* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Drugs prescription during pregnancy
Survey
Document related concepts
Compounding wikipedia , lookup
Orphan drug wikipedia , lookup
Polysubstance dependence wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
Drug design wikipedia , lookup
Drug discovery wikipedia , lookup
Neuropharmacology wikipedia , lookup
Pharmacogenomics wikipedia , lookup
Pharmaceutical industry wikipedia , lookup
Pharmacokinetics wikipedia , lookup
Pharmacognosy wikipedia , lookup
Prescription costs wikipedia , lookup
Transcript
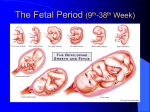
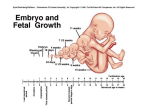
Drugs in Pregnancy and Lactation Dr Safaeian DRUG THERAPY IN PREGNANCY Most drugs taken by pregnant women can cross the placenta and expose the developing embryo and fetus to their pharmacologic and teratogenic effects. Pharmacokinetics Factors affecting placental drug transfer and drug effects on the fetus : (1) Physicochemical properties of drug (2) The rate at which drug crosses placenta and the amount of drug reaching fetus (3) Duration of exposure to drug (4) Distribution characteristics in different fetal tissues (5) Stage of placental and fetal development at time of exposure to drug (6) Effects of drugs used in combination LIPID SOLUBILITY Lipophilic drugs → diffuse readily across placenta. Thiopental used for cesarean sections, crosses placenta almost immediately → sedation or apnea in newborn Highly ionized Succinylcholine and Tubocurarine cross placenta slowly → very low concentrations in fetus. Impermeability of placenta to polar compounds is relative rather than absolute. In high enough maternal-fetal concentration gradients → polar compounds cross placenta. MOLECULAR SIZE Molecular weight influences rate and amount of drug transferred. MW of 250-500 → cross placenta easily, depending upon their lipid solubility and degree of ionization. MW of 500-1000 cross more difficulty. MW ˃1000 cross very poorly (Heparin is safe unlike warfarin). Yet placental transporters can carry larger molecules to fetus (maternal antibodies as in Rh incompatibility). PLACENTAL TRANSPORTERS Many drug transporters have been identified in placenta. P-glycoprotein transporter: pumps back into maternal circulation a variety of drugs, including cancer drugs (Vinblastine, Doxorubicin) and viral protease inhibitors (↑risk of vertical HIV infection from mother to fetus). Glyburide is effluxed from the fetal circulation by specific transporters. PROTEIN BINDING (PB) PB may affect rate and amount transferred. Very lipid-soluble (some anesthetic gases) diffuse so rapidly will not be affected greatly by PB → more dependent on placental blood flow Transfer of poorly lipid-soluble and ionized drug is slow and will probably be impeded by its binding to maternal plasma proteins. Differential protein binding is also important: some drugs (sulfonamides, barbiturates, phenytoin, local anesthetic agents) exhibit greater PB in maternal plasma than in fetal plasma because of a lower binding affinity of fetal proteins. PLACENTAL DRUG METABOLISM Placenta plays role both as: A semipermeable barrier A site of metabolism of some drugs: hydroxylation, N-dealkylation, demethylation (Pentobarbital is oxidized). Conversely, some metabolites may be toxic → augment toxicity (Ethanol, Benzpyrenes). FETAL DRUG METABOLISM Drugs enter fetal circulation via umbilical vein. About 40-60% of umbilical venous blood flow enters fetal liver and may be partially metabolized drugs. FETAL DRUG METABOLISM In addition, a large proportion of drug present in umbilical artery (returning to placenta) may be shunted through placenta back to umbilical vein and into the liver again. It should be noted: metabolites of some drugs may be more active than parent compound and may affect fetus adversely. Pharmacodynamics: MATERNAL DRUG ACTIONS Alteration of drugs effects on reproductive tissues (breast, uterus, …) in pregnancy No significantly changes in drug effects on other maternal tissues (heart, lungs, kidneys, CNS, …) Alteration of physiologic context (cardiac output, renal blood flow,…) → requiring the use of new drugs. Cardiac glycosides and diuretics may be needed for heart failure precipitated by ↑cardiac workload of pregnancy Insulin may be required for control of blood glucose in pregnancy-induced diabetes. Pharmacodynamics: THERAPEUTIC DRUG ACTIONS IN FETUS Fetal therapeutics: drug administration to pregnant woman with the fetus as the target of drug Corticosteroids → stimulate fetal lung maturation when preterm birth is expected. Phenobarbital → near term, can induce fetal hepatic enzymes responsible for glucuronidation of bilirubin → ↓incidence of jaundice in newborn Antiarrhythmic drugs → treatment of fetal cardiac arrhythmias Zidovudine →↓transmission of HIV from mother to fetus Pharmacodynamics: PREDICTABLE TOXIC DRUG ACTIONS IN FETUS Chronic use of opioids → dependence in fetus and neonatal withdrawal syndrome after delivery ACEIs during pregnancy → irreversible renal damage in fetus → contraindicated in pregnant women. Delayed Adverse effects: female fetuses exposed to diethylstilbestrol → ↑risk for adenocarcinoma of vagina after puberty. Pharmacodynamics: TERATOGENIC DRUG ACTIONS Teratogen: Thalidomide Tragedy A substance: • 1957 until 1961 1)Results in a malformation, indicating • 10,000 birth defects selectivity for certain target organs; 2) Exerts its effects at a particular stage of fetal development, ie, during limited time period of organogenesis of target organs (thalidomide phocomelia risk occurs during 4-7th weeks of gestation); 3)Show a dose-dependent incidence. Teratogenic mechanisms: 1. Direct effect on maternal tissues with secondary or indirect effects on fetal tissues. 2. Interfere with passage of oxygen or nutrients through placenta and effects on the most rapidly metabolizing tissues of fetus. 3. Important direct actions on processes of differentiation in developing tissues (vitamin A, isotretinoin, etretinate as potent teratogens). Teratogenic mechanisms: 4. Deficiency of a critical substance plays role in some abnormalities (spina bifida in folic acid deficiency). 5. Continued exposure to a teratogen → cumulative effects or affect several organs through varying stages of development. Counselling women about teratogenic risk Ability of appropriate counselling to prevent unnecessary abortions. Up-to-date and evidence-based information should be provided. Woman should understand that baseline teratogenic risk in pregnancy (a neonatal abnormality in the absence of any known teratogenic exposure) is about 3%. It is critical to address maternal-fetal risks of untreated condition if a medication is avoided → serious morbidity in women who discontinued SSRIs for depression in pregnancy. Schematic diagram of critical periods of human development FDA Teratogenic Risk Categories Category Description A No evidence of a risk in the first and late trimesters from controlled studies. B Either animal-reproduction studies have not demonstrated a fetal risk, but there are no controlled studies in pregnant women, or animal-reproduction studies have shown an adverse effect that was not confirmed in controlled studies in women in the first and late trimester. C Studies in animals have revealed adverse effects on fetus (teratogenic or embryocidal,….) and there are no controlled studies in women. Drugs should be given only if the potential benefit justifies the potential risk to fetus. FDA Teratogenic Risk Categories Category Description D There is positive evidence of human fetal risk, but the benefits from use in pregnant women may be acceptable despite the risk (if drug is needed in a life-threatening situation or for a serious disease for which safer drugs cannot be used or are ineffective). X Studies in animals or human beings have demonstrated fetal abnormalities or there is evidence of fetal risk based on human experience or both. The drug is contraindicated in women who are or may become pregnant. Drugs with significant adverse effects on fetus Drug ACE inhibitors (D) Antidepressants tricyclic (C) Anti-neoplastics (B) (D) (X) Barbiturates, Diazepam (C) Trimester Effect All, especially Renal damage second and third Third Neonatal withdrawal symptoms with clomipramine, desipramine, and imipramine All Various congenital malformations; low birth weight All Chronic use can lead to neonatal dependence. Drugs with significant adverse effects on fetus Drug Trimester Effect Carbamazepine(D) First Neural tube defects Ethanol All Risk of fetal alcohol syndrome and alcohol-related neurodevelopmental defects Heroin, Methadone(C) All Chronic use leads to neonatal dependence Iodide All Congenital goiter, hypothyroidism Isotretinoin, Etretinate (X) All Extremely high risk of CNS, face, ear, other malformations Lithium (D) First Ebstein's anomaly Drugs with significant adverse effects on fetus Drug Trimester Effect Propylthiouracil(C) All Hypothyroidism, Congenital goiter Organic solvents First Phenytoin (D) All Streptomycin(D) All Multiple malformations Valproic acid(D) All Neural tube defects, cardiac and limb malformations Warfarin (D) First, Second Third Fetal hydantoin syndrome Eighth nerve toxicity Hypoplastic nasal bridge, CNS malformations Risk of bleeding. Discontinue use 1 month before delivery. Teratogenic Effects Ebstein's anomaly: congenital heart defect in tricuspid valve — the valve between chambers on the right side of heart — and possibly shunt between right and left atria. Teratogenic Effects Fetal alcohol syndrome: a pattern of mental and physical defects Teratogenic Effects Fetal hydantoin syndrome: intrauterine growth restriction with microcephaly and develop minor dysmorphic craniofacial features and limb defects including hypoplastic nails. DRUG USE DURING LACTATION Most drugs are excreted into breast milk in amounts too small (1% of drug) to adversely affect neonatal health. More lipid soluble and more basic drugs →more excreted into milk (milk has lower pH than serum; pH 7) Examples of basic drugs: Antihistamines, Opioids alkaloids, Isoniazid, Imipramine Higher maternal plasma levels (renal insufficiency) → higher breast milk concentrations DRUG USE DURING LACTATION Nursing mother should optimally take relatively safe drug 30-60 minutes after nursing and 3-4 hours before next feeding. Newborn is more susceptible to drugs effects during first weeks. Breast-feeding is contraindicated in cancer chemotherapy, treating with cytotoxic or immune-modulating agents and after large doses radioactive substances. Drugs often used during lactation and possible effects on nursing infant Drug Effect on Infant Comments Possibility of bone marrow suppression; Chloramphenicol Significant recommend not taking in breast-feeding. Diazepam Significant Accumulation and sedation Iodine (radioactive) Significant Thyroid suppression,↑risk of thyroid cancer Milk concentrations equal maternal concentrations. Possibility of pyridoxine deficiency Isoniazid (INH) Minimal Lithium Mother should avoid breast-feeding unless Significant levels can be measured. Propylthiouracil Significant Suppress thyroid function in infant. Drugs often used during lactation and possible effects on nursing infant Drug Effect on Infant Comments Breast-feeding under close physician supervision. Signs of opioid withdrawal in Significant Methadone infant if mother stops taking methadone or stops breast-feeding abruptly. Hypnotic doses cause lethargy, sedation, poor Moderate Phenobarbital suck reflexes in infant. Low maternal doses (5 mg/d) probably safe. Moderate Doses 2 or more times physiologic amounts Prednisone (> 15 mg/d) should probably be avoided. Possibility of permanent staining of Tetracycline Moderate developing teeth in the infant. Should be avoided during lactation.