* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
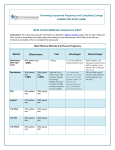
Download Postpartum contraception
Survey
Document related concepts
Transcript
U IS H T W E t sho CONTEMPOR ARY OB / GYN JANUARY 2012 , Vol. 57, No. 1 Translating Science into Sound Clinical Practice I H T W noSn haps NEW ig hoists on H THIS ighRisk ISSU Preg E nan cy JANUARY 2012 ContemporaryOBGYN.net POSTPARTUM CONTR ACEPTION ◾ MIDURETHR AL SLINGS ◾ FETAL MONITORING MY THBUSTERS Postpartum contraception Ways to avoid VTE Paul D. Blumenthal, MD, MPH Amy J. Voedisch, MD, MS Keys to success with midurethral slings Mary T. McLennan, MD FM MYTHBUSTERS VOLUME 57, NUMBER 1 Atypical variable decelerations David A. Miller, MD magenta yellow cyan black obgyn0112_cv1.pgs 12.20.2011 08:49 ADVANSTAR_PDF/X-1a A smart combination to support prenatal health* • A complete multivitamin plus a DHA/EPA liquid gel with key nutrients to support prenatal health* • From One A Day®, a brand women trust • Conveniently available over the counter and may be more affordable than some branded prescription prenatal vitamins Recommend Changing expectations OUR MISSION For nearly a half century, busy practitioners have trusted Contemporary OB/GYN to translate the latest research into outstanding patient care. We are dedicated to providing them with evidence-based information on scientific advances in a clinically useful format. EDITORIAL DAN SCHWARTZ Director of Editorial PATRICIA M FERNBERG Editor 440-891-2757 [email protected] CATHERINE M RADWAN Senior Editor 440-891-2636 [email protected] KAREN BARDOSSI MARIAN FREEDMAN LISA A HACK Contributing Editors EDITOR IN CHIEF CHARLES J LOCKWOOD, MD, MHCM Dean of the College of Medicine and Vice President for Health Sciences, The Ohio State University School of Medicine, Columbus, OH DEPUTY EDITOR JON I EINARSSON, MD, MPH Associate Professor of Obstetrics and Gynecology, Harvard Medical School, Director, Division of Minimally Invasive Gynecologic Surgery, Brigham and Women’s Hospital, Boston, MA ART & PRODUCTION PETER SELTZER Group Art Director ROBERT M c GARR Group Art Director TERRI JOHNSTONE Sr. Production Manager EDITORIAL BOARD HAYWOOD L BROWN, MD SARAH J KILPATRICK, MD, PHD Chair, Obstetrics and Gynecology, Duke University Medical Center Durham, NC Chair, Department of Obstetrics and Gynecology, Cedars-Sinai Medical Center, Los Angeles, CA JOSHUA A COPEL, MD ELLIOTT K MAIN, MD Professor, Obstetrics, Gynecology, and Reproductive Sciences, and Pediatrics, Yale University School of Medicine, New Haven, CT Director, California Maternal Quality Care Collaborative, Chair and Chief, Department of Obstetrics and Gynecology, California Pacific Medical Center, San Francisco, CA JOHN O L DELANCEY, MD LAURIE J MCKENZIE, MD Norman F Miller Professor of Gynecology, Director, Pelvic Floor Research, Group Director, Fellowship in Female Pelvic Medicine and Reconstructive Surgery, University of Michigan Medical School, Ann Arbor, MI Director of Oncofertility, Houston IVF, Director, Houston Oncofertility Preservation and Education (H.O.P.E.), Houston, TX SALES & MARKETING KEN SYLVIA Vice President, Group Publisher [email protected] 732-346-3017 AVIVA BELSKY Publisher [email protected] 732-346-3044 ALISON O’CONNOR National Account Manager [email protected] 732-346-3075 BILL SMITH Account Manager, Classified/Display Advertising [email protected] 440-891-2718 MAUREEN CANNON Permissions/International Licensing [email protected] JACQUELINE MORAN Account Manager, Recruitment Advertising [email protected] 440-891-2762 RENEE SCHUSTER List Account Executive [email protected] REPRINT SERVICES 800-290-5460, ext. 100 [email protected] AUDIENCE DEVELOPMENT JOE MARTIN Audience Development Manager [email protected] CHRISTINE SHAPPELL Audience Development Director 201-391-2359 or 201-240-0867 [email protected] ROBIN FARIAS-EISNER, MD, PHD SHARON T PHELAN, MD Chief, Gynecology and Gynecologic Oncology, Department of Obstetrics and Gynecology, Director of the Center for Biomarker Discovery and Research, UCLA Health System, Los Angeles, CA Professor, Department of Obstetrics and Gynecology, University of New Mexico, Albuquerque, NM PAULA J ADAMS HILLARD, MD JOE LEIGH SIMPSON, MD Professor, Department of Obstetrics and Gynecology, Chief, Division of Gynecologic Specialties, Stanford University School of Medicine, Stanford, CA Executive Associate Dean for Academic Affairs, Professor of Obstetrics and Gynecology, and Human and Molecular Genetics, Florida International University College of Medicine, Miami, FL Chief Executive Officer JOE LOGGIA Executive Vice President, Chief Administrative Officer TOM EHARDT Executive Vice President, Chief Marketing Officer STEVE STURM Executive Vice President, Finance and Chief Financial Officer TED ALPERT President ANDREW POLLARD Executive Vice President GEORGIANN DECENZO Executive Vice President CHRIS DEMOULIN Executive Vice President DANNY PHILLIPS Executive Vice President RON WALL Executive Vice President ERIC LISMAN Vice President, Media Operations FRANCIS HEID Vice President, General Counsel WARD D. HEWINS Vice President, Human Resources NANCY NUGENT Chief Information Officer J VAUGHN FOUNDING EDITOR—JOHN T QUEENAN, MD Professor of Obstetrics and Gynecology, Georgetown University School of Medicine, Washington, DC ADDRESS EDITORIAL AND BUSINESS CORRESPONDENCE to CONTEMPORARY OB/GYN, 24950 Country Club Boulevard, Suite 200, North Olmsted, OH 44070 MAIN NUMBERS: 440-243-8100 or 800-225-4569 DIRECT REPRINT REQUESTS: 800-290-5460, ext. 100; International: 717-505-9701, ext. 100; e-mail: [email protected] CUSTOMER SERVICE: 877-922-2022, or write: Circulation Dept, Advanstar Communications Inc, 131 West 1st Street, Duluth, MN 55802 CLASSIFIED ADVERTISING: 800-225-4569 Advanstar Communications Inc. provides certain customer contact data (such as customers’ name, addresses, phone numbers, and e-mail addresses) to third parties who wish to promote relevant products, services, and other opportunities that may be of interest to you. If you do not want Advanstar Communications Inc. to make your contact information available to third parties for marketing purposes, simply call toll-free 866-529-2922 between the hours of 7:30 a.m. and 5 p.m. CST and a customer service representative will assist you in removing your name from Advanstar’s lists. Outside the U.S., please phone 218-740-6477. CONTEMPORARY OB/GYN does not verify any claims or other information appearing in any of the advertisements contained in the publication, and cannot take responsibility for any losses or other damages incurred by readers in reliance on such content. CONTEMPORARY OB/GYN cannot be held responsible for the safekeeping or return of unsolicited articles, manuscripts, photographs, illustrations, or other materials. Library Access Libraries offer online access to current and back issues of CONTEMPORARY OB/GYN through the EBSCO host databases. To subscribe, call toll-free 877-527-7008. Outside the U.S. call 218-740-6477. JANUARY 2012 CONTEMPORARY OB/GYN 1 JANUARY 2012 . N G B Y A R O P M E T N CO VOL. 57, NO. 1 TTranslating Science into Sound Clinical Practice 20 Postpartum contraception: Ways to avoid VTE PAUL D. BLUMENTHAL, MD, MPH AMY J. VOEDISCH, MD, MS Postpartum contraception is an important consideration for new mothers. Providers and patients should discuss the advantages and disadvantages of each method, breastfeeding intention, risk of VTE, and timing. 20 FETAL MONITORING MYTHBUSTERS 16 Fetal heart monitoring: Atypical variable decelerations DAVID A. MILLER, MD NEWSLINE This second article in the series reviews levels of scientific evidence supporting the prognostic value of “atypical” variable decelerations. 32 10 CLINICAL INSIGHTS IVF increases risk for ovarian tumors ■ Keys to success with midurethral slings 6 MARY T. MCLENNAN, MD Are all midurethral slings equal? Is there still a role for the Burch procedure? Judicious patient selection is critical to selecting the most appropriate treatment for stress urinary incontinence. EDITORIAL CHARLES J. LOCKWOOD, MD, MHCM Washington’s political failures and your practice 12 LEGALLY SPEAKING ANDREW I. KAPLAN, ESQ Missed bradycardia, decelerations alleged as cause of periventricular leukomalacia 41 46 47 CLASSIFIED AD INDEX PROTOCOLS FOR HIGH-RISK PREGNANCY PATRICK M. CATALANO, MD The effects of obesity on pregnancy and delivery CONTEMPORARY OB/GYN (Print ISSN#0090-3159, DIGITAL ISSN#2150-6264), is published monthly by Advanstar Communications, Inc, 131 West First St, Duluth, MN 55806-2065. One-year subscription rates: $110.00 per year (USA and Possessions); $140.00 per year (elsewhere). Single copies (prepaid only) $12.00 in the USA; $18.00 per copy elsewhere. Include $6.50 per order plus $2.00 for US postage and handling. Periodicals postage paid at Duluth, MN 55806 and additional mailing offices. POSTMASTER: Please send address changes to Contemporary OB/GYN, PO Box 6084, Duluth, MN 55806-6084. Return Undeliverable Canadian Addresses to: Pitney Bowes, PO Box 25542, London, ON N6C 6B2, CANADA. Canadian GST number: R-124213133RT001. Publications Mail Agreement Number 40612608. Printed in USA. Subscription inquiries/address changes: toll-free 888-527-7008, or dial direct 218-740-6477. ©2012 Advanstar Communications Inc. All rights reserved. No part of this publication may be reproduced or transmitted in any form or by any means, electronic or mechanical, including by photocopy, recording, or information storage and retrieval without permission in writing from the publisher. Authorization to photocopy items for internal/educational or personal use, or the internal/educational or personal use of specific clients is granted by Advanstar Communications Inc for libraries and other users registered with the Copyright Clearance Center, 222 Rosewood Dr, Danvers, MA 01923, 978-750-8400 fax 978-646-8700 or visit http://www. copyright.com online. For uses beyond those listed above, please direct your written request to Permission Dept, fax 440-756-5255 or email: [email protected]. 2 CONTEMPORARYOBGYN.NET JANUARY 2012 COVER ILLUSTRATION FOR CONTEMPORARY OB/BYN BY 3FX, 3D LIFE SCIENCE ANIMATION & EFFECTS GRAND ROUNDS Alexis O ® C-Section Retractor RE TRA TION C PR OTECTION EX POSURE “Easier surgery, shorter surgery time, better exposure, less blood loss, less pain, and fewer post-op wound infections.” Ron Lichtenstein M.D. Scan QR-Code with your mobile device to learn more about the Alexis O C-Sec tion Retrac tor. A New Generation Medical Device Company For more information, please visit www.alexiscsection.com or call 800.282.2212 ©2011 Applied Medical Resources Corporation. All rights reserved. Applied Medical, the Applied Medical logo design and marks designated with a ® are trademarks of Applied Medical Resources Corporation, registered in one or more of the following countries: Australia, Canada, Japan, the United States and/or the European Union. 1266AL1211 magenta yellow cyan black obgyn0112_003.pgs 12.19.2011 10:36 ADVANSTAR_PDF/X-1a Translating Science into Sound Clinical Practice ONLINE Part of the Your guide to what’s happening online at Contemporary OBGYN.net Y Yo Contemporary OB/GYN is part of the ModernMedicine Network, a Web-based portal for health professionals offering best-in-class content and tools in a rewarding and easy-to-use environment for knowledge-sharing among members of our community. Should you offer office-based gynecologic surgery? Follow Dr. Morris Wortman step by step through an endomyometrial resection in an office setting. Scan to view this video or go to HTTP://CONTEMPORARYOBGYN.NET/OFCSURG AHRQ’s Effective Health Care Clinician site offers best practice summaries, physician and patient guides, and more: Read Dr. Joshua Copel’s latest blog on ob/gyn issues HTTP://CONTEMPORARYOBGYN.NET/BLOG HTTP://CONTEMPORARYOBGYN.NET/EFFECTIVE 1 3 Novel imaging device tells breast surgeons if they’ve left any tumor behind A new ultrasound device helps improve the surgeon’s ability to complete lumpectomy in one procedure. Autoimmune disease deters chronic wound healing Patients with chronic wounds who had autoimmune disease have worse outcomes than those without it. 6 4 Mode of delivery doesn’t affect later maternal stress Whether a woman gives birth by elective cesarean or vaginal delivery may not affect her anxiety or stress levels afterward. Dating violence common among teens in the ED More than half of teens and young adults treated at an inner-city ED said they had experienced dating violence. contemporaryobgyn.net/dapagliflozin 7 5 Moratorium urged on lengthy antibiotics for chronic rhinosinusitis EMRs are rarely encrypted, so a data breach could be triggered by theft of a laptop or lost jump drive. Symptoms of chronic rhinosinusitis are often nonspecific and do not warrant antibiotic treatment, according to findings reported in Clinical Infectious Disease. contemporaryobgyn.net/encrypt contemporaryobgyn.net/sinusitis contemporaryobgyn.net/violent contemporaryobgyn.net/ birthstress Dapagliflozin: An emerging treatment option for type 2 diabetes mellitus Dapagliflozin is a sodium glucose co-transporter inhibitor under review for FDA approval for the treatment of type 2 diabetes mellitus. contemporaryobgyn.net/heal contemporaryobgyn.net/margin 2 The top ob/gyn clinical and practice management resources from ModernMedicine.com Electronic medical records rarely encrypted LEARN WHAT YOU’RE MISSING: Our online digital editions let you flip through the pages of your favorite Advanstar Communications publications from any computer. Sign up free at the following Web sites: Contemporary Pediatrics: ContemporaryPediatrics.com/digital Medical Economics: memag.com/digital 4 CONTEMPORARYOBGYN.NET Formulary: formularyjournal.modernmedicine.com/digital Managed Healthcare Executive: managedhealthcareexecutive.com/digital JANUARY 2012 Drug Topics: drugtopics.com/digital STELLA/GETTY IMAGES (BOTTOM LEFT); PURESTOCK/GETTY IMAGES (BOTTOM MIDDLE); IMAGE SOURCE/GETTY IMAGES (BOTTOM RIGHT) THE TOP 7 HIT LIST The Best Is Now The Easiest 1. Slide On. Engineered With Our New Easy Load Design Always the Best: 2. Slide Back. • Superior strength – Metal construction ensures better durability and tactile feedback • Precise control – 140° of articulation at the cervix, with locking handle • Safer surgery – Multiple tip and KOH Cup™ sizes provide unparalleled delineation of the fornix Now the Easiest: 3. Insert tip into uterus. Inflate balloon. 4. Push Koh-Efficient forward to advance around cervix. • Faster set up – Integrated KOH Cup and pre-attached occluder balloon facilitates assembly • Easier insertion – Easy load design permits insertion under direct visualization • Better visibility – Koh-Efficient™ slides forward to securely lock cup in place around the cervix • Longer length – Accommodates larger patients • Single-use cup – Sterile, accurate and stable cutting surface for each surgery During TLH procedures, the Koh-Efficient creates a ‘margin of safety’ by providing a visual landmark and backstop for full circumferential colpotomy, as well as distancing the ureters during the incision. Vaginal length is maximized and pneumoperitoneum is maintained. RUMI II is engineered with our easy load system making it simple and easy to insert. Scan. Watch. Learn. or go to coopersurgical.com/RUMI To schedule a demonstration or trial of the RUMI II System, call 800.243.2974 or 203.601.5200. Visit coopersurgical.com or see us at youtube.com/coopersurgical ©2011 CooperSurgical, Inc. 81944 Rev. 03/14 BY CHARLES J. LOCKWOOD, MD, MHCM Washington’s political failures and your practice T o say I am frustrated by the failure of the Joint Select Committee on Deficit Reduction (aka the “super committee”) to reach a sensible plan to reduce the federal government’s crushing debt burden is an understatement. Ostensibly fueled by conservative intransigence over tax increases and liberal immobility over entitlement reform, it seems that the net effect is continued governmental paralysis amid the greatest intergenerational wealth transfer in history. In his new book, Boomerang: Travels in the New Third World, Michael Lewis details how a similar lack of political will, fiduciary responsibility, and simple common sense is eroding Europe’s future economic stability as well.1 In this fascinating little book, Lewis also points out that in addition to ballooning federal governmental deficits, US state and local governments face a $500 billion collective annual deficit and a $1.5 trillion gap between what they owe retired workers and the funds they have on hand to pay them. He ascribes both America’s addiction to debt and our accelerating obesity epidemic to our primitive midbrain “reptilian core” that, after millennia of periodic famines, wars, and other external threats, prompts us to “acquire as much as we can of things we perceive as scarce.” While one is free to ascribe the super committee’s abject failure to an inherent collective neurophysiologic dysfunction, a more prosaic explanation is that it is just another symptom of the increasing polarization of the American polity. However, I would like to offer a third, less charitable and far more cynical interpretation. The super committee’s failure will, after all, automatically trigger $1.2 trillion in cuts, equally divided between social programs and defense spending, over the next 10 years.2 Moreover, these reductions in government spending will likely be coupled with $3.9 trillion in added tax revenue accruing expiration of the Bush-era tax cuts, assuming our current governmental gridlock conveniently continues.3 Thus, through simple inaction Congress would have reduced by a significant portion the $8.4 trillion in additional debt the US government would have otherwise accumulated by 2021.4 The best part for them is that politicians facing an angry electorate can deny, with some justification, that they were personally responsible for either cuts in social services or increases in taxes. But this is a cynical interpretation. Perhaps it is best to blame our lizard-derived hypothalami. 6 CONTEMPORARYOBGYN.NET JANUARY 2012 Implications to healthcare So what are the implications of Congress’ extraordinary feat of budgetary legerdemain for US healthcare? The immediate impacts of the pending across-the-board cuts include: • a 2% cut to Medicare amounting to $123 billion over 8 years.2 These cuts will fall on physicians and hospitals and could reduce their availability to care for elderly patients. This assumes Congress will come to its senses and not enact the scheduled 27% SGR-mandated physician payment reduction5 scheduled for January 1, which, in my opinion, would effectively end the program. In any case, this Medicare cut will be exacerbated by Medicaid cuts to providers being implemented by virtually every state. • a $ 600 million reduction in the Special Supplemental Nutrition Program for Women, Infants, and Children at a time when poverty affects more and more Americans.6 • a 2%, or about $2.5 billion, cut in the National Institutes of Health budget in 2013, which will exacerbate the stagnant funding that has occurred since 2006.7 • a potential 2% cut in graduate medical education (GME) layered onto the GME cap put into effect in 1997. This could reduce available residency slots just as there has been a sizeable increase in medical student admissions over the past 5 years.8 Thus, US medical school graduates may find it more difficult to obtain residency slots, exacerbating the pending physician shortage. Implications for ob/gyns While all this is bad news for ob/gyns, the fiscal outlook is further darkened by the impact that prolonged economic woes are having on obstetric volume. While the Great Recession has technically ended, the economy remains extremely anemic, and unemployment continues to hover at around 9%.4 In an April 2009 editorial, I noted that the period from 2003 to 2007 had seen a “boomlet” in births, peaking in 2007 at 4,316,233, and that as a consequence of the recession births would fall to 2003 levels in the future.9 Thus far, this has proved to be a fairly accurate prediction. Figures from the latest National Center for Health Statistics (NCHS) report 4,000,279 births in 2010, a 9% decline from 2007 and within 20,000 deliveries of 2002-2003 levels. The main drivers of the decrease appear to be that birth rates for women in their twenties and thirties declined somewhat in 2010 while the rate for women aged EMERGING EXPERTS Contemporary OB/GYN is pleased to announce the members of our new Emerging Experts panel: active, involved young clinicians distinguished by their leadership within the specialty. You’ll read and hear their influence within our pages and online in the months ahead. Rebecca H. Allen, MD, MPH Tamara Helfer, MD Jessica A. Shepherd, MD Brown University Providence, RI Christie Clinic Champaign, IL University of Louisville Louisville, KY René Allen, MD Michelle Y. Owens, MD Dane M. Shipp, MD Santa Barbara Fertility Center Santa Barbara, CA University of Mississippi Jackson, MS Pacific Coast Women’s Health Encinitas, CA May H. Blanchard, MD Richard B. Rosenfield, MD M. Jonathon Solnik, MD University of Maryland Baltimore, MD Pearl Women’s Center Portland, OR Cedars-Sinai Medical Center Los Angeles, CA Erin T. Carey, MD Matthew Seidhoff, MD, MSCR Barton Staat, MD University of North Carolina Chapel Hill, NC University of North Carolina Chapel Hill, NC Denver, CO Stella M. Dantas, MD, FACOG Kaiser Permanente Beaverton, OR EDITORIAL 20 to 24 dropped 6% to 90.0 births per 1,000 women, the lowest level ever reported. In contrast, the birth rate for women in their early forties rose in 2010, the only agespecific rate to do so, although the total number of births is too small to have an impact in terms of overall births.10 Not to sound overly pessimistic, the latest NCHS data10 also contain some good news: • Te birth rate for US teenagers aged 15-19 years dropped 9% to 34.3 per 1,000, a record low for the nation. • Te cesarean delivery rate declined slightly to 32.8%, the first drop in this rate in more than a decade. Many theories have been proffered to explain the prior relentless increase in cesarean deliveries, including a decrease in vaginal births after cesarean delivery, an increase in cesareans performed for maternal request, increased numbers of high-risk expectant mothers, the medicolegal environment, and changes in provider practice patterns. In contrast, the reasons for this unexpected, albeit salutary, decline remain obscure. • Te preterm birth rate fell for the fourth year in a row to 11.99% from its peak of 12.8% in 2006. Preterm birth is the leading cause of infant morbidity and mortality in the US, so this is welcome news indeed. The decline in the rate for 2010 was primarily among infants delivered late preterm (34 to 36 weeks), down from 8.66% to 8.49%, while the rate for early preterm births (less than 34 weeks) remained stable at 3.5%. Tese downward trends may be partly because of recent efforts to reduce iatrogenic prematurity.9 While these three positive trends are welcome and bode well for public health, they don’t do much for an ob/gyn’s practice income. Worse, the super committee’s failure could further depress overall birth rates because Congress’ apparent ineffectiveness may lead to another downgrade in the US credit rating, which on August 5 was reduced by Standard & Poor’s Ratings Services from AAA to AA+. This would increase interest rates, slowing the economy further. In addition, the resultant, rather indiscriminate removal of $5.1 trillion from the economy could trigger a double-dip recession. Overall, there appears to be near unanimity of opinion that the decline in US births is related to the present economic climate.11 For example, North Dakota, with one of the nation’s lowest unemployment rates in 2008, at about 3%, was 1 of only 2 states to show a slight increase in its birth rate from 2008 to 2009.12 Thus, Congressional ennui could prompt a decline in US birth rates to levels not seen since the Great Depression. Take-home message The super committee’s failure will lead to cuts in Medicare and Medicaid funding that will modestly hurt many ob/ gyns’ incomes. However, these untoward economic effects may be amplified by parallel reductions in commercial and 8 CONTEMPORARYOBGYN.NET JANUARY 2012 managed care payments that are often pegged to Medicare fees. Reductions in revenue are hitting at a time when practice expenses are increasing because of implementation of electronic health records. In addition, any worsening of the economy could exacerbate downward pressure on birth rates, preventing most ob/gyn practices from mitigating these financial threats through increased obstetrical volume. But maybe I am viewing the world through reptilian eyes. DR LOCKWOOD, editor in chief, is Dean of the College of Medicine and Vice President for Health Sciences at The Ohio State University School of Medicine, Columbus, Ohio. REFERENCES 1. Lewis M. Boomerang: Travels in the New Third World. New York, NY: W.W. Norton & Company; 2011. 2. Bingham A. Grandma, grandpa spared from bulk of automatic supercommittee cuts. ABC News Web site. http://abcnews.go.com/blogs/politics/ 2011/11/grandma-grandpa-spared-from-bulk-of-automatic-super-committeecuts/. Published November 21, 2011. Accessed December 2, 2011. 3. US House of Representatives Republican Caucus, Committee on the Budget. CBO’s budget update: the looming lost decade. http://www.budget. house.gov/UploadedFiles/cbohbcanalysis8192010.pdf. Published August 19, 2010. Accessed December 2, 2011. 4. Manuel D. CBO estimates that United States will post deficit of “close“ to $1.5 trillion in 2011. Dave Manual.com Web site. http://www.davemanuel. com/2011/01/26/cbo-148-trillion-deficit-expected-for-2011/. Posted November 29, 2011. Accessed December 2, 2011. 5. McDermott Will & Emery. Final 2011 Medicare physician fee schedule update implements key reform provisions. http://www.mwe.com/info/news/ wp1210a.pdf. Published December 2, 2010. Accessed December 2, 2011. 6. Khan H. Automatic budget cuts put public education, health care on the line. ABC News Web site. http://abcnews.go.com/blogs/politics/2011/11/ automatic-budget-cuts-put-public-education-health-care-on-the-line/. Published November 25, 2011. Accessed December 2, 2011. 7. Przybyla H. Deficit panel’s failure aims at defense while sparing Medicaid. Bloomberg Businessweek Web site. http://www.businessweek.com/ news/2011-11-24/deficit-panel-s-failure-targets-defense-while-sparingmedicaid.html. Published November 22, 2011. Accessed December 2, 2011. 8. Helfand D. Medical school enrollment is on the rise. Los Angeles Times. October 25, 2011. http://articles.latimes.com/2011/oct/25/business/la-fimedical-school-enrollment-20111025. Accessed December 2, 2011. 9. Donovan EF, Lannon C, Bailit J, et al; Ohio Perinatal Quality Collaborative Writing Committee. A statewide initiative to reduce inappropriate scheduled births at 36 (0/7)-38 (6/7) weeks’ gestation. Am J Obstet Gynecol. 2010;202(3):243.e1-243.e8. Erratum in: Am J Obstet Gynecol. 2010;202(6):603. 10. Hamilton B, Martin JA, Ventura SJ. Births: Preliminary data for 2010. National vital statistics reports; vol 60, no 2. Hyattsville, MD: National Center for Health Statistics; November 2011. http://www.cdc.gov/nchs/data/nvsr/ nvsr60/nvsr60_02.pdf. Accessed December 2, 2011. 11. US birth rates dip with the economy, plummet for young women, CDC report shows. Washington Post. November 17, 2011. http://www. washingtonpost.com/national/health-science/cdc-report-birth-ratesplummet-for-young-women-as-economy-worries-likely-keep-the-storkaway/2011/11/17/gIQA9qwiUN_story.html. Accessed December 2, 2011. 12. Tavernise S. Dip in birth rates reflects recession, report suggests. New York Times. October 12, 2011. http://www.nytimes.com/2011/10/13/ us/birth-rate-decline-reflects-recession-pew-center-says.html. Accessed December 2, 2011. TWIN-TWIN TRANSFUSION SYNDROME (TTTS) KNOWING WHAT TO LOOK FOR MAY NOT BE EASY. KNOWING WHERE TO LOOK FOR HELP IS. While twin fetuses may simply appear unbalanced in size, it could be twin-twin transfusion syndrome (TTTS). This potentially fatal condition causes an uneven flow of blood between fetuses and occurs in 10% of monochorionic diamniotic pregnancies. Early detection and intervention are key. At Texas Children’s Fetal Center, our experts have refined the use of a delicate in utero laser ablation to stop the uneven blood exchange when it occurs, saving hundreds of twins’ lives. As national leaders in the diagnosis and treatment of abnormalities such as TTTS, our multidisciplinary team at Texas Children’s Fetal Center takes on the most complicated fetal conditions and ensures the best possible outcomes for high risk patients. Send us your toughest cases. We’re known for delivering. Learn more: fetal.texaschildrens.org or 1-877-FetalRx ©2011 Texas Children’s Hospital. All rights reserved. FC188_080911 Emergent TTTS, where the recipient twin is much larger than the donor twin. Clinical Insights IVF increases risk for ovarian tumors Ovarian stimulation for in vitro fertilization (IVF) may double or even quadruple a woman’s risk for an ovarian tumor in the next 15 years, according to a cohort study from the Netherlands involving almost 20,000 women who received IVF treatment between 1983 and 1995 and a comparison group of about 6,000 subfertile women not treated with IVF. After a median follow-up of 14.7 years, the authors calculated 77 ovarian malignancies in the full cohort, of which 42 were invasive ovarian cancers and 35 were borderline ovarian tumors. Sixty-one malignancies occurred in the IVF group (standardized incidence ratio [SIR], 1.59; 95% confidence interval [CI], 1.21-2.04) and 16 occurred in the non-IVF group (SIR, 1.02; 95% CI, 0.59-1.66). The SIR for a borderline ovarian tumor in the women undergoing IVF across all intervals was 1.93 (95% CI, 1.31-2.73) versus 0.67 (95% CI, 0.18-1.71) in the non-IVF group. Compared with the non-IVF group, the overall SIR for invasive ovarian cancer was not significantly elevated in the IVF group except at 15 or more years post-IVF, when it was 3.54 (95% CI, 1.62-6.72) versus 1.09 (0.30-2.79). In both groups, the SIRs were strongly increased in the first year after IVF, possibly because of greater vigilance during workups for subfertility diagnosis and treatment. Excluding the first year of follow-up, the SIR for all ovarian malignancies was 1.49 (95% CI, 1.12-1.94) for the IVF group and 0.85 (95% CI, 0.45-1.45) for the non-IVF group. The authors write that although their findings give some cause for concern, they are based on relatively small numbers. They also found no dose-response relationship, and the risk increase for invasive ovarian cancer was not statistically significant in multivariable analyses. van Leeuwen FE, Klip H, Mooij TM, et al. Risk of borderline and invasive ovarian tumours after ovarian stimulation for in vitro fertilization in a large Dutch cohort. Hum Reprod. 2011;26(12):3456-3465. Small practices slow to adopt EMRs Although the number of physician practices that have adopted electronic medical records (EMRs) is rising 10 magenta yellow cyan black CONTEMPORARYOBGYN.NET NEWSLINE overall, the smallest and largest practices have vastly different adoption rates. A recent survey of almost 238,000 medical sites found that 40.4% of physician offices used EMRs as of July 2011, up from 38.7% in October 2010. Whereas 75.5% of practices with 26 or more physicians used EMRs, only 51% of practices with 3 to 5 physicians had adopted the technology. For two-physician and solo practices, the proportion was even lower: 41.6% and 30.8%, respectively. The cost of EMR systems, confusion about federal incentives for using them, concerns about practice disruptions they might cause, and questions about whether their benefits exceed their cost are deterring small practices from adopting EMRs, according to analysts. Under a provision of the 2009 economic stimulus package, practices can earn up to $44,000 per physician over 5 years from Medicare or almost $64,000 over 6 years if they show meaningful use of EMRs. Depending on the system a practice chooses, however, these incentive payments might not be enough to cover the investment by the practice. Indeed, according to the survey that was conducted by SK&A, an Irvine, California, marketing firm, 16.7% of practices that didn’t buy systems indicated that cost was a major factor. The survey also showed that 21% of respondents weren’t even familiar with the government incentive program. Dolan PL. Why small medical practices lag in EMR adoption. American Medical News. November 7, 2011. www.ama-assn.org/ amednews/2011/11/07/bil21107.htm. Accessed December 6, 2011. Clinicians not properly screening, treating osteoporosis According to the findings of a recent study from Pennsylvania, many women who are at risk for osteoporosis are not being properly screened or treated by their physicians. Researchers studied 615 postmenopausal women of at least 49 years of age who were sent for dual-energy x-ray absorptiometry (DXA) bone density screening between 2007 and 2009, using the 2006 Osteoporosis Position Statement of the North American Menopause Society (NAMS) as a guideline. Among other things, the JANUARY 2012 obgyn0112_010.pgs 12.21.2011 12:29 ADVANSTAR_PDF/X-1a CLIN ICA L INSIGHTS guidelines stipulate that in the absence of certain risk factors, clinicians should not initiate DXA screening until women are at least 65 years of age and should not initiate treatment unless postmenopausal women already are osteoporotic or have T scores between -2.5 and -2.0. Among the participants, 41.3% should not have been tested because they did not meet the testing criteria. Even when the 2010 version of the NAMS guidelines were applied, 40% still did not meet the criteria. Of the 41.3%, one-fourth (25.5%) were not taking calcium, one-third (31.1%) were not taking vitamin D, and more than one-half (52.9%) were not exercising at least 2 hours per week. Of the 102 women with any of the approved indications for treatment, 15.7% were not taking calcium, 18.6% were not taking vitamin D, 52.7% were not exercising at least 2 hours per week, and 35.3% were not receiving pharmacotherapy. Interestingly, among the women without an indication for treatment, 17.8% were receiving bisphosphonate, raloxifene, or calcitonin therapy. Although clinicians may follow other guidelines, all current recommendations are largely similar. The researchers conclude that although it is time-consuming, clinicians must take time to educate their patients about why screening may be unnecessary and about the longterm risks associated with bisphosphonate use. Schnatz PF, Marakovits KA, DuBois M, O’Sullivan DM. Osteoporosis screening and treatment guidelines: are they being followed? Menopause. 2011;18(10):1072-1078. Self-collected specimens more sensitive for HPV than a Pap test A community-based, randomized, equivalence trial conducted in Mexico suggests that human papillomavirus (HPV) testing using self-collected specimens was more than 3 times more sensitive than cervical cytology samples taken in a clinician’s office. The researchers say the results indicate that we may want to change to front-line, largescale use of HPV testing in areas with limited cervical cytology availability. The trial involved more than 25,000 Mexican women of low socioeconomic status aged 25 to 65 years from medically underserved, rural areas. The researchers randomly assigned the women to either HPV DNA testing of a vaginal sample self-collected at home or conventional cervical cytology with samples obtained professionally at the nearest health center. NEWSLINE The authors calculated an HPV prevalence of 9.8% (95% CI, 9.1-10.4) and an abnormal cytology rate of 0.38% (0.23-0.45). HPV testing identified 117.4 per 10,000 women (95.2-139.5) with CIN 2 or worse, while cytology identified 34.4 per 10,000 (23.4-45.3), meaning HPV testing was about 3.4 times (2.4-4.9) more sensitive. Similarly, HPV testing detected 4.2 (1.9-9.2) times more invasive cancers than did cytology (30.4 per 10,000 [19.1-41.7] vs 7.2 per 10,000 [2.2-12.3]). Although the positive predictive value of HPV testing using self-collected vaginal specimens for CIN 2 or worse was considerably lower than for cytology (12.2% [9.9-14.5] vs 90.5% [61.7-100], respectively), such testing has a lower price tag, easier implementation, and a lower false-negative rate than cytology. This, combined with its high sensitivity, make it an ideal choice for women in underserved areas who may be screened only a few times in their lives, say the researchers. In this way, coverage is greatly expanded without the expense of cytology clinics. Lazcano-Ponce E, Lorincz AT, Cruz-Valdez A, et al. Self-collection of vaginal specimens for human papillomavirus testing in cervical cancer prevention (MARCH): a community-based randomised controlled trial. Lancet. 2011;378(9806):1868-1873. More teens using hormonal contraceptive methods The proportion of teenage girls who use hormonal contraceptive methods other than the pill during their first sexual encounter increased significantly from 2% in 2006 to 6% in 2010, according to a report from the Centers for Disease Control and Prevention. In the most recent period, 78% of females and 85% of males used contraception at their first sexual encounter. Eight in 10 males used a condom, an increase of 9% since 2002, and it remained the most common contraceptive choice. Dual contraceptive use at first sex—a condom combined with a partner’s hormonal contraceptive—was 16%, an increase of 6%. About 43% of never-married teenage girls have had sexual intercourse at least once; for never-married teen boys, this figure is 42%. Although levels of sexual experience have not changed significantly since 2002, the percentages of teens with sexual experience has declined within the past 20 years. Non-Hispanic black males were most likely to be sexually experienced and Hispanic males were most likely to have used no contraception at last sex. Centers for Disease Control and Prevention. More teen males using condoms. October 12, 2011. www.cdc.gov/media/releases/2011/p1012_teen_condoms. html. Accessed December 6, 2011. JANUARY 2012 CONTEMPORARY OB/GYN 11 BY A ANDREW I KAPLAN, ESQ Missed bradycardia, decelerations alleged as cause of periventricular leukomalacia A 32-year-old woman pregnant with her second child had her fi rst prenatal visit at the defendant obstetrician’s office in August, at which her initial screening and evaluation were within normal limits and her estimated date of confi nement (EDC) was April 3. At 16 weeks, the fetal heart rate (FHR) was recorded via Doppler ultrasound and the patient’s maternal serum alpha-fetoprotein (MSAFP) test results were within normal limits. However, she was anemic and was given a prescription for an iron supplement. A follow-up ultrasound at 20 weeks showed a “questionable abnormality” (pyelectasis of both kidneys with decreased amniotic fluid) in the fetus. An amniocentesis was performed the next day; no abnormalities were Read about a found. The patient’s new noninvasive glucose stress test at algorithm 25 weeks’ gestation was that predicts morbidity risk in normal, as was a 29-week preterm infants: ultrasound. contemporaryobgyn.net/PhysiScore At 36 weeks, an ultrasound revealed that the infant was in breech position; the patient’s full examination and urinalysis otherwise were within normal limits. The obstetrician discussed the possibility of an external cephalic version, including risks, benefits, and alternatives, and cesarean delivery. 12 CONTEMPORARYOBGYN.NET JANUARY 2012 Four days later, another ultrasound revealed the infant was still in breech lie; however, there was positive fetal movement. The patient deferred version and agreed to schedule a cesarean delivery. Examination at 37 weeks found the patient’s cervix long, closed, and posterior, and she was not in labor. Follow-up ultrasound revealed that the infant had shifted spontaneously to the vertex position. At the last prenatal visit in March, the obstetrician met with the patient and her spouse and discussed the risks of cesarean delivery. The couple opted for a cesarean delivery by maternal request. The next day, the patient presented to the co-defendant hospital for an elective cesarean delivery. She was admitted to labor and delivery (L&D) at 3:35 pm. Consent for the procedure was obtained by the nurse midwife and L&D nurse, who continued to follow her via external FHR monitoring for the next 55 minutes. The strips reflected an FHR between 130 and 140 beats per minute (bpm) with moderate variability and contractions as well as evidence of fetal movement. The L&D nurse was concerned about bradycardia, but realized that she was picking up the maternal heartbeat. PHOTODISC/DAVID JOEL/GETTY IMAGES THE FACTS LEGALLY SPEAKING Over the next 24 hours the infant’s vital signs were stable, he had a strong suck reflex and good muscle tone, and he was alert and in no distress. The patient was continuously monitored until 10 minutes prior to being moved to the delivery room. Contractions lasting 30 to 90 seconds were documented at 2-minute intervals without dilation. At the commencement of the FHR tracing, the defendant obstetrician entered the room, looked at the strips, and spoke with the patient, but did not look at subsequent strips. She was not advised of any fi ndings on them until the patient was taken to the delivery room. At approximately 3:50, the FHR fell into the 90 bpm range for approximately 10 minutes; both late and variable decelerations were ostensibly picked up thereafter. The L&D nurse was concerned about bradycardia, but soon realized that she was picking up the maternal heartbeat, whereupon she adjusted the monitor. The readings returned to baseline, consistent with the FHR of 154 bpm, which was confi rmed by Doppler in the delivery room. First incision was made at 4:50, and the report ref lects that the infant was in an oblique lie that changed to breech when membranes were ruptured. He was delivered 9 minutes later as abreech presentation without meconium in the amniotic f luid and with Apgar scores of 3 at 1 minute and 8 at 5 minutes. Positive pressure ventilation was administered for 30 seconds as well as blow-by-blow oxygen with saturations at 95%. The infant pinked up immediately, cried with stimulation and oxygen, and was pink, vigorous, and breathing comfortably with a 100% oxygen saturation 30 minutes after delivery. A nuchal cord was observed during delivery. The infant was moved to the well-baby nursery where he had good color, slept well, voided urine and feces, and was fed. Over the next 24 hours his vital signs were stable, he had a strong suck reflex and good muscle tone, and he was alert and in no distress. The impression was of a well baby with mild neonatal hyperbilirubinemia. Mother and infant were discharged 3 days later. One year later an MRI performed on the boy reflected “most likely periventricular leukomalacia,” and thinning of the corpus callosum. He had dysmorphic features, including relative macrocephaly, was significantly developmentally delayed, and did not walk until he was 3 years of age. He later attended public school in a special needs program and had daily occupational, physical, and speech therapy. At age 7 he was nonverbal and could feed himself only with assistance. ALLEGATIONS The plaintiff alleged that because of fetal bradycardia and late decelerations, an earlier cesarean delivery should have been urgently or emergently performed, and that failure to do so resulted in hypoxic ischemic anoxia and brain damage to the fetus. She further alleged that because she had been placed on fetal monitoring, the L&D physician and nurses may have delayed the cesarean delivery by considering a trial of labor. She also asserted that the FHR under 100 bpm at the time of delivery suggested a prolonged period of bradycardia and that the 1-minute Apgar score of 3 was consistent with perinatal asphyxia. DISCOVERY At deposition the plaintiff acknowledged that at her last prenatal visit, she had requested an elective cesarean delivery. The L&D nurse confi rmed that she had placed the patient on external fetal monitoring after obtaining consent for the cesarean; she testified that she had continually monitored the strips from 3:35 PM to almost 4:20 PM. Further, at approximately 3:50 PM—the time the plaintiff contended that a bradycardic change in the FHR had occurred—the nurse testified that she determined it was the maternal heart rate and adjusted the device to listen for the FHR. She said that when she did so, the heart rate was normal; had there been something abnormal or worrisome on the strips, she would have told the obstetrician. The obstetrician would not normally have reviewed the strips unless alerted to something out of the ordinary. JANUARY 2012 CONTEMPORARY OB/GYN 13 LEGALLY SPEAKING The nurse confi rmed that she did not advise the attending that she believed the strips were picking up the maternal heartbeat, but she did note the word “maternal” on the strips. She said she had not seen the obstetrician evaluating the strips after the FHR monitoring commenced. The obstetrician testified that she would not normally have reviewed the strips thereafter unless alerted by the nurse to something out of the ordinary. The nurse and the attending obstetrician confi rmed that the attending occasionally checked on the patient and had not been told that anything of concern had occurred. Despite the plaintiff ’s contentions, the attending testified that the nuchal cord was not a significant fi nding because it was not tight and did not have to be cut. She reduced it from around the infant’s neck and testified that there was no evidence it was causing fetal asphyxia, nor did it affect the timing or mode of delivery. The defense’s pediatric neurology expert testified that the 1-minute Apgar score was not predictive of the infant’s future neurological course and the 5-minute Apgar argued against the hypoxic incident occurring in utero. Furthermore, the fact that the infant had a benign course in the nursery and had lusty/strong cries, was alert and active, was pink in color with an oxygen saturation of 100% within 30 minutes after the delivery, and had good muscle tone and suck argued against an acute hypoxic insult during delivery. The defense’s maternal-fetal medicine expert opined that the defendant obstetrician did not depart from the standard of care prenatally or perinatally, noting the generally reassuring ultrasounds and normal serum testing, and that the patient’s prenatal complaints had been attended to and evaluated. She testified that it was appropriate to admit the patient to the hospital for labor and delivery, evaluate the initial FHR monitoring strips to ensure that they were reassuring, and leave the management of the mother to the nurses, with sporadic physician visits prior to delivery. She also noted that it was appropriate for the The nuchal cord was not a significant finding because it was not tight and did not have to be cut. 14 CONTEMPORARYOBGYN.NET JANUARY 2012 attending to rely on reports from the delivery room nurse prior to the actual delivery. OUTCOME Given the profound injury suffered by the infant plaintiff, the exposure on the case made it a risk to take to trial. The defense entered a motion for summary judgment based on the testimony of the delivery nurse and attending physician, the mother’s concession that she had requested cesarean delivery, and the affidavits of the maternal-fetal medicine expert and pediatric neurologist. The maternal-fetal expert said that in the absence of advice from the L&D nurse of concerning fi ndings or tracings on the FHR strips, the attending had no responsibility to act independent of her routine evaluations of the patient prior to delivery. Further, the delivery room nurse’s actions appeared appropriate, given that FHR strips generated 10 minutes before and at the time the mother was moved to the delivery room documented an infant whose heart rate was in the normal range, supporting the nurse’s observation that the “bradycardia” actually was the maternal heart rate. The maternal-fetal expert agreed that the nuchal cord was unrelated to any subsequent difficulty suffered by the infant, and an affidavit from the neurologist confi rmed that the immediate presentation of the infant argued against an acute hypoxic event. Consequently, the plaintiff discontinued the case against the obstetrician and her group; however, the case against the hospital is pending. ANALYSIS Th is is the rare case in which the plaintiff incurs catastrophic injuries and is not able to formulate a theory of liability sufficient either to settle the case or try it before a jury. Attorneys often hesitate to make summary judgment motions on these cases because if the motion is denied, the plaintiff will by defi nition have established a prima facie case in opposition and the trial probably will go to verdict. The decision to move for summary judgment never should be automatic; however, in cases such as this, a pretrial motion is preferable to a jury trial and possible award. MR. KAPLAN is a partner at Aaronson Rappaport Feinstein & Deutsch LLP, specializing in medical malpractice defense and healthcare litigation. BY D B DAVID A. MILLER, MD Fetal heart monitoring: atypical variable deceleration This second article in the series reviews levels of scientific evidence supporting the prognostic value of “atypical” variable decelerations. T he first article in this series reviewed standard electronic fetal heart rate monitoring (EFM) definitions and categories proposed by the National Institute of Child Health and Human Development (NICHD) and endorsed by the major organizations representing providers of obstetric care in the United States.1-5 This article will review the scientific evidence underlying the predictive value of “atypical” variable decelerations. Before electronic monitoring, fetal condition was assessed by audible changes in the fetal heart rate (FHR).6 The advent of EFM allowed the FHR to be displayed graphically and analyzed visually. Hon, Kubli, and others described visual decelerations in the FHR that were variable in shape and timing relative to uterine contractions.7-9 They attributed these “variable decelerations” to compression of the umbilical cord. Later, Krebs and others described atypical features of variable decelerations, including slow return to baseline rate after the deceleration, loss of variability within the deceleration, loss of primary and secondary accelerations, prolonged acceleration following the deceleration, continuation at a lower baseline rate, and biphasic decelerations.10 Atypical variable decelerations have been reported to confer an increased risk of adverse newborn outcome.10-12 Level I and Level II analytic evidence is capable of establishing statistically significant relationships; Level III descriptive evidence is not. 16 CONTEMPORARYOBGYN.NET JANUARY 2012 TABLE Hierarchy of research design Level I Properly conducted randomized controlled trial Level II-1 Well-designed controlled trial without randomization Level II-2 Well-designed cohort or case-control analytic study Level II-3 Multiple time series with or without the intervention; dramatic results from uncontrolled experiments Level III Opinions of respected authorities, based on clinical experience; descriptive studies or case reports; reports of expert committees US Preventive Services Task Force13 Published evidence regarding atypical variable decelerations will be stratified according to the method outlined by the US Preventive Services Task Force (USPSTF), summarized in the Table.13 Criteria for welldesigned cohort or case-control analytic studies include “appropriate attention to potential confounding variables.” Evidence that does not rise to this standard does not meet USPSTF criteria for definition as Level II. Level I and Level II analytic evidence is capable of establishing statistically significant relationships; Level III descriptive evidence is not. Slow return to baseline after the deceleration Slow return to baseline often is described as a “variable with a late component.” It has been putatively linked to a higher rate of adverse outcomes in newborns. However, no published studies have controlled for the presence or absence of important confounding factors, such as normal baseline rate, moderate variability, or accelerations.10-12 In addition, no published studies have distinguished If you have a question on fetal monitoring, we’d like to hear from you. Those of interest to a wide audience will be answered in future installments of Fetal Monitoring Mythbusters. Send your question to [email protected]. SUBMIT YOUR CLINICAL QUESTION FETAL MONITORING MYTHBUSTERS between clinically benign respiratory acidemia and potentially harmful metabolic acidemia. Hamilton and colleagues found no association between slow return to baseline and metabolic acidemia or neonatal encephalopathy when a “late component” was the only atypical feature.14 There is no Level I or Level II evidence that a “late component” predicts adverse neonatal outcome more often than any other type of deceleration, independent of other clinically important FHR features.10-12,14 Loss of variability within the deceleration The visual similarity between FHR fluctuations within a deceleration and fluctuations in the baseline that define variability has led to speculation that these observations have similar predictive value.10-12,14 The concept of “variability within a deceleration” is misleading on several levels. Standard EFM terminology defines variability as irregular fluctuations in the baseline FHR.1,2 The definition of baseline excludes decelerations1,2; therefore, the definition of variability excludes fluctuations within a deceleration. The 2008 NICHD consensus report stated that moderate baseline variability reliably predicts the absence of metabolic acidemia, an essential prerequisite to intrapartum hypoxic neurologic injury.2,15,16 No published Level I or Level II scientific evidence supports the notion that “variability within a deceleration” has the same predictive value. Loss of primary and secondary accelerations Increases in FHR immediately before and after a variable deceleration have been referred to as “shoulders.” These increases can be visually similar to accelerations, leading to speculation that they have similar predictive value. The 2008 NICHD consensus report stated that FHR accelerations reliably predict the absence of metabolic acidemia2,15,16; however, no published Level I or Level II scientific evidence supports the notion that “shoulders” have the same predictive value as accelerations. baseline.18 Descriptive reports have postulated a range of possible causes, including “mild fetal hypoxia above the deceleration threshold,” “chronic fetal distress,” “transient central nervous system ischemia,” and preexisting neurologic injury.10,17,19 Hamilton and colleagues found no relationship between the overshoot pattern and metabolic acidemia or neonatal encephalopathy.14 Moreover, there is no published Level I or Level II evidence regarding the predictive value of overshoot. In light of inconsistent descriptions in the literature regarding the visual appearance of the overshoot pattern and the existence of multiple conflicting theories regarding etiology, the most reasonable approach is to avoid assigning undue clinical significance to this enigmatic observation. Hamilton and colleagues found no relationship between the overshoot pattern and metabolic acidemia or neonatal encephalopathy. Continuation at a lower baseline rate There are no published Level I or Level II studies of the independent predictive value of continuation of the FHR at a lower baseline rate following a variable deceleration. All available evidence regarding this “atypical” feature is descriptive (Level III).13 Biphasic decelerations Biphasic decelerations, sometimes called “W-shaped” decelerations, have never been shown to predict adverse outcome independent of baseline rate, variability, or accelerations. There is no published Level I or Level II evidence regarding this “atypical” feature. All available evidence is Level III.13 Prolonged acceleration after a deceleration Summary The observation of a prolonged acceleration following a deceleration has been referred to as the “overshoot” pattern. In human fetuses, it has been described as a mild variable deceleration followed by a smooth acceleration less than 20 beats per minute (bpm) above the baseline lasting less than 20 seconds.17 In sheep, the term “overshoot” has been used to describe an abrupt deceleration followed by a sharp spike peaking 25 bpm to 100 bpm above the Electronic fetal monitoring is intended to assess the adequacy of fetal oxygenation during labor. To that end, it is essential for clinicians to have a realistic appreciation of the scientific evidence underlying the relationships between FHR patterns and fetal oxygenation. Such relationships cannot be assumed to exist unless they have been subjected to analytic study with appropriate control of confounding factors. JANUARY 2012 CONTEMPORARY OB/GYN 17 FETAL MONITORING MYTHBUSTERS Planning Workshop. Am J Obstet Gynecol. 1997;177(6):1385-1390. 2. Macones GA, Hankins GD, Spong CY, Hauth J, Moore T. The 2008 National Institute of Child Health and Human Development workshop report on electronic fetal monitoring: update on definitions, interpretation, and research guidelines. Obstet Gynecol. 2008;112(3): 661-666. 3. American College of Obstetricians and Gynecologists. ACOG Practice Bulletin No. 106: Intrapartum fetal heart rate monitoring: nomenclature, interpretation, and general management principles. (Replaces Practice Bulletin No. 70, December 2005). Obstet Gynecol. 2009;114(1):192-202. 4. Feinstein N, Torgerson KL, Atterbury J; Association of Women’s Health, Obstetric, and Neonatal Nurses. Fetal Heart Monitoring: Principles and Practices. 3rd ed. Dubuque, IA: Kendall/Hunt Publishing Co; 2003. 5. American College of Nurse-Midwives. Position Statement: Standardized Nomenclature for Electronic Fetal Monitoring. Silver Spring, MD: American College of Nurse-Midwives; 2006. 6. Gültekin-Zootzmann B. The history of monitoring the human fetus. J Perinat Med. 1975;3(3):135-144. 7. Hon EH. The classification of fetal heart rate. I. A working classification. Obstet Gynecol. 1963:22(2); 137-146. 8. Kubli FW, Hon EH, Khazin AF, Takemura H. Observations on heart rate and pH in the human fetus during labor. Am J Obstet Gynecol. 1969;104(8): 1190-1206. 9. Caldeyro-Barcia R, Mendez-Bauer C, Poseiro JJ, Pose SV. Fetal monitoring in labor. In: Wallace HM, Gold EM, Lis EF, eds. Maternal and Child Health Practices: Problems, Resources, and Methods of Delivery. Springfield, IL: Charles C. Thomas, Publisher; 1973:332-394. 10. Krebs HB, Petres RE, Dunn LJ. Intrapartum fetal heart rate monitoring. VIII. Atypical variable decelerations. Am J Obstet Gynecol. 1983;145(3): 297-305. 11. Özden S, Demirci F. Significance for fetal outcome of poor prognostic features in fetal heart rate traces with variable decelerations. Arch Gynecol Obstet. 1999;262(3-4):141-149. 12. Kazandi M, Sendag F, Akercan F, Terek MC, Gundem G. Different types of variable decelerations and their effects to neonatal outcome. Singapore Med J. 2003;44(5):243-247. 13. Agency for Healthcare Research and Quality. U.S. Preventive Services Task Force Procedure Manual. Rockville, MD: Agency for Healthcare Research and Quality; 2008. AHRQ Publication No. 08-05118-EF. http:// www.uspreventiveservicestaskforce.org/uspstf08/methods/procmanual.htm. Accessed December 12, 2011. 14. Hamilton E, Warrick P, O’Keeffe D. Variable decelerations: do size and shape matter? J Matern Fetal Neonatal Med. August 1, 2011. (Epub ahead of print.) 15. MacLennan A. A template for defining a causal relation between acute intrapartum events and cerebral palsy: international consensus statement. BMJ.1999;319(7216):1054-1059. 16. American College of Obstetricians and Gynecologists. Neonatal Encephalopathy and Cerebral Palsy: Defining the Pathogenesis and Pathophysiology. Washington, DC: American College of Obstetricians and Gynecologists; 2003. 17. Shields JR, Schifrin BS. Perinatal antecedents of cerebral palsy. Obstet Gynecol.1988;71(6 Part 1):899-905. 18. Westgate JA, Bennet L, de Haan HH, Gunn AJ. Fetal heart rate overshoot during repeated umbilical cord occlusion in sheep. Obstet Gynecol. 2001;97(3):454-459. 19. Goodlin RC, Lowe EW. A functional umbilical cord occlusion heart rate pattern. The significance of overshoot. Obstet Gynecol. 1974;43(1):22-30. Level of evidence supporting an independent relationship between “atypical” features of variable decelerations and newborn outcome in the form of low 5-minute Apgar scores or metabolic acidemia. FIGURE In the case of atypical variable decelerations, this requirement has not been met. Scientific evidence regarding the predictive value of “atypical” features of variable decelerations is summarized in the Figure. The lack of Level I or Level II evidence supporting an independent link between atypical variable decelerations and adverse newborn outcome is underscored by the 2008 NICHD recommendation that such features require further investigation to establish clinical significance.2 In the absence of such evidence, the most reasonable approach is to avoid assigning undue clinical significance to atypical variable decelerations. The Fetal Monitoring Mythbusters series will continue in 2 months with a detailed examination of the scientific evidence underlying the classification of decelerations as “mild,” “moderate,” or “severe.” DR. MILLER is professor of clinical obstetrics, gynecology, and pediatrics in the Division of Maternal-Fetal Medicine, Keck School of Medicine, University of Southern California, and in the department of pediatrics, Children’s Hospital Los Angeles. He is a consultant for Clinical Computer Systems and is in partnership with GE Healthcare to promote multidisciplinary fetal monitoring education. REFERENCES 1. Electronic fetal heart rate monitoring: research guidelines for interpretation. National Institute of Child Health and Human Development Research 18 CONTEMPORARYOBGYN.NET JANUARY 2012 It All Comes Down to ONE ONE SCOPE. EVERY DIRECTION. ONE ENERGY SOURCE. INFINITE OPTIONS. ONE PORT SYSTEM. MULTIPLE INSTRUMENTS. ONE VISUALIZATION PLATFORM. ANY PROCEDURE. The first deflectable-tip technology brings triangulation inside the patient. Newly engineered ports will revolutionize access by allowing more instruments and greater flexibility. Versatile ultrasonic and advanced bipolar solutions including the new, ergonomically designed HALO™ PKS™ Cutting Forceps. A single video platform that’s compatible with any Olympus scope, rigid or flexible. TOGETHER WE CAN DO LESS LAPARO-ENDOSCOPIC SINGLE SITE (LESS) SURGERY For more information, visit olympusamerica.com/LESS or call 888-524-7266 © 2011 Gyrus ACMI, Inc. AD618-0811 GRAND ROUNDS Postpartum contraception Ways to avoid VTE Postpartum contraception is an essential consideration for new mothers. Providers and patients should discuss the relative advantages and disadvantages of each method, intentions about breastfeeding, risk of VTE, and timing of implementation. By amy J. VoeDIScH, mD, mS; paUL D. bLUmentHaL, mD, mpH P For a thorough review of the current array of contraceptive options available, visit contemporaryobgyn.net/ contracept 20 contemporaryobgyn.net January 2012 take-home messages ◾ Postpartum contraception should be discussed and planned during the antenatal period and implemented before the 6-week postpartum visit to prevent unintended pregnancy. ◾ Considerations include the impact on lactation, infant growth and development, and risk of VTE. The definitive contraceptive plan should be determined after delivery and before discharge if it was not decided during antenatal care. Indeed, the majority of women will initiate sexual intercourse before the 6-week postpartum visit, and the earliest reported ovulation occurs at 25 days postpartum in nonbreastfeeding women.1-3 Terefore, contraception should be initiated before the conventional 6-week followup visit to prevent unintended pregnancy. Some authorities have even suggested that the PHOTODISC/SPIkE MAFFORD/GETTy IMAGES ostpartum contraception is essential for any new mother wishing to space pregnancies or limit family size, but it is ofen confusing for the provider and patient to navigate the evolving recommendations for the best method of postpartum birth control. The World Health Organization (WHO) and the United States Centers for Disease Control and Prevention (CDC) have published guidelines on contraception in the postpartum period that can assist in choosing the right plan for your patient. The CDC guidelines, which are more recent than the WHO document and more familiar to clinicians, will be referenced in this discussion. Choosing or planning a method of postpartum contraception ideally should be done during the antenatal period to allow adequate time for discussion about the various options available. Antenatal counseling is also necessary to obtain consent for those options, such as tubal ligation, that require a decision before the admission to labor and delivery. ILLUSTRATIOn FOR COntEMpOrary Ob/Gyn By 3Fx, 3D LIFE SCIEnCE AnIMATIOn AnD EFFECTS Under conditions of stasis, hypercoagulability and/or endothelial injury, deep vein thrombosis may occur in the veins of the leg, such as the femoral or popliteal veins. this can result in Vte, a risk that may be further exacerbated by the use of certain postpartum contraceptives. postpartum visit should occur at 3 weeks afer delivery to ensure that contraceptive needs are met.1 Further advantages of moving the postpartum visit include earlier screening for depression and lactational issues. Among the many considerations when deciding on an appropriate method of postpartum contraception are the impact of the contraceptive on breastfeeding and the risk of postpartum venous thromboembolism (VTE). Tese two issues have influenced the recommendations of the CDC. Whether or not a woman chooses to breastfeed, and for what period of time, will largely determine the contraceptive options available to her. Te evidence surrounding the impact of various methods on lactation and infant growth has been conflicting. Recent systematic reviews may provide insight on how to counsel patients, as discussed below. Given the well-known maternal and infant benefits of breastfeeding, patients should be encouraged to breastfeed if possible and to choose a contraceptive that meets their contraceptive and lactational goals. The ma in clinica l concern about contraception for puerperal women is the risk of VTE. One recent review reported that the risk of VTE during the flrst 6 weeks postpartum ranges from 25 to 99 per 10,000 woman-years, which represents a 22- to 84fold increase compared with controls. 4 Risk of VTE may be further increased by delivery complications, anemia, inherited January 2012 contemporary ob/gyn 21 POSTPARTUM CONTRACEPTION POWER POINTS The main clinical concern about contraception for puerperal women is the risk of VTE. A plan for postpartum contraception should be decided upon before discharge. thrombophilias, cesarean delivery, smoking, obesity, age greater than 35 years, infection, preeclampsia, and transfusion.4-7 Fortunately, this risk declines rapidly in the frst 21 days postpartum and returns to near baseline by 42 days aTer delivery4 (Figure 1). For nonlactating women, VTE risk is the prominent issue when deciding on a contraceptive method because the potential impact on lactation is not a consideration. Furthermore, nonlactating women will return to fertility sooner than their breastfeeding counterparts and, as stated previously, they may start ovulating as soon as 25 days aTer delivery. Therefore, their need for contraception is potentially more critical before the 6-week postpartum visit, and a plan should be decided upon before discharge. This article describes the contraceptive options available to lactating and nonlactating women, taking into account the impact of the method on lactation and VTE risk and citing the recommendations in the CDC guidelines. Lactational amenorrhea The lactational amenorrhea method pertains to those women who are exclusively breastfeeding, have not resumed menstrual bleeding, and are within 6 months of delivery.8,9 Using this defnition, the contraceptive efficacy of lactational amenorrhea is 98%.10 However, once women resume menstrual bleeding, start supplemental feedings, and/or reach 6 months postpartum, they must start a new method of contraception if they do not desire pregnancy. If a woman leaves the hospital intending to use lactational amenorrhea as her method of contraception, she should be counseled about backup methods such as condoms or emergency contraception to use in the event of resumption of menses, supplemental feedings for the infant, or reaching more than 6 months postpartum. According to one US study, 8% of women who planned to breastfeed never actually started to do so upon discharge from the hospital, and another 23.5% stopped breastfeeding before the 6-week postpartum visit, putting them at risk for an unintended pregnancy.11 It should also be noted that an increasing number of women in the US are not only 22 contemporaryobgyn.net January 2012 breastfeeding, but are also pumping breast milk for various reasons, such as having to return to work. This raises the question as to whether pumping has the same physiologic effect on ovulation and amenorrhea as exclusive breastfeeding. There are no data specifcally addressing this issue. In the only study to directly compare maternal oxytocin and prolactin levels between various pumping methods and a breastfeeding group, no difference was found in oxytocin levels.12 Prolactin levels were similar between the electric pulsatile pump and breastfeeding groups, whereas women using manual, battery, or mechanical methods had lower prolactin responses.12 These diflerences were of uncertain clinical importance and shed no light on any diflerence between pumping and breastfeeding with respect to contraceptive eflect. Combined hormonal contraception Combined hormonal contraception (CHC), which contains both estrogen and a progestin, is the most commonly used form of reversible contraception in the US and a frequent choice among new mothers.13,14 However, for lactating mothers, there is considerable debate regarding the eflect of the hormones on the quality and quantity of breast milk, infant growth and development, and other direct eflects on the infant of hormones secreted in breast milk. Previous studies of milk composition among women taking oral contraceptives have been largely inconsistent, with some studies showing an increase, others a decrease, and still others showing no change in the protein content. Studies in general have shown no changes in lactose, fat, or energy concentrations.15,16 A Cochrane Review from 2003 did not demonstrate a consistent effect of hormonal contraception on milk quality or quantity and was unable to make recommendations about the use of hormonal contraception in breastfeeding women.17 A recent systematic review focused on the duration of breastfeeding, use of supplemental feedings, and infant weight gain and growth. Kapp and Curtis attempted to answer lingering concerns about the eflects of CHC, especially oral contraceptives, on these parameters.14 The authors determined that POSTPARTUM CONTRACEPTION Figure 1 Venous thromboembolism events by week postpartum according to 3 studies. Incidence rate of VTE events (per 10,000 WY) 400 Heit et al. 2005 350 300 250 200 150 100 50 0 1 2 3 4 Postpartum week 5 6 Percentage of VTE events occuring each week 45 Pomp et al. 2008 40 35 30 25 20 15 10 5 0 1 2 3 4 5/6 Incidence proportion of VTE events (per 1000 deliveries) Postpartum week* 0.16 Jacobsen et al. 2008 0.14 0.12 0.10 0.08 0.06 0.04 0.02 0 1 2 3 4 5 6 Postpartum week Vte events by week postpartum for three studies reporting weekly data: Heit et al, 34 pomp et al,35 and Jacobsen et al.39 In all studies, events decline markedly between postpartum Weeks 2 and 4 *Data for Weeks 5 and 6 are presented together. reprinted with permission from Elsevier (http://www.sciencedirect.com/science/journal/00493848). January 2012 contemporary ob/gyn 23 POSTPARTUM CONTRACEPTION Table 1 Maternal condition postpartum CHC POP DMPA Implant <1 month 3 2 2 2 >1 month 2 1 1 1 <21 days 3 1 1 1 ≥21 days 1 1 1 1 IUS IUD Breastfeeding Not breastfeeding Postpartum (in breastfeeding or nonbreastfeeding, including post-cesarean delivery) <10 minutes after delivery of placenta 2 1 >10 minutes to <4 weeks 2 2 ≥4 weeks 1 1 Puerperal sepsis 4 4 Abbreviations: CHC, combined hormonal contraception; POP, progestinonly contraception; DMPA, depot medroxyprogesterone acetate; IUS, levonorgestrel-releasing intrauterine system; IUD, copper-containing intrauterine device. *Category 1: a condition for which there is no restriction on the use of the contraceptive method. Category 2: a condition for which the advantages of using the method generally outweigh the theoretical or proven risks. Category 3: a condition for which the theoretical or proven risks usually outweigh the advantages of using the method. Category 4: represents an unacceptable health risk if the contraceptive method is used. Centers for Disease Control and Prevention.19 the available data were limited and pertained to outdated formulations of hormones with higher doses of estrogen. Furthermore, most of the studies were considered to have poor methodologic quality and showed an inconsistent effect of CHC on breastfeeding success and duration. In the longest observational follow-up study (8 years), infants exposed to hormonal contraceptives in breast milk did not show any differences in growth, health, or school performance.18 Infants in the exposed group of this study were breastfed for 1 month less than the controls, but that was the only difference between the groups. In addition, the Cochrane Review from 2003 did not show a significant diference in infant growth or weight as a result of hormonal contraceptive use during lactation.17 In light of this evidence, the CDC now recommends waiting 4 weeks before the initiation of CHC in breastfeeding women (Table 1).19 This concurs with the American College of Obstetricians and Gynecologists 24 contemporaryobgyn.net January 2012 (ACOG), which also recommends delaying initiation of CHC until at least 4 weeks postpartum and only if lactation is well established. Women who desire to both breastfeed and use CHC can be advised to use condoms until they are at least 4 weeks postpartum, lactation has been well established, and they have started their new method of contraception. If women are concerned about CHC and lactation, they should be counseled that CHC and lactation are not mutually exclusive and can be used successfully together.20 CHC does affect the hemostatic system to increase a woman’s risk of VTE in the postpartum period, although no studies have directly assessed the risk of VTE in postpartum women using contraceptives.4 In nonbreastfeeding women without additional concerns about the impact of CHC on lactation, the CDC recommends delaying the initiation of any type of CHC, including oral, patch, and ring, until at least 21 days postpartum.19 By that time, the elevated postpartum risk is much reduced, and these women have levels of VTE risk similar to those of their nonpregnant counterparts using CHC.4 Progestin-only contraception Progestin-only contraception (POC) has long been accepted as an alternative to CHC for lactating mothers and is often initiated before discharge from the hospital. Progestinonly contraceptives do not interfere with or potentiate hypercoagulability during the postpartum period and are safe to use from a hematologic perspective immediately after delivery in both lactating and nonbreastfeeding women.21 However, there have been concerns regarding the potential impact of POC on breastfeeding and on infant growth and development.22 A recent systematic review of progestinonly methods among breastfeeding women helped to clarify these concerns. It analyzed studies on oral, injectable, implantable, and hormonal intrauterine devices (IUDs) and found that these methods do not compromise a woman’s ability to breastfeed, in terms of either initiation or duration. 22 It also demonstrated that POC does not adversely POSTPARTUM CONTRACEPTION afect infant growth or development during at least the Trst year of life. The optimal time to start POC remains unresolved because of these persistent, mainly theoretical concerns about its impact on lactation and infant growth and development. Manufacturing inserts on progestin-only contraceptives generally recommend waiting to begin using them until 6 weeks postpartum. However, the CDC classifies POC initiation at less than 4 weeks in breastfeeding women as category 2 (Table 1), meaning that the advantages of use generally outweigh the theoretical risks.19 nonpregnant population. The exception is the use of the copper-containing IUD, which is generally discouraged between discharge from the hospital and 4 weeks postpartum. Given the low likelihood of ovulation before 4 weeks, its use is not likely to be necessary during this period. Sterilization Emergency contraception Sterilization has no impact on lactation or VTE risk and can be performed safely postpartum. Most postpartum sterilization procedures are performed in the Trst 48 hours after delivery. The most common method used in the US is partial salpingectomy, including the Pomeroy technique. 26, 27 However, studies also have shown the Filshie clip to be efective and easy to use.28-30 One recent systematic review suggested lower overall eflcacy with the Filshie clip than with the Pomeroy method,31 but another literature review found no statistically significant difference. 32 Appropriate patient selection and careful attention to technical detail are likely to be important to reduce failures of postpartum tubal sterilization, particularly for Filshie clip procedures.31 No discussion of postpartum sterilization techniques would be complete without mention of vasectomy. The postpartum period, commonly associated with abstinence by the woman for the Trst few weeks afier delivery, is an opportune time for her male partner to undergo a vasectomy procedure. Vasectomies are quick and easily performed, are highly effective, carry less overall risk and expense than female sterilization, and clearly have no implications with respect to lactation or VTE risks. The two most common vasectomy techniques are the conventional incisional approach and the no-scalpel method. According to a recent Cochrane Review comparing these approaches, the no-scalpel method resulted in less bleeding, hematoma formation, infection, and pain and had a shorter operating time.33 There was no difference in efectiveness between the methods. All types of emergency contraception can be used as needed in the postpartum period without concern about the effect on lactation or VTE risk, the same as in the Barrier methods are safe for lactating mothers and don’t afect the risk of VTE. Diaphragms Levonorgestrel-releasing intrauterine system The levonorgestrel-releasing intrauterine system (IUS) contains 52 mg of levonorgestrel and releases 20 mcg of hormone daily into the endometrial environment with minimal systemic absorption. The IUS has no appreciable effect on VTE risk.23 There are, however, theoretical concerns regarding the potential impact of the small amount of absorbed progestin on lactation. A recent randomized controlled trial showed no diferences in breastfeeding duration or infant growth and development between the IUS and the copper-containing IUD.24 The CDC19 and ACOG25 consider the immediate postpartum placement of the IUS acceptable regardless of breastfeeding status (Table 1). This is described in more detail below. Copper-containing intrauterine device The copper-containing IUD has the advantage of being nonhormonal with no potential or theoretical impact on lactation, making it an excellent choice for postpartum mothers who want to avoid all hormonal methods of contraception. This IUD also has no efect on VTE risk and may be initiated immediately postpartum, as described below. 23 POWER POINTS Women planning to use the lactational amenorrhea method should be counseled about backup methods. The CDC recommends that breastfeeding women wait 4 weeks before starting combined hormonal contraceptive use. Barrier methods January 2012 contemporary ob/gyn 25 POSTPARTUM CONTRACEPTION and cervical caps should be fitted at 4 to 6 weeks postpartum afer the cervix and vagina have returned to their nonpregnant state. If a woman used either method before her pregnancy, she should be reTtted afer delivery to ensure that she is using the appropriate size of device. Male and female condoms can be used once a woman resumes sexual intercourse. POWER POINTS Progestin-only contraception should not be started before 6 weeks postpartum. The coppercontaining IUD is an option for women who want to avoid hormonal birth control. Barrier methods should be fitted at 4 to 6 weeks postpartum. 26 inserted within 48 hours are referred to as “immediate postpartum” insertions, or sometimes as “morning after delivery” IUD insertions (Table 2). This distinction is important because older studies of PPIUDs reported a higher rate of expulsion compared with interval insertions, which had an expulsion rate of approximately 3% to 5%.36-38 PPIUD expulsion rates appear to be dependent Immediate postpartum or on the timing of the insertion and skill of the provider in ensuring that the IUD is placed as postplacental insertion high as possible in the fundus.39 of intrauterine contraception Postpartum placement of an intrauterine device An epidemiologic study indicated that (PPIUD) refers to insertion of the device afer insertion of a PPIUD within 10 minutes afer delivery and before discharge from the hospital. delivery of the placenta resulted in an expulsion Similar to interval IUDs, PPIUDs are safe rate of 9.5%, whereas those inserted between 2 and effective. 34,35 This approach optimizes and 72 hours afer delivery had expulsion rates the cost-effective use of healthcare services as high as 29% to 37%.39 However, regardless during delivery and eliminates the need for a of timing, the most important determinant separate postpartum visit to initiate a family of PPIUD retention is proper placement. As planning method. Furthermore, the PPIUD is mentioned previously, the IUD must be placed a long-term method of contraception that has at the fundus of the uterus to reduce the risk of no adverse effect on breastfeeding. flerefore, expulsion. flis may explain why insertions 2 if a patient is a candidate for an IUD and is to 72 hours afer delivery had higher expulsion appropriately counseled during prenatal care, rates; the uterine fundus may be more early labor, or early in the postpartum period, dificult to reach because of contraction of the she may have it inserted before discharge lower uterine segment, thus making proper from the hospital regardless of her lactation placement of the IUD less likely. intentions. fle importance of proper fundal placement Because insurance and Medicaid coverage may also explain why insertions at cesarean of PPIUD placement varies, providers deliveries have lower expected expulsion rates considering this form of contraception for than insertions after vaginal deliveries. In a their patients are advised to consult applicable review of more than 3,000 insertions at the state and institutional regulations. time of cesarean delivery, the expulsion rate at IUDs inser ted w it hin 10 minutes 1 year was 5.5% for cesarean insertion versus after delivery of the placenta are termed 24.5% for vaginal insertion.40 “postplacental” insertions, whereas those Provider experience also affects the rate of expulsion, most likely as a function of proper IUD placement. In Table 2 Comparison of postpartum and interval a study by Chi et al, providers intrauterine device insertions with experience in vaginal PPIUD insertion had a 6.9% Morning-after- Postplacental Interval Post-cesarean delivery IUD expulsion rate at 6 months, whereas inex perienced Timing ≥6 weeks ≤48 hours after ≤10 minutes After delivery of the of insertion postpartum delivery after delivery of placenta and before providers had a 12.0% rate of placenta hysterotomy closure expulsion.39 To further address Expulsion risk 3% ≤30%* <10% 5.5% the expulsion risk, it is possible Follow-up 4-6 weeks 4-6 weeks after 4-6 weeks after 4-6 weeks after to review the experience with after insertion insertion insertion insertion IUD placement at the time Abbreviation: IUD, intrauterine device of second-trimester surgical * The rate is significantly less for experienced providers and may be comparable to that of postplacental placement in current, ongoing studies. abortions. The condition of contemporaryobgyn.net January 2012 POSTPARTUM CONTRACEPTION the uterus after a second-trimester dilation and evacuation procedure is similar to that of a uterus at 24 to 48 hours afer delivery. A recent randomized controlled trial evaluating IUD expulsion rates after second-trimester dilation and evacuation procedures did not Tnd a signiTcant difference in rates between immediate insertion and delayed insertion (ie, 2 to 4 weeks afer the procedure).41 Both the levonorgestrel-releasing IUS and copper-containing IUD can be inserted as Table 3 Task Preinsertion Insertion Postinsertion PPIUDs, and the insertion technique is similar for both. See Table 3 and Figures 2-8 for a description of the insertion process. Although the ring forceps technique is described in detail, the levonorgestrel IUS may be inserted with the package inserter and the strings trimmed flush with the level of the external os afer placement. If the IUS inserter does not work properly for PPIUD placement, the IUS may be removed from its inserter and placed using the forceps technique described here. The CDC classifies both the levonorgestrel-releasing Overview of the postplacental and post-cesarean IUS and the copper IUD insertion of an intrauterine device as category 2 for PPIUD insertions (Table 1). A PPIUD Description should never be inserted Postplacental insertion technique in the setting of puerperal 1. Palpate the uterus to evaluate the height of the fundus. sepsis, and insertion should 2. Clean the external genital area with a clean cloth. be delayed until 4 weeks afer 3. Place a clean drape over the patient’s abdomen and underneath her buttocks. resolution of the infection.19 A consent form should 4. Insert a retractor into the vagina and visualize the cervix. 5. Prep the cervix and the vagina with antiseptic. be signed and a “time out” 6. Gently grasp the anterior lip of the cervix with ring forceps. (Do not use a performed before insertion of toothed tenaculum because it may tear the cervix). the PPIUD. 7. Grasp the IUD with ring forceps (Figures 3-4*). Follow-up for PPIUDs is 8. Exert gentle traction toward you on the cervix-holding forceps. 9. Insert the forceps holding the IUD through the cervix and into the lower similar to that for interval uterine cavity. Avoid touching the walls of the vagina with the IUD. IUD insertions. Women 10. Release the hand that is holding the cervix-holding forceps, and move the should return to the clinic 4 hand to the abdomen, placing it on top of the uterine fundus. 11. With the abdominal hand, stabilize the uterus with firm downward pressure to 6 weeks afer the insertion through the abdominal wall. Prevent the uterus from moving upward in the for a “string check ” and abdomen as the IUD is inserted. possible trimming. The 12. Move the IUD-holding forceps in an upward motion toward the fundus (in an angle toward the umbilicus) (Figure 5*). Note: The lower uterine segment strings may be longer after may be contracted, and slight pressure may be necessary to achieve fundal a PPIUD insertion because placement. 13. Feel the uterus through the abdominal wall, and confirm that the tips of the the uterus is returning to forceps reach the fundus. its nonpregnant size; as the 14. Open the forceps to release the IUD (Figure 6*). uterus contracts, the string in 15. Slowly remove the forceps from the uterine cavity, keeping it slightly open (Figures 7-8*). the vagina may lengthen Additionally, the strings 16. Examine the cervix for strings. Note: Sometimes when the uterus is well contracted or small, the copper-containing IUD strings can be seen through may not be present after a the cervix. The levonorgestrel IUS strings will be visualized at the cervix, and PPIUD insertion. In this case, the strings should be cut flush with the external os. 17. Remove the cervix-holding forceps from the anterior lip of the cervix. an ofice bedside ultrasound can be performed to conTrm Post-cesarean insertion technique the proper IUD positioning 1. Massage the uterus. within the uterus. 2. Remove any tissue left in the uterine cavity. 3. Place the IUD at the uterine fundus manually or with a grasping instrument. 4. Before suturing the uterine incision, place the strings in the lower uterine segment near the internal cervical os. Do not pass the strings through the cervix because this increases the risk of infection. Abbreviations: IUD, intrauterine device; IUS, intrauterine system. *Refer to the figures within this article for illustration of specific insertion stages. Adapted from the EngenderHealth provider and training manual. 28 contemporaryobgyn.net January 2012 Conclusion Postpartum contraception is an important consideration for a new mother, and her provider is responsible for POSTPARTUM CONTRACEPTION Figure 2 Instruments needed for postplacental insertion of an intrauterine device (PPIUD). necessary items include a vaginal retractor or valve or Sims speculum (for visualization of the cervix), sterile gloves, ring forceps to grasp the cervix, ring forceps to place the IUD, gauze, antiseptic solutions, and sterile drapes to cover the patient. adapted with permission from the acQUIre project. 2008. The postpartum intrauterine device: A training course for service providers. Participant handbook. new york: engenderHealth. assisting her in choosing the right method for her and her family. Whether a woman is breastfeeding or not determines the degree to which she qualifes for certain contraceptive options, the objective being a balance between her desire to breastfeed and her need for an effective family planning method. Mothers who do not breastfeed have a slightly wider range of contraceptive options available to them. Although expulsion rates are higher than for interval insertions, the postplacental or immediate postpartum insertion of IUDs represents a cost-effective option that should be oTered to all women, regardless of breastfeeding status. DR. VOEDISCH is a clinical instructor in obstetrics and gynecology, Stanford University School of Medicine, Palo Alto, California. DR. BLUMENTHAL is professor of obstetrics and gynecology and director of the Ambulatory Care and the Family Planning Services and Research programs of the Department of Obstetrics and Gynecology and director of the International Reproductive Education and Services (SPIRES) program, Stanford University School of Medicine in Palo Alto. Dr. Voedisch reports no conflicts of interest with the content of this article; Dr. Blumenthal reports that he has received a salary or honoraria from Merck. Figure 3 Grasping the intrauterine device within the packing to maintain sterile technique. adapted with permission from the acQUIre project. 2008. The postpartum intrauterine device: A training course for service providers. Participant handbook. new york: engenderHealth. Figure 4 Proper placement of the intrauterine device (IUD) within the ring forceps. note the angle of the IUD to ensure that the strings do not get caught in the forceps when they are removed from the uterus after placement of the IUD at the fundus. adapted with permission from the acQUIre project. 2008. The postpartum intrauterine device: A training course for service providers. Participant handbook. new york: engenderHealth. RefeRences 1. Speroff L, Mishell DR Jr. The postpartum visit: it’s time for a change in order to optimally initiate contraception. Contraception. 2008;78(2):90-98. 2. Gray RH, Campbell OM, Zacur HA, Labbok MH, MacRae SL. Postpartum return of ovarian activity in nonbreastfeeding women monitored by urinary assays. J Clin Endocrinol Metab. 1987;64(4):645-650. 3. Jackson E, Glasier A. Return of ovulation and menses in postpartum nonlactating women: a systematic review. Obstet Gynecol. 2011;117(3):657-662. January 2012 contemporary ob/gyn 29 ILLUSTRATIOnS FOR COntEMpOrary Ob/Gyn By ALExAnDRA BAkER, DnA ILLUSTRATIOnS, InC. BASED On ORIGInAL ART By TRACy AnGULO AnD SARAH PRAGER, MD POSTPARTUM CONTRACEPTION FigureS 5-8 30 Technique for postpartum insertion of an intrauterine device. contemporaryobgyn.net January 2012 POSTPARTUM CONTRACEPTION 4. Jackson E. Controversies in postpartum contraception: when is it safe to start oral contraceptives after childbirth? thromb res. 2011;127(Suppl 3):S35-S39. 5. Heit JA, kobbervig CE, James AH, Petterson TM, Bailey kR, Melton LJ 3rd. Trends in the incidence of venous thromboembolism during pregnancy or postpartum: a 30-year population-based study. ann Intern Med. 2005;143(10):697-706. 6. Pomp ER, Lenselink AM, Rosendaal FR, Doggen CJ. Pregnancy, the postpartum period and prothrombotic defects: risk of venous thrombosis in the MEGA study. J thromb Haemost. 2008;6(4):632-637. 7. Jacobsen AF, Skjeldestad FE, Sandset PM. Ante- and postnatal risk factors of venous thrombosis: a hospital-based case-control study. J thromb Haemost. 2008;6(6):905-912. 8. kennedy kI, Trussell J. Postpartum contraception and lactation. In: Hatcher RA, Trussell J, nelson AL, Cates W Jr, Stewart FH, kowal D, eds. Contraceptive technology. 19th ed. new york, new york: Ardent Media, Inc; 2007:403-431. 9. Diaz S, Croxatto HB. Contraception in lactating women. Curr Opin Obstet Gynecol. 1993;5(6):815-822. 10. kennedy kI, Rivera R, Mcneilly AS. Consensus statement on the use of breastfeeding as a family planning method. Contraception. 1989;39(5):477-496. 11. Halderman LD, nelson AL. Impact of early postpartum administration of progestin-only hormonal contraceptives compared with nonhormonal contraceptives on short-term breast-feeding patterns. am J Obstet Gynecol. 2002; 186(6):1250-1256. 12. Zinaman MJ, Hughes V, Queenan JT, Labbok MH, Albertson B. Acute prolactin and oxytocin responses and milk yield to infant suckling and artificial methods of expression in lactating women. pediatrics. 1992;89(3): 437-440. 13. Mosher WD, Martinez GM, Chandra A, Abma JC, Willson SJ. Use of contraception and use of family planning services in the United States: 1982-2002. adv Data. 2004;350:1-36. 14. kapp n, Curtis kM. Combined oral contraceptive use among breastfeeding women: a systematic review. Contraception. 2010;82(1):10-16. 15. Hull VJ. The effects of hormonal contraceptives on lactation: current findings, methodological considerations, and future priorities. Stud Fam plann. 1981;12(4):134-155. 16. Costa TH, Dorea JG. Concentration of fat, protein, lactose and energy in milk of mothers using hormonal contraceptives. ann trop paediatr. 1992;12(2):203-209. 17. Truitt ST, Fraser AB, Grimes DA, Gallo MF, Schulz kF. Combined hormonal versus nonhormonal versus progestinonly contraception in lactation. Cochrane Database Syst rev. 2003;(2):CD003988. 18. nilsson S, Mellbin T, Hofvander y, Sundelin C, Valentin J, nygren kG. Long-term follow-up of children breast-fed by mothers using oral contraceptives. Contraception. 1986;34(5):443-457. 19. Centers for Disease Control and Prevention (CDC). U.S. medical eligibility criteria for contraceptive use, 2010. MMWr recomm rep. 2010;59(RR-4):1-86. 20. ACOG Committee on Practice Bulletins-Gynecology. ACOG practice bulletin. no. 73: Use of hormonal contraception in women with coexisting medical conditions. Obstet Gynecol. 2006;107(6):1453-1472. 21. Gomes MP, Deitcher SR. Risk of venous thromboembolic disease associated with hormonal contraceptives and hormone replacement therapy: a clinical review. arch Intern Med. 2004;164(18):1965-1976. 22. kapp n, Curtis k, nanda k. Progestogen-only contraceptive use among breastfeeding women: a systematic review. Contraception. 2010;82(1):17-37. 23. van Vliet HA, Tchaikovski Sn, Rosendaal FR, Rosing J, Helmerhorst FM. The effect of the levonorgestrel-releasing intrauterine system on the resistance to activated protein C (APC). thromb Haemost. 2009;101(4):691-695. 24. Shaamash AH, Sayed GH, Hussien MM, Shaaban MM. A comparative study of the levonorgestrel-releasing intrauterine system Mirena® versus the Copper T380A intrauterine device during lactation: breast-feeding performance, infant growth and infant development. Contraception. 2005;72(5):346-351. 25. American College of Obstetricians and Gynecologists. ACOG practice bulletin no. 121: Long-acting reversible contraception: implants and intrauterine devices. Obstet Gynecol. 2011;118(1):184-196. 26. Peterson HB, xia Z, Hughes JM, Wilcox LS, Tylor LR, Trussell J. The risk of pregnancy after tubal sterilization: findings from the U.S. Collaborative Review of Sterilization. am J Obstet Gynecol. 1996;174(4):1161-1168. 27. Peterson HB. Sterilization. Obstet Gynecol. 2008;111(1): 189-203. Review. Erratum in: Obstet Gynecol. 2011; 117(4):989. 28. kohaut BA, Musselman BL, Sanchez-Ramos L, kaunitz AM. Randomized trial to compare perioperative outcomes of Filshie clip vs. Pomeroy technique for postpartum and intraoperative cesarean tubal sterilization: a pilot study. Contraception. 2004;69(4):267-270. 29. Penfield AJ. The Filshie clip for female sterilization: a review of world experience. am J Obstet Gynecol. 2000;182(3):485-489. 30. yan JS, Hsu J, yin CS. Comparative study of Filshie clip and Pomeroy method for postpartum sterilization. Int J Gynaecol Obstet. 1990;33(3):263-267. 31. Rodriguez MI, Edelman AB, kapp n. Postpartum sterilization with the titanium clip: a systematic review. Obstet Gynecol. 2011;118(1):143-147. 32. Madari S, Varma R, Gupta J. A comparison of the modified Pomeroy tubal ligation and Filshie clips for immediate postpartum sterilisation: a systematic review. Eur J Contracept reprod Health Care. 2011;16(5):341-349. 33. Cook LA, Pun A, van Vliet H, Gallo MF, Lopez LM. Scalpel versus no-scalpel incision for vasectomy. Cochrane Database Syst rev. 2007;(2):CD004112. 34. Grimes D, Schulz k, Van Vliet H, Stanwood n. Immediate post-partum insertion of intrauterine devices. Cochrane Database Syst rev. 2003;(1):CD003036. 35. kapp n, Curtis kM. Intrauterine device insertion during the postpartum period: a systematic review. Contraception. 2009;80(4):327-336. 36. Grimes DA. Intrauterine devices (IUDs). In: Hatcher RA, Trussell J, nelson AL, Cates W Jr, Stewart FH, kowal D, eds. Contraceptive technology. 19th ed. new york, new york: Ardent Media, Inc; 2007:117-144. 37. Zhang J, Feldblum PJ, Chi IC, Farr MG. Risk factors for copper T IUD expulsion: an epidemiologic analysis. Contraception. 1992;46(5):427-433. 38. Mansour D. Copper IUD and LnG IUS compared with tubal occlusion. Contraception. 2007;75(6 Suppl): S144-S151. 39. Chi IC, Wilkens L, Rogers S. Expulsions in immediate postpartum insertions of Lippes Loop D and Copper T IUDs and their counterpart Delta devices--an epidemiological analysis. Contraception. 1985;32(2):119-134. 40. xu Jx, Connell C, Chi IC. Immediate postpartum intrauterine device insertion--a report on the Chinese experience. adv Contracept. 1992;8(4):281-290. 41. Cremer M, Bullard kA, Mosley RM, et al. Immediate vs. delayed post-abortal copper T 380A IUD insertion in cases over 12 weeks of gestation. Contraception. 2011;83(6):522-527. January 2012 contemporary ob/gyn 31 MIDURETHRAL SLINGS Keys to success with midurethral slings Open or laparoscopic Burch? Retropubic tension-free transvaginal or transobturator tape? Single-incision slings? When and for whom is each method most effective? BY mary t. mcLennan, mD ith Ulmsten’s introduction of the midurethral sling in 19961 and the procedure’s subsequent refinement and redefinition, it would appear that treatment choices for a woman presenting with stress urinary incontinence (SUI) have narrowed considerably and that deciding which one to use would be easy. However, although the midurethral sling has excellent short-term success, questions remain: Are all midurethral slings created equal? Are they equally effective in all types of patients? Is there still a role for the Burch procedure? This article will review the success and complication rates of the various treatment options and the patient variables that may affect success or failure. For the purposes of this article, retropubic tension-free transvaginal tape, irrespective of brand, will be referred to as TVT and transobturator placement will be referred to as TOT. W For more information about surgical and nonsurgical treatment options for stress urinary incontinence, go to contemporaryobgyn.net/ continent 32 contemporaryobgyn.net January 2012 take-home messages ◾ The open Burch procedure is a viable surgical option for stress urinary incontinence, particularly in conjunction with sacrocolpoplexy or other abdominal surgery. ◾ Women with intrinsic sphincter deficiency, mixed incontinence, high body mass index, or advanced age require special consideration. The Burch procedure versus the retropubic sling Te open Burch remains a very successful surgery for stress incontinence (Figure 1). A 2009 Cochrane Review that included 46 trials and 4,738 women noted a cure rate of between 69% and 88%. At 5 years, the cure rate still hovered around 70%.2 Some research suggests that the procedure results in slightly higher objective measures of success when it is performed in an open fashion rather than laparoscopically.3 MIDURETHRAL SLINGS FIGURe 1 Burch procedure showing two periurethral sutures attached to Cooper’s ligament. Iliopectineal (Cooper’s) ligament with Burch sutures Inguinal ligament Elevation of vaginal wall Obturator neurovascular bundle Paravaginal sutures FIGURES 1-3 ILLUSTRATED FOR CONTEMPORARY OB/GYN BY ALEXANDRA BAKER, DNA ILLUSTRATIONS, INC. BASED ON ORIGINAL ART BY GEOFFREY W. CUNDIFF, MD FIGURe 2 TVT: The insert shows the retropubic location with reference to the bony landmarks. Currently, the major role for the Burch appears to be in conjunction with a sacrocolpopexy: Research has shown that it decreases the rate of postoperative stress incontinence.4 It also is appropriate for women with SUI undergoing other abdominal surgery. For women not requiring a laparotomy for other reasons, most practitioners have moved to the midurethral sling (Figure 2). Several meta-analyses have evaluated eficacy, complications, and reoperation rates. A Cochrane 2009 analysis of randomized controlled trials comparing TVT with the Burch method showed that, based on any deffnition of “cure,” the TVT resulted in higher success.5 Results revealed fewer perioperative complications, shorter operative times and hospital stay, less de novo urgency, and less voiding dysfunction with TVT; however, none of these was statistically signiffcant. Te January 2012 contemporary ob/gyn 33 MIDURETHRAL SLINGS FIGURe 3 POWER POINTS Performed at the time of other abdominal surgery, the open Burch procedure improves postsurgical urinary continence. Data indicate that TVT is superior to Burch in efficacy, with fewer postoperative complications. 34 TOT: The insert shows the transobturator location with reference to the bony landmarks. researchers also reported significantly more bladder perforations with TVT (6% versus 1%). A recent “short-version Cochrane Review” of 62 trials and 7,101 women confirmed the earlier findings.6 The largest and the best performed study, by Ward et al, reported objective (based on a negative 1-hour pad test) success rates at 2 years of 81% for TVT and 80% for colposuspension; however, only 25% of the TVT patients and 20% of the Burch patients reported no urine leakage.7 This is important for clinicians to understand because patients typically describe themselves as “not cured” or “unhappy” if they still experience leakage. Retropubic versus transobturator sling TOT was developed largely to minimize complications by avoiding the space of Retzius (Figure 3).8 In a meta-analysis of 12 randomized control trials comparing TOT and TVT, objective cure rates were comparable.9 A short Cochrane Review including 657 women noted no statistically significant difference in subjective or objective cure.6 The largest randomized multicenter trial in the US, which involved 298 women randomized to retropubic contemporaryobgyn.net January 2012 TVT and 299 women randomized to TOT, reported overall cure rates of 81% for TVT and 78% for TOT.10 Subjective cure rates of 62% for TVT and 56% for TOT were reported. Urinary retention was higher with TVT, at 2.7%. In contrast, neurologic symptoms were more common with TOT (9.4%), with 60% of these consisting of weakness in the upper leg. In a large published study from Norway, researchers prospectively analyzed 5,942 women (4,281 receiving TVT, 731 undergoing TVT obturator, and 373 receiving TOT). Follow-up at 8 months showed similar success rates, with 88% versus 80% versus 82%, respectively, achieving negative stress tests.11 Although short-term results for the procedures are similar, consideration must be given to long-term success. Most of the longer-term data available are for TVT. Two randomized controlled trials reported success at 5 years of 71% to 81%.12,13 Two descriptive studies followed women for 11.5 years; one reported 84% objective and 77% subjective cure,14 and the other reported 90% objective and 77% subjective success.15 It appears that the data on TVT at a range of 5 to 11.5 years are robust. Bio-Oil® is a skincare oil that helps improve the appearance of scars, stretch marks and uneven skin tone. It contains natural oils, vitamins and the breakthrough ingredient PurCellin Oil™. For comprehensive product information and results of clinical trials, please visit bio-oil.com. Bio-Oil is the No.1 selling scar and stretch mark product in 11 countries. $11.99 (2fl.oz.). MIDURETHRAL SLINGS POWER POINTS However effective surgery is, patients may express dissatisfaction if they experience any leakage. Although TVT and TOT have comparable short-term efficacy, long-term results favor TVT. TOT is newer, so the data are sparse. One randomized control trial reported a success rate at 4 years of 69.5%.16 Another reported a success rate of 73% at 5 years.13 It appears likely that all traditional midurethral slings are efiective, but long-term effcacy data for the TOT sling are lacking. Complications for the procedures Complications associated with the various incontinence procedures may influence a surgeon’s choice of procedure. The types of complications that occur with TVT and TOT are similar, but they occur with varying incidence, with the exception of bowel and major vessel injuries, which are completely avoided by the transobturator route. 5 The complications of bladder perforation,11 hematoma, and voiding difficulty are signiTcantly less common with TOT.5,6 Despite this, it is diffcult to speciTcally recommend that women with borderline flow rates or evidence of obstructive voiding, or those with a previous retropubic procedure who are at a higher risk for bladder perforation, have a TOT based on this information because the randomized controlled trials did not seek to answer these questions. Vaginal erosions and pain in the thigh and/ or groin are signiTcantly more common with TOT.5 Current slings made of low molecular weight, macroporous polypropylene mesh may have lower rates of erosion than original studies indicate, given the inclusion of other types of mesh in some of those earlier studies. Single-incision slings Few data exist for single-incision slings. One randomized control trial looked at 90 women with SUI randomized to undergo either a TVT-O (Ethicon, Somerville, New Jersey), a TVT-Secur (Ethicon), or a Mini-Arc (American Medical Systems, Minnetonka, Minnesota).17 The success rate for the TVT-Secur was lowest at 67%, compared with 83% for the TVT-O and 87% for the Mini-Arc. In observational studies, objective success rates have ranged from 52% to 82%, which are generally lower than those reported for the TVT or the TOT.17-19 Few longterm data exist, but the longest study, which involved 45 women receiving TVT-Secur plus 36 contemporaryobgyn.net January 2012 Prolift (Ethicon) procedures, noted a success rate at Trst visit of 93%; this dropped to 54% at 6 months and to 40% at a range of 11 to 40 months.20 Reasons for the decrease in effcacy are not well understood at this time. The MiniArc may have better short-term success. Isolated reports of other single-incision sling procedures exist. As single-incision slings evolve, it may be prudent for clinicians to await more long-term effcacy data prior to widespread adoption, particularly given the high effcacy rates and favorable safety proTles of current standard midurethral slings. Special patient characteristics Intrinsic sphincter deficiency Intrinsic sphincter deficiency (ISD) (Table) has difierent deTnitions. It is most commonly deTned as either a maximal urethral closure pressure (MUCP) <20 cm and/or a leak point pressure (LPP) <60 cm of water. Observational studies of women with ISD generally have shown a lower success rate with TVT, with an average of 77%, compared with cure rates in those without ISD.21 Very little information exists on TOT for this group. Three studies involving a total of 228 women receiving the transobturator approach all showed a higher failure rate with TOT than with TVT. 22-24 Success rates hovered between 35% and 55%. Mixed incontinence C ou nsel i ng for women w it h mi xed incontinence is important because cure rates for all procedures generally are lower: between 67% to 85%.25-27 Surgical management still is an appropriate option, however, because medication for the overactive component will not cure stress incontinence, and approximately 50% to 60% of those treated with medicine will have persistent urge.28 In addition, evidence exists that a reasonable rate of resolution of detrusor overactivity and symptoms occurs after surgery in the range of 30% to 60%. 25,29 However, some evidence reveals lower rates of cure in women with mixed incontinence who are urge predominant (49%) rather than stress predominant (73%).30 Early evidence indicates that TOT may be the preferred procedure. Gamble et al in 2008 reported a persistence MIDURETHRAL SLINGS of urge symptoms in 53% of women who underwent TOT versus in 64% who underwent TVT31; 14% to 16% worsened with the retropubic approach versus 6% with TOT.32 Table Special patient characteristics potentially influencing choice of surgery Diagnosis Intrinsic sphincter deficiency (mobile) Preferred procedure Success Other considerations TVT 50% to 81% Higher failure for TOT Intrinsic sphincter Body mass index therapy recommended as deficiency TVT 17% to 77% Injectionfirst-line treatment Observational studies show (non-mobile) comparable rates of success— Slightly higher rates of resolution Mixed incontinence TOT 67% to 85% of OAB; lower rates of worsening in the range of 82% to 90%— OAB compared with TVT for women with higher body Either (no Success appears lower for BMI >35; mass index (BMI). However, BMI comparative data) 52% to 90% higher rate of urgency and OAB cure generally is slightly ISD is higher; higher rate of urgency Age TVT 70%+ lower w it h T V T when and OAB specific comparisons are Cure similar to sling alone; longer made bet ween dif ferent Concomitant pelvic Either (no time to voiding; one-third of patients surgery comparative data) 80% to 95% have cure of SUI with prolapsed BMI categories and normal surgery only 27,33 BMI. Hellberg et al reportHigher rates of ISD; higher failure Previous failed ed cure rates of 81% with a TVT 71% for TOT; higher rate of urgency sling and OAB BMI less than 30, 71% with Abbreviations: ISD, intrinsic sphincter deficiency; OAB, overactive bladder; SUI, stress urinary a BMI of 30 to 34, and 52% incontinence; TOT, transobturator; TVT, tension-free transvaginal tape for a BMI greater than 35 with Data: Richter HE, et al.10; Segal JL, et al21; Schierlitz L, et al24; Stav K, et al27; Gamble T, et al31; Botros SM, 34 the TVT. fiey also reported et al32; Rechberger T, et al33; Hellburg D, et al34; Groutz A, et al35; Stav K, et al37; Clemons JL, et al.40 greater urgency rates and detrusor overactivity but similar complication similar to those of the midurethral sling alone. rates. Little literature exists regarding TOT; A number of studies have reported that time however, Rechberger et al reviewed 268 TOT to resumption of normal voiding is longer procedures and did not ffnd obesity to be a risk when midurethral slings are performed at the factor for failure.33 fius, no current evidence time of prolapse surgery, so it’s important to exists to support one midurethral sling over set the patient’s expectations appropriately. another for obese women. Correction of prolapse may uncover occult stress incontinence in many cases; however, Age approximately one-third of women may Some evidence exists to support lower success be cured of their stress incontinence by the rates with increasing age.33,34 In a randomized prolapse surgery alone. 36 Decisions in this controlled trial of the retropubic approach setting are not always easy or clear. versus the TOT, Rechberger noted that for each increasing decade of life, midurethral Previous failure of midurethral sling slings had higher failure rates, with the TVT Very little information exists regarding what having slightly higher success to age 70.33 fie to do with women who already have failed one problem is that ISD increases with age, and type of midurethral sling. Stav et al reported this is typically not distinguished in studies. on 77 women with repeat slings versus 1,035 Overall, however, success rates are acceptable, receiving a primary procedure. 37 ISD was but may decrease aTer the age of 75 years to noted to be higher in the repeat group. Cure approximately 60% to 70%.34 De novo urge rate was higher when the repeat procedure incontinence also is more common.35 was TVT (71%) versus TOT (48%). De novo urgency and urge incontinence were greater in Concomitant pelvic surgery repeat procedures for both the TVT and TOT, Success rates for midurethral tape placed in with a range of 22% to 30% versus 5% to 14% conjunction with other repairs appear to be for primary procedures. Consider referring January 2012 POWER POINTS Women with intrinsic sphincter deficiency have a lower success rate with TVT. Cure rates are lower in women with mixed incontinence who are urge predominant. contemporary ob/gyn 37 MIDURETHRAL SLINGS complicated patients and those who have failed prior anti-incontinence procedures to a urogynecologist or a physician with specific expertise in the treatment of complicated incontinence. No discussion of the midurethral sling would be complete without mention of the October 2008 US Food and Drug Administration’s (FDA) press release regarding concerns about the use of transvaginal mesh. The FDA concluded at that time that physicians should require specialized training, should be aware of the risks, should be vigilant for potential adverse events, and should inform patients that complications may arise from the implantation of mesh.38 In July 2011, FDA issued another warning regarding mesh for prolapse repair and specifically excluded slings; however, our patients may equate mesh from sling procedures with the mesh from prolapse surgery procedures.39 Conclusions It appears from the information presented that TVT is more effective than the Burch method. Long-term results are available for TVT, and they appear to be robust. TOT appears to have similar efficacy in the short term; however, only one randomized control trial exists and it includes only 3 years of experience. TVT may be superior for women with ISD; however, most procedures have lower efficacy rates if the urethra is immobile. TOT may have some advantage for women with mixed incontinence in terms of greater resolution of their urgency symptoms. It is appropriate to offer a sling to women who are very obese (>35 BMI) but they may have a lower success rate. Te newest single-incision slings, at least on initial report, appear to have lower success rates for most patients. All of these procedures have similar complications, although rates vary. Te rates of bladder perforation and voiding dysfunction appear to be less for TOT; this may be a consideration for women who have undergone previous surgery or have preexisting voiding dysfunction. All of the procedures work well when combined with procedures for prolapse. The advent of the midurethral sling has improved the quality of life of many women, enabling them to have highly successful 38 contemporaryobgyn.net January 2012 surgeries with minimal morbidity and disruption to their lives. DR. MCLENNAN is professor of obstetrics, gynecology, and women’s health in the Department of Obstetrics, Gynecology, and Women’s Health, and director, Division of Urogynecology, Saint Louis University, Missouri. She reports that she has no conflicts of interest to disclose. RefeRences 1. Ulmsten U, Henriksson L, Johnson P, Varhos G. An ambulatory surgical procedure under local anesthesia for treatment of female urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct. 1996;7(2):81-85; discussion 85-86. 2. Lapitan MC, Cody JD, Grant A. Open retropubic colposuspension for urinary incontinence in women. Cochrane Database Syst Rev. 2009;(4):CD002912. 3. Dean NM, Ellis G, Wilson PD, Herbison GP. Laparoscopic colposuspension for urinary incontinence in women. Cochrane Database Syst Rev. 2006;3:CD002239. 4. Brubaker L, Cundiff GW, Fine P, et al; Pelvic Floor Disorders Network. Abdominal sacrocolpopexy with Burch colposuspension to reduce urinary stress incontinence. N Engl J Med. 2006;354(15):1557-1566. 5. Ogah J, Cody JD, Rogerson L. Minimally invasive synthetic suburethral sling operations for stress urinary incontinence in women. Cochrane Database Syst Rev. 2009;(4):CD006375. 6. Ogah J, Cody DJ, Rogerson L. Minimally invasive synthetic suburethral sling operations for stress urinary incontinence in women: a short version Cochrane review. Neurourol Urodyn. 2011;30(3):284-291. 7. Ward KL, Hilton P; UK and Ireland TVT Trial Group. A prospective multicenter randomized trial of tension-free vaginal tape and colposuspension for primary urodynamic stress incontinence: two-year follow-up. Am J Obstet Gynecol. 2004;190(2):324-331. 8. Novara G, Galfano A, Boscolo-Berto R, et al. Complication rates of tension-free midurethral slings in the treatment of female stress urinary incontinence: a systematic review and meta-analysis of randomized controlled trials comparing tension-free midurethral tapes to other surgical procedures and different devices. Eur Urol. 2008;53(2):288-308. 9. Latthe PM, Singh P, Foon R, Toozs-Hobson P. Two routes of transobturator tape procedures in stress urinary incontinence: a meta-analysis with direct and indirect comparison of randomized trials. BJU Int. 2010;106(1):68-76. 10. Richter HE, Albo ME, Zyczynski HM, et al; Urinary Incontinence Treatment Network. Retropubic versus transobturator midurethral slings for stress incontinence. N Engl J Med. 2010;362(22):2066-2076. 11. Dyrkorn OA, Kulseng-Hanssen S, Sandvik L. TVT compared with TVT-O and TOT: results from the Norwegian National Incontinence Registry. Int Urogynecol J. 2010;21(11):1321-1326. 12. Ward KL, Hilton P; UK and Ireland TVT Trial Group. Tension-free vaginal tape versus colposuspension for primary urodynamic stress incontinence: 5-year follow up. BJOG. 2008;115(2):226-233. WE’RE CHANGING THE WAY OVARIAN CANCER PATIENTS FEEL ABOUT THE FUTURE Intraperitoneal (IP) chemotherapy was introduced as a way to treat ovarian cancer by administering chemotherapy directly to the abdomen rather than through a vein. While this treatment extended median survival for women, the side effects were harsh and many women were unable to complete treatment. Our faculty at Magee-Womens Hospital of UPMC and UPMC Cancer Centers played a major role in the adaptation of IP to a modern outpatient regimen, reducing side effects and improving outcomes by adjusting dosing and anticipating and controlling symptoms. Oncologists at Magee and throughout UPMC were also among the first to use hyperthermic IP chemotherapy for the treatment of ovarian cancer. Snap the code and learn more at UPMCPhysicianResources.com. UPMC is affiliated with the University of Pittsburgh School of Medicine. MIDURETHRAL SLINGS 13. Angioli R, Plotti F, Muzii L, Montera R, Panici PB, Zullo MA. Tension-free vaginal tape versus transobturator suburethral tape: five-year follow-up results of a prospective, randomised trial. Eur Urol. 2010;58(5):671-677. 14. Olsson I, Abrahamsson AK, Kroon UB. Long-term efficacy of the tension-free vaginal tape procedure for the treatment of urinary incontinence: a retrospective follow-up 11.5 years post-operatively. Int Urogynecol J. 2010;21(6):679-683. 15. Nilsson CG, Palva K, Rezapour M, Falconer C. Eleven years prospective follow-up of the tension-free vaginal tape procedure for treatment of stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19(8):1043-1047. 16. Ballester M, Bui C, Frobert JL, et al. Four-year functional results of the suburethral sling procedure for stress urinary incontinence: a French prospective randomized multicentre study comparing the retropubic and transobturator routes. World J Urol. Mar 16, 2011. [Epub ahead of print.] 17. Oliveira R, Botelho F, Silva P, et al. Exploratory study assessing efficacy and complications of TVT-O, TVT-Secur, and Mini-Arc: results at 12-month follow-up. Eur Urol. 2011;59(6):940-944. 18. Oliveira R, Botelho F, Silva P, et al. Single-incision sling system as primary treatment of female stress urinary incontinence: prospective 12 months data from a single institution. BJU Int. 2011;108(10):1616-1621. 19. Krofta L, Feyereisl J, Velebil P, Otcenásek M, Kasíková E, Krcmár M. TVT-S for surgical treatment of stress urinary incontinence: prospective trial, 1-year follow-up. Int Urogynecol J. 2010;21(7):779-785. 20. Cornu JN, Sèbe P, Peyrat L, Ciofu C, Cussenot O, Haab F. Midterm prospective evaluation of TVT-Secur reveals high failure rate. Eur Urol. 2010;58(1):157-161. 28. Osman T. Stress incontinence surgery for patients presenting with mixed incontinence and a normal cystometrogram. BJU Int. 2003;92(9):964-968. 29. Jain P, Jirschele K, Botros SM, Latthe PM. Effectiveness of midurethral slings in mixed urinary incontinence: a systematic review and meta-analysis. Int Urogynecol J. 2011;22(8):923-932. 30. Kulseng-Hanssen S, Husby H, Schiøtz HA. Follow-up of TVT operations in 1,113 women with mixed urinary incontinence at 7 and 38 months. Int Urogynecol J Pelvic Floor Dysfunct. 2008;19(3):391-396. 31. Gamble TL, Botros SM, Beaumont JL, et al. Predictors of persistent detrusor overactivity after transvaginal sling procedures. Am J Obstet Gynecol. 2008;199(6): 696.e1-696.e7. 32. Botros SM, Miller JJ, Goldberg RP, et al. Detrusor overactivity and urge urinary incontinence following trans obturator versus midurethral slings. Neurourol Urodyn. 2007;26(1):42-45. 33. Rechberger T, Futyma K, Jankiewicz K, Adamiak A, Bogusiewicz M, Skorupski P. Body mass index does not influence the outcome of anti-incontinence surgery among women whereas menopausal status and ageing do: a randomised trial. Int Urogynecol J. 2010;21(7):801-806. 34. Hellberg D, Holmgren C, Lanner L, Nilsson S. The very obese woman and the very old woman: tension-free vaginal tape for the treatment of stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct. 2007;18(4):423-429. 21. Segal JL, Vassallo BJ, Kleeman SD, Hungler M, Karram MM. The efficacy of the tension-free vaginal tape in the treatment of five subtypes of stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct. 2006;17(2):120-124. 35. Groutz A, Cohen A, Gold R, Pauzner D, Lessing JB, Gordon D. The safety and efficacy of the “inside-out” transobturator TVT in elderly versus younger stressincontinent women: a prospective study of 353 consecutive patients. Neurourol Urodyn. 2011;30(3):380-383. 22. Miller JJ, Botros SM, Akl MN, et al. Is transobturator tape as effective as tension-free vaginal tape in patients with borderline maximum urethral closure pressure? Am J Obstet Gynecol. 2006;195(6):1799-1804. 36. Borstad E, Abdelnoor M, Staff AC, Kulseng-Hanssen S. Surgical strategies for women with pelvic organ prolapse and urinary stress incontinence. Int Urogynecol J. 2010;21(2): 179-186. 23. Jeon MJ, Jung HJ, Chung SM, Kin SK, Bai SW. Comparison of the treatment outcome of pubovaginal sling, tension-free vaginal tape, and transobturator tape for stress urinary incontinence with intrinsic sphincter deficiency. Am J Obstet Gynecol. 2008;199(1):76.e1-76.e4. 37. Stav K, Dwyer PL, Rosamilia A, et al. Repeat synthetic mid urethral sling procedure for women with recurrent stress urinary incontinence. J Urol. 2010;183(1):241-246. 24. Schierlitz L, Dwyer PL, Rosamilia A, et al. Effectiveness of tension-free vaginal tape compared with transobturator tape in women with stress urinary incontinence and intrinsic sphincter deficiency: a randomized controlled trial. Obstet Gynecol. 2008;112(6):1253-1261. 25. Lee JK, Dwyer PL, Rosamilia A, Lim YN, Polyakov A, Stav K. Persistence of urgency and urge urinary incontinence in women with mixed urinary symptoms after midurethral slings: a multivariate analysis. BJOG. 2011;118(7):798-805. 26. Houwert RM, Venema PL, Aquarius AE, Bruinse HW, Kil PJ, Vervest HA. Predictive value of urodynamics on outcome after midurethral sling surgery for female stress urinary incontinence. Am J Obstet Gynecol. 2009;200(6):649.e1-649.e12. 27. Stav K, Dwyer PL, Rosamilia A, Schierlitz L, Lim YN, 40 Lee J. Risk factors of treatment failure of midurethral sling procedures for women with urinary stress incontinence. Int Urogynecol J. 2010;21(2):149-155. contemporaryobgyn.net January 2012 38. US Food and Drug Administration. FDA.Serious complications associated with transvaginal placement of surgical mesh in repair of pelvic organ prolapse and stress urinary incontinence. Available at: www. fda.gov/MedicalDevices/safety/AlertsandNotices/ PublicHealthNotifications/ucm061976.htm. Issued October 20, 2008. Accessed October 30, 2011. 39. US Food and Drug Administration. FDA safety communication: UPDATE on serious complications associated with transvaginal placement of surgical mesh for pelvic organ prolapse. Available at: www.fda.gov/ medicaldevices/safety/alertsandnotices/ucm262435.htm. Issued July 13, 2011. Accessed October 30, 2011. 40. Clemons JL, LaSala CA. The tension-free vaginal tape in women with a non-hypermobile urethra and low maximum urethral closure pressure. Int Urogyncol J Pelvic Floor Dysfunct. 2007;18(7):727-732. PRODUCTS & SERVICES SHOWCASE ▶ Professional Services For special charter advertising rates, call Bill Smith at 1-800-225-4569, ext. 2718 JANUARY 2012 CONTEMPORARY OB/GYN 41 MARKETPLACE CONTINUING MEDICAL EDUCATION For Products & Services Advertising, contact: Bill Smith (800) 225-4569 ext. 2718, [email protected] CONTINUING MEDICAL EDUCATION 7th Annual CHALLENGES IN OBSTETRICS, GYNECOLOGY, & WOMEN’S HEALTH A GLOBAL HEALTH PERSPECTIVE Friday, May 11, 2012, Mount Sinai School of Medicine, New York City Dr. Rhoda Sperling & Dr. Michael Brodman, Course Directors ACOG credits available Please contact: [email protected] 35th Annual Advanced Ultrasound Seminar: OB/GYN February 16-18, 2012 Disney’s Yacht & Beach Club Lake Buena Vista, Florida ~ Featuring ~ Distinguished Guest Faculty Pre-Conference Workshops 336-716-4505 www.WakeHealth.edu/ultrasound 2012 Quality CE Conferences Contraceptive Technology Contraceptive Contraceptive Technology Technology Contraceptive Technology Obstetric Nursing Obstetric Nursing Health Care for Women Over 40 Health CareHealth for Women Adolescent Care Over 40 Adolescent Health Care Perinatal Dilemmas Perinatal Hot TopicsDilemmas In Primary Care Hot Topics In Primary Care Office Gynecology Office Gynecology Pharmacology For Adv. Practice Clinicians Pharmacology For Adv. Practice Clinicians Ambulatory OB/GYN Nursing Ambulatory OB/GYN Nursing Pharmacology For Adv. Practice Clinicians PharmacologyTechnology For Adv. Practice Clinicians Contraceptive Contraceptive PharmacologyTechnology For Adv. Practice Clinicians Pharmacology For Adv. Practice Clinicians San Francisco, CA San Francisco, Boston, MA CA Boston, MANV Las Vegas, Las Vegas, Vegas, NV NV Las Las NV CA San Vegas, Francisco, San Francisco, CA Jackson Hole, WY Jackson Jackson Hole, Hole, WY WY Jackson Hole, Snowmass, COWY Snowmass, COCA San Francisco, San Francisco, Boston, MA CA Boston, MA DC Washington, Washington, Atlanta, GA DC Atlanta, GA NV Las Vegas, Las Vegas, NV March 7-10 March 28-31 7-10 March March 28-31 April 15-18 April 17-19 15-18 May May May 17-19 31 - June 2 May 15-18 31 - June 2 July July July 15-18 29 - August 1 July 29 5-8 - August 1 August August 5-8 10-16 September September September 10-16 27-29 September 27-29 October 8-14 October 8-14 November 1-3 1-3 November 5-11 November 5-11 Register Today! www.ContemporaryForums.com/OBGYN Phone: (800) 377-7707 To see the latest Products & Services ads, visit http://products.modernmedicine.com 42 ContemporaryObgyn.net MEDICAL EQUIPMENT & SUPPLIES JANUARY 2012 Boot-Style Stirrups Fit Office Exam Tables Fits Tables By: A Must For Office-Based Surgery Midmark® Ritter® Hamilton Brewer www.harveystirrups.com 585-455-8229 CLASSIFIED WORKS! MARKETPLACE SEMINARS SEMINARS Marketplace Advertising Can Work For You! For Recruitment Advertising, contact: Jacqueline Moran (800) 225-4569 ext. 2762, [email protected] NATIONAL RECRUITMENT CONNECTICUT Chicago/Pittsburgh CHICAGO: 1-4 call-584 bed Level III teaching hospital with obgyn residency program-30 minutes to downtown. PITTSBURGH: 1-3 call-289 bed hospital-30 minutes to downtown$350-400K income potential. Excellent salary, bonus, benefits and partnership positions. OBGYN Search, 800-831-5475, Fax: 314-984-8246, [email protected], www.obgynpractices.com FOR RECRUITMENT ADVERTISING, CONTACT: JACQUELINE MORAN 440-891-2762 [email protected] MATERNAL FETAL MEDICINE CENTRAL CONNECTICUT Saint Francis Hospital and Medical Center in Hartford, Connecticut, has an exceptional opportunity for a BC/BE Maternal Fetal Medicine Specialist to join a dynamic and evolving group within a multi-specialty teaching hospital. Join three Maternal Fetal Medicine physicians in a department led by Dr. John Rodis, Chairman of the Department of Obstetrics and Gynecology. The Hospital and Medical Center performs 3,200 deliveries per year, and houses a 30-bed postpartum unit and 28-bed Level III NICU. The ideal candidate should have expertise in targeted ultrasound, amniocentesis, CVS, fetal echocardiography and medical complications of pregnancy. The successful candidate will have the opportunity to train residents and fellows in a fully accredited Obstetrics and Gynecology program and to contribute to clinical research endeavors. We offer a competitive salary commensurate with experience and an attractive benefits package. If you are an experienced Maternal Fetal Medicine physician interested in an excellent clinical and teaching opportunity in beautiful New England, please contact Christine Bourbeau, Physician Recruitment, at 855.894.5590, or email a letter of interest and CV to [email protected]. EEO/AA – M/F/D/V, pre-employment drug testing JANUARY 2012 CONTEMPORARY OB/GYN 43 RECRUITMENT FLORIDA ORLANDO AREA 45 Miintu Freo mT Beace! Seeking BC/BE OB/GYN physician to join 5 physician group Level 3 hospital ~ No emergency room call Income potential unlimited Send CV to e-mail: [email protected] or fax: 407-209-3575 For more information, please call 407-418-9103 MAINE MAINE SEACOAST General OBGYN position with leadership opportunity. Seeking BC OBGYN physician with 3+ years experience. Competitive salary, full benefits, relocation, student loans assistance. Coastal community one hour from Portland. Great schools, boating, scenic venues. Contact: Susan Edson [email protected], 207-866-5680 www.HealthSearchNewEngland.com IDAHO Maternal Fetal Medicine Flexible Practice & Quality Lifestyle • Live and work in a great location • Family-oriented, safe city with all Boise, Idaho amenities • Flexible schedule including part-time • New 32-bed Level III NICU, OB unit, maternal transport team and collegial subspecialty support. • MFM back-up/consultation • Competitive compensation and benefits with exceptional performance-based bonuses ▪ 24/7 laborist model MICHIGAN GYNECOLOGY ONLY - Take over established gynecology practice. 25-bed hospital. Prefer experienced board certified gynecologist with skills in some of the newest gyn procedures except robotics. Beautiful rural community in central Michigan close to 2 universities and gorgeous resort lake communities. Hospital employment position with salary, productivity and comprehensive benefits. Contact Todd Dillon at 800-883-7345 or [email protected]; www.cejkasearch.com. ID#141672CO. MISSOURI Contact: Sylvia Chariton at 800.309.5388 Email: [email protected] or FAX: 208.367.7964 http://www.saintalphonsus.org/careers-video.html KANSAS Kansas College Community Hospital employed obgyn position joining well established obgyn practice in new modern office adjacent to hospital in family oriented college community 45 minutes to Wichita associated with a financially stable hospital with modern L/D doing 300 annual deliveries. Heavy office gyn and gyn surgery. 1-2 call going to 1-3. Excellent salary, bonus and benefits. OBGYN Search, 800-831-5475, Fax: 314-984-8246, [email protected], www.obgynpractices.com Visit Us at http://careers.modernmedicine.com Missouri College Community Hospital employed obgyn position in desirable college community one hour to Kansas City and Columbia associated with a modern and financially stable 50 bed hospital with state-of-the-art Labor and Delivery Department doing 370 annual deliveries. 1-2 call backing up CNM. Excellent salary,bonus and benefits. OBGYN Search, 800-831-5475, Fax: 314-984-8246, [email protected], www.obgynpractices.com NEW YORK OBSTETRICIAN/ GYNECOLOGISTS WANTED New York Hospital Queens, a 519–bed acute care teaching hospital with 4,200 annual obstetrical deliveries seeks attending obstetrician/gynecologists for full time positions including office practice, deliveries, inpatient call, ER consults, inpatient consults, resident/Physician Assistant/ medical student teaching and surgery as indicated. Competitive salary. Recent residency graduates and current residents are encouraged to apply. We are an equal opportunity employer. Please email CV to Gary S. Eglinton, MD, Chairman: [email protected] Recruitment Advertising Can Work For You! 44 ContemporaryObgyn.net JANUARY 2012 RECRUITMENT NEW YORK Buffalo Suburb Hospital employed in dynamic Buffalo family oriented suburb associated with a progressive 100 bed hospital with modern L/D doing 500 annual deliveries. 1-2 call backing up 2 Certified Nurse Midwives in brand new office. Negotiable salary, bonus and benefits. OBGYN Search, 800-831-5475, Fax: 314-984-8246, [email protected], www.obgynpractices.com OHIO Ohio One Exceptional Opportunity! • Does living in a university town a short drive to other cosmopolitan cities excite you? • How does call 1:4 sound? Wood County Hospital is seeking an additional OB/GYN to join the staff of the Wood County Women’s Care. The gorgeous hospital has been completely renovated with a $45 million addition, now on par with any other of the best in the country. The group believes their highly skilled nursing staff is second to none. This community offering so much, including the arts and cultural amenities was rated the top 5 best place to live in Ohio! Contact Jane Dierberger: 800-243-4353 [email protected] CONNECT with qualified leads and career professionals Post a job today PENNSYLVANIA Pocono Medical Center Seeks OB/GYN Physicians Pocono Medical Center is seeking BC/BE physicians to join its hospital-owned practice. PMC sees 25,000 ofice visits per year at three locations and more than 900 births. Practice consists of six OB/GYNs, two Urogynecologist, two CRNPs, two midwives, and one physician assistant/first assist. All aspects of OB/GYN care are provided. Superb clinical and interpersonal skills are required. PMC has a Level II NICU and offers perinatal services. PMC is a 235-bed community hospital transitioning to a regional medical center. Located in Monroe County, the second-fastest growing county in Pennsylvania, PMC is just 75 miles from Manhattan and 90 minutes from Philadelphia. The Pocono Mountains boast spectacular year-round activities including skiing, biking, boating, fishing, hiking, and more than 30 golf courses. PMC offers an excellent compensation and benefits package, included fully funded malpractice insurance. For more information, contact: Holly Sheesley Physician Sourcing Specialist, Pocono Medical Center 206 East Brown Street • East Stroudsburg, PA 18301 Phone: (570) 476-3557 • Fax: (570) 420-2433 Email: [email protected] Visit us online: poconomedicalcenter.org UTAH Intermountain is frequently referenced nationally as one of the leaders in delivering high quality/low cost health care. Intermountain Healthcare needs one BC/BE OB/GYN in Mt. Pleasant, Utah. Send CV to Intermountain Healthcare, Physician Recruiting, 36 S. State St, 21 Fl, Salt Lake City, UT 84111. 800-888-3134. http://physicianjobsintermountain.org. VIRGINIA Opportunity for early to mid July, 2012 for a Board Certified/ Board Eligible physician to join a group of University-trained Board Certified Obstetricians and Gynecologists, including one Board Certified MFM. We have a regional referral center with a Level III NICU and a new state of the art Labor & Delivery unit as of 2012. Winchester is nestled in the Shenandoah Valley of Virginia just 70 miles from downtown Washington, DC. Outdoor and cultural activities abound. Call approximately 1/6 with five weeks vacation to start. Please contact Janie Smith c/o Winchester Obstetrics & Gynecology 1330A Amherst Street, Winchester, VA 22601 CALL (540) 667-2313, or EMAIL at [email protected] Inquiries will be kept confidential. Jacqueline Moran RECRUITMENT MARKETING ADVISOR (800) 225-4569, ext. 2762 [email protected] To place a RECRUITMENT ad, contact Jacqueline Moran 800.225.4569, ext. 2762 [email protected] JANUARY 2012 CONTEMPORARY OB/GYN 45 ADVERTISER INDEX APPLIED MEDICAL Alexis BAYER HEALTHCARE LLC One A Day Women’s Prenatal COOPER SURGICAL Uterinem 5 GYRUS ACMI Innovate 19 LACLEDE INC Luvena 27 NEOCUTIS NeoGyn 15 PACIFIC WORLD Bio-Oil 35 PFIZER Premarin TEXAS CHILDREN’S HOSPITAL Fetal Center UNIVERSITY OF PITTSBURGH MEDICAL CENTER US News Rankings FEATURED NEXT MONTH in 3 Inside front cover 48, inside back cover, back cover • Are oral antidiabetes agents appropriate for use in gestational diabetes? • Examining the evidence on vitamin D, calcium, and risk of cardiovascular disease • MFM Consult: Spinal injury 46 CONTEMPORARYOBGYN.NET JANUARY 2012 9 39 PROTOCOLS FOR HIGH-RISK PREGNANCIES SNAPSHOT Protocol 27—Obesity AUTHOR: PATRICK CATALANO, MD, METROHEALTH MEDICAL CENTER, CASE WESTERN RESERVE UNIVERSITY, CLEVELAND, OHIO SYNOPSIS: In this chapter, Dr. Catalano reviews the pathophysiology, diagnosis, prevention, and treatment of obesity in pregnancy. Included are guidelines for avoiding obesity-related complications in pregnancy, notes on postpartum follow-up, and a list of seminal reports in this subject area. As the author notes, pregnancy offers a woman the unique opportunity to affect her long-term health and that of her offspring. The ultimate treatment of obesity during pregnancy lies in preventing further weight gain. This can be achieved by avoiding excessive weight gain during pregnancy and implementing lifestyle measures to attain a more normal body mass index (BMI) prior to the next pregnancy. Based on preliminary evidence, achieving these measures also may have both short- and long-term benefits for the offspring. KEY MESSAGES: ⦁ Based on recent CDC data, approximately 60% of women of reproductive age are overweight and obese (BMI [weight/height2] >25). ⦁ Risk of developing preeclampsia, gestational diabetes mellitus, and delivery complications such as deep venous thrombophlebitis is increased in overweight and obese women. ⦁ The fetus of the obese woman is at risk for congenital anomalies, stillbirth, prematurity, insulin resistance, and increased adiposity. ⦁ As in nonpregnant individuals who are obese, the pathophysiology of obesity in pregnancy is related to “metabolic syndrome” and the insulin resistance associated with it that is seen in both pregnant women and their fetuses. ⦁ Preventing obesity is the best treatment and the role of healthcare professionals--including nutritionists and exercise instructors—in lifestyle modification should not be underestimated. READ the complete chapter on Obesity from Protocols for HighRisk Pregnancies, 5th Edition, edited by John T. Queenan, MD, John C. Hobbins, MD, and Catherine Y. Spong, MD, now. (Link to full chapter on COG Web site and/or in COG’s digital edition.) EditEd by John t. Queenan, John C. Hobbins and Catherine y. Spong Protocols for High-Risk Pregnancies Fifth Edition BUY the book (http:// www.wiley.com/ WileyCDA/WileyTitle/ productCd-1405196505. html) WATCH an interview with Drs. Queenan and Spong here: http://www.youtube.com/ watch?v=pdgqNUOtnk4 ⦁ For the fetus, treatment begins in utero with the mother’s efforts to avoid excessive weight gain and treatment of complications such as gestational diabetes and preeclampsia, should they develop. ⦁ A simple first step to diagnosing obesity in pregnancy is calculation of BMI at the first antenatal visit, based on measurements of height and weight on a calibrated scale. ⦁ Other cornerstones of management of the pregnant woman who is obese include establishing viability and assessing fetal anatomy; screening for diabetes in early and late pregnancy; monitoring for hallmarks of metabolic syndrome, such as elevated liver function; assessing fetal well-being; encouraging breastfeeding; and being prepared for the increased risk of cesarean delivery and the potential for attendant complications. MATERIAL USED WITH THE PERMISSION OF WILEY-BLACKWELL JANUARY 2012 CONTEMPORARY OB/GYN 47 PREMARIN® (CONJUGATED ESTROGENS) VAGINAL CREAM BRIEF SUMMARY: See Package Insert for Full Prescribing Information. For further product information and current package insert, please visit www.premarinvaginalcreamhcp.com or call our medical communications department toll-free at 1-800-934-5556. WARNING: CARDIOVASCULAR DISORDERS, ENDOMETRIAL CANCER, BREAST CANCER and PROBABLE DEMENTIA ESTROGEN-ALONE THERAPY ENDOMETRIAL CANCER There is an increased risk of endometrial cancer in a woman with a uterus who uses unopposed estrogens. Adding a progestin to estrogen therapy has been shown to reduce the risk of endometrial hyperplasia, which may be a precursor to endometrial cancer. Adequate diagnostic measures, including directed or random endometrial sampling when indicated, should be undertaken to rule out malignancy in postmenopausal women with undiagnosed persistent or recurring abnormal genital bleeding [see Warnings and Precautions (5.3)]. CARDIOVASCULAR DISORDERS AND PROBABLE DEMENTIA Estrogen-alone therapy should not be used for the prevention of cardiovascular disease or dementia [see Warnings and Precautions (5.2, 5.4), and Clinical Studies (14.2, 14.3) in full prescribing information]. The Women’s Health Initiative (WHI) estrogen-alone substudy reported increased risks of stroke and deep vein thrombosis (DVT) in postmenopausal women (50 to 79 years of age) during 7.1 years of treatment with daily oral conjugated estrogens (CE) [0.625 mg], relative to placebo [see Warnings and Precautions (5.2), and Clinical Studies (14.2) in full prescribing information]. The WHI Memory Study (WHIMS) estrogen alone ancillary study of WHI reported an increased risk of developing probable dementia in postmenopausal women 65 years of age or older during 5.2 years of treatment with daily CE (0.625 mg) alone, relative to placebo. It is unknown whether this finding applies to younger postmenopausal women [see Warnings and Precautions (5.4), Use in Specific Populations (8.5), and Clinical Studies (14.3) in full prescribing information]. In the absence of comparable data, these risks should be assumed to be similar for other doses of CE and other dosage forms of estrogens. Estrogens with or without progestins should be prescribed at the lowest effective doses and for the shortest duration consistent with treatment goals and risks for the individual woman. ESTROGEN PLUS PROGESTIN THERAPY CARDIOVASCULAR DISORDERS AND PROBABLE DEMENTIA Estrogen plus progestin therapy should not be used for the prevention of cardiovascular disease or dementia [see Warnings and Precautions (5.2, 5.4), and Clinical Studies (14.2, 14.3) in full prescribing information]. The WHI estrogen plus progestin substudy reported increased risks of DVT, pulmonary embolism, stroke and myocardial infarction in postmenopausal women (50 to 79 years of age) during 5.6 years of treatment with daily oral CE (0.625 mg) combined with medroxyprogesterone acetate (MPA) [2.5 mg], relative to placebo [see Warnings and Precautions (5.2), and Clinical Studies (14.2) in full prescribing information]. The WHIMS estrogen plus progestin ancillary study of the WHI, reported an increased risk of developing probable dementia in postmenopausal women 65 years of age or older during 4 years of treatment with daily CE (0.625 mg) combined with MPA (2.5 mg), relative to placebo. It is unknown whether this finding applies to younger postmenopausal women [see Warnings and Precautions (5.4), Use in Specific Populations (8.5), and Clinical Studies (14.3) in full prescribing information]. BREAST CANCER The WHI estrogen plus progestin substudy also demonstrated an increased risk of invasive breast cancer [see Warnings and Precautions (5.3), and Clinical Studies (14.2) in full prescribing information]. In the absence of comparable data, these risks should be assumed to be similar for other doses of CE and MPA, and other combinations and dosage forms of estrogens and progestins. Estrogens with or without progestins should be prescribed at the lowest effective doses and for the shortest duration consistent with treatment goals and risks for the individual woman. INDICATIONS AND USAGE Treatment of Atrophic Vaginitis and Kraurosis Vulvae Treatment of Moderate to Severe Dyspareunia, a Symptom of Vulvar and Vaginal Atrophy, due to Menopause CONTRAINDICATIONS PREMARIN Vaginal Cream therapy should not be used in women with any of the following conditions: • Undiagnosed abnormal genital bleeding • Known, suspected, or history of breast cancer • Known or suspected estrogen-dependent neoplasia • Active deep vein thrombosis, pulmonary embolism or a history of these conditions • Active arterial thromboembolic disease (for example, stroke, and myocardial infarction), or a history of these conditions • Known liver dysfunction or disease • Known thrombophilic disorders • Known or suspected pregnancy WARNINGS AND PRECAUTIONS Risks From Systemic Absorption Systemic absorption occurs with the use of PREMARIN Vaginal Cream. The warnings, precautions, and adverse reactions associated with oral PREMARIN treatment should be taken into account. Cardiovascular Disorders An increased risk of stroke and deep vein thrombosis (DVT) has been reported with estrogen-alone therapy. An increased risk of pulmonary embolism, DVT, stroke and myocardial infarction has been reported with estrogen plus progestin therapy. Should any of these occur or be suspected, estrogens with or without progestins should be discontinued immediately. Risk factors for arterial vascular disease (for example, hypertension, diabetes mellitus, tobacco use, hypercholesterolemia, and obesity) and/or venous thromboembolism (for example, personal history of venous thromboembolism [VTE], obesity, and systemic lupus erythematosus) should be managed appropriately. Stroke In the Women’s Health Initiative (WHI) estrogen-alone substudy, a statistically significant increased risk of stroke was reported in women 50 to 79 years of age receiving daily CE (0.625 mg) compared to women in the same age group receiving placebo (45 versus 33 per 10,000 women-years). The increase in risk was demonstrated in year one and persisted [see Clinical Studies (14.2) in full prescribing information]. Should a stroke occur or be suspected, estrogens should be discontinued immediately. Subgroup analyses of women 50 to 59 years of age suggest no increased risk of stroke for those women receiving CE (0.625 mg) versus those receiving placebo (18 versus 21 per 10,000 women-years).1 In the WHI estrogen plus progestin substudy, a statistically significant increased risk of stroke was reported in all women receiving daily CE (0.625 mg) plus MPA (2.5 mg) compared to placebo (33 versus 25 per 10,000 women-years) [see Clinical Studies (14.2) in full prescribing information]. The increase in risk was demonstrated after the first year and persisted.1 Coronary Heart Disease In the WHI estrogen-alone substudy, no overall effect on coronary heart disease (CHD) events (defined as nonfatal myocardial infarction [MI], silent MI, or CHD death) was reported in women receiving estrogen-alone compared to placebo [see Clinical Studies (14.2) in full prescribing information].1 Subgroup analyses of women 50 to 59 years of age suggest a statistically non-significant reduction in CHD events (CE 0.625 mg compared to placebo) in women with less than 10 years since menopause (8 versus 16 per 10,000 women-years). In the WHI estrogen plus progestin substudy, there was a statistically non-significant increased risk of CHD events in women receiving daily CE (0.625 mg) plus MPA (2.5 mg) compared to women receiving placebo (41 versus 34 per 10,000 women-years).1 An increase in relative risk was demonstrated in year 1, and a trend toward decreasing relative risk was reported in years 2 through 5 [see Clinical Studies (14.2) in full prescribing information]. In postmenopausal women with documented heart disease (n = 2,763), average age 66.7 years, in a controlled clinical trial of secondary prevention of cardiovascular disease (Heart and Estrogen/Progestin Replacement Study [HERS]), treatment with daily CE (0.625 mg) plus MPA (2.5 mg) demonstrated no cardiovascular benefit. During an average follow-up of 4.1 years, treatment with CE plus MPA did not reduce the overall rate of CHD events in postmenopausal women with established coronary heart disease. There were more CHD events in the CE plus MPA-treated group than in the placebo group in year 1, but not during subsequent users. Two thousand, three hundred and twenty-one (2,321) women from the original HERS trial agreed to participate in an open label extension of HERS, HERS II. Average follow-up in HERS II was an additional 2.7 years, for a total of 6.8 years overall. Rates of CHD events were comparable among women in the CE (0.625 mg) plus MPA (2.5 mg) group and the placebo group in HERS, HERS II, and overall. Venous Thromboembolism (VTE) In the WHI estrogen-alone substudy, the risk of VTE (DVT and pulmonary embolism [PE]) was increased for women receiving daily CE (0.625 mg) compared to placebo (30 versus 22 per 10,000 women-years), although only the increased risk of DVT reached statistical significance (23 versus 15 per 10,000 women-years). The increase in VTE risk was demonstrated during the first 2 years 3 [see Clinical Studies (14.2) in full prescribing information]. Should a VTE occur or be suspected, estrogens should be discontinued immediately. In the WHI estrogen plus progestin substudy, a statistically significant 2-fold greater rate of VTE was reported in women receiving daily CE (0.625 mg) plus MPA (2.5 mg) compared to women receiving placebo (35 versus 17 per 10,000 women-years). Statistically significant increases in risk for both DVT (26 versus 13 per 10,000 women-years) and PE (18 versus 8 per 10,000 women-years) were also demonstrated. The increase in VTE risk was observed during the first year and persisted 4 [see Clinical Studies (14.2) in full prescribing information]. Should a VTE occur or be suspected, estrogens should be discontinued immediately. If feasible, estrogens should be discontinued at least 4 to 6 weeks before surgery of the type associated with an increased risk of thromboembolism, or during periods of prolonged immobilization. Malignant Neoplasms Endometrial Cancer An increased risk of endometrial cancer has been reported with the use of unopposed estrogen therapy in a woman with a uterus. The reported endometrial cancer risk among unopposed estrogen users is about 2- to 12-fold greater than in non-users, and appears dependent on duration of treatment and on estrogen dose. Most studies show no significant increased risk associated with use of estrogens for less than 1 year. The greatest risk appears to be associated with prolonged use, with increased risks of 15- to 24-fold for 5 to 10 years or more, and this risk has been shown to persist for at least 8 to 15 years after estrogen therapy is discontinued. Clinical surveillance of all women using estrogen-alone or estrogen plus progestin therapy is important. Adequate diagnostic measures, including directed or random endometrial sampling when indicated, should be undertaken to rule out malignancy in postmenopausal women with undiagnosed persistent or recurring abnormal genital bleeding. There is no evidence that the use of natural estrogens results in a different endometrial risk profile than synthetic estrogens of equivalent estrogen dose. Adding a progestin to postmenopausal estrogen therapy has been shown to reduce the risk of endometrial hyperplasia, which may be a precursor to endometrial cancer. In a 52-week clinical trial using PREMARIN Vaginal Cream alone (0.5 g inserted twice weekly or daily for 21 days, then off for 7 days), there was no evidence of endometrial hyperplasia or endometrial carcinoma. Breast Cancer The most important randomized clinical trial providing information about breast cancer in estrogen-alone users is the Women’s Health Initiative (WHI) substudy of daily CE (0.625 mg). In the WHI estrogen-alone substudy, after an average follow-up of 7.1 years, daily CE (0.625 mg) was not associated with an increased risk of invasive breast cancer [relative risk (RR) 0.80] 5 [see Clinical Studies (14.2) in full prescribing information]. The most important randomized clinical trial providing information about breast cancer in estrogen plus progestin users is the WHI substudy of daily CE (0.625 mg) plus MPA (2.5 mg). After a mean follow-up of 5.6 years, the estrogen plus progestin substudy reported an increased risk of breast cancer in women who took daily CE plus MPA. In this substudy, prior use of estrogen-alone or estrogen plus progestin therapy was reported by 26 percent of the women. The relative risk of invasive breast cancer was 1.24, and the absolute risk was 41 versus 33 cases per 10,000 women-years, for estrogen plus progestin compared with placebo.6 Among women who reported prior use of hormone therapy, the relative risk of invasive breast cancer was 1.86, and the absolute risk was 46 versus 25 cases per 10,000 women-years for estrogen plus progestin compared with placebo. Among women who reported no prior use of hormone therapy, the relative risk of invasive breast cancer was 1.09, and the absolute risk was 40 versus 36 cases per 10,000 women-years for estrogen plus progestin compared with placebo. In the same substudy, invasive breast cancers were larger and diagnosed at a more advanced stage in the CE (0.625 mg) plus MPA (2.5 mg) group compared with the placebo group. Metastatic disease was rare, with no apparent difference between the two groups. Other prognostic factors, such as histologic subtype, grade and hormone receptor status did not differ between the groups [see Clinical Studies (14.2) in full prescribing information]. Consistent with the WHI clinical trial, observational studies have also reported an increased risk of breast cancer for estrogen plus progestin therapy, and a smaller increased risk for estrogen-alone therapy, after several years of use. The risk increased with duration of use, and appeared to return to baseline over about 5 years after stopping treatment (only the observational studies have substantial data on risk after stopping). Observational studies also suggest that the risk of breast cancer was greater, and became apparent earlier, with estrogen plus progestin therapy as compared to estrogen-alone therapy. However, these studies have not generally found significant variation in the risk of breast cancer among different estrogen plus progestin combinations, doses, or routes of administration. The use of estrogen-alone and estrogen plus progestin therapy has been reported to result in an increase in abnormal mammograms, requiring further evaluation. All women should receive yearly breast examinations by a healthcare provider and perform monthly breast self-examinations. In addition, mammography examinations should be scheduled based on patient age, risk factors, and prior mammogram results. Ovarian Cancer The WHI estrogen plus progestin substudy reported a statistically non-significant increased risk of ovarian cancer. After an average follow-up of 5.6 years, the relative risk for ovarian cancer for CE plus MPA versus placebo, was 1.58 (95 percent nCI 0.77-3.24). The absolute risk for CE plus MPA versus placebo was 4 versus 3 cases per 10,000 women-years.7 In some epidemiologic studies, the use of estrogen-only products, in particular for 5 or more years, has been associated with an increased risk of ovarian cancer. However, the duration of exposure associated with increased risk is not consistent across all epidemiologic studies, and some report no association. Probable Dementia In the estrogen-alone Women’s Health Initiative Memory Study (WHIMS), an ancillary study of WHI, a population of 2,947 hysterectomized women 65 to 79 years of age was randomized to daily CE (0.625 mg) or placebo. In the WHIMS estrogen-alone ancillary study, after an average follow-up of 5.2 years, 28 women in the estrogen-alone group and 19 women in the placebo group were diagnosed with probable dementia. The relative risk of probable dementia for CE-alone versus placebo was 1.49 (95 percent nCI 0.83-2.66). The absolute risk of probable dementia for CE-alone versus placebo was 37 versus 25 cases per 10,000 women-years 8 [see Use in Specific Populations (8.3), and Clinical Studies (14.3) in full prescribing information]. In the WHIMS estrogen plus progestin ancillary study, a population of 4,532 postmenopausal women 65 to 79 years of age was randomized to daily CE (0.625 mg) plus MPA (2.5 mg) or placebo. After an average follow-up of 4 years, 40 women in the CE plus MPA group and 21 women in the placebo group were diagnosed with probable dementia. The relative risk of probable dementia for CE plus MPA versus placebo was 2.05 (95 percent nCI 1.21-3.48). The absolute risk of probable dementia for CE plus MPA versus placebo was 45 versus 22 cases per 10,000 women-years 8 [see Use in Specific Populations (8.3), and Clinical Studies (14.3) in full prescribing information]. When data from the two populations were pooled as planned in the WHIMS protocol, the reported overall relative risk for probable dementia was 1.76 (95 percent nCI 1.19-2.60). Since both substudies were conducted in women 65 to 79 years of age, it is unknown whether these findings apply to younger postmenopausal women 8 [see Use in Specific Populations (8.5), and Clinical Studies (14.3) in full prescribing information]. Gallbladder Disease A 2- to 4-fold increase in the risk of gallbladder disease requiring surgery in postmenopausal women receiving estrogens has been reported. Hypercalcemia Estrogen administration may lead to severe hypercalcemia in women with breast cancer and bone metastases. If hypercalcemia occurs, use of the drug should be stopped and appropriate measures taken to reduce the serum calcium level. (continued on next page) Visual Abnormalities Retinal vascular thrombosis has been reported in patients receiving estrogens. Discontinue medication pending examination if there is sudden partial or complete loss of vision, or a sudden onset of proptosis, diplopia, or migraine. If examination reveals papilledema or retinal vascular lesions, estrogens should be permanently discontinued. Addition of a Progestin When a Woman Has Not Had a Hysterectomy Studies of the addition of a progestin for 10 or more days of a cycle of estrogen administration or daily with estrogen in a continuous regimen have reported a lowered incidence of endometrial hyperplasia than would be induced by estrogen treatment alone. Endometrial hyperplasia may be a precursor to endometrial cancer. There are, however, possible risks that may be associated with the use of progestins with estrogens compared to estrogen-alone regimens. These include an increased risk of breast cancer. Elevated Blood Pressure In a small number of case reports, substantial increases in blood pressure have been attributed to idiosyncratic reactions to estrogens. In a large, randomized, placebo-controlled clinical trial, a generalized effect of estrogen therapy on blood pressure was not seen. Hypertriglyceridemia In patients with pre-existing hypertriglyceridemia, estrogen therapy may be associated with elevations of plasma triglycerides leading to pancreatitis. Consider discontinuation of treatment if pancreatitis occurs. Hepatic Impairment and/or Past History of Cholestatic Jaundice Estrogens may be poorly metabolized in women with impaired liver function. For women with a history of cholestatic jaundice associated with past estrogen use or with pregnancy, caution should be exercised, and in the case of recurrence, medication should be discontinued. Hypothyroidism Estrogen administration leads to increased thyroid-binding globulin (TBG) levels. Women with normal thyroid function can compensate for the increased TBG by making more thyroid hormone, thus maintaining free T4 and T3 serum concentrations in the normal range. Women dependent on thyroid hormone replacement therapy who are also receiving estrogens may require increased doses of their thyroid replacement therapy. These women should have their thyroid function monitored in order to maintain their free thyroid hormone levels in an acceptable range. Fluid Retention Estrogens may cause some degree of fluid retention. Patients with conditions that might be influenced by this factor, such as cardiac or renal dysfunction, warrant careful observation when estrogens are prescribed. Hypocalcemia Estrogens should be used with caution in individuals with hypoparathyroidism as estrogen-induced hypocalcemia may occur. Exacerbation of Endometriosis A few cases of malignant transformation of residual endometrial implants have been reported in women treated post-hysterectomy with estrogen-alone therapy. For women known to have residual endometriosis posthysterectomy, the addition of progestin should be considered. Angioedema Exogenous estrogens may induce or exacerbate symptoms of angioedema, particularly in women with hereditary angioedema. Exacerbation of Other Conditions Estrogen therapy may cause an exacerbation of asthma, diabetes mellitus, epilepsy, migraine, porphyria, systemic lupus erythematosus, and hepatic hemangiomas and should be used with caution in women with these conditions. Effects on Barrier Contraception PREMARIN Vaginal Cream exposure has been reported to weaken latex condoms. The potential for PREMARIN Vaginal Cream to weaken and contribute to the failure of condoms, diaphragms, or cervical caps made of latex or rubber should be considered. Laboratory Tests Serum follicle stimulating hormone and estradiol levels have not been shown to be useful in the management of moderate to severe symptoms of vulvar and vaginal atrophy. Drug-Laboratory Test Interactions Accelerated prothrombin time, partial thromboplastin time, and platelet aggregation time; increased platelet count; increased factors II, VII antigen, VIII antigen, VIII coagulant activity, IX, X, XII, VII-X complex, II-VII-X complex, and beta-thromboglobulin; decreased levels of antifactor Xa and antithrombin III, decreased antithrombin III activity; increased levels of fibrinogen and fibrinogen activity; increased plasminogen antigen and activity. Increased thyroid-binding globulin (TBG) leading to increased circulating total thyroid hormone, as measured by protein-bound iodine (PBI), T4 levels (by column or by radioimmunoassay) or T3 levels by radioimmunoassay. T3 resin uptake is decreased, reflecting the elevated TBG. Free T4 and free T3 concentrations are unaltered. Women on thyroid replacement therapy may require higher doses of thyroid hormone. Other binding proteins may be elevated in serum, for example, corticosteroid binding globulin (CBG), sex hormone-binding globulin (SHBG), leading to increased total circulating corticosteroids and sex steroids, respectively. Free hormone concentrations, such as testosterone and estradiol, may be decreased. Other plasma proteins may be increased (angiotensinogen/renin substrate, alpha-1-antitrypsin, ceruloplasmin). Increased plasma HDL and HDL2 cholesterol subfraction concentrations, reduced LDL cholesterol concentrations, increased triglyceride levels. Impaired glucose tolerance. ADVERSE REACTIONS The following serious adverse reactions are discussed elsewhere in the labeling: • Cardiovascular Disorders [see Boxed Warning, Warnings and Precautions (5.2)] • Endometrial Cancer [see Boxed Warning, Warnings and Precautions (5.3)] Clinical Study Experience Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trial of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in practice. In a 12-week, randomized, double-blind, placebo-controlled trial of PREMARIN Vaginal Cream (PVC), a total of 423 postmenopausal women received at least 1 dose of study medication and were included in all safety analyses: 143 women in the PVC-21/7 treatment group (0.5 g PVC daily for 21 days, then 7 days off), 72 women in the matching placebo treatment group; 140 women in the PVC-2x/wk treatment group (0.5 g PVC twice weekly), 68 women in the matching placebo treatment group. A 40-week, open-label extension followed, in which a total of 394 women received treatment with PVC, including those subjects randomized at baseline to placebo. In this study, the most common adverse reactions * 5 percent are shown below (Table 1) [see Clinical Studies (14.1) in full prescribing information]. Table 1: Number (%) of Patients Reporting Treatment Emergent Adverse Events * 5 Percent Only Treatment a Body System Adverse Event PVC 21/7 (n=143) Placebo 21/7 (n=72) PVC 2x/wk (n=140) Placebo 2x/wk (n=68) Number (%) of Patients with Adverse Event Any Adverse Event Body As A Whole 95 (66.4) 45 (62.5) 97 (69.3) 46 (67.6) Abdominal Pain 11 (7.7) 2 (2.8) 9 (6.4) 6 (8.8) Accidental Injury 4 (2.8) 5 (6.9) 9 (6.4) 3 (4.4) Asthenia 8 (5.6) 0 2 (1.4) 1 (1.5) Back Pain 7 (4.9) 3 (4.2) 13 (9.3) 5 (7.4) Headache 16 (11.2) 9 (12.5) 25 (17.9) 12 (17.6) Infection 7 (4.9) 5 (6.9) 16 (11.4) 5 (7.4) Pain Cardiovascular System 10 (7.0) 3 (4.2) 4 (2.9) 4 (5.9) Vasodilatation 5 (3.5) 4 (5.6) 7 (5.0) 1 (1.5) Table 1: Number (%) of Patients Reporting Treatment Emergent Adverse Events * 5 Percent Only Digestive System Diarrhea 4 (2.8) 2 (2.8) 10 (7.1) 1 (1.5) Nausea Musculoskeletal System 5 (3.5) 4 (5.6) 3 (2.1) 3 (4.4) Arthralgia Nervous System 5 (3.5) 5 (6.9) 6 (4.3) 4 (5.9) Insomnia Respiratory System 6 (4.2) 3 (4.2) 4 (2.9) 4 (5.9) 0 1 (1.4) 7 (5.0) 3 (4.4) Pharyngitis Cough Increased 3 (2.1) 2 (2.8) 7 (5.0) 3 (4.4) Sinusitis Skin And Appendages 1 (0.7) 3 (4.2) 2 (1.4) 4 (5.9) 12 (8.4) 7 (9.7) 16 (11.4) 3 (4.4) Urogenital System Breast Pain 8 (5.6) 1 (1.4) 4 (2.9) 0 Leukorrhea 3 (2.1) 2 (2.8) 4 (2.9) 6 (8.8) Vaginitis 8 (5.6) 3 (4.2) 7 (5.0) 3 (4.4) a Body system totals are not necessarily the sum of the individual adverse events, since a patient may report two or more different adverse events in the same body system. Postmarketing Experience The following adverse reactions have been reported with PREMARIN Vaginal Cream. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure. Genitourinary System Abnormal uterine bleeding/spotting, dysmenorrhea/pelvic pain, increase in size of uterine leiomyomata, vaginitis (including vaginal candidiasis), change in cervical secretion, cystitis-like syndrome, application site reactions of vulvovaginal discomfort, (including burning, irritation, and genital pruritus), endometrial hyperplasia, endometrial cancer, precocious puberty, leukorrhea. Breasts Tenderness, enlargement, pain, discharge, fibrocystic breast changes, breast cancer, gynecomastia in males. Cardiovascular Deep venous thrombosis, pulmonary embolism, myocardial infarction, stroke, increase in blood pressure. Gastrointestinal Nausea, vomiting, abdominal cramps, bloating, increased incidence of gallbladder disease. Skin Chloasma that may persist when drug is discontinued, loss of scalp hair, hirsutism, rash. Eyes Retinal vascular thrombosis, intolerance to contact lenses. Central Nervous System Headache, migraine, dizziness, mental depression, nervousness, mood disturbances, irritability, dementia. Miscellaneous Increase or decrease in weight, glucose intolerance, edema, arthralgias, leg cramps, changes in libido, urticaria, anaphylactic reactions, exacerbation of asthma, increased triglycerides, hypersensitivity. Additional postmarketing adverse reactions have been reported in patients receiving other forms of hormone therapy. DRUG INTERACTIONS No formal drug interaction studies have been conducted for PREMARIN Vaginal Cream. Metabolic Interactions In vitro and in vivo studies have shown that estrogens are metabolized partially by cytochrome P450 3A4 (CYP3A4). Therefore, inducers or inhibitors of CYP3A4 may affect estrogen drug metabolism. Inducers of CYP3A4, such as St. John’s Wort (Hypericum perforatum) preparations, phenobarbital, carbamazepine, and rifampin, may reduce plasma concentrations of estrogens, possibly resulting in a decrease in therapeutic effects and/or changes in the uterine bleeding profile. Inhibitors of CYP3A4, such as erythromycin, clarithromycin, ketoconazole, itraconazole, ritonavir and grapefruit juice, may increase plasma concentrations of estrogens and may result in side effects. USE IN SPECIFIC POPULATIONS Pregnancy PREMARIN Vaginal Cream should not be used during pregnancy [see Contraindications (4)]. There appears to be little or no increased risk of birth defects in children born to women who have used estrogens and progestins as an oral contraceptive inadvertently during early pregnancy. Nursing Mothers PREMARIN Vaginal Cream should not be used during lactation. Estrogen administration to nursing mothers has been shown to decrease the quantity and quality of the breast milk. Detectable amounts of estrogens have been identified in the breast milk of mothers receiving estrogens. Caution should be exercised when PREMARIN Vaginal Cream is administered to a nursing woman. Pediatric Use PREMARIN Vaginal Cream is not indicated in children. Clinical studies have not been conducted in the pediatric population. Geriatric Use There have not been sufficient numbers of geriatric women involved in clinical studies utilizing PREMARIN Vaginal Cream to determine whether those over 65 years of age differ from younger subjects in their response to PREMARIN Vaginal Cream. The Women’s Health Initiative Study In the Women’s Health Initiative (WHI) estrogen-alone substudy (daily conjugated estrogens 0.625 mg versus placebo), there was a higher relative risk of stroke in women greater than 65 years of age [see Clinical Studies (14.2) in full prescribing information]. In the WHI estrogen plus progestin substudy, there was a higher relative risk of nonfatal stroke and invasive breast cancer in women greater than 65 years of age [see Clinical Studies (14.2) in full prescribing information]. The Women’s Health Initiative Memory Study In the Women’s Health Initiative Memory Study (WHIMS) of postmenopausal women 65 to 79 years of age, there was an increased risk of developing probable dementia in women receiving estrogen-alone or estrogen plus progestin when compared to placebo [see Clinical Studies (14.3) in full prescribing information]. Since both ancillary studies were conducted in women 65 to 79 years of age, it is unknown whether these findings apply to younger postmenopausal women 8 [see Clinical Studies (14.3) in full prescribing information]. Renal Impairment The effect of renal impairment on the pharmacokinetics of PREMARIN Vaginal Cream has not been studied. Hepatic Impairment The effect of hepatic impairment on the pharmacokinetics of PREMARIN Vaginal Cream has not been studied. OVERDOSAGE Overdosage of estrogen may cause nausea and vomiting, breast tenderness, dizziness, abdominal pain, drowsiness/fatigue, and withdrawal bleeding in women. Treatment of overdose consists of discontinuation of PREMARIN therapy with institution of appropriate symptomatic care. This brief summary is based on PREMARIN Vaginal Cream Prescribing Information W10413C022 ET01, Rev 05/10.