* Your assessment is very important for improving the work of artificial intelligence, which forms the content of this project
Download eprint_11_21608_689
Transtheoretical model wikipedia , lookup
Women's medicine in antiquity wikipedia , lookup
Maternal physiological changes in pregnancy wikipedia , lookup
Prenatal development wikipedia , lookup
Prenatal nutrition wikipedia , lookup
Prenatal testing wikipedia , lookup
Fetal origins hypothesis wikipedia , lookup
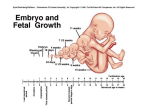
MANAGEMENT OF LABOUR: When a pregnant woman started labour or when she has spontaneous rupture of membranes at term she should be admitted and full assessment of her condition is accomplished. To start with: FULL HISTORY ON ADMISSION about the The frequency, strength and duration of her contractions and when they began Is there any history of watery vaginal discharge or bleeding, and ask about the colour and amount of the amniotic fluid lost if there is SROM. Details of her past obstetrical history, mode of deliveries, any history of delivering big baby? C/S LMP, GA , ask her about her ANC (it is better if she is bringing her ANC card with her), any problem during the current pregnancy (medical or obstetrical) like PIH, APH or reduction in the fetal activity or IUGR. Ask her about the recent activity of her fetus. Then we PROCEED FOR EXAMINATION of the woman General examination, her vital signs: BP, temp., PR, Then abdominal examination: for any previous scars, Leopold's maneuvers are a series of four abdominal palpations of the gravid uterus that can be used to ascertain fetal lie, presentation, and estimated weight. The fundus is palpated to ascertain the presence or absence of a fetal pole (longitudinal or transverse lie) and the nature of the fetal pole (cephalic or breech). The lateral walls of the uterus are examined using one hand to palpate and the other to fix the fetus. In longitudinal lies, the lateral uterus is usually occupied by the fetal spine (long, firm, and linear) and small parts or extremities. The nature and station of the presenting part is determined by palpating above the symphysis pubis. If the presentation is vertex, the cephalic prominence is palpated to determine the position of the fetal head. If the head is well flexed, neither chin nor occiput will be prominent. also assess the engagement which is an important sign for good progress of labor, unengaged head should raise the suspicion of malposition or deflexed head or may be any abnormality in the pelvis that prevent the descent of the presenting part like a uterine fibroid, ovarian mass or placenta previa. In case of deeply engaged head then the head can not be felt by abdominal examination (rule of five fifths) and it is called to be in zero station while if you can feel the whole of the head suprapubically it is called to be floating head which is a bad sign, if only two fifths of the fetal head can be palpated abdominally so the head is engaged . Assessment of the uterine contractions is performed by direct abdominal palpation for at least ten minutes to count the number of contractions, strength and frequency during these ten minutes. Also FHR should be checked at the start by a pinard stethoscope or sonicaid to prove viability and exclude fetal compromise. Vaginal examination after taking her consent, we have to explain the purpose and technique of the procedure for the patient: Then the index and middle fingers are passed to the top of vagina and cervix gently to assess the dilatation of the cervix digitally in centimeters (if the cervix is not palpable this means 10 cm dilatation), effacement by % of the cervical canal length which is normally 3 cm at 36 weeks of gestation (if I find it 1.5 cm I can say that it is 50% effaced). (Effacement) If the cervix is 3 cm dilated or more the position of the presenting part can be assessed, the position is defined by the relation of the land mark or the denominator of the presenting part to the maternal pelvis as in vertex presentation the occiput must be determined if it is (RT or LT) occipito-transverse, or if it is in oblique position like the( RT or LT) occipito-anterior, or the (RT or LT) occipito- posterior when the occiput related to the RT sacroiliac joint or the LT one respectively. (positions) The occiput can be identified by vaginal examination if the patient has ruptured membranes, by identifying the posterior fontanel(triangular), failure to find the posterior fontanel may be due to deflexed head or due to caput which is the edema of the presenting part which obscure the landmarks during examination. If there is ruptured membranes the color and amount of the coming fluid should be assessed if large amount of clear fluid or scanty with blood or meconeum staining which is a warning sign of fetal distress. MANAGEMENT OF THE 1ST STAGE: Woman in the latent phase should be encouraged to mobilize. Intervention during the latent phase is better to be avoided unless it is indicated, give her simple analgesia, light foods and drinks are allowed. urine testing (for protein and glucose), CBC, and drawing of a blood bank sample to be available for cross-matching if needed. Intravenous access is recommended. Maternal blood pressure (BP) and pulse should be recorded every hour during the first stage of labor and every 10 minutes during the second stage of labor. Vaginal examination in early labour is infrequently performed (4 hourly is the standard) and the frequency may be increased accordingly to assess dilatation and descent of the presenting part. If the membranes are intact it is not necessary to do ARM if the labor is progressing well. Adequate monitoring of both the maternal and fetal conditions should be done, giving her antacid, adequate analgesia and may be urinary catheter if labor is prolonged and abnormal. It is better to evacuate the rectum ( may be done by enema) in the 1st stage in preparation for the 2nd stage because if the rectum is full there will be soiling and contamination of the vulva in the 2nd stage when the presenting part start to compress the rectum. All of the data obtained since the admission to the labour world should be recorded in a graphical manner which is called partogram. (PARTOGRAM) MANAGEMENT OF THE SECOND STAGE: When the cervix is fully dilated and the presenting part starts to distend the perineum the mother start to experience an urge to push (valsalva manoeuvre). The woman adopt a lithotomy position, or left lateral position to prevent the compression of the inferior vena cava by the gravid uterus, or semi sitting position in order to get benefit from the gravity, the pushing should be organized with the contractions to be effective. The fetal heart must be listened to during contractions and after contractions to be sure of the fetal wellbeing. When the head stretch the perineum the anus will begin to open and the baby's head is visible at the vulva with the contractions. When the head pass under the subpubic arch, the biparietal diameter is seen at the vulva which is known as the crowning (the head passed the pelvic floor and delivery is imminent), and here the midwife must prevent the head from being delivered suddenly which may cause perineal laceration, so she has to advice the mother to stop pushing down and ask her to take rapid shallow breaths, she has to press through the perineum onto the forehead to prevent the head from extension while controlling the rate of escape of the head by the other hand( called modified Ritgen's manoeuvre). The goals of assisted spontaneous vaginal delivery are reduction of maternal trauma, prevention of fetal injury, and initial support of the newborn. Episiotomy is an incision into the perineal body to enlarge the vulval outlet and facilitate delivery, it is of two types: 1- Midline episiotomy which may extend into the anal sphincter and cause 3rd or 4th degree perineal tears. 2-Mediolateral : less sphincteric injury but more blood loss and more post partum pain. Once the head is delivered the cord must be checked if around the neck it may cause difficulty in delivering the rest of the body. Then the delivery of the anterior and posterior shoulders is performed as mentioned in previous lecture then the delivery of the rest of the body. If the amniotic fluid is meconeum stained a nasopharyngeal suction for the baby must be done before it takes its 1st breath to prevent meconeum aspiration. There is no need for immediate cord clamping it is advisable to waite for a while to infuse more blood from the placenta to the baby to prevent neonatal iron deficiency anemia. Before discharging the baby from the delivery room apgar score at 1minute must be checked and a wrist label is applied for identification. MANAGEMENT OF THE THIRD STAGE OF LABOUR: It the stage of placental separation and expulsion, we mentioned its normal duration, and signs of placental separation I a previous lecture. Placental separation occurs as a result of reduction of the volume of the uterine cavity by the contractions and retraction. A cleavage plane developed within the deciduas basalis and the placenta lies free in the lower uterine cavity. We can actively follow: manage the 3rd stage by a controlled cord traction as 1) Give her 10 units oxytocin or syntometrin( 5 unit oxytocin+ 0.5 mg ergometrine) with the delivery of the anterior shoulder to induce uterine contractions immediately after the delivery of the baby 2) 1-2 minutes after baby's delivey clamping the cord 3) When contraction is felt by the midwife's left hand placed suprapubically gentle pushing of the uterus upward and by the other hand grasp the cord and apply gentle traction downward to facilitate placental separation, all of the membranes must be peeled off with twisting motion. 4) Never pull the cord when the uterus is not contracted because of risk of uterine inversion Active management of the 3rd stage shortens the 3rd stage and reduce the risk of postpartum haemorrhage. Figure above shows: (A and B)- Controlled cord traction. C- Manual removal of the placenta in case of retained placenta. After placental delivery it should be inspected for any lost cotyledons or succenturiate lobe. Finally the vulva must be inspected for any tears or lacerations in order to repair them. What are the CRITERIA or the features of normal labour? 1- spontaneous onset 2- single cephalic presentation 3- 37-42 weeks gestation 4- no artificial interventions 5- unassisted spontaneous vaginal delivery 6- > than 12 hrs in nulliparous and > than 8 hrs in multiparous 7- healthy mother and baby 8- retrospective diagnosis.