* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Stage of Differentiation
Women's medicine in antiquity wikipedia , lookup
Prenatal testing wikipedia , lookup
Reproductive health wikipedia , lookup
Birth control wikipedia , lookup
Dental emergency wikipedia , lookup
Maternal physiological changes in pregnancy wikipedia , lookup
Breech birth wikipedia , lookup
Menstrual cycle wikipedia , lookup
Menstruation wikipedia , lookup
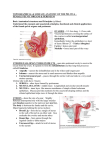
CONGENITAL ABNORMALITIES OF THE FEMALE REPRODUCTIVE TRACTS: In this chapter congenital anomalies of the genital tract will be discussed under two headings; Anomalies of the external genital organs (ambiguous genitalia), which can result in disturbance of the fetal phenotype, and anomalies of the internal genital organs (Müllerian Ducts Anomalies). Anomalies of the external genital organs: A) Ambiguous Genitalia (Defect of the clitoris and labia): The term ambiguous genitalia describe genitalia with unrecognizable sexual features. In case of female fetuses, ambiguous genitalia usually occur as a result of in utero exposure to androgen hormones during critical time of development of the genital tract. This will result in variable degree of virilization of the external genitalia, mainly in the form of elongation of the clitoris and/or labial fusion. Ambiguous genitalia can result from administration of androgenic substances to pregnant mothers particularly during the early weeks of embryogenesis. However the condition is more commonly seen in infants with congenital adrenal hyperplasia. This syndrome is an inherited autosomal recessive syndrome. Characterized by deficiency of some of the enzymes involved in the biosynthesis of cortisol, the most common variety is deficiency of the 21-hydroxylase enzyme. In response to a low cortisol level the pituitary produces increasing amount of ACTH to further stimulate the fetal adrenal in attempts to compensate for the low cortisol level. However some of the adrenal products are androgenic and will result in virilization of a female fetus e.g. elongation of the clitoris and fusion of the labia. Anomalies of the internal genital tract "Müllerian anomalies" Normal development of the internal female genitalis (fallopian tubes, uterus, cervix, and the upper two thirds of the vagina) depends on three consecutive embryologic processes; first the differentiation of two paired mullerian ducts, second, lateral fusion of the lower segment of the mullerian ducts in the midline to form the uterus, cervix and upper two third of the vagina and finally resorption of the central septum between the two mullerian ducts in order to form a single uterine cavity and cervix. The lower third of the vagina embryologically originates from the sinovaginal bulb. A normal patent vagina depends on complete vertical fusion of the ascending sinovaginal bulb with the descending müllerian system (i.e., fusion of the lower one third and upper two thirds of the vagina). Etiology of Mullerian Duct anomalies: The pathogenesis of mullerian anomalies is not very well understood but in some cases there may be a genetic linkage as evident by the occasional association with other somatic anomalies as well as reports of familial recurrence (Stelling J.R., et al 2000). It has been suggested that some cases may be due to genetic defect in Mullerian Inhibitory factor or its receptors. Most probably however the major genetic mechanism is polygenic or multifactorial. Some cases may result from in utero exposure of the fetus to teratogenic substances during a critical period of its development such as in case of exposure to diethylstilbestrol. Frequency of Mullerian Ducts Anomalies: The actual incidence of müllerian anomalies is unknown. This is due to a number of factors most important is the source of data. When data are obtained from women with recurrent pregnancy loss the prevalence of müllerian anomalies is 8-10% (Stray-Pedersen, 1984; Stampe Sorenson, 1988). This is in contrast to the reported prevalence rate of 2-3% among in the general population (Ashton, 1988; Simon, 1991). The incidence is higher among women with late miscarriage and preterm deliveries (Table from ref # 87 page 145 Speroof). Classification of mullerian anomalies Classification of mullerian anomalies is based on its embryological origin as well as its anatomical type. The classification system recommended by the American Society for Reproductive Medicine in 1998 categories the mullerian anomalies into seven categories (Table….). The vaginal anomalies are considered separately since it is mostly obstructive in nature and the uterus is usual present (table ...). In attempt to simplify the matter other classification system which is related to the nature of the surgical disorder has been described (Rock JA, Adam RA: 2000). In this classification four classes of Mullerian anomalies are identified; the two major ones are; disorders that compromise patency of the reproductive tract (obstructive mullerian anomalies) and disorders of lateral fusin of patent reproductive tract (longitudinal fusion anomalies). The remaining two classes are agenesis/hypoplasia (as in AFS class 1) and other miscellaneous anomalies that are difficult to classify Obstructive Müllerian anomalies: Obstructive Mullerian anomalies include disorders compromising patency of the reproductive tract these include; transverse vaginal septa and cervical agenesis and dysgenesis with or without obstruction. Imperforate hymen is embryologically not of mullerian origin although clinically have a similar presentation. Obstructive Müllerian anomalies preclude the outflow of menstruation and allow the collection of blood in the uterus and the vagina. Patients with this type of anomaly will usually presents with amenorrhea or pain due to accumulated menstrual flow. Management goals are relief of symptoms such as pain, as well as preservation of sexual and reproductive function. The true incidence of obstructive Müllerian anomalies is unknown, but studies reports an incidence of between 0.1% and 3.8%. b) Imperforate Hymen: The hymen represents the junction of the sinovaginal bulbs with the urogenital sinus; hence it is formed form the endoderm of the urogenital sinus epithelium. Normally it is perforated during embryonic life. The incidence of imperforate hymen is estimated around 1 in 2,000 girls or even less (Parazzini F., and Cecchetti G. 1990, Dickson C.A., et 1985). There have been reports of familial occurrence of imperforate hymens suggesting a genetic background. An acquired condition similar to imperforate hymen has been described due to scarring at the vaginal introitus secondary to child sexual abuse (Botash A.S., Jean-Louis F. 2001). An imperforate hymen may be discovered at birth because of the presence of a suprapubic mass "mucocolpos or hydrocolpos" which is formed by retention of fluid secretion behind the imperforate hymen. This fluid results from maternal estrogen effects on the vaginal epithelium and/or cervical glands. It may cause urinary obstruction due to pressure on the anterior urethra. More commonly however an imperforate hymen remains undetected until puberty when over time repeated accumulation of menstrual flow in the vagina produce a condition known as hematocolpos. The fluid component of the menstrual flow gets absorbed and the remaining blood and debris acquire an altered chocolate thick appearance. In more advanced cases the uterus and the fallopian tubes becomes distended with retained menstrual blood resulting in hematometra and hematosalpinx, respectively. Eventually the retained menstrual flow may trickle back, into the pelvic peritoneal cavity, with the risk of development of endometriosis. Typically patients with imperforate hymen presents at puberty with primary amenorrhea despite apparently normal pubertal development. They often complain of recurrent cyclic pelvic pain in the absence of menstrual flow. The pain tends to be localized to the lower abdomen or perineum, although it can be referred to the lower back as a result of irritation of the sacral plexus by a posteriorly positioned vaginal mass. Nonspecific symptoms, such as nausea, vomiting, or diarrhea, can also occur. On abdominal examination, a suprapubic mass is rarely felt and if present it usually reflects a distended bladder rather than a hematocolpos. On local inspection the accumulation of menstrual blood behind the hymen gives the blue bulging pathognomonic appearance of imperforate hymen (Figure 1). Variations of an imperforate hymen include microperforation, septate, stenotic, and cribriform hymen. Imperforate hymen should be differentiated from low transverse vaginal septum. This can be accomplished with Valsalva. Imperforate hymen should bulge with Valsalva and transverse vaginal septum should not (Burgis J 2001). A pelvic ultrasound scan will confirm the diagnosis and demonstrate normal internal anatomy. The treatment of imperforate hymen is by surgical release of the retained contents in the hematocolpos. The components of the hematocolpos are a very receptive medium for bacterial growth. Thus during surgical release of hematocolpos, complete antiseptic measures should be undertaken and prophylactic antibiotics have been recommended. Most importantly no vaginal examination or mopping inside the vagina should be made during operation. The operation is accomplished by a cruciate incision in the hymen extending between 2, 10 and 6 o’clock. Because of the viscosity of this material, a double suction apparatus is sometimes required. After adequate drainage the vaginal mucosa some have suggested suturing the hymenal ring to prevent re-accumulation of menstrual blood. Long-term follow-up of patients with imperforate hymen reveals normal fertility rates. Imperforate hymen is usually not associated with any other Müllerian abnormalities (Gidwani G, Falcone T. 1999). Cervical Atresia: Congenital atresia of the cervix is a relatively rare mullerian developmental disorder less than 100 cases have been reported in the literature (Fujimoto V. Y, et al 1997). Patients present with primary amenorrhea and cyclic pelvic pain, and the condition is often associated with absence of all or part of the vagina (Figure …a, b). Some cases are also associated with uterine anomalies (Fujimoto V. Y, et al 1997). In a large number of patients in the literature endometriotic implants have been described at the time of laparoscopy or laparotomy. The optimum management of cervical atresia remains controversial. The options are between either conservative management in which a surgical canalization is performed in order to provide patients some potential (albeit limited) opportunity for fertility or hystrectomy. The choice depends on whether the vagina is present or absent and if the there are associated uterine anomalies. Careful preoperative evaluation and counseling is required. In most of the reported cases the nature of uterine outflow obstruction was only confirmed intraoperatively. Presently magnetic resonance imaging (MRI) is the gold standard and should offer better chance for preoperative assessment and delineation of pelvic anatomy (Markham S, et al 19787). In some cases menstrual suppression with continuous oral contraceptive pills or medroxyprogesterone acetate (Depo-Provera) may be used to relieve symptoms and delay the need for surgery. It also provides valuable time for discussing the options for therapy (Rock JA. 1997). In patients with little or no vagina, hysterectomy is generally recommended, as canalization is usually unsuccessful and may be associated with infection, sepsis, and even death(Breech LL, Laufer MR. 1999, Rock JA. 1997, Fujimoto MD, et al 1997). Surgical recanalization is reserved for selected patients with functional vaginas. In a minority of patients spontaneous pregnancy has been reported (Fujimoto V. Y, et al 1997). Vaginal Agenesis: Absence of the vagina (vaginal atresia or agenesis), can be encountered either as an isolated developmental defect or within a complex of more extensive anomalies such as Bardet-Biedl syndrome (BBS), or McKusick-Kaufman syndrome (MKKS). Both syndromes are autosomal recesssive disorders with multiple anomalies other than vaginal agenesis. However as an isolated anatomical defect in the presence of normal female phenotype there are two verities of vaginal agenesis either complete or incomplete. Complete vaginal agenesis, the most common one (80%-90%), is the Rokitansky-Mayer-Küster-Hauser (RMKH) syndrome in which there is absence of most or all the entire vagina, all or almost all of the uterus and cervix. Ovarian function is normal thus growth and development are normal. Complete vaginal atresia occasionally is termed müllerian agenesis. Incomplete or partial vaginal agenesis is due to failure of canalization of the contribution made by the urogenital sinus to the caudal part of the vagina (Leduc B, et al 1968). In this type the lower fifth to third of the vagina is replaced by 2 to 3 cm of fibrous tissue, above which lie a well-differentiated upper vagina, cervix, uterine corpus, and fallopian tubes (Figure …). This variant is due to different pathophysiologic events and more correctly classified as a variant of transverse vaginal septum. The etiology of vaginal agenesis is unknown, and most cases occur sporadically. Approximately 4% of reported cases are familial, with affected siblings (Cramer, 1987). Mutation in either the müllerian inhibitory substance (MIS) gene or its receptor gene has been suggested (Lindenman, 1997, Amesse, 1999). Vaginal agenesis has been associated with variants of the galactose-1-phosphate uridyltransferase enzyme, suggesting that increased exposure to galactose is responsible for abnormal vaginal development (Chen, 1981; Cramer, 1987; Aughton, 1993). Frequency: Müllerian agenesis is a relatively common cause of primary amenorrhea (1 in 4000 live female births) more frequent than congential androgen insensitivity and second only to gonadal dysgenesis (Reindollar RH, et al 1981, Speerof page 441). Partial vaginal agenesis is less common, with a reported incidence of 1 in 70,000 females (Banerjee R, Laufer MR 1998). Clinical Presentation: The most common presentation is at presents at puberty with primary amenorrhea. In the rare cases the endometrium in rudimentary uterus may function causing cyclic abdominal or cramping pain. On examination the appearance of the vagina can be diverse; it can be completely absent, a short vaginal pouch, or a short vaginal dimple 1-2 cm superior to the hymenal ring. On rectal examination the uterus is either absent or replaced by rudimentary structure. The main differential diagnosis is from cases of androgen resistance syndrome or the XY female (Table…). Investigations include karyotyping to exclude cases of androgen resistant syndrome (XY female), an ultrasound examination or if necessary magnetic resonance imaging examination for defining the uterus and detailed anatomy of the pelvic organs. Rarely if MRI can not define the degree of uterine development, laparoscopy may be necessary to define the uterus and the ovaries . Approximately one third of cases of mullerian aplasia are associated with renal anomalies (Carson SA, et al 1983). The most frequent renal anomalies are pelvic kidney, renal ectopia and unilateral aplasia. Skeletal anomalies, especially vertebral anomalies, are also not uncommon. Treatment of vaginal atresia: The timing of treatment whether it is surgical or non surgical requires certain level of psychological and sexual maturity. Surgical treatment is better planned to coincide with subsequent opportunity for intercourse in order to maintain vaginal patentcy. However it may be instituted sooner if a patient presents with vaginal outflow obstruction, abdominal or pelvic pain, or is at risk for secondary endometriosis. The objective of treatment is to creat a functioning vagina. In the rare instances in which a well formed uterus and cervix are present it may be possible to restore potential fertility function through recanalization. Each case should be assessed carefully. Preoperative MRI is very helpful in assessing the status of the cervix. In some cases laparotomy should be performed and if the cervix is atretic the uterus should be removed (Ref 74 page 478 in Sperof). In the majority of cases of mullerian aplasia it is hardly necessary to remove rudimentary uteri unless it is a functioning one. Non surgical treatment (Frank technique or perineal dilation): The technique involves the forceful dilation of a shallow rudimentary vaginal pit with the sequential application of progressively wider and longer dilators which may be administered either manually or using a specially designed bicycle-seat stool to hold a dilator in place. The goal is to create a blind-ending vaginal pouch. The technique requires strong patient motivation and compliance. Patients with a vaginal dimple or no vagina may experience discomfort and abandon the dilator. However the method has been successful in creating an adequate vagina for normal sexual activity (Hendren WH, Donahoe PK: 1980). Surgical treatment of vaginal agenesis "vaginoplasty": Surgical treatment should be considered only when the patient wishes to become sexually active. The aim of surgical treatment is to create a neovagina. Various methods of vaginal reconstruction have evolved, and more than 100 different surgical variations have been reported (Fedele, 1994; Ghirardini, 1994). The principle is dissection and creation of vaginal space between the rectum posteriorly and the urethra anteriorly. This new vaginal space is maintained by using epithelial tissue obtained either from partial skin graft (as in McIndoe technique), an ileal loop or amniotic membrane. Any of these tissues may be stretched over a formed mould and should be kept in place until the epithelial graft is well taken after about 7-10 days. Subsequently the patient needs to reinsert the mould into the neovagina every day and night for 3 months, followed by nightly insertion for 3 more months to prevent contraction William's vaginoplasty is a simpler operation with no risk for damage to the urethra or rectum. In this operation vulval flap is used to make a vaginal tube. Still dilation is needed for a lengthy period, and the neovagina has a physiologically abnormal angle. More recently a technique of laparoscopic-assisted creation of a vagina was described, which thought to provide effective and safer mean for creation of a new vagina. Genetic offspring has been achieved in patients with mullerian aplasia using surrogate uteri to carry the fertilized oocytes of patients. The experience reported so far with more than 34 offspring none of them showed inheritance of the condition suggest that the most logical explanation for müllerian aplasia inheritance (Petrozza JC, 1997). Transverse Vaginal Septum: is polygenic/multifactorial A transverse vaginal septum results from failure of fusion and/or complete canalization of the urogenital sinus and müllerian ducts. It is a very rare anomaly occurs in approximately 1 in 30,000 to 1 in 80,000 women (Rock, JA, Azziz, R. 1987). These septa may occur at any level in the vagina with the following frequencies: 46%, upper vagina; 40%, mid vagina; and 14%, lower vagina (Gidwani G, Falcone T. 1999) (Figure ----). Vaginal septa may be complete or incomplete with a small central or eccentric perforation which is not adequate to drainage of the menstrual flow. Complete vaginal septa have a similar presentation to cases of imperforate hymen. Except that on local examination the sign of a bulging bluish hymen, which is more prominent with Valsalva's maneuver, is not present. Instead the vagina appears as a closed short pouch. Patient with incomplete transverse septum may have little bleeding, however over time they develop hematocolpos and hematometra and may complain of foul-smelling vaginal discharge. Ultrasonographic or magnetic resonance (MR) imaging helps to define the location and thickness of the septum and to differentiate between a high septum and congenital absence of the cervix. The treatment depends on the thickness of the vaginal septum. Usually the septum is thin (< 1cm) and is treated more or less similar to cases of imperforate hymen. However, a thick septum requires formal dissection in order to remove the septum. The vaginal skin in the upper and lower parts of the vagina should then be undermined, mobilized and stitched together with interrupted absorbable sutures. Subsequent utilization of the vagina is also necessary in order to prevent stenosis. In more advanced cases, split thickness skin graft may be required to join the two ends of the vagina. Transverse vaginal septum has been reported in diethylstilbestrol (DES) exposed females. Defects of Mullerian Duct fusion: Non obstructive anomalies of the mullerian ducts are relatively common (2-3%). Unlike obstructive anomalies that usually presents with primary amenorrhea, fusion anomalies are often associated with gynecological as well as obstetrics complications such as infertility, recurrent pregnancy loss and poor obstetrics outcome in pregnancy (Ref 83-86 Speerof page 145). Some case where there is partial obstruction e.g. a unilateral rudimentary horn, may present early in the years following puberty usually with primary cyclic dysmenorrhea. Anomalies of lateral fusion of the mullerian ducts: This may be partial or complete failure of fusion. Complete failure of fusion of mullerian ducts is characterized by duplication of the vagina, uterus and cervix a condition known as "didelphic uteri". This anomaly is usually asymptomatic until menarche. The most frequent complaint is failure of a tampon to obstruct menstrual flow. Occasionally one side may be obstructed and causes cyclic pelvic pain, despite the presence of normal menstrual flow. In such cases there is often ipsilateral renal agenesis, and early diagnosis and excision of the obstructing vaginal septum preserve fertility and prevent development of endometriosis. In general in patients with didelphic uteri, fertility is not affected but reproductive outcomes is compromised with a high spontaneous abortion rate (40%) (Propst, 2000). Patients who carry a pregnancy to term have no obstetrical difficulties (Rock, 1985). The treatment for uterus didelphys with an obstructed unilateral vagina is surgical excision of the obstructing vaginal septum in order to preserve reproductive capacity and prevent impairment of the uterus and tubes on the obstructed side, reduce the risk of development of endometriosis and pelvic adhesions (Olive, 1987). For uterus didelphys with a non-obstructed vagina, indications for surgical correction are limited. The place for metroplasty operation is very limited and should only be considered in selected cases. In pregnancy the optimum management of a non-obstructed longitudinal septum in pregnancy is not clear. Some authors advocate excision, while others recommend leaving it undisturbed unless it becomes obstructed during labor (Rock, 1985). Partial failure of Mullerian tubes fusion is characterized by the presence of one vagina and one cervix and a ‘bicornis uteri. In this anomaly, the lower uterus and cervix are completely fused, but the uterine chamber is divided into 2 separate but communicating endometrial cavities with a muscular uterine septum which varies in length. Cases in which the septum is confined to the fundal region is considered partial bicornuate. Complete bicornis uteri are cases in which the septum reach down to the cervix. The complete verity could be "bicornuate unicollis" if the septum extends to the internal os, or "bicornuate bicollis" if the septum reach down to the external os. Pregnancy outcome has been reported as near normal. Approximately 60% of patients can expect to deliver a viable infant (Rock, 1977). However, the rate of early miscarriage, preterm labor and breech presentation is still higher than normal (ref 86, 92 Sperof). Apparently this depends on whether the bicornate uterus is partial or complete. In one study, women with a partial bicornuate uterus experienced a spontaneous abortion rate of 28%; the preterm delivery rate was 20%. This contrasts to a spontaneous abortion rate of 66% and a higher rate of preterm deliveries in women with complete bicornuate uterus (Heinonen, 1982). A bicornuate uterus should be distinguished from a septate uterus for several important reasons; a bicornuate uterus is associated with minimal reproductive problems, but septate uterus has a high association with reproductive failure. Additionally, corrective surgical approaches markedly differ in the two cases. Surgical reconstruction is seldom required in cases of bicornuate uterus (Jones, 1992). However several surgical methods for that aims at unification of the two cavities "Metroplasty" have been described. It should be reserved for women who have experienced recurrent spontaneous abortion, midtrimester loss, premature birth, and in whom no other etiologic factor has been identified (Patton, 1988; Propst, 2000). Strassman procedure and its modified approach is the surgical treatment of choice for bicornuate uterus and didelphys uterus. It involves the removal of the septum by wedge resection, with subsequent unification of the 2 cavities. Septet Uterus: Septate uterus is the most common structural abnormality of all müllerian duct defects. In this condition the two mullerian ducts have completely fused together but there is failure of resorption of the intervening fibromuscular septum. The septum is considered complete if it extends to the internal os, thus dividing the endometrial cavity, and partial if it does not. In addition, septa may be segmental, which results in partial communication between the endometrial cavities (Candiani, 1983). A total failure in resorption can cleave a longitudinal vaginal septum (a double vagina). Externally, the uterus appears as a normal single uterine body, which differentiate it from bicornuate uterus. Septate uterus is not a cause of infertility but associated with the poorest reproductive outcomes of all mullerian duct anomalies. Spontaneous abortion rate occur in 80% of cases (Daly, 1984). Treatment by hysteroscopic resection yield excellent results with posttreatment miscarriage rate around 10%. However because septate uterus is not always associated with an unfavorable obstetrical outcome its presence alone is not an indication for surgery. Therefore the decision to perform metroplasty should be based on poor reproductive performance rather than the presence of a septate uterus (Heinonen, 1982). Candidates for surgery include women who have had recurrent spontaneous abortion, a single second-trimester loss, or history of preterm delivery (Simon, 1991). The Arcuate Uterus: A term that describes a mild form of fusion defect in the uterine cavity in which there is a small indentation at the uterine fundus. It is the most commonly observed uterine anomaly detected on hysterosalpingography findings. Arcuate uterus is benign condition with probably has no consequences and require no treatment. Anomalies due to unilateral defects of Mullerian duct development: Failure of development of one mullerian duct results in "unicornuate uterus" where there is a single uterine horn, single cervix and vagina. There is almost always a missing kidney and ureter on the same side. Such a uterus can support a pregnancy but there is an increased rate of obstetric complications. In a rare type, there may be a unilateral non-functioning rudimentary horn. A functioning horn however may be the site of pregnancy with subsequent high risk of obstetric complications. Most obstetric complications occur within the first 20 weeks and can result in abortion, uterine rupture, and maternal death (Kirschner, 1979; Raman, 1993). A non-communicating functioning horn can be a cause of chronic pain and surgical exesion is indicated. Excision of a rudimentary horn can now be accomplished through laparoscopic hemi-hysterectomy (Donnez J, Nisolle M: 1997, Nisolle M, Donnez J 1996) Cases of unicornuate uterus should undergo urological assessment because of high rate of associated urological anomalies (44%), especially when the rudimentary horn is obstructed. Associated urological anomalies include ipsilateral renal agenesis at a rate of 67%, horseshoe kidneys, and ipsilateral pelvic kidney at a rate of 15% (Rock, 1985). Diethylstilbestrol Associated anomalies: DES is a synthetic estrogen that was prescribed to women for recurrent pregnancy loss, premature delivery, and other pregnancy complications during the late 1940s and early 1970s. Latter it was realized that the exposure to high level of estrogen during mullerian development was associated with increased rate of vaginal clear cell adenocarcinoma and various benign vaginal, cervical and uterine abnormalities (Herbst, 1971). DES-related uterine anomalies are quite common in women with a history of in utero DES exposure. In one study, 69% of 267 women exposed to DES in utero demonstrated uterine abnormalities identified based on hysterosalpingography findings (Kaufman, 1980). Uterine anomalies associated with in utero DES exposure include a Tshaped endometrial cavity, a widened lower uterine segment, midfundal constrictions, endometrial filling defects, irregular margins, and a hypoplastic uterus (Patton, 1988). Cervical structural abnormalities were also detected in 44% of these women. These anomalies included hypoplasia, an anterior ridge, a collar, and pseudopolyps. Vaginal adenosis and vaginal constrictions are associated abnormalities (Kaufman, 1980; Patton, 1988). This group of anomalies are probably associated with high rate of obstetric complications although no specific anomaly has been associated with any form of adverse obstetric outcome (Kaufman, 1980; Patton, 1988). However cervical incompetence may be an associated factor in these women and cervical cerclage is the only prophylactic treatment that can be offered (Goldberg, 1999). Complications and Clinical Presentations of Uterine Anomalies: Müllerian duct anomalies (MDAs) are often recognized after the onset of puberty. In the prepubertal period, the presence of normal external genitalia and age-appropriate developmental milestones often mask abnormalities of the internal reproductive organs. After the onset of puberty, young women with müllerian anomalies often present to the gynecologist with menstrual disorders. Later presentations include infertility and obstetric complications. Uterine anomalies usually present as cases of obstetric complications in the form of repeated miscarriages, premature labor intrauterine growth retardation, malpresentation, or retained placenta. A unilateral functioning rudimentary horn, which fails to communicate with the other horn, may present early in the years following puberty usually with primary cyclic dysmenorrhea. Recurrent miscarriages, due to uterine anomalies, usually occur as a result of failure of the uterus to accommodate the growing pregnancy. The timing of miscarriage is usually in second trimester miscarriage and the duration of pregnancy tends to increase in subsequent pregnancy. Hence, conservative management of such cases will eventually lead to the achievement of a successful pregnancy. Early first trimester miscarriage is more common in cases of septet uterus if the developing embryo gets implanted on the septum where there is often deficient vascular development. Delayed obstetric complications in the form of malpresentation, breech or transverse lie may occur in cases of uterine anomaly due to loss of the normal pear-shaped uterine cavity, which encourages the cephalic presentation.