* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Overview-Arrhythmias are caused by disturbances of the electrical
Survey
Document related concepts
Coronary artery disease wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Myocardial infarction wikipedia , lookup
Jatene procedure wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Ventricular fibrillation wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Transcript
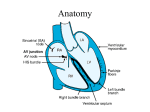
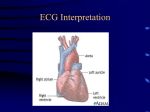
Overview-Arrhythmias are caused by disturbances of the electrical conduction system of the heart. They can result in either bradycardia or taccycardia, and be anywhere from aystompatic to lethal. This section will rapidly review normal conduction, and the electrocardiogram (ECG), with that as a basis we will move onto a discussion in outline form of bradycardias and taccyarthmias. The management of stable and unstable rhythms is in accordance with the current 2010 American Heart Association guidelines. Normal Conduction: The sinoatrial (SA) node discharges, and depolarization spreads through the atrial muscle. A delay occurs as the charge passes through atrial ventricular (AV) node, made up of specialized atrial tissue. The charge then passes through the single pathway A-V bundle (Bundle of His) in the ventricle before it divides into the right and left bundle branches. ECG: The normal ECG consists of a P wave a QRS wave and a T wave. All ECG machines run at standard rate and print on standard paper. Each large 5 mm square is 0.2 s, so there are 5 large squares to one second. Each small square is 0.04s (40 ms). The R-R interval is the time between beats, and can be used to calculate the HR from the rhythm strip; if there is one beat every 5 squares the HR is 60 bpm, if there is a beat every square it is 300 bmp. The PR interval is the time it takes for the excitation to spread from the SA node, through the atrial muscle and AV node, down the AV bundle and into the ventricular muscle. It is measured from the beginning of the P-wave to the beginning of the QRS wave. The normal PR interval is 120-200 ms or 3-5 small squares on the ECG strip. The normal QRS is <120 ms (3 squares). The ST segment is measured from the end of the S segment to the beginning of the P. The P-wave is atrial de-polarization and the QRS ventricular. T wave is re-polarization of the ventricular conduction pathway. ST elevation can result from a failure of ischemic tissue to re-polarize. BRADYCARDIA Sinus Bradycardia: Arises from the SA node, normal PR. HR <60/min, not generally symptomatic unless <50/min. It can be normal or a result of the vasovagal reflex. AV Nodal Block: Can be caused by hyperkalemia, hypermagnesemia, digoxin and b-blockers. o First-Degree: Prolonged PR > 0.2 s (one large box on ECG), all P-waves are conducted, and the PR interval is fixed. Usually asymptomatic, no treatment or further work-up required. o Second-Degree Type 1 (Wenckebach): The P waves occur at regular intervals but there is, progressive prologation of the PR interval with each eventual missed beat (P-wave with no QRS). It is a stable rhythm, once causal medication stopped resolves. Second-Degree Type 2: Sudden nonconducted P-wave without change in the PR interval. A sudden dropped QRS is observed. It is inherently unstable with P:QRS ratios of 3 or 4:1, and almost always an infra AV nodal conduction disturbance. It can be caused by an anterior wall MI, and can progress into third degree block o Third-Degree: Complete dissociation of the P and QRS waves. The Pwaves march through at regular intervals. The QRS waves can be narrow or complex. It can result from inferior and anterior wall MIs, and often requires permanent pacemaker placement. Treatment o Stable: Observation, identify and treat the cause, permanent pacemaker o Unstable: Indentify and treat the cause, 1) Atropine (0.5 mg bolus, repeat every 3-5 minutes) 2) Transcutaneous pacing 3) Dopamine (2-10 mcg/kg/min) or Epinephrine (2-10 mcg/min) infusions 4) Transvenous pacing if available. BUNDLE BRANCH BLOCK: Right and left-bundle branch block can be a sign of ischemic disease. In addition if the patient is tachycardic they can be confused with more malignant rhythms, and ischemia. Right Bundle Branch Block (RBBB): No RB conduction-RV depolarizes from the left causing the r wave before the QRS (rSR) in V1, and a small Q-wave in V6. The RV depolarizes after the left, causing R´ in V1 and deep S in V6. Left Bundle Branch Block (LBBB): No LB conduction, depolarizes from the right; causing a very small Q wave in V1, and an R wave in V6. Further depolarization causes an S-wave in V1 and a second R wave in V6. TACCYCARDIA: Is defined as a HR> 100 bpm and is characterized as wide complex or narrow complex QRS, regular or irregular, and stable or unstable. A narrow complex QRS is < 120 ms. Rates <150 bpm do not usually in cause instability. SUPRAVENTRICULAR: Narrow-complex, however can be wide if LBBB/RBBB Sinus Tachycardia (Narrow QRS, regular): A physiologic response to an external stimuli (pain, fever etc), usually not a source of instability in the short term. Re-entry Tachycardia, nodal taccycardia (Narrow QRS, regular) Younger, healthy patients rate 120-250 bpm, twice as common in women, rapid onset, often relieved by Valsava, can be wide complex if impulse enters non-specialized ventricular myocardium and depolarizes slowly. Atrial Fibrillation (Irregular, no P-waves, HR variable) and Flutter (Saw-tooth Pwaves, usually 150 bpm and regular). Associated with cardiovascular pathologies, including CAD and HTN, effects 1-2% of the population, can be associated with slow conduction or AV block, often unstable. Multifocal Atrial Tachycardia (MAT) (P waves present, irregular) o Rapid and irregular, P wave morphology variable, rarely causes instability and reverses with electrolyte correction, usually stable Treatment: Correction of electrolyte abnormalities, removal of inciting causes o Stable: Atrial Fibrillation/Flutter: B-blocker, amiodarone, digoxin (in HF patients), calcium channel blockers, burst pacing in pts with pacemaker. Amiodarone: Effective in converting both fibrillation and flutter, controls HR, low Torsades risk, not a negative inotrophic agent, safe in critical illness o Unstable: Synchronized Cardioversion Irregular QRS (atrial fibrillation/flutter): 120-200 J Narrow regular: 50-100 J, can consider adenosine 1st Adenosine: Terminates AV nodal re-entry taccycardia, will not terminate atrial fibrillation/flutter but can slow the rate to make the diagnosis. 6 mg IV given rapidly (1-3 sec), 2nd dose 12 mg IV. POST OPERATIVE ATRIAL FIBRILLATION Incidence and Outcome o Better studied in cardiac surgical patients, but it is a common issue in trauma and non-cardiac surgical patients o Often self limited but recurs in 40% of patients o Increases ICU and HLOS, increased rate of CVA and mortality Prevention o B-blocker PeriOperative Ischemia Study Evaluation (POISE)-non-cardiac post-op, prospective, randomized trial of post-op b-blocker for prevention of cardiac events Decreased rate of cardiovascular events but, INCREASED rate of death and CVA, especially in patients with low risk for cardiac events. Increased rates of bradycardia and hypotension Still recommended in cardiac surgical patients, no longer as a preventative treatment in non cardiac surgery, but b- blockers should be restarted as soon as it is safe in patients who were taking them pre-operatively o Statins Randomized trail in Cardiac Surgical Patients, decreased rate of afib and other cardiac events, no increase in hypotension or bradycardia Accumulating evidence that statins may be cardioprotective in a variety of post-operative patients, may also protect against sepsis (patients on statins less likely to die from septic shock) Restart in any patients who were on them pre-operatively, or preICU stay-higher mortality if not. Minimal risk of liver injury o Magnesium May prevent afib, somewhat controversial, consider maintaining levels above 2.5 in at risk patients Treatment o Rate Control B-blockers and Calcium Channel Blockers B-blockers better control of ventricular responsive B-blockers more conversion to NSR in post-operative patients Target rate 90-110 b/min (higher then outpatient target) Amiodarone Effective in both rate control and cardioversion Not a cardiac depressent (like B-blockers) Safe in the short term o Cardioversion Electrical synchronized in unstable patients (load with amiodarone) Chemical agents Flecainide, Ibutilide (Class 1) Amiodarone (Class 2) o Anticoagulation o Ongoing questions How long to continue therapy (especially Amiodarone) in patients with new onset difficult to convert/control post-operative afib Length of anticoagulation in patients who with paroxysmal new onset post-op afib Hard to know if post-operative period caused a transient episode, or if it unmasked structural cardiac dysfunction which requires longer term treatment VENTRICULAR ARRYTHMIAS: Wide complex >120 ms, morphology of QRS is different then in prior ECGs, abnormal T waves, usually regular rate 120-170. It is caused by underlying ischemic disease, hypothermia and electrolyte abnormalities. Ventricular Tachycardia (VT): 3 or more beats, prolonged if > 30 seconds o Monomorphic: QRS waves have similar morphologies Consider supra-ventricular tachycardia with LBBB/RBBB (look at prior ECG) If A-V dissociation VT o Polymorphic (normal QT): QRS waves have different morphologies can degenerate into ventricular fibrillation. o Polymorphic (Torsades de points): Evolves from prolonged QT interval, often caused by medications that prolong the QT. Rapid VT that vary in amplitude and polarity, or twisting around the baseline. Initiated when a beat falls prematurely on a T-wave. o Treatment: Oxygen, remove inciting events, electrolyte correction, IV access 12 lead ECG. Stable: Monomorphic ONLY consider adenosine. Polymorphic anti-arrhythmic infusion: Procainimide o 20-50 mg/min until suppressed, follow by infusion o Stop if hypotesion, or QRS increase by > 50% Amiodarone o 150 bolus over 5 mins, then drip, repeat as needed if VT recurs Sotalol o 100 mg (1.5mg/kg) over 5 minutes o Avoid if prolonged QT Unstable: Synchronized cardioversion, ACLS protocol if loss of vital signs. Ventricular Fibrillation (VF): No waveform, may be course or fine o Treatment: ACLS protocol ACLS protocol for Cardiac Arrest with VT/VF: Call for help, give O2, attach monitor o Shock-Biphasic at maximum dose (120-200 J), 2 full minutes of CPR, IV access, check rhythm , Shock, 2 full minutes of CPR, Epinephrine, advanced airway, capnography, check rhythm, Shock, 2 full minutes of CPR, Amiodarone References: 1. Fink MP, Abraham E, Vincent JL, Kochanek PM. Textbook of Critical Care, Fifth Edition. Chapters 95-98 (pages 771-821) © 2005, Elsevier Sanders, Philadelphia PA, USA 2. Sinz E, Navarro K, American Heart Association, Advanced Cardiovascular Life Support, Guidelines CPR 2010 © 2011 American Heart Association Dallas TX, USA 3. Omae T, Kanmura Y. Management of postoperative atrail fibrillation. J Anesth (2012)26:429-437 4. Link MR. Evaluation and Initial Treatment of Supraventricular Tachycardia. N Engl J Med 2012;376:1438-48 5. Patti G, Chello M, Candura D, et al. Randomized Trial of Atorvastatin for Reduction of Postoperative Atrial Fibrillation in Patients Undergoing Cardiac Surgery. Circulation 2006;114(14):1455-1461