* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Heart Failure - Laura J. Langenhop RN, BSN, PCCN, CHFN
Survey
Document related concepts
Saturated fat and cardiovascular disease wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Electrocardiography wikipedia , lookup
Rheumatic fever wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Heart failure wikipedia , lookup
Heart arrhythmia wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Transcript
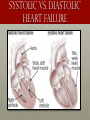
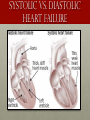
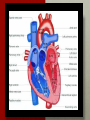
Hemodynamics and common medications in the heart failure patient Laura J Langenhop BSN, RN, PCCN, CHFN The Wright State University Class of 2015 oBJECTIVEs • Identify the difference between systolic and diastolic heart failure. • Demonstrate understanding for the use of inotropes in heart failure patients. • Describe the pathophysiology of heart failure. • Identify medications used in heart failure. • Demonstrate understanding of the heart failure core measures. HOW DID MY PATIENT GET HEART FAILURE? • 1. Poorly Treated HTN • 5. CAD • 2. Myocardial Infarction • 6. Cardiomyopathies (ex. Alcohol-induced, viral, drug-induced, restrictive, hypertrophic) • 3. Valve Disease • 4. Atrial Fibrillation • 7. Congenital Heart Defects (Yancy et al., 2013; Papadakis, McPhee, & Rabow, 2014) SYSTOLIC VS. DIASTOLIC HEART FAILURE Systolic Heart Failure • The problem is with the ejection or the “pumping ability” • EF<40% by definition • Common Causes: MI, CAD, untreated HTN, dilated cardiomyopathy (Yancy et al., 2013) SYSTOLIC VS. DIASTOLIC HEART FAILURE Diastolic heart failure • The problem is with a stiff ventricle and not being able to fill. • EF >40% • Common Causes: Age, Women, HTN, AFIB, CAD, Restrictive Cardiomyopathy, Amyloidosis (Yancy et al., 2013) NYHA versus ACC/AHA Stages of heart failure What does the patient look like? Now We’re going to the cath lab…. Are they….. • Wet? • Dry? • Have Low cardiac Output? • Pulmonary HTN? • Do they have a blockage? Right Heart Catheterization Left Heart Catheterization • Venous sheath is placed • Arterial sheath is placed • Looking at filling pressures of the heart to assess volume status • Looking at coronary arteries and need for intervention (i.e. PCI, balloon) • DO NOT need IV fluids or aspirin prior to procedure. • Need Aspirin 324 mg ordered and 0.9% NS @ 30mL/hr. CATH LAB REPORT Normal Pressures Example of Report RA 0-8 mm/Hg 10 RV 15-25/0-8 mmHg 42/14/24 PA 15-25/8-10 mmHg 44/17/27 PCWP 6-12 mmHg 15 CO ~4 to 8 L/min 3.8 L/min CI 2.4 to 4 L/min/m2 2.0 L/m/m2 Common Inotropic agents renalfellow.blogspot.com MILRINONE (Primacor) • Phosphodiesterase inhibitor • • • Vasodilation Inotropic Effects Little chronotropic effect • Onset: 5-15 minutes • Half-life: ~2.5 hours • Adverse Reactions: Hypotension, Arrhythmias, Headache, Chest Pain • Uses: Volume overload with decreased CO/CI, Right-sided heart failure following LVAD implant (Marino, 2014) Dobutamine (dobutrex) • Stimulates beta1-adrenergic receptors causing increased contractility and heart rate. • Onset of Action: 1-10 minutes • Half-Life: ~2 minutes • Adverse Reactions: Arrhythmias, Tachycardia, Angina, Palpitations • Uses: Cardiac Decompensation, Low CO/CI, Cardiogenic/Septic Shock • **Should not be on beta-blockers if on this medication. (Marino, 2014) DOPAMINE • Stimulates both adrenergic and dopaminergic receptors. Goal is to increase cardiac stimulation and increase renal vasodilation. • Onset of Action: ~5 minutes • Half-Life: ~2 minutes • Adverse Reactions: Low/High BP, Palpitations, Arrhythmias, Nausea, Vomiting, Tissue Necrosis (must go through central line) • Uses: Inotropic support and renal blood flow. (Marino, 2014) Qualifications for inotropic agents • Cardiac Index <2.2 L/min/m2 prior OR Wedge >20 mmHg prior to starting. • Dyspnea at rest • Maximum dosage of Digoxin, Loop Diuretic, ACE, or vasodilator (unless reason documented). • Qualification for Home Inotropic Therapy: Need CI increased by 20%, wedge pressure decrease by 20%, and improved shortness of breath pathophysiology OF heart failure (Marino, 2014) DIURETICS lOOP DIUERTICS (Furosemide (Lasix), Torsemide (demadex), and bumetanide (Bumex) • Given for Acute Decompensated Heart Failure in Intravenous Form. • Loop diuretics work by increasing the excretion of water and sodium excreted by the kidneys. • Side Effects: Muscle cramps, hypokalemia, hypomagnesemia, increase in Creatinine, dizziness, hypotension. • Consider to Hold: Dramatic increase in Creatinine or patient is hypotensive. • On discharge, patient’s will go home with oral Lasix, Bumex, oral Demadex Felker et al., 2011 dIURETIC CONVERSION Bumex Lasix Demadex Equivalent Dose 1 mg 40 mg 20 mg Bioavailability ~60-80% 50-60% 80% Usual Dose 0.5 mg-2 mg (QD or BID) 20 mg-80 mg (QD-BID) 10 mg-40 mg (QD-BID) Duration 4 hours 6 hours 6 hours (LexiComp, 2015) Thiazide diuretics (Metolazone, hydrochlorOthiazIDe, DIURIL) • Inhibits sodium reabsorption in the distal tubules causing increased excretion of sodium and water. • Diuril will be seen in combination with lasix in the IV form • Metolazone may be given as needed, depending on the patient’s resistance to diuresis. • Side Effects: Hypotension, Dizziness, fatigue, headache, N/V/D, hypokalemia, hypomagnesemia Aldosterone antogonists (ex. Spirolactone, Eplerenone) • Competes with aldosterone for receptor sites thereby increasing sodium and water excretion. • Uses: NYHA Class III-IV Heart Failure • Adverse Effects: Hyperkalemia, Hypotension, Headache, Confusion, Gynecomastia, Renal Failure, Nausea, Vomiting, Diarrhea. • Reasons to Hold: If K is >5 or Cr. >2.5 ACCF/AHA 2013 Heart Failure Guidelines Tolvaptan (samsca) • Used in patients with hypervolemic or euvolemic hyponatremia • Vasopressin antagonist causing excretion of free water without loss of electrolytes. This results in fluid loss, increased urine output, and increased serum Na levels. • Normal dosing: 15 mg-60 mg • When to hold: If serum Na level increases >10 mEq in 24 hours or if serum Na level is within normal level. Ace-iNHIBITORS (i.e. lisinopril, captopril, enalapril) • Prevents conversion of Angiotensin 1 to Angiotensin 2 causing vasodilation. Reduce Afterload and help with remodeling. • Indication: High Blood pressure, <40% EF. • Adverse Reactions: Hypotension, Renal Insufficiency, Hyperkalemia, Angioedema, Cough, Swelling of the tongue *EMERGENCY. • Reasons to Hold: Acute increase in Creatinine, K >5, and hypotension www.medictest.com Angiotensin II RECEPTOR BLOCKERS [Volsartan (Diovan,), losartan (cozaar)] • Indications: HTN, EF <40% • Blocks vasoconstriction and aldosterone-secreting effects of angiotensin II. Increases urinary flow rate and increases excretion of chloride, magnesium, uric acid, calcium, and phosphate. • Adverse Reactions: Fatigue, Hyperkalemia, Hypotension • Reasons to hold: Acute increase in Cr., K >5, and hypotension Vasodilators Hydralazine Isosorbide Mononitrate (Imdur) • Direct vasodilation of arterioles with decreased systemic resistance. • Vasodilates peripheral veins and arteries. Decreases cardiac oxygen demand by decreasing pre-load. • Adverse Reactions: Headache, Hypotension, dizziness. • Improves collateral flow to ischemic regions. • Consider holding for hypotension • Adverse Reactions: headache, flushing, dizziness, fatigue, N/V/D, hypotension. Taylor et al., 2004 African American Heart Failure Trial Beta-bLOCKERS (I.e. mETOPROLOL SUCCINATE, CARVEDILOL) • Metoprolol Succinate • Beta-1 adrenergic Selective inhibitor • Shown to decrease mortality and hospitalizations in patient’s with class IIIV heart failure • Carvedilol • Non-selective Beta-1 and Beta-2 adrenergic Selective inhibitor. • Has shown to decrease PCWP, pulmonary resistance, renal vascular resistance, decreased SVR • Helps to decrease heart rate and blood pressure in order for the heart to “pump” more effectively as well as remodeling the heart. • Adverse Reactions: Fatigue, bradycardia, dizziness, hypotension (COMET Trial, MERIT-HF Trial, Yancy et al., 2013) DIGOXIN • Heart Failure: • Increases intracellular sodium promoting calcium influx in the cell leading to increased contractility. • Inhibits reabsorption of sodium • Increases CO and renal blood flow • +Inotropic effect • AFIB: • Used to suppress the AV node conduction in order to increase refractory period. • Enhances Vagal Tone Reasons we stop this: Bradycardia, Renal insufficiency Heart failure CORE MEASURES • Documented Left Ventricular Ejection Fraction • ACE/ARB (EF <40%) • Documentation of Beta-Blocker (Carvedilol, Metoprolol Succinate, or Bisoprolol) • Post-discharge heart failure appointment within 7 days of Discharge (GWTG, CMS, & TJC, 2014) References • American Heart Association (2014). Heart Failure Core Measures.http://www.heart.org/idc/groups/heartpublic/@wcm/@private/@hcm/@gwtg/documents/downloadable/ucm_458657.pdf • Centers of Medicare and Medicaid. (2015). Medicare inotropic qualification checklist. http://www.pdfdrive.net/medicare-inotropic-qualification-checklist-e9799412.html • Felker, G. M., O’Connor, C. M., & Braunwald, E. (2009). Loop Diuretics in Acute Decompensated Heart failure necessary? evil? A necessary evil? Circulation, 2, 56-62. doi:10.1161/_CIRCHEARTFAILURE.108.821785 • Felker, M.G., Lee, K.L., Bull, D.A., Redfield, M.M., Stevenson, L.W.,…& O’Connor C.W. (2011). Diuretic strategies in patients with acute decompensated heart failure. New England Journal of Medicine, 364, 797-805. doi: 10.1056/NEJMoa10005419. • Fuster, V., Asinger, R.W., Cannom, D.S., Crijns, H.J., Frye, R.L., & Torbicki, A. (2001). Guidelines for the management of patients with atrial fibrillation. Circulation, 104: 2118-2150. http://circ.ahajournals.org/content/104/17/2118.full • Jessup, M., Abraham, W. T., Casey, D. E., Feldman, A. M., Francis, G. S., Ganiats, T. G., ... Yancy, C. W. (2009, March 26). 2009 focused update: ACCF/AHA guidelines for the diagnosis and management of heart failure in adults. Circulation, 119, 1977-2016. doi:10.1161/CIRCULATIONAHA.109.192064 • Lexicomp (2014). Retrieved from http://webstore.lexi.comPDA-software-for-nurses • Lindenfeld, J., Albert, N.M., Boehmer, J.P., Collins, S.P., Ezekowitz, J.A.,…Walsh, M.A. (2010). Executive summary: HFSA 2010 Comprehensive heart failure practice guideline. Journal of Cardiac Failure, (16)6. 1-259. http://www.heartfailureguideline.org/_assets/document/Guidelines.pd • Marino, P. L. (2014). The ICU book (4th ed.). Philadelphia, PA: Wolters Kluwer Health/Lippincott Williams & Wilkins. • Papadakis, S. J. McPhee, S. J. & Rabow, M.W. (2014), Current medical diagnosis & treatment 2014 (49th ed). New York, NY: Appleton & Lange • Taylor AL, Ziesche S, Yancy C, et al; (2004). the African-American Heart Failure Trial Investigators. Combination of isosorbide dinitrate and hydralazine in blacks with heart failure. New England Journal of Medicine, 351:2049-2057 • Yancey, C.W., Jessup, M., Bozkurt, B., Butler, B.,..& Wilkoff, B.L. (2013). 2013 ACCF/AHA guidelines for the management of heart failure. Circulation, 128:1810-1852. doi: 10.1161/CIR.0b013e31829e8776