* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Drug allergy
Survey
Document related concepts
Transcript
DRUG ALLERGY:
MAKING SAFE TREATMENT
DECISION
William Chui
Chief of Pharmacy Service, HKW Cluster
1
2
Adverse Drug Reaction
Adverse drug reactions are classified as
predictable or unpredictable.
A predictable drug reaction is related to the
pharmacological actions of the drug.
An unpredictable reaction is related to
immunological response ( hypersensitivity
reactions ) or nonimmunological response
3
Adverse Drug Reactions
Drug Hypersensitivity
Drug Allergy
Drug Intolerance
4
Definition of drug allergy
It is defined as an adverse reaction to
a drug by a specific immune response
either directly to the drug or one or
more of its metabolites alone, or to a
drug bound to a body protein such as
albumin, (Hapten).
Such binding alters the structure of
the drug/protein complex, rendering it
antigenic.
5
Distinctive features of
allergic drug reactions
No correlation with known
pharmacological properties of the drug
No linear relationship with drug
dosage
Often include a rash, angioedema, the
serum sickness syndrome, anaphylaxis
and asthma which are reactions similar
to those of classical protein allergy
6
Distinctive features of
allergic drug reactions
Require an induction period on primary
exposure but not on readministration
Disappear on cessation of therapy and
reappear after readministration of a small
dose
Occur in a minority of persons receiving the
drug
Desensitization may be possible
7
Classification of
hypersensitivity
The criteria of the classification
1) Based on the time required for the
symptoms or skin test reactions to
appear after exposure--- immediate
and delayed hypersensitivity.
2) Based on the nature of organ
involvement.
•Fewer than 10 percent of adverse drug reactions are allergic.
8
Hypersensitivity Reactions
I (immediate)
II (cytotoxic)
III (immune
complex)
IV (delayed)
V
(stimulating/blocking)
#
Antigens
Pollens, moulds,
mites, drugs, food
and parasites
Cell surface or tissue
bound
Exogenous
(viruses,
bacteria,
fungi,
parasites)
Autoantigens
Cell/tissue
bound
Cell surface receptors
Mediators
IgE and mast cells
IgG, IgM and
complement
IgG, IgM, IgA
and
complement
TD, Tc activated
macrophages
and
lymphokines
IgG
Diagnostic
tests
Skin-prick tests:
wheal and flare
Specific IgE in
serum
Coombs’ test
Indirect
immunofluorescence
(antibodies)
Red cell agglutination
Precipitating
antibodies
ELISA
Immune
complexes
Skin test:
erythema
induration (e.g.
tuberculin test)
Indirect
Immunofluorescence
Time taken for
reaction to
develop
5-10min
6-36 hours
4-12 hours
48-72 hours
Variable
#Type V hypersensitivity may also be classified with type II reactions
9
I (immediate)
II (cytotoxic)
III (immune complex)
IV (delayed)
V
(stimulating/blocking)
Immunopathology
Oedema, vasodilation,
mast cell
degranulation,
eosiniophils
Antibody-mediated
damage to target
cells
Acute inflammatory
reaction, neutrophils,
vasculitis
Perivascular
inflammation,
mononuclear cells,
fibrin
Granulomas
Caseation and
necrosis in TB
Hypertrophy or
normal
Diseases and
conditions produced
Asthma (extrinsic)
Urticaria/oedema
Allergic rhinitis
Anaphylaxis
Autoimmune
Haemolytic anaemia
Transfusion reactions
Haemolytic disease of
newborn
Goodpasture’s
syndrome
Addisonian pernicious
anaemia
Myasthenia gravis
Autoimmune (e.g.
SLE,
glomerulonephritis,
rheumatoid arthritis)
Low-grade persistent
infections (e.g. viral
hepatitis)
Disease caused by
environmental
antigens (e.g.
farmer’s lung)
Pulmonary TB
Contact dermatitis
Graft-versus-host
disease
Insect bites
Leprosy
Neonatal
hyperthyroidism
Graves’ disease
Myasthenia gravis
Treatment
Antigen avoidance
Antihistamines
Corticosteroids
(usually topical)
Sodium cromoglicate
Epinephrine for lifethreatening
conditions
Exchange transfusion
Plasmapheresis
Immunosuppressives
/cytotoxics
Corticosteroids
Immunosuppressives
Plasmapheresis
Immunosuppressives
Corticosteroids
Removal of antigen
Treatment of
individual disease
RAST, radioallergosorbent test; SLE, systemic lupus erythematosus; TB, tuberculosis;
Tc, T cytotoxic; TD, T delayed hypersensitivity
10
Overview of Drug Allergy
Drug allergy is an uncommon and
unwanted side effect of medication.
Reactions to drugs range from a mild
localized rash to serious effects on
vital systems.
The body’s response can affect many
organ systems, but the skin is the
most frequently involved.
17
The most common drug to
cause allergy
Analgesics, such as codeine, morphine,
nonsteroidal anti-inflammatory drugs
(NSAIDs, such as ibuprofen or
indomethacin), and aspirin
Antibiotics such as penicillin, sulfa drugs,
and tetracycline
18
Risk factors for Drug Allergy
Frequent exposure to the drug
Large doses of the drug
Drug given by injection rather than pill
Family tendency to develop allergies
and asthma.
19
Drug Allergy Symptoms
Drug allergies may cause many
different types of symptoms
It depends on the drug and how often
you have taken it.
20
Most common allergic reactions
Rash
Fever
Muscle and joint aches
Lymph node swelling
Inflammation of the kidney
Anaphylactic shock
21
Allergic reactions on skin
Measles-like rash
Hives - Slightly red and raised swellings on
the skin, irregular in shape, itchy
Photoallergy - Sensitivity to sunlight, an
itchy and scaly rash when you go out in the
sun
Erythema multiforme - Red, raised and itchy,
sometimes look like bull's-eye targets,
sometimes with swelling of the face or
tongue
24
Allergic reactions on skin
Stevens-Johnson Syndrome (SJS) and
Toxic Epidermal Necrolysis (TEN)
-A manifestation of acute graft versus
host disease
-Medications with longer half-lives are
more likely than those with shorter
half-lives to pose a risk for SJS and
TEN
25
Stevens Johnson’s syndrome
26
Toxic epidermal necrosis
28
SJS & TEN
SJS & TEN develop 1-3 weeks after
the culprit medication is initiated
Sulphonamides, other antibiotics,
NSAIDs, anticonvulsant and
antiretroviral agents are the most
common causative medications.
29
Signs and Symptoms of SJS & TEN
Mucosal erosions
Asymmetric skin
involvement with
blisters
Widespread of skin
distribution
<10% total body
surface area
affected
Mucosal erosions
Flaccid blisters and
denuded skin
Widespread of skin
distribution
> 30% total body
surface area
affected
30
Signs and Symptoms of SJS & TEN
Fluid and electrolyte imbalance
Compromised cutaneous integrity promotes
bacterial colonization and infection of the
skin with the risk for sepsis.
Debilitated, bedridden patients are
susceptible to aspiration pneumonia, deep
vein thrombosis and pulmonary embolism
Ocular involvement may manifest to
blindness
31
Guideline for Treatment of SJS & TEN
Admit to intensive care or burn unit
Discontinue culprit medication and all
unnecessary medications
Sterile technique in handling patient
Place intravenous or central line in
area of uninvolved skin if possible
32
Guideline for Treatment of SJS & TEN
Culture skin, blood, urine daily
Avoid prophylactic systemic antibiotics
and silver sulfadiazine to skin
Fluid and electrolyte monitoring and
replacement
Initiate total parenteral nutrition or
nasogastric feedings if unable to take
po
33
Guideline for Treatment of SJS &TEN
Remove oral and nasal debris daily;
antiseptic mouthwashes or oral sprays
daily
Antiseptic eye drops daily and
ophthalmology consultation
Anticoagulation to prevent deep vein
thrombosis and pulmonary embolism
35
Anaphylactic Reaction
Life threatening
Almost all anaphylactic reactions occur
within 4 hours of the first dose of the
drug. Most occur within 1 hour of
taking the drug, and many occur
within minutes or even seconds.
36
Symptoms of anaphylactic shock
Skin reaction - Hives, redness/flushing,
sense of warmth, itching
Difficulty breathing - Chest tightness,
wheezing, throat tightness
Fainting - Light-headness or loss of
consciousness due to drastic decrease in blood
pressure ("shock")
Rapid or irregular heart beat
Swelling of face, tongue, lips, throat, joints,
hands, or feet
37
The causative antigens causing anaphylaxis
Blood products
ß-lactam antibiotics
X-ray contrast agent
Other drugs
38
Prophylaxis of anaphylaxis
Routine skin testing before giving serum is
mandatory.
When a drug or serum is essential, rapid
desensitization.
For x-ray contrast agent anaphylaxis, the
patient is pretreated with prednisolone
50mg q 6h for 3 doses, diphenhydramine
50mg po 1h beforehand and adrenaline 25
mg po 1h beforehand for adult.
46
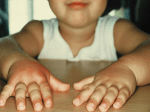
Urticaria
What is urticaria?
It is local wheals and erythema in the
superficial dermis
Urticaria induced by drug is generally
acute and is limited to the skin and
subcutaneous tissues.
48
Urticaria
49
Urticaria
Signs and symptoms
Pruritus (generally the first symptom)
Crops of hives
Lesion (if lesion persists more than 24
hours, the possibility of vasculitis
should be considered)
Diagnostic tests are seldom required
50
Urticaria
Treatment for acute urticaria
Symptoms subside in 1 to 7 days,
treatment is chiefly palliative.
All nonessential drugs should be
stopped until the reaction has
subsided.
Symptoms can be relieved by oral
antihistamine and glucocorticoid.
51
Drugs for Acute Urticaria
Oral antihistamine: diphenhydramine
50-100mg q4h, hydroxyzine 25-100mg
bid or cyproheptadine 4-8mg q4h
Glucocorticoid for more severe
reactions, especially when associated
with angioedema (prednisone 30-40
mg/ day po)
52
Angioedema
What is angioedema?
It is a deeper swelling due to
edematous areas in the deep dermis
and subcutaneous tissue and may also
involve mucous membranes.
55
Signs & Symptoms of Angioedema
Diffuse and painful swelling of loose
subcutaneous tissue, dorsum of hands
or feet, eyelids, lips, genitalia and
mucous membranes.
Edema of the upper airways may
produce respiratory distress
56
Angioedema
57
Management for Angioedema
Glucocorticoid (e.g. prednisone 3040mg/day po)
Adrenaline 1:1000, 0.3ml subcutaneously
should be the 1st line treatment for acute
pharyngeal or laryngeal angioedema
IV antihistamine (e.g. diphenhydramine 50100mg) to prevent airway obstruction
Intubations or tracheotomy and oxygen
administration may be necessary
58
Example of Drug Allergy
59
Penicillin Allergy
Symptoms
Fever
Rash
Urticaria
Angioedema
Nephritis
Lymphadenopathy
Arthralgias
60
Immunological reactions resulting in
signs and symptoms
Type I : immediate hypersensitivity
Antigens with specific IgE antibodies that
are bound to mast cells or basophils and
lead to the release of histamine and
leukotrienes.
Clinical presentation : urticaria, laryngeal,
edema, bronchospasm, hypotension and
cardiovascular collapse, anaphylaxis.
61
Immunological reactions resulting
in signs and symptoms
Type II : Cytotoxic reaction
Cytotoxic reactions result when IgG or IgM
β-lactam specific antibodies become
attached to circulating blood cells or renal
interstitial cells which have β-lactam
antigens bound to their surface.
Clinical presentation: hemolytic anemia,
thrombocytopenia, granulocytopenia or
drug-induced nephritis.
62
Immunological reactions resulting
in signs and symptoms
Type III :immune complex reactions
β-lactam specific IgG or IgM antibodies may
form circulating complexes with β-lactam
antigens. These complexes causing serum
sickness like reaction and possibly drug
fever.
Clinical presentation: fever, rash, urticaria,
lymphadenopathy and arthralgias
63
Immunological reactions resulting
in signs and symptoms
Type IV: cell-mediated hypersensitivity
T lymphocytes recognize the β-lactam
antigen through an antigen-specific Tcell receptor, triggering cytokine
release, resulting in tissue
inflammation.
Clinical presentation: contact dermatitis.
64
Mechanism of Penicillin Allergy
Only proteins and large polypeptide
drugs can stimulate specific antibody
production by straightforward
immunologic mechanisms.
The drug, or one of its metabolites
must be chemically reactive with
protein can act as haptens and bond
covalently to proteins.
65
Mechanism of Penicillin Allergy
The breakdown products can bond to
ε-amino groups of lysine residues,
most importantly globulins.
This binding leads to a spectrum of
potentially immunologically active
moieties on serum proteins that can
cross-link with a variety of preformed
anti-penicillin IgE bond to mast cells.
66
Cross-reactivity
The most important part of penicillin
antigen appears to be the core
structure
The structure of the penicillin is a βlactam ring with the five-membered
thiazolidine ring
67
The structure of Penicillin
68
Cross-reactivity
Carbapenems have a bicyclic nucleus
containing β-lactam ring and an adjacent
five-membered ring.
It showed 50% cross-reactivity in allergy
skin testing between penicillin major and
minor determinants and the analogous
imipenem reagents.
Patients especially with positive penicillin
skin test should withhold carbapenems
69
The Structure of Carbapenem
70
Cross-reactivity
The structure of cephalosporin contains a βlactam ring with a six-membered
dihydrothiazine ring.
Side chain antigens may be more significant
and probably dominate in cephalosporin
(patients with positive penicillin skin test
results who were given cephalosporin had a
cross reaction rate of 10%-20%)
71
72
Prophylaxis of Penicillin Allergy
Skin test
Skin tests for immediate-type (IgE-mediated)
hypersensitivity are very useful in diagnosis of
reactions to penicillin, enzymes, and some
vaccines.
74
Prophylaxis of Penicillin Allergy
Skin test
It should be performed in patients
With a history of penicillin allergy
β-lactam antibiotic is indicated drug
of choice.
75
Prophylaxis of Penicillin Allergy
Skin test
The major degradation product of
penicillin, benzylpenicillenic acid, can
combine with tissue proteins to form
benzylpenicilloyl ( BPO ), the major
antigenic determinant of penicillin.
76
Prophylaxis of Penicillin Allergy
If the patient has a history of a severe
explosive reaction, the reagents
should be diluted 100-fold for initial
testing.
78
Prophylaxis of Penicillin Allergy
Intradermal test
0.5 or 1 ml dilute is injected to
produce a 1 or 2 mm bled.
Each set of skin tests should include
the diluents alone as a negative
control and histamine as a positive
control.
79
Intradermal Test
80
Prophylaxis of Penicillin Allergy
Intradermal test
A skin test is considered positive if it
produces a wheal and flare reaction in
15 min with a wheal diameter at least
5 mm larger than the control.
81
Prophylaxis of Penicillin Allergy
If skin tests are positive, the patient
risks an anaphylactic reaction if
treated with penicillin
Negative skin tests minimize but do
not exclude the risk of a serious
reaction.
82
Caution with the skin test
Antihistamines, tricycle antidepressants and
adrenergic drugs can inhibit skin tests
results and should be discontinued before
the testing procedure.
Patients using β-adrenergic blocking drugs
or angiotensin-converting enzyme inhibitors
at the same time of skin testing may not
respond to emergency treatment with
adrenaline if a systemic reaction occurs.
84
When will desensitization perform?
When penicillin is the drug of choice.
The alternate drugs fail, induce
unacceptable side effects or are less
effective.
When anaphylaxis of the penicillin
present
85
Contraindication of Desensitization
Patients with a history of StevensJohnson syndrome and toxic epidermal
necrolysis present an almost absolute
contraindication to the
readministration of any β-lactam
antibiotic since an accelerated lifethreatening reaction may occur.
86
Procedure of desensitization
Baseline evaluation
Intravenous access,
electrocardiogram, spirometry, blood
pressure, pulse, respiratory rate and
clinical status should be reevaluated
prior to the next dose.
87
Procedure of desensitization
Premedication with antihistamine or
steroids is not recommended
1) They are not effective in preventing
severe reactions and may mask early
signs of reaction that would otherwise
result in a modification of the protocol
88
Procedure of desensitization
Dose that causes mild systemic reactions,
such as pruritus, urticaria, rhinitis or mild
wheezing should be repeated until the
patient tolerates the dose without systemic
symptoms or signs.
More serious reactions, such as hypotension,
laryngeal edema, asthma and if
desensitization is continued, withheld until
the patient is stable.
89
Procedure of desensitization
Once desensitized, the patient’s
treatment with penicillin should not
lapse because the risk of an allergic
reaction increases when restarting
treatment.
If the patient requires β-lactam
antibiotic in the future and his skin
test result remains positive,
desensitization is required again.
90
The protocol of desensitization
91
Latex allergy
Latex is derived from natural rubber,
which is itself composed of various
polymers of isoprene.
The potential contamination of
medications and the fact that latexallergic reactions in some situations
could be mistakenly interpreted as
medication allergies or allergic
reactions to general anesthesia.
96
100
101
Conclusion
As drug allergy can pose risk to
patients’ health,
Healthcare professions should…
Be aware of patients’ drug allergy
history
Record such information properly
Double check patients’ drug allergy
history before drug administration
102
Thank You
103