* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Rare Neurovascular Variants Arising from the Internal Carotid Artery
Survey
Document related concepts
Transcript
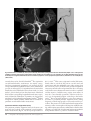
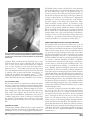
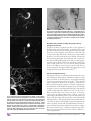
EXTRACRANIAL VASCULAR CME ABBREVIATIONS KEY Rare Neurovascular Variants Arising from the Internal Carotid Artery M. Gajjar, A.R. Honarmand, B.M. Patel, M.C. Hurley, A. Shaibani, and S.A. Ansari AChA ⫽ anterior choroidal artery CCA ⫽ common carotid artery CT ⫽ computed tomography DSA ⫽ digital subtraction angiography ECA ⫽ external carotid artery ICA ⫽ internal carotid artery MRA ⫽ magnetic resonance angiography PCA ⫽ posterior cerebral artery PCoA ⫽ posterior communicating artery Received October 13, 2013; accepted April 15, 2015. CME Credit The American Society of Neuroradiology (ASNR) is accredited by the Accreditation Council for Continuing Medical Education (ACCME) to provide continuing medical education for physicians. The ASNR designates this enduring material for a maximum of one AMA PRA Category one creditTM. Physicians should claim only the credit commensurate with the extent of their participation in the activity. To obtain credit for this activity, an online quiz must be successfully completed and submitted. ASNR members may access this quiz at no charge by logging on to eCME at http://members.asnr.org. Nonmembers may pay a small fee to access the quiz and obtain credit via http://members.asnr.org/ecme. ABSTRACT We reviewed rare cervical and intracranial ICA anatomic variants, aberrant ECA origins; aberrant or aplastic ICAs; CCA absence; persistent proatlantal, stapedial, hypoglossal, and trigeminal arteries; primitive maxillary and mandibular arteries; and duplicated posterior communicating arteries, including a persistent primitive fetal branch or hyperplastic anterior choroidal artery, infraoptic anterior cerebral artery, and dorsal-ventral ophthalmic arteries. Variants of the ICA are rare, typically asymptomatic, and incidental findings. However, these variants can occasionally influence surgical or endovascular strategies, temporary occlusion times, inadvertent embolization risk, and collateral pathways, with a potential impact on procedural complications and patient outcomes. From the Northwestern University Feinberg School of Medicine, Chicago, Illinois. Presentation at American Society of Neuroradiology Annual Meeting, San Diego, CA, May 18-23, 2013. Please address correspondence to Sameer A. Ansari, MD, PhD, Departments of Radiology, Neurology, and Neurological Surgery, Northwestern University Feinberg School of Medicine, 676 N. St. Clair Street, Suite 800, Chicago, IL 60611-2927; e-mail: [email protected] http://dx.doi.org/10.3174/ng.4160164 Learning Objective: Review anatomic variations of the internal carotid artery (ICA), including imaging appearances, embryologic development, prevalence, and associations of clinically relevant variants with neurovascular pathology. INTRODUCTION The development of the primitive carotid artery appears by the third or fourth week of gestation, from which all major intracranial branches arise at 7.5 weeks of gestation. The internal carotid artery (ICA) can be identified at Padget stage 1 of brain vascular development (28 –29 day) in which both the hindbrain and forebrain are supplied by primitive carotid arteries. The primitive ICA connects to the contralateral ICA posterior to the Rathke pouch after dividing into anterior (olfactory, rostral) and posterior (mesencephalic, caudal) branches. The early anterior cerebral artery will develop from an olfactory branch, and the middle cerebral artery (MCA) will arise as a lateral branch of the anterior cerebral artery. Two branches from the proximal ICA and 2 branches from the primitive aorta will supply the hindbrain by connecting to the longitudinal neural arteries, and are named according to the accompanying nerves: trigeminal and otic branches from the proximal ICA, and hypoglossal and proatlantal branches from the primitive aorta.1 At the time of the developing diencephalon and mesencephalon, the posterior communicating artery (PCoA) extends as the primary caudal division (caudal ramus) of the distal primitive ICA (which terminates as the primitive mesencephalic branches). It connects the carotid and vertebrobasilar systems and is the major supply for the deep white matter (diencephalic Neurographics 2016 July/August; 6(4):237–246; www.neurographics.org 兩 237 and some mesencephalic territories) via multiple thalamotuberal penetrating arteries. The PCoA connects to the P1 segment of the posterior cerebral artery (PCA), which is the terminal branch of the basilar artery (formed by midline fusion of longitudinal neural arteries) and supplies the occipital and posteromedial temporal lobes. The anterior choroidal artery (AChA) arises from the rostral division of primitive ICA that supplies the posteromedial hemispheric territory.2 As the gestational age increases, a posterior choroidal artery develops from the caudal division and takes over the supply to this region. At age 35 days of gestation, 2 primitive ophthalmic arteries are recognizable: a ventral ophthalmic artery, which arises from the anterior cerebral artery, and the dorsal ophthalmic artery, which originates from the ICA carotid siphon with subsequent intraorbital and intradural anastomoses, respectively. The ophthalmic artery forms after regression of the proximal parts of the dorsal and ventral ophthalmic arteries.3 The purpose of this review article was to explore anatomic variations along the ICA and highlight unusual configurations that might be encountered when performing a conventional cervical-cerebral angiogram or interpreting CTA-MRA imaging. The angiographic appearances, embryologic development, prevalence, and associations of these clinically relevant variants with neurovascular pathology are discussed. DEVELOPMENTAL AND PRIMITIVE EMBRYOLOGIC ICA ANOMALIES ICA Agenesis and Aplastic ICA Congenital absence of the ICA has a prevalence of 0.01% and is secondary to the failure in development of the primordial ICA from the third aortic arch and dorsal aorta before 24 days of embryogenesis.4 A CT of the skull base and CTA in such cases demonstrate an absence or hypoplasia of the carotid canal and the ICA.5 The anomaly may be unilateral or, more rarely, bilateral, and has been described in association with PHACES (Posterior fossa malformations– hemangiomas–arterial anomalies– cardiac defectseye abnormalities–sternal cleft and supraumbilical raphe syndrome) and congenital Horner syndrome.4,6 Fig 1. CCA absence. Three-dimensional CTA reconstruction depicts the absence of the right CCA, with separate ICA and ECA origins arising directly from the brachiocephalic trunk (white arrows). the brachiocephalic artery proximal to the ECA. In the absence of the left CCA, the aortic arch gives rise to both the ECA and the ICA.9 The ductus caroticus (a segment of the embryonic dorsal aorta connecting the third and fourth aortic arches that normally regress) provid the origin to the primitive CCA during developmental stage IV.1 Either a persistent ductus caroticus with concurrent regression of the third aortic arch or the persistent third aortic arch with concurrent regression of the fourth aortic arches have been proposed as the embryologic abnormalities that lead to the absence of the CCA.10,11 Persistence of the ductus caroticus also has been proposed as a congenital mechanism for low or early carotid bifurcation. Intrathoracic carotid bifurcations have been described in association with the Klippel-Feil anomaly.12 In addition, we previously described a very unusual anomaly of the left ICA, which arises directly from the pulmonary artery. The embryologic mechanism was postulated to be secondary to impaired regression of the primitive aortic arch (Fig 2).13 Aberrant ICA Congenital Common Carotid Artery Absence and Early ICA Bifurcation or Aberrant Origin The exact incidence of common carotid artery (CCA) agenesis is not well described; however, ⬍35 cases of the absence of CCA have been reported in the literature to date (Fig 1).7 Unilateral and bilateral agenesis of CCA has been described.7,8 They are usually asymptomatic and incidentally detected during the evaluation for other conditions or at autopsies. In the absence of the right CCA, in most cases, the external carotid artery (ECA) originates from the brachiocephalic artery proximal to the ICA, which arises from the distal subclavian artery. However, in an unusual case described by Maybody et al,9 the right ICA originated from 238 兩 Neurographics 2016 July/August; 6(4):237–246; www.neurographics.org Recognized aberrant ICAs include intratympanic and retropharyngeal variants. The normal ICA anatomy of the carotid canal is characterized by entry into the petrous bone medial to the styloid process. The initial vertical petrous segment of the ICA courses anterior to the tympanic cavity, adjacent to the middle ear cavity, and is covered by a thin bony plate, which is absorbed in adulthood (Fig 3). An unusual course of the ICA directly toward the middle ear is exceedingly rare and is termed an “aberrant ICA.” This anomaly may be secondary to disturbed differentiation of the third branchial artery, which results in an enlarged inferior tympanic artery (branch of the ascending pharyngeal artery) that enters the tympanic cavity via the inferior tym- inferolateral trunk and as a branch of the meningohypophyseal trunk.1 The posterior inferior hypophyseal artery gives rise to the medial clival artery and its branches, which then go on to anastomose with the contralateral posterior inferior hypophyseal artery. These transclival anastomoses provide a collateral or developmental route to the contralateral ICA in a setting of ICA occlusion. Alternatively, persistent primitive maxillary artery supply to the ICA may become a dominant pathway as an intercarotid anastomosis in cases of embryologic ICA agenesis at or below the petrous segment. Primitive Mandibular Artery Fig 2. Aberrant ICA origin via the pulmonary artery. Aberrant aortic arch anatomy demonstrates the origin of the enlarged left ECA (LECA) that overlaps the right CCA (RCCA) origin (white arrowhead), pigtail catheter (black arrow) in the ascending aorta, aberrant right subclavian artery (asterisk) that supplies the right vertebral artery (RVERT), and the normal left subclavian artery (LSUB). Delayed imaging demonstrates retrograde filling of the left ICA (LICA) from the carotid bifurcation down to an unusual left pulmonary artery origin (black arrowhead). Contrast opacification and washout into the left pulmonary artery (double arrowheads) due to its low-pressure venous system, which results in a functional arteriovenous shunt (with permission from Hurley et al, J Neurosurg Pediatr 200813). panic canaliculus (Jacobsen canal) and develops a persistent anastomosis to the distal horizontal petrous segment of the ICA via the caroticotympanic branch (hyostapedial remnant). Preoperative recognition of an aberrant intratympanic ICA is essential to avoid potentially serious complications during otologic surgery.14 Accidental injury may result in uncontrollable intratympanic hemorrhage and require surgical occlusion and risk for anterior circulation ischemia. This intratympanic variant, as with a persistent stapedial artery, may mimic a hypervascular tumor, such as a glomus tympanicum. The rare retropharyngeal variant of an aberrant ICA is an anomalous course of the distal cervical segment that extends to or near the midline of the posterior pharyngeal wall, which lies beneath the mucosa.15 Its presence places a patient at higher surgical risk for carotid injury during traumatic intubation, oropharyngeal tumor resection, tonsillectomy, adenoidectomy, or palatopharyngoplasty. The etiology has been assumed to be secondary to the disturbance in the descent process of the heart and large vessels, including the dorsal aortic root (which is the origin of the ICA), into the mediastinum and results in the persistence of the embryologic angulations of the cervical ICA.16 During early development, the ventral aorta and dorsal aorta are connected via arterial anastomoses known as the primitive aortic arches.1 As the fetus reaches the 4-mm stage, the first and second primitive aortic arches involute and their remnants become the primitive mandibular artery and hyoid artery, respectively, incorporated as branches of the dorsal aorta. At this stage, the primitive mandibular artery and the hyoid artery anastomose with a complex vascular plexus in the region that will later become the future face and pharynx, with its territory later annexed by the external carotid circulation. As the third primitive aortic arch develops and gives rise to the cervical ICA in the 5– 6 –mm stage, the primitive mandibular artery starts to regress, and by 7–12 mm, it is no longer present. The remnants of its plexus consolidate to become the mandibulovidian artery that arises from the foramen lacerum segment of the ICA, rarely noted in normal angiographic studies. The mandibular branch courses anteroinferiorly to supply the soft tissues of the pterygoid muscles, posterior pharyngeal wall, and possibly, the mandibular condyle. The vidian branch enters its attenuated osseous canal, along with the greater superficial petrosal nerve, and anastomoses with the vidian branches of the internal maxillary artery in the region of the pterygopalatine fossa, with potential persistent supply to the posterior nasopharynx, nasal septum, and turbinates in response to the internal maxillary artery developmental hypoplasia or injury and/or occlusion. The clinical significance of this mandibulovidian remnant is most often evident in recruitment of the ICA–vidian artery supply to hypervascular tumors such as juvenile nasopharyngeal angiofibromas (Fig 4). In addition, ECA collateral networks to the ICA-mandibulovidian artery (via both the internal maxillary artery– vidian branch and ascending pharyngeal artery–superior pharyngeal branch) require caution when performing head and neck embolizations in this region.17 Primitive Maxillary Artery PERSISTENT PRIMITIVE CAROTID– VERTEBROBASILAR ANASTOMOSES The primitive maxillary artery is derived from the proximal remnant of the first pharyngeal arch and is represented in the adult pattern as the posterior inferior hypophyseal artery, which arises from the cavernous ICA, posterior to the Primitive carotid anastomoses to the longitudinal neural arteries provide a transient arterial supply to the hindbrain in the very early 4-mm embryo, thus persistent ICA-vertebrobasilar anastomoses represent the oldest brain vascular Neurographics 2016 July/August; 6(4):237–246; www.neurographics.org 兩 239 Fig 3. Aberrant ICA. Coronal MRA (A), anteroposterior DSA (B), and axial CT (C) images demonstrate an aberrant intratympanic course of the right ICA, exhibiting a relatively hypoplastic proximal caliber, lateral deviation into the middle ear, acute angulation (A, B) (white and black arrows) into the horizontal petrous segment, which indicates the level of inferior tympanic to caroticotympanic artery anastomosis, and a thin osseous carotid plate (C) (white arrow). anomaly that can be clinically identified.18 The 4 primitive carotid-vertebrobasilar anastomoses are mainly categorized into presegmental (trigeminal, otic, and hypoglossal) and proatlantal intersegmental arteries. These anastomoses provide carotid supply to 2 longitudinal neural arteries that distally fuse to form the basilar artery. Later in the 5– 6 –mm embryo, a PcoA develops from the anastomosis of the distal ICA and the corresponding longitudinal neural artery respectively, followed by obliteration of primitive otic, hypoglossal, trigeminal, and proatlantal intersegmental arteries.19 Failure in regression of these primitive arteries leads to formation of persistent carotid-vertebrobasilar anastomoses. Persistent Primitive Trigeminal Artery The persistent primitive trigeminal artery is the most common and most cephalic of the persistent carotid-vertebrobasilar anastomoses (Fig 5A, -B). Its reported prevalence is 240 兩 Neurographics 2016 July/August; 6(4):237–246; www.neurographics.org 0.1%– 0.6%.20 This artery originates from the ICA immediately after its exit from the petrous carotid canal and anastomoses with the midbasilar artery. After arising from the cavernous portion of the ICA, the persistent trigeminal artery may enter the sella and penetrate the dura connecting to the basilar artery between the anterior inferior cerebellar and the superior cerebellar artery origins (trans-sellar). It may also course laterally (parasellar), adjacent to the sensory root of trigeminal ganglion connecting to the basilar artery.21 Due to its higher incidence, it is not uncommon to encounter a persistent primitive trigeminal artery during diagnostic cerebral angiography or neuroendovascular procedures. The presence of carotid-vertebrobasilar anastomoses warrants caution in transsphenoidal surgeries and Wada testing, which require superselective catheterization distal to these variants to avoid the risk of inadvertent brain stem anesthesia from primitive anterior to posterior circulation shunts. Saltzman20 classified the angiographic appearance of a persistent primitive trigeminal artery into 3 types. In type 1, the PcoA is hypoplastic or absent and the persistent primitive trigeminal artery joins the basilar artery between the anterior inferior cerebellar arteries and superior cerebellar arteries, which provides the main supply for the distal basilar, bilateral superior cerebellar arteries, and PCA. In type 2, the persistent primitive trigeminal artery joins the basilar artery, as in type 1, by supplying the bilateral superior cerebellar arteries, but the ICA may supply the PCAs via patent PcoAs. The prevalence of these 2 types is relatively equal, and the basilar artery is usually hypoplastic caudal to the anastomosis of the persistent primitive trigeminal artery. In a type 3 variation, usually considered a combination of the previous types, the persistent primitive trigeminal artery joins the ipsilateral superior cerebellar arteries (Fig 5C) directly with variable supply to the PCAs.20 Persistent Primitive Otic Artery The persistent primitive otic artery is the rarest variant of the primitive carotid–vertebrobasilar anastomoses due to its earliest obliteration between the presegmental and proatlantal intersegmental arteries in the fourth week of embryogenesis. It arises from the petrous ICA within the carotid canal, coursing in the internal acoustic meatus, and joins the caudal basilar artery between the anterior inferior cerebellar and superior cerebellar arteries.18 Approximately 8 cases of this variant have been reported; and it has even been associated with an intracranial aneurysm.5 Persistent Primitive Hypoglossal Artery The persistent primitive hypoglossal artery is the second most common carotid-vertebrobasilar anastomosis, with a prevalence of 0.02%– 0.10%.22 It originates from the ICA at the C1 through C3 levels, courses through the hypoglossal canal (not the foramen magnum), and joins the proximal basilar artery. In 79% of cases, the PcoAs are hypoplastic, and, in 78% of cases, the proximal vertebral artery is hypoplastic.5 A definitive diagnosis is based on the recognition of an anomalous artery centered within an enlarged hypoglossal canal. Clinically, a persistent hypoglossal artery is the most likely to cause neurovascular compression symptoms and may present with glossopharyngeal neuralgia and hypoglossal nerve paralysis. Fig 4. Primitive mandibular artery. Lateral oblique DSA image identifies a mandibolovidian artery–vidian branch (black arrow) arising from the foramen lacerum segment of the ICA due to recruitment from a hypervascular juvenile nasopharyngeal angiofibroma. Note the prominent hypertrophied arteries arising superiorly from the inferolateral trunk (foramen rotundum and ovale branches [black arrowhead]) to also supply the hypervascular tumor (arrowhead). Proatlantal Intersegmental Artery The proatlantal intersegmental artery (Fig 6) originates from the CCA bifurcation, ECA, or ICA at the C2 through C4 levels, joins the horizontal V3 segment of the vertebral artery in the suboccipital region, and traverses the foramen Fig 5. Persistent primitive trigeminal artery. Three-dimensional TOF MRA (A) and oblique DSA (B) images show a prominent Saltzman type 1 persistent primitive trigeminal artery (white and black arrows) arising from the cavernous right ICA with direct anastomosis to the basilar artery. Note the hypoplasia of the vertebral-basilar artery proximal to the anastomosis. An oblique DSA (C) image demonstrates a rare Saltzman type 3 persistent primitive trigeminal artery variant (black arrow) directly supplying the ipsilateral superior cerebellar artery. Neurographics 2016 July/August; 6(4):237–246; www.neurographics.org 兩 241 The AChA arises from the rostral division of the primitive ICA and supplies the posteromedial hemispheric territory in the early embryologic stage. As the gestational age increases, a posterior choroidal artery develops from the caudal division and replaces the supply to this region. If there is a failure of the posterior choroidal artery to augment this distribution, it can lead to the persistence of the AChA as the main supply for the temporal-occipital lobes. Other AChA anomalies include agenesis, an anomalous origin from the middle cerebral artery and PCoA, and AChA duplication. A hyperplastic AChA may mimic a duplicated PCoA–fetal PCA in the setting of a separate prominent PCoA or fetal PCA. A duplicated branch that arises from the ICA distal to the origin of the native PCoA–fetal PCA, and that courses as an isolated temporal branch has been classified as a persistent primitive PCA, although it can easily be mistaken for a hyperplastic AChA (Fig 7).26 PERSISTENT PRIMITIVE ICA-ECA ANASTOMOSES Fig 6. Proatlantal intersegmental artery. Oblique lateral DSA image demonstrates a rare proatlantal intersegmental artery (white arrow) arising from the CCA, consistent with a persistent primitive carotid–vertebral anastomosis. magnum. Three variants have been described: type 1 originates from the dorsal aspect of the ICA and accounts for 38% of cases, type 2 arises from the ECA and comprises 57% of cases, and type 3 rarely arises from the CCA or bifurcation (5%).19 Associated cerebrovascular abnormalities, including intracranial aneurysms, have been described in patients with carotid-vertebrobasilar anastomoses, including the proatlantal intersegmental artery.19,23,24Also, aplasia or hypoplasia of one or both vertebral arteries proximal to the anastomosis may be identified in 50% of cases.24 PcoA and Fetal PCA PCoA variants have been extensively described with multiple types of anatomic anomalies and morphologies related to its early embryologic development as described: hypoplasia and/or aplasia (agenesis), different lengths and courses, fetal configuration of the PCA branching directly from the ICA, vessels that originate directly from the PCoA (eg, AChA), PCoA infundibulum, fenestration, and partial or complete duplications (with or without a patent basilar P1 segment).2 Interestingly, the variations of the right PCoA have been described to be more common than the left. Hyperplastic AChA A hyperplastic AChA is defined by the posterior temporal branch of the PCA that arises from the AChA and can be identified in 1.1% to 2.3% of angiographic examinations.25 242 兩 Neurographics 2016 July/August; 6(4):237–246; www.neurographics.org The primitive ICA arises from the third aortic arch. Although there are controversial comments regarding the origins of the CCA and ECA in the literature, it seems that the CCA evolves from the ductus caroticus and the ECA develops from the ventral pharyngeal artery that arises either directly from the third aortic arch or from the aortic sac that migrates to the third aortic arch.12,27 Anastomoses between the ICA and ECA branches become angiographically apparent and are commonly identified secondary to high-flow recruitment from neurovascular pathologies, such as hypervascular tumors, dural arteriovenous fistulas (AVF), arteriovenous malformations (AVM), or proximal ICA occlusions. Multiple primitive ICA-ECA anastomoses persist into adulthood, and several notable collateral pathways include intracavernous meningohypophyseal trunk branches of the ICA with the ascending pharyngeal artery; the inferolateral trunk of the ICA via the foramen rotundum and foramen ovale branches of the internal maxillary artery and middle meningeal arteries, the mandibulovidian trunk of the intrapetrous ICA via branches of the internal maxillary and the ascending pharyngeal artery; and ophthalmic artery via branches of the facial, internal maxillary artery, and the middle meningeal artery. Conversely, persistent primitive ICA-ECA anastomoses are very rare. The very early anastomosis between ICA and ECA forms at 4 –5 weeks of fetal life via the hyostapedial trunk when the inferior division stapedial artery (arising from the hyoid artery near the proximal ICA as a dorsal remnant of the second aortic arch) transiently connects to the ventral primitive pharyngeal arteries, which will develop the final ECA. The stapedial artery regresses after this anastomosis, but the hyoid artery persists to form the adult caroticotympanic branch of the petrous portion of the ICA. Abnormal or interrupted stapedial artery regression allows for the congenital manifestation of ICA-ECA anastomoses.1,28 Fig 8. Persistent primitive ECA-ICA anastomoses. Lateral DSA images depict direct origins of the occipital artery (A) and ascending pharyngeal artery (B) arising directly from the ICA (black arrowhead). Note hypertrophied ascending pharyngeal artery–neuromeningeal trunk supplies a contralateral dural AVF of the left anterior condylar vein via multiple ascending clival branches. Occipital Artery and Ascending Pharyngeal Artery Arising from the ICA Usually no branches originate from the cervical segment of the ICA in the neck. Occasionally, as described above, the proatlantal intersegmental and hypoglossal arteries persist from the cervical segment of the ICA into adult life. The occipital artery (Fig 8A) seems to be the most common ECA branch to arise directly from the cervical ICA, followed by the ascending pharyngeal artery (Fig 8B). The occipital artery and ascending pharyngeal artery develop a pharyngealoccipital system at the craniocervical junction, which supplies cervical somites C1, C2, C3, and the third branchial arch.3,29 In addition, several case reports describe the unusual origination of lingual, middle meningeal, facial, and laryngeal arteries from the CCA and ICA.30-33 Persistent Stapedial Artery Fig 7. Duplicated fetal PCA with hyperplastic AChA. A, Three-dimensional rotational DSA axial multiplanar reconstructions demonstrates separate origins of both proximal PCoA–fetal PCA (1) and a distal fetal PCA (2), initially suspected to be a persistent primitive PCA that supplies an isolated posterior temporal branch territory. B, However, a small AChA branch is identified arising from the distal fetal PCA and extends through the choroidal fissure (arrow), consistent with a hyperplastic AChA. C, 3-dimensional reconstructions further delineate the distal hyperplastic AChA supplying the posterior temporal branch (curved arrow), and separate proximal PCoA–fetal PCA (arrow). The stapedial artery is a normally transient embryonic anastomosis between the branches of the future external carotid artery and ICA, as described above. A persistent stapedial artery has a reported prevalence of 0.48%.34 The stapedial artery originates from the vertical segment of the petrous ICA, passes through the obturator foramen of the stapes, and terminates as the middle meningeal artery. CT findings along the course of a persistent stapedial artery may include a small canaliculus at the distal end of the carotid canal; a linear structure that crosses the promontory of the tympanic cavity; an enlarged facial nerve canal or a separate canal that parallels the facial nerve canal; and the absence of the foramen spinosum, which normally contains the middle meningeal artery.5 The stapedial artery may be mistaken for a vascular neoplasm of the middle ear (glomus tympanicum tumor) and may present with pulsatile tinnitus. It is important to identify a persistent stapedial artery before surgery because its presence may complicate tympanotomy, stapedectomy, and cholesteatoma resection as well as hinder cochlear implantation. Neurographics 2016 July/August; 6(4):237–246; www.neurographics.org 兩 243 PARACLINOID AND SUPRACLINOID ICA ANOMALIES According to the classification by Lasjaunias and SantoyoVazquez,35 the first embryologic segment of the ICA is derived from the third aortic arch, whereas the remaining 6 embryologic distal segments come from the dorsal aorta. The embryonic branches of the ICA, including the hyostapedial trunk, primitive mandibular artery, primitive maxillary artery, trigeminal artery, dorsal ophthalmic artery, and primitive ophthalmic artery separate the ICA segments consecutively as the cervical ICA (segment 1), ascending petrous (segment 2), horizontal petrous (segment 3), ascending cavernous (segment 4), horizontal cavernous (segment 5), clinoid (segment 6), and supraclinoid-terminal (segment 7) ICAs. The origin of the dorsal ophthalmic artery (defined by Lasjaunias and Santoyo-Vazquez35) is between segments 5 and 6, which form the adult inferolateral trunk, whereas the origin of the primitive ophthalmic artery (defined by Padget1) is between segments 6 and 7, and forms the adult ophthalmic artery. Infraoptic Anterior Cerebral Artery An infraoptic course of the precommunicating anterior cerebral artery is a rare anomaly. In 2008, Wong et al36 summarized a total of only 42 examples reported in the literature, and they reported 2 additional cases. Overall, 59% of these cases were associated with cerebral aneurysms. An infraoptic A1 segment (Fig 9) is characterized by 3 features: (1) the anomalous artery branches off the ICA at the level of the ophthalmic artery, (2) it travels beneath the optic nerve, and (3) it supplies the vascular territory of a normal anterior cerebral artery. The configurations of the proximal anterior cerebral arteries in the presence of an infraoptic A1 may be classified into 4 types according to the presence or absence of ipsilateral supraoptic A1 and contralateral A1 segments.36 The embryogenesis of this anomaly is still controversial. Proposed explanations in the literature are as follows: (1) the persistence of the embryonic anastomosis between the primitive maxillary artery and the anterior cerebral artery, (2) the persistence and enlargement of an embryologic anastomotic loop between the primitive dorsal and ventral ophthalmic arteries, and (3) the enlargement of the prechiasmal arterial anastomosis. Dorsal and Ventral Ophthalmic Arteries During early embryonic development, 2 primitive ophthalmic arteries are present: the ventral and dorsal ophthalmic arteries. The ventral ophthalmic artery, which is thought to normally persist by migrating toward the normal ophthalmic artery origin, arises from the anterior cerebral artery passing through the optic canal. Subsequently, the medial posterior ciliary artery arises from the ventral ophthalmic artery and supplies the medial side of the optic vesicle. The proximal segment of the ventral ophthalmic artery regresses.37 The dorsal ophthalmic artery eventually regresses with its vestiges represented by the anteromedial branch of 244 兩 Neurographics 2016 July/August; 6(4):237–246; www.neurographics.org Fig 9. Infraoptic anterior cerebral artery. Oblique DSA (A) and 3-dimensional TOF MRA axial source images (B, C) demonstrate an anomalous, infraoptic course of the left A1 segment (white arrows) arising at the level of the ophthalmic artery (arrowhead), coursing under the optic nerve and supplying the A2 segments of bilateral anterior cerebral arteries. the inferolateral trunk or the recurrent tentorial branch of the ophthalmic artery. In some instances, the dorsal ophthalmic artery may persist as the dominant supply to the orbit, which arises from the carotid siphon between the fifth (horizontal cavernous) and sixth (clinoid) ICA segments (Fig 10). On CT, this anomalous artery is seen to arise from the dorsal aspect of the extracranial paraclinoid segment of the ICA as a branch of the inferolateral trunk and enters the 7. 8. 9. 10. 11. 12. Fig 10. Persistent dorsal ophthalmic artery. A lateral DSA image demonstrates a prominent dorsal ophthalmic artery (black arrow) with an extracranial origin from the expected location of the inferolateral trunk and supplies the orbit via the superior orbital fissure. orbit through the superior orbital fissure instead of the optic canal. 13. 14. 15. CONCLUSION Variants of the cervical and intracranial ICA are rare, typically asymptomatic, and often incidental findings. However, these variants can occasionally influence surgical strategy, balloon test occlusion studies, temporary occlusion time, Wada testing, and embolization risk in the setting of hypervascular tumors or dural AVFs, with potential impact on procedural complications and patient outcomes. In addition, they inherently provide redundant but valuable embryologic collaterals to maintain intracranial flow in settings of ICA compromise or occlusion. REFERENCES 1. Padget DH. The development of the cranial arteries in the human embryo. Contrib Embryol 1948;32:207– 62 2. Abrahams JM, Hurst RW, Bagley LJ, et al. Anterior choroidal artery supply to the posterior cerebral artery distribution: embryological basis and clinical implications. Neurosurgery 1999;44:1308 –14 3. Lasjaunias P, Berenstein A. Surgical Neuroangiography vol 3. Functional Vascular Anatomy in Brain Spinal Cord and Spine. New York: Springer Verlag Berlin Heidelberg; 1992: 15– 87 4. Din H, Alioglu Z, Erdl H, et al. Agenesis of the internal carotid artery associated with aortic arch anomaly in a patient with congenital Horner’s syndrome. AJNR Am J Neuroradiol 2002;23:929 –31 5. Dimmick SJ, Faulder KC. Normal variants of the cerebral circulation at multidetector CT angiography. Radiographics 2009;29:1027– 43. 10.1148/rg.294085730 6. Weon YC, Chung JI, Kim HJ, et al. Agenesis of bilateral 16. 17. 18. 19. 20. 21. 22. 23. 24. internal carotid arteries and posterior fossa abnormality in a patient with facial capillary hemangioma: presumed incomplete phenotypic expression of PHACE syndrome. AJNR Am J Neuroradiol 2005;26:2635–39 Ulger FE, Ulger A, Colak M. Absence of the right common carotid artery: Doppler ultrasonographic and MR angiographic findings. Vascular 2014;22:364 – 67. 10.1177/ 1708538113516316 Kobayashi D, Natarajan G, Joshi A, et al. Congenital absence of bilateral common carotid arteries. Ann Thorac Surg 2013; 95:719. 10.1016/j.athoracsur.2012.06.052 Maybody M, Uszynski M, Morton E, et al. Absence of the common carotid artery: a rare vascular anomaly. AJNR Am J Neuroradiol 2003;24:711–13 Moncada R, Shannon M, Miller R, et al. The cervical aortic arch. Am J Roentgenol Radium Ther Nucl Med 1975;125: 591– 601. 10.2214/ajr.125.3.591 Sadler T. Langman’s Medical Embryology. 8th ed. Baltimore: Lippincott Williams & Wilkins; 2000 Gailloud P, Murphy KJ, Rigamonti D. Bilateral thoracic bifurcation of the common carotid artery associated with Klippel-Feil anomaly. AJNR Am J Neuroradiol 2000;21:941– 44 Hurley MC, Nguyen PH, DiPatri AJ, et al. Isolated origin of the left internal carotid artery from the pulmonary artery. J Neurosurg Pediatr 2008;2:207–11. 10.3171/PED/2008/2/9/ 207 Tugrul S, Eren SB, Dogan R, et al. Intratympanic aberrant and hypoplastic carotid artery. Am J Otolaryngol 2013;34:608 – 10. 10.1016/j.amjoto.2013.02.010 Srinivasan S, Ali SZ, Chwan LT. Aberrant retropharyngeal (submucosal) internal carotid artery: an under-recognized, clinically significant variant. Surg Radiol Anat 2013;35:449 – 50. 10.1007/s00276-012-1047-3 Paulsen F, Tillmann B, Christofides C, et al. Curving and looping of the internal carotid artery in relation to the pharynx: frequency, embryology and clinical implications. J Anat 2000;197(pt 3):373– 81. 10.1046/j.1469-7580.2000. 19730373.x Marden FA. Persistent primitive mandibular artery associated with congenital absence. Neurographics 2011;1:91–95. 10. 3174/ng.3110016 Raybaud C. Normal and abnormal embryology and development of the intracranial vascular system. Neurosurg Clin N Am 2010;21:399 – 426. 10.1016/j.nec.2010.03.011 Luh GY, Dean BL, Tomsick TA, et al. The persistent fetal carotid-vertebrobasilar anastomoses. AJR Am J Roentgenol 1999;172:1427–32. 10.2214/ajr.172.5.10227532 Saltzman GF. Patent primitive trigeminal artery studied by cerebral angiography. Acta Radiol 1959;51:329 –36 Rhee SJ, Kim MS, Lee CH, et al. Persistent trigeminal artery variant detected by conventional angiography and magnetic resonance angiography-incidence and clinical significance. J Korean Neurosurg Soc 2007;42:446 – 49. 10.3340/jkns. 2007.42.6.446 Oelerich M, Schuierer G. Primitive hypoglossal artery: demonstration with digital subtraction-, MR- and CT angiography. Eur Radiol 1997;7:1492–94. 10.1007/s003300050322 Morita A, Fukushima T, Miyazaki S, et al. Tic douloureux caused by primitive trigeminal artery or its variant. J Neurosurg 1989;70:415–19. 10.3171/jns.1989.70.3.0415 Kolbinger R, Heindel W, Pawlik G, et al. Right proatlantal artery type I, right internal carotid occlusion, and left internal ca- Neurographics 2016 July/August; 6(4):237–246; www.neurographics.org 兩 245 25. 26. 27. 28. 29. 30. 31. 246 rotid stenosis: case report and review of the literature. J Neurol Sci 1993;117:232–39. 10.1016/0022-510X(93)90178-2 Takahashi S, Suga T, Kawata Y, et al. Anterior choroidal artery: angiographic analysis of variations and anomalies. AJNR Am J Neuroradiol 1990;11:719 –29 Uchino A, Kamiya K, Suzuki C. Duplicate origin of the posterior communicating artery diagnosed by magnetic resonance angiography. Surg Radiol Anat 2013;35:741– 43. 10. 1007/s00276-013-1095-3 Drazin D, Choulakian A, Alexander MJ. Congenital absence of the common carotid artery in a patient with a ruptured anterior communicating artery aneurysm. J Neurointerv Surg 2010;2:208 –10. 10.1136/jnis.2009.001966 Steffen TN. Vascular anomalites of the middle ear. Laryngoscope 1968;78:171–97. 10.1288/00005537-196802000-00001 Chitra R. Trifurcation of the right common carotid artery. Indian J Plast Surg 2008;41:85– 88. 10.4103/0970-0358.41121 Kawai K, Yoshinaga K, Koizumi M, et al. A middle meningeal artery which arises from the internal carotid artery in which the first branchial artery participates. Ann Anat 2006;188: 33–38. 10.1016/j.aanat.2005.08.013 Lucev N, Bobinac D, Maric I, et al. Variations of the great arteries in the carotid triangle. Otolaryngol Head Neck Surg 2000;122:590 –91 兩 Neurographics 2016 July/August; 6(4):237–246; www.neurographics.org 32. Iimura A, Oguchi T, Yamazaki Y, et al. Anomalous bifurcation and island formation of the carotid artery. Okajimas Folia Anat Jpn 2010;86:121–28. 10.2535/ofaj.86.121 33. Matsumoto M, Okuda H, Ishidoh E, et al. An anomalous case of the common carotid artery giving off several branches and high division of the internal carotid artery. Okajimas Folia Anat Jpn 1986;63:37– 43. 10.2535/ ofaj1936.63.1_37 34. Moreano EH, Paparella MM, Zelterman D, et al. Prevalence of facial canal dehiscence and of persistent stapedial artery in the human middle ear: a report of 1000 temporal bones. Laryngoscope 1994;104:309 –20 35. Lasjaunias P, Santoyo-Vazquez A. Segmental agenesis of the internal carotid artery: angiographic aspects with embryological discussion. Anat Clin 1984;6:133– 41. 10.1007/ sBF01773165 36. Wong ST, Yuen SC, Fok KF, et al. Infraoptic anterior cerebral artery: review, report of two cases and an anatomical classification. Acta Neurochir (Wien) 2008;150:1087–96. 10.1007/ s00701-008-0016-4 37. Komiyama M. Letter to the editor—embryology of the ophthalmic artery: a revived concept. Interv Neuroradiol 2009; 15:363– 68