* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Cardiac Conducting System AND Cardiac cycle
Management of acute coronary syndrome wikipedia , lookup
Coronary artery disease wikipedia , lookup
Heart failure wikipedia , lookup
Cardiac contractility modulation wikipedia , lookup
Antihypertensive drug wikipedia , lookup
Artificial heart valve wikipedia , lookup
Mitral insufficiency wikipedia , lookup
Hypertrophic cardiomyopathy wikipedia , lookup
Cardiac surgery wikipedia , lookup
Electrocardiography wikipedia , lookup
Myocardial infarction wikipedia , lookup
Quantium Medical Cardiac Output wikipedia , lookup
Lutembacher's syndrome wikipedia , lookup
Atrial fibrillation wikipedia , lookup
Atrial septal defect wikipedia , lookup
Dextro-Transposition of the great arteries wikipedia , lookup
Arrhythmogenic right ventricular dysplasia wikipedia , lookup
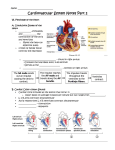
Cardiac Conducting System Cardiac muscle tissue contracts on its own No neural nor hormonal control “autorhythmicity’ Specialized cells: initiate and distribute depolarization 1. Sinoatrial node (SA node) a. Near entrance of superior vena cava/posterior wall of R. atrium b. “pacemaker cells” establish heart rate c. Connected to AV node via conducting pathways d. Stimulus affects only ATRIA i. Fibrous skeletal separates atria from ventricle 2. AV node: a. Floor of right atrium b. Near opening of coronary sinus c. From AV node to bundle of His( Left and right bundle branches) which run along interventricular septum d. Delay at AV node allows atria to complete contraction before ventricular contraction begins 3. Bundle branches(bundle of His) a. Impulse reaches bundle branches- travels along septum, splits between L & R bundle branches b. Purkinje fibers – where the bundle branches diverge into smaller branches i. Cause ventricular contraction ii. Wave action from apex(bottom) to base(top) toward right ventricle first iii. Blood is pushed out aortic and pulmonary trunk ELECTROCARDIOGRAM Monitors electrical activity of heart 1. P wave: small bump, atria contract after start of P wave – depolarization of atria(SA node) 2. QRS complex: ventricles depolarize – STRONG electrical signal – ventricles contract AFTER peak at R (AV node) 3. T wave small bump after QRS – ventricles relax 4. Do not “see” atrial relaxation due to strong QRS Problems detected: Extension of P-R interval = damage to conducting pathways or damage to AV node Extension of Q-T interval = myocardial damage HEART ATTACK – myocardial infarction Infarct = nonfunctional area of myocardium Enzymes that detect MI= LDH; SGOT; CPK(creatine phosphokinase) Systole – contraction Diastole – relaxation Interpretation of heart sounds via stethoscope Lubb- AV valves close – start of ventricular systole Dupp – semilunar valves close, ventricular diastole begins Patients upper area right of sternum – hear pulmonary semilunar valve Lower right of sternum – hear right atrioventricular valve (tricuspid) Upper right of sternum – hear aortic semilunar valve Lower right of sternum – left atrial ventricular valve – bicuspid CARDIAC CYCLE Heart beat to heartbeat – period of contraction(systole) and relaxation(diastole) Start of cycle: atrial systole – atria contract forcing a small amount of blood into ventricles to fill to capacity(already 70% full due to passive flow during diastole of both atria and ventricles following ventricular systole) Atrial diastole ventricular systole Ventricular pressure exceeds arterial pressure and semilunar valves open blood flows into pulmonary trunk or aorta Ventricular diastole pressure lowers in ventricles causing higher pressure in arteries(pulmonary trunk/aorta) causes Semi lunar valves to close BOTH atria and ventricles in diastole – blood flows passively from the veins into atria then to ventricles Before systole of atria begins again the ventricles are 70% filled with blood! If atria are damaged, the heart can still function! Stroke volume: amount of blood ejected by a single ventricle Cardiac output : amount of blood pumped by each ventricle in 1minute – provides idea of amount of peripheral blood flow – regulated so that all tissues are receiving an adequate blood supply CLINICAL NOTES – 1. Caffeine – acts directly on the conducting system increasing the rate of depolarization at SA node 2. Nicotine – stimulates the sympathetic neurons that innervate the heart – stress, speed, strength of contraction 3. Hypo or hyper kalemia (K+) concentrations – hyper polarize or depolarize the cell membrane – can result in death 4. Hypo or hyper calcium ion concentrations – prevent polarization – death 5. Low body temperature – lowers heart beat and contractility strength – until it stops… 6. High body temp – increases heart beat, contractility 7. Epinephrine – Norepinephrine – and thyroid hormones increase contractility – (positive inotropic effects) – sympathetic stimulation (cardiac nerve) 8. Ach – parasympathetic stimulation (vagus nerve) negative inotropic effect) – hyperpolarization/inhibition – slows heart 9. Cardiac center of medulla oblongata (regulated by reflex pathways from hypothalamus) a. Cardioaccelatory center – sympathetic neurons – increase heart rate b. Cardioinhibitory center – parasympathetic neurons – slow heart rate 10. Heart attack? – diagnostic blood test – enzymes enter blood if cardiac cells are imploding – cardiac troponin T, cardiac troponin 1, CK-MB(creatine phosphokinase) 11. 3 weeks – 21 days after conception – a beating heart!