* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Thermoregulation and Heart Rate Variability
Survey
Document related concepts
Transcript
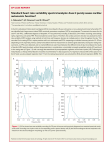
Clinical Science (1996) 90. 97-103 (Printed in Great Britain) 97 Thermoregulation and heart rate variability Lee A. FLEISHER, Steven M. FRANK, Daniel I. SESSLER, Christi CHENG, Takashi MATSUKAWA and Carole A. VANNIER Departments of Anaesthesiology and Critical Care Medicine and Medicine, Johns Hopkins University School of Medicine, Baltimore, Maryland, U.S.A., and the Thermoregulation Research Laboratory, Department of Anaesthesia, University of California, San Francisco, U.S.A. (Received 10 Augustfl8 October 1995; accepted 24 October 1995) 1. Heart rate variability is modulated by multiple control systems, including autonomic and hormonal systems. Long-term variability, Le, the very lowfrequency band of the power spectra, has been postulated to reflect thermoregulatory vasomotor control, based upon thermal entrainment experiments. However, the relationship between thermoregulatory responses (vasoconstriction and shivering) and heart rate variability has not been studied. 2. We performed two distinct protocols in a series of human subjects. In the first protocol, core temperature was reduced by intravenous infusion of cold saline, while skin temperature was unchanged. The second protocol involved skin-surface warming and cooling until shivering developed. Power spectral analysis was performed using a fast Fourier transformation, and the area in three distinct band-widths was determined. 3. Very low-frequency power (0.0039-0.04 Hz) increased significantly in response to core cooling, peripheral vasoconstriction and sbivering, wbile botb very low- and low- (0.04-0.15 Hz) frequency power increased in response to skin-surface cooling. Heart rate decreased during core cooling-induced vasoconstriction, suggesting a direct tbermal response, and increased in relation to the metabolic demands associated with shivering. 4. Our results suggest tbat very low-frequency power is modulated by tbermal stimuli wbicb result in core hypothermia and thermoregulatory activity, wbile skin-surface cooling witbout core bypothermia does not selectively modulate this frequency band. INTRODUCTION Heart rate is controlled by the interaction of multiple homoeostatic mechanisms [1-3]. The presence of beat-to-beat or heart rate variability (HRV) has been associated with cardiovascular health [4]. In contrast, lack of variability has been associated with morbid events [5-7]. Heart rate pattern can be evaluated. by multiple methods, including the use of Fourier analysis, and three distinct frequency bands can be recognized: (i) the high-frequency peak, centred around 0.2 Hz, (ii) the low-frequency peak, centred around 0.1 Hz, and (iii) the very low-frequency band, described as the power between 0.0039 and 0.04 Hz [5]. Several investigators have proposed that discrete frequency components of HRV correlate with different components of the autonomic nervous system [2, 3, 8]. In general, short-term HRV (high frequency) is thought to be controlled by the parasympathetic nervous system, while intermediate variability (low frequency) is under the control of the sympathetic and parasympathetic systems, and may reflect the activity of Mayer waves [2]. The ratio of low/highfrequency power has been proposed as a measure of sympathovagal balance [9]. Control of long-term variability (very low frequency) is less well described, but is thought to reflect an interaction of the renin-angiotensin system and thermoregulatory vasomotor control [8, 10-12] The physiological importance of the very lowfrequency range remains unclear. The natural contractile oscillations of the smooth muscle of the peripheral vascular bed undergo spontaneous fluctuations with a periodicity of 10s [13]. It has been demonstrated that the oscillations of cutaneous blood flow can be synchronized to skin or vascular blood temperature. Kitney and co-workers [II, 12, 14] demonstrated thermal entrainment of the very low-frequency power of both blood pressure and HR V to the frequency of alteration of a subject's hand in warm and cold water baths. However, the hypothesis that thermal synchronization of blood flow and heart rate occurs with oscillation of cutaneous skin temperature has not been uniformly accepted [15]. Additionally, thermal entrainment. at frequencies between 0.01 and 0.1 Hz (encompassmg both the very low- and low-frequency band) predominantly increased the 0.10 Hz periodic HRV; however, the 0.01-0.12 Hz frequency band oscillations did not increase significantly [16]. Therefore, the basis for a thermoregulatory component to the very low-frequency HRV power remains controversial. Key words: electrocardiography, heart rate variability. hypothermia. measurement, spectral analysis. thermoregulation. Abbreviation: HRV, heart rate variability. Correspondence: Dr L. A. Fleisher. The Johns Hopkins Hospital. 600 N. Wolfe Street, Carnegie ....2 Baltimore. MD 21287, U.S.A. 98 L. A. Fleisher et 31. Although the above studies evaluated the effect of external temperature entrainment on HRV, no study directly evaluated the relationship of HRV to activation of thermoregulatory responses. We hypothesized that if thermoregulation was related to the very low-frequency component of HRV then it would be related to thermoregulatory vasoconstriction during core hypothermia and not to peripheral cold stimulus, which has a much less significant effect on thermoregulation [17]. To determine the influence of thermoregulation on HRV, we studied human volunteers subjected to different types of cold challenge. These stimuli included the effects of two methods of systemic warming and cooling sufficient to provoke sweating, vasoconstriction and shivering. METHODS AND MATERIALS Volunteers were studied under two circumstances, as part of a larger study of anaesthetics and thermoregulatory changes [17]. The first protocol reduced core temperature while maintaining constant skin temperatures, while the second reduced both skin and core temperatures. Since respiratory rate can affect the frequency of the 'parasympathetic' band, as well as influence the power in all frequency bands, we measured respiratory rate in order to ensure that it was greater than 12 breaths/min in all protocols [18]. Protocol I: core cooling With approval from the Committee on Human Research at the University of California, San Francisco, we studied six male volunteers between the ages of 25 and 35 years. These volunteers were not conditioned athletes. None was obese, taking medication or had a history of thyroid disease. The volunteers were advised to eat lightly before arriving at the laboratory. They were minimally clothed during the protocol and rested supine on a standard operating room table. A 16-g catheter was inserted into the superior vena cava via the right internal jugular vein. A circulating-water mattress and forced-air cover were used to maintain skin temperature (weighted average of 15 sites) between 32 and 34C. However, mean skin temperature in individual volunteers was nearly constant throughout the study. Volunteers were then cooled by central venous infusion of lactated Ringer's solution at 3°e, as previously described [19, 20]. The solution was cooled by passing it through an aluminium cardiopulmonary bypass heat exchanger immersed in an ice-and-water slurry. The rate of infusion was initially 10 ml/rnin and was adjusted at I-min intervals to maintain a core cooling rate near 1.6'C/h. Core cooling was continued until sustained shivering was identified (approximately 1.5-2.51). Respira- tory rate did not significantly change during the course of the study. Protocol 2: skin surface cooling With approval from the Committee on Human Research at the University of California, San Francisco, five male volunteers were studied. As in protocol I, these volunteers were not conditioned athletes. None was obese, taking medication or had a history of thyroid disease. The volunteers were advised to eat lightly before arriving at the laboratory. They were minimally clothed during the protocol and rested supine on a standard operating room table. Mean skin temperature was initially increased to 37°C by a circulatingwater mattress and forced-air warmer. After sweating was observed, the temperature of the circulatingwater mattress and forced-air cover was gradually decreased until vasoconstriction and then shivering were triggered. Respiratory rate did not significantly change during the course of the study Measurements (for both protocols) Core temperature was measured in the distal oesophagus using disposable Mon-a-Therm thermocouple probes (Mallinckrodt Medical, Inc., St Louis, MO, U.S.A.). Optimal insertion length of the oesophageal probe was calculated using the formula of Mekjavic and Rempel [21]. The aural probes were inserted by the volunteers until they felt the thermocouple touch the tympanic membrane; appropriate placement was confirmed when the volunteers easily detected a gentle rubbing of the attached wire. The probe was then securely taped in place, the aural canal occluded with cotton and a gauze bandage positioned over the external ear. We have previously demonstrated that distal oesophageal and tympanic membrane temperatures are virtually identical under the circumstances of this study [22]. Sweating was continuously quantified on the left upper chest using a ventilated capsule. A sustained sweating > 40 g h ~ 1 m ~ 2 was considered significant. Vasoconstriction was monitored using forearm minus fingertip skin-temperature gradients. This measure correlates well with absolute finger blood flow as determined by volume plethysmography [23]. As in previous investigations, a gradient exceeding 4"C identified significant vasoconstriction [23, 24] Shivering was evaluated using oxygen consumption (Deltatrac; SensorMedics Corp., Yorba Linda, CA, U.S.A.). The system was used in canopy-mode, and measurements were averaged over I-min intervals and recorded every 5 min. A sustained 30% increase in oxygen consumption identified significant shivering; this increase was identified by an observer blinded to treatment, as well as core and skin temperatures. The core temperatures triggering sig- Thermoregulation and R-R variability nificant sweating, vasoconstriction and shivering identified the thresholds for each response. Power spectral analysis VO.lunteers were monitored by a calibrated amplitude-modulated AECG monitor (SpaceLabs ambulatory ECG model 90205. Redmond, WA, U.S.A.) with modified bipolar lead V5 and modified bipolar lead VI or V3. The AECG recordings were analysed at the end of the monitoring period using lead V5 on a computerized analysis system (SpaceLabs FT3000a). The peak of the QRS was identified for each beat by a computer algorithm and beat identification was confirmed by an investigator, Those periods in which beat identification was poor were excluded from the analysis. Hour-long files containing successive R-R intervals were created. Shiver~ng did not interfere with the ability of the analysis system to accurately identify the QRS peak and determine R-R interval length. The power spectral density for representative R-R in~erval series was determined by investigators blinded to temperature. A series of R-R intervals were reviewed visually for R-wave determination and ectopic beats. Each series contained fewer than five ectopic beats. The intervals surrounding ectopic beats were removed and the average R-R interval for the previous three beats was inserted to eliminate the effects of ectopy on the Fourier transformation. The method of analysis of the power spectrum was adapted from Berger et al. [25]. Initially, the time series of interest was reviewed to ensure stationariness. Fourier time-series analysis requires evenly spaced values. Therefore, the R-R interval data were plotted as a function of length in milliseconds and resampled at 4 Hz (using a cubic spline function) to obtain an evenly spaced series of 4 min of instantaneous heart rates (four instantaneous heart rates per second). The mean heart rate was then subtracted and a Hanning window was applied. Po.wer spectral density plots were obtained by plotting the square of the amplitude of the fast Fourier transformation of the time series against frequency (Hz) for both 4 and 15min datasets during a 15min steady-state period of core temperature and after each of the thresholds of sweating, shivering and vasoconstriction were reached (SpaceLabs FT3000a analysis system and MatLab 4.0 for Macintosh). Power (ms 2/band-width) in high frequency (0.125-0.5 Hz) and low frequency (0.05-0.125 Hz) was determined by integrating the area under the power spectral density plots for the initial 4min-long datasets for each study period. Power in the very low-frequency (0.0039-0.05 Hz) band was determined by integrating the area under the power spectral density plots for the 15-min-long datasets for protocols I and 2, since analysis of very lowfrequency power requires longer datasets. The coeffi- dent lated since HRV 99 of variance for each 15min series was calcuby dividing the SD by the mean R-R interval it has been suggested as a means of assessing independent of heart rate. Statistical analysis The results of core temperature, heart rate and of HRV are expressed as meant SEM . .olfferenc~s over time were determined using analysis of vanance for repeated measures with P <0.05 considered significant (SuperAnova v1.11, Abacus Concepts). Differences between two time pe~iods within. one group were compared using a paired t-test WIth P < 0.05 considered significant. measure~ents RESULTS Protocol I: core cooling The core temperature thresholds for vasoconstriction and shivering were 36.6 ± 0.2°C and 36.1 ± 0.1DC, respectively (Fig. 1). Heart rate was 67 ± 3 beats/min at baseline, decreased significantly with vasoconstriction (63 ± 3 beats/min, P < 0.01) and then increased significantly over baseline with the onset of shivering (72 ± 4 beats/min, P < 0.05). The coefficient of variance was 0.074+0.008 at baseline, 0.089 ± 0.009 with vasoconstriction and ~.126±0.013 with shivering and significantly increased overall (P < 0.05). However, it did not significantly increase between each temperature phase, i.e. from baseline to vasoconstriction or vasoconstriction to shivering. Very low-frequ~ncy power increased significantly at the time vasoconstricti?n .occurred (P < 0.05), and was higher w~en shivering was observed (P not significant) (FIg. 2). Low-frequency power remained unchanged with vasoconstriction and increased nonsignificantly with shivering (P = 0.13). Highfrequency power remained relatively constant over the temperature ranges evaluated in the protocol. The ratio of low/high-frequency power was unchanged with vasoconstriction and increased with borderline significance with shivering (P = 0.055) (Fig. 3). When the time series were evaluated, long duration oscillations (2 min) were greater during vasoconstriction (Fig. 4). Protocol 2: skin-surface cooling Sweating occurred when body temperature increased O.5°C from baseline values. Thermoregulatory vasoconstriction occurred at a core temperature of 37.1 ±O.I°C and skin temperature of 33.0±0.4°C (Fig. 1). Shivering occurred at a core temperature of 37.1 ± 0.1°C and skin temperature of 29.9 ±0.4°C. Heart rate was 68 ±7 beats/min at baseline, increased to 78 ± 7 beats/min with sweating and returned to near-baseline with vasoconstriction L. A. Fleisher et al. 100 38~ (a) 37 36 ~ II ~7000 a E ~6000 ~ I U 35 ::0 0000 Core temperature &.5000 t;5-4000 ].4 ~a. 33 ~32 f3000 .22000 t- ~ 1000 31 0 0000 30 -.....,r-------r-----""T"'-- 29..... 8aseline Vasoconstriction Shivering N' 38 (b) Core temperature 37 36 ~ 35 7000 . !-6000 l5000 t;5::0 -4000 ...,.. .:;: 3000 ~ 0 ~ H --' 2000 133 1000 0000 5 32 l-- 31 30 29 ......-.,....---.,r----~---_r-Sweating Vasoconstriction Shivering 8aseline N' 7000 .§.6000 5000 it;--4000 .. <: ~3000 Fig. I. Core temperature changes associated with core cooling (~, protocol I) and skilHurfacf cooling (b, protocol 2). Core coaling was associated with a significant decrease in core temperature at the onset of vasoconstriction and shivering. Skin-surface temperature was unchanged. Skin-surface cooling was associated with a significant increase in skin temperature with sweating. and a Significant decrease when shivering occurred. Core temperature was unchanged. Statistical significance: 'p < 0.05 compared with baseline. (63 ± 5 beats/min) and shivering (60 ± 4 beats/min). The coefficient of variance was 0.078 ± 0.0 18 at baseline, 0.072 ± 0.009 with sweating, 0.102 ± 0.013 with vasoconstriction and 0.119 ± 0.021 with shivering and significantly increased overall (P < 0.0 I). The only discrete period during which the coefficient increased significantly was from sweating to vasoconstriction (P < 0.0 I). Power in all frequency bands decreased in value between baseline and sweating. Very low-frequency power did not change significantly during sweating nor increase significantly from baseline with either vasoconstriction or shivering (Fig. 5). Neither the ratio of low/high-frequency power nor high-frequency power changed significantly between the different states. Low frequency increased between baseline and vasoconstriction (P=0.055) and increased significantly with shivering (P < 0.05) When power values in the frequency bands during vasoconstriction and shivering were compared with those during sweating, both very low-frequency and low-frequency power were shown to increase significantly. ~ -i.2000 :f 1000 I I Baseline Vasoconstriction Shivering Fig. 2. Power in the very low-, low- and high-frequency bands associated with core cooling by infusion of coldsaline.Thermoregulatory vasoconstriction was associated with a significant increase in very low-frequency power. Statistical Significance: 'P < 0.05 compared with baseline. DISCUSSION As opposed to the work described previously, we evaluated the thermoregulatory response effects on the power spectra by independently manipulating core and skin temperature. Core cooling, which triggered thermoregulatory vasoconstriction, selectively increased power in the very low-frequency band, which was associated with no change in the ratio of low/high power and a significant decrease in average heart rate. In contrast, peripheral cooling selectively increased power in the low-frequency band, with no significant change in power in the very low-frequency band or in heart rate. These findings suggest that the change in particular frequency bands of the power spectra depends upon the mode of thermoregulatory challenge, and not thermoregulation per se. Thermoregulation and R-R variability 8 (0) .§ 101 8000 t i 7000 t6000 7 6 l5000 ~5 ~ f .. e- f~ f3000 ii.fOOO ~ -2000 I -..,..----1""""'----.--Baseline Vasoconstriction Shivering $'000 0..L.........,r----~--....,.--......,..._- 0 ... 8000 t 7000 8 .S! • 16000 (b) [5000 7 t-.fOOO c i! 6 ~ 5 r~3000 2000 1 ~ 1000 ~ f .. ::!; f~ 0 ...........,...------......- - - - 8000 - I 7000 0 ...._ - - -......- - - . - - - _ _ .......Baseline Sweating Vasoconstriction Shivering Fia. 3. The ratio of low/hi......requency power for core coolllll (.) and skllHUrface coolllll (b). The ratio increased with borderline signifIcance with sweating during core hypothermia (/'= 0.055), while no change was observed with skilHurface cooling. !:6OOO [5000 ~.fOOO ~3000 f 1..2000 :f 1000 o .....__.......--~--....,.--......,..._Baseline 1200 R-R interval (ms) 1000 800 rw"WIII'Mrul...,.~ ...'l,I.lw.M.."\R~AlJI,I.Wd. 1200 R-R interval (ms) 1000 Sweating Vasoconstriction Shivering Fla. 5. Power In the very low-, low- and hl......requency bands associated with skllHUrface coolllll. Shivering was associated with significant increases in low-frequency power. but not very low-frequency power. When compared with the lower power observed during sweating, both very low- and low-frequency power increased significantly. Statistical significance: '/' < 0.05 compared with baseline, tP < 0.05 compared with sweating. 800 Beat number Fla. 4.Two representatlYe R-R time series of 10 min duration from one volunteer In protocol I. An increase in the amplitude and components of HRV, particularly long-term oscillations, can be noted from baseline (0) to a period ofcore hypothermia and cutaneous vasoconstriction (b). R-R interval duration significantly increased from 905 ± 57 (SO) ms at baseline to 1027 ± 81 ms with vasoconstriction. Several investigators have suggested that thermoregulatory control systems alter arterial blood pressure, causing spontaneous oscillations characteristic of non-linear systems [8, 26]. Such systems are subject to selective entrainment, whereby the oscillatory frequency changes in response to an applied stimulus. Hyndman et al. [13] applied a thermal stimulus by placing one hand alternately in two different temperature baths, with the frequency con- sidered as the time in the bath for a complete cycle. When the stimulus was varied in the range of 8 to 120s, the heart rate and blood pressure power spectrum showed a dominant peak at the stimulus frequency, which is different from the peak observed in the spontaneous situation. When the stimulus lasted for more than 2 min, selective entrainment did not occur. The frequencies in which selective entrainment of thermoregulatory challenges occur coincide with the very low-frequency band of the heart rate power spectra. Lindqvist et al. [27] have attempted to replicate previous work by studying selective entrainment of the power spectra using cutaneous temperature challenges. They performed alternating rhythmic warm and cool immersion of different skin areas at different frequencies and water temperatures. When 102 L. A. Fleisher et al. the frequency of the thermal stimulation was between 0.013 and 0.096 Hz, forearm skin blood flow oscillations synchronized to the thermal stimulation. When periodicity of heart rate was evaluated, thermal oscillating stimulation resulted in an increase of the low-frequency periodic HRV. In contrast, non-specific sham stimulation significantly modified the frequency distribution of the lowfrequency periodic HRV without changes in the total low-frequency power compared with spontaneous conditions. The authors concluded that both thermal stimulation and non-specific central nervous influences induced significant and reproducible interactions with HRV. In contrast to the changes in very low-frequency power seen with core cooling, the low/high ratio did not initially change in response to thermoregulatory vasoconstriction, but increased with the onset of shivering. Although several investigators have suggested the usc of this ratio to indicate sympathovagal balance, others have demonstrated that the changes in the power spectrum depend on factors other than cardiac sympathetic nerve firings, and do not directly relate to cardiac noradrenaline spillover [28]. Malik and Camm [29] have suggested that the heart rate power spectrum does not directly measure sympathetic activity but more accurately reflects the modulation of the autonomic nervous system at the level of the heart. Therefore, the changes in the low/high ratio suggest that postsynaptic sympathetic modulation of heart rate does not occur with core hypothermia until lower body temperatures are reached and the increased metabolic demands of shivering are induced. Vasoconstriction was associated with a decrease in heart rate in both protocols. The response to cold challenge involves afferent input of temperature information to the hypothalamic centres, central processing of this information and an efferent response [30]. This efferent response is characterized by peripheral sympathetic activation as indicated by increased noradrenaline, but no adrenal medullary or cortical activation as determined by adrenaline and cortisol [24, 31]. The peripheral sympathetic activation is marked by profound vasoconstriction, as demonstrated by an increase in the forearmfingertip temperature gradient [23]. The increase in peripheral vascular resistance resulting from core cooling may have been balanced by a reflex increase in vagal tone; however, this was not supported by the power spectral analysis. Studies in isolated rat atrial preparations demonstrate a linear relationship between atrial rate and temperature between 35.6°C and 38'C [32]. This suggests that the bradycardia observed with core cooling may have been a direct effect of temperature on the sino-atrial node. Shivering was associated with a marked increase in heart rate and an increase in the low/high ratio of borderline significance. Shivering is associated with a two- to three-fold increase in oxygen consumption [33]. This increase in metabolic demand is met by an increase in cardiac output; results suggest that the increase in heart rate associated with shivering is a result in part of an increase in sympathetic 'tone' to compensate for the increased metabolic demand. Skin-surface cooling results in different changes in the heart rate power spectra than core cooling. Sweating resulted in a decrease in HRV with an increase in heart rate, suggesting that the increase in heart rate is not autonomically mediated. The initial tachycardia may be a direct thermal effect on the sino-atrial node [32]. The difference in heart rate power spectra between peripheral and core cooling most probably reflects the fact that core temperatures are unchanged by peripheral cooling. However, if changes in frequency ranges of the power spectra were compared with those during sweating, as opposed to baseline, then power in both the very low- and low-frequency ranges increased significantly, while heart rate decreased. This most probably reflects the profound peripheral vasoconstriction associated with this degree of skinsurface cooling. The lack of a specific response in the very low-frequency range, as observed during core cooling, suggests that these changes reflect a generalized peripheral vasoconstriction, and not a specific thermoregulatory change. There are several limitations to the current study. Firstly, our subjects were spontaneously breathing. Several investigators have demonstrated that both the respiratory rate and tidal volume can influence the peak frequency and amplitude of the highfrequency power [34, 35]. As described in the methods, we attempted to minimize this effect by observing respiratory rate and determining that all subjects breathed at greater than 12 breaths/min, which should result in the respiratory peak being greater than 0.125 Hz. Additionally, our primary observations regarded the very low-frequency component, which should not be significantly affected by these factors. Secondly, the sampling frequency of our equipment was 120 Hz. Merli et at. [36] have suggested that this sampling rate is the minimal acceptable rate for calculating the power spectrum of heart rate. In order to accurately detect the very lowfrequency component, longer data series are required. We used a 15 min data series in the first two protocols, which should allow us to detect changes in the frequency band of interest. Thirdly, our volume of cold infusion in protocol 1 may have been sufficient to change cardiopulmonary volumes and pressures. However, a similar volume of warm saline was not shown to change blood pressure, heart rate or H RV [31]. Therefore, it is unlikely that the effect we observed was due to the fluid infusion, but rather due to the change in core temperature. In summary, we observed a specific thermoregulatory influence on the very low-frequency component of HRV related to core hypothermia, while skin- Thermoregulation and R-R variability surface temperature changes were associated with less specific HRV changes. Further studies are required to determine how the thermoregulatory component modulates HRV and its importance in relation to cardiovascular morbidity. ACKNOWLEDGMENTS This work was supported in part by the National Institutes of Health GM49670, the Joseph Brown Foundation, Mallinckrodt Medical, Inc. and Augustine Medical, Inc. L.A.F. is supported by the Richard S. Ross Clinician Scientist Award of the Johns Hopkins University School of Medicine. We acknowledge the technical expertise of Michelle Langston for initial analysis of the electrocardiographic recordings. REFERENCES I. Sayers BM. Analysis of heart rate variability. Ergonomics 1973; 16: 17-32. 2. Malliani A, Pagani M. Lombardi F, Cerutti S. Cardiovascular neural regulation explored in the frequency domain. Circulation 1991; 84: 482-92. 3. Appel ML, Berger RD. Saul IP. Smith 1M. Cohen RI. Beat to beat variability in cardiovascular variables: noise or music! I Am Coli Cardiol 1989; 14: 1139-48. 4. Bigger IT, Fleiss IL. Steinman RC, Rolnitzky LM, Schneider WI. Stein PK. RR variability in healthy. middle-aged persons compared with patients with chronic heart disease or recent myocardial infarction. Circulation 1995; 91: 1936-43. 5. Bigger IT, Kleiger RE, Fleiss IL, Rolnitzky LM. Steinman RC. Miller IP. Components of heart rate variability measured during healing of acute myocardial infarction. Am J Cardiol 1988; 61: 208-15. 6. Kleiger RE, Miller IP, Bigger IT, Moss AI. Decreased heart rate variability and its association with increased mortality after acute myocardial infarction. Am I Cardiol 1987; 59: 256-62. 7. Fleisher LA. Pincus SM, Rosenbaum SH. Approximate entropy of heart rate as a correlate of postoperative ventricular dysfunction. Anesthesiology 1993; 78: 68l-92. 8. Akselrod S. Gordon 0, Ubel FA, Shannon DC, Barger AC, Cohen RI. Power spectrum analysis of heart rate fluctuation: a quantitative probe of beat-to-beat cardiovascular control. Science (Washington DC) 1981; 213: 226-2. 9. Lombardi F. Sandrone G, Pernpruner S.et al. Heart rate variability as an index of sympathovagal interaction after acute myocardial infarction. Am I Cardiol 1987; 60: 1239-45. 10. Akselrod S, Gordon 0, Madwed 18, Snidman NC, Shannon DC, Cohen RI. Hemodynamic regulation: investigation by spectral analysis. Am I Physiol 1985; 249: H867-75. II. Kitney RI. An analysis of the thermoregulatory influences on heart rate variability. In: Kitney RI, Rompelman I, ed. The study of heart rate variability. Oxford: Clarendon Press, 1980: 81-106. 12. Kitney RI. The analysis and simulation of the human thermoregulatory control system. Med 8iol Eng 1974; 12: 57-64. 13. Hyndman BW, Kitney RI. Sayers BM. Spontaneous rhythms in physiological control systems. Nature (London) 1971; 233: 339-41. 103 14. Kitney RI, Rompelman O. The beat-by-beat investigation of cardiovascular function: measurement. analysis. and applications. Oxford: Clarendon Press. 1987. 15. Edmonds IR. Critical tomment on the thermal entrainment of blood flow. Med Bioi Eng Comput 1981; 5: 186-8. 16. Lindqvist A. lalonen J. Parviainen P, Antila K. Laitinen LA. Effect of posture on spontaneous and thermally stimulated cardiovascular oscillations. Cardiovasc Res 1990; 24: 37l-8O. 17. Cheng C. Matsukawa T, Sessler 01. et al. Increasing mean skin temperature linearly reduces the core-temperature thresholds for vasoconstriction and shivering in humans. Anesthesiology 1995; 82: 1I~. 18. Aguirre A, Wodicka GR. Muyan C. Shannon DC. Interaction between respiratory and RR interval oscillations at low frequencies. I Auton Nerv Syst 1990; 29: 241-6. 19. Sessler 01. Rubinstein EH. Moayeri A. Physiologic responses to mild perianesthetic hypothermia in humans. Anesthesiology 1991; 5: 594-610. 20. Sessler 01. Central thermoregulatory inhibition by general anesthesia [editorial; comment]' Anesthesiology 1991; 75: S57-9. 21. Mekjavic lB. Rempel ME. Determination of esophageal probe insertion length based on standing and sitting height. J Appl Physiol 1990; 69: 376-9. 22. Stoen R. Sessler 01. The thermoregulatory threshold is inversely proportional to isoflurane concentration. Anesthesiology 1990; 72: 822-7. 23. Rubinstein EH. Sessler 01. Skin-surface temperature gradients correlate with fingertip blood flow in humans. Anesthesiology 1990; 73: 541-S. 24. Frank SM, Higgins MS, Breslow MI. et al. The catecholamine. cortisol. and hemodynamic responses to mild perioperative hypothermia: a randomized clinical trial. Anesthesiology 1995; 82: 8l-93. 25. Berger RD. Akselrod S,Gordon D. Cohen RI. An efficient algorithm for spectral analysis of heart rate variability. IEEE Trans Biomed Eng 1986; 33: 900-4. 26. Kitney RI, Fulton T. McDonald AH, Linkens DA. Transient interactions between blood pressure, respiration and heart rate in man. I Biomed Eng 1985; 7: 217-24. 27. Lindqvist A, Parviainen P, lalonen J. Tuominen J. Valimaki I. Laitinen LA. Clinical testing of thermally stimulated cardiovascular oscillations in man. Cardiovasc Res 1991; 25: 666-75. 28. Kingwell BA, Thompson JM. Kaye OM. McPherson GA, lennings GL. Esler MD. Heart ratespectral analysis, cardiac norepinephrine spillover. and muscle sympathetic nerve activity during human sympathetic nervous activation and failure. Circulation 1994; 90: 23+40. 29. Malik M. Camm AI. Components of heart rate variability-what they really mean and what we really measure [editorial]. Am I Cardiol 1993; 72: 821-2. 30. Sessler 01. Perianesthetic thermoregulation and heat balance in humans. FA5EB I 1993; 7: 638--+4. 31. Higgins MS. Frank SM, Breslow MI, Fleisher LA, Beattie C. The adrenergic response to mild core hypothermia [abstractl. Anesthesiology 1994; 81: A234. 32. Bolter CP, Atkinson KI. Influence of temperature and adrenergic stimulation on rat sinoatrial frequency. Am I Physiol 1988; 254: R84G-4. 33. Horvath GB. Spurr GB, Hutt BK. Hamilton LH. Metabolic cost ofshivering. I Appl Physiol 1956; 8: 595-602. H. Elghozi JL, Laude 0, Girard A. Effects of respiration on blood pressure and heart rate variability in humans. Clin Exp Pharmacol Physiol 1991; 18: 735-42. 35. Hayano I, Mukai S. Sakakibara M. Okada A. Takata K. Fujinami T. Effects of respiratory interval on vagal modulation of heart rate. Am J Physiol 1994; 267: H3l-4O. 36. Merli M, Farden DC, Mottley IG. Titlebaum El. Sampling frequency of the electrocardiogram for spectral analysis of the heart rate variability. IEEE Trans Biomed Eng 1990; 37: 99-105.