* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download conjunctiva anatomy and physiology
Antibiotics wikipedia , lookup
Neglected tropical diseases wikipedia , lookup
Marburg virus disease wikipedia , lookup
West Nile fever wikipedia , lookup
Leptospirosis wikipedia , lookup
Chagas disease wikipedia , lookup
Oesophagostomum wikipedia , lookup
Clostridium difficile infection wikipedia , lookup
Hospital-acquired infection wikipedia , lookup
Trichinosis wikipedia , lookup
Human cytomegalovirus wikipedia , lookup
Middle East respiratory syndrome wikipedia , lookup
Onchocerciasis wikipedia , lookup
Hepatitis C wikipedia , lookup
Herpes simplex virus wikipedia , lookup
Sarcocystis wikipedia , lookup
Schistosomiasis wikipedia , lookup
Traveler's diarrhea wikipedia , lookup
Gastroenteritis wikipedia , lookup
Coccidioidomycosis wikipedia , lookup
Neonatal infection wikipedia , lookup
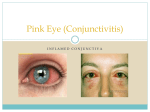
CONJUCTIVITIS THE 2017 FAMILY MEDICINE JOINT WOR KSHOP BY DR F A OLANIYAN MBBS Ib., MSc Ib.( Med Stat.& Epid), FWACP, FMCG P, CaRT Fellow Learning objectives At the end of the session your should be able to: • Correlate the structure with functions and com mon clinical presentations. • Identification of important anatomical landmar ks of conjunctiva. • Classify conjunctivitis. • Identify the common symptoms and signs of c onjunctival disease, differentiate various conju ntivitidies and manage. ANATOMY It is the mucous membrane covering the under surface of the lids and anterior part of the ey eball up to the cornea. Parts of conjunctiva • Palpebral; covering the lids—firmly adherent. • Forniceal; covering the fornices—loose—thro wn into folds. • Bulbar; covering the e yeball—loosely attach ed except at limbus. Conjunctival fornices • Transitional region between palp ebral and bulbar conjunctivae. • Superior fornix 10 mm from limb us. • Inferior fornix 8 mm from limbus . • Lateral fornix 14mm from limbus . • Medially absent. • Ducts of lacrimal glands open int o lateral part of superior fornix. Lymphatic drainage • Lymph vessels are arrang ed as a superficial and a d eep plexus in sub mucosa. • Ultimately as in the lids t o the pre auricular and su b-mandibular lymph glan ds. Incidence • Conjunctivitis is the most common cause of 'red eye'. • Conjunctivitis accounts for around 44% of al l eye problems presenting in general practic e [Manners 1997]. • 2-5% of all general practice consultations ar e eye related [Manners 1997]. • Viral conjunctivitis is more common than ba cterial conjunctivitis [Baum 1995]. Conjunctivitis The most common extraocular disorder Etiology: infection of microorganism physical injuries chemical injuries allergic disorder immunological disorder nutritional deficiency Symptomatology Non-Specific; • Lacrimation. • Irritation. • Stinging. • Burning. • Photophobia. • Redness. Specific; • Pain and FB sensation in corneal involvement. • Itching in allergic, blephritis and dry eyes. SIGNS • Type of discharge. • Type of conjunctival reaction. • Presence of membrane/ pseudomembrane. • Lymphadenopathy. DISCHARGE Exudate plus debris plus mucus plus tears. • Serous; watery exudate in acute viral and acute all ergic conjunctivitis. • Mucoid; mucus discharge in VKC and KCS (dry eyes). • Purulent; pus in severe acute bacterial conjunctivit is. • Mucopurulent; pus plus mucus in mild bacterial c onjunctivitis and Chlamydial conjunctivitis. Lymphadenopathy • Pre auricular and sub mandibular. 1. Viral infection. 2. Chlamydial infection. 3. Severe bacterial infections. (Gonococcal). Laboratory Investigations Indications: • • • • Sever purulent conjunctivitis. Follicular conjunctivitis: viral vs chlamydial. Conjunctival inflammation. Neonatal conjunctivitis. Laboratory Investigations—cont… • • • • • Cultures. Cytological investigations. Inoculation. Detection of viral and chlamydial antigens. Impression cytology for dry eyes, ocular cicatricia l pemphigoid, infection. • Polymerase chain reaction: small quantity of DNA for adenovirus, herpes simplex, chlamydia tracho matis. CLASSIFICATION OF CONJUNCTIVIS Morphological • • • • Papillary Follicular Pseudomembranous Membranous Discharge • • • • Serous Mucous Purulant Mucopurulant Etiological • Infective • Non-Infective: Allergic Autoimmune Toxic Chemical Degenerations Clinical • • • • Acute Sub-acute Chronic Recurrent Age • Neonatal • Childhood • Adult Neonatal • • • • • Chlamydial Gonococcal Other bacteria Viral Chemical Common Bacterial • Mucopurulant • Purulant • Membraneous CHLAMYDIAL OCULAR INFECTION S • Adult inclusion conjunctivitis. • Neonatal chlamydial conjunctivitis. • Trachoma. Viral • • • • • Adenoviral Picarna viral Herpes simplex Measles Chicken pox Allergic • • • • Acute allergic conjunctivitis Vernal keratoconjunctivitis Atopic keratoconjunctivitis Phlactenular keratoconjunctivitis Autoimmune • Phempegoid (Essential shrinkage of conjun ctiva) • Steven Johnson syndrome Chemical • Acid burns • Alkali burns • Others Management • Treat the cause: Anti-inflammatory agents Antibacterial • Antiallergic • Supportive • Specific Acute Bacterial Conjunctivitis Mucopurulant conjunctivitis • Caused by: Staph epidermidis and Staph aureus –usually. Strep pneumonae, H influensae and Morexella lucanatae occasionally Acute Bacterial Conjunctivitis • Symptoms: *Acute onset of redness, grittiness, burning and discharge. *Photophobia may be present (corneal involvement) *Stickiness of the eyelids *Usually bilateral disease • Signs: *Conjunctival hyperaema *Mild papillary reaction *Mucopurulant discharge *Lid crusting *No lymphadenopathy. *Normal VA Acute Bacterial Conjunctivitis Purulant cojunctivitis (Adult gonococcal) • Symptoms: *Hyperacute condition *Extremely profuse, thick, creamy pus from the eye or eyes • Signs: *Severe conjunctival chemosis *May be membrane formation *Periocular edema *Ocular tenderness *Gaze restriction *Lamphadenopathy *Corneal involvement • Treatment Systemic and topical antiboitics Chronic bacterial conjunctivitis • Causes: *Acute becoming chronic *Refractive errors *Secondary Misplaced lashes, CDC, chronic blephritis • Symptoms: • Burning and photophobia • Signs: *Congestion, and sticky discharge Treat: remove the cause antibiotics COMMON TOPICAL ANTIBIOTICS • • • • • • • • • • Trimethoprim + polymyxin B Azithromycin Genticin chloramphenicol Tobramycin Neomycin Ciprofloxacin Ofloxacin Levofloxacin gatifloxacin CHLAMYDIAL OCULAR INFE CTIONS CHLAMYDIAL OCULAR INFECTION S • Adult inclusion conjunctivitis. • Neonatal chlamydial conjunctivitis. • Trachoma. TRACHOMA • Etiology: Serotypes A, B, Ba & C of Chlamydia trach omatis. • Transmission: Common fly (major Vector), fomites, fi ngers. • Epidemiology: – – – – Endemic in Africa, Asia, Middle East & Australia. Leading cause of preventable blindness. Worldwide 360 million people affected. Six million people are blind from trachoma. TRACHOMA • Risk factors: – Poverty & deprived members of community. – Poor personal & community hygiene. – Infectious pool: Preschool children of both sexes & their c are providers. • Age: – Children: Follicular & inflammatory trachoma. – Young adults: Trachomatous scarring. – Middle-aged: Trichiasis & corneal opacity. • Sex: Trichiasis & blindness 2-4 times more common in wo men than men. PRESENTATION • During childhood. • Symptoms: – FB sensation. – Redness. – Lacrimation. – Scanty mucoid discharge. – Mucopurulent discharge if secondary infection. STAGES • I) Incipient: Characterized by: – Minute immature follicles in upper tarsal conjunctiva. – Cytoplasmic inclusions in conjunctival epithelium. – Stromal hyperemia & oedema. • IIa): Follicular hypertrophy: – Large soft expressible follicles in upper tarsus, fornix & limbus. – Punctate keratitis. – Follicular necrosis---Herbert’s pits. – Stromal infilteration by plasma cells & macrophages. STAGES • IIb): Papillary hypertrophy: – Trachoma of intense activity or chronic trachoma with superimposed bacterial infections. – Obscuration of follicles by papillary hypertrophy. • III): Cicatrizing trachoma: – Conjunctival Scarring. – Pannus formation. – Lacrimal gland obstruction. – Trichiasis. – Entropion. STAGES • IV): Healed stage: – Resolution of inflammation. – Replacement of follicles & papillae by scar tissue. DIAGNOSIS Clinical diagnosis of trachoma requires the presence of at least two of the following features: – – – – Conjunctival follicles on upper tarsal conjunctiva. Limbal follicles and their sequelae. Tarsal conjunctival scarring. Fibrovascular pannus. COMPLICATIONS • • • • • • • • Upper lid entropion Trichiasis. Xerosis – obliteration of lacrimal ducts or glands. Chlazion. Symblepharon – obliteration of lower fornix. Corneal ulceration. Corneal opacity. Pseudoptosis. MANAGEMENT • SAFE strategy developed by WHO: • Surgery: – To prevent blindness & limits progression of corne al scarring. – Can improve vision. • Antibiotics: – Azithromycin—1 G single dose (adults). – Children: 20mg/kg single dose MANAGEMENT • Erythromycin 250 mg QID for 4 weeks. (childr en 125mg/kg). • Tetracycline 250 mg QID for 4 weeks. • Topical tetracycline 1% 0.5 inch ribbon BD for 6 weeks. MANAGEMENT • Facial cleanliness: – Reduces risk & severity of trachoma. • Environmental change: – Improved water supply & household sanitation. – Personal & community hygiene. – Adequate housing & water & sewage system. VIRAL CONJUNCTIVITIS • • • • • Inflammation with follicle formation—may be associate d with enlargement of regional lymph glands. Severe conjunctival inflammation, minimal discharge, l acrimation, Sub-conjunctival hemorrhage. Mild hyperemia. Conjunctival ulcers or membrane formation. Corneal involvement; 1.Superficial punctate keratitis. 2.Superficial erosions. 3.Stromal infiltrates. 4.Necrotic stromal ulcer. EPIDEMIC KERATOCONJUNCTIV ITIS • • • • Adeno virus serotypes 8 & 19. Transmission: Direct or Indirect contact. Epidemics: Schools, work places & physicians. Mode of Spread: Contaminated fingers, medica l instruments (tonometer), swimming pool or se xual contact. • Self limiting. • Highly infectious. EPIDEMIC KERATOCONJUNCTIV ITIS • Conjunctivitis: Acute onset watering, redness, discomfort & p hotophobia, both eyes (60%). • Signs: – Eyelids (oedematous). – Scanty discharge (watery). EPIDEMIC KERATOCONJUNCTIV ITIS • Conjunctiva: – Follicular conjunctivitis. – Mild-moderate chemosis. – Haemorrhage. – Pseudomembrane formation. • Tender pre-auricular lymphadenopathy. • Keratitis (80%)- 7 to 10 days later in the form of sup erficial punctate keratitis, subepithelial opacities and may remain for quite a long time. EPIDEMIC KERATOCONJUNCTIV ITIS • Treatment: Symptomatic & supportive. • Spontaneous resolution within 2 weeks. • Topical steroids to be avoided. • Antivirals ineffective. • Cold compresses, topical vasoconstrictors. ACUTE HAEMORRHAGIC CONJU NCTIVITIS • • • • • • • • Enterovirus 70 & Coxsackie virus A 24. Sudden onset. Short duration. Bilateral, profuse watering and discharge. Palpebral follicles. Sub-conjunctival haemorrages. Lymphadenopathy. Mild transient epithelial keratitis. Allergic Conjunctivitides Definitions Allergy is an altered or exaggerated susceptibility t o various foreign substances or physical agents w hich are harmless to the great majority of individu als. It is due to an antigen antibody reaction. Allergens is an agent capable of producing a state or manifestation of allergy. TYPES OF ALLERGIC CONJUNCTIVIT IS 1: ALLERGIC RHINOCONJUNCTIVITIS. 2: ACUTE ALLERGIC CONJUNCTIVITIS. 3:VERNAL KERATOCONJUNCTIVITIS. 4: ATOPIC KERATOCONJUNCTIVITIS. 5: GIANT PAPILLARY KERATOCONJUNCTI VITIS. 6: CONTACT OCULAR ALLERGY. 7: PHLACTENULAR CONJUNCTIVITIS. Allergic Rhinoconjunctivitis • Hypersensitivity reacti on to specific airborn a ntigens. • Frequently associated nasal symptoms. • May be seasonal or per ennial. Transient conjunctival oedema VERNAL KERATOCONJUNCTIVITIS • Common, recurrent, bilateral, external, ocular infl ammation affecting children & young adults. • 6 – 20 years. • Males > Females. • VKC IgE & cell mediated immune mechanism pl ay an important role. • 3/4 patients have associated Atopy. • 2/3 have close family hx. of Atopy. VERNAL KERATOCONJUNCTIV ITIS • Atopic pts. have Asthma & Eczema in infancy. • Peripheral blood shows esinophilia & increase ser um IgE levels. • Onset: After 5 years. • Resolves: around puberty. • Sign/Symptoms: occur on seasonal basis. • Peak Incidence: April - August. • More common in warm, dry climates e.g., Medite rranean basin, Africa & East Asia. Clinical Features Symptoms: Itching, lacrimation, photophobia, FB sensation, burning. Signs: Giant papilla, ptosis, hyperemia, mucus, trantas dots, punctate keratopathy, corneal u lcer. Clinical Types 1: Palpebral VKC: • Conjunctival hyperemia followed by a diffuse pa pillary hypertrophy (marked on superior tarsus). • Papilla enlarge & have flat topped polygonal appe arance of cobble stones. • In severe cases C.T. septa rupture giving giant pa pillae which is coated by copious mucus. • Active discharge by redness, swelling & tightly p acked papilla. 2: Limbal VKC: characterized by mucoi d nodules having smoot h round surface discrete white superfici al spots. trantas dots c omposed predominantl y esinophils, fibroblasts & necrotic epithelium, scattered around limbus & the apices of the lesi ons. Limbal vernal Mucoid nodule Trantas dots Progression of vernal conjunctivitis Diffuse papillary hypertrophy, most marked on superior tarsus Formation of cobblestone papillae Rupture of septae - giant papillae Progression of vernal keratopathy Punctate epitheliopathy Plaque formation (shield ulcer) Epithelial macroerosions Subepithelial scarring Treatment 1.Topical Steroid: Fluorometholone, Dexamethason, Prednisolone. 2. Mast cell stabilizers: Nedocromil 0.1%, Lodoxamide, Sodium Cromo glycate. 3. Acetyl-cysteine 5%. 4. Topical Cyclosporin 2%. 5. Debridement of early mucous plaque. Treatment 6. Lamellar keratectomy of densely adherent pla ques. 7. Excimer laser phototherapeutic keratectomy. 8. Amniotic membrane transplantation. 9. Supratarsal inj. of steroid: Betamethasone or tr iamcinolone. 10. Desensitizing immunotherapy. ATOPIC KERATOCONJUNCTIVIT IS Rare, potentially serious co ndition affects young (18-5 0 yrs) patients with atopic dermititis. Involved skin areas and lat eral neck folds; antecubital and popliteal fossae. Pts have Asthma, hay fever , urticaria, Migraine, Rhinit is. Chronic conjuntivitis. Serum IgE raised. Atopic keratoconjunctivitis Typically affects young patients with atopic dermatitis. Eyelids are red, thickened, macerated and fissured. TOXIC KERATOCONJUNCTIVITIS Contact blepharoconjunctivitis due to drugs 1. Anaesthetics. 2. Atropine. 3. Gentamycin. 4. Neomycin. 5. Tobramycin. 6. Antivirals. 7. Epinephrine. 8. Pilocarpine. 9. Timolol. 10. Preservatives: Benzalkonium chloride Chlorobutanol Chlorhexidine EDTA Thimerosal 11. Cosmetics. THANK YOU