* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Common Catheter Problems_Bon
Survey
Document related concepts
Transcript
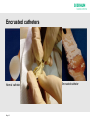
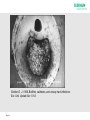
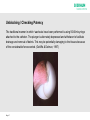
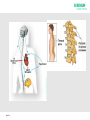
Urinary Catheters & Problem Solving William Ryan Nurse Advisor Aim of Presentation • Cover common issues related to Indwelling Urinary Catheters (IDC & SPC) • Always consider why is the catheter in-situ? • Is it required? • Is there an alternative? • Documentation!!!! Page 2 Intermittent Catheterization The GOLD STANDARD of artifical drainage of the bladder (Barton 2000;Bardsley and Kaighin,2008) Page • To prevent risk of over-distension • Generally the procedure is carried out 4-5 times/24hours (Barton 2000; Robinson,2007) • Number of times may need adjusting depending on residual (less then 100mls) • Should be considered for patients attending A&E with ROU as an immediate or planned alternative method of bladder emptying instead of an IDC. Not suitable for all patients! Advantages • Reduced risk of infection (Bakke & Digranes,1991) • Improvement in urinary symptoms & bladder health – maintains bladder tone • Offers opportunity to be self caring • Regain personal control over bladder function • Allows easier & more spontaneous sexual relations • Reduced need for equipment / appliances – easier to choose clothing – mobility less hindered Page Advantages contd Less risk of problems associated with indwelling catheters Helps maintain positive body image (Addison 2001) “Ready to go”, saves time & more cost effective Improved quality of life and independence Page To Begin! Indwelling Catheters! Page 6 Bypassing Kinked Tubing Constipation Infection Detrusor Instability Trigone Irritation (Catheter Size? Traction?) Encrustation (Struvite) Debris & Mucous Page 7 No Drainage Kinked Tubing, Constipation, Debris & Encrustation Renal Impairment - Anuria (Cessation of urine production) Page 8 Infection CAUTI (Catheter Associated Urinary Tract Infections) account for 45% of all hospital acquired infections Dougherty, L. and Lister, S. (2004) The Royal Marsden Hospital Manual of Clinical Nursing Procedures 22.5% of Healthcare Associated Infections or nosocomial Infection are UTIs of those 56.2% Catheter related (2006 prevalence survey of HCAI) Patients do die from urinary sepsis (Stewart 1998) Page 9 Managing / Reducing Risk of Infection Aseptic Technique When Catheterising Maintain Closed System Hygiene - - Meatal Cleansing / Bathing etc - - Wash Hands/Wear PPE Aprons when carrying out catheter care - - Daily washing of catheter Adequate Fluid Intake Frequency of drainage bag changes and use of night drainage systems Page 10 Encrustation What is encrustation and how do we deal with it? Page 11 Encrusted catheters Normal catheter Page 12 Encrusted catheter Encrustation of the catheter from deposits of mineral salts is a complication in approximately 50% of all longterm catheterised patients. Encrustation on catheter surface can cause trauma to the urethra during catheter removal. The risks associated with CMS use may be outweighed by increasing catheter life SARI 2011 Page 13 Process of Encrustation BACTERIA (Proteus, E-Coli, Klebsiella) Produce UREASE Spliting Urinary Urea into AMMONIA Change in pH (6.8 - 9.5) Alkaline Urine MINERAL PRECIPITATION ENCRUSTATION Page 14 CARBON DIOXIDE Stickler, D. J. 1996. Biofilms, catheters, and urinary tract infections. Eur. Urol. Update Ser. 5:1-8. Page 15 Assess • Inspect retrieved catheter – Visual examination of tip and cut catheter along its length to determine cause of catheter failure. Document findings – photograph if possible. Page 16 Unblocking / Checking Patency The traditional manner in which ‘washouts have been performed is using 50-60ml syringe attached to the catheter. The plunger is alternately depressed and withdrawn to facilitate drainage and removal of debris. This may be potentially damaging to the tissues because of the considerable force exerted. (Getliffe & Dolman, 1997) Page 17 Urotainer Solutions Uro-Tainer Twin SUBY-G (3.23% Citric Acid) Uro-Tainer Twin SOLUTIO-R (6% Citric Acid) SODIUM CHLORIDE (0.9%) Page 18 When to use Uro-Tainer Prophylactic Treatment for known “BLOCKERS” To Clear an Encrusted Catheter Prior to Catheter Removal To Remove Debris, Mucous, Haematuria from the Bladder To instil Prescribed Drugs Page 19 Using Uro-Tainer Assessment of the Problem Promotes Patient Comfort Prolongs Catheter Life (within manufacturers guidelines) Patients and/or carers may be taught self administration Page 20 Note: Catheter Maintenance Solutions are not bladder washouts. Do not provide a therapeutic effect Are Class 1 (Sterile) Medical Devices Page 21 Contraindication Autonomic Dysreflexia Autonomic dysreflexia (also known as autonomic hyperreflexia) is one of the most serious conditions affecting people with spinal cord injury at or above the 6th thoracic vertebrae. Develops secondary to any noxious stimulus below the level of injury. Nerve impulses cannot pass normally to the brain, therefore, the body produces exaggerated abnormal nerve signals that cause problems above and below the spinal injury. Page 22 Symptoms range from mild to sever and patients may present with one or more of the following: • • • • • • • • • • Pounding headache Flushing and/blotching above the level of spinal injury Slowed heart rate Profuse sweating above the level of injury Palpitations Goosebumps Blurred vision or seeing spots Stuffy nose Feeling of impending doom, anxiety or apprehension Elevated blood pressure. TREAT AS A MEDICAL EMERGENCY Page 23 Page 24 Page 25 Antimuscarinic medications block the messages that initiate bladder contractions and reduce frequency of bladder emptying. These can be very effective in managing an overactive bladder but risk causing a dry mouth as common side effect. Source: MS Trust UK Page 26