* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Assessing Visual Quality With the Point Spread Function Using the
Survey
Document related concepts
Transcript
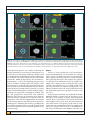
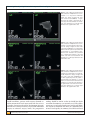
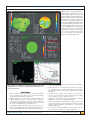
Assessing Visual Quality With the Point Spread Function Using the NIDEK OPD-Scan II Edoardo A. Ligabue, MD; Cristina Giordano, OD ABSTRACT PURPOSE: To present the use of the point spread function (PSF) metric pre- and postoperatively for the assessment of visual quality in cataract and refractive surgery. METHODS: Case examples of cataract and refractive surgery and the effect of accommodation are presented. All PSF measurements were obtained using the NIDEK OPD-Scan II, and corneal internal and total aberrations were simulated using the NIDEK OPD-Station software. All eyes underwent corneal topography, wavefront aberrometry, autorefraction, keratometry, and pupillometry measurements pre- and postoperatively using the OPDScan II. The PSF was used to assess visual quality. RESULTS: Four case examples including refractive surgery, aspheric multifocal intraocular lens (IOL) implantation, toric IOL implantation, and the difference in PSF due to accommodation are presented. CONCLUSIONS: The PSF in refractive and cataract surgery is a clinically valuable metric to evaluate the patient’s visual quality pre- and postoperatively. The OPD-Scan II can measure the effect of accommodation and distant fixation providing an assessment of changes in visual quality. [J Refract Surg. 2009;25:S104-S109.] T he measurement of high-contrast visual acuity is not an adequate representation of the patient’s visual quality. Visual acuity can be described by the following expression1: V • A • = 1/, where represents the minimum angle of resolution. Snellen acuity is a measure of the ability of the eye to resolve details, and the recorded value provides a metric of the functional integrity of the optical system. However, vision is a complex neural process, and the perception of scotopic symptoms such as halos and glare cannot be described by a single value metric. Theoretically, a perfect optical system would focus all incoming light rays into one single point that would not cause halos or glare. In the human eye, however, light is distorted, and this distortion can be measured using wavefront aberrometry.2 The wave theory of light can be used to explain interference and the diffraction primarily responsible for less-than-perfect optics in the human eye that form the basis of the point spread function (PSF).3 For example, when the crest of one light wave meets the crest of another, the crests combine and undergo constructive interference. Waves that combine in this manner are considered in phase. Alternately, when the crest of one light wave meets the trough of another, the light waves cancel and undergo destructive interference. These waves are considered out of phase. Diffraction is defined as “any deviation of light rays from a rectilinear path which cannot be interpreted as reflection or refraction.”2 Diffraction occurs when light waves meet an aperture (eg, the pupil in the eye) or an obstacle (eg, the diffractive steps in a multifocal intraocular lens [IOL]). A small aperture causes greater diffraction compared with a large aperture. In the eye, the pupil serves as the aperture, and optics of the eye determine the wavefront aberrations that can be used to simulate objective visual quality using the PSF.4 From CDI Eye Clinic, Milan, Italy. The authors have no financial interest in the materials presented herein. Correspondence: Edoardo A. Ligabue, MD, CDI Eye Clinic, Corso di Porta Vittoria 5, 20122 Milan, Italy. Tel: 39 248 317260; Fax:39 258 303888; E-mail: [email protected] S104 Commercially Sponsored Section journalofrefractivesurgery.com Assessing Visual Quality With the Point Spread Function/Ligabue & Giordano Geometric optics defines the image of a point source as a point. Physical optics states that light waves from a point source can interfere. Optically, these effects determine the pattern of the PSF. The PSF for a perfect optical system is the Airy Disk that is calculated using Fraunhofer’s approximation.5 The PSF is the image of a point source of light formed on the retina by the eye’s optical system. Every object can be considered a combination of a number of point sources of light. The mathematical process of overlapping all of these points forming an object is called a convolution, from which the PSF is calculated.6 In a normal eye, the PSF is generally dependent on pupils because as the pupil diameter increases, so do the wavefront aberrations that directly affect the PSF. To assess visual quality, the PSF, modulation transfer function (MTF), Strehl ratio, and wavefront maps can be evaluated. The MTF represents perhaps the most intuitive representation of visual quality. Basically, it is picture of how the optics of an eye distorts a point source of light. The MTF represents the visual performance of the eye across the range of spatial frequencies used in daily life. Image quality is improved when the area under the MTF is increased or maximized. The Strehl ratio is the ratio of the peak height of the PSF being measured to the peak height of a perfect optical system. The Strehl ratio range is from 0 to 1. In a normal eye, the Strehl ratio does not reach 1, because diffraction and the optical aberrations limit the visual resolution of the eye. A typical higher order Strehl ratio value for a 5-mm pupil is 0.05. The higher the Strehl ratio, the better the potential image quality. The assessment of visual quality is important because of the introduction of newer IOL and excimer laser technologies that purport to increase visual quality compared with conventional models. In addition, a more informed and more demanding patient base makes it necessary to assess the visual quality preoperatively for treatment planning. We report the use of these image quality metrics in cases of cataract and refractive surgery and assess changes due to accommodation. Clinically, the surgeon will be able to understand image perception and visual disturbances that make the patient symptomatic. CASE 1 Refractive Surgery Screening and Postoperative Changes. A 30-year-old woman presented for LASIK. The right eye is presented as an example. The manifest refraction was 4.25 0.25 164. The OPD-Station evaluation is presented in Figure 1. The Holladay summary displays the total, corneal, and internal wavefront maps of the eye along with the corresponding PSF measurements. All wavefront maps in Figure 1 present the effect of lower and higher order aberrations of the eye. Using the Holladay summary, one can determine whether the corneal or internal components (or a combination) of the eye are detrimental to visual quality. In this case, the total PSF and internal PSF patterns were similar, indicating that the majority of refractive error and visual quality was determined by the internal aberrations of the eye. The wavefront maps show a bull’s eye pattern consistent with myopia. The patient underwent LASIK. The corneal wavefront map did not show significant aberration 3 months postoperatively compared with preoperatively. The postoperative corneal PSF was slightly worse compared with preoperative corneal PSF, likely due to the lamellar cut. Postoperatively, the total eye PSF resembled a point of light indicating successful reduction of refractive error and higher order aberrations. The Strehl ratio for the total wavefront increased from 0 preoperatively to 0.100 postoperatively, indicating an increase in visual quality. PATIENTS AND METHODS The OPD-Scan II with OPD-Station software (NIDEK Co Ltd, Gamagori, Japan) was used in four cases that included toric IOL implantation, preoperative LASIK candidate assessment, aspheric multifocal IOL implantation, and the effect of accommodation on visual quality. The OPD-Scan II measures ocular wavefront, corneal topography, autorefraction, autokeratometry, and pupil- CASE 2 Cataract Screening and Toric IOL Implantation Assessment. A 65-year-old man reporting reduction in vision along with ghosting at night presented for routine assessment. Only the left eye is presented for illustrative purposes. The manifest refraction was 1.50 0.75 15 with 20/30 vision. Slit-lamp examination revealed a cataract in both eyes. Preoperatively, the total and in- Journal of Refractive Surgery Volume 25 January (Suppl) 2009 lometry. All measurements were performed on the same optical axis without moving the instrument or the patient; hence, the corneal and whole eye wavefront data can be directly correlated. The OPD-Station software separates corneal (anterior corneal surface) from the internal aberrations (posterior cornea surface, lenticular, vitreous, and retina) to determine the effect of each optical element in the visual system separately. The PSF, early treatment of diabetic retinopathy study (ETDRS) chart, and MTF can be simulated for the total eye or the lenticular or corneal components of the eye. The OPD-Scan and OPD-Station have been described previously.7-9 CASE REPORTS Commercially Sponsored Section S105 Assessing Visual Quality With the Point Spread Function/Ligabue & Giordano Figure 1. Case 1. A) Pre- and B) postoperative OPD-Station evaluation of a patient who underwent LASIK. Postoperatively, the point spread function (PSF) due to all components (PSF/OPD/Tot) is significantly smaller and less distorted than preoperatively, indicating better uncorrected visual quality. WF/OPD/Tot denotes the higher and lower order aberrations of all components of the eye combined; WF/Corn/Tot denotes the higher and lower order wavefront aberrations of the corneal front surface; and WF/Int/Tot denotes the higher and lower order wavefront aberration of the internal (primarily lenticular) aberrations of the eye. All measurements and simulations were performed for a 4-mm pupil diameter to the eighth Zernike order. ternal aberration patterns were similar, indicating the internal aberrations were causing the reduction in visual acuity (Fig 2A). The patient underwent SN60T3 24.00 D AcrySof toric IOL implantation (Alcon Laboratories Inc, Ft Worth, Tex). Figure 2B presents the OPD-Station evaluation 1 month postoperatively. The wavefront refraction shows 0.50 D of astigmatism postoperatively with an excellent wavefront total PSF despite a total wavefront error 0.800 µm. The discrepancy between the wavefront error and PSF highlights the fact that one metric or one map cannot suffice in clinical assessment using wavefront aberrometry and that multiple indices and maps are required for a thorough assessment. The pre- and postoperative corneal PSF were somewhat different, likely because of placement of the incision. The internal total wavefront was reduced to half the preoperative value after IOL implantation. The internal wavefront map showed a band of little to no optical distortion (green), indicating that the IOL is positioned on axis without significant tilt (see Fig 2B). Significant tilt and IOL decentration lead to coma-like patterns in the wavefront maps. S106 Commercially Sponsored Section CASE 3 Changes in Visual Quality Due to Accommodation. During accommodation, the crystalline lens changes shape so that it is thicker centrally than peripherally. This peripheral flattening increases negative longitudinal spherical aberration.1 This changes the asphericity and high order aberrations of the crystalline lens, which cause a change in the visual quality (Fig 3). For example, measurement of a 24-year-old patient looking at distance then near induces a myopic shift, a significant distortion in the PSF, and a 10-fold decrease in the Strehl ratio from 0.022 at distance to 0.002 at near (see Fig 3). During cataract formation, the amplitude of accommodation declines, causing little or no change in the PSF (Fig 4). For example, a patient with an incipient cataract shows little change in the PSF or Strehl ratio when looking at distance or near. The measurement of near and distance visual quality can be used to evaluate the effect of accommodative IOLs. For example, the PSF of this patient who received an accommodative IOL shows no difference when looking at distance verjournalofrefractivesurgery.com Assessing Visual Quality With the Point Spread Function/Ligabue & Giordano Figure 2. Case 2. A) Pre- and B) postoperative OPD-Station evaluation of a patient who underwent toric IOL implantation. Postoperatively, the point spread function (PSF) due to all components (PSF/OPD/Tot) is significantly smaller and less distorted than preoperatively, indicating better uncorrected visual quality. Postoperatively, the internal PSF also became significantly smaller and less distorted. WF/OPD/Tot denotes the higher and lower order aberrations of all components of the eye combined; WF/Corn/Tot denotes the higher and lower order wavefront aberrations of the corneal front surface; and WF/Int/Tot denotes the higher and lower order wavefront aberration of the internal (primarily lenticular) aberrations of the eye. All measurements and simulations were performed for a 4.8-mm pupil diameter to the eighth Zernike order. sus near, indicating that the IOL remains stable when presented with a near stimulus (Fig 5). CASE 4 Aspheric IOL Implantation. Figure 6 presents OPDScan II evaluation of a patient who underwent implantation of an aspheric AcrySof ReStor IOL (Alcon Laboratories Inc) in which some residual positive spherical aberration was targeted in the right eye. Postoperatively, the ocular spherical aberration was 0.188 µm at 5.8 mm of pupil, and corneal spherical aberration remained unchanged at 0.368 µm at 5.8 mm of pupil. The PSF showed some glare, likely due to a combination of the residual astigmatism optics of the IOL. The A/B ratio on the MTF graph was 50.3%, indicating the visual performance of the patient’s eyes without correction compared with a pair of emmetropic eyes with excellent visual acuity and contrast sensitivity. The H/B ratio was 62.4%; this ratio indicates the best corrected visual performance of the patient’s eyes compared Journal of Refractive Surgery Volume 25 January (Suppl) 2009 with the emmetropic eyes. Based on this result, only a 12% increase in visual performance will be achieved by eliminating the residual refractive error (primarily astigmatism). This small increase did not warrant an IOL exchange procedure. The patient remained asymptomatic and was satisfied with the unaided distance and near vision 6 months postoperatively. DISCUSSION Visual quality simulations and metrics represent an indication of the success of corneal refractive and cataract surgeries. Wavefront aberrometry allows the surgeon to plan the procedure and determine whether the origin of visual symptoms is optical. For example, aspheric IOLs could be selected on the basis of corneal spherical aberration values provided in the OPD-Station. The surgeon could select the IOL that leaves the patient with a slight residual spherical aberration for depth of focus or completely negate the spherical aberration depending on the patient’s requirements. As with Commercially Sponsored Section S107 Assessing Visual Quality With the Point Spread Function/Ligabue & Giordano Figure 3. Case 3. A) Point spread function (PSF) at distance and B) PSF due to accommodation of a 24-year-old emmetropic patient. The change in higher and lower order ocular PSF (PSF/OPD/Tot) is significant when the patient is presented with a near target. All measurements and simulations were performed for a 5.8-mm pupil diameter to the eighth Zernike order. Figure 4. Case 3. A) Point spread function (PSF) at distance and B) PSF due to accommodation of a patient with an incipient cataract. The change in higher and lower order ocular PSF (PSF/OPD/Tot) is not significantly different when the patient is presented with a near stimulus of 3.00 D. Distance measurement and simulation were performed for a 2.9-mm pupil diameter to the sixth Zernike order and near measurement and simulation for a 4-mm pupil diameter to the sixth Zernike order. Figure 5. Case 3. A) Point spread function (PSF) at distance and B) PSF due to accommodation for a patient with an accommodative IOL implant. The changes in higher and lower order ocular PSF (PSF/OPD/Tot) do not differ significantly when the patient is presented with a near stimulus of 3.00 D. Distance measurement and simulation were performed for a 5.6-mm pupil diameter to the eighth Zernike order and near measurement and simulation for a 5.8-mm pupil diameter to the eighth Zernike order. LASIK candidates, patients with cataracts demand excellent uncorrected visual acuity with little loss of visual quality. Patient needs and the development of premium IOLs have changed cataract surgery from functional surgery to refractive surgery; hence, the preoperative S108 Commercially Sponsored Section workup should be similar to that for LASIK for which wavefront aberrometers are routinely used. The ability to measure visual quality both at near and far will allow the surgeon to determine the effects of a multifocal IOL on near visual quality. In summary, the OPD-Scan II and journalofrefractivesurgery.com Assessing Visual Quality With the Point Spread Function/Ligabue & Giordano Figure 6. Case 4. Postoperative OPD-Scan II measurement of a patient who received a multifocal aspheric IOL. Axial denotes axial corneal topography (top left); OPD map (top right) is a refractive wavefront map plotting the distribution of refractive power across the pupil due to all wavefront aberrations of the eye. The WF/OPD/Gp map (middle) plots the longitudinal spherical aberration of the eye, the PSF/OPD/Tot plots the PSF of the eye. The MFT/OPD/Tot plots the modulation transfer function of the eye. The corneal and ocular spherical aberration is shown in the red circle. All measurements and simulations were performed for a 5.9-mm pupil diameter to the eighth Zernike order. OPD-Station are important instruments for the pre- and postoperative assessment of point spread function in a variety of patients. REFERENCES 4. Diffraction. Available at: http://en.wikipedia.org/wiki/Diffraction. Accessed June 2008. 5. Ligabue E, Giglio S, Ort AA, Giordano C. Objective and subjective evaluations in vision quality after diffractive IOLs implant. Presented at: Refractive Surgery online; September 14-17, 2006; Milan, Italy. 1. Visual acuity and contrast sensitivity. In: Bennett AG, Rabbetts RB, eds. Clinical Visual Optics. 3rd ed. Oxford, United Kingdom: Butterworth Heinemann; 1998:21-57. 6. Giordano C. PSF e qualità visiva: La diagnostica del segmento anteriore. Presented at: 88° Congresso Nazionale Società Oftalmologica Italiano; April 18, 2008; Rome, Italy. 2. Williams DR, Porter J, Yoon G, Guirao A, Hofer H, Chen L, Cox I, MacRae SM. How far can we extend the limits of human vision? In: Krueger RR, Applegate RA, Macrae SM, eds. Wavefront Customized Visual Correction: The Quest for Super Vision II. Thorofare, NJ: SLACK Incorporated; 2004:19-38. 7. MacRae S, Fujieda M. Slit skiascopic-guided ablation using the NIDEK laser. J Refract Surg. 2000;16:S576-S580. 3. Freeman MH, Hull CC. The nature of light sources and detectors. In: Bennett AG, Rabbetts RB, eds. Clinical Visual Optics. 11th ed. Oxford, United Kingdom: Butterworth Heinemann; 2003:304. Journal of Refractive Surgery Volume 25 January (Suppl) 2009 8. Gatinel D, Hoang-Xuan T. Measurement of combined corneal, internal, and total ocular optical quality analysis in anterior segment pathology with the OPD-scan and OPD-station. J Refract Surg. 2006;22:S1014-S1020. 9. Klyce SD, Karon MD, Smolek MK. Screening patients with the corneal navigator. J Refract Surg. 2005;21:S617-S622. Commercially Sponsored Section S109