In addition, 2 ATP is formed by substrate level phosphorylation catalyzed by succinate thiokinase. Glyoxylate Pathway The glyoxylate cycle, a variation of the TCA cycle, is an anabolic pathway occurring in plants, bacteria and fungi. In microorganisms, the glyoxylate cycle allows cells to utilize simple carbon compounds as a carbon source when complex sources such as glucose are not available. The glyoxylate cycle utilizes three of the five enzymes associated with the TCA cycle and shares many of its intermediate steps. The two cycles vary when, in the glyoxylate cycle, IsoCitrateLyase enzyme converts isocitrate into glyoxylate and succinate instead of α-ketoglutarate as seen in the TCA cycle. The glyoxylate cycle then continues on, using glyoxylate and acetylCoA to produce malate. Glyoxylate Pathway Electron transport chain Electron transport chain 4. Series of electron carriers in inner mitochondrial membrane reduced and oxidized As electrons pass through chain, exergonic reactions release energy used to form ATP Chemiosmosis Final electron acceptor is oxygen to form water Chemiosmosis Carriers act as proton pumps to expel H+ from mitochondrial matrix Creates H+ electrochemical gradient – concentration gradient and electrical gradient Gradient has potential energy – proton motive force As H+ flows back into matrix through membrane, generates ATP using ATP synthase Summary of cellular respiration Uronic acid Pathway of Glucose Importance in humans: Provides UDP-glucuronic acid for conjugation [conjugation of bilirubin, steroids etc] and synthesis of glycosaminoglycans. In lower animals (not in primates- deficiency of enzyme L- gulonolactone oxidase), this pathway leads to synthesis of Vit C. Essential Pentosuria: one of Garrod’s tetrad [alkaptonuria, albinism, pentosuria, cystinuria- inborn error of metabolism]: *1 in 2500 births due to deficiency of xylitol dehydrogenase → L-xylulose excreted in urine gives + benedict’s test-not harmful. *Diffentiated from DM by + Bials test [orcinol in HCL-Bial’s reagent] by pentose sugars. URONIC ACID PATHWAY G-6-P Phosphoglucomutase G-1-P + UTP [UDPG Phosphorylase] UDP- Glucose enters Uronic acid pathway Aldose reductase- Glucose to Sorbitol [glucitol]: Lens, retina, Schwann cell of peripheral nerves, kidney, placenta, RBC, cells of ovaries and seminal vesicles. Sorbitol dehydrogenase- Sorbitol to Fructose Glucoe to Sorbitol to Fructose: in seminal vesicles for sperm cell [fructose is preferred carbohydrate energy source] Hyperglycemia: Uncontrolled DM-large amt Glucose enters Lens, Retina,Nerve, Kidney – with action of aldose reductase →↑Sorbitol, cannot pass through cell memb, so trapped inside cell. Sorbitol dehydrogenase is absent in Lens, retina, kidney and nerve cell →↑sorbitol accumulates →Osmotic effects →cell swelling and water retention: cause of cataract formation, peripheral neuropathy, vascular problems leading to nephropathy and retinopathy