* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Popular Links
Menstruation wikipedia , lookup
Birth control wikipedia , lookup
Women's medicine in antiquity wikipedia , lookup
Prenatal nutrition wikipedia , lookup
Fetal origins hypothesis wikipedia , lookup
Reproductive rights wikipedia , lookup
Reproductive health wikipedia , lookup
Prenatal testing wikipedia , lookup
Prenatal development wikipedia , lookup
Maternal physiological changes in pregnancy wikipedia , lookup
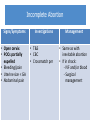
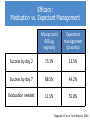
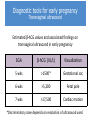
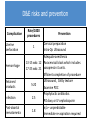
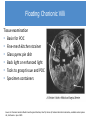
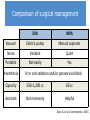
First Trimester Bleeding and Abortion Objectives Develop a differential for first trimester vaginal bleeding Differentiate the types of spontaneous abortion (missed, complete, incomplete, threatened, septic) Describe the causes of spontaneous abortion List the management options for spontaneous abortion Describe reasons for induced abortion List methods of induced abortion Understand the public health impact of the legal status of abortion Case No. 1 24yo G1P0 presents to your office and reports spotting dark blood for 4 days. What are your initial history questions? What steps will you take to make the final diagnosis? Most Common Differential Diagnosis of 1st Trimester Bleeding Ectopic pregnancy Normal intrauterine pregnancy Threatened abortion Abnormal intrauterine pregnancy Diagnosis tools for early pregnancy Urine pregnancy test (UPT) Accurate on first day of expected menses β-hCG 6-8 days after ovulation – present Date of expected menses (@14 days after ovulation) – βhCG is 100 IU/L Within first 30 days – β-hCG doubles in 48-72 hours Important for pregnancy diagnosis prior to ultrasound diagnosis Diagnosis of threatened abortion Diagnosis made by ultrasound and/or ßhCG – normally growing early pregnancy, but with vaginal bleeding More formal definition: Vaginal bleeding before the 20th week Bleeding in early pregnancy with no pregnancy loss Threatened abortion Signs/ Symptoms • • • • • Closed cervix Viable fetus Uterine size = GA Minimal bleeding Minimal/no pain Work Up • Ultrasound for viability • T&S Management • No specific treatment Threatened abortion: outcomes 25-50% will progress to spontaneous abortion However – if the pregnancy is far enough along that an ultrasound can confirm a live pregnancy then 94% will go on to deliver a live baby Case No. 1 Continued On the ultrasound exam you note a CRL consistent with 8 weeks but no cardiac motion. – What kind of abortion does she have? – What proportion of clinically recognized pregnancies will end in spontaneous abortion? – What proportion of spontaneous abortions are due to chromosomal abnormalities? – What are some of the non-chromosomal etiologies of spontaneous abortion? – What are her options for management? – What are the advantages of each option? Diagnosis of Spontaneous Abortion (SAB) or Early Pregnancy Failure (EPF) SAB/EPF if Ultrasound measurements are: > 7mm CRL and no fetal heart rate > 25mm Mean Sac Diameter and no embryo Absence of embryo with heartbeat > 2 weeks after scan showing gestational sac w/o yolk sac > 11 days after scan showing gestational sac w/ yolk sac Gestational sac growth <2mm over 5 days <3mm over 7 days Change in β-hCG is <35% (vs 15%) rise in β-hCG over 48 hours* Doubilet, NEJM 2013 Morse, Fert Ster 2012 Abortion definitions Definition Any pregnancy loss before 28 weeks or a fetus < 500 g Types of abortion Miscarriage – Also called spontaneous abortion (SAB) or early pregnancy failure (EPF) Induced Consider in any woman of reproductive age with: Amenorrhea Bleeding, abdominal pain Partial expulsion of products of conception, dilated cervix Uterus smaller than expected Types of spontaneous abortion Inevitable: intrauterine pregnancy with cervical dilation & vaginal bleeding Incomplete: cervix open, some tissue has passed Complete: pregnancy has been expelled completely Missed: embryo never formed or demised, but uterus has not expelled the sac Septic: missed/incomplete abortion becomes infected Chemical pregnancy: (+)β-hcg but no sac formed Blighted ovum/anembryonic pregnancy: empty gestational sac, embryo never formed Spontaneous abortion: Epidemiology and etiology Epidemiology 15-25% of all clinically recognized pregnancies Offer reassurance: probability of 2 consecutive miscarriages is 2.25% 85% of women will conceive and have normal third pregnancy if with same partner 80% in the first 12 weeks Etiologies Chromosomal – 50% Non-chromosomal – 50% SAB/EPF: Chromosomal Etiologies 50% trisomies 50% triploidy, tetraploidy, X0 SAB/EPF: Non-Chromosomal Etiologies Maternal systemic disease Antiphospholipid antibody syndrome, lupus, coagulation disorders Infectious factors Brucella, chlamydia, mycoplasma, listeria, toxoplasma, malaria, tuberculosis Endocrine factors Diabetes, hypothyroidism, “luteal phase defect” from progesterone deficiency SAB/EPF: Non-Chromosomal Etiologies Abnormal placentation Anatomic considerations fibroids, polyps, septum, bicornuate uterus, incompetent cervix, Asherman’s Environmental factors Smoking >20 cigarettes per day (increased 4X) Alcohol >7 drinks/week (increased 4X) Increasing age Inevitable Abortion Signs/Symptoms • Open cervix • Bleeding, but no passage of POCs • Abdominal pain • Uterine size = GA Work Up • • • • T&S CBC prn Crossmatch prn Vitals – if concern for infection, treat as with septic abortion Management Three options: 1) Expectant 2) Medical 3) Surgical • Bereavement counseling • Contraception prn Incomplete Abortion Signs/Symptoms Investigations • Open cervix • POCs partially expelled • Bleeding/pain • Uterine size < GA • Abdominal pain • T&S • CBC • Crossmatch prn Management • Same as with inevitable abortion • If in shock: - IVF and/or blood - Surgical management Complete Abortion Signs/Symptoms • Closed cervix • POCs completely expelled • Small uterus • Minimal pain/bleeding Work Up • T&S • CBC prn • Ultrasound to confirm empty uterus Management • Bereavement counseling • Fe supplement prn • Contraception prn: start immediately if passage of POCs within past 2 weeks Missed Abortion Signs/Symptoms • Closed cervix • No bleeding/pain • Loss of pregnancy symptoms Investigations • T&S • CBC prn • Ultrasound to confirm nonviability Management 1) Expectant – okay for longer than inevitable abortion 2) Medical 3) Surgical Management of spontaneous abortion 1. Expectant management 2. Uterine evacuation by medication 3. Uterine evacuation by suction Manual Electric Efficacy: Medication vs. Expectant Management Misoprostol 600 μg vaginally Expectant management (placebo) Success by day 2 73.1% 13.5% Success by day 7 88.5% 44.2% Evacuation needed 11.5% 55.8% Bagratee JS, et al. Hum Reprod. 2004. Medication management of SAB/EPF Misoprostol Synthetic prostaglandin E1 analog Inexpensive Orally active Multiple effective routes of administration Can be stored safely at room temperature Effective at initiating uterine contractions Effective at inducing cervical ripening Surgical management SAB/EPF Manual Vacuum Aspiration Ensures products of conception (POCs) are fully evacuated Minimal anesthesia needed Comfortable for women due to low noise level Portable for use in physician office familiar to the woman Do not need electricity Dilators if os is closed Women very satisfied with method MVA Label. Ipas. 2007. Surgical management SAB/EPF Electric Vacuum Aspirator Electric vacuum aspirator Uses an electric pump or suction machine connected via flexible tubing Creinin MD, Obstet Gynecol Surv. 2001 Goldberg AB, Obstet Gynecol. 2004 Hemlin J, Acta Obstet Gynecol Scand. 2001 Floating Chorionic Villi Tissue examination Basin for POC Fine-mesh kitchen strainer Glass pyrex pie dish Back light or enhanced light Tools to grasp tissue and POC Specimen containers Source: A Clinicians Guide to Medical and Surgical Abortion; Paul M, Grimes D, National Abortion Federation, available online Hyman AG, Castleman L. Ipas. 2005 Comparison of surgical management EVA MVA Vacuum Electric pump Manual aspirator Noise Variable Quiet Portable Not easily Yes Anesthesia IV or oral sedation and/or paracervical block Capacity 350–1,200 cc 60 cc Assistant Not necessary Helpful Dean G, et al. Contraception. 2003. EVA and MVA risks and prevention Complication Uterine perforation Hemorrhage Rate/1000 procedures Prevention Cervical preparation 1 Intra-Op Ultrasound <12 wks – 0 Efficient completion of procedure Retained products 3 Infection 2.5 Post-abortal hematometra 1.8 Ultrasound Gritty texture Examine POC Prophylactic antibiotics PO doxy or IV cephalosporin N/a – unpredictable Immediate re-aspiration required Pain Management Aspiration/vacuum Medication abortion Preparation Music Support during procedure PO or IV sedation Paracervical block NSAIDS Oral narcotics and antiemetics if necessary Case No. 2 27yo G5P4 with LMP 8 wks ago presents with fever to 101.4, abdominal pain, and vaginal bleeding. What is in your differential diagnosis? What are your initial history questions? What pertinent findings might you look for on physical exam? Case No. 2 Continued The patient states that she “took a pill to make her period come down” a couple weeks ago and has had spotting ever since. The fever started last night, and the bleeding has now gotten heavier. On exam, her os is open and she has purulent discharge. She also has fundal tenderness. What kind of abortion does she have? What risk factors does she have for this diagnosis? What are her options for management? Septic Abortion Signs/Symptoms Investigations • Any of above types • CBC with diff of abortion with • T&S any of the • T&C prn following: - T ≥ 38◦C - Tachycardia - Purulent discharge - Pelvic pain - Possible pregnancy interference Management • • • • • IVF and/or blood Monitor VS and UOP IV antibiotics D&C At risk for coagulopathy Case No. 3 32yo G2P1 presents with lower abdominal pain, vaginal spotting, and an LMP 6 weeks ago. What’s in your differential diagnosis? What pertinent things about her history would you like to know? What would you look for on physical exam? What labs/imaging studies would you order? Diagnostic tools for early pregnancy Transvaginal ultrasound Estimated β-hCG values and associated findings on transvaginal ultrasound in early pregnancy EGA β-hCG (IU/L) Visualization 5 wks >1500* Gestational sac 6 wks >5,200 Fetal pole 7 wks >17,500 Cardiac motion *Discriminatory zone depends on resolution of ultrasound used. Case No. 3 Continued Her β-HCG returns as 3200 and a pelvic ultrasound does not demonstrate an intrauterine pregnancy What is her likely diagnosis? What are some risk factors for this diagnosis? What are her treatment options? What would you tell her about future pregnancies? Case No. 4 A 38 year-old G1P0 had an ultrasound that showed fetal anencephaly at 20 weeks. You know that most anencephalic fetuses do not survive birth. How do you counsel this patient? What are her options for management? What questions do you ask her to help her make a decision for management? Induced Abortion/Pregnancy Termination Language: Indications Personal choice Medical indication (hemorrhage, infection) Medical recommendation (SLE, Pulmonary HTN, PPROM) Fetus diagnosed with anomalies Termination Abortion Elective abortion Therapeutic abortion Interruption of pregnancy Definition The removal of a fetus or embryo from the uterus before the stage of viability Methods Dependent upon gestational age and provider abilities Induced Abortion History Any discussion of abortion needs to include some of the legal and political aspects Providers should be familiar with the abortion laws in their own states Providers performing abortions must know the laws in their own state Induced Abortion Epidemiology 1 in 3 women by the age of 44 years 1/3 occur in women older than 24 years Gestational age: 90% within first 12 weeks 50% within first 8 weeks Complications Dependent upon gestational age 7-10 weeks have lowest complication rates mortality: 1/100,000 Complications are 3-4x higher for second-trimester than first trimester Putting Induced Abortion into Perspective… Incident Chance of death Terminating pregnancy < 9 weeks 1 in 500,000 Terminating pregnancy > 20 weeks 1 in 8,000 Giving birth 1 in 7,600 Driving an automobile 1 in 5,900 Using a tampon 1 in 350,000 Gold RB, Richards C. Issues Sci Technol. 1990.; Hatcher RA. Contracept Technol Update. 1998.; Mokdad AH, et al. MMWR Recomm Rep. 2003. Earlier Procedures are Safer Abortions at < 8 weeks = lowest risk of death 1 Gestational Age Strongest risk factor for abortion-related mortality Weeks Gestation 4 ≤8 6 9 to 10 10 61% 18 11 to 12 ≤8 weeks 13 to 15 16 to 20 ≥21 Bartlet L, et al. Obstet Gynecol. 2004. Induced Abortion Methods Uterine evacuation (basically the same as treatment of abortion; however, the cervix is closed) Manual vacuum aspiration Electric vacuum aspiration Medication Mifepristone and misoprostol Medical abortion methods Mifepristone 19-norsteroid that specifically blocks the receptors for progesterone and glucocorticosteroids Antagonizing effect blocks the relaxation effects of progesterone Results in uterine contractions Pregnancy disruption Dilation and softening of the cervix Increases the sensitivity of the uterus to prostaglandin analogs by an approximate factor of five Takes 24-48 hours for this to occur* Misoprostol Synthetic prostaglandin E1 analog Inexpensive Multiple effective routes of administration Can be stored safely at room temperature Effective at initiating uterine contractions Effective at inducing cervical ripening Used in decreasing doses as pregnancy advances Contraindications to Medical Abortion • Suspected or confirmed ectopic pregnancy • Anemia (Hb < 9.5 g/dL) • IUCD • Coagulopathy or use of anti-coagulants • Chronic adrenal failure • Intolerance or allergy to medications • Inability to follow instructions Medical abortion protocols 1. Mifepristone 200 mg orally 2. Misoprostol 800 mcg - Vaginally 6 hours later or - Buccal or sublingual 24-48 hours later 3. Follow up 1-2 weeks later with history and pelvic exam or ultrasound Gestational age (days) Complete abortion rate (%) < 63 95-99% 64-70 93% SFP Guidelines, Contraception 2014. 2nd Trimester Induced Abortion Counseling Discuss pain management Informed Consent Discuss contraception – even those with abnormal or wanted pregnancy may not want to follow immediately with another pregnancy Ovulation can occur 14-21 days after a second trimester abortion; risk of pregnancy is great and must be addressed Lactation can occur between days 3-7 post-abortion Procedure Follow-up Nyoboe 1990 2nd trimester induced abortion • Labor induction • Dilation & evacuation (D&E) 2nd trimester induced abortion Management Dilation and evacuation Labor induction abortion Two visits in 1-2 days Requires inpatient hospital stay usually lasting 1-3 days Anesthesia/analgesia required Average time to delivery 13 hrs Procedure room required Increased likelihood of retained placenta resulting in uterine evacuation compared to D&E Skilled surgeon Medication used misoprostol and/or mifepristone Cervical preparation required before procedure Labor Induction Abortion Patient is awake Fetus delivered intact Labor Induction Abortion Hospital admission Misoprostol or misoprostol and mifepristone to cause contractions and uterine evacuation 20% may require vacuum aspiration for retained placenta Requirements for a safe D&E Program Surgeons skilled and experienced in D&E provision Adequate pain control options with appropriate monitoring Requisite instruments available Staff skilled in patient education, counseling, care and recovery Established procedures at free standing facilities for transferring patients who require emergency hospitalbased care D&E Step 1 cervical Preparation Laminaria Osmotic dilators Dried compressed seaweed sticks, 5-10mm diameter in size 4-19 dilators can be placed Slow swelling to exert slow circumferential pressure and dilation 1-2 days prior to procedure Paracervical block with 20cc 0.25% bupivicaine D&E Procedure Adequate anesthesia Ultrasound guidance Uterine evacuation using suction and instruments Paracervical block with 20cc 0.5% lidocaine and 4U vasopressin to decrease blood loss D&E risks and prevention Complication Uterine perforation Hemorrhage Retained products Infection Post-abortal hematometra Rate/1000 procedures Prevention Cervical preparation 1 Intra-Op Ultrasound Adequate anesthesia 13-15 wks: 12 Paracervical block which includes 17-25 wks: 21 vasopressin 4 units. Efficient completion of procedure Ultrasound, Gritty texture 5-20 Examine POC Prophylactic antibiotics 2.5 PO doxy or IV cephalosporin n/a – unpredictable 1.8 Immediate re-aspiration required Bottom Line Concepts First trimester bleeding occurs in 25% of all pregnancies and 25-50% will progress to a spontaneous abortion Etiologies of first trimester bleeding include normal pregnancy, spontaneous abortion/early pregnancy failure, or ectopic pregnancy. Diagnosis of normal vs abnormal early pregnancy made using physical exam and ultrasound and/or ß-hCG 50% of spontaneous abortions are the result of genetic abnormalities Management of spontaneous abortion can be medical or surgical and surgical options can be in the operating room or in the clinic 1/3 women will have an induced abortion Induced abortion before 8 weeks is safest Risks associated with induced abortion are less than childbirth or driving a car Methods for induced abortion include medication or surgical References and Resources Additional references not included in slides: APGO Medical Student Educational Objectives, 9th edition, (2009), Educational Topic 16 (p34-35), 34 (72-73) Beckman & Ling: Obstetrics and Gynecology, 6th edition, (2010), Charles RB Beckmann, Frank W Ling, Barabara M Barzansky, William NP Herbert, Douglas W Laube, Roger P Smith. Chapter 13 (p147-150). Hacker & Moore: Hacker and Moore's Essentials of Obstetrics and Gynecology, 5th edition (2009), Neville F Hacker, Joseph C Gambone, Calvin J Hobel. Chapter 7 (p74-78). These slides were modified from the original slides created by Jennifer Tang, MD and Erika Levi, MD.