* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Internal Medicine Board Review: Cardiology Acute Coronary
Survey
Document related concepts
Saturated fat and cardiovascular disease wikipedia , lookup
Cardiovascular disease wikipedia , lookup
Electrocardiography wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Cardiac surgery wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Remote ischemic conditioning wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
History of invasive and interventional cardiology wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Transcript
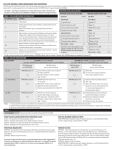
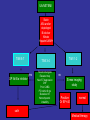
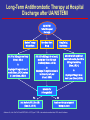
Internal Medicine Board Review: Cardiology Acute Coronary Syndrome Christine Nardi May 20, 2009 Hospitalizations in the U.S. Due to ACS Incidence rate of MI has not changed but survival has Acute Coronary Syndromes* 1.57 Million Hospital Admissions - ACS UA/NSTEMI† STEMI 1.24 million 0.33 million Admissions per year Admissions per year *Primary and secondary diagnoses. †About 0.57 million NSTEMI and 0.67 million UA. Heart Disease and Stroke Statistics – 2007 Update. Circulation 2007; 115:69–171. Acute Coronary Syndrome • Clinical syndromes caused by acute myocardial ischemia – Unstable angina • Angina at rest or new onset angina, accelerating symptoms • No detectable increase of biomarkers – Non-ST-elevation MI • Angina at rest or new onset angina, accelerating symptoms • Detectable release of biomarkers – ST-elevation MI • Clinical presentation of acute myocardial infarction with EKG evidence of ST-segment elevation Timing of Release of Various Biomarkers After Acute Myocardial Infarction Shapiro BP, Jaffe AS. Cardiac biomarkers. In: Murphy JG, Lloyd MA, editors. Mayo Clinic Cardiology: Concise Textbook. 3 rd ed. Rochester, MN: Mayo Clinic Scientific Press and New York: Informa Healthcare USA, 2007:773–80. Anderson JL, et al. J Am Coll Cardiol 2007;50:e1–e157, Figure 5. Pathophysiology: unstable angina and NSTEMI • Spontaneous rupture of lipid-laden, macrophage rich atherosclerotic plaques leading to platelet activation and thrombosis • Leads to episodic cessation of coronary blood flow, ischemia and pain • Rarely, caused by vasospasm (Prinzmetal’s or cocaine) Causes of UA/NSTEMI* • Thrombus or thromboembolism, usually arising on disrupted or eroded plaque – Occlusive thrombus, usually with collateral vessels† – Subtotally occlusive thrombus on pre-existing plaque – Distal microvascular thromboembolism from plaque-associated thrombus – Thromboembolism from plaque erosion • Non–plaque-associated coronary thromboembolism • Dynamic obstruction (coronary spasm‡ or vascoconstriction) of epicardial and/or microvascular vessels • Progressive mechanical obstruction to coronary flow • Coronary arterial inflammation • Secondary UA • Coronary artery dissection§ *These causes are not mutually exclusive; some patients have 2 or more causes. †DeWood MA, et al. N Engl J Med 1986;315:417–23. ‡May occur on top of an atherosclerotic plaque, producing missed-etiology angina or UA/NSTEMI. §Rare. Modified with permission from Braunwald E. Circulation 1998;98:2219–22. Anderson JL, et al. J Am Coll Cardiol. 2007;50:e1-e157, Table 3. Pathophysiology of STEMI • Occlusive thrombus that develops on a dissected or ulcerative atherosclerotic plaque, resulting in complete epicardial coronary artery occlusion • Moderately sized plaques are more common than those causing severe stenosis Evaluation • • • • History Physical exam EKG Cardiac biomarkers Variables Used in the TIMI Risk Score •Age ≥ 65 years •At least 3 risk factors for CAD •Prior coronary stenosis of ≥ 50% 0-2 low risk (5%) 3-4 intermediate risk 5-7 high risk (40%) •ST-segment deviation on ECG presentation •At least 2 anginal events in prior 24 hours •Use of aspirin in prior 7 days •Elevated serum cardiac biomarkers The TIMI risk score is determined by the sum of the presence of the above 7 variables at admission. 1 point is given for each variable. Primary coronary stenosis of 50% or more remained relatively insensitive to missing information and remained a significant predictor of events. Antman EM, et al. JAMA 2000;284:835–42. TIMI = Thrombolysis in Myocardial Infarction. Selection of Initial Treatment Strategy: Initial Invasive Versus Conservative Strategy Invasive Recurrent angina/ischemia at rest with low-level activities despite intensive medical therapy Elevated cardiac biomarkers (TnT or TnI) angiography New/presumably new ST-segment depression Signs/symptoms of heart failure or new/worsening mitral regurgitation High-risk findings from noninvasive testing Hemodynamic instability Sustained ventricular tachycardia PCI within 6 months Prior CABG High risk score (e.g., TIMI, GRACE) Reduced left ventricular function (LVEF < 40%) Conservative Low risk score (e.g., TIMI, GRACE) Patient/physician presence in the absence of high-risk features Stress testing UA/NSTEMI Statin ASA and/or clopidogrel B-blocker Nitrate Heparin/LMWH TIMI 5-7 yes GP IIb/IIIa inhibitor TIMI 1-2 TIMI 3-4 Recurrent angina Elevated trop New ST depression CHF Prior CABG PCI within 6 mo Sustained VT Hemodynamic instability no Stress imaging study Positive Or EF<40 normal cath Medical therapy Short-Term Risk of Death/Nonfatal MI in Patients With UA/NSTEMI Feature High Risk Intermediate Risk Low Risk ≥ 1 of the features below must be present: No high-risk features, but must have 1 of the following: No high- or intermediaterisk features but may have any features below: History Accelerating tempo of ischemic sx in preceding 48 h Prior MI, peripheral or cerebrovascular disease, or CABG; prior ASA use Character of pain Prolonged ongoing (> 20 min) rest pain • Prolonged (> 20 min) rest angina, • ↑ Angina frequency, now resolved, w/ moderate/high severity or duration likelihood of CAD • Angina provoked at • Rest angina (> 20 min) or relieved lower threshold with rest or sublingual NTG • New onset angina with • Nocturnal angina onset 2 wks to 2 mos prior to presentation • New-onset or progressive CCS class III/IV angina in past 2 wks w/o prolonged (> 20 min) rest pain but with intermediate/high likelihood of CAD Short-Term Risk of Death/Nonfatal MI in Patients With UA/NSTEMI, Continued Feature High risk Intermediate risk Low risk Clinical findings • Pulmonary edema, most likely due to ischemia • New/worsening MR murmur • S3 or new/worsening rales • Hypotension, bradycardia, tachycardia • Age > 75 y Age > 70 y ECG •Angina @ rest with transient ST-segment changes > 0.5 mm •BBB, new/presumed new •Sustained VT • T-wave changes • Pathological Q-waves/resting STdepression < 1 mm in multiple lead groups (anterior, inferior, lateral) Normal or unchanged ECG Cardiac markers ↑ Cardiac TnT, TnI, or CK-MB (e.g., TnT/TnI > 0.1 ng/mL) Slightly ↑ cardiac TnT, TnI, or CKMB (e.g., TnT > 0.01, but < 0.1 ng/mL) Normal Estimation of the short-term risk of death and nonfatal cardiac ischemic events in UA/NSTEMI is a complex multivariable problem that cannot be fully specified in a table such as this; this table is mean to offer general guidance & illustration rather than rigid algorithms. Braunwald E, et al. AHCPR Publication No. 94-0602:1–154. Anderson JL, et al. J Am Coll Cardiol 2007;50:e1–e157, Table 7. Long-Term Antithrombotic Therapy at Hospital Discharge after UA/NSTEMI UA/NSTEMI Patient Groups at Discharge Medical Therapy without Stent ASA 75 to 162 mg/d indefinitely (Class I, LOE: A) Bare Metal Stent Group Drug Eluting Stent Group ASA 162 to 325 mg/d for at least 1 month, then 75 to 162 mg/d indefinitely (Class I, LOE: A) & & Clopidogrel 75 mg/d for at least 1 month and up to 1 year (Class I, LOE:B) Clopidogrel 75 mg/d at least 1 month (Class I, LOE: A) and up to 1 year (Class I, LOE: B) ASA 162 to 325 mg/d for at least 3 to 6 months, then 75 to 162 mg/d indefinitely (Class I, LOE: A) & Clopidogrel 75 mg/d for at least 1 year (Class I, LOE: B) Indication for Anticoagulation? Yes Add: Warfarin (INR 2.0 to 2.5) (Class IIb, LOE: B) No Continue with dual antiplatelet therapy as above Anderson JL, et al. J Am Coll Cardiol 2007;50:e1–e157, Figure 11. INR = international normalized ratio; LOE = level of evidence. Management of STEMI • PCI – Higher vessel patency, lower reinfarction and stroke rates, immediate risk stratification – Should be performed if presenting within 12 hours of symptom onset if a skilled PCI lab is available • Fibrinolytic therapy – Highly available, ease of use – If no contraindications and no PCI available, fibrinolytics should be administered within 30 minutes from arrival to ED (if symptoms started within the last 12 hours) Absolute Contraindications to Fibrinolytics • • • • • • • Prior intracranial hemorrhage Known structural cerebral vascular lesion (AVM) Known malignant intracranial neoplasm Ischemic stroke without 3 months Suspected aortic dissection Active bleeding (excluding menses) Significant closed-head injury or facial trauma within 3 months Mortality Predictors in STEMI • • • • • • Age > 65 years Clinically evident heart failure Diabetes Renal failure Previous myocardial infarction Time of presentation (reperfusion less successful 12 hours after symptom onset) Complications during STEMI • Hypotension – Hypovolemia, increased vagal tone, low CO, hypoxia, rhythm disturbances • Pulmonary congestion – O2, nitrates, morphine, diuretics when appropriate • RV infarction – Hypotension, elevated JVP, inferior STEMI, bradcardia – ST-elevation in V4R – Treatment: fluids, temporary pacemaker Complications after STEMI • Occur in 0.1% of STEMI patients 2-7 days after infarction – – – – Ventricular septal defect Papillary muscle rupture (acute MR) Left ventricular free wall rupture (tamponade) pericarditis • New systolic murmur (VSD or MR) • Diagnosed with echo or Swan-Ganz catheter – VSD: O2 saturation step-up – Tamponade: equalization of diastolic pressures in all heart chambers Key Points • Intermediate and high risk patients with UA or NSTEMI benefit from an early invasive strategy with angiography • Early management of UA or NSTEMI includes ASA, heparin, nitrates, b-blocker, GP IIb/IIIa inhibitor, clopidogrel and statin • LMWH (enoxaparin) is a suitable alternative to unfractionated heparin for patients with acute coronary syndrome or STEMI and those undergoing early PCI Key Points • Clinical predictors of mortality in patients with acute STEMI are time to presentation after symptom onset, age>65, heart failure, DM, renal failure and previous MI • Immediate reperfusion, preferable with PCI, should be performed for any STEMI • Most patients with STEMI should be started early on oral b-blocker • STEMI patients with anterior infarction, pulmonary congestion, or a LVEF<40% should be started on an ACE inhibitor Differential Diagnosis • • • • • Aortic dissection Pulmonary embolus Perforating ulcer Tension pneumothorax Esophageal rupture (Boerhaave’s syndrome) Key Points • In patients with STEMI, successful fibrinolysis is suggested by resolution of chest pain and STsegment elevation and/or transient ventricular arrhythmias early after reperfusion. • In patients with STEMI, reperfusion arrhythmias usually do not require therapy. • Immediate coronary angiography is not indicated unless recurrent ischemia, persistent ST elevation or hemodynamic instability (including CHF) occurs. Key Points • Patients with STEMI should undergo coronary reperfusion in the most expeditious manner • STEMI patients who cannot be reperfused by direct coronary intervention within 90 to 120 minutes should receive fibrinolytic therapy if there are no contraindications Key Points • Ascending aortic dissection may involve the coronary arteries, most commonly the RCA • Ascending aortic dissection may lead to disruption of the aortic valve, leading to aortic regurgitation Key Points • Glycoprotein receptor blockade is indicated for patients with acute coronary syndrome who will undergo coronary angiography and intervention Key Points • Medical therapy for acute, recent myocardial infarction includes B-blocker, aspirin, ACE-inhibitor and statins • This is an uncomplicated (based on the absence of further symptoms and EKG changes) anterior STEMI • Late fibrinolysis is not beneficial for most patients and may be associated with an increase of transformation to a hemorrhagic zone of infarction • A glycoprotein IIb/IIIa blocker in addition to aspirin and heparin is indicated for patients with continuing ischemia, elevated troponin level or other high-risk features including angina at rest with ST changes and CHF Key Points • In patients with chest pan and intermediate risk of CAD, non-invasive testing is indicated • Patients with chest pain and low coronary artery disease risk with a normal EKG and a normal exercise EKG can be discharged without coronary angiography • Immediate coronary angiography would be appropriate if there were high risk markers: – – – – Elevated enzymes Hypotension Decreased LVEF New EKG changes in a patient with unstable angina or NSTEMI Key Points • Right ventricular infarction is a cause of hypotension following inferior infarction and typically requires appropriate volume infusion • Right ventricular infarction should be suspected as a cause of hypotension when findings of right heart failure coincides with an absence of evidence of pulmonary congestion Key Points • Papillary muscle rupture and ventricular septal defect are recognized mechanical complications that occur early after myocardial infarction • Both papillary muscle rupture and ventricular septal defect present with hypotension and acute dyspnea