* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download Sexually transmitted infections (STI)
Survey
Document related concepts
Transcript
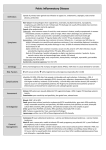
Sexually transmitted infections (STI) Recommend In remote Indigenous settings, all sexually active men and women under 40 years should be offered a test for chlamydia, gonorrhoea, syphilis and (trichomonas for women only) at least once each year and men and women aged 40-49 years should have syphilis serology annually Symptomatic cases and contacts of individuals with a known STI must be treated on the spot at first presentation (presumptive treatment). Do not wait for pathology results Background Chlamydia is the most common notifiable STI in Australia. Chlamydia and genital herpes are seen in all areas; gonorrhoea and trichomoniasis are common in rural/ remote regions while genital warts are a frequent presentation in urban areas. Syphilis persists in remote populations and a significant epidemic is continuing among urban non-Indigenous men who have sex with men Excessively high rates of chlamydia and gonorrhoea persist in remote regions leading to psycho-social distress, gynaecological problems, pregnancy loss, infertility and a population particularly vulnerable to an epidemic of HIV infection Related topics: How to do an STI check, page 466 1. May present with: The following tables are a guide to STI presentations: Males may present with / as: Symptom Urethral discharge Pain / swelling in the testes/scrotum (Epididymo – orchitis) Genital sores ulcers Contact of a person with an STI Contact has positive test for chlamydia and/or gonorrhoea Contact has positive test for trichomonas Contact has infectious syphilis Contact has donovanosis Contact of symptomatic person Contact has vaginal discharge, pelvic inflammatory disease (PID) Contact has genital sores ulcers Contact has urethral discharge or testicular pain/swelling Positive pathology (index) Chlamydia &/or gonorrhoea Syphilis (Always call the Public Health Nurse, Syphilis Register for up to date results and treatment details on 1800 032 238) Herpes Donovanosis Trichomonas Refer to: Females may present with / as: Symptomatic Vaginal discharge Low abdominal pain Genital sores ulcers Contact of a person with an STI Contact has positive test for chlamydia and/or gonorrhoea Contact has infectious syphilis Contact has Donovanosis Contact has positive test for Trichomonas Vaginalis Contact of a symptomatic person Contact has urethral discharge Contact has testicular pain/swelling Contact has genital sores/ulcers Positive pathology test (index) Chlamydia and/or gonorrhoea Trichomonas Candida Refer to: Urethral Discharge / Dysuria Epididymo-orchitis Genital Sores / Ulcers Urethral Discharge/ Dysuria Urethral Discharge / Dysuria Syphilis Genital Sores / Ulcers Urethral Discharge / Dysuria Genital Sores / Ulcers Urethral Discharge / Dysuria Urethral Discharge/ Dysuria Genital Sores / Ulcers Genital Sores / Ulcers Genital Sores / Ulcers Urethral Discharge / Dysuria Vaginal discharge Low abdominal pain Genital sores ulcers Vaginal discharge - Cervicitis Syphilis Genital sores ulcers Vaginal discharge - Vaginitis Vaginal discharge - Cervicitis Vaginal discharge - Cervicitis Genital sores ulcers Vaginal discharge - Cervicitis Vaginal discharge - Vaginitis Vaginal discharge - Vaginitis Bacterial Vaginosis Syphilis (Always call the Public Health Nurse, Syphilis Register for up to date results and treatment details on 1800 032 238) Donovanosis Genital Herpes Vaginal discharge - Vaginitis Syphilis Genital sores ulcers Genital sores ulcers Men with gonorrhoea and chlamydia may present with: Positive gonorrhoea or chlamydia test (asymptomatic infection) Named as a “contact” of someone with gonorrhoea, chlamydia, PID or other STI Urethral discharge, and/or pain or burning on passing urine (dysuria) Pain and swelling in the testes (epididymo-orchitis) See Testicular / scrotal pain or Epididymo-orchitis Women with gonorrhoea and chlamydia may present with: Positive gonorrhoea or chlamydia test (asymptomatic infection). Named as a “contact” of a male with gonorrhoea, chlamydia, urethritis (discharge or dysuria) or epididymo-orchitis Cream, yellow or blood stained discharge or cervix bleeds easily when swabbed Abnormal bleeding: inter menstrual bleeding, after sex (post coital) Low abdominal pain (PID) PV bleeding during pregnancy: threatened miscarriage, preterm rupture of membranes, preterm labour, neonatal infection, post partum infection 2. Immediate management: Symptomatic cases and contacts of individuals with a known STI must be treated on the spot at first presentation (presumptive treatment). Do not wait for pathology results 3. Clinical assessment: Recommend Offer all sexually active young women and men under 40 years an STI check for chlamydia, gonorrhoea, syphilis and trichomonas (for women) and men and women aged 40-49 years should have syphilis serology at least once each year in Aboriginal and Torres Strait Islander settings Please read: Important information relating to history, examination, testing, management, contact tracing and follow up How to do an STI check? An STI check includes reproductive / sexual history, physical examination, appropriate testing and education. History: The extent of the history depends on the presentation. If someone presents with symptoms, is a named “contact” or requests an STI check then: take a reproductive history including menstrual, obstetric, contraceptive and Pap smear history take sexual history assess STI risk: new partner, multiple partners (or partner has multiple partners), regular, casual partners, same sex partners condom use recent history of STI nature of sexual intercourse - do they have oral, vaginal, anal intercourse Assess blood born infection (BBI) risk: injecting drug use (IDU), tattooing, body piercing, prison term Symptoms, ask about: urethral / vaginal discharge; onset, colour, odour etc pain on passing urine (dysuria) abnormal vaginal or rectal bleeding genital rashes, lumps and sores itching / discomfort in the perineum, perianal and pubic region low abdominal pain in women pain with sex (dyspareunia) if an STI spreads it may cause symptoms such as fever, muscle / joint pains, rashes, enlarged lymph nodes Examination: if a client has no symptoms and is not a “contact”, then examination is often not necessary. The extent and nature of the examination depends on the history and requires client consent. It may include: the mouth, the skin (rash), lymph nodes for swelling or tenderness the abdomen for tenderness See Acute abdominal pain, and Low abdominal pain in female the external genitalia including the perianal area for rashes, lumps, sores in men - urethra for discharge, inflammation; testes and epididymis for tenderness, swelling women – vulva / vagina / cervix for inflammation, discharge, bleeding and bi-manual examination for tenderness and masses See Health Check – women Testing: See STI Specimen collection All STI testing must be done with the client’s knowledge and informed consent; pre-test information and discussion is particularly important in relation to HIV testing See HIV Infection STI tests should be appropriate to the sex acts performed (oral, anal, vaginal) The regional sexual health service will provide advice if needed In remote Indigenous settings an STI check should include tests for chlamydia, gonorrhoea, trichomonas, syphilis, HIV, hepatitis B (if not immune), hepatitis C virus (testing is offered for surveillance purposes) If there is a genital sore, in addition to the above, collect tests for Genital Ulcer Disease (GUD) The STI tests offered to young clients annually (in the 15-54 year Health Check) and opportunistically are: chlamydia gonorrhoea syphilis trichomonas (women only) The investigation of an STI diagnosis e.g. chlamydia, includes the offer of testing for the other common STI, and for HIV and Hepatitis C. Hepatitis B immune status should be established and vaccination offered if not immune and not a carrier (See Hepatitis); if immune or documented to be fully vaccinated, it is not necessary to repeat at each STI check 4. Management: Education and Prevention: Assure the client that his/her confidentiality will be protected Give information about the transmission, symptoms and complications of STI Discuss safe sex practices and provide condoms If treatment is needed, explain: - the need to abstain from sex until the partner has been treated, and contact tracing: why and how (see next page) Medication management Symptomatic cases and contacts of individuals with a known STI must be treated on the spot at first presentation (presumptive treatment). Do not wait for pathology results. Aim to treat all pathology detected cases within one week of testing Clients with symptoms are treated on day of presentation syndromically: urethral discharge / dysuria: treat for chlamydia, gonorrhoea and trichomoniasis; see Urethral discharge vaginal discharge / cervicitis: treat for chlamydia, gonorrhoea and trichomoniasis see Vaginal discharge genital ulcer disease: consider treatment for syphilis, donovanosis and/or genital herpes. see Genital sores / ulcers If single dose treatments are used, watch the client take the medication and document this in the medical record Once only treatment is highly effective and if taken, a “proof of cure” test for chlamydia / gonorrhoea is not necessary. Re-test at three months to check for re-infection If a course of treatment is indicated, explain that the course must be completed to be reasonably sure of cure Tell the client that if they have problems with the medication, to notify the clinic and seek advice rather than stopping the treatment Contact Tracing: Is essential to prevent reinfection in the client (index case) you are treating, may also stop further transmission to others and must always be done in private. Confidentiality must be ensured. Names of all “contacts” from the previous 3 months (at minimum) are requested (this may be longer depending on the STI (GUDs) The name of the index case must never be disclosed to the “contacts” Document in the “contact’s” medical record that they need immediate treatment for that STI and testing for the other common STI Do not write the name of the index case in the “contact’s” medical record, do not write the name of the “contact” in the medical record of the index case The client may choose to inform their “contacts” themselves or may want the clinic staff to do this If clinic staff are initiating contact tracing, then three attempts (telephone or home visits) should be made and documented Notify the appropriate health service staff if a named contact is outside your health centre’s area. Consult the MO or sexual health clinic if you need advice or help with contact tracing 5. Follow-up Encourage follow up at one week: check adherence with medication and symptom resolution check test results: STI results (especially HIV results) should be given in person check that partner/s have been tested and treated and contact tracing initiated reinforce education and prevention information and check condoms supplied encourage client to return at 2-3 months for a repeat check and encourage client to present for a check any time they get symptoms or are at risk of STI (eg new partner) Every client with an STI diagnosis should have an STI check at 2 to 3 months after initial treatment people who have had an STI are at high risk of being reinfected, often because their partner was not treated. About 33% become reinfected within 3 months therefore a follow up STI check in 3 months is extremely important clients treated for infectious syphilis ie syphilis of less than 2 years duration, should be tested at 3 - 6 months and again at 12 months see Syphilis HIV test should be offered at the time of initial STI diagnosis, however a repeat test may be needed at 6 weeks - after the “window period” see HIV Infection Condoms Make sure condoms are freely available and can be obtained easily and in private To use a condom: check expiry date when opening packet (take care with sharp fingernails, rings, etc.) squeeze the end of the condom to keep air out of the tip gently roll condom down the shaft of the erect penis before having sex use only water based lubricant (eg. wet stuff, glyde, sylk) do not use paraffin based lubricants such as baby oil or vaseline as this can make the rubber perish when finished, the base of the condom should be held on withdrawal so it is not left inside the partner used condoms should be put in the rubbish, not down the toilet do not store condoms in a hot place as this can make the rubber perish The recommendation for (at least) annual STI testing (chlamydia, gonorrhoea, syphilis) for men and women (plus trichomonas vaginalis for women) under 40 years of age can be incorporated into routine care in a number of ways; offer STI tests when clients (particularly 15-24 years age group) present for other reasons (opportunistic screening) as part of an annual Health Check (in Qld, see current edn. of Chronic Disease Guidelines) women presenting for a Pap smear (cervical screening) – include a PCR swab for trichomonas women presenting for contraception, emergency contraception or referral for termination of pregnancy Reporting in relation to sexual acts involving young people. See Abuse and neglect (child) and Rape / sexual assault If an STI is diagnosed in a young person (<16 years of age), Queensland Health guidelines require a comprehensive assessment of the young person’s safety if an STI is diagnosed in someone <14 years of age, then staff are required to notify the Queensland Health Child Safety officer within the District for more information go to qheps.health.qld.gov.au/csu/Factsheets.htm for clinical risk factors and indicators for sexual abuse qheps.health.qld.gov.au/csu/pdf/fact_sheets/FactSheet4-5.pdf