* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Agents to Treat Gastric Acidity and Gastroesophageal Reflux (GERD)
Survey
Document related concepts
Discovery and development of neuraminidase inhibitors wikipedia , lookup
Nicotinic agonist wikipedia , lookup
Psychopharmacology wikipedia , lookup
5-HT3 antagonist wikipedia , lookup
Discovery and development of ACE inhibitors wikipedia , lookup
Hyaluronic acid wikipedia , lookup
Cannabinoid receptor antagonist wikipedia , lookup
Neuropharmacology wikipedia , lookup
Discovery and development of angiotensin receptor blockers wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
NK1 receptor antagonist wikipedia , lookup
Discovery and development of proton pump inhibitors wikipedia , lookup
Transcript
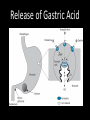
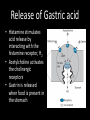
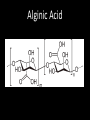
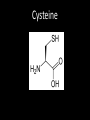
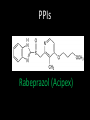
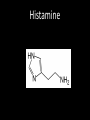
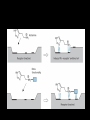
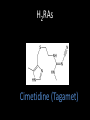
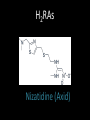
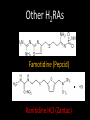
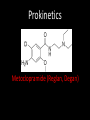
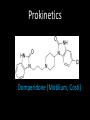
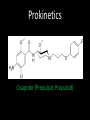
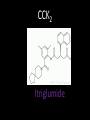
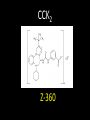
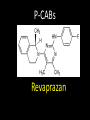
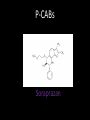
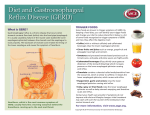
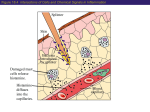
Agents to Treat Gastric Acidity and Gastroesophageal Reflux Disease (GERD) Presented by Abby Roth Overview • Introduction – Symptoms • Causes – Peptic Ulcer Disease • H. pylori • NSAIDs – GERD • Treatments Who is Affected? Gastric acidity and GERD affects people of all ages, races, and gender Symptoms • Heartburn • Regurgitation • Acid Indigestion • Nausea Symptoms Continued • Hoarseness • Sore Throat • Chest Pain • Bad Breath • Dry Cough • Asthma* Symptoms in Children • Vomiting • Coughing • Breathing Problems Acid-Peptic Disorders • Peptic Ulcer Disease –Occurs when there is an imbalance between the mucosal defense factors and the acid and pepsin. Helicobacter pylori Infection • Causes 80% of peptic ulcers • Survives the acid environment by attaching to the sugar molecules that line the stomach wall • Uses the mucus layer as protection H. pylori • Produce large amounts of urease Urease H20 Urea 3 NH3 + CO2 H. pylori • Secret proteins and toxins that interact with the stomach’s epithelial cells • Leads to inflammation and damage NSAIDs • Aspirin, Ibuprofen, Naproxen • Can have an affect at very low doses • Suppresses cylooxygenase-1 • Decrease production of prostaglandins What is GERD? • Condition where the stomach acid/content is pushed back or “refluxed” into the esophagus • Affects 10 million Americans • Approximately 7% have daily symptoms • Link GERD vs. NERD • Patients suffering symptoms are placed in two groups –Non-erosive reflux disease, or NERD –Erosive esophagitis • Erosive esophagitis is characterized by swelling and Inflammation –Barrett’s Esophagus –Precursor to Esophageal Cancer Causes of GERD • Abnormalities with the Lower Esophageal Sphincter, or LES • Stomach Abnormalities –Hiatal hernia –Link Causes • Medications –NSAIDs –Calcium Channel Blockers (high blood pressure, angina) Medications –Anticholinergics (urinary tract disorders) –Beta Adrenergic Agonists (asthma) –Dopamine (Parkinson’s disease) Causes • Food and Drinks – Carbonated beverages – Chocolate – Alcohol – Citrus Fruits – Coffee or Tea – Fatty foods – Containing tomatoes – Mint – Spicy Food Causes • Smoking – Damages mucus membranes – Impairs muscle reflexes in the throat – Increases acid secretion – Reduces LES function and salivation Causes • Obesity • Laying down after a large meal • Eating close to bed time • Exercise Release of Gastric Acid Release of Gastric acid • Histamine stimulates acid release by interacting with the histamine receptor, H2 • Acetylcholine activates the cholinergic receptors • Gastrin is released when food is present in the stomach Treatments • • • • • • • Antacids Alginates Sucralfate Proton Pump Inhibitors Histamine H2-Recptor Antagonists Prokinetics New Treatments Antacids • Quick but short term • Buffer gastric acid, increasing the pH • Neutralize acid by the following reaction Al(OH)3 + 3 HCl AlCl3 + 3 H2O Antacids –Maalox • Al(OH)3 (aluminum hydroxide), Mg(OH)2 (magnesium hydroxide) Antacids • Tums • CaCO3 (calcium carbonate) Antacids –Pepto-Bismol • C7H5BiO4 (bismuth subsalicylate) Antacids –Alka-Seltzer • NaHCO3 (sodium bicarbonate) Alginates • Alginates –Usually combined with an antacid –Forms protective barrier on top of gastric contents –Gaviscon • Sodium Alginate, Sodium Bicarbonate, and Calcium Carbonate –Link Alginates • Polysaccharide found in the cell walls of brown algae • Sodium alginate is the sodium salt of alginic acid Alginic Acid Sucralfate • Reacts with stomach acid to from a cross linked viscous polymer that acts as an acid buffer • Can bind to proteins on the surface of an ulcer to prevent further acid damage • Has been shown to aid in healing by promoting epidermal growth factors and prostaglandins Sucralfate (Carafate) Proton Pump Inhibitors • Proton pump inhibitors (PPIs) – Inhibits the gastric acid pump, H+/K+ ATPase – Are prodrugs PPIs • Diffuse into the parietal cells of the stomach and accumulates • Activated by proton-catalyzed formation of sulfenic acid • This prevents the drug from diffusing out • Activated form then irreversibly binds at the sulfhydryl groups of the cysteins of the H+/K+ ATPase • Link Cysteine PPIs Rabeprazol (Acipex) PPIs Lansoprazole (Prevacid) PPIs Esomeprazole (Nexium) PPIs Omeprazole (Prilosec) Omeprazole/sodium bicarbonate (Zegerid) PPIs Pantoprazole (Protonix) Treatments • Histamine H2-recptor antagonists (H2RAs) • The hormone, histamine stimulates the release of acid by interacting with the histamine receptor, or H2 receptor. • Inhibit acid secretion by competitively and reversibly blocking parietal cell H2receptors • Less potent then PPI’s Agonist vs. Antagonist • An agonist is a drug that produces the same response at a receptor as the natural messenger • An antagonist is a drug which binds to a receptor without activating it, prevent an agonist or natural messenger from binding Histamine H2RAs Cimetidine (Tagamet) H2RAs Nizatidine (Axid) Other H2RAs Famotidine (Pepcid) Ranitidine HCl (Zantac) Treatments • Prokinetics –Increase LES function –Release stomach contents by •Activating serotonin receptors •Acting on dopaminergic receptors Prokinetics Metoclopramide (Reglan, Degan) Prokinetics Domperidone (Motilium, Costi) Prokinetics Cisapride (Prepulsid, Propulsid) Prokinetics • Rarely used because of severe side effects – Fatigue –Tremors –Parkinsonism –Tardive Dyskinesia –Severe cardiac events New Treatments • Cholecystokinin2 receptor antagonists (CCK2) • Potassium competitive acid blockers (P-CABs) Treatments • Cholecystokinin2 receptor antagonists (CCK2) –Block the CCK2 receptors inhibiting acid secretion –Still in clinical trials –Best use in combination with PPI’s CCK2 Itriglumide CCK2 Z-360 Treatments • Potassium competitive acid blockers (P-CABs) – Target H+/K+ ATPase – Ionically binds to the proton pump – Specific for the K+ binding region and prevents acid secretion – Binds reversibly – Still in clinical trials P-CABs Revaprazan P-CABs Soraprazan Treatment for H. pylori • Amoxicillin + clarithromycin + proton pump inhibitor • Metronidazole + clarithromycin + proton pump inhibitor • Bismuth subsalicylate + metronidazole + tetracycline + proton pump inhibitor Assigned Reading • Vesper, J.B. et all, Gastroesophageal Reflux Diesease, Is there More to the Story?, ChemMedChem (2008), 3, 552-559. Homework Questions • What is an antagonist and how do the H2RAs (histamine receptor antagonists) act as one? • Explain the precise biological mechanism whereby prokinetics achieve their effect, including the receptors they act upon. Are they agonists or antagonists? Of which chemical messenger? • What is a prodrug? What causes the PPI’s to become an active drug? • Bacteria in the upper GI tract may play a role in GERD. Explain. References • Bak, Young-Tae. Management Strategies for Gastroesophageal Reflux Disease. Journal of Gastroenterology and Hepatology (2004), 19, S49-S53. • Horn, J. Understanding the Pharmacodynamic and Pharmacokinetic Differences between proton pump inhibitors- focus on pKa and metabolism. AP&T (2006), 2, 340-350. • Pettit, M. Treatment of Gastroesophageal Reflux Disease. Pharm World Sci (2005) 27, 432-435. • Vakil, N., New Pharmacological Agents for the Treatment of Gastroesophageal Reflux Disease. AP&T (2006), 19, 1041-1049. • Vesper, J.B. et all, Gastroesophageal Reflux Diesease, Is there More to the Story?, ChemMedChem (2008), 3, 552-559. • Goodman and Gilman pg 967-980. • Patrick pg 643-671.