* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Experimental induction of retinal ganglion cell death in adult mice.
Survey
Document related concepts
Transcript
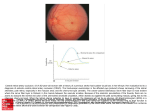
1000 Reports 6. Bunt-Milam AH, SaariJC. Immunocytochemical localization of two retinoid-binding proteins in vertebrate retina. / Cell Biol. 1983;97: 703-712. 7. Bok D. The retinal pigment epithelium: a versatile partner in vision./ Cell Sci. 1993;17:189-195. 8. Bernstein PS, Law WC, Rando RR. Isomerization of all-trans-retinoids to 11-czs-retinoids in vitro. Proc Natl Acacl Sci USA. 1987;84: 1849-1853. 9. Deigner PS, Law WC, Canada FJ, Rando RR. Membranes as the energy source in the endergonic transformation of vitamin A to 11-cfe-retinol. Science. 1989;244:968-971. 10. SaariJC, Bredberg L, Garwin GG. Identification of the endogenous retinoids associated with three cellular retinoid-binding proteins JOVS, April 1999, Vol. 40, No. 5 11. 12. 13. 14. from bovine retina and retinal pigment epithelium. / Biol Chem. 1982;257:13329-13333. Saari JC, Bredberg D, Noy N. Control of substrate flow at a branch in the visual cycle. Biochemistry. 1994;33:3106-3112. Morimura H, Berson EL, Dryja TP. Recessive mutations in the RLBP1 gene encoding cellular retinaldehyde-binding protein in a form of retinitis punctata albescens. Invest Ophthalmol Vis Sci. 1999;40:1000-1004. Broman KW, Murray JC, Sheffield VC, White RL, Weber JL. Comprehensive human genetic maps: individual and sex-specific variation in recombination. 1998 http://www.marshmed.org/genetics/. Hudson T, Stein L, Gerety S, et al. An STS-based map of the human genome. Science. 1995;270:1945-1954. Recessive Mutations in the RLBP1 Gene Encoding Cellular Retinaldehyde-Binding Protein in a Form of Retinitis Punctata Albescens Hiroyuki Morimura,1 Eliot L Berson,2 and Thaddeus P. Dryja1'1 PURPOSE. TO determine the frequency and spectrum of mutations in the RLBP1 gene encoding cellular retinaldehyde-binding protein (CRALBP) in patients with hereditary retinal degeneration. The single-strand conformation polymorphism (SSCP) technique and a direct genomic sequencing technique were used to screen the coding exons of this gene (exons 2-8) for mutations in 324 unrelated patients with recessive or isolate retinitis pigmentosa, retinitis punctata albescens, Leber congenital amaurosis, or a related disease. Variant DNA fragments revealed by SSCP analysis were subsequently sequenced. Selected alleles that altered the coding region or intron splice sites were evaluated further through segregation analysis in the families of the index cases. METHODS. RESULTS. Four novel mutations were identified in this gene among three unrelated patients with recessively inherited retinitis punctata albescens. Two of the mutations were From the 'Ocular Molecular Genetics Institute and the 2 BermanGuncl Laboratory for the Study of Retinal Degenerations, Harvard Medical School and the Massachusetts Eye and Ear Infirmary, Boston, Massachusetts. Supported by Grants EY08683 and EY00169 from the National Eye Institute, National Institutes of Health, Bethesda, Maryland; the Foundation Fighting Blindness, Hunt Valley, Maryland; and the Massachusetts Lions Eye Research Fund, Northborough; and by private donations to the Taylor Smith Laboratory and the Ocular Molecular Genetics Institute. TPD is a Senior Scientific Investigator of Research to Prevent Blindness, New York, New York. Submitted for publication October 16, 1998; accepted December 11, 1998. Proprietary interest category: N. Reprint requests: Thaddeus P. Dryja, MD, Massachusetts Eye and Ear Infirmary, 243 Charles Street, Boston, MA 02114. missense: one was a frameshift, and one affected a canonical splice donor site. Recessive mutations in the RLBP1 gene are an uncommon cause of retinal degeneration in humans. The phenotype produced by RLBP1 mutations seems to be a form of retinitis punctata albescens. (Invest Ophthalmol Vis Sci. 1999;40:1000 -1004) CONCLUSIONS. T he first step in vision occurs when a photon converts an 1 l-cis retinal chromophore, which is covalently linked to rod or cone opsin, to the all-trans isomer.1 In mammals, this reaction takes place in the outer segments of the photoreceptor cells of the retina. The aH-trans chromophore subsequently leaves rod or cone opsin and travels as all-fraws-retinol to a neighboring retinal pigment epithelial cell,2 where it is converted through a series of intermediates back to 11-m-retinaldehyde. The protein CRALBP seems to play a role in this pathway. CRALBP is present in the retinal pigment epithelium and the Miiller cells of the retina.3 The protein forms complexes with regenerated 11-a's-retinaldehyde and its immediate precursor 11-czs-retinol.4'5 Still uncertain is whether these complexes are essential intermediates in this pathway or whether CRALBP has another physiological role. The requirement for CRALBP in the retina was highlighted by a recent report of the missense mutation Argl50Gln in the RLBP1 gene (chromosome 15q26)6 in a family from India with a recessive retinal degeneration that was termed retinitis pigmentosa.7 The mutation was homozygous in the affected members but not in the unaffected members of an 11-member sibship that was the product of a first-cousin marriage. Evidence for the pathogenicity of this mutation came from the observations that the mutant protein in vitro was less water soluble than normal and that it did not bind to 11-m-retinaldehyde.7 In the present report, we provide additional evidence, through the identification of mutations in patients of European ancestry, that recessive defects in the human RLBP1 gene are pathogenic. Furthermore, the clinical findings from our cases and those in the report by Burstedt et al8 in this issue suggest that the phenotype can be distinguished from typical retinitis pigmentosa. METHODS Ascertainment of Patients This study, which involved human subjects, conformed to the tenants of the Declaration of Helsinki. The index patients in Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933211/ on 08/12/2017 Reports IOVS, April 1999, Vol. 40, No. 5 this study had a diagnosis of retinal degeneration or malfunction made through ophthalmologic examination including electroretinography (ERG). Most patients resided in the United States or Canada. Patients with autosomal recessive retinitis pigmentosa had unaffected parents and at least one affected sibling or were the offspring of a consanguineous mating. If all affected siblings with retinitis pigmentosa in a sibship were males, the possibility of X-linked disease was evaluated through an ophthalmologic examination of the mother, including an ERG to search for the carrier state of X-linked retinitis pigmentosa; families with X-linked retinitis pigmentosa were excluded from this study. Some isolate cases were included. They had no affected relatives and were not the offspring of a consanguineous mating. Atypical retinitis pigmentosa was diagnosed in these patients if they had some combination of the following features: reduced but unusually large ERGs for their age, an unusual pigmentary pattern, or no abnormality of dark adaptation threshold after 45 minutes of dark adaptation; all were isolate cases. Patients with retinitis punctata albescens had ERG findings indicating a generalized retinal degeneration, elevated dark adaptation threshold after 45 minutes of dark adaptation, and fundi that showed attenuated arterioles and subretinal yellow or yellow-white deposits as a predominant feature. Some also had intraretinal pigment deposits. Patients with Leber congenital amaurosis had absent or severely diminished vision within the first year of life and markedly diminished ERGs; all had unaffected parents. Patients with fundus albipunctatus had normal retinal vessels, diffuse subretinal white deposits, elevated dark adaptation thresholds, and reduced ERGs after 45 minutes of dark adaptation that became normal after 6 to 12 hours of dark adaptation. Patients with other forms of stationary night blindness had fundi without the stigmata of retinitis pigmentosa, elevated dark-adaptation thresholds, reduced rod ERGs, and cone ERGs that were normal when corrected for age and refractive error. Control subjects had no known blood relative with hereditary retinal degeneration and no symptoms of retinal malfunction. After informed consent, we collected between 3 ml and 50 ml venous blood from each patient or control subject. Leukocyte nuclei were prepared from the blood samples and stored at — 70°C before DNA was purified from them. Screening for RLBP1 Mutations Exons 2 through 8 of the RLBP1 gene were individually amplified from human genomic DNAs by polymerase chain reaction (PCR) using the following primer pairs based on the published genomic sequence6 (sense, antisense, respectively): exon 2, TGAGATCCACAGTTCTGAGAC, AGGAGAGCCCTGGAGGACA; exon3, GGCTGATGCGGTTGGCTGTT, CCCCTCATGTTGCCTCCCTA; exon 4, CTCATCACCTGTGTGTCCTGCC, GAGAGCGGATAGCATCCTCATG; exon 5, CTTCTGAGTCCCACTAGGAGG, CCAGTAGAGGCCAGGGTTGA; exon 6, CCTCAGGACCTCAAGCCTTA, CTGCAAGCACCATGAAAGGA; exon 7, AATGAGTGGGAGCCTCTGAG, CCCTCTTGTCTCATTGTCTGG; and exon 8, CTCCTGCTCAGTTCTGTCTC, AGTTCAGCTGGCAGGAGATG. The single-strand conformation polymorphism (SSCP) technique was used to screen for point mutations and other small-scale sequence changes. PCRs were performed in the wells of 96-well microtiter plates. In each well was 50 ng to 100 ng leukocyte DNA in 20 /al of a solution 1001 containing 20 mM Tris-HCl (pH 8.4 or 8.6), 0.25 to 1.5 mM MgCl2, 50 mM KC1, 0.02 mM deoxyadenosine triphosphate (dATP), 0.02 mM deoxythymidine triphosphate (dTTP), 0.02 mM deoxyguanosine triphosphate (dGTP), and 0.002 mM deoxycytidine triphosphate (dCTP), 0.6 mCi [a-32P] deoxycytidine triphosphate (3000 Ci/millimole), 0.1 mg/ml bovine serum albumin, 0% or 10% dimethyl sulfoxide, and 0.25 units of Taq polymerase. The pH, Mg2+ concentration, and presence or absence of 10% dimethyl sulfoxide were tailored to each primer pair to yield optimal amplification. After initial denaturation (94°C for 5 minutes), 35 cycles of PCR amplification were performed. Each cycle consisted of denaturation (94°C for 30 seconds), primer annealing (54°C for 30 seconds), and extension (71°C for 30 seconds). The final extension was at 71°C for 5 minutes. The amplified DNA fragments were heat denatured, and the single-stranded fragments were separated, each through two sets of 6% polyacrylamide gels, one set with and one without 10% glycerol. Gels were run at 8 W to 12 W for 5 to 20 hours before drying and autoradiography. Variant bands were evaluated by sequencing of corresponding PCR-amplified DNA segments using a cycle-sequencing protocol in a radiolabeled terminator cycle sequencing kit (Thermo Sequenase; Amersham Life Science, Cleveland, OH). Sequence variations expected to affect protein sequence or expression were evaluated further by recruiting the relatives of the index patient to participate in a study to determine whether the variant allele cosegregated with the disease. For this purpose, leukocyte DNA samples from the relatives were analyzed by SSCP or direct genomic sequencing for the presence of the variant sequence. RESULTS Based on the previously reported 5' untranslated, 3' untranslated, and flanking intron sequences for the human RLBPJ gene,6 we developed assays using the SSCP technique to screen for mutations in the entire coding sequence and the intron sequences immediately flanking exons 2 through 8. With these assays, we evaluated DNA from 189 patients from separate families with autosomal recessive retinitis pigmentosa, 45 unrelated patients with congenital amaurosis, 6 unrelated patients with retinitis pigmentosa sine pigmento, 16 unrelated patients with atypical retinitis pigmentosa, 28 unrelated patients with Bardet-Biedl syndrome, 28 unrelated patients with retinitis punctata albescens, 2 unrelated patients with fundus albipunctatus with night blindness, and 10 unrelated patients with stationary night blindness. Three index patients were found to be homozygotes or compound heterozygotes for mutations listed in Table 1. All reported European ancestors. One patient (003-188) was homozygous for a frameshift mutation in codon 278 (Gln278[l-bp del]; Fig. 1A). This frameshift changes the amino acid sequence downstream of codon 278 and extends the length of the encoded protein from 316 to 326 residues. This patient's parents were third cousins. Only the mother was alive, and she was found to be a heterozygote for this mutation. The patient had one living sibling. This sister was unaffected and was a heterozygote. No other family members were affected. Another patient (097-001) heterozygously carried two sequence abnormalities: One was a point mutation involving the canonical splice donor site of intron 3 (TVS3 + 2 T—>C; Fig. IB) and Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933211/ on 08/12/2017 1002 IOVS, April 1999, Vol. 40, No. 5 Reports TABLE 1. Mutations Found in the RLBPl Gene Patient Genomic Location Region of Gene or Codon Affected 003-188 097-001 097-001 274-007 9483delC Exon 8, Gln*278(l-bp del) (GAG to -AG) Intron 3 splice donor site, IVS3+2 (GT to GC) Exon 6, Met°226Lys+ (ATG to AAG) Exon 7, Arg+234Trp° (CGG to TGG) Nucleotide numbers are based on a published RLBPl genomic sequence.6 The codon numbering includes the initiation methionine, a residue that is not present in the final protein product.15 The superscript symbol after each three-letter amino acid abbreviation indicates the type of R group: * polar; 0 nonpolar; + positively charged. the other a missense change (Met226Lys; Fig. 1C). Each of this patient's parents, who were unaffected, carried one of these changes heterozygously (the mother had the splice-site mutation and the father the missense mutation), indicating that the mutations were allelic and that the patient was therefore a compound heterozygote (data not shown). There were no other affected members in this family. There was one unaffected sibling (a brother) who carried the missense mutation heterozygously. A third patient (274-007) was homozygous for the missense mutation Arg234Trp (not shown). This patient was a member of a Swedish kindred that we subsequently learned was fortuitously and independently being studied by another group (see the accompanying report8). None of the four mutations found in these patients was found among 69 or 70 normal control subjects. Ten other sequence anomalies were encountered during this study (Table 2). One was a biallelic, single-base polymorphism in intron 6 with a minor allele frequency of 035 to 0.39Most of the others were interpreted as rare variants, because they were not predicted to alter the sequence or expression of the encoded protein. An exception was the missense change Phel82Cys that was found heterozygously in an isolate case of retinitis pigmentosa sine pigmento (patient identification number 008-005). No defect was found in the homologous allele in this patient, and it was not studied further. Clinical examination of patients 097-001 at age 19 years and 003-188 at age 52 years showed small yellow deposits at the level of the retinal pigment epithelium across the fundus. In the older patient, there were round areas of atrophic retinal pigment epithelium in the midperiphery and far periphery that A. Gin278(1-bp del) were reminiscent of those seen in gyrate atrophy (Fig. 2). Intraretinal pigment deposits were sparse and were sometimes seen at the borders of the atrophic patches of retinal pigment epithelium. Retinal vessels were attenuated in both patients, more so in the older patient. The funduscopic findings of the Swedish patients with an RLBPl mutation were similar.8 Our patients with RLBPl mutations had reduced rod and cone ERGs with predominant loss of rod function. DISCUSSION The mutations in the RLBPl gene encountered in this study are likely to be pathogenic, .because they were not found among normal control subjects and because affected people, who had recessively inherited disease, were either homozygotes or compound heterozygotes. Except for the mutation found in the Swedish patient (see the accompanying report8), the probands were from small families and had no affected relatives, so that meaningful cosegregation analyses were not possible. Ah1 the mutations could be predicted to have major effects on the encoded protein. One of the mutations is a frameshift that would alter the carboxyl terminus of the protein. Another is a splice-site mutation that is likely to interfere with proper processing of the RNA transcript. Two of the mutations are missense and one changes a nonpolar residue to a positively charged one (Met226Lys), whereas the other changes a positively charged residue to a nonpolar one (Arg234Trp). Additional work will be necessary to determine whether the corresponding mutant proteins have a reduced affinity for the B. IVS3+2T->C C. Met226Lys wild type mutarrt Control 097-001 CTAG CTAG Control 003-188 CTAG C T A G Gln228 Leu227 Met226Lys Asp225 Val224 Phe27$ Met223 FIGURE 1. Sequence of the mutations found in the RLBPl gene. In each panel, the relevant region of the RLBPl genomic sequence is shown with the sense direction going from the bottom to the top. The corresponding regions from a subject with the wild-type sequence are shown for comparison. Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933211/ on 08/12/2017 IOVS, April 1999, Vol. 40, No. 5 TABLE Reports 1003 2. RLPB1 Polymorphisms, Rare Silent Variants, and Rare Variants of Uncertain Pathogenicity Number of Respective Alleles* Genomic Location 878C-»A 2779delGAGGCC 4674G->A 8008T-*G 8l67C-»T Region of Gene or Codon Affected Patients Exon 2, 5' untranslated region (G versus A) Exon 2, 5' untranslated region (C versus A) Exon 2, 5' untranslated region (T versus C) Exon 3, Arg + 42Arg + (CGC versus CGT) IVS3-3 (T versus G) rVS4+3 (GAGGCC versus —) Exon 5, Arg + 121Arg + (CGG versus CGA) Exon 6, Leu°177Leu° (TTG versus CTG) Exon 6, Phe°182Cys* (TTC versus TGC) IVS6+20 (C versus T) 646:2 647:1 647:1 647:1 647:1 645:3 647:1 647:1 647:1 397:251 (0.39) Controls 140:0 140:0 140:0 140:0 138:0 134:4 140:0 138:0 138:0 90:48 (0.35) Nucleotide numbering, codon numbering, and symbols are the same as in Table 1. * Minor allele frequency in parentheses. retinoids that are thought normally to form complexes with CRALBP, an abnormality found in the previously reported missense mutation. 7 Certain clinical characteristics of the patients with RLBP1 mutations are similar to those found in patients with retinitis pigmentosa, such as night blindness as an early symptom, FIGURK 2. (A, B) Fundus photographs of the right eye of patient 097-001 at age 19 show slight retinal arteriolar attenuation with yellow subretinal deposits throughout the retina and areas of atrophic retinal pigment epithelium in the periphery. (A) Temporal midperiphery; (B) posterior pole. (C, D) Photographs of the right eye of patient 003-188 at age 52 show retinal arteriolar attenuation and peripheral and midperipheral atrophy of the retinal pigment epithelium. (C) Posterior pole; (D), nasal midperiphery. Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933211/ on 08/12/2017 1004 Reports funduscopic findings of attenuated retinal vessels and intraretinal pigment deposits, and reduced ERGs. Other clinical findings shared by patients carrying RLBP1 mutations may be sufficiently distinguishing to warrant a separate diagnostic category. All patients had small yellow deposits at the level of the retinal pigment epithelium. Subretinal yellow deposits were also described in the affected members of the previously reported family with an RLBP1 mutation,7 suggesting that this feature may be a characteristic of the disease caused by defective or absent CRALBP. A second feature is the development of patches of atrophic retinal pigment epithelium with well-defined, rounded margins in the retinal periphery that are reminiscent of those found in patients with gyrate atrophy. The term "retinitis punctata albescens" is probably the best existing one for the patients with RLBP1 defects, because it is commonly used by ophthalmologists to describe a photoreceptor degeneration with or without intraretinal pigmentation that has minute yellow or yellow-white deposits deep in the retina or at the level of the retinal pigment epithelium.910 Areas of chorioretinal atrophy have been described in some patients with retinitis punctata albescens.10'11 Similar to retinitis pigmentosa, retinitis punctata albescens is genetically heterogeneous, with reports documenting cases caused by defects in the RDS gene on chromosome 6p or in the rhodopsin gene on chromosome 3q.12'13 The RLBP1 gene seems to be a rare cause of recessive retinal disease, accounting for only 3 of 324 unrelated patients with retinitis pigmentosa or an allied retinal degeneration or malfunction in our series. A previous search among an overlapping set of patients for mutations in the RLBP1 gene using Southern blot techniques14 was understandably negative, because the types of mutations found here involving single-base changes or deletions are beyond the resolution of Southern blot techniques. With recognition of the clinical features that seem to be characteristic of this disease, it may be possible to identify patients with a similar phenotype and to determine whether they also have RLBP1 gene defects. Acknowledgments The authors thank Sten Andreasson for obtaining blood samples from some of the patients. Experimental Induction of Retinal Ganglion Cell Death in Adult Mice Yan Li, Cassandra L Schlamp, and Robert W. Nickells Retinal ganglion cells die by apoptosis during development and after trauma such as axonal damage and exposure to excitotoxins. Apoptosis is associated with changes in the expression of genes that regulate this process. The genes that regulate apoptosis in retinal ganglion cells have not been characterized primarily because previous studies have been limited to animal models in which gene function is not easily manipulated. To overcome this limitation, the rate and mechanism of retinal PURPOSE. IOVS, April 1999, Vol. 40, No. 5 References 1. Schoenlein RW, Petenau LA, Mathies RA, Shank CV. The first step in vision: femtosecond isomerization of rhodopsin. Science. 1991; 254:412-415. 2. Dowling JE. Chemistry of visual adaptation in the rat. Nature. 1960;188:ll4-118. 3- Bunt-Milam AH, Saari JC. Immunocytochemical localization of two retinoid-binding proteins in vertebrate retina. / Cell Biol. 1983;97: 703-712. 4. Saari JC, Bredberg DL, Noy N. Control of substrate flow at a branch in the visual cycle. Biochem. 1994;33:31O6-3112. 5. Crabb JW, Carlson A, Chen Y, et al. Structural and functional characterization of recombinant human cellular retinaldehydebinding protein. Protein Sci. 1998;7:746-757. 6. Intres R, Goldflam S, Cook JR, Crabb JW. Molecular cloning and structural analysis of the human gene encoding cellular retinaldehyde-binding protein. JBiol Chem. 1994;269:254l 1-25418. 7. Maw MA, Kennedy B, Knight A, et al. Mutation of the gene encoding cellular retinaldehyde-binding protein in autosomal recessive retinitis pigmentosa. Nat Genet. 1997;17:198-200. 8. Burstedt MSI, Sandgren O, Holmgren G, Forsman-Semb K. Bothnia dystrophy caused by mutations in the cellular retinaldehyde-binding protein gene (RLBP1) on chromosome 15q26. Invest Ophthalmol Vis Sci. 1999;40:995-1000. 9. Lauber H. Die sogenannte Retinitis punctata albescens. Klin Monatsbl Augenbeilkd. 1910;48:133-l48. 10. Franceschetti A, Francois J, Babel J. Chorioretinal Heredodegenerations. Springfield, IL: Charles C. Thomas; 1963. 11. Pillat A. Tapetoretinal degeneration of the central fundus region. Am J Ophthalmol. 1930;13:l-12. 12. Kajiwara K, Sandberg MA, Berson EL, Dryja TP. A null mutation in the human peripherin/RDS gene in a family with autosomal dominant retinitis punctata albescens. Nat Genet. 1993;3:208212. 13- Souied E, Soubrane G, Benlian P, et al. Retinitis punctata albescens associated with the Argl35Trp mutation in the rhodopsin gene. Am J Ophthalmol. 1996;121:19-25. 14. Cotran PR, Ringens PJ, Crabb JW, Berson EL, Dryja TP. Analysis of the DNA of patients with retinitis pigmentosa with a cellular retinaldehyde binding protein cDNA. Exp Eye Res. 199O;51:1519. 15. Crabb JW, Goldflam S, Harris SE, Saari JC. Cloning of the cDNAs encoding the cellular retinaldehyde binding protein from bovine and human retina and comparison of the protein sequences. J Biol Chem. 1988; 263:18688-18702. ganglion cell death in mice was characterized using optic nerve crush and intravitreal injections of the glutamate analog ./V-methyl-D-aspartate (NMDA). METHODS. TO expose retinal ganglion cells (RGCs) to excitotoxins, adult CB6F1 mice were injected intravitreally in one eye with NMDA. In an alternative protocol to physically damage the axons in the optic nerve, the nerve was crushed using self-closing fine forceps. Each animal had one or the other procedure carried out on one eye. Loss of RGCs was monitored as a percentage of cells lost relative to the fellow untreated eye. Thyl expression was examined using in situ hybridization. DNA fragmentation in dying cells was monitored using terminal transferasedUTP nick-end labeling (TUNEL). comprise 67.5% ± 6.5% (mean ± SD) of cells in the ganglion cell layer (GCL) of control mice based RESULTS. RGCS Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933211/ on 08/12/2017 Reports IOVS, April 1999, Vol. 40, No. 5 on nuclear morphology and the presence of mRNA for the ganglion cell marker Thyl. One week after optic nerve crush, these cells started to die, progressing to a maximum loss of 57.8% ± 8.1% of the cells in the GCL by 3 weeks. Cell loss after NMDA injection was dose dependent, with injections of 10 nanomoles having virtually no effect to a maximum loss of 72.5% ± 12.1% of the cells in the GCL within 6 days after injection of 160 nanomoles NMDA. Cell death exhibited features of apoptosis after both optic nerve crush and NMDA injection, including the formation of pyknotic nuclei and TUNEL staining. Quantitative RGC death can be induced in mice using two distinct signaling pathways, making it possible to test the roles of genes in this process using transgenic animals. (Invest Ophthalmol Vis Set. 1999;40: 1004-1008) CONCLUSIONS. etinal ganglion cells (RGCs) are the retinal neurons most R affected in disorders of the optic nerve, of which glaucoma is the most prevalent. Recent studies indicate that RGCs die with characteristics of apoptosis during normal development of the retina and after injury to the axons of adult RGCs such as axotomy of the optic nerve, experimental glaucoma in animals, and glaucoma and anterior ischemic optic neuropathy in humans.' Various stimuli cause the death of RGCs. During development these cells acquire absolute dependence on neurotrophins secreted by the brain as part of the mechanism to ensure proper synaptic connection with higher visual centers. Loss of neurotrophic support stimulates the death of RGCs in culture.2 Similar neurotrophic loss may be encountered after optic nerve transection, because RGC death under this condition can be delayed by injecting exogenous growth factors into the vitreous.3 RGCs are also sensitive to the toxic effects of high concentrations of excitatory amino acids such as glutamate. In the retina, RGCs and a subset of cells in the inner nuclear layer express subunits for the 7V-methyl-D-aspartate (NMDA) receptor. In an excitotoxic response, glutamate hyperactivates the NMDA receptor and precipitates a Ca2+-dependent chain of events that can lead to apoptosis or necrosis, depending on the magnitude of the excitatory response. RGCs are exquisitely sensitive to the effects of glutamate and the glutamate analog NMDA, which cause a dose-dependent loss of RGCs both in vitro and in vivo.4'5 Both neurotrophin deprivation and gluta- From the Department of Ophthalmology and Visual Sciences, University of Wisconsin, Madison. Supported by grants from the American Health Assistance Foundation, Rockville, Maryland and the Retina Research Foundation, Houston, Texas; Grant 1 R29 EY12223 from the National Institutes of Health, Bethesda, Maryland; and a Career Development Award to RWN and an unrestricted gift to the Department of Ophthalmology and Visual Sciences from Research to Prevent Blindness, New York, New York. YL was the recipient of the Shaffer International Fellowship from the Glaucoma Research Foundation, San Francisco, California. Submitted for publication July 16, 1998; revised November 19, 1998; accepted December 21, 1998. Proprietary interest category: N. Reprint requests: Robert W. Nickells, Department of Ophthalmology and Visual Sciences, K6/458 CSC, University of Wisconsin, 600 Highland Avenue, Madison, WT 53792. 1005 mate toxicity have been implicated in the pathophysiology of glaucoma.' The genes that regulate the cell death program in RGCs have also been studied. These studies have traditionally been carried out on rats after axotomy of the optic nerve and entail measuring the changes in the expression of select genes such as bax and bcl-x.6'7 These observations are limited, however, in that they only provide circumstantial evidence of gene function in RGCs. Ideally, the most rigorous test of function is to genetically alter a select gene and test the effect of either the loss-of-function or the gain-of-function of that gene after experimentally activating RGC death. Currently, the ability to alter genes in a mammalian system is most well developed in mice. Until recently, however, these animals have not been used to study RGC death, in part because of the technical difficulties in stimulating the death of these cells. The ability to use mice to study RGC death would represent an advance in this area of research. Here, we report the characterization of RGC death in adult mice using two protocols that activate apoptosis via different signaling pathways. METHODS Experimental Animals The animals used in this study were handled in accordance with the ARVO Resolution for the Use of Animals in Ophthalmic and Vision Research. All protocols were reviewed and approved by the Research Animal Resource Center of the University of Wisconsin. The experiments shown here were all conducted on CB6F1 mice (an Fl hybrid generation of a BALB/c female crossed with a C57BL/6 male) of an average age of 4 months, weighing 20 g to 25 g. No obvious differences in cell loss after treatment were detected in several other strains tested (data not shown). For each surgical procedure the mice were first anesthetized by intraperitoneal injection of 0.2 ml to 0.3 ml of solution containing ketamine (6 mg/mL) and xylazine (0.4 mg/mL). At select time points after surgery, the mice were killed by cervical dislocation. Optic Nerve Crush Mice were first anesthetized. A lateral canthotomy was made on one eye to allow access to the posterior pole. The bulbar conjunctiva was cut 90° in die superior temporal region and gently peeled back to the posterior region of the globe. The optic nerve was then exposed through a small window made between the surrounding muscle bundles by gentle bluntdissection using a pair of watchmaker forceps. Care was taken not to cut the muscles or the vessels in the surrounding fascia, because this leads to excessive bleeding. At a site approximately 1 mm from the posterior pole, the nerve was clamped using a pair of Dumont No. 5 self-closing forceps for 3 to 5 seconds. After this procedure, the conjunctiva and lateral canthotomy were closed with sutures and the mice allowed to recover. These mice exhibited normal eating and drinking behaviors and showed no signs of ill effects for a period of at least 6 weeks. Operated eyes were monitored for signs of ischemia due to damage of the central retinal artery both by direct observation of the retinal blood vessels using a dissecting microscope and histologically after they had been killed. Typically, an eye with a severed artery showed signs of acute damage within 2 days after the operation. This occurred in less Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933211/ on 08/12/2017 1006 Reports IOVS, April 1999, Vol. 40, No. 5 than 5% of the cases of partial optic nerve crush, but in 100% of the cases of intraorbital axotomy of the optic nerve (data not shown). Intravitreal Injection of NMDA Mice were first anesthetized. A small incision was made with a 30-gauge needle 0.5 mm to 1,0 mm behind the limbus in the superior region of the globe of one eye, through the conjunctiva and sclera. For microinjcctions, a glass micropipet was passed through this incision at a 40° to 50° angle to the equator. In animals with dilated pupils, it was possible to view the needle entering the vitreous. The eyes were routinely injected with 2 /xl of solution. For NMDA injections, we prepared balanced saline solution containing 5 mM to 80 mM NMDA (Research Biochemicals International, Natick, MA). For control experiments, eyes were injected with balanced saline solution alone. Only one eye of each mouse was ever injected. Occasionally, this procedure created cataracts in mice, possibly due to damage to the lens with the micropipet. Mice that had developed cataracts were killed and not used for analysis. Quantification of Cell Loss in the Retinal Ganglion Cell Layer Experimentally induced cell loss in the retinal ganglion cell layer (GCL) was measured from histologic sections of the mouse retina. In each mouse, one eye was operated on leaving the other eye for the unoperated control. At select time points after surgery, the mice were killed and the eyes were enucleated and fixed in 100 mM phosphate buffer containing 4% (wt/vol) paraformaldehyde and 2.5% (wt/vol) glutaraldehyde. After fixation the retinas were removed and embedded in glycolmethacrylate (|B4-Plus; Polysciences, Warrington, PA). Each retina was cut into transverse sections (2-jxm thickness) extending from the peripheral retina to the optic disc. Histologic landmarks, such as the ciliary epithelium and the edge of the optic disc, allowed for orientation of the sections from both eyes of each mouse for counting. Representative sections (12-16 total for each eye) were cut from both the superior and inferior retinas. The sections were then stained with 4,6-diamidino-2-phenylindole (DAPI; Boehringer Mannheim Biochemicals, Indianapolis, IN) to fluorescently label all the nuclei. Stained nuclei in the GCL were then counted in photographs of 2 microscopic fields of each section corresponding to approximately 400 /u.m of retina extending from the ciliary epithelium (peripheral retina) or from the optic disc (central retina). To compensate for slightly oblique sections, the number of cells in the GCL was corrected to the number of cells in the outer nuclear layer in the same field. The amount of cell loss was then calculated as a percentage of the cells present in the control eye of the same individual. In Situ Hybridization In situ hybridization to localize Thy-1 mRNA, a DNA sequence corresponding to the third exon of murine Thyl was amplified by the polymerase chain reaction using sequence-specific primers (5'-CTTGCAGGTGTCCCGAGGGC-3'J forward primer; 5-ATGGGATTCGCGCCCGAGAC-3', reverse primer) and mouse genomic DNA as a template. These primers generated a 305-bp DNA that was blunt-end cloned into the Smal site of the plasmid pBK-CMV (Stratagene, La Jolla, CA). Sequence analysis confirmed both the identity and orientation of this DNA. In situ FIGURE 1. DAPi-staLned sections of central regions of mouse retinas showing cell loss after optic nerve crush or intravitreal injection of NMDA. (A) Section from a control retina of a mouse 3 weeks after the optic nerve of the fellow eye was crushed. ONL, outer nuclear layer; INL, inner nuclear layer; GCL, ganglion cell layer. (B) Section from the same region of the retina of an experimental eye 3 weeks after optic nerve crush. (C) Section through the central retina of a control eye 6 days after intravitreal injection of 160 nanomoles NMDA into the fellow eye. (D) Section through the same region of an experimental eye 6 days after injection. Both treatments cause similar percentage losses of cells in the GCL at the times shown. Scale bar, 20 pm. hybridization was carried out using a whole-mount procedure described for the rat retina.7 Quantification of the number of positive cells was determined by comparing photographs of the DAPI-stained image with the Nomarski image of 5 to 8 sections from a minimum of two mice at each time point. Analysis of DNA Fragmentation Cells with fragmented DNA in histologic sections were identified by TUNEL staining. Harvested retinas were embedded in paraffin. Sections of 4-/xm thickness along the horizontal meridian were cut and stained as described previously. To quantify the TUNEL staining, all the positive cells in each layer of the retina of a section (6 sections per retina) were counted. RESULTS Cell Loss in the GCL after Optic Nerve Crush and NMDA Injection Optic nerve crush caused a gradual loss of the principle cell type in the GCL, which contained large round nuclei with prominent nucleoli consistent with the nuclear moq^hology of RGCs in the mouse retina (Figs. 1A, IB). A consistent loss of cells was first detected 1 week after crush and maximum loss occurred by 3 weeks (Fig. 2A). On average, this maximum loss was 57.8% ± 8.1% (mean ± SD, n = 6 mice) of the cells in the GCL. No further loss was detected in eyes examined up to 6 weeks after crush (data not shown). Intravitreal injections of NMDA caused the dose-dependent loss of the same principal population of cells in the GCL Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933211/ on 08/12/2017 IOVS, April 1999, Vol. 40, No. 5 Reports 8 10 12 Days Days B FIGUKE 2. Graphic representation of cell loss in the GCL. All data are shown as a percentage of cells in the GCL remaining in the treated eye relative to the control fellow eye for each mouse. Each data point represents the mean of at least four eyes ( ± SD). (A) Cell loss after optic nerve crush. No further loss of cells was detected after 3 weeks (data not shown). (B) Cell loss measured after intravitreal injection of 10 nanomoles NMDA (filled circles) or 160 nanomoles NMDA (open circles'). Injection of 10 nanomoles NMDA caused virtually no cell death, whereas maximal cell loss was measured after injection of 160 nanomoles. Intermediate doses of NMDA had proportionately intermediate effects on the kinetics of cell death (data not shown). Cell number was also observed to increase in the GCL after longer periods of exposure to high doses of NMDA. These additional cells did not resemble ganglion cells and may have appeared in the GCL as a consequence of gliosis. (Figs. 1C, ID). Low doses of NMDA (10 nanomoles) had virtually no effect on cell number, whereas higher doses (160 nanomoles injected) rapidly stimulated cell loss (Fig. 2B). Maximum loss in the GCL occurred 6 days after injection of 160 nanomoles NMDA and averaged 72.5% ± 12.1% (n = 6) of the cells. Depletion of Cells in the GCL Correlates with the Loss of Thyl mRNA To confirm that optic nerve crush and NMDA injection caused the death of RGCs, we also examined the loss of expression of Thyl by in situ hybridization. Thyl is predominantly expressed by RGCs in the retina, so it serves as a marker for these cells in this tissue. In control retinas 67.5% ± 6.5% (n = 8) of the cells in the GCL were Thyl-positive. By 2 weeks after optic nerve crush, no Thy 1 -positive cells were detected in the GCL. Similarly, no Thy-1 -positive cells were detected in retinas 4 days after injection of 160 nanomoles NMDA. Time-course experiments suggest that loss of Thy-1 mRNA precedes actual cell death in the retina (Li Y, Schlamp CL, and Nickells RW, unpublished data). It is also noteworthy that the maximum number of cells lost after NMDA injection (72.5% ± 12.1%) closely matched the number of Thyl-posixive cells in the control retina (67.5% ± 6.5%). Characteristics of Cell Death in the GCL Dying cells resulting from optic nerve crush or NMDA injection exhibited identical characteristics, including highly condensed (pyknotic) nuclei, fragmentation of the cell body, and a lack of residual debris (data not shown). Neither procedure elicited an inflammatory response, even though NMDA injection caused the rapid death of the majority of GCL cells. Dying cells also exhibited DNA fragmentation as assayed by TUNEL staining (Fig. 3). Peak TUNEL staining in the GCL occurred 2 days after injection of 160 nanomoles NMDA and 1 week after optic nerve crush (Fig. 4). NMDA injection also stimulated cell death in the inner nuclear layer, although the total number of TUNEL-positive cells was lower than in the GCL. DISCUSSION We adapted two protocols that stimulate RGC death in rats to study RGC death in mice. The first method, optic nerve crush, causes ganglion cell death possibly by blocking retrograde transport of neurotrophic factors from the brain to the RGC soma. In mice, this procedure causes a gradual loss of cells in the GCL over a 3-week period, which is similar to the rate of cell loss observed in rats after optic nerve transection.8 The major difficulties in adapting this protocol for mice were accessing the optic nerve in the orbit without causing excessive bleeding from damaged vessels in the fascia surrounding the ocular muscles and damaging the RGC axons without severing the central retinal artery. Bleeding can be avoided by using GCL A — B 1007 ft, FIGURE 3- TUNEL-stained mouse retinas after various treatments. (A) Control retina from a mouse 2 days after intravitreal injection with 2 /xl balanced saline solution. ONL, outer nuclear layer; INL, inner nuclear layer; GCL, ganglion cell layer. (B) Control retina treated with DNase I to nick the DNA in all the nuclei as a positive control for TUNEL. (C) Retina harvested from an eye 1 week after optic nerve crush. A single TUNEL-positive cell is present in the GCL. (D) Retina harvested from an eye 2 days after intravitreal injection of 160 nanomoles NMDA. At least 7 TUNEL-positive cells are visible in the GCL. Scale bar, 20 /urn. Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933211/ on 08/12/2017 1008 Reports IOVS, April 1999, Vol. 40, No. 5 c o do not survive this procedure long enough to measure an effect on RGC survival (data not shown). In mice, the injection of NMDA causes a dose-dependent loss of cells in the GCL, which occurs over a period of 6 days at the highest concentration tested. As with optic nerve crush, similar kinetics of RGC loss have been reported in rats injected with comparable doses of NMDA.4 NMDA injection also stimulated the death of a small number of cells in the inner nuclear layer. These cells were situated in the proximal region of this cell layer, which is generally populated by amacrine cells. Several different cell types in this layer express NMDA receptor subunits, although only amacrine cells appear to express the same subunits detected in RGCs. In addition, biochemical and histologic evidence also suggest that amacrine cells are adversely affected by NMDA.4 It is also possible that some of the affected cells were displaced RGCs, although the number of TUNEL-positive cells in this layer exceeded the number of 7frj//-positive cells identified in control retinas (data not shown). The characteristics of cell death stimulated by both optic nerve crush and NMDA injection included features of apoptosis. Dying cells contained pyknotic condensed nuclei, cellular fragmentation, and DNA fragmentation. In addition, neither treatment resulted in the accumulation of cellular debris and inflammation normally associated with necrosis. The observation that cells in the GCL of mice die by apoptosis is consistent with several other studies in rats, rabbits, and primates. 1 5, I 4- 0) a> '55 o a•. 1. UJ z 1 2 3 4 Weeks Acknowledgments 8 B 10 12 Days FIGURE 4. Graphs showing the peak periods of cell death in sections of the entire retina as a function of TUNEL staining. Each data point represents the mean number of TUNEL-positive cells/section obtained from 4 mice (6 sections each) (± SD). (A) Optic nerve crush showing the results for the GCL only. No TUNEL-positive cells were detected in other retinal layers after optic nerve crush. (B) NMDA (160 nanomoles) injection showing the counts for both the ganglion cell layer (GCL) and the inner nuclear layer (INL). For each treatment, maximum TUNEL staining preceded the point of maximum cell loss. blunt dissection to create a window in the fascia to access the nerve. Damage to the central retinal artery can be avoided by clamping the nerve with a pair of self-closing Dumont forceps. This clamp is sufficient to damage axons without permanently damaging the major blood vessels. The alternative to crushing the optic nerve is axotomy. A complete transection of the optic nerve in the eye orbit is impossible because the artery is still closely apposed to the nerve at this point. Others have circumvented this problem by accessing the nerves of newborn mice at a more posterior site using an intracranial approach. This method proved to be unsuitable for adult mice, many of which The authors thank Paul Kaufman and Leonard Levin of the University of Wisconsin, Madison, for helpful discussions and critical review of the manuscript and Soesiawati Darjatmoko for assistance with the handling of the mice. References 1. Nickells RW. Retinal ganglion cell death in glaucoma: the how, the why, and the maybe./ Glaucoma. 1996;5:345-356. 2. Johnson JE, Barde Y-A, Schwab M, Thoenen H. Brain-derived neurotrophic factor supports the survival of cultured rat retinal ganglion cells. / Neurosci. 1986;6:3031-3038. 3. Mey J, Thanos S. Intravitreal injections of neurotrophic factors support the survival of axotomized retinal ganglion cells in adult rats in vivo. Brain Res. 1993;602:304-317. 4. Siliprandi R, Canella R, Carmignoto G, et al. N-methyl-D-aspartateinduced neurotoxicity in the adult rat retina. Vis Neurosci. 1992; 8:567-573. 5. Vorwerk CK, Lipton SA, Zurakowski D, Hyman BT, Sabel BA, Dreyer EB. Chronic low-dose glutamate is toxic to retinal ganglion cells: toxicity blocked by memantine. Invest Ophthalmol Vis Set. 1996;37:l6l8-l624. 6. Isenmann S, Wahl C, Krajewski S, Reed JC, Bahr M. Up-regulation of Bax protein in degenerating retinal ganglion cells precedes apoptotic cell death after optic nerve lesion in the rat. Eur JNeurosci. 1997:9:1763-1772. 7. Levin LA, Schlamp CL, Spieldoch RL, Geszvain KM, Nickells RW. Identification of bcl-2 family genes in the rat retina. Invest Ophthalmol Vis Sci. 1997;38:2545-2553. 8. Berkelaar M, Clarke DB, Wang Y-C, Aguayo AJ. Axotomy results in delayed death and apoptosis of retinal ganglion cells in adult rats. J Neurosci. 1994;l4:4368-4374. Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933211/ on 08/12/2017 JOVS, April 1999, Vol. 40, No. 5 Effect of Staurosporine on Outflow Facility in Monkeys Baohe Tian, B'Ann T. Gabelt, and Paul L Kaufman PURPOSE. TO determine the effect of the serine-threonine kinase inhibitor staurosporine on outflow facility in living monkeys. METHODS. Total outflow facility was determined by two- level constant pressure perfusion of the anterior chamber bilaterally before and after intracameral infusion of staurosporine or vehicle in opposite eyes. RESULTS. Intracameral staurosporine dose-dependently doubled outflow facility, with 0.1 \xM, 1 /LIM, and 10 juM being subthreshold, effective, and maximal doses, respectively. At 50 /xM, intracameral staurosporine was less effective than 10 /xM on facility and induced corneal toxicity. CONCLUSIONS. The broad-spectrum protein kinase inhibitor staurosporine increases outflow facility in living monkeys, perhaps by affecting the trabecular meshwork cytoskeleton. (Invest Ophthalmol Vis Sci. 1999;40:1009 -1011) T he serine-threonine kinase inhibitor H-7 (l-(5-isoquinolinylsulfonyl)-2-methylpiperazine) inhibits acto-myosin contractility and thereby leads to deterioration of the actin microfilament system and perturbation of its membrane anchorage, in turn reducing tension at cell- cell and cell- extracellular matrix adherens junctions in several types of cultured cells, including human trabecular meshwork cells.1"4 H-7 also inhibits pilocarpine-induced contraction of isolated monkey ciliary muscle strips in vitro and pupillary constriction in vivo, probably by disrupting the actin filament network in the ciliary and iris sphincter smooth muscle cells.5 In living monkeys, topical or intracameral H-7 increases outflow facility and reduces intraocular pressure,3 perhaps due to similar effects on the actin cytoskeleton of the trabecular meshwork. The serine-threonine kinase inhibitor staurosporine depletes actin microfilament bundles in cultured rat astrocytes,6 inhibits contraction of guinea pig airway smooth muscle cells induced by the protein kinase C activator phorbol myristate acetate,7 and inhibits intracellular Ca2+-dependent contractions induced by various agonists in rabbit aortic strips.8 In view of the similarity of the effects of H-7 and staurosoprine on the actin filament network in cultured cells and on smooth From the Department of Ophthalmology and Visual Sciences, University of Wisconsin, Madison. Supported by grants from the National Eye Institute (EY02698), National Institutes of Health, Bethesda, Maryland; Glaucoma Research Foundation, San Francisco, California; Research to Prevent Blindness, New York, New York; and the Ocular Physiology Research & Education Foundation, Madison, Wisconsin. Submitted for publication May 7, 1998; revised November 3, 1998; accepted December 17, 1998. Proprietary interest category: P, C3, C5, Ccl, Cc3, Cc4, Cc6. Reprint requests: Paul L. Kaufman, Department of Ophthalmology and Visual Sciences, University of Wisconsin-Madison, F4/328 CSC, 600 Highland Avenue, Madison, WI 53792-3220. Reports 1009 muscle contraction, we determined the effect of staurosporine on the outflow facility in living monkey eyes. METHODS Fourteen adult cynomolgus monkeys (Macaca fascicularis) of both sexes, weighing 2.5 kg to 6.0 kg, were anesthetized with intramuscular ketamine (10 mg/kg), followed by intramuscular (35 mg/kg) or intravenous (15 mg/kg) pentobarbital-Na. Total outflow facility was determined by two-level constant pressure perfusion of the anterior chamber (AC) with Bariiny's solution, using one double-branched and one single-branched needle and correcting for internal apparatus resistance.9 Most monkeys were used in more than one protocol, had undergone more than one prior perfusion, or both, but none within the preceding 5 to 6 weeks; all were free of AC cells and flare. After 35 minutes of baseline facility measurement, the AC was exchanged with 2 ml of 0.1 /nM to 50 /xM staurosporine (Sigma, St. Louis, MO) solution in one eye, vehicle (0.01% to 5% dimethyl sulfoxide [DMSO] in Barany's solution) in the other, for 10 to 15 minutes. The reservoirs were then immediately filled with the corresponding solutions, closed for 45 minutes, and reopened for 45 minutes of post-drug facility measurement. In some experiments, the monkey received two different doses on one occasion, with a higher dose (1.0 JLLM or 10 /xM) administered to the same eye following post-lower dose (0.1 JLLM or 1.0 /xM) facility measurements. All investigations were in accordance with University of Wisconsin and NIH guidelines and with the ARVO Statement on the Use of Animals in Ophthalmic and Vision Research. RESULTS AC exchange with 0.1 /LtM to 50 /xM staurosporine produced a dose-dependent facility increase; 0.1 /xM was ineffective, whereas 1 /nM, 10 /LIM, and 50 /uM staurosporine increased facility by 69% ± 20% (n = 8, P < 0.02), 168% ± 48% (n = 8, P < 0.01), and 117% ± 39% (n = 4, P < 0.1), respectively, relative to baseline and adjusted for contralateral control eye changes (Fig. 1, Table 1). The initial facility values on restarting the perfusion after die closed reservoir waiting period were only slightly increased relative to the control eyes, but the increase was dose-dependent (Fig. 1). At 50 ju,M, corneal cloudiness and edema were present the day after perfusion and persisted for at least several months. No apparent corneal toxicity was observed by casual examination under normal room light 1 day after or by slit-lamp 5 to 8 weeks after 0.1 jixM, 1 /LtM, or 10 /xM intracamerally. DISCUSSION The serine-threonine kinase inhibitor staurosporine, which has cytoskeletal effects similar to those of H-7 in cultured cells,6 also has a similar facility-increasing effect in the living monkey eye at concentrations (^1 jtxM) comparable to that (100 nM) reported for cytoskeletal effects in rat astrocytes.6 Similar to H-7, the initial facility values were only slightly elevated compared with the ipsilateral baselines after intracameral exchange infusion of 1 /xM or 10 |LtM staurosporine, with substantial facility elevation produced only after continued perfusion.3 Most likely, drug-induced Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933211/ on 08/12/2017 1010 IOVS, April 1999, Vol. 40, No. 5 Reports 1.3 Staurosporine 1.1 n=4 n=8 Vehicle 0.9 0.1 p.M Staurosporine LOjiM Staurosporine 0.7- X 0.5- T Hi-1! 0.3" I Res Closed 0.1- a 1.2- O 1^ I I I0.1 \iM Staurosporine Res Closed I l.OuM Staurosporine n=8 n=4 lOuM Staurosporine 50nM Staurosporine 9 O 0.8 H 0.6- X^ 0.4- j.-1- Res Closed 0.2- Res Closed 50)iM Staurosporine 10(iM Staurosporine 10 I 30 50 70 90 110 i 130 10 30 i BL 50 70 90 110 130 1 BL Time (min) FIGURE 1. Effect of intracameral exchange infusion with 0.1 JUM to 50 JU-M staurosporine on outflow facility in monkeys. BL, Baseline; Res, Reservoir. Data are means ± SEM /xl/min per mm Hg for n animals, each contributing one staurosporine- and one vehicle-treated eye. Difference between eyes =£0.0 by the two-tailed paired f-test: *P < 0.1, }P < 0.05. architectural changes within the meshwork produce only slight resistance washout at physiological flow rates, whereas at the higher flow rates and pressure heads during perfusion, disruption of resistance-relevant structures and reduction of flow resistance are more substantial.3 At 50 /xM, staurosporine produced a substantial initial facility increase, perhaps suggesting that at higher doses the drug may render the meshwork architecture unstable even at normal flow rates. TABLE 1. Effect of Intracameral Staurosporine on Outflow Facility Outflow Facility (fil/min/mm Hg) Stau Dose 0.1 pM in 0.01% DMSO (n = 4) BL Rx Rx/BL 1.0 jaM in 0.1% DMSO (n = 8) BL Rx Rx/BL 10 JU-M in 1% DMSO (n = 8) BL Rx Rx/BL 50 jaM in 5% DMSO (n = 4) BL Rx Rx/BL 0.30 ± 0.27 ± 0.97 ± 0.28 ± 0.50 ± 1.96 ± 0.32 ± 0.74 ± 2.26 ± 0.33 ± 0.51 ± 1.55 ± 0.09 0.07 0.05 0.05 0.08 0.25 0.05 0.18 0.33 0.06 0.10 0.14 Veh 0.29 ± 0.28 ± 0.99 ± 0.30 ± 0.33 ± 1.19 ± 0.44 ± 0.39 ± 1.00 ± 0.32 ± 0.24 ± 0.79 ± 0.09 0.08 0.04 0.05 0.04 0.12 0.08 0.08 0.20 0.07 0.04 0.15 Stau/Veh 1.04 ± 0.14 1.03 ± 0.17 0.98 ± 0.04 0.96 ±0.11 1.57 ± 0.25 1.69 ± 0.20t 0.81 ± 0.12 1.99 ± 0.43 2.68 ± 0.48* 1.05 ± 0.09 2.17 ± 0.28f 2.17 ± 0.39* Values are means ± SEM for n animals. Staurosporine administered by exchange perfusion; BL, baseline; Rx, post-drug facility; Stau, staurosporine-treated eye; Veh, vehicle-treated eye; post-drug data encompasses 45 min, beginning 45 min after drug administration. i * P < 0.1, t P < 0.05, t P < 0.01 for ratios different from 1.0 by the two-tailed paired f-test. Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933211/ on 08/12/2017 Reports IOVS, April 1999, Vol. 40, No. 5 The overall facility increase, relative to both ipsilateral baseline values and contralateral vehicle-treated control eyes, induced by 50 p,M staurosporine was no greater, and may have been less, than that induced by 10 yM staurosporine. A similar phenomenon was observed with cytochalasin D, l 0 where a 5X maximal intracameral dose for increasing facility actually caused a facility decrease in —40% of eyes. Also, because a concentration of DMSO in the AC of 4% or greater tends to reduce outflow facility and blunt resistance washout,'' the 5% concentration likely caused the trend toward reduction of facility in the control eyes, and presumably in the drug-treated eyes as well, for 50 /AM staurosporine. Staurosporine at 50 JLLM produced corneal cloudness and edema, perhaps suggesting separation of corneal endothelial cells and elevation of corneal endothelium permeability. However, 1 JXM and 10 ju,M staurosporine significantly increased facility without corneal toxicity apparent to gross observation. Studies involving multiple doses, more sensitive measurements of corneal structure and function, and older animals are needed. Preliminary ultrastructural studies indicate that administration of H-7 into monkey eyes induces generalized relaxation and apparent expansion of the trabecular meshwork and Schlemm's canal (Sabanai I, Gabelt B, Tian B, Kaufman P, and Geiger B, unpublished data, August 1998). This, in conjunction with data showing that H-7 relaxes human trabecular meshwork cells in culture, 12 suggests that H-7 may affect facility by inhibiting cell contractility, leading to "relaxation" of the trabecular outflow pathway and expansion of the draining surface, and thus allowing more extensive flow through the meshwork. Although staurosporine has somewhat different specificities than H-7,13'14 both are relatively broad serine-threonine protein kinase inhibitors and have similar cytoskeletal and physiological effects in cultured cells and smooth muscles, and on outflow facility in living monkeys. Nonetheless, further physiological and morphologic studies are needed to clarify the mechanisms by which these and related compounds affect outflow facility. References 1. Birrell GB, Hedberg KK, Habliston DL, Griffith OH. Protein kinase C inhibitor H-7 alters the actin cytoskeleton of cultured cells.y Cell Physiol. 1989;l4l:74-84. Mechanism of Exercise-Induced Ocular Hypotension Bruce Martin? Alon Harris,2 Ted Hammel,1 and Vic Malinovsky5 PURPOSE. Although acute dynamic exercise reduces intraocular pressure (IOP), the factors that provoke this response remain ill-defined. To determine whether changes in colloid osmotic pressure (COP) cause the IOP changes during exercise, standardized exercise was performed after dehydration and hydration with isosmotic fluid. METHODS. Progressive cycle ergometer exercise to volitional exhaustion was performed after 4 hours' dehydration, and after hydration with 946 ml isosmotic liquid (345 1011 2. Volberg T, Geiger B, Citi S, Bershadsky AD. Effect of protein kinase inhibitor H-7 on the contractility, integrity, and membrane anchorage of the microfilament system. Cell Motil Cytoskel, 1994;29:321338. 3. Tian B, Kaufman PL, Volberg T, Gabelt BT, Geiger B. H-7 disrupts the actin cytoskeleton and increases outflow facility. Arch Ophthalmol. 1998; 116:633-643. 4. Liu X, Glasser A, Croft MA, Polansky JR, Fauss DJ, Kaufman PL. Effect of H-7 on cultured human trabecular meshwork (HTM) cells [ARVO Abstract]. Invest Ophthalmol Vis Set. 1998;39(4):S705. Abstract nr 3235. 5. Tian B, Millar C, Kaufman PL, Bershadsky A, Becker E, Geiger B. H-7 effects on the iris and ciliary muscle in monkeys. Arch Ophthalmol. 1998;116:1070-1077. 6. Mobley PL, Hedberg K, Bonin L, Chen B, Griffith OH. Decreased phosphorylation of four 20-kDa proteins precedes staurosporineinduced disruption of the actin/myosin cytoskeleton in nit astrocytes. Exp Cell Res. 1994;2l4:55-66. 7. Souhrada M, Souhrada JF. Inhibitor)' effect of staurosporine on protein kinase C stimulation of airway smooth muscle cells. Am Rev Respir Dis. 1993; 148:425- 430. 8. Sasaki Y, Seto M, Komatsu K, Omura S. Staurosporine, a protein kinase inhibitor, attenuates intracellular Ca (2+)-dependent contractions of strips of rabbit aorta. EurJPharmacol. 1991 ;202:367372. 9. Baniny EH. Simultaneous measurement of changing intraocular pressure and outflow facility in the vervet monkey by constant pressure infusion. Invest Ophthalmol, 1964;3:135-l43. 10. Kaufman PL, Erickson KA. Cytochalasin B and D dose-outflow facility response relationships in the cynomolgus monkey. Invest Ophthalmol Vis Sci. 1982;23:646-650. 11. Kiland JA, Peterson JA, Gabelt BT, Kaufman PL. Effect of DMSO and exchange volume on outflow resistance washout and response to pilocarpine during anterior chamber perfusion in monkeys. Curr Eye Res. 1997;l6:1215-1221. 12. Gills JP, Roberts BC, Epstein DL. Microtubule disruption leads to cellular contraction in human trabecular meshwork cells. Invest Ophthalmol Vis Sci, 1998;39:653-658. 13- Takagi A, Yamada Mizutani M, Tomioka N, Itai A. Inhibition mechanisms of staurosporine and H7 to cAMP-dependent protein kinase through docking study. Chem Pharm Bull. 1996;44:6l8-620. 14. Cagnoli CM, Kharlamov E, Atabay C, Uz T, Manev H. Apoptosis induced in neuronal cultures by either the phosphatase inhibitor okadaic acid or the kinase inhibitor staurosporine is attenuated by isoquinolinesulfonamides H-7, H-8, and H-9. /Mol Neurosci. 1996; 7:65-76. mOsM). In each experiment, venous blood taken before and immediately after exercise was analyzed for hematocrit, plasma protein concentration, total plasma osmolality, and plasma COP. RESULTS. Exercise in both experiments significantly reduced IOP and elevated COP (each P < 0.01). Dehydration, compared with hydration, also significantly reduced IOP and elevated COP, when measured before and after exercise (P < 0.05). The correlation of mean IOP with mean COP, over the entire range created by varying exercise and hydration statuses, was statistically significant (r = -0.99; P < 0.001). In contrast, other indexes of hydration status, including hematocrit, total plasma osmolality, and plasma protein concentration, failed to change as IOP changed and failed to correlate with IOP, on either a group or individual basis, in conditions of varying levels of exercise and hydration. Downloaded From: http://iovs.arvojournals.org/pdfaccess.ashx?url=/data/journals/iovs/933211/ on 08/12/2017