* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download 投影片 1 - cmcuro.net
Survey
Document related concepts
Common cold wikipedia , lookup
Childhood immunizations in the United States wikipedia , lookup
Gastroenteritis wikipedia , lookup
Rheumatic fever wikipedia , lookup
Staphylococcus aureus wikipedia , lookup
Multiple sclerosis signs and symptoms wikipedia , lookup
Infection control wikipedia , lookup
Neonatal infection wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
Carbapenem-resistant enterobacteriaceae wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Transcript
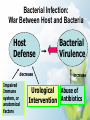
Prevention Of UTIs in Endourological Surgery: Regulation, Guideline, Evidence, and Practice In Taiwan Stephen SD Yang, M.D., PhD. Associate Professor of Department of Urology, Tzu Chi Uninersity, Hualien, Taiwan Chief of Department of Surgery Tzu Chi General Hospital, Taipei Branch,Taipei, Taiwan 楊緒棣 副教授,外科部 主任 慈濟綜合醫院台北分院 2007/06/09 Welcome to Buddhist Tzu Chi General Hospital, Xindian, Taipei,Taiwan: The First Buddhist chain hospital in the world Fight for Antibiotic Abuse! • In 1990s, • 30% of URI cases used antibiotics • 6 days for SSI prophylaxis 1990 Active Surveillance 1995 NHI: strict regulations TQIP 1999 Surveillance for SSI Another field is animal use of antibiotics 2002 TMAC Medical students 2002 Public education School Education (junior high school) 2000 Control Yuan Involvement 2001 National Surveillance Program 2003 Hospital Evaluation In 2004 17% of URI cases used antibiotics. 3 days for SSI prophylaxis Less use of 2nd line antibiotics 張上淳 感控 雜誌 200616:205 -18 Use and Abuse of Surgical Antibiotic Prophylaxis in Hospitals in Taiwan • Sep 1998 –March 1999, 629 patients in 14 hospitals. • 499 (79%) for surgical prophylaxis (not including GU) . 89% clean wound. • Mean no. of antibiotics: 2 kinds. • 1st Cepha 449 (90%) and Aminoglycosides 233 (50%) • Mean duration of use: 6 days. • More than 70 % use longer than 3 days. • Mc Donald LC, et al: J Formos Med Assoc 2001;100:5-13. Bacterial Infection: War Between Host and Bacteria Host Defense decrease Impaired Immune system, or anatomical factors Bacterial Virulence increase Urological Abuse of Intervention Antibiotics Materials and Methods • Regulations: the publications of the National Health Insurance Bureau, Taiwan. The Payer of medical fee. The Boss!! • Guidelines: (1) Taiwanese Association of Infectious Disease. (2) EAU UTI guideline 2006. (3) CampbellWalsh Urology 9th edition, 2007. The academic consensus? • Evidences: Published reports from Taiwan and around the world. Retrospective or prospective data from TCH, Taipei, Taiwan • Practice: Email survey to 69 (17.3%) of 400 Urologists in Taiwan. • The prescribers. The possible benefits/risks takers. Practice of Urologists in Taiwan Workplace distribution N=69 Age distribution Clinic 3% 61-65 y/o 4% 56-60 y/o 1% Area hosipital 12% M edical center 49% regional hosipital 36% Years of practice >65 y/o 0% ≦35 y/o 16% 51-55 y/o 16% 46-50 y/o 22% 36-40 y/o 25% 41-45 y/o 16% Grades of academic position 25 years 3% Associate Professor 13% 21-25 years 12% ≦5 years 25% 16-20 years 17% 11-15 years 17% Professor 7% 6-10 years 26% Nil 49% Assistant Professor 7% Lecturer 29% Regulations (I) of Perioperative Antibiotics in Surgery: Taiwan Health Insurance Bureau • 4. Price of the agents should be considered. • 5. First line antibiotics should be used first. (table) • 6. The following conditions may use second line antibiotics: (3) Confirmed by infection men, (4) Apparent surgical infections. • Chap. 10. Antimicrobial agents. Pp 58-65. Regulations of the payment for pharmaceutical agents. Central Health Insurance Bureau. 2006/07. (WWW.nhi.gov.tw) Regulations (II) of Perioperative Antibiotics in Surgery: Taiwan Health Insurance Bureau • 7. Conditions to use second line antibiotics: (1) Culture proved that second line antibiotics is required in cases of using 1st line antibiotics longer than 72 hours. (2) 7 days later after using first line antibiotics for 72 hours and still not effective after changing to another first line antibiotics. Regulations (III) of Perioperative Antibiotics in Surgery: Taiwan Health Insurance Bureau • 8. Prophylatic antibiotics for surgery. • (1) Clean wound: -A) clean wound such as herniorraphy, thyroidectomy: no antibiotics, or at most one dose before op. • (2) Clean contaminated wound: GU, GI, Chest, Gyn, etc. First line medicine for 24 hours. Specify indication of using antibiotics longer than 48 hours or second line ABx. List of First Line Antibiotics Allowed in Taiwan • Oral: amoxicillin, Cefalexin, Clindamycin, doxycyclin, minocycline, nalidixic acid, nitrofurantoin, trimethoprime/ sulf methoxazole, etc. • Parental: Cefazoline, cephalothin, gentamicin, penicillin, etc. • Table 1. p75. List of first line antibiotics. Central Health Insurance Bureau. 2006/07. (WWW.nhi.gov.tw) • BREAKING THE RULES, GETTING NO PAY AND PENALTY!!! Guidelines for the use of prophylatic antibiotics in urological surgery in Taiwan (only 3 procedures) Site/proc edure Likely Recommend pathoge ed ns antibiotics Alternative Durati on TRUSPBx Enteric GNB Cefazoline 1gm IV at IA GM 2mg/kg IV on call to OR or Ciproxacin 500mg oral or 400mg IV on call to OR 1 dose TU-P-Bx Enteric GNB Cefazoline 1gm IV at IA GM 2mg/kg IV on call to OR or Ciproxacin 500mg oral or 400mg IV on call to OR 1 dose TUR-BT Enteric GNB Cefazoline 1gm IV at IA GM 2mg/kg IV on call to OR 1 dose Microbiol Immunol Infect 2004;37:71-4 Prophylaxis for Cystoscopy Regulations: 0-1 dose 1st line antibotics? Guideline for Prophylaxis for Cystoscopy • EAU 2006: no prophylaxis. (2nd gen Cephalosporines or TMP +/- SMX for patients at risk of UTI). • Campbell-Walsh 2007: No absolute indication for antimicromial prophylaxis for cystoscopy, but indicated in patients at risk of UTI. Prophylaxis for UTI after single catheterization or cystoscopy • The risk of infection after one time catheterization in healthy woman: 1-2%. • Of patients with sterile urine, 2.2% -7.8% reported culture-proven UTIs. While Rane, et al, (2001) reported a high rate of 21% after cystoscopy. • Single dose prophylaxis reduced infections to 1% to 5%. No significant systemic infection. – Campbell –Walsh Urology, 2007, 9th ed. UTI after Urodynamics and/or cystoscopy • After UDS, 19 (20%) of 97 pt with negative culture developed a positive culture afterward. No significant risk factor was detected Okorocha I, et al: BJU International 2002;89:863-7 • Two doses nitrofurantoin (n=74) vs. placebo (n=68) for women undergoing combined urodynamics and cystourethroscopy: No difference in rate of post exam UTI . Cundiff GW, et al: Obstet Gynecol 1999;93(5 pt 1):749-52. • One dose 400mg Norfloxacin: no significant effect in cases received flexible cystoscopy. Wilson L, et al: J Endourol 2005;19:1006-8. Temporary Data for Single dose Cephalexin prophylaxis for Cystoscopy • Up to Apr. 30, 2007 • Placebo: 9 (M7, F2), one female with carruncle had post exam UTI. • Cephalexin : 7 (6M, 1F). Nil had UTI. • Temporary conclusion: no prophylaxis is required in case with no risk factor, e.g. Bladder outlet obstruction. Conclusions on prophylactic antibiotics for cystoscopy • UTI after UDS or cystoscopic examinations varied from 2% to 21%. • Symptoms of UTI after cystoscopy were usually not severe, and spontaneous resolution of UTI occurred. • Pre-instrumentation prophylactic antibiotics may be not necessary. • Postmenopausal women and all men undergoing cystoscopy may need prophylaxis. Prophylaxis for Shock Wave Lithotripsy (SWL) Regulations : 0-1 dose 1st line antibotics? • EAU guideline: no prophylaxis for SWL • Campbell-Wash: prophylaxis! (In patients with stone and sterile urine, infection rate after SWL reduced from 5.7% to 2.1%, Pearle 1997) • A history of a recent UTI or of infectious stones should warrant a full treatment course of antimicrobial agents before SWL. Prophylaxis for SWL: a meta-analysis • 8RCT, 885 patients. • The incidence of UTIs after SWL without prophylaxis: 0%-28%., with a median of 5.7%. • Prophylactic antibiotics in cases with sterile urine decrease UTIs: 0-7.7%, with a median of 2.1%. (Pearle MS and Roehrborn CG, Urology 1997; 49:679-86) SWL 100% (A) No pyuria、APN or UTI N=69 Antibiotic use 91% pr e-op Rat e Post -op Rat e 90% 80% 65% 70% 60% 50% 40% 30% 16% 16% 20% 7% 0% 0% 10% 0% 1% 1% 0% N o ant i bi ot i c use 1 t h l i ne cephal 1 . 0 gm 1 t h l i ne am i no Com bi ne w i t h cephal + am i no O t her s : pr e-op Rat e 91% 7% 0% 1% 0% Post -op Rat e 65% 16% 0% 1% 16% 20% 20% Antibiotic dose 18% 16% 14% 12% 10% 8% 7% 7% 6% 3% 4% 1% 2% 1% 3% 0% 0% 0% 0% 0% 0% 0% 0% 0% 0% 3 days 5 days 7 days 1 4 days m i ssi ng answ er 0% 0% 0% 0% 0% 0% 3% 20% 0% 0% 0% 7% 1 dose 1 day 2 days pr e-op Rat e 7% 1% Post -op Rat e 1% 3% Discussion: Prophylactic Antibiotics in SWL without UTIs • 91% did not use preop ABx. 65% did not use post op. ABx. • 23% use post op. ABx for >1 days.! • But preoperative oral antibiotics is more important and postop antibiotics may be not necessary in cases without postop fever! • Stone size and location may have an impact on post SWL infection rate. Further study is required. • Our impression: stone less than 10mm may not need prophylaxis. • Recent pain attack and no fever no prophylaxis? Prophylaxis for Ureteroscopoic lithotripsy (USL) Regulations: Clean contaminated wound. First line medicine for 24 hours. • EAU 2006: uncomplicated distal ureteral stone no prophylaxis. Proximal or impacted stone, or PCNL all patients need prophlaxis with 2nd or 3rd cepha or TMP +/- SMX or Aminopenicillin/BLI or fluoroquinolones. Short course (1-3days) is recommended. • Campbell-Walsh 2007: recommended prophylaxis. Prophylaxis for USL • Incidence of UTI after USL is 1.3% in a large series. (Sosa RE, 159-68.) • Knopf et al, 2003: RCT to prove that prophylactic fluoroquinolone administration significantly reduced postop UTIs in a healthy population (n=113) with ureteral stone and uninfected preop urine (12.5% 1.8%). (F-Q not allowed in Tw) • Taylor AL, et al, 2002: 63 URS in 56 cases, including URSL in 54 sides. Perioperative use of antibiotics: 3 (7%) UTIs (pyrexia, PN, pyonephrosis). recommend perioperative antibiotics. (BJU International 89:181-5) Antimicrobial prophylaxis for URSL in TCH, Taipei: A Retrospective Study • Between Sep. 2006 and Apr. 2007, 168 patients underwent URSL. Of them 127 had single ureteral stone. • Preoperative no signs of UTI in 62 patients (Prophylaxis Group), 57 patients had signs of UTI (Therapeutic groups), and 8 patients did not check urinalysis. • Preop urine culture: 0/2 positive in the prophylaxis group ; 7/10 (70%) positive in the therapeutic group (2 E coli, 2 P mirabilis, 2 mixed growth, 1 Group B streptoccous • Cefazoline 1.0 gm IV at induction was used preoperatively in all. 10% add GM. • DJ was inserted as the clinician’s decision. Stone Size and Postoperative Infection Size N (mm) Post Pyuria Back to ER + - ? Pain UTI* Others 7 (44%) 9 9 0 0 1 5-10 44 11 (52%) 10 23 3 <5 17 (50%) 17 24 Total 127 35 (49%) 36 56 >10 25 58 1 (2.3%) 2 3 (5.2%) 5 4 (3.9%) (3.1%) 1 0 2 (1.6%) Stone fragmentation rate: 99.2%. ER rate: 8.6% * Febrile UTI Antimicrobial prophylaxis for USL in TCH, Taipei: Stone Size Groups Prophylactic Therapeutic Antibiotics N Mean stone size (mm) Stone location Up Mid Low Post Op ABx (-) 32 6.7 ± 4.4 14 8 10 Post Op ABx (+) 26 6.2 ± 5.3 9 2 13 Subtotal 58 6.5 ± 4.7 23 10 23 Post Op ABx (-) 7 11.2 ± 5.1 2 4 1 Post Op ABx (+) 39 7.4 ± 5.5 16 9 14 subtotal 46 8.0 ± 5.4 18 13 15 Total 104 7.2 ± 5.0 41 23 38 * Patients without preoperative antibiotics were excluded. Antimicrobial prophylaxis for URSL in TCH, Taipei: Prophylactic Group N Post op Pyuria Back to ER Positive Negative NA UTI Pain * Post Op ABx (+) 26 6 (37.5%) 10 10 1 3 Post Op ABx (-) 32 7 (64%) 4 21 1 1 DJ (+) 46 11 (85%) 2 26 2 (4%) DJ (-) 2 (40%) 3 5 10 DJ + in 22/26 of post anti + in 24/32 of post anti - 0 3 (6.5%) 1 Post op use of antibiotics tended to reduce pyuria rate (p=0.18), but not febrile UTI rate. Antimicrobial prophylaxis for URSL in TCH, Taipei: Therapeutic Group N Post op Pyuria Back to ER Positive Negative NA UTI Pain * 1 (2.6%) 0 1 1 (2.6%) 0 1 Post Op ABx (+) 39 13 (54%) 11 15 Post Op ABx (-) 7 0 5 2 13 (52%) 12 14 0 4 3 DJ (+) 39 DJ (-) 7 DJ + in x/39 of post anti + in y/7 of post anti - 0 0 Post op use of antibiotics did not reduce pyuria rate, nor febrile UTI rate. Postoperative Use of Antibiotics Did not Reduce Pyuria post op Pyuria* Antibiotic s Yes 19/40 (47.5%) Febrile UTI Pain 2/65 (3.1%) 4/65 (6.2%) Nil 1/39 (2.6%) 1/39 (2.6%) 7/16 (43.8%) * P=0.80 DJ insertion: a strong impact on postoperative outcome DJ Positive Pyuria* Febrile UTI Pain 24/38 (63%) 3/85 (3.5%) 4/85 (4.7%) 0 1/17 (5.9%) DJ 2/9 negative (22%) * P=0.026 <0.05 Discussion : Antimicrobial prophylaxis for URSL in TCH, Taipei • Preoperative pyuria usually meant bacteriuria. (70% + predictive rate). • Totally, febrile UTI occurred in 4/127 (3.1%) and All the 4 patients with UTI had DJ inserted. • Stone size does not matter!! • Postop antibiotics were used more frequently in patients with preop pyuria, while it was resulted in no gain. • DJ insertion had a strong impact on postop. Pyuria (63%), and febrile UTI (3.5%). USL (A) No pyuria、nor APN No post fever Antibiotic use 59% 60% 51% pr e-op Rat e Post -op Rat e 50% 40% 30% 26% 23% 20% 3% 10% 10% 10% 13% 0% 1% 0% N o ant i bi ot i c use 1 t h l i ne cephal 1 . 0 gm 1 t h l i ne am i no Com bi ne w i t h cephal + am i no pr e-op Rat e 26% 59% 3% 10% 1% Post -op Rat e 23% 51% 0% 10% 13% O t her s : 70% 64% Antibiotic dose 60% 50% 40% 29% 30% 20% 26% 23% 23% 16% 6% 10% 6% 0% 1% 0% 0% 0% 0 1% 4% 0 0% 0% 1 dose 1 day 2 days 3 days 5 days 7 days 1 4 days mi ssi ng answ er no request pre-op Rat e 64% 6% 0% 0% 0% 0 0 4% 26% Post -op Rat e 16% 29% 1% 23% 0% 1% 0% 6% 23% Discussion: Practice of Prophylactic Antibiotics in USL without signs of UTI • 26% did not use pre-op antibiotics. (Not complying to the rules!) • 23% did not use post op antibiotics. Follow our results. • 10% use two kinds of antibiotics. (Break the rule!) • 23% use postop. antibiotics for 3 days. (Break the rule!) USL (B) With pyuia, no fever, no APN 58 % 60% 52 % pr e-o p Rat e Po st -o p Rat e 50% 33 40% % Antibiotic 30% 20% 23 % 6% 13 % 10 % 10% 0% 3% 0% 0% N o ant i bi ot i c use 1 t h l i ne cephal 1 . 0 gm 1 t h l i ne am i no Com bi ne w i t h cephal + am i no 6% 58% 0% 33% 3% 10% 52% 0% 23% 13% pr e-op Rat e Post -op Rat e 60% N=42 55 O t her s : % 50% Antibiotic dose 40% 33 % 30% 23 25 % % 20% 6% 10% 12 % 9% 7% 3% 3% 6% 3% 0% 0% 0 %0 % 0% pre-op Rat e Post -op Rat e 10 % 6% 1 dose 1 day 2 days 3 days 5 days 7 days 1 4 days mi ssi ng answ er no request 55% 23% 3% 7% 0% 0% 0% 6% 6% 6% 33% 3% 25% 3% 9% 0% 12% 10% Discussion: Practice of Prophylactic Antibiotics in USL in patients with pyuria, without fever • Almost all (94%) use pre-op antibiotics. • 23% did not use post op antibiotics. Follow our results. • 33% use two kinds of antibiotics. (Adequate?) • 40% use postop. antibiotics ≧ 3 days. (Break the rule!) • Afraid of infection without evidence? Discussion: Practice of Prophylactic Antibiotics in USL in Patients Without fever • USL is frequently associated with pyuria (around 50%), febrile UTI (3.1%) and possible ureteral stricture. • Recommend prophylaxis for all patients. • Optimal dose: 1 dose for cases with single ureteral stone without postoperative fever. • Preoperatvie pyuria did not need additional antibiotics. Prophylaxis for PCNL Regulations : short course, 1-3 days? • EAU guideline:2nd or 3rd cepha or TMP +/- SMX or Aminopenicillin/BLI or fluoroquinolones. Short course (<72 hrs.) • Campbell 2007: Ampicillin + GM or Fluoroquinolones. Single dose to 1 day. Antibiotic prophylaxis in PCNL: prospective study • 81 patients with preop sterile urine. • 43 cases with single dose (ofloxacin 200mg iv) vs. 38 cases with standard tx (ofloxacin 400mg iv per day) till catheter removal. • 19 (23%)patients had positive stone culture. • Post fever: 9/43 (21%) and 8/38 (21%). • The febrile patients had longer operations with the use of more irrigation fluid and longer postoperative hospital stays. • Short-term prophylaxis has no advantage over singledose prophylaxis. • Dogan HS, et al. J Enodourol 2002;16:649-53. PCNL (A) No pyuria、APN or UTI 49 % 48 % N=69 41 % 50% pr e-op Rat e Post -op Rat e 45% 40% 32 35% Antibiotic use % 30% 25% 13 20% % 7% 15% 1% 10% 5% 0% 1% 1% N o ant i bi ot i c use 1 t h l i ne cephal 1 . 0 gm 1 t h l i ne am i no Com bi ne w i t h cephal + am i no O t her s : 13% 49% 1% 32% 1% 7% 48% 1% 41% 3% pr e-op Rat e Post -op Rat e 70% 62 % 3% antibiotic dose 60% 50% 36% 40% 30% 30% 19 20% % 13% 13 6% 10% 0% 0% 3% 0% 1% 6% 0% 0% 0% 0% pr e-op Rat e Post -op Rat e 1 dose 1 day 62% 19% 0% 30% % 7% 3% 3 days 5 days 7 days 1 4 days m i ssi ng answ er no r equest 0% 3% 0% 0% 0% 3% 13% 13% 36% 1% 6% 0% 6% 7% 2 days Discussion on Prophylactic Antibiotics in PCNL without signs of preoperative infection • 81% use pre-op antibiotics, and of them 41% use combination therapy. • 79% use short course (1-3 days) post op antibiotics. • Few cases of staghorn stone had sterile urine. • Renal function impairment is common in these cases. • More studies are needed to confirm the adequacy of single dose prophylaxis. Prophylaxis for TURP Regulations : short course, 1-3 days?. • EAU guideline: all patients. • Campbell: all patients till catheter removal. • Taiwan guideline for TUR BT: cefazoline 1.0 gm IV at induction. Antimicrobial Prophylaxis for TURP • A meta analysis of 32 RCT showed that a risk reduction in bacteriuria from 26% to 9%. Septicemia from 4.4% to 0.9%. • FluoroQ, aminoglycosides, TMP/SMX , Cephalosporines. Used for a short course (2-5 days), or while catheter remained in place. • Failure to eradicate bacteriuria resulted in bactereuria in 50% of patients (Morris 1976). TURP N=69 Antibiotic use 59% 60% pr e-op Rat e Post -op Rat e 49% 50% 40% 26% 30% 16% 17% 20% 10% 9% 10% 4% 0% 0% 0% N o ant i b i o t i c use 1 t h l i ne cephal 1 . 0 gm 1 t h l i ne am i no Co m b i ne w i t h cephal + am i no O t her s : pr e-o p Rat e 16% 59% 0% 17% 4% Po st -o p Rat e 10% 49% 0% 26% 9% 70% 68 % Antibiotic dose 60% 50% 40% 29 % 25 % 30% 20% 14 % 9% 10% 3% 6% 0% 1% 0% 1% 0% 4% Post -op Rat e 14 % 9% 0% 0% pre-op Rat e 10 % 6% 1 dose 1 day 2 days 3 days 5 days 7 days 1 4 days mi ssi ng answ er no request 68% 6% 0% 1% 0% 0% 0% 10% 14% 3% 29% 14% 25% 1% 4% 9% 6% 9% Discussion on Prophylactic Antibiotics in TURP • 16% did not use AMP: no complying to guidelines. • 17%-26% use combination therapy: abuse? • 14% use antibiotics longer than 3 days: break the rule? Infection: War Between Host and Bacteria Host Defense Proper AMP Proper Disinfection decrease Impaired Immune system, or anatomaica factors Urological Intervention Dirty instrument Bacterial Virulence increase Abuse of Antibiotics The Host: SSI in the Elderly Population • Kaye KS, et al: CID 2004;39:1835-41. A review. • THE RISK OF SSI DOES NOT SEEM TO INCREASE AFTER THE AGE OF 65 YEARS. • More co-morbidity in the elder patients. • Independent risk factors of SSI: obesity, COPD, contaminated or dirty wound. • Protective factor: private insurance. (MONEY MATTERS) • Sharing the same clinical presentation of infection and the pathogens that cause infection. • However, the mortality rate, the duration of hospitalization, and the costs associated with hospital care are greater for elderly patients with SSI than for younger patients with SSI. Obese Patients Run Higher Risk of Postoperative Complications • Bamgbade OA, et al: World J Surg 2007 (3) • Analyze 6773 patients. 2217 were obese, including 993 morbid obesity. • Heart attack rate 0.5% vs. 0.1%. • Wound infection 6% vs. 3.5%. • Peripheral nerve injury 0.4% vs. 0.15. • UTI 3.9% vs. 2.6%. • Death rate: 2.2% vs. 1.2%. • Suggestions: Morbid obesity patient have outpatient surgery should undergo a 23-hour hospital stay for post-op monitoring. ‘Complicated' UTIs: They are not standard patients! • Foreign bodies in the urinary tract, such as indwelling urinary catheters and stents; • Increased postvoiding residual urine >=100 mL • urinary tract stones • congenital developmental or anatomic anomalies; • obstructive uropathy (eg, as a result of stones, fibrosis, or bladder outlet obstruction); • vesicoureteric reflux, or structural urologic abnormalities, including surgically created structural changes, such as ileal loops; • neurogenic bladder disorder (with residual urine and/or overactive detrusor) • uremia from renal causes; and • renal transplantation. Proper Disinfection General measures recommended for prevention of surgical infections • Bathing patients preoperatively with an antimicrobial soap has been suggested as a preventive strategy. Proper vaginal disinfection. • Preoperative removal of hair from the operative site by clipping rather than by shaving, reduces the overall incidence of SSI and should minimize the risk of S. aureus infection. • Adequate Scrubbing of surgeons’ and all assistants’ hands before the procedure. Inappropriate Disinfection of Endoscope • Painful experiences in TCH, Taipei, Taiwan. • Cluster infection in patients after prostate biopsy in 2005. • Cluster infections in patients after USL in 2006. • All were pseudomonas infection. • Reluctant to report! A war between Urologists and OR nurses? A punishment form superior? Local Bacterial Resistance!!! Susceptibility of Isolates in TCH, Taipei Ampic Amox Cefaz illin +clavu oline Genta micin Ciprox Levofl Ceftria Vanco in oxacin xone mycin E- Coli 25 44 75 73 70 75 87 - Paerugi nosa - - 83 76 73 - - Kpneu monia e 0 78 82 81 86 86 88 - S aureu s - - - 55 59 66 - 100 - - - - - - 100 E 96 faecali s Proper AMP Timing of Antibiotics • Parental agents: 30-60 minutes IV at induction of anesthesia. • Oral agents: 2 hours before operation. • Additional dose in prolonged operation. E.g. >3-4 hours. Monotherapy Versus Combination Therapy • Most UTIs can be treated with monotherapy. • Some complicated infections, especially CAUTI, may have a polymicrobial etiology, in which case multiple antibiotics may be needed. Combination therapy is often used (eg, ampicillin is often combined with gentamicin), but there is little evidence that such combination therapy is more effective than monotherapy in most cases. • Note: Taiwanese doctors tend to combine cefalosporines with aminoglycosides. Oral Versus Intravenous Administration • Most uncomplicated UTIs, and many complicated infections can be treated adequately with oral therapy. (Equally effective?!!) • Generally, intravenous therapy would be indicated in seriously ill patients with complicated UTIs; and patients with pyelonephritis at risk. Surgery and Cephalosporines: A Marriage Made In Heaven Or Time For Divorce • Morgan M. Internet J Surg. 2006; 8(1) • Cephalosporines are ineffective against the common pathogens causing SSI and are associated with superinfection. • In UK, 47% of microorganism identified as causing SSIs were staphylococci, of which 82% were Staph aureus. 62% Staph aureus were MRSA. • Enterococcal infections (predominantly UTI and enodcarditis) are on the increase, and this may well be due to overuse of the cephalosporines. Proactive Monitoring to Decrease SSI • Dellinger EP, et al. Am J Surg 2005;190:9-15. • 56 hosptials and 42 quality-improvement organizations form 50 states or territories in the USA agreed to participate. • Administration of the prophylactic antibiotic prior to incision increased from 72% to 92%. • Antibiotic prophylaxis was discontinued within 24 h increased from 67% to 85%. • The overall SSI decreased from 2.28% in the first 3 months of the study to 1.65% in the last 3 months. • Examine our results and Change our practice. • May we all have reduced SSI in enodurological surgeries! Gaps Between Practice and Regulations/Guidelines (I) • Controversy exists between different guidelines. • The guidelines were conducted by experts and based on published results that may be the best clinical results, and that may be not true for average doctors. • Regulations were made for financial causes rather than scientific evidence. • Regulations/Guidelines may be out of date. • Urologists were not involved in making up the Guidelines. Gaps Between Practice and Regulations/Guidelines (II) • Details or variations of each procedure were not discussed yet! • Invasiveness of the procedure was less discussed in the guidelines. • Serious infection did occur! (Strong and permanent memory to use more antibiotics). Gaps Between Practice and Regulations/Guidelines (III) • High Drug resistance in local community. • Surgeons Do not trust the disinfection procedures. Too many points to miss! • Surgeons’ heavy duty to kill any pathogens entering the patients. Safety for the patients? • Afraid of law suing? Safety for the doctors: overuse of antibiotics to prevent minor infections. Fill the Gap and Become A HUMANE DOCTOR 志為人醫 Welcome to Taipei, Taiwan 11th WPCCID and 5th AAUS! November 29 ~ December 03, 2008 歡 迎 蒞 臨 台 北 E-mail: wpccid2008@ elitepco.com. tw Deadline for Abstract Submission: June 30, 2008 Sat. Nov.29 Sun. Nov.30 07:00-08:30 Mon. Dec.1 Tue. Dec.2 Meet the Experts Meet the Experts Wed. Dec.3 08:30-09:15 Keynote 2 Keynote 3 Keynote 4 Keynote 5 09:15-10:00 Plenary 1-4 Plenary 9-12 Plenary 17-20 Plenary 25-28 10:00-10:30 Break Break Break Break Symposium 1-4 Symposium 9-12 Symposium 17-20 Symposium 2528 Satellite Symposium & Lunch 1-2 Satellite Symposium & Lunch 5-6 Satellite Symposium & Lunch 9-10 12:00-12:30 Closing Ceremony 13:30-14:30 Poster Session Poster Session Poster Session 14:30-15:00 Plenary 5-8 Plenary 13-16 Plenary 21-24 15:00-15:30 Break Break Break Symposium 5-8 Symposium 13-16 Symposium 21-24 10:30-12:00 12:00-13:30 4th Annual Meeting of GCAMID 15:30-17:00 City Tour 17:30-18:00 18:00-19:00 19:00-19:30 Registration (08:30-18:00) Satellite Satellite Symposium Symposiu GCAMID 3-4 m & Dinner Forum 7-8 Opening Ceremony & Keynote 1 Congress Banquet 19:30-21:00 Satellite Symposium 11-12 Welcome Reception GCAMID Gala Dinner Farewell Party (WPSC) Asian Association of UTI and STD (AAUS) in conjunction with 5th Asian UTI/STD Forum (AAUS 2008) Ms. Emily Shih Address: 10F-2, No. 51, Sungjiung Road, 104 Taipei, Taiwan Tel: +886-2-2504-4338 ext.18 Fax: +886-22504-4362 E-mail: [email protected] Important Dates Deadline for Abstract Submission: June 30, 2008 Deadline for Early Bird Registration: August 31, 2008 Deadline for Pre-Registration: September 15, 2008 Congress Dates: November 29 ~ December 03, 2008 Congress Secretariat Antimicrobial Prophylaxis for Clean Wound Surgery: Kaoshiung VGH • In 1999~2000, 3110 surgical cases. • 156 (2%) cases did not use antibiotics at all. • Mean antibiotic days: 6.39 days (parental 2.41days and oral 4.02 days). • SSI rate in clean surgery: one dose of AMP: 0.9%, one dose after surgery: 3.2%, no use : 1.9%. • 90% use 1st Cepha as AMP, and 50% aminoglycosides. • Conclusion: one dose of AMP is enough and better than no use of AMP. • Ho M: My route to education and medicine. 2002. Back to ER rate N Prophylactic Group Therapeutic Group No Preop data ER UTI Pain 62 2 (3.2%) 4 (6.4%) 57 1 (1.8%) 1 (1.8%) 8 1 (12.5%) 2 (25%) Correctable Urologic Abnormalities That Cause Bacterial Persistence Infection stones • • • • • • • • • • • • Infection stones Chronic bacterial prostatitis Unilateral infected atrophic kidneys Ureteral duplication and ectopic ureters Foreign bodies Urethral diverticula and infected periurethral glands Unilateral medullary sponge kidneys Nonrefluxing, normal-appearing, infected ureteral stumps after nephrectomy Infected urachal cysts Infected communicating cysts of the renal calyces Papillary necrosis Perivesical abscess with fistula to bladder Guidelines for the use of prophylatctic antibiotics in surgery in Taiwan Site/procedu Likely re pathogens Recommended antibiotics Alternative Herniorraphy S. aureus + mesh, open CoNS or LPS Cephazolin 1gm, IV at IA Clindamycin 1 dose 600mg IV at IA Herniorraphy No mesh, open or LPS Nil or Cephazolin 1gm, IV at IA Clindamycin 1 dose 600mg IV at IA Oral Neomcin 1gm QID+ metronidazole 1gm qid the day before op or cefa+/- GM +/metron IV at IA Clindamycin +GM IV at IA. Or … or … S. aureus CoNS Colorectal Enteric ( clean GNB contaminated) Anaerobes Duration <1 day J Microbiol Immunol Infect 2004;37:71-4 Guidelines for Antimicrobial Therapy of UTIs in Taiwan Alternative Choice Diagnosis Drug of Choice Asymptomatic bacteriuria or Acute bacterial cystitis Nitrofurantoin, Ampicillin or amoxicillin 1st or 2nd cepha, Ampicillin/sulbactam TMP+SMX Amoxicillin/calvulanate Quinolones (pimpemic acid, etc) NO FLUOROQUINOLONES Acute uncomplicated Pyelonephritis TMP+SMX 1st or 2nd cephalo Aminoglycosides NO FLUOROQUINOLONES Ampicillin or amoxicillin Ampicillin/sulbactam Amoxicillin/calvulanate Aminoglycosides (single) + 1st or 2nd cepha, • J Microbiol Immunol Infect 2000;33:271-2. Discussion: Prophylactic Antibiotics in TURP • 16% did not use AMP (Did not comply to guidelines) • 14% use postop ABx longer than 3 days. (Break the rule!) • More use of combination antibiotics (preop. 17%, and postop.26%). (Cefazoline plus Gentamycin). Prophylaxis for Nephrectomy Regulations for : 0-1 dose 1st line antibotics? • EAU guideline: • Campbell-Walsh 2007: • Taiwan: single dose or short course, 13 days?. Clean wound after op for RCC. Clean contaminated wound after op for TCC. Open or Laparoscopic Nephrectomy/Nephrourerectomy • In general, LPS procedures lowers the risk of surgical site infections. (Kluytmans, 1997) • Regarded as clean wound. • Entry into urinary tract clean contaminated wound. prophylaxis with 1st gen. Cephalosporines. For 1-3 days. • Using bowel neomycin + erythromycin or neomycin +metronidazole 18-24 hrs before op. and parental cefotetan or cefoxitin 30-60 min before incision. Bacteria of preoperative urinary tract infections contaminate the surgical field and develop surgical site infections in urological operations. • • • • • • Hamsuna R, et al: Int J Urol 2004;11:941-7 134 major open urological operations. Surgical wound swab cuture at the end of op: AMP after op and lasting for 3 days. 34 (25%) infectious complications.(SSI and UTI, etc) Of 20 SSI (+), 15 (75%) had swab culture (+) and the bacteria was sensitive to AMP in 20%. • Of 114 SSI (-), 14 (12%) had swab culture (+) and the bacteria was sensitive to AMP in 86%. • Preop UTI was observed in 11 (55%) patients with SSI.Of them 4 had same species in urine and wound. • Conclusions: preop UTI was the most important risk factor for SSI following urological op. Open nephrectomy- N=69 Antibiotic use 67 % pr e-op Rat e Post -op Rat e 70% 52 % 60% 50% 40% 29 % 30% 13 % 20% 13 % 10 % 0% 10% 0% 3% 1% 0% N o ant i bi ot i c use 1 t h l i ne cephal 1 . 0 gm 1 t h l i ne am i no Com bi ne w i t h cephal + am i no O t her s : pr e-op Rat e 13% 67% 0% 13% 1% Post -op Rat e 10% 52% 0% 29% 3% 80 % 80% Antibiotic dose 70% 60% 53 % 50% 40% 30% 20% 12 % 10% % 0% 3 9% 0% 0% 1 dose pr e-op Rat e Post -op Rat e 6% 0% 0% 0% 3% % 0% 3 4% % 4 13 % 10 % 3 days 5 days 7 days 1 4 days m i ssi ng answ er no r equest 0% 0% 0% 0% 0% 4% 13% 9% 53% 6% 3% 3% 4% 10% 1 day 2 days 80% 3% 0% 12% Hand -assisted Laparoscopic nephrectomy 54 % 60% 52 pr e-op Rat e Post -op Rat e % N=69 50% Antibiotic use 40% 30% 22 12 % 20% 13 % 6% 10% 0% pr e-op Rat e % 0% 0% 0% N o ant i bi ot i c use 1 t h l i ne cephal 1 . 0 gm 1 t h l i ne am i no Com bi ne w i t h cephal + am i no O t her s : 12% 54% 0% 13% 0% 6% 52% 0% 22% 0% Post -op Rat e 0% 70% 61 % 60% 50% Antibiotic dose 39 % 40% 30% % 22 23 % 20% 13 % 12 % 12 6% 10% 0% 0% 0% 0% 3% 0% 1 dose pr e-op Rat e Post -op Rat e 1 day 2 days 0% 1% 0% % 6% 3% 3 days 5 days 7 days 1 4 days m i ssi ng answ er no r equest 61% 6% 0% 0% 0% 0% 0% 22% 12% 0% 13% 12% 39% 3% 1% 3% 23% 6% Discussion: Prophylactic Antibiotics in Open Nephrectomy • 12% did not use preop. ABx. (Not complying to guidline) • 58%-74% use postop ABx longer than 1 day. (Break the rule!) • More use of Two kinds of antibiotics (preop. 13%, and postop.22%-29%) (Break the rule!) • The rate of using antibiotics was less in LPS nephrectomy. • But this is a clean op!! What are urologists afraid of? Invasiveness of the procedure and possible major adverse events after op. Bacterial Virulence Reliable Coverage of Antimicrobials Antimicrobial or Antimicrobial Class Gram-Positive Pathogens Gram-Negative Pathogens Amoxicillin or ampicillin Streptococcus Enterococci Escherichia coli Proteus mirabilis Amoxicillin with clavulanate Streptococcus E. coli Ampicillin with sulbactam Staphylococcus (not MRSA) Enterococci P. mirabilis Haemophilus influenzae, Klebsiella species First-generation cephalosporins Streptococcus Staphylococc us (not MRSA) E. coli P. mirabilis Klebsiella species Second-generation cephalosporins (cefamandole, cefuroxime, cefaclor) Streptococcus Staphylococc us (not MRSA) E. coli, P. mirabilis H. influenzae, Klebsiella species Second-generation cephalosporins (cefoxitin, cefotetan) Streptococcus E. coli, Proteus species (including indole +) H. influenzae, Klebsiella species Third-generation cephalosporins (ceftazidime, ceftriaxone) Streptococcus Most, including P. aeruginosa Aminoglycosides Staphylococcus (urine) Most, including P. aeruginosa Fluoroquinolones Streptococcus * Most, including P. aeruginosa Gap Between Regulations/ Guidelines and Practice on AMP for Herniorraphy • Surgeons’ heavy duty? Safety for the patients or for the doctors? Empiric use of antibiotics to kill any pathogen that may enter through the open wound. • Personal experience is not so good as the published reports and Severe mesh infection did occur. Are we afraid of legal problem? • Selection of standard patients: Good results of Shouldice repair come from good selection of patients Cephalosporin resistant urinary tract infections in young children • Mehr SS, et al: J Paediatr Child Health 2004;40:48-52. (Melbourne, Australia) • • • • <6 y/o 100 culture proved UTI. E coli 90%. Proteus mirabilis 5%. In vitro resistance to Ampicillin/amoxicillin: 52%, to TMP 14%, to cephalothin/cephalexin 24%. • High resistance to TMP in Taiwan!! Once Daily vs. Conventional use of Gentamicin Emergence of Reduced Sucsceptibility and Resistance to F-Quinolones in E Coli • Taiwan had been ‘famous’ as one of the countries with highest resistant bacteria. • In 1998, 1203 E coli isolates from 44 hospitals in Taiwan. • 136 (11.3%) isolates were resistant to F-Q. and another 261 (21.7%) had reduced susceptibility. • Acute and chronic quinolone use in cancer patients is a major selective pressure for resistance. • McDonald LC, et al: Antimicrobial agents and chemotherapy 2001;45:3084-91. Taiwan Surveillance On Antimicromial Resistance: Use of Antibiotics in Hospitals • 6 medical centers + 8 regional hospitals • 663 adult inpatients in early 1999. • A total of 447 (67%) patients received antibiotics for an overall rate of 813 antibiotic days per 1000 hospital days. • Reasons to use antibiotics: 36% by experience, 29% by culture, and 30% for prophylaxis for SSI. • Medical center was an independent predictor for increased use of antibiotics. • McDonald LC, et al: Infection Control & Hospital Epidemiology 2001;22:565-71. Taiwan Surveillance of Antimicromial Resistance in Taiwan: Bacteria • 1st Cephalosporines were the most frequent (50%) prescribed antibiotics (Data from NHI). • In 22 hospitals, The most common isolates were Enterobacteriaceae (E coli, K pneuomniae), S aureus, P aeruginosa. Accinobacter spp accounted for 10% isolates. • MRSA accounts for 82% of hospital acquired infection, and . 40% of community acquired infection. • Ho M, et al: J Microbio Immuno Infect 1999;32:239-49. Lessons from clean wound surgery Prophylaxis for Herniorraphy Regulations: 0-1 dose Guidelines for the use of prophylatctic antibiotics in Herniorraphy in Taiwan Site/proced ure Likely Recommended pathogens antibiotics Alternative Duration Mesh +, open or LPS No mesh, open or LPS S. aureus CoNS Cephazolin 1gm, Clindamycin IV at IA 600mg IV at IA 1 dose S. aureus CoNS Nil or Clindamycin Cephazolin 1gm, 600mg IV at IV at IA IA 1 dose J Microbiol Immunol Infect 2004;37:71-4 Prophylactic Antibiotics for mesh ingunal hernioplasty: a meta-analysis Terzi C, J Hosp Infect. 2006 Jan. meta-analysis: the value of prophylaxis on heriorraphy is inconclusive • Sanabria A, et al: Ann Surg 2007;245:392-6 • 6 RCT, 2507 eligible patients. • Antibiotic prophylaxis use in patients submitted to mesh inguinal hernioplasty decreased the rate of SSI by almost 50%. (2.89% 1.38%) •Tzovaras G, et al: Int J ClinPract 2007;61:236-9: No effectiveness of prophylactic antibiotics for tension-free mesh hernia repair. (amoxicillin + clavoulani acid vs. placebo. 4.2% vs. 5.8%. SSI in Inguinal Herniorraphy, TCH, Taipei (2005-2006) *All men had preoperative antibiotics, including 10 boys less than 18years. *54 (69.2%) cases used post op antibiotics. (Breaking regulations) *56 Mesh (+) cases. one (1.78%) had SSI. *22 Mesh (-) cases. None had SSI. *The only one SSI occurred in the mesh (+) patient who took post op antibiotics. *Conclusions: post op antibiotics is not necessary in herniorraphy. Hernia N=69 Antibiotic use 65% 70% pr e-op Rat e Post -op Rat e 54% 60% 50% 40% 35% 25% 30% 20% 7% 6% 10% 0% 0% 0% 0% 0% N o ant i b i o t i c use 1 t h l i ne cephal 1 . 0 gm 1 t h l i ne am i no Co m b i ne w i t h cephal + am i no O t her s : pr e-o p Rat e 35% 54% 0% 6% 0% Po st -o p Rat e 65% 25% 0% 0% 7% 70% 60% 65 % Antibiotic dose 57 % 50% 40% 35 % 30% 20% 16 % 10 % 10% 4% 4% 3% 0% 0% 0% 0% 0% 1% 4% % % 0 0 0% 0% 1 dose 1 day 2 days 3 days 5 days 7 days 1 4 days mi ssi ng answ er no request pre-op Rat e 57% 4% 0% 0% 0% 0% 0% 4% 35% Post -op Rat e 10% 4% 3% 16% 0% 1% 0% 0% 65% Discussions: AMP for Hernia Repair • Regulations and Guidelines: No antibiotics for repair without mesh. One dose for repair with mesh. • Evidence: published reports on SSI rates after Inguinal hernia repair were around 2%, mostly skin infection. • Mesh infection 0.9% in one report. (Jezupovs A, Mihelsons M: World J Surg 2006;30:2270-8) • Our SSI rate after Mesh free repair was 0%, while that after mesh repair was 1.8%. • Practice: 57% Taiwanese urologists followed the regulation. While 16% urologists used postoperative antibiotics for 3 days (much lower than 70% in 1990s) and 70% of cases in our hospital did not follow the regulations. (Better figures than that in 2000) Lessons learned: Identifying Patients at risk of SSI in Herniorraphy • Old age (>65 yrs or >75 yrs) (Chronological age vs. Biological Age) • Obesity • Urinary catheterization. • Previous herniorraphy • Lengthy op time • DM • COPD. • Other factors to decrease host immunity?