* Your assessment is very important for improving the workof artificial intelligence, which forms the content of this project
Download Effects of the Abused Inhalant Toluene on the
NMDA receptor wikipedia , lookup
Axon guidance wikipedia , lookup
Artificial general intelligence wikipedia , lookup
Neuroplasticity wikipedia , lookup
Multielectrode array wikipedia , lookup
Synaptogenesis wikipedia , lookup
Single-unit recording wikipedia , lookup
Endocannabinoid system wikipedia , lookup
Neural oscillation wikipedia , lookup
Aging brain wikipedia , lookup
Environmental enrichment wikipedia , lookup
Caridoid escape reaction wikipedia , lookup
Metastability in the brain wikipedia , lookup
Stimulus (physiology) wikipedia , lookup
Biological neuron model wikipedia , lookup
Development of the nervous system wikipedia , lookup
Spike-and-wave wikipedia , lookup
Neural correlates of consciousness wikipedia , lookup
Neurotransmitter wikipedia , lookup
Mirror neuron wikipedia , lookup
Neuroeconomics wikipedia , lookup
Nonsynaptic plasticity wikipedia , lookup
Central pattern generator wikipedia , lookup
Molecular neuroscience wikipedia , lookup
Neural coding wikipedia , lookup
Chemical synapse wikipedia , lookup
Activity-dependent plasticity wikipedia , lookup
Circumventricular organs wikipedia , lookup
Neuroanatomy wikipedia , lookup
Premovement neuronal activity wikipedia , lookup
Nervous system network models wikipedia , lookup
Optogenetics wikipedia , lookup
Feature detection (nervous system) wikipedia , lookup
Pre-Bötzinger complex wikipedia , lookup
Channelrhodopsin wikipedia , lookup
Neuropsychopharmacology wikipedia , lookup
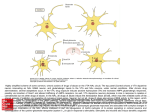
Ashdin Publishing Journal of Drug and Alcohol Research Vol. 3 (2014), Article ID 235838, 8 pages doi:10.4303/jdar/235838 ASHDIN publishing Review Article Effects of the Abused Inhalant Toluene on the Mesolimbic Dopamine System John J. Woodward1 and Jacob Beckley1,2 1 Department of Neurosciences, Medical University of South Carolina, Charleston, SC 29425, USA of Neurology, University of California, San Francisco (UCSF), San Francisco, CA 94117, USA Address correspondence to John J. Woodward, [email protected] 2 Department Received 10 December 2013; Revised 3 January 2014; Accepted 27 January 2014 Copyright © 2014 John J. Woodward and Jacob Beckley. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Abstract Toluene is a representative member of a class of inhaled solvents that are voluntarily used by adolescents and adults for their euphorigenic effects. Research into the mechanisms of action of inhaled solvents has lagged behind that of other drugs of abuse despite mounting evidence that these compounds exert profound neurobehavioral and neurotoxicological effects. Results from studies carried out by the authors and others suggest that the neural effects of inhalants arise from their interaction with a discrete set of ion channels that regulate brain activity. Of particular interest is how these interactions allow toluene and other solvents to engage portions of an addiction neurocircuitry that includes midbrain and cortical structures. In this review, we focus on the current state of knowledge regarding toluene’s action on midbrain dopamine neurons, a key brain region involved in the initial assessment of natural and drug-induced rewards. Findings from recent studies in the authors’ laboratory show that brief exposures of adolescent rats to toluene vapor induce profound changes in markers of glutamatergic plasticity in ventral tegmental area (VTA) dopamine (DA) neurons. These changes are restricted to VTA DA neurons that project to limbic structures and are prevented by transient activation of the medial prefrontal cortex prior to toluene exposure. Together, these data provide the first evidence linking the voluntary inhalation of solvents to changes in reward-sensitive dopamine neurons. Keywords synaptic plasticity; AMPA/NMDA ratio; solvents; addiction 1. Abused inhalants as drugs of abuse The term, abused inhalant, is used to denote a volatile solvent or gas that is voluntarily used to produce intoxication and feelings of reward [2]. Many abused inhalants are industrial solvents or volatile organic solvents and have important uses in industry and commercial business applications. Their widespread use and legal status makes them easily accessible to individuals seeking a cheap intoxicating substance. Abused inhalants are organized This article is a part of a Special Issue on “Advances in the Neurobiological Basis of Inhalant Abuse.” Preliminary versions of the papers featuring this special issue were originally presented at the 4th Meeting of the International Drug Abuse Research Society (IDARS) held in Mexico City, April 15–19, 2013. into three large classes based largely upon chemical and structural similarity: (1) volatile alkyl nitrites such as amyl nitrite, (2) anesthetic gas nitrous oxide, and (3) volatile solvents, fuels, and anesthetics [1]. Volatile solvents and fuels in the last category represent the largest class of abused inhalants and include compounds such as toluene and similar alkylbenzenes, trichloroethane, butane, and propane; and even gasoline that is a complex mixture of volatile hydrocarbons. Although anesthetic gases such as nitrous oxide and isoflurane are also used as drugs of abuse, their use is more restricted due to licensing and regulatory standards designed to limit their availability. It is clear from this classification scheme that abused inhalants represent a diverse set of chemical structures that share the ability to induce actions that some individuals “like” or find rewarding. In this regard, abused inhalants are similar to the more classical drugs of abuse such as cocaine, heroin or marijuana. However, in contrast to drugs of abuse that have high affinity for known protein targets (e.g., DAT, mu-opiate receptor, and CB1 receptor), abused inhalants have been thought of as relatively nonselective due to their relatively simple nonpolar chemical structure. However, as reviewed below, results from a series of studies show that solvents such as toluene have a surprising degree of molecular and brain region selectivity. 2. Who uses abused inhalants? The use and abuse of volatile solvents and gases is widespread and ranges from young children to licensed and practicing physicians. The use of these compounds by children and adolescents are of particular concern to health professionals and parents due to their effects on cognition and brain maturation and their toxicity following acute or chronic use. National surveys of drug use reveal that up to 20% of adolescents and teenagers have used or tried inhalants at least once although the percent of regular users 2 Journal of Drug and Alcohol Research of inhalants is much lower. In addition, there is an agedependence in the reported use of inhalants with individuals from 13 to 20 years old showing similar rates of use that drops markedly in persons older than 22–23 [16]. The reason for this age-dependency of inhalant use is currently unknown and may involve economic and social reasons as well as neurobiological factors that make inhalants especially rewarding in children and adolescents. 3. Adverse consequences of abused inhalants Significant health concerns related to the use of inhalants as drugs of abuse are many and include a sudden sniffing death that is associated with cardiac arrhythmia. Motor incoordination and other signs of intoxication following acute solvent inhalation may also contribute to injury or death in motor vehicle accidents. Chronic use of abused inhalants can lead to a variety of disorders including hearing loss, peripheral neuropathies, kidney damage, and loss of white matter in various brain regions [9]. The neurobehavioral consequences of chronic inhalant abuse are consistent with actions on the central nervous system [5] and include dementia, loss of memory and significant impairments in hippocampal-dependent maze learning [14] as well as deficits in PFC-dependent abilities such as executive function and working memory [22]. In addition, exposure to abused inhalants during the prenatal period can produce changes in the developing fetus that, like those associated with prenatal alcohol exposure, involve both anatomical and cognitive changes [17, 25]. Together, the serious health effects of abused inhalants combined with their use among a highly vulnerable adolescent population underscores the significance of defining the actions of inhalants on brain function. However, despite their importance as drugs of abuse, it is clear that funding for research on abused inhalants is below that for other drugs. Figure 1 shows a graph comparing the 30-day prevalence for use of various drugs among American 8th, 10th, and 12th graders versus the number of investigatorinitiated R01 grants per drug of abuse that are funded by the U.S. National Institute on Drug Abuse (NIDA, collected from http://projectreporter.nih.gov/). As of March 2013, the number of NIDA funded inhalants grants found in the NIH database is 10, as determined by the presence of at least one of five keywords in the title or abstract (inhalant, volatile solvent, alkyl nitrite, or nitrous oxide). In contrast, the number of NIH research grants involving cocaine, a drug with a comparable prevalence of use among adolescents, is 410. 4. Sites of action for toluene The molecular and cellular targets for abused inhalants including toluene are discussed in more detail in another paper of this issue [8]. In summary, a wide variety of voltage-gated and ligand-gated ion channels are affected Figure 1: Trends in drug prevalence and funding from the National Institute of Drug Abuse (NIDA). The graph depicts a relationship between a 30-day prevalence of drug use by a class and the number of R01s currently funded by NIDA for that drug class. Data for volatile solvents are indicated by a gold encircled triangle. Prevalence data are from the work of Johnston et al. [16]. Funding data are obtained from NIH Project Reporter for fiscal year 2013. Keywords are marijuana: marijuana, cannabis, THC, cannabidiol; inhalants: inhalant, volatile solvent, alkyl nitrite, nitrous oxide; cocaine: cocaine, crack; amphetamine: amphetamine, Adderall; methamphetamine; heroin; tranquilizers: benzodiazepine, Xanax, valium, klonopin, tranquilizer; hallucinogen: hallucinogen, psilocybin, LSD, PCP, ketamine; MDMA: MDMA, ecstasy. by toluene with both inhibition and potentiation being reported. These actions are similar to those produced by some volatile anesthetics and ethanol although in some cases, toluene’s effects appear to be more selective than these agents. In addition to these effects, toluene has actions on intracellular signaling pathways including those linked to generation of retrograde signaling molecules such as endocannabinoids [4, 24]. 5. Mesolimbic dopamine neurons Dopamine (DA) neurons are expressed in a variety of brain areas with two major nuclei being located in the substantia nigra (SN; A9) and the ventral tegmental area (VTA; A10). DA neurons in the SN project massively to the dorsal striatum and are most well known for their involvement in sensorimotor function while VTA DA neurons project to limbic and cortical structures. The dopaminergic projection to the ventral striatum or nucleus accumbens (NAc) is particularly important in signaling rewarding aspects of environmental stimuli as well as to drugs of abuse. A prevailing theory of drug use suggests that continued use of drugs of abuse may shift behavior from goal-directed responses involving reward-sensitive mesolimbic circuitry to that characterized by stimulus-response or habitual responding driven by nigrostriatal circuits. Journal of the International Drug Abuse Research Society Electrophysiological studies reveal that most midbrain DA neurons display low tonic rates of firing (1–5 Hz) interspersed with bursts of firing (20–80 Hz) that are associated with novel or rewarding stimuli [31]. The mechanisms that underlie the transition between tonic and burst modes of VTA DA neuron firing are still being elucidated but involve activation of synaptic N-methyl-Daspartate (NMDA) glutamate receptors and modulation of potassium channels including SK and KCNQ subtypes. Firing of VTA DA neurons is strongly suppressed via activation of D2 dopamine receptors and this feature is often used to identify putative DA neurons during in vitro and in vivo recordings. However, there is now a convincing evidence that D2 modulation of firing is produced in only a subpopulation of DA neurons and that the VTA expresses an array of dopamine neurons with divergent electrophysiological properties [29]. Classic DA neurons are defined by a set of functional criteria including broad action potentials with prominent afterhyperpolarization (AHP), a low firing frequency, a large hyperpolarization-induced inward current (IH ), and a strong D2-mediated inhibition of firing [15]. Within the VTA, these classic DA neurons occupy a more lateral position and project to the lateral shell of the nucleus accumbens. VTA DA neurons that project to the core or more medial aspects of the NAc and those that project to the PFC show smaller amplitude AHPs, less regular firing patterns, and often no evidence of the inward IH current. While electrophysiological criteria are by themselves often insufficient to unequivocally identify VTA DA neuron subtypes, combining recordings with retrograde labeling can identify projection specific populations of DA neurons. Using these techniques, Lammel et al. revealed that mesolimbic and mesocortical projecting VTA DA neurons display cell-type specific alterations in glutamatergic signaling in response to drugs of abuse or stress [20]. 6. Toluene and VTA DA neurons Work by Riegel, French, and colleagues first established that toluene could alter the firing rate of VTA DA neurons. Single unit recordings of classic DA neurons (see Section 5 above) in ketamine anesthetized rats showed that toluene, administered via a tracheal breathing tube at a concentration of 11,500 ppm, either enhanced or inhibited the firing of VTA DA neurons [27]. Each neuron showed either an increase or a decrease with no evidence of a single neuron showing both patterns of response. Recordings performed in midbrain slices of rat brain also showed that toluene could affect cell firing with differences noted depending on the subregion examined. For example, toluene enhanced the firing rate of classic DA neurons within the VTA and also increased firing of putative non-DA neurons [28]. Interestingly, in other midbrain areas, toluene inhibited the firing of neurons in the interpeduncular nucleus but had no effect on 3 neurons in the retrorubral field. The increase in firing of DA neurons in the presence of toluene persisted when synaptic transmission was inhibited suggesting that toluene may act on intrinsic mechanisms that regulate firing. Data from preliminary studies in the author’s laboratory suggest that toluene may interact with ion channels on VTA DA neurons that regulate firing as toluene-induced increases in firing are blocked in the presence of quinine, a compound that blocks various gap junction and potassium channels [10, 32]. As expected from results of the electrophysiological studies, toluene exposure in animals leads to increases in extracellular dopamine in areas such as striatum [33], nucleus accumbens [18, 28], VTA [28], and prefrontal cortex [13, 18]. In addition, toluene infused directly into the posterior but not anterior VTA increased extracellular dopamine levels in the NAc [28]. The behavioral consequences of toluene exposure have also been investigated and reveal that, in rodents, solvent inhalation enhances locomotor activity [19, 26], produces a conditioned place preference [11, 21], and produces anxiolytic effects in the elevated plus maze [6]. 7. Toluene effects on VTA DA neuron plasticity As discussed above, VTA DA neurons are critical elements of the brain’s reward circuitry and brief exposures to toluene alter DA neuron firing and release of DA in rewardassociated areas. Results from previous studies show that a single in vivo exposure to a drug of abuse such as cocaine or ethanol induces a change in glutamatergic signaling of VTA DA neurons [30, 34]. This is reflected in an increase in the ratio of α-amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid (AMPA) to NMDA excitatory postsynaptic currents (EPSCs) that is thought to reflect an initiation of long-term potentiation of synaptic glutamatergic transmission [23]. Anecdotal evidence suggests that volatile solvents are abused for their intoxicating effects and as discussed above, toluene has been shown to directly enhance VTA DA neuron firing. Despite these findings, prior to a recent publication from the authors’ laboratory [3], no previous studies had examined whether in vivo exposure to toluene induces a change in VTA DA neuron plasticity that is similar to that produced by other drugs of abuse. A challenge in these studies was the knowledge that there are different subpopulations of DA neurons in the VTA that have different signaling properties and projection targets [20]. In the standard acute slice preparation, it is not possible to determine the efferent projection of the DA neuron being recorded from or to verify that the recorded neuron is in fact dopaminergic. To circumvent this limitation, we microinjected fluorescent retrobeads into selective projection regions of VTA DA neurons. Once injected, these beads are taken up by presynaptic terminals in the target area and transported back to the cell body where they can be 4 Journal of Drug and Alcohol Research concentration-dependent as exposure to 5,700 ppm toluene (equivalent to that used by human solvent abusers) increased the AMPA/NMDA ratio while 2,850 ppm had no effect. The altered ratio in mesolimbic core neurons persisted for at least 3 days after exposure and returned to baseline values within 1 week (Figure 3(d)). Remarkably, the AMPA/NMDA ratio of mesolimbic shell neurons was still significantly enhanced 3 weeks following the brief exposure to toluene vapor (Figure 3(e)). In contrast, exposure to 5,700 ppm toluene vapor had no effect on the AMPA/NMDA ratio of VTA DA neurons that project to the mPFC (Figure 4). These results demonstrate that a brief exposure to toluene vapor induces highly selective and long-lasting effects on VTA DA neuron excitability and show that these compounds, like other drugs of abuse, impact dopaminergic neurons involved in reward. Figure 2: Identification of VTA neurons by immunohistochemistry. (a) Examples of tyrosine hydroxylase (TH) positive (left) and negative (right) VTA neurons. Red indicates the biocytin label in a recorded neuron and green represents the presence of TH, while yellow indicates both. (b) Proportion of TH+ recorded neurons from each retrobead-labeled region. Blue is TH positive; red is TH negative. Derived from the work of Beckley et al. [3]. To determine a mechanism for the change in the AMPA/NMDA ratio following toluene exposure, we measured spontaneous AMPA EPSCs in core-projecting VTA DA neurons in control and toluene exposed animals. These data revealed an increase in the amplitude but not frequency of AMPA EPSCs suggesting that the enhanced AMPA/NMDA ratio was due to an increase in the postsynaptic expression of AMPA receptors (Figure 5). This was confirmed by experiments showing that following toluene exposure, the rectification index of electrically evoked AMPA EPSCs was significantly increased, consistent with an upregulation of calcium-permeable, GluA2 lacking AMPA receptors in VTA DA neurons following toluene exposure (Figure 5, bottom panels). visualized in living cells under epifluorescence microscopy. In our VTA studies, we microinjected retrobeads into either the NAc core or shell or the medial prefrontal cortex (mPFC) of adolescent male rats. Each animal received an injection in only one area in order to label a specific pathway. Based on the injection site, these beads will label either mesolimbic or mesocortical DA neurons that are known to be involved in different aspects of reward processing [29]. Animals were returned to their home cage to allow for retrograde transport of beads and then animals were exposed to two brief (10 min each separated by 10 min of air) sessions of toluene vapor to mimic that experienced by human solvent abusers (high vapor concentration; short duration). At different times following exposure (1 day to 3 weeks), animals were sacrificed and whole-cell patch-clamp electrophysiology was used to determine the AMPA/NMDA ratio in beadlabeled DA neurons. Post-hoc immunohistochemistry with an antibody to tyrosine hydroxylase was used to confirm that bead-labeled neurons were dopaminergic (Figure 2). As shown in Figure 3, the brief exposure to toluene vapor induced a highly significant two-fold increase in the AMPA/NMDA ratio of mesolimbic core and shell VTA DA neurons when measured 24 h later [3]. This effect was In a final set of studies, we determined whether in vivo manipulation of the mPFC could influence toluene’s ability to induce changes in VTA DA neuron plasticity. To do this, we microinjected pharmacological modulators of GABA receptors into the mPFC of the rat just prior to vapor exposure and then examined changes in the AMPA/NMDA ratio of bead-labeled DA neurons 24 h later. In animals pretreated with the GABAA receptor blocker picrotoxin that enhances mPFC neuronal firing, 5,700 ppm toluene no longer increased the AMPA/NMDA ratio of mesolimbic core VTA DA neurons (Figure 6(b)). In contrast, in animals injected with a cocktail of the GABAA/B receptor agonists muscimol/baclofen to reduce mPFC neuronal firing, 2,850 ppm toluene, a concentration that had no effect in control animals, now produced a significant increase in the AMPA/NMDA ratio of mesolimbic DA neurons (Figure 6(c)). These results are the first to demonstrate that the PFC can modulate the response of VTA DA neurons to a drug of abuse. They suggest that output from the prefrontal cortex critically determines whether abused solvents and likely other drugs of abuse will induce longlasting changes in glutamatergic signaling in brain reward areas such as the VTA. The mechanisms underlying the PFC modulation of VTA DA neuron excitability are not yet Journal of the International Drug Abuse Research Society 5 Figure 3: Toluene vapor enhances the AMPA/NMDA ratio of mesoaccumbens DA neurons. Top panels show the location of retrobead injections in the NAc core (a) and shell (b) and examples of bead-labeled neurons in VTA. Values represent the distance in mm from bregma. Middle panels show the effects of toluene on the AMPA/NMDA ratio of VTA DA neurons in the NAc core (c), (d) and shell (e). Panels (f) and (g) show representative traces from control and toluene exposed animals. Calibration bar: 20 pA, 10 ms. Symbol (∗) indicates a significant difference (P < .05) in ratio between air- and tolueneexposed animals. Derived from the work of Beckley et al. [3]. known. Detailed tracing and electron microscopy studies by Carr and Sesack show that mPFC neurons make excitatory synapses on mesocortical but not mesoaccumbens VTA DA neurons [7]. In addition, a recent study using a modified rabies virus to transynaptically label VTA DA neuron inputs showed that mesolimbic DA neurons receive few if any direct connections from mPFC neurons while those from orbitofrontal cortex and other areas are relatively robust [35]. Carr and Sesack also showed that medial prefrontal neurons make excitatory synapses onto local interneurons in the VTA and those that project to the NAc. This arrangement would allow mPFC neurons to regulate mesolimbic DA neuron activity via activation of GABA neurons that inhibit VTA DA neurons and NAc medium spiny neurons (MSNs). Such circuitry could explain how pharmacological manipulation of mPFC activity in the study of Beckley et al. [16] could bidirectionally alter the response of VTA DA neurons to toluene vapor exposure. Studies are currently underway in the author’s laboratory to test this hypothesis. 6 Journal of Drug and Alcohol Research Figure 4: Toluene vapor has no effect on AMPA/NMDA ratio in mesocortical DA neurons. (a) Location of retrobead injections into medial prefrontal cortex and an example of bead-labeled VTA DA neurons. Values represent the distance in mm from bregma. (b) The graph shows a lack of change in ratio between air- and toluene-exposed animals. (c) Representative traces from PFC projecting VTA DA neurons. Calibration bar: 20 pA, 10 ms. Derived from the work of Beckley et al. [3]. Figure 5: Toluene exposure increases AMPA EPSC amplitude but not frequency and enhances AMPA current rectification. Top panels: (a) Averaged EPSCs from air-exposed (gray) and toluene-exposed (black) animals (calibration bar: 5 pA, 5 ms) and examples of spontaneous AMPA EPSCs (calibration bar: 25 pA, 500 ms). (b) Cumulative probably chart of AMPA EPSC amplitude (±SEM) from air- and toluene-exposed animals (5,750 ppm). Inset shows mean (±SEM) amplitude of AMPA EPSCs from air- and toluene-exposed animals. (c) A cumulative probability chart of AMPA EPSC interevent interval (±SEM). Inset shows mean (±SEM) for air- and toluene-exposed animals. Symbol (∗ ∗ ∗) indicates a significant (P < .001; mixed ANOVA) amplitude x treatment interaction; symbol (∗) indicates a value significantly (P < .05; t-test) different from control. Bottom panels: (a) A current-voltage relationship for evoked AMPA EPSCs from air- and toluene-exposed animals. (b) Representative examples of AMPA EPSCs evoked from air (left) and toluene (right) exposed animals. Downward traces were obtained at −70 mV and upward traces are at +40 mV. Note a blunted outward current amplitude in a toluene-treated neuron. Calibration bar: 25 pA, 5 ms. (c) A summary of the effect of toluene vapor exposure on the rectification index of evoked AMPA EPSCs. Symbol (∗∗∗) indicates a significant (P < .001; mixed ANOVA, Bonferroni multiple comparison test) difference in current at +40 mV between toluene-treated and air-treated animals; symbol (∗) indicates a value significantly (P < .05; t-test) different from control. Derived from the work of Beckley et al. [3]. Journal of the International Drug Abuse Research Society 7 Figure 6: PFC output regulates the toluene’s effect on AMPA/NMDA ratio in mesoaccumbens core DA neurons. (a) Placement of microinjection cannula in the medial prefrontal cortex. Values represent the distance (mm) from bregma. (b) Intra-PFC injection of picrotoxin blocks the toluene-induced increase in AMPA/NMDA ratio in mesoaccumbens VTA DA neurons. (c) Intra-PFC injection of muscimol/baclofen allows a previously inactive dose of toluene vapor to enhance the AMPA/NMDA ratio of mesoaccumbens VTA DA neurons. (∗∗) indicates a value significantly (P < .01; two-way ANOVA, Bonferroni post-hoc test) different from all other groups; (∗) indicates a value significantly (P < .05; two-way ANOVA, Bonferroni post-hoc test) different from all other groups. Derived from the work of Beckley et al. [3]. 8. Summary and implications for treatment The studies outlined above clearly indicate that toluene has important actions on midbrain dopamine neurons and higher cortical areas that regulate reward-based brain areas. Repeated use of toluene and other abused inhalants would be expected to profoundly alter the reward circuitry and may predispose individuals to further use of these compounds as well as other abused substances. The use of inhalants by children and adolescents is particularly troubling as a persistent use of these agents may lead to deficits in normal brain development especially in the frontal cortical areas that do not fully mature until young adulthood. Despite these adverse consequences, treatment of individuals who abuse inhalants is not well developed and there are relatively few reports of effective pharmacotherapies for inhalant abuse. A recent review of volatile solvent misuse and its treatment described the use of either lamotrigine, an anticonvulsant, or aripiprazole, a dopamine D2 partial agonist, to treat ongoing inhalant abuse. These compounds appeared to reduce the number of days of inhalant use by adolescents and prevented relapse in an adult patient for the 6-month study period [12]. Lamotrigine and aripiprazole have been used to treat other addictive disorders and may target dysfunctional glutamatergic and dopaminergic signaling pathways in mesolimbic and mesolimbic-reward sensitive brain areas. Other agents may be used to treat the acute signs of withdrawal from inhalant use that resemble those associated with alcohol withdrawal. These compounds include GABAergic agents including baclofen and benzodiazepines that reduce excitability and antiseizure medications that may target hyperactive glutamatergic signaling pathways. A difficulty in treating inhalant abuse is that it is often accompanied by neuropsychiatric symptoms associated with mood and conduct disorders. Thus, successful diagnosis and treatment of the underlying psychiatric disorder with wellestablished pharmacotherapies may alleviate the misuse of solvents. Finally, there are likely long-term effects of inhalant abuse on cortical-based processes including memory, attention, and self-control that contribute to the likelihood of relapse to solvent use. Treatment of these deficits by agents or approaches that enhance cognition (e.g., Ampakines, nicotinic agonists, etc.) or improve cognitive control over impulsive behaviors (cognitive behavioral therapy; coping strategies) may be particularly beneficial in regaining control over inhalant use. In conclusion, as with many other aspects of inhalant research, the treatment of inhalant abuse lags behind that of other addictive substances and more effort is needed to develop rationale and effective treatments of inhalant abuse. Acknowledgments This work was supported by NIH Grants R01 DA013951 (JJW) and F31 DA030891 (JTB). References [1] R. L. Balster, Neural basis of inhalant abuse, Drug Alcohol Depend, 51 (1998), 207–214. [2] R. L. Balster, The pharmacology of inhalants, in Principles of Addiction Medicine, R. K. Ries, D. A. Fiellin, S. A. Miller, and R. Saitz, eds., Lippincott Williams & Wilkins, Philadelphia, PA, 4th ed., 2009, 241–250. [3] J. T. Beckley, C. E. Evins, H. Fedarovich, M. J. Gilstrap, and J. J. Woodward, Medial prefrontal cortex inversely regulates tolueneinduced changes in markers of synaptic plasticity of mesolimbic dopamine neurons, J Neurosci, 33 (2013), 804–813. [4] J. T. Beckley and J. J. Woodward, The abused inhalant toluene differentially modulates excitatory and inhibitory synaptic transmission in deep-layer neurons of the medial prefrontal cortex, Neuropsychopharmacology, 36 (2011), 1531–1542. 8 [5] S. E. Bowen, J. C. Batis, N. Páez-Martı́nez, and S. L. Cruz, The last decade of solvent research in animal models of abuse: Mechanistic and behavioral studies, Neurotoxicol Teratol, 28 (2006), 636–647. [6] S. E. Bowen, J. L. Wiley, and R. L. Balster, The effects of abused inhalants on mouse behavior in an elevated plus-maze, Eur J Pharmacol, 312 (1996), 131–136. [7] D. B. Carr and S. R. Sesack, Projections from the rat prefrontal cortex to the ventral tegmental area: target specificity in the synaptic associations with mesoaccumbens and mesocortical neurons, J Neurosci, 20 (2000), 3864–3873. [8] S. L. Cruz, M. T. Rivera-Garcı́a, and J. J. Woodward, Review of toluene actions: clinical evidence, animal studies, and molecular targets, J Drug Alcohol Res, 3 (2014), art235840. [9] C. M. Filley, W. Halliday, and B. K. Kleinschmidt-DeMasters, The effects of toluene on the central nervous system, J Neuropathol Exp Neurol, 63 (2004), 1–12. [10] J. E. Freedman and F. F. Weight, Quinine potently blocks single K+ channels activated by dopamine D-2 receptors in rat corpus striatum neurons, Eur J Pharmacol, 164 (1989), 341–346. [11] M. Funada, M. Sato, Y. Makino, and K. Wada, Evaluation of rewarding effect of toluene by the conditioned place preference procedure in mice, Brain Res Protoc, 10 (2002), 47–54. [12] E. L. Garland and M. O. Howard, Volatile substance misuse: clinical considerations, neuropsychopharmacology and potential role of pharmacotherapy in management, CNS Drugs, 26 (2012), 927–935. [13] M. R. Gerasimov, W. K. Schiffer, D. Marstellar, R. Ferrieri, D. Alexoff, and S. L. Dewey, Toluene inhalation produces regionally specific changes in extracellular dopamine, Drug Alcohol Depend, 65 (2002), 243–251. [14] J. M. Gmaz, L. Yang, A. Ahrari, and B. E. McKay, Binge inhalation of toluene vapor produces dissociable motor and cognitive dysfunction in water maze tasks, Behav Pharmacol, 23 (2012), 669–677. [15] A. A. Grace and B. S. Bunney, The control of firing pattern in nigral dopamine neurons: single spike firing, J Neurosci, 4 (1984), 2866–2876. [16] L. D. Johnston, P. M. O’Malley, J. G. Bachman, and J. E. Schulenberg, Monitoring the Future—National results on adolescent drug use: Overview of key findings, 2012. Institute for Social Research, The University of Michigan, Ann Arbor, MI, 2013. [17] H. E. Jones and R. L. Balster, Inhalant abuse in pregnancy, Obstet Gynecol Clin North Am, 25 (1998), 153–167. [18] Y. Koga, S. Higashi, H. Kawahara, and T. Ohsumi, Toluene inhalation increases extracellular noradrenaline and dopamine in the medial prefrontal cortex and nucleus accumbens in freelymoving rats, J Kyushu Dent Soc, 61 (2007), 39–54. [19] H. Kondo, J. Huang, G. Ichihara, M. Kamijima, I. Saito, E. Shibata, et al., Toluene induces behavioral activation without affecting striatal dopamine metabolism in the rat: Behavioral and microdialysis studies, Pharmacol Biochem Behav, 51 (1995), 97–101. [20] S. Lammel, A. Hetzel, O. Häckel, I. Jones, B. Liss, and J. Roeper, Unique properties of mesoprefrontal neurons within a dual mesocorticolimbic dopamine system, Neuron, 57 (2008), 760– 773. [21] D. E. Lee, M. R. Gerasimov, W. K. Schiffer, and A. N. Gifford, Concentration-dependent conditioned place preference to inhaled toluene vapors in rats, Drug Alcohol Depend, 2006 (85), 87–90. [22] B. F. Lin, M. C. Ou, S. S. Chung, C. Y. Pang, and H. H. Chen, Adolescent toluene exposure produces enduring social and cognitive deficits in mice: an animal model of solvent-induced psychosis, World J Biol Psychiatry, 11 (2010), 792–802. Journal of Drug and Alcohol Research [23] C. Luscher and R. C. Malenka, Drug-evoked synaptic plasticity in addiction: from molecular changes to circuit remodeling, Neuron, 69 (2011), 650–663. [24] M. MacIver, Abused inhalants enhance GABA-mediated synaptic inhibition, Neuropsychopharmacology, 34 (2009), 2296–2304. [25] M. Pascual, J. Boix, V. Felipo, and C. Guerri, Repeated alcohol administration during adolescence causes changes in the mesolimbic dopaminergic and glutamatergic systems and promotes alcohol intake in the adult rat, J Neurochem, 108 (2009), 920–931. [26] A. C. Riegel and E. D. French, Acute toluene induces biphasic changes in rat spontaneous locomotor activity which are blocked by remoxipride, Pharmacol Biochem Behav, 62 (1999), 399–402. [27] A. C. Riegel and E. D. French, An electrophysiological analysis of rat ventral tegmental dopamine neuronal activity during acute toluene exposure, Pharmacol Toxicol, 85 (1999), 37–43. [28] A. C. Riegel, A. Zapata, T. S. Shippenberg, and E. D. French, The abused inhalant toluene increases dopamine release in the nucleus accumbens by directly stimulating ventral tegmental area neurons, Neuropsychopharmacology, 32 (2007), 1558–1569. [29] J. Roeper, Dissecting the diversity of midbrain dopamine neurons, Trends Neurosci, 36 (2013), 336–342. [30] D. Saal, Y. Dong, A. Bonci, and R. C. Malenka, Drugs of abuse and stress trigger a common synaptic adaptation in dopamine neurons, Neuron, 37 (2003), 577–582. [31] W. Schultz, Reward signaling by dopamine neurons, Neuroscientist, 7 (2001), 293–302. [32] M. Srinivas, M. G. Hopperstad, and D. C. Spray, Quinine blocks specific gap junction channel subtypes, Proc Natl Acad Sci U S A, 98 (2001), 10942–10947. [33] K. Stengård, G. Höglund, and U. Ungerstedt, Extracellular dopamine levels within the striatum increase during inhalation exposure to toluene: A microdialysis study in awake, freely moving rats, Toxicol Lett, 71 (1994), 245–255. [34] M. A. Ungless, J. L. Whistler, R. C. Malenka, and A. Bonci, Single cocaine exposure in vivo induces long-term potentiation in dopamine neurons, Nature, 411 (2001), 583–587. [35] M. Watabe-Uchida, L. Zhu, S. K. Ogawa, A. Vamanrao, and N. Uchida, Whole-brain mapping of direct inputs to midbrain dopamine neurons, Neuron, 74 (2012), 858–873.