* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Just the Facts... - Excellus BlueCross BlueShield
Survey
Document related concepts
Transcript
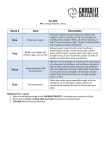
Just the Facts... A nonprofit independent licensee of the BlueCross BlueShield Association Excellus BlueCross BlueShield, Utica Region Volume 10.12 The newsletter for Medical Office and Facility Staff Inside this Issue Clarification: Radiology Codes that Require Prior Authorization, p. 2 Decreasing your Wait Time When Calling Provider Service, p. 2 Recent Product Updates, p. 3 After-hours Requirements, p.4 2005 Benefit Updates for Medicare Blue PPO, p. 4 Updated Clinical Guidelines are on our Web site, p. 5 December 2004 Reminder-Medical Management Changes Effective January 1, 2005 We would like to remind you that, effective January 1, 2005, the medical management guidelines for HMO, point-of-service and governmentsponsored safety net products will be changing. Please be sure to review the new medical management guidelines, which were included in the November edition of Just the Facts, as well as in a recent provider bulletin. If you have any questions about these requirements, please contact your local Provider Service department. FLRx-Changes and Updates for 2005 QM Purpose, p. 5 Coding Corner-Correct use of BH CPT Codes 90801 and 90808, p. 5 Helping Patients with Chronic Conditions through HM Programs, p. 6 We have included a new FLRx Prescribing Tip Sheet, which describes upcoming changes in the 2005 medication guide, as well as a complete copy of the 2005 3-Tier Medication Guide of Commonly Prescribed Drugs in this newsletter. For additional information, please visit us on the Web at www.excellusbcbs.com or contact your Provider Relations Representative. Reminder-FHP and MMC Approvals, p. 7 Reminder-CAQH-Credentialed Providers Need to Supply Contract/Payment Info, p. 7 Reminder-Correct Suffix for BluePreferred and BluePoint Members, p. 7 Medical Policy/Protocol Update, p. 8 Provider Call Flow Chart FLRx Tip Sheet (Nov. 2004) 2005 3-Tier Medication Guide www.excellusbcbs.com Save the Date: Eating Disorders Conference in February As a reminder, Excellus BlueCross BlueShield, in conjunction with our Caring for Communities program, is sponsoring the first annual New York State Eating Disorders Initiative Conference. The conference is being held at the OnCenter Complex in Syracuse on February 24 and 25, 2005. The conference represents a partnership with many organizations and individuals, among them Clear Channel Communications, New York State Sen. John DeFrancisco and Ophelia’s Place, a nonprofit organization in Liverpool that provides support to individuals with eating disorders, their friends and their families. Please join us for workshops and training sessions, including discussions held by eating disorder experts. If you would like more information about the eating disorders conference, please go to www.opheliasplace.org. Clarification: Radiology Codes that Require Prior Authorization Last April, we revised our prior authorization requirements regarding which radiology CPT procedure codes require prior authorization. We sent a provider bulletin to physicians, imaging facilities and chiropractors that included a list of codes. (See Provider Bulletin No. 2004-06.) Our recent provider bulletin (#2004-17) regarding changes to our managed care medical management guidelines effective January 1, 2005, did not include specific codes or anatomical body areas for CT, MRA, MRI or PET scans. We have not, however, changed the CT, MRA, MRI or PET scan codes that require prior authorization. Please continue to use the same list provided with the April communication. Choosing the Right Option When Calling Provider Service can Decrease your Wait Time Our Provider Service Department has been experiencing an increase in the number of callers choosing option 1 once they’ve entered the claim information queue. Choosing option 1 transfers callers to the PPO claim unit. As you are probably aware, the PPO claim queue is not automated, so callers are sent directly to a provider service representative. The problem is that many callers are choosing option 1 regardless of whether or not they have a PPO claim issue, hoping that the representative can either help them or transfer them to the appropriate area. This is causing tremendous delays within Provider Service. At this time, our representatives are trained to handle certain types of inquiries. For example, the representatives who are able to help you with PPO questions are not the same representatives who can help you with indemnity questions. Therefore, when a caller chooses the PPO option when the issue is not with a PPO claim, the representative can only transfer him/her to the appropriate service area. When this happens, the call is placed at the end of the queue. This actually increases the caller’s wait time. In order to decrease wait time, please be sure the telephone prompt you choose corresponds to the product within which the member is enrolled. Once you choose option 1 to enter the claim information queue, you will have two options, 1) PPO claims, and 2) all other claims. Your prefix list can help you decide which option to choose. For example, you would choose option 1 for PPO claims if the prefix is ZFA or ZFG. You can find an updated prefix list, which includes the prefix and product type, in the October 2004 edition of Just the Facts. Additionally, please note that calls for Medicare Blue PPO (ZFM) should be directed to the managed care queue rather than the PPO queue. To help you better understand the options when calling Provider Service, we’ve included an updated Provider Call Flow Chart in this newsletter. Page 2 December 2004 Recent Product Updates Medicare Blue PPO We now have approval to market Medicare Blue PPO in the following counties: Broome, Cayuga, Chemung, Chenango, Clinton, Delaware, Essex, Franklin, Fulton, Hamilton, Herkimer, Jefferson, Lewis, Madison, Montgomery, Oneida, Onondaga, Oswego, Otsego, Schuyler, St. Lawrence, Steuben and Tioga. We anticipate approval in other counties in 2005. It’s important to remember that Medicare Blue PPO participating providers may provide services to any Medicare Blue PPO member even if you are not located in one of the approved counties. The member ID card has the words “Medicare Blue PPO” on it. The prefix is ZFM. You should collect copays at the time of service and submit claims directly to Excellus BCBS. You do not need to bill Medicare first. Primary payment is made by Excellus BCBS. For additional information, please refer to the September edition of Just the Facts, or call your local Provider Service. FourFront As you may recall, we recently introduced a new product called “FourFront.” FourFront is an innovative, consumer-driven health care plan that encourages members to take good care of themselves while making wise, cost-conscious decisions. Because FourFront is based on our EPO product, members have access to our BluePPO network, including BlueCard. The name FourFront hints at the unique benefit design, which follows the “rule of four” for the first four diagnostic office visits and first $400 of diagnostic lab and X-ray. Diagnostic Office Visits • The first four diagnostic office visits are covered at a low office copay. • Preventive care is covered in full or with a low office copay; it is not included in the first four visits, and is never subject to deductible or coinsurance. • The fifth and subsequent diagnostic office visit is subject to coinsurance and deductible. Diagnostic Lab and X-ray • The first $400 of diagnostic lab and X-ray services are covered in full. • After the allowance is used, coinsurance and deductible applies. Providers should always collect at least the office copay at the time of service (the remittance will indicate if the visit is subject to deductible or coinsurance). Providers can identify members by their ID card, which has the name “FourFront” on it. The prefix is ZFF. For additional information, please refer to the August edition of Just the Facts, Provider Bulletin No. 2004-12, or call your local Provider Service. BluePPO HSA Effective January 1, 2005, Excellus BCBS will be introducing a new version of our BluePPO product. BluePPO HSA is a high-deductible health plan that can be combined with a health savings account (HSA). Members will utilize the BluePPO network, including BlueCard. Additionally, both the prefix (ZFA) and the prior authorization requirements will be the same as BluePPO; however, the ID card will say “HSA." Please note that the HSA indicator on the ID card tells you that the member is in a high deductible PPO plan. The member may or may not have an actual HSA account. For additional information, please refer to the October edition of Just the Facts, or call your local Provider Service. December 2004 Page 3 After-hours Coverage Requirements In order to provide members with access to care 24 hours a day, seven days a week, Excellus BlueCross BlueShield has made a determination of what constitutes acceptable versus unacceptable methods of after-hours coverage for managed care PCPs and specialists. (For behavioral health providers, acceptable methods differ from those for other providers. A listing of acceptable behavioral health after-hours methods of contact can be found in the November edition of Just the Facts.) Members must be able to: • • Reach the practitioner or a person with the ability to patch the call through to the practitioner (i.e., answering service); or Reach an answering machine with instructions on how to contact the practitioner or his/her backup (i.e., message with number for home, cell phone or beeper). Unacceptable means of after-hours coverage include the following: • An answering machine with instructions on how to contact the practitioner, but no live voice at the contact phone number; • An answering machine with instructions to go to or to call the emergency room; • An answering machine that recommends calling during business hours; • An answering machine with no instructions; • No answer; • A busy signal three times within 30 minutes. PCPs and physician specialists, please be sure that you are compliant with one of the acceptable methods of after-hours contact. 2005 Benefit Updates Planned for Medicare Blue PPO Pending approval from CMS, we are planning some enhancements to our Medicare Blue PPO product options during 2005. These are based on feedback from informational meetings we’ve hosted for the Medicare-eligible population, as well as from current members. Among the changes we plan to make are: • An unlimited $10 generic drug benefit with discounts on brand drugs for Plan Two • Fixed copays rather than coinsurance for Plan Two • Lower copays for Plan Three • A flexible fitness benefit where members will be reimbursed up to $40 per month (depending on the plan) for a variety of fitness and/or qualified weight management programs • Round-the-clock access to a “personal health coach” – a registered nurse, respiratory therapist or dietician who can answer members questions about medications they are taking, health food choices and other health-related topics. Look for further information in future issues of this newsletter. Page 4 December 2004 Updated Clinical Guidelines are Available on our Web site We’ve recently updated the following clinical guidelines: • Prenatal Care • Anticoagulation Principles • Asthma They are available on our Web site at www.excellusbcbs.com, along with many other clinical practice guidelines and materials. Click on For Providers, then on Patient Care. Select Clinical Practice Guidelines from the menu on the left. Scroll down to the guideline you need. To have a paper copy of guidelines or other materials mailed to you, please contact our Quality Management Department at (315) 671-7140. QM Purpose to Improve Quality of Life The purpose of our Quality Management Program is to support our mission by contributing to, and being recognized for, improving the quality of life in the communities we serve. The program works in partnership with our members, our participating physicians and other health care practitioners, as well as with community agencies, to improve quality of care and services delivered to our members. Evaluation of our success is the ability to measurably improve the health and satisfaction of the population we serve. If you would like a copy of our QM Program Description or most recent program evaluation, please contact the Quality Management Department at (315) 671-7140. CODING CORNER Correct use of Behavioral Health CPT Codes 90801 and 90808 Our Behavioral Health Department has noticed that some behavioral health practitioners occasionally bill 90801, psychiatric diagnostic interview examination, more than once for an initial assessment of the same patient. While components of a diagnostic interview may be part of all therapy sessions, practitioners should use procedure code 90801 for only the initial diagnostic examination. The same provider can rebill 90801 for the same patient only after a 12-month break in treatment. The exception to this is for child psychiatrists who see children and adolescents. We recognize that the initial assessment of these patients is more time-consuming. Therefore, child psychiatrists may use 90801 for a maximum of two sessions, where necessary, for initial assessment of a child or adolescent. CPT procedure code 90808 is for an extended face-to-face contact (75-80 minutes). This amount of time is not necessary for routine care and should only be used in unusual circumstances. The clinical record should reflect the exceptional nature of this extended visit, with specific clinical justification. Excellus BCBS behavioral health staff members review these CPT codes for utilization and make appropriate adjustments when needed. December 2004 Page 5 Helping Patients with Chronic Conditions through Health Management Programs Excellus BlueCross BlueShield is committed to helping patients with chronic conditions through our health management (HM) programs. We have developed HM programs for the following chronic diseases: asthma, coronary artery disease, diabetes, and depression. We have designed our integrated, population-based health management programs to help members with the above chronic conditions become more proactive when managing their conditions. The programs use a systematic approach to improving the health care of people with these chronic diseases. We have established evidence-based guidelines for each of these chronic diseases in order to provide information and direction for managing the disease. The goal of each disease-specific program is to enhance the primary care physician’s ability to provide excellent care to his/her patients with the disease. Member Education One of the prime components of each health management program is member education. Members benefit from educational programs such as mailed and telephoned reminders specific to their chronic disease. Information regarding standards of care is routinely distributed through these targeted reminders and also through other educational tools and newsletters. Periodic reminders to obtain screening services recommended for optimal health management, per evidence-based clinical guidelines, are also sent to members. Practitioner Support Support for practitioners is available through various tools designed to assist practitioners with their patient communications and management. Information explaining the function and purpose of the support tools, how to contact the Plan for patient referrals into the program as well as answers to other questions, is included in materials distributed to practitioners. Physician CME programs may also be provided at various times throughout the year. Evidence-based clinical guidelines that provide standards of care from which the programs are based can also be accessed through the Web site (www.excellusbcbs.com). Most of the clinical guidelines also include useful tools and patient education sheets. The patient sheets are also available in Spanish. Physicians are encouraged to browse the Web site as a source of clinical care and health management program information. Please call us Health management programs are free to members and participating health care practitioners. Please contact us at 1 (877) 586-1990 with any questions, concerns, or patient referrals. Our goal is to provide health care practitioners and their patients with a quality and comprehensive approach to managing chronic disease. Page 6 December 2004 Reminder: Family Health Plus and Medicaid Managed Care Approvals We have been introducing Family Health Plus (FHP) and HMOBlue Option (Medicaid managed care) on a county-by-county basis since 2000. We currently have membership in the following counties: Oneida, Onondaga, Oswego and Herkimer. Additionally, we have FHP members in Clinton, Essex and Franklin counties. Pending approval, we will continue to introduce Family Health Plus and HMOBlue Option on a county-by-county basis throughout 2005. Please remember that, with our seamless network, you may see FHP and HMOBlue Option members from the active counties regardless of whether or not your specific county is enrolling members. Reminder: CAQH-Credentialed Providers Still Need to Supply Contract/Payment Info If you are a participating provider using the Council for Affordable Quality Healthcare’s (CAQH) universal credentialing data source, please remember that you still need to inform Excellus BlueCross BlueShield directly, in writing, of any changes in your practice such as address, telephone number, or tax ID. We need this information for directories and/or claims processing systems (separate from CAQH, which is strictly for credentialing and recredentialing). As a convenience, you may use the Provider Information Update form, available on our Web site. You may also contact your Provider Relations Representative for a copy. Addresses and fax numbers for returning the completed form are listed at the end of the form. Reminder: Please use Correct Suffix for BluePreferred and BluePoint (POS) Members Since discontinuing the old claim system for local PPO and POS products in Central New York (CNY) and CNY Southern Tier, we have found that some providers are still submitting with the old member ID suffix. We have noticed this specifically with claims for members with prefixes SYU or ONC. Providers in the Utica region may also see members with the prefixes SYU or ONC. We would like to remind you that the suffix for BluePreferred and BluePoint (POS) subscribers is “00." Suffixes for dependents would be "01, 02, etc." Please ask your patients for their ID card and use the appropriate suffix. As always, it is extremely important to check the member’s ID card, as it contains vital information that can help to process claims more efficiently. December 2004 Page 7 Important Addition to Medical Policy Update Section Beginning with this issue of Just the Facts, we are including a brief description of Medicare coverage when significant differences exist for high volume/high profile Health Plan medical policies and medical policies maintained by the Centers for Medicare & Medicaid Services (CMS) for determining coverage under Medicare. Please note that the absence of a comparison with CMS coverage determinations does not necessarily constitute an agreement in coverage between CMS and the Health Plan. Medical Policy/Protocol Update To ensure that the development of corporate medical policies occurs through an open, collaborative process, we encourage our participating practitioners to become actively involved in medical policy development. Each month, draft policies are posted in the Provider section of our Web site (www.excellusbcbs.com) for participating practitioners’ review and comment. Click on For Providers, then select the Patient Care button along the top, and then View Our Medical Policies. At the bottom of the menu on the left side is a short list under Medical Policies. Click on Preview & Comment on Draft Policies. The following policies are tentatively scheduled to be available for comment in December 2004: • • • • • • • Allergy Immunotherapy Biochemical Markers for Bone Turnover Cardiac Bioimpedance H Pylori Testing HPV Testing Preconception and Prenatal Genetic Testing/Counseling and Preimplantation Genetic Diagnosis Wireless Endoscopy Corporate medical policies are used as a guide. Coverage decisions are made on a case-by-case basis and in accordance with the member's contract. While a technology or service may be medically necessary, payment of benefits is subject to the member's eligibility on the date the service is rendered and the benefit/exclusion provisions of the member's contract. Before rendering care, providers should verify the member's eligibility and coverage by calling the Provider Service Department of your local plan. The following new and updated medical policies have been reviewed and approved by the Corporate Medical Policy Committee, including practitioner representatives from Excellus BlueCross BlueShield, Central New York Region, Central New York Southern Tier Region, Utica Region, and Rochester Region. Complete detailed policies are available on our Web site at www.excellusbcbs.com. Click on the Patient Care menu option, then on View Our Medical Policies. Questions regarding medical policies may be directed to your Provider Relations representative or to the Provider Service Department of your local health plan. Medical policies are also located on the Web site for Excellus BlueCross BlueShield members at www.excellusbcbs.com. To access our policies, members need to click on For Members, followed by Health and Wellness, then Research Health Conditions and lastly View our Medical Policies. Policies and protocols referenced in this newsletter are written for commercial contracts only. A brief description of CMS coverage has been provided for particular Excellus BlueCross BlueShield medical policies that differ from CMS. Please refer to CMS for medical policies pertaining to Senior contracts. Web sites for review of CMS policies are: • • www.cms.hhs.gov/mcd/indexes.asp for the Medicare Manual http://www.umd.nycpic.com/lmrp.html for local Upstate New York Medicare policies. Please note: Although medical policies are effective on the date they are approved by the Medical Policy Committee, updates to the claims processing systems may not occur for up to 90 days in order to allow you to update your billing systems accordingly. NEW POLICIES recently approved by Corporate Medical Policy Committee There were no new policies this reporting period. CURRENT POLICIES recently updated by Corporate Medical Policy Committee Excimer Laser for the Treatment of Psoriasis treats only specific areas of the body with a concentrated narrow beam of ultraviolet light. Excimer laser for psoriasis has not been proven to be effective in improving clinical outcomes and is considered investigational. There have been no studies to provide comparative outcomes or assessment of long-term outcomes of this treatment. Positron Emission Tomography (PET) for Non-Oncologic Conditions (considered a high profile policy; we are highlighting where the Excellus BlueCross BlueShield policy differs from CMS) is an imaging technology that can reveal both anatomical and metabolic information in various tissue sites. PET is considered medically appropriate as a diagnostic tool for several conditions/disorders, as outlined in the policy. Research on the current update focused on its use in Alzheimer’s disease/dementia. Based upon our review and analysis, the use of a PET scan has not been proven effective in improving patient outcomes (even in subsets) and is considered investigational as a diagnostic tool for Alzheimer’s disease. CMS recently published a Decision Memorandum regarding FDG-PET in the diagnosis and treatment of mild cognitive impairment (MCI) and early dementia in elderly patients, which states the following: evidence is adequate to conclude that a FDG-PET scan is reasonable and necessary in patients with documented cognitive decline of at least six months and a recently-established diagnosis of dementia who meet diagnostic criteria for both Alzheimer’s disease (AD) and fronto-temporal dementia (FDD), who have been evaluated for specific alternate neurodegenerative diseases or causative factors, and for whom the cause of the clinical symptoms remains uncertain. CMS has also determined that the evidence is not adequate to conclude that FDG-PET is reasonable and necessary for the diagnosis of patients with mild cognitive impairment (MCI) or early dementia in clinical circumstances other than that specified above, absent safeguards that would be present in formal, protocol-driven clinical investigations. CMS would cover PET for these patients in a setting of a clinical trial that met specific criteria set by CMS. Pulmonary Rehabilitation (considered a high profile policy; we are highlighting where the Excellus BlueCross BlueShield policy differs from CMS) is an individualized, multidisciplinary therapeutic program to improve the quality of life and functional capacity of patients with chronic lung disease. Pulmonary rehabilitation is medically appropriate for COPD patients with the following characteristics: • • • • undergoing lung transplantation or lung volume reduction surgery; or have moderate COPD and multiple exacerbations; or have severe COPD; and do not have a short life expectancy or a condition that would prohibit safe participation in the program; have the mental stability, motivation and physical mobility to attend sessions and complete the program; and require a medically-comprehensive, supervised pulmonary exercise program. The local CMS policy addressing Pulmonary Rehabilitation states that, while there is no benefit category for payments to be made for these services, Medicare does recognize that there are components of the programs that are reimbursable when medically necessary. Signal-averaged Electrocardiogram (SAECG) and T-Wave Alternans (TWA) have been evaluated as technologies that stratify patient risk for fatal ventricular arrhythmias. SAECG is a modification of a conventional ECG recording in which the signals are first amplified, then filtered, and finally averaged with the assistance of computer software. TWA is a beat to beat measurement of the magnitude and morphology of the ECG measurement of repolarization in the ST segment and T-wave. Based upon our criteria and assessment of peer-reviewed literature, neither signal-averaged electrocardiography nor T-Wave Alternans improve patient outcomes and, therefore, are considered not medically necessary for risk stratification regarding ventricular arrhythmia in patients following acute myocardial infarction. The evidence demonstrates that SAECG and TWA have little clinical value in selecting patients who are at high risk for an arrhythmic event. Evidence is also lacking to demonstrate that the information could be used to alter treatment strategy and improve health outcomes. CURRENT POLICIES recently updated with minimal changes The following policies only required minimal changes (e.g., updating of references, changing language to meet legal needs). The coverage intent of the policies was not altered. These policies were recently approved for updating by the Health Plan Medical Directors and are available on our Web site: • • • • Intervertebral Disc Decompression techniques Photodynamic Therapy for Malignant Conditions Transendoscopic Therapies for Gastroesophageal Reflux Disease (GERD) Home Automatic External Defibrillators (AED) and Wearable Defibrillator (WCD) Vests NEW PROTOCOLS recently approved by Corporate Protocol Committee The Oximetry and Oximeters for Home Use protocol provides coverage criteria for the use of short-term, home-based oximetry (e.g., overnight oximetry) and for the use of home oximeters for long-term, continuous monitoring. CURRENT PROTOCOLS recently updated by Corporate Protocol Committee Enteral Nutrition formulas consist of nutritional liquids administered by mouth or enterally. This protocol provides coverage information for conditions as required by the New York Insurance Law mandate. External Insulin Pumps are utilized by diabetic patients for continuous insulin infusion. These pumps contain an insulin-filled syringe connected to a catheter that is inserted into a patient’s subcutaneous tissue. External insulin pumps are considered medically appropriate when specific criteria are met as outlined within the medical protocol. The criteria for coverage have been expanded with our recent review. Our medical protocol mirrors the regional CMS coverage criteria related to external insulin pumps. Hospital Beds provide the positioning required for a patient with certain medical condition(s). Hospital beds are considered durable medical equipment and are medically appropriate when: • • • The patient's condition requires positioning of the body (such as the head or foot of bed elevated to alleviate pain, promote good body alignment, prevent contractures, avoid respiratory infections) in ways not possible in an ordinary bed; or The patient's condition requires a bed height different than an ordinary bed to permit transfers from bed to chair or bed to standing; or The patient's condition requires special attachments that cannot be fixed and used on an ordinary bed. The Respiratory Therapy Devices protocol provides definitions and the medical appropriateness of various devices (e.g., nebulizers, peak flow meters) used in the treatment of respiratory conditions. 165 Court Street Rochester, NY 14647 A nonprofit independent licensee of the BlueCross BlueShield Association Prescribing Tip Sheet November 2004 Prescription Drug Medication Guide Changes for 2005 Excellus BlueCross BlueShield is committed to effectively managing prescription drug benefit costs and providing our members with affordable access to prescription drugs. One way we do this is by having our medication guides reflect the latest in clinical developments, effectiveness, quality and value. Our Pharmacy and Therapeutics Committee, which is made up of practicing community physicians and clinical pharmacists, regularly reviews the drugs on the 3-Tier list. Its most recent evaluation has resulted in changes of tier classifications for a small number of medications effective January 1, 2005. A summary of those changes is printed on the reverse. PRESCRIBING GUIDELINES ♦ For new prescriptions: please refer to reclassifications effective January 1, 2005 when considering prescription options. ♦ For patients with a 3-Tier benefit: Patients on medications that are being reclassified will continue to have coverage and will pay the applicable lower or higher copayment/ coinsurance amount based on reclassification effective January 1, 2005. If you decide to prescribe a Tier 3 medication the medication will be covered, but at the higher copayment/ coinsurance cost. ♦ For patients with a closed formulary benefit: Medications that are being reclassified as nonformulary generally will not be covered under the benefit. If you decide to prescribe a nonformulary medication, authorization will be required for coverage. ♦ This is not a benefit change or a mandate. Patients are not required to change medications. Patients whose medications are being reclassified from Tier 2 (lower copayment/ coinsurance) to Tier 3 (higher copayment/coinsurance) and from formulary (covered) to nonformulary (generally not covered) will be notified later this fall. Summary of Formulary Reclassifications Effective January 1, 2005 for Prescribers 3-Tier Medication Guide Reclassifications: Drugs Reclassified from Tier 3 to Tier 2 Reclassification Decreases member Co-Payment/Coinsurance Amount Therapeutic Class Asthma Cardiovascular/Heart: Diuretics Growth Hormone Intranasal Steroids/Antihistamines/Misc. Migraine Stomach: Inflammatory Bowel Drug Reclassified to Tier 2 Foradil Zaroxolyn Norditropin Astelin Amerge Dipentum Drugs Reclassified from Tier 2 to Tier 3 Reclassification Increases member Co-Payment/Coinsurance Amount Therapeutic Class Antipsychotics Men’s Health: Erectile Dysfunction Mental Health: Antidepressants Thyroid Women’s Health: Oral Contraceptives Drug Reclassified to Tier 3 NEW STARTS ONLY: AbilifyV, ZyprexaV Viagra Paxil 20mg, 30mg Synthroid Levlen, Levlite, Modicon, Ortho-Cept, OrthoCyclen, Ortho Micron, Ortho-Novum, Tri-Levlen, Triphasil Generic now available V Tier 2 for select prescribers/diagnoses Formulary Guide Reclassifications: Drugs Reclassified from Non-Formulary to Formulary Drugs classified as Formulary are generally covered under the benefit Therapeutic Class Drug Reclassified Allergy Astelin Asthma Foradil Cardiovascular/Heart: Diuretics Zaroxolyn Growth Hormone Norditropin Migraine Amerge Stomach: Inflammatory Bowel Dipentum Drugs Reclassified from Formulary to Non-Formulary Drugs classified as Non-Formulary are generally not covered under the benefit Therapeutic Class Mental Health: Antidepressants Thyroid Women’s Health: Oral Contraceptives Generic now available 9.1.04 Drug Reclassified Paxil 30mg, 40mg NEW STARTS ONLY: Synthroid Cylessa, Levlen, Levlite, Modicon, Ortho-Cept, Ortho-Cyclen, Ortho Micron, Ortho-Novum, Tri-Levlen, Trinorinyl, Triphasil 2005: 3-Tier Medication Guide of Commonly Prescribed Drugs The designation of drugs in the following categories is for reference only and is not a clinical comparison. Drug placement does not establish clinical comparability of products in individual situations. This list provides examples within categories and is not comprehensive. A nonprofit independent licensee of the BlueCross BlueShield Association DRUG CLASS Tier 1 Tier 2 Tier 3 ALLERGY Antihistamines (oral) Antihistamine/Decongestant Combinations Intranasal: Steroids/ Antihistamines/ Miscellaneous ALZHEIMER’S ARTHRITIS* ASTHMA Inhaled Beta Agonists/ Inhaled Respiratory Agents Inhaled Steroids Leukotriene Inhibitors Respiratory Drugs (oral) ATTENTION DEFICIT DISORDER BLOOD Anticoagulants Antiplatelet Anemia* CANCER CARDIOVASCULAR / HEART ACE Inhibitors (high blood pressure) Angiotensin II Receptor Blockers (high blood pressure) Antiarrhythmics (for normal heart rhythm) Antihyperlipidemics (high cholesterol) Antihypertensive Combinations (high blood pressure) Beta Blockers (high blood pressure) Calcium Channel Blockers Diuretics (highest member co-payment) Drugs listed CAPITALIZED IN BOLD/ITALICS are considered NON-FORMULARY under the closed formulary benefit (lowest member co-payment) clemastine, cyproheptadine, diphenhydramine, hydroxyzine R-Tanna No drugs listed at this time Allegra, CLARINEX, Zyrtec No drugs listed at this time ALLEGRA-D, OPTIMINE, RYNATAN SA, SEMPREX-D, TRINALIN, ZYRTEC-D flunisolide, ipratropium nasal spray Astelin, Beconase AQ, Flonase, Nasonex, Rhinocort AQ ATROVENT NASAL SPRAY, NASACORT, NASACORT AQ, NASAREL, NASALIDE, TRI-NASAL, VANCENASE, VANCENASE AQ, VANCENASE DS No drugs listed at this time Aricept COGNEX, EXELON, azathioprine, cyclophosphamide, gold, hydroxychloroquine, methotrexate, penicillamine, sulfasalazine No drugs listed at this time Arava, Enbrel§, Humira§, Kineret§, RHEUMATREX albuterol, cromolyn sodium, metaproterenol solution No drugs listed at this time Atrovent Inhaler, Combivent, Intal, Foradil, Pulmozyme, Serevent Azmacort, Beclovent, Flovent, Pulmicort Singulair (Tier 2 if asthmatic) No drugs listed at this time Advair, MAXAIR, MAXAIR AUTOHALER, PROVENTIL, PROVENTIL HFA, Spiriva, TILADE, TORNALATE, VENTOLIN, XOPENOX Advair, AEROBID, AEROBID M, QVAR, VANCERIL, VANCERIL DS No drugs listed at this time ADDERALL, Adderall XR, Concerta, DEXEDRINE, DEXEDRINE SPANSULES, DEXTROSTAT, FOCALIN, METADATE CD, RITALIN, RITALIN LA, Strattera heparin, warfarin dipyridamole No drugs listed at this time Coumadin Agrylin, Plavix Epogen§, Neupogen, Procrit§ ARIXTRA, FRAGMIN, INNOHEP, methotrexate, tamoxifen All brands are Tier 2 No drugs listed at this time benazepril, captopril, enalapril, fosinopril, lisinoprilp, moexepril Altace No drugs listed at this time Avapro\, Diovan §, ACEON§, CAPOTEN§, LOTENSIN§, MAVIK, §, PRINIVIL§, UNIVASC§, VASOTEC§, ZESTRIL§ ATACAND, BENICAR, COZAAR§, MICARDIS, TEVETEN amiodarone, digoxin, disopyramide, mexiletine, procainamide, quinidine, sotalol cholestyramine, clofibrate, (20mg only) gemfibrozil, lovastatinp Betapace AF, Lanoxin, Rythmol, Tonocard Betapace, CORDARONE, MEXITIL, NORPACE CR, PROCAN, Procanbid, PRONESTYL, QUINIDEX, QUINIGLUTE, TAMBOCOR, No drugs listed at this time albuterol, metaproterenol, theophylline dextroamphetamine, methylin, methylin ER, methylphenidate benazepril/HCTZ, bisoprolol/HCTZ, captopril/HCTZ, enalapril/HCTZ, fosinopril/HCTZ, lisinopril/HCTZ, quinapril/HCTZ (25mg only) acebutolol, atenololp , bisoprolol, labetolol, metoprolol, nadolol, propranolol, propranolol solution, pindolol, timolol diltiazem, diltiazem-XR, nicardipine, nifedipine, Taztia XT, verapamil, verapamil (SR) amiloride, furosemide, (25mg only) hydrochlorothiazidep , indapamide, spironolactone, triamterene/hydrochlorothiazide ACCOLATE Namenda, Reminyl § ALUPENT, BRETHINE, PROVENTIL SA, T-PHYL, THEO-DUR, UNIPHYL, VOLMAX AGGRENOX, Lovenox Pletal, TICLID, TRENTAL Aranesp§ ACCUPRIL MONOPRIL TIKOSYN §, ADVICOR, CADUET§, COLESTID, CRESTOR§\, §, LESCOL XL§, MEVACOR§, PRAVIGARD, QUESTRAN, Lipitor\, Lofibra, Niaspan, Pravachol\, Tricor, Vytorin, Zocor\, Zetia ALTOCOR LESCOL Welchol §, ATACAND HCT, BENICAR HCT, CADUET§, §, HYZAAR§, LEXXEL, LOPRESSOR HCT, LOTENSIN HCT§, LOTREL, MICARDIS HCT, MONOPRIL HCT§, PRINZIDE§, TARKA, TECZEM, TENORETIC, TEVETEN HCT, UNIRETIC§, VASERETIC§, ZESTORETIC§, ZIAC Avalide, Diovan HCT ACCURETIC CAPOZIDE Coreg, Toprol XL 25mg, 50mg\, 100mg, 200mg CORGARD, Inderal LA, INNOPRAN XL, KERLONE, LEVATOL, LOPRESSOR, SECTRAL, TENORMIN, TRANDATE, VISKEN, ZEBETA Norvasc: (Tier 2 if age 55 or older ADALAT CC, CALAN, CALAN SR, CARDENE, CARDENE SR , CARDIZEM, CARDIZEM CD, CARDIZEM LA , COVERA, COVERA HS, § and on concurrent ACE/ARB therapy or on nitrate therapy) §, PLENDIL§, §, TIAZAC, VERELAN, VERELAN PM DILACOR XR, DYNACIRC, DYNACIRC CR PROCARDIA XL, SULAR Zaroxolyn ALDACTONE, BUMEX, DEMADEX, DYAZIDE, DYRENIUM, §, LOZOL, MAXZIDE HYDRODIURIL, HYGROTON, INSPRA 1 Co-payment/Coinsurance for each tier is based on the specific rider chosen by the employer group. The majority of benefits include additional member payment when a brand drug is used and a generic equivalent is available. Brand drugs not listed are considered Tier 3. All compounds are considered Tier 3. § = Requires Prior Authorization \ = Half Tablet opportunity: Certain strength tablets may be split to obtain lower dosage and reduce member out-of-pocket cost * = Select self-injectable medications within this drug class are available through national specialty pharmacies CuraScript Pharmacy and Priority Healthcare p V = Generic Trial opportunity: For select doses of these medications member copayment is waived for a two-week trial prescription = Tier 2 for select prescribers/diagnoses B-1462y5 10/6/04 List Subject to Change DRUG CLASS Tier 1 Tier 2 Tier 3 (highest member co-payment) Drugs listed CAPITALIZED IN BOLD/ITALICS are considered NON-FORMULARY under the closed formulary benefit (lowest member co-payment) Nitrates (angina) Numerous generics No drugs listed at this time Potassium Supplements CENTRAL NERVOUS SYSTEM COUGH / COLD Antitussives and Expectorants potassium chloride generics pemoline Urocit-K No drugs listed at this time benzonatate, guiafenesin products, hydrocodone products No drugs listed at this time AMIBID LA, DURATUSS G, HUMABID LA, Antitussive Combinations gauifenesin/codeine, hydrocodone/homatropine, promethazine/codeine No drugs listed at this time GENESIN DM, GUAITUSS AC, HISTUSSIN, HISTUSSIN HC, HYCODAN, HYCOTUSS, PHENERGAN W/CODEINE, RONDEC-DM No drugs listed at this time No drugs listed at this time benzoyl peroxide, clindamycin, erythromycin, erythromycin/benzoyl peroxide, isotretinoin, sulfacetamide, tretinoin products, tetracycline bacitracin/polymyxin, erythromycin, gentamycin, mupirocin ointment, neo/poly, tobramycin ketoconazole cream, ketoconazole shampoo, mycostatin, triamcinolone/nystatin, betamethasone/clotrimazole betamethasone, clobetasol, dexamethasone, fluocinolone, fluocinonide, hydrocortisone, triamcinolone selenium sulfide No drugs listed at this time ENBREL§, RAPTIVA§, SORIATANE Accutane, A/T/S, AVITA, AZELEX, BenzaClin, Benzamycin, CLEOCIN T, DESQUAM E, Differin, EMGEL, DEPONIT, IMDUR, ISMO, MONOKET, NITREK, NITRODISK, NITRO-DUR, TRANSDERM-NITRO K-DUR, K-LYTE, K-TAB, MICRO-K, SLOW K CYLERT, Desoxyn, DEXEDRINE, DEXEDRINE SPANSULES, Provigil§, Xyrem§ Tussionex DERMATOLOGY Psoriasis Products* Topical/Oral Acne Products Topical Antibiotics Topical/Combination Antifungals Topical/ Oral Steroids Topicals: Psoriasis/Eczema DIABETES Blood Glucose Supplies Insulin FINACEA, FINEVIN, KLARON, METROCREAM, METROGEL, NOVACET, RETIN-A, SULFACET-R, T-STAT Bactroban cream BACTROBAN OINTMENT, EMGEL, NORITATE, SILVADENE No drugs listed at this time EXELDERM, LOPROX, LOTRIMIN, LOTRISONE, MENTAX, MYCELEX, MYCOLOG II, NAFTIN, NIZORAL CREAM, NIZORAL SHAMPOO, OXISTAT, SPECTAZOLE Capex Shampoo, Florinef ACLOVATE, CLODERM, CORDRAN, Cordran Tape, Cutivate, CYCLOCORT, DECADRON, DESOWEN, DIPROLENE/AF, ELOCON, FLORONE/E, HALOG/E, LOCOID, MEDROL DOSE PACK, PANDEL, PSORCON/E, TEMOVATE, TOPICORT, ULTRAVATE, UTICORT Dovonex, Drithocreme CAPITROL, Elidel, Protopic, Selsun, Tazorac Diabetic benefit and/or DME benefit applies: Preferred Meters are: Accu-check Active, Accu-check Advantage, Accu-check Compact, Accu-check Complete, One Touch Sure Step, One Touch Ultra (All meters are paid through DME Benefit) DIABETIC BENEFIT APPLIES FOR ALL INSULINS If Diabetic benefit DOES NOT apply please refer to the following tier classifications: No drugs listed at this time Oral Hypoglycemics Humalog, Humulin, Lantus, No drugs listed at this time Novolin, Novolog DIABETIC BENEFIT APPLIES FOR ALL ORAL HYPOGYLCEMICS If Diabetic benefit DOES NOT apply, please refer to the following tier classifications: EAR ENTERAL FORMULAS EYE Ophthalmic Antiallergics Ophthalmic Antiinfectives Ophthalmic Anti-Inflammatory Ophthalmic Antivirals Ophthalmic Combinations glipizide, glipizide ER, glyburide, glyburide/metformin, metformin, metformin XR Numerous generics Cipro HC and Floxin Otic AURULGAN, CERUMENEX, CORTISPORIN, PEDIOTIC, VOSOL, VOSOL HC No drugs listed at this time PKU Formulas§ All branded enteral products§ cromolyn sodium Optivar, Zaditor, Acular, Acular PF No drugs listed at this time ALAMAST, ALOCRIL, ALOMIDE, ALREX, EMADINE, LIVOSTIN, OPTICROM, PATANOL bacitracin, bac/poly/neo, ciprofloxacin, neosporin, ofloxacin, polysporin, erythro, gent, sodium sulfacetamide, TMP/pol, tobra dexameth, dexa/neo, fluorometholone, flurbiprofen, prednisolone No drugs listed at this time neomycin, neomycin/polymixin, dexamethasone sodium phosphate solution Actos, Amaryl, Avandia, Glyset, Prandin, Precose, Starlix Avandamet, DIABETA, GLUCOPHAGE, GLUCOPHAGE XR, GLUCOTROL, GLUCOTROL XL, GLUCOVANCE, GLYNASE, Metaglip, MICRONASE CHIBROXIN, CILOXAN, OCUFLOX, QUIXIN, VigamoxV, ZymarV Lotemax, Voltaren, PredForte FML FORTE, OCUFEN, VEXOL Vira A, Viroptic FML-S, Poly-Pred No drugs listed at this time HMS, PRED-G, TobradexV 2 Co-payment/Coinsurance for each tier is based on the specific rider chosen by the employer group. The majority of benefits include additional member payment when a brand drug is used and a generic equivalent is available. Brand drugs not listed are considered Tier 3. All compounds are considered Tier 3. § = Requires Prior Authorization \ = Half Tablet opportunity: Certain strength tablets may be split to obtain lower dosage and reduce member out-of-pocket cost * = Select self-injectable medications within this drug class are available through national specialty pharmacies CuraScript Pharmacy and Priority Healthcare p V = Generic Trial opportunity: For select doses of these medications member copayment is waived for a two-week trial prescription = Tier 2 for select prescribers/diagnoses B-1462y5 10/6/04 List Subject to Change DRUG CLASS Tier 1 Tier 2 Tier 3 Glaucoma GOUT GROWTH HORMONES* carbachol, carteolol, dipivefrin, levobunolol, pilocarpine, timolol, timolol XE allopurinol, colchicine, colchicine/probenecid, probenecid, sulfinpyrazone No drugs listed at this time (highest member co-payment) Drugs listed CAPITALIZED IN BOLD/ITALICS are considered NON-FORMULARY under the closed formulary benefit (lowest member co-payment) Alphagan P, Lumigan, Trusopt, Xalatan AZOPT, BETAGAN, BETIMOL, BETOPTIC, BETOPTIC-S, COSOPT, IOPIDINE, OCUPRESS, OPTIPRANOLOL, PILOPINE GEL, PROPINE, RESCULA, TIMOPTIC, TIMOPTIC XE, TRAVATAN No drugs listed at this time ZYLOPRIM §, HUMATROPE§, SAIZEN§, SEROSTIM§, §, TEV-TROPIN§, ZORBTIVE§ Infergen§, Intron-A, REBETOL§, Rebetron§, Roferon A HEPATITIS* HIV ribavirin§ Nutropin§, Nutropin AQ§, Norditropin§, Protropin§ Copegus§, Pegasys§, §PegIntron No drugs listed at this time All brands are Tier 2 No drugs listed at this time IMMUNE SYSTEM azathioprine, cyclosporine Cellcept, Neoral, Prograf, Rapamune, Sandimmune, Sandostatin IMURAN All brands when prescribed for patients under age 11 Augmentin, AUGMENTIN XR, Avelox, Biaxin, CECLOR CD, CEDAX, CEFTIN, Cefzil, Cipro, CIPRO XR, CLEOCIN, DYNABAC§, Floxin, Ketek, Levaquin, LORABID, Macrobid, MAXAQUIN, MONUROL, NOROXIN, OMNICEF, PCE, PENETRAX, Spectracef, SUPRAX, Tequin, Tobi, TROVAN, VANTIN, Vancocin, XIFAXAN, Zagam, Zithromax, Zyvox§ Griseofulvin Suspension, Lamisil§ Hepsera, Valtrex Diflucan, PENLAC§, Sporanox§, Vfend INFECTIONS: BACTERIAL, FUNGAL, VIRAL amoxicillin, Antibiotics amoxicillin/clavulanate, ampicillin, dicloxacillin, cefaclor, cefadroxil, cefuroxime tablets, cephalexin, ciprofloxacin, doxycycline, erythromycins, ofloxacin, penicillin fluconazole, griseofulvin, nystatin Antifungal Drugs (Oral) Antiviral Drugs MALARIA MEN’S HEALTH BPH Agents (prostate) acyclovir, amantadine, gancyclovir, rimantadine chloroquine, hydroxychloroquine, quinine doxazosin, prazocin, terazosin GENOTROPIN SOMAVERT Lariam Relenza§, Tamiflu, VALCYTE, ZOVIRAX Daraprim, Fansidar, MALARONE, Plaquenil Flomax (Tier 2 after failure to Tier 1 AVODART, CARDURA, HYTRIN, CYTOVENE, DENAVIR, FAMVIR, FLUMADINE, SYMMETREL, Proscar, UROXATRAL options) Erectile Dysfunction Hormones Oral Androgens MENTAL HEALTH Antidepressants yohimbine testosterone No drugs listed at this time None Android, Depo-Testosterone Casodex, Eulexin amitriptyline, amoxipine, desipramine, doxepin, (20 mg only) , imipramine, fluoxetinep mirtazapine, nortriptyline, paroxetine, trazodone buproprion, buproprion SR, nefazodone Celexa 40mg\, Paxil suspension, Zoloft 100mg\ Caverject, Cialis, Edex, Levitra, Muse, Viagra Androgel, TESTIM, TESTODERM No drugs listed at this time ANDRODERM, CELEXA 10MG, 20MG\, DESYREL, ELAVIL, LEXAPRO\, LUVOX, Nardil, PAMELOR, Parnate, PAXIL, PAXIL CR, §, PROZAC WEEKLY§, Remeron, SARAFEM§, SINEQUAN, SURMONTIL, SYMBYAX, TOFRANIL, ZOLOFT 25MG, 50MG\ CYMBALTA§, SYMBYAX, WELLBUTRIN, PROZAC Effexor, Effexor XR: Tier 2 only if prescribed by a psychiatrist or failure of SSRI. WELLBUTRIN SR Welllbutrin XL: Tier 2 only if prescribed by a psychiatrist, patient under age 13, or failure of SSRI. Antipsychosis Sedatives/Hypnotics/ Anxiety MIGRAINE MULTIPLE SCLEROSIS* OSTEOPOROSIS clozapine, haloperidol, trifluoperazine, thioridazine Geodon, Risperdal, Seroquel benzodiazepines (alprazolam, clonazepam, diazepam, triazolam), hydroxyzine ergotamine, isometheptene/dichlor/APAP Ambien (only if over age 65) ATIVAN, BUSPAR, SERAX, SONATA, VALIUM, XANAX Amerge, Depakote ER, Maxalt, Maxalt MLT, Migranal, Imitrex 100mg & 50mg tablets, Imitrex nasal spray and injection AXERT, FROVA, IMITREX 25MG TABLETS, RELPAX, ZOMIG, ZOMIG INTRANASAL, ZOMIG ZMT No drugs listed at this time Betaseron, Copaxone Actonel, Actonel Weekly, Evista, Fosamax, Fosamax Weekly No drugs listed at this time CLOZARIL, HALDOL, MELLARIL, NAVANE, PROLIXIN, STELAZINE, THORAZINE, TRILAFON Abilify, Zyprexa (Tier 2 when prescribed by a psychiatrist and failure to Tier 2 options) Avonex, Rebif DIDRONEL, Forteo, SKELID, Miacalcin Nasal 3 Co-payment/Coinsurance for each tier is based on the specific rider chosen by the employer group. The majority of benefits include additional member payment when a brand drug is used and a generic equivalent is available. Brand drugs not listed are considered Tier 3. All compounds are considered Tier 3. § = Requires Prior Authorization \ = Half Tablet opportunity: Certain strength tablets may be split to obtain lower dosage and reduce member out-of-pocket cost * = Select self-injectable medications within this drug class are available through national specialty pharmacies CuraScript Pharmacy and Priority Healthcare p V = Generic Trial opportunity: For select doses of these medications member copayment is waived for a two-week trial prescription = Tier 2 for select prescribers/diagnoses B-1462y5 10/6/04 List Subject to Change DRUG CLASS Tier 1 Tier 2 Tier 3 (lowest member co-payment) PAIN / INFLAMMATION Muscle Relaxants NSAIDs Pain Relievers (narcotic) PARKINSON’S SEIZURE / PAIN SMOKING DETERRENTS STOMACH / INTESTINAL Antiemetics baclofen, methocarbamol, carisoprodol, cyclobenzaprine diclofenac, fenoprofen, flurbiprofen, ibuprofen, indomethacin, ketoprofen, nabumetone, naproxen, naproxen sodium, oxaprozin, piroxicam, salsalate, sulindac, tolmetin No drugs listed at this time acetaminophen/codeine, acetaminophen/propoxyphene, hydrocodone combinations, methadone, morphine, oxycodone SR amantadine, anticholinergics, benztropine, bromocriptine, carbidopa/levodopa, selegiline carbamazepine, clonazepam, phenytoin, valproic acid (highest member co-payment) None NORFLEX, SKELAXIN, ZANAFLEX No drugs listed at this time Step Therapy applies: ARTHROTEC, CATAFLAM, DAYPRO, EC-NAPROSYN, LODINE XL, MOBIC, NAPRELAN, ORUVAIL, PONSTEL, RELAFEN, TORADOL, VOLTAREN XR No drugs listed at this time Step Therapy applies: Bextra\, Celebrex DuragesicV, OxycontinV AVINA, AVINZA, KADIAN, MS CONTIN, MSIR, NORCO, ORAMORPH SR, OXYIR, ULTRAM, ZYDONE (Tier 2 for chronic, intractable pain with letter of medical necessity) Comtan, Permax, Requip APOKYN, COGENTIN, DOPAR, ELDEPRYL, LARODOPA, LODOSYN, MIRAPEX, PARLODEL, SINEMET CR, STALEVO, TASMAR Depakote, Dilantin, Felbatol, Gabitril, Keppra, Klonopin, Neurontin, Tegretol XR, Trileptal, Zarontin No drugs listed at this time No drugs listed at this time buproprion SR No drugs listed at this time NICOTROL INHALER, NICOTROL SPRAY, ZYBAN meclizine, prochlorperazine, Zofran ALOXI, ANZEMET, EMEND, TRANSDERM-SC bethanechol, clidinium products, dicyclomine, hyoscyamine, oxybutyninp pancrealipase No drugs listed at this time DETROL, LamictalV , TopamaxV, ZonegranV (for nausea) Antispasmotic Drugs Digestants Inflammatory Bowel Irritable Bowel Syndrome Ulcer/Heartburn sulfasalazine, hydrocortisone enema No drugs listed at this time cimetidine, famotidine, ranitidine No drugs listed at this time omeprazole§, Prilosec OTCp Kytril, MARINOL, Detrol LA, DITROPAN, DITROPAN XL, LEVSIN, § LEVSINEX, OXYTROL PATCH, SANCTURA , URECHOLINE, URISPAS Cotazym, Cotazym S, Creon, Kutrase, Pancrease, Pancrease MT, Ultrase MT, Viokase, Zymase Asacol, Canasa, Cortenema, Dipentum, Pentasa, Rowasa enema No drugs listed at this time No drugs listed at this time No drugs listed at this time Prevacid, Protonix No drugs listed at this time AZULFIDINE (ENTERIC COATED), Colazal, Entocort EC Lotronex§, Zelnorm§ AXID, PEPCID, TAGAMET, ZANTAC Helidac, Prevpac,TRITEC ACIPHEX§ NEXIUM§, PREVACID NAPRAPAK§, PRILOSEC§, § THYROID WEIGHT MANAGEMENT metoclopramide, sucralfate levothyroxine, levoxyl, levothroid, PTU diethylpropion RAPINEX CARAFATE Cytotec Cytomel, Tapazole ARMOUR THYROID, SYNTHROID, THYROLAR, UNITHROID No drugs listed at this time ADIPEX-P, ADIPOST, BONTRIL-SR, DIDREX, Meridia§, phentermine, Xenical§ WOMEN’S HEALTH Fertility Drugs* clomiphene citrate No drugs listed at this time Bravelle§, Clomid, Crinone, Fertinex§, Follistim§, Gonal-F§, Humegon§, Metrodin§, Ovidrel§, Pergonal§, Repronex§ estradiol, medroxyprogesterone Estratest, Estratest HS, Premarin, Premphase, Prempro, Prometrium Climara, Climara Pro Ortho Evra, Ortho-Tri-Cyclen LO, Yasmin ACTIVELLA, CENESTIN, ENJUVIA, ESTRACE, ESTRATAB, FEMHRT, MENEST, OGEN, ORTHO-PREFEST Note: Not all prescription drug benefits provide coverage Hormones Oral Transdermal Oral Contraceptives estradiol patch Alora, Combipatch, ESTRADERM, VIVELLE/DOT ALESSE, BREVICON, CYLESSA, DEMULEN, DESOGEN, Apri, Aviane, Camila, Cryselle, ESTROSTEP, ESTROSTEP FE, LEVLEN, LEVLITE, LOESTRIN, Enpresse, Jolivette, Kariva, Note: Not all prescription drug LOESTRIN FE, LO-OVRAL, MIRCETTE, MODICON, NORDETTE, Lessina, Levora, Low-Ogestrel, benefits provide coverage NORINYL, NOR QD, NUVARING, ORTHO-CEPT, ORTHOCYCLEN, ORTHO MICRON, ORTHO-NOVUM, ORTHO TRIMicrogestin FE, Necon, Nelova, CYCLEN, OVCON, OVRAL, PREVIFEM, TRI-LEVLEN, Nora B, Nortrel, Ogestrel, Portia, TRINORINYL, TRIPHASIL Sprintec, Tri-Nessa, Tri-Previfem, Tri-Sprintec, Trivora, Zovia Miscellaneous Tier 2 agents: DDAVP tablets, Diamox Sequels, Elmiron, Epipen, Epipen Jr., Evoxac, Glucagen, Mestinon, Metrogel Vaginal, Metrolotion, Phoslo, Premarin Vaginal, Pulmozyme, Renagel, Rilutek, Salagen, Stimate, Synarel 4 Co-payment/Coinsurance for each tier is based on the specific rider chosen by the employer group. The majority of benefits include additional member payment when a brand drug is used and a generic equivalent is available. Brand drugs not listed are considered Tier 3. All compounds are considered Tier 3. § = Requires Prior Authorization \ = Half Tablet opportunity: Certain strength tablets may be split to obtain lower dosage and reduce member out-of-pocket cost * = Select self-injectable medications within this drug class are available through national specialty pharmacies CuraScript Pharmacy and Priority Healthcare p V = Generic Trial opportunity: For select doses of these medications member copayment is waived for a two-week trial prescription = Tier 2 for select prescribers/diagnoses B-1462y5 10/6/04 List Subject to Change Utica Business Park, 12 Rhoads Drive Utica, New York 13502-6398 PRSRT STD U.S. POSTAGE PAID ROCHESTER, NY Permit No. 201